Abstract
A growing number of studies suggest that migrant and ethnic minority populations are at higher risk for being diagnosed with psychosis. However, the reasons why have been disputed. This study aims to explore different interpretations of the observed higher rates of psychosis diagnosis among immigrants and ethnic minorities in some parts of the world. We sought to examine these interpretations through a critical lens, acknowledging the social underpinnings of discourses and their power to shape real-world practices. Peer-reviewed editorials, commentaries and letters regarding the topics of interest were retrieved from database searches and subjected to a pattern-based critical discourse analysis. Across a 30-year span of literature, conceptualizations and explanations of higher psychosis rates amongst migrant and minoritized populations evolved in relation to the larger social context, at times opposing one another. Three discursive themes were identified, reflecting intersecting explanations: institutional racism in psychiatry; psychiatry as a scientific discipline that sees and treats all patients equally; and the social locus of high rates. Tensions surrounding psychiatry as a field, including issues of evidence, biological reductionism, and the conceptualization of psychiatric nosological categories have played out within the evolution of this discourse. Exploring how discursive constructions in relation to psychosis and minoritization have been shaped by historical and social factors, we consider the role of local and global dynamics of social power in favouring one explanatory model over another and how these may have affected efforts to prevent and better treat psychosis amongst immigrant and minoritized groups.
For several decades now, higher rates of psychosis have been reported for some migrant and ethnic minority populations, making migration, as a risk factor for psychosis, one of the most consistently replicated findings in psychosis research (Radua et al., 2018). This higher risk has been reported to persist in later generations, and to be higher for racialized minorities and for individuals migrating from the Global South to Northern European countries such as the Netherlands and the United Kingdom (UK) (Selten et al. 2020). Currently, these findings have been framed in the context of higher exposure to social adversity (e.g., material and social deprivation, childhood adversity experiences, marginalization and discrimination) that punctuates the everyday realities of individuals belonging to some minoritized populations. Prior explanations, like biological causes or selective migration, have largely been discredited (Morgan et al., 2019).
Several scholars have also highlighted that migrant and ethnic minority populations (and in particular, Black ethnic minorities) have been historically subject to diagnosis bias (Hairston et al., 2019; Hampton, 2007), and that the psychosis diagnosis has been used as a means to exert social control, following political agendas, for instance, by conflating issues of violence and mental illness and labelling those who rebel against the system or do not conform to social norms as dangerous, deviant or mentally ill (Metzl, 2010). Relatedly, given that social and cultural backgrounds shape human experience and behaviour, the use of diagnostic instruments that disregard such backgrounds has been seen as problematic, as these have been developed within a western framework of health, illness and self (Adeponle et al., 2012; Gara et al., 2012; 2019; Zandi, Havenaar, Smits, et al., 2010).
The various interpretations of these findings demonstrate the complexity inherent to explanation of psychiatric disorders. Indeed, the breadth of psychiatry has fostered input from diverse disciplines that use remarkably different languages and follow distinct philosophical paradigms (Cooper, 2007) that are sometimes at odds with each other. For instance, mental disorders may be conceptualized as factual entities or as value-laden social constructions; their causes may be perceived to arise primarily from inside or outside the individual; and the preferred ways to understand them may place more emphasis on causes or processes, on case-stories/narratives, or on global/universal laws (Zachar & Kendler, 2007). Preferred explanations depend on the diagnosis being considered, the stakeholder group in question (clinicians, researchers, or patients) and the overarching social and cultural context (Kirmayer, 2018; Kleinman, 1977; 1987; Rosenthal Oren et al., 2021; Young, 1982). For instance, many psychiatrists and scholars from Europe and North America emphasize that psychotic disorders arise more from biogenetic than psychosocial causes. (Brog & Guskin, 1998; Colombo et al., 2003; Harland et al., 2009; Miresco & Kirmayer, 2006).
How different causes of a specific phenomenon of interest are valued and which ones take precedence over others are shaped by the opinions of academics about what gets published, along with the social and cultural contexts in which they are generated. As such, discursive constructions put forward by academics regarding mental disorders set the tone for what is considered valid knowledge and deeply influence general opinion, research, clinical work, policymaking, and possibly the very manifestation of mental disorders, through looping effects, in the settings where these categories are being used (Hacking, 1995; 1999). In turn, these discourses are largely determined by the social, political and historical contexts in which research and clinical activities are embedded (Foucault, 1972; Jarvis & Kirmayer, 2021; Kuhn, 1970).
Objectives
In this study, we describe and critically analyze academic discursive constructions regarding the reported findings of more psychosis diagnosis among migrants and ethnic minorities. By doing this, we aim to unpack underlying assumptions and attributed meanings concerning causality, processes, consequences and proposed courses of action, while retaining focus on the social and historical contexts in which these discursive constructions emerged and played out.
Method
As the focus of the study was not only to describe discourses on the topic of interest but also to elucidate their underlying social meanings, we conducted a critical discourse analysis (Fairclough, 1985; 1989; 1992), using a pattern-based approach (Potter and Wetherell, 1994; Willig (1999). Accordingly, we developed this study under the assumption that discourses express tacit knowledge systems embedded in particular social structures that are in turn influenced by power dynamics and relationships. Furthermore, discourses also have an active role in shaping social realities (Foucault, 1972). Analysis of discourses was thus centred on the multiplicity of their meanings, and their connections and functions and their social relatedness.
According to Fairclough (1992), the corpus of data for critical discourse analysis should be constituted by a comprehensive (although not necessarily exhaustive) collection of documents that are representative of discourses on the topic of interest. These documents should cover a broad range of discourses and be considered relevant for people in the specific context of the social practice in focus (in this case, scholars and clinicians in psychiatry doing research and/or working with minoritized communities). Considering this and the study's aims, an online search was conducted to identify editorials, letters, opinion articles and commentaries. These documents were chosen because they are inherently argumentative, revealing implicit beliefs and motivations. Furthermore, these are usually concise papers that focus on specific issues that influential scholars consider to be of relevance.
The online search started with major databases in the field of psychiatry, such as PubMed/Medline, EMBASE and PsycINFO, using general keywords related to the topics under investigation (e.g., psychosis, migrants, immigrants, ethnic minorities, racial minorities). Additional searches were conducted on an ongoing basis during the process of analysis and writing of results to generate a more comprehensive collection of documents. This was achieved by adding new search terms (e.g., Black, race, racism, Asian, African American, Latino, African-Caribbean); searching in additional databases (JSTOR, SCOPUS); and searching the online archives of high-impact psychiatric journals. Attention was paid to retrieving research materials containing interpretative repertoires from various fields within and related to psychiatry (e.g., social psychiatry, phenomenology, epidemiology, etc.). The initial data corpus was complemented by searches within the reference lists of the initially retrieved documents and the final choice of editorials, letters, opinion articles and commentaries was refined by consulting experts in the field. Searches were restricted to peer-reviewed journals published in English, starting from 1990. The authors chose this date range with the intent of focusing on material reflecting a contemporary era in the study and treatment of psychotic disorders. By then, atypical antipsychotics were on the market, first episode psychosis was taking off as a clinical organizing construct, and the fourth and 10th versions of the DSM and ICD-10 were underway (Bürgy, 2008; McGorry et al., 1996).
After an initial stage of familiarization with the data, initial discursive themes were identified by the first author. These were grouped together checking for patterns, variability, consistency, functions and effects. The interpretation of the themes was conducted by a process of multiple readings, referring to relevant literature to situate discourses in historical, political and sociocultural contexts. Themes were checked against the texts, examined for differences and convergences, combined and aligned with examples of quotations defining main and sub-themes (Potter & Wetherell, 1994).
Both authors of this article are clinicians and researchers in the fields of psychosis, and social and cultural psychiatry. Both have experience in the field of interest to this paper and in qualitative research methodologies. Overall, data analysis was guided by a contextualist paradigm (Braun & Clarke, 2006), aligned with the critical discourse analysis method (Jorgensen & Philips, 2002). This approach is situated between essentialist and constructivism paradigms and assumes an ontological stance of critical realism. This perspective acknowledges the existence of a concrete social reality, which may only be partially grasped, namely, through the analysis of discursive constructions. Epistemologically, this study adopted a position of subjectivism, acknowledging that meaning is co-constructed by the interpreter and the phenomenon of interest and is fundamentally shaped by social, cultural, historical and political contexts. (Braun & Clarke, 2006). To ensure rigor, several measures were implemented, including prolonged engagement, multiple readings, debriefing sessions, consulting with specialists, and the elaboration of an audit trail (Cho & Trent, 2006; Padgett, 1998).
Results
A total of 54 documents was subjected to analysis. Of these, 40 were written by scholars based in Western European countries, of which 32 came from the UK, 7 from Netherlands and 1 from Germany. The remaining publications came from the United States of America (USA) (n = 10), Canada (n = 2), Georgia (n = 1) and India (n = 1). The analyzed documents portray a vivid debate about issues related to excess rates of psychosis diagnosis and coercive hospitalization in migrant and ethnic minority communities. The titles of the chosen papers varied in their tone and purpose, being at times provocative, alarming, blaming, and at other times serving as calls to action or reconciliatory statements (see Table 1 for more details about included papers). Scientific arguments and personal ideologies were often conflated, shaped by the historical and sociocultural context of the nations where these discourses were generated (mostly the UK and to a lesser extent the USA), acknowledging that discourses may originate in one place and time, be picked up somewhere else and then appear again later at the point of departure. The different discursive themes correspond to attempted explanations of psychosis risk among minoritized communities and map onto larger, often opposing, discourses on psychiatry, psychosis, migration, race and ethnicity: 1) Institutional racism in psychiatry; 2) Psychiatry as a scientific discipline that sees and treats all patients equally; and 3) The social locus of high rates (Figure 1). Additionally, two sub-themes were identified under the first discursive theme (Misdiagnosis and Problematizing psychiatry as a discipline), and one sub-theme was identified under the third theme (Aiming for interdisciplinarity). Sub-themes refer to aspects discussed under the first and third themes that deserved particular attention across the analyzed documents. Discursive constructions suggested links to underlying assumptions about what the problem was considered to be (i.e., the higher risk for psychosis among some ethnic minorities versus racism within psychiatric institutions), and about its causes and possible solutions. For each theme, we sought to describe and give examples of a given discursive construction, and to situate it within the larger landscape of discourses and counter-discourses. Accordingly, while all quotations were extracted from the analyzed documents (see Table 1), in agreement with the chosen methodology, we referred to other publications throughout the text to establish context. For clarity, all citations referring to analyzed documents are indicated with an asterisk. While the first two themes coexisted temporally and developed in opposition to each other, the third theme portrays a relatively more recent focus on the social determinants of (mental) health and an attempt to integrate social adversity within prominent explanatory models in psychiatry.
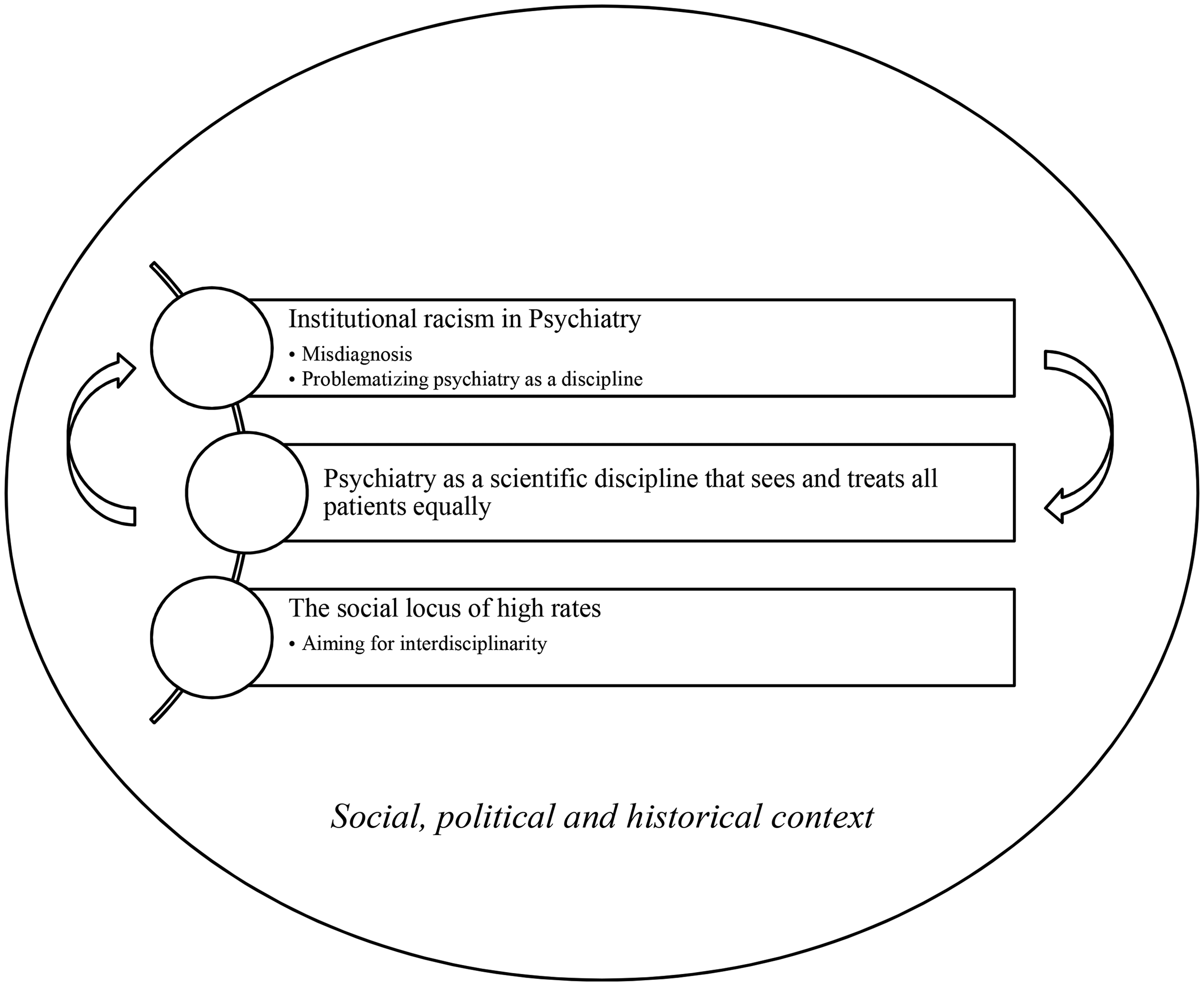
Discursive constructions on explanations for the high rates of psychosis among migrant and ethnic minority populations. The depicted themes and sub-themes represent explanations of the epidemiological findings of higher rates of psychosis in minoritized populations. The themes emerged from a critical discourse analysis of academic papers across a 30-year span. The first two themes were contemporary and evolved in opposition to each other; the third theme represents a more recent focus on the social determinants of (mental) health.
Articles included in the analysis.
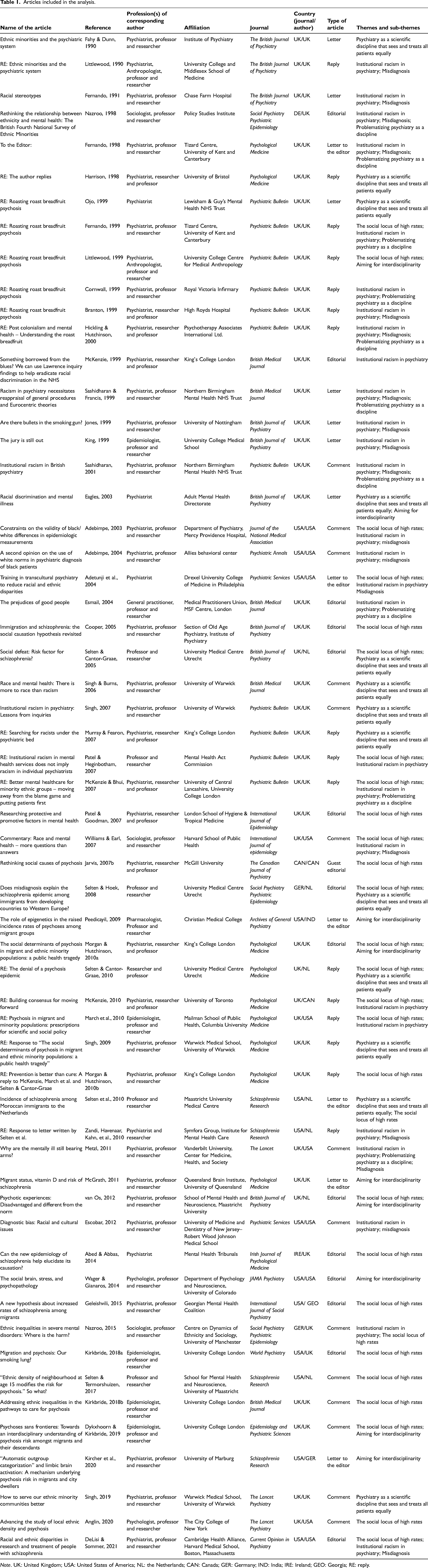
Note. UK: United Kingdom; USA: United States of America; NL: the Netherlands; CAN: Canada; GER: Germany; IND: India; IRE: Ireland; GEO: Georgia; RE: reply.
The most vivid academic debate regarding rates of psychosis in migrants took place in the UK from the late 1990s to the early 2000s. The discussions were underpinned by historical events, notably two national inquiries on racial discrimination that prompted a national debate on institutional racism. The first concerned the contentious conduct of the police over the investigation of the racially motivated murder of a Black teenager, culminating with a report that denounced and criticized the practices of the police and suggested ways to tackle institutional racism (Macpherson, 1999). The second concerned the death of a young Black man with schizophrenia following the use of physical restraints in a psychiatric institution. The report mentioned that the patient had earlier been involved in an altercation that had followed his being racially abused by another patient (Norfolk, Suffolk and Cambridgeshire Strategic Health Authority, 2003). This last inquiry extended to broadly analyze the ways that Black and other ethnic minority communities were treated in mental health services, concluding that these populations were not getting the care they needed due to institutional racism within the National Health Service in England. At that time, service users and practitioners expressed concerns over racial inequalities within mental healthcare. Simultaneously, higher rates of psychosis diagnosis (Harrison, 1990; Harrison et al., 1997) and coercive admissions (Cole et al., 1995) were reported among Black (especially Black Caribbean) communities in the UK. The debate surrounding the issues of race, ethnicity and psychosis has been alive ever since and it has extended to other locations in Europe where similar findings have been reported (Selten et al., 2001; Zolkowska et al., 2001). The three themes (and their sub-themes) are detailed below.
Institutional racism in psychiatry
Across some analyzed documents, psychiatry, as an institution, was criticized for its inability to provide good care to ethnic minorities and for discriminating against these communities, and for contributing to the maintenance of patterns of social stratification based on race. Several scholars pointed out that besides having less access to mental health services and facing harsher pathways to care, minoritized populations have also been targets of prejudiced diagnostic procedures and research agendas by psychiatric institutions, attitudes or practices that can be traced back to 19th century “race science”, whereby theories of racial or ethnic inferiority attempted to justify or support biased and discriminatory attitudes toward certain groups based on their race or ethnicity. As two scholars from the UK, put it, The testimony of Black patients and carers and the perceptions of the Black communities also appear to be consistent with this general theme that there is no aspect of contemporary psychiatric care that favours Black people when compared to White patients and, in overall terms, psychiatry, like policing, the criminal justice system, educational institutions and social work, militates against the interests of Black people in this country. (Sashidharan, 2001, p. 246)*1 The disproportionate numbers of black people in psychiatric detention, the overdiagnosis of schizophrenia in black people, the exclusion of black people from the “softer end” of psychiatric practice […] the alienation of black patients from mainstream psychiatric services, the general lack of trust and extreme skepticism about psychiatric practices […] the professional preoccupation with theories of ethnic vulnerability or inferiority, which continue to echo the sentiments of 19th century “race science”, all confirm the similarities between policing the black communities and controlling their minds. (Sashidharan & Francis, 1999, p. 254)*
The previous quotation also aligns psychiatry with the police—both are institutions concerned with surveillance, control and risk management of Black communities. The points raised by these authors greatly overlapped with earlier discourses from North American scholars, that were particularly prolific in the aftermath of the civil rights movement (Adebimpe, 1981; De Hoyos & De Hoyos, 1965; Neighbors et al., 1989; Simon et al., 1973). In the documents included in our analysis, we saw this issue being brought up by Metzl (2011)*, who underlined the ways in which societal structures of power had permeated psychiatric ideologies and practices, namely, by defining the typical patient with mental illness as a violent Black man: From a historical perspective, shifting connections between violence and mental illness also connect uncomfortably with shifting anxieties about race. In the 1960s and 1970s, many of the men depicted as being armed, violent, and mentally ill were, it turned out, African American. (p. 2172)
Misdiagnosis
The excess rate at which psychosis is diagnosed among ethnic minorities has been interpreted by some scholars, physicians and minoritized populations to be the result of diagnostic error due to clinician racial biases. These biases have been suggested to arise from a misinterpretation of culturally shaped emotional distress and social suffering, such as mistrust of authority and reluctance to be open with treatment providers, as paranoia. This point was supported by Sashidharan and Francis (1999)*, who argued against the uncritical attribution of diagnostic categories based on Eurocentric theories: The theories and assumptions of psychiatry are problematic when they are applied to people who are socially excluded or culturally marginalized. Black communities in the United Kingdom will continue to bear the brunt of such a professional bias as long as the coordinates of psychiatric practice remain fixed. (p.254)
One important argument used to support the misdiagnosis hypothesis was that the high rate of psychosis diagnosis found in clinical reports and treated incidence studies was not as pronounced in population-based studies in the UK (Nazroo, 2015)*.
A similar point had previously been made by North American scholars, such as Adebimpe (2004)*: The evidence for racial equality in the distribution of mental disorders came from two national surveys in which major technical problems of earlier studies were solved. […] Each showed an equal distribution of mental disorders in its community sample, putting to rest more than a century of controversy and biased debates. (p. 544)
While the results of these surveys contributed to a shift of discourse in the USA, scholars involved in the studies reporting higher rates of psychosis among minoritized populations in the UK stressed that these findings were too pronounced to be disregarded or solely attributed to misdiagnosis. Moreover, some scholars considered that denying these rates hindered scientific progress and fostered distrust in the system. As a result, vulnerable populations would be further alienated from adequate care: The question of the increased rates of psychotic disorders reported in these papers is too important to be reduced to simplistic formulations […]. In particular, we must avoid unwise generalizations about misdiagnosis, which risk alienating mentally ill people from the services they need and which may delay effective and speedy intervention and treatment. (Harrison, 1998, p. 497)*
The debate has so far been conducted in a Black and White manner, with psychiatrists seen as oppressors and patients as victims […]. We would not consider blaming hospital physicians for the rising rates of obesity in the population […]. Staff in such services need our support for doing a difficult job in difficult circumstances, not our disdain for failing this or that group. (Singh, 2007, pp. 365, 364)*
Statements like the one above, that interpret statements about institutional racism in psychiatry as directly attacking healthcare providers, were considered by some to be over-reactions born of misunderstanding. As Patel and Heginbotham (2007, p. 367)* pointed out, “they appear to misunderstand the concept of institutional racism and dismiss the legitimate concerns of the Black community. We have yet to find recent articles that charge psychiatrists or psychiatry with racism.”
Problematizing psychiatry as a discipline
The challenge in accurately diagnosing and providing adequate care to ethnic minorities was considered by some authors as evidence of deeply rooted ideological problems in psychiatry. In other words, not only institutional practices but also fundamental aspects of psychiatry as a scientific discipline should be considered problematic and questioned, so as to address larger issues of discrimination, power, and postcolonial dynamics in western psychiatry. As stated in the following excerpts: Until we begin to address racism within psychiatry, its knowledge base, its historical and cultural roots and its practices and procedures, we are unlikely to achieve significant progress in improving services for minority ethnic groups. (Sashidharan, 2001, p. 244)* The construction of semiotic equivalence of knowledge and cultural systems that are widely diverse is another demonstration of the moulding of otherness into terms and perceptions understandable to the European mind and is as such the sine qua non of the European colonial experience. […] We must be consistently aware that society legitimises psychiatry diagnosis in the same ways that it does racism. Uncritical acceptance of these concepts can be used and reflected in the relegation of otherness and difference to illness. (Hickling & Hutchinson, 2000, p. 94)*
Psychiatry as a scientific discipline that sees and treats all patients equally
While acknowledging social and cultural factors, some scholars accorded greater relevance in psychiatric practice to clinical judgment; the universality of suffering rather than distinct forms it may take among various groups; and a commitment to sound science. As pointed out by Singh (2007)*, Although it is important to be aware of and be sensitive to cultural issues, we must not treat our patients as members of groups rather than as individuals. This is what racists do […]. By focusing inappropriately on culture and ethnicity at the expense of sound clinical judgement, we risk offering poorer rather than better care to patients from minority ethnic groups […]. Our shared humanity and the commonality of human suffering, pain and loss should allow us to understand the influences of culture without demanding that patients from minority ethnic groups be treated in a fundamentally different way. (p. 364)
Criticism of nosology in cross-cultural contexts was considered misleading and diagnostic categorizations were conceptualized as the best possible approximations to natural kinds in psychiatry, which could therefore be operationalized as universal structures as opposed to social constructions (Branton, 1999)*.
It was also contended that issues of pathways to care and related concerns about institutional racism should be detached from matters of causality: In the same way that improving customer services for insurance claimants following an accident is irrelevant to reducing the rate at which such accidents occur, so reforming mental health services (important as this no doubt is) will have no impact on population rates of disorder. (Morgan & Hutchinson, 2010a, p. 876)* An important consequence of conflating issues of service use and population rates of disorder is that there has been no single policy initiative directed at reducing the high rates of psychosis in these populations, in the UK or elsewhere. A crucial public and social health problem has been obscured and ignored. (p. 706)
Publications devaluing institutional practices in psychiatry as a possible explanation for higher rates of psychosis among minoritized populations might have had the unintended effect of adding to discourses undermining the focus on structural racism and the impetus to implement structural reforms in psychiatric institutions in the UK (Bhui et al., 2012). This could be because, as pointed out by Nazroo (2015, p. 1066)*, “Addressing contemporary racism is difficult to pursue, particularly in the current UK climate where questions of racial inequality have disappeared from the policy agenda. Redressing the legacies of historic racism is even more challenging”.
Institutional racism has also been de-emphasized as an explanation for more challenging pathways to care experienced by migrants and ethnic minorities: Serious mental illnesses such as schizophrenia are more prevalent in migrant and ethnic minority groups, therefore so are the consequences of treating these disorders, including detention. (Singh, 2019, p. 276)*
In sum, these perspectives imply that future interventions should focus on evidence arising from epidemiological studies, and science will slowly unravel the mechanisms underlying the reported higher risk of psychosis in ethnic minorities and migrant populations.
The social locus of high rates
As stated by Fernando (1999, p. 374)*, “We may then see that treatment must be directed at society rather than the individual”.
Despite the mentioned differences, as per the analyzed documents and their temporal sequence, the idea that society should also be held responsible for the reported higher rates of psychosis among minoritized populations gathered strength over the years, particularly in the UK (see Table 1). This interest was accompanied by a more general tendency to look into social determinants of health (Marmot & Wilkinson, 2005) and mental health (Allen et al., 2014), which was represented in public reports, such as the one by the WHO Commission on Social Determinants of Health (2008) which stated that measures should be taken to tackle inequality in the distribution of resources and to improve the daily living conditions of all individuals.
With respect to social determinants of psychosis, different authors have privileged different environmental aspects (risk or protective factors), aligned with their research focus. These have been mostly at the individual level of exposure. For example, while Morgan & Hutchinson's (2010a)* opinion statements and research focused on the concept of social disadvantage (parental separation, low educational attainment, unemployment, housing instability, social isolation and their cumulative effects), Selten & Cantor-Graae (2010)* focused on the theory and biological underpinnings of social defeat: We feel that the concept of social adversity is too broad. If poverty, which is also a form of social adversity, were a risk factor for psychotic disorders, one would expect to find very high rates in developing countries […]. Consequently, we feel that the concept of social defeat, defined as the chronic experience of an inferior position or social exclusion, may fit the data better. (p. 732) Victimised individuals and ethnic minority populations at risk of discrimination and exclusion have higher rates of service use for syndromes that in DSM are conceptualised as psychotic disorder […]. These populations also display higher rates of (subclinical) psychotic experiences […]. Stress-induced alterations in how a person attributes meaning to internal and external stimuli may represent the first step in explaining how population ethnic minority–majority interactions affect mental health. (p. 258)
Finally, studies showing that ethnic density, or living in neighbourhoods where one's own ethnic group comprises a relatively substantial share of the population, could partially buffer the effects of discrimination and social disadvantage (Baker et al., 2021) were seen as important breakthroughs. They helped recognize both the role played by supportive communities and the deleterious effects of discriminatory and exclusionary experiences when minoritized populations comprised a small part of the population (Patel & Goodman, 2007)*.
Even in the most recent articles, racism was still an important part of the story, but it was mainly approached through its interpersonal and intergroup dimensions and its individual-level consequences. Institutional racism continued to be mentioned, but mostly at a larger societal level (and not particularly with respect to psychiatric institutions): If institutional racism is relevant, it is that which affects every institution in society, structuring access to decent housing and heating, to an adequate education, to employment and effective social services. The problem is not “in” migrant populations, it is not “in” psychiatry. The problem is “in” society. (Morgan & Hutchinson, 2010a, p. 707)* It is worth interrogating the role of psychiatric institutions and consequent practice within our society and how this sits alongside and interacts with other regulatory and surveillance institutions […] When we ask “where is the harm?” we should consider the implications of psychiatric diagnosis and (often aggressive) treatment for the life-course. (Nazroo, 2015, p. 1067)*
This trend implies that scholars came to accept the high rates findings as fact, so it was time to move on to uncovering its mechanisms and causes. How would social factors affect people in such a way that they would end up developing psychosis? Where, in society, should we be looking? As another UK scholar pointed out: We need to move beyond studies which consistently and robustly demonstrate a disproportionate burden of psychotic disorders is shouldered by a few migrants and ethnic minority groups, to novel population-based studies which seek to identify the determinants and mechanisms through which this risk is shaped. (Dykxhoorn & Kirkbride, 2019, p. 146)*
The same authors have suggested that this goal should be achieved by embracing interdisciplinary research: We now need to develop novel, epidemiologically informed interdisciplinary longitudinal studies to identify the risk and protective factors which underpin this risk. These studies should include qualitative components and input from a variety of stakeholders, including public and patient involvement. (Dykxhoorn & Kirkbride, 2019, p. 149)
As for ways to address the social determinants of psychosis, suggestions ranged from interventions targeting populations at risk to larger public health promotion and prevention interventions that tackle various societal risk/protective factors for psychosis. A harder question was whether the responsibility for these larger promotion and prevention interventions fell to public health, psychiatric institutions or governments. As per Selten and Cantor-Graae (2010, p. 876)*: “Since the causes of the epidemic are mainly of a social nature, prevention is primarily a job for politicians, not for psychiatrists. Psychiatrists could develop useful prevention strategies for those immigrants who are at an extremely high risk”. However, as pointed by Morgan and Hutchinson (2010b)*: Of course, achieving significant policy change that may ameliorate the impact of social disadvantage, particularly in high-risk groups, is extremely difficult. But we do not agree […] that this is primarily a job for politicians. Psychiatry has a role – perhaps even a moral responsibility – in advocating for, and contributing where possible to, the implementation of change. (p. 876)
All in all, however, it was noticeable that discourses on interventions to address the higher rates for psychosis among ethnic and migrant minorities were still infrequent in the more recent literature in psychiatry or public mental health. Ambivalence about the best course of action and associated actors may have stemmed from evolving explanations for the higher psychosis rates among minoritized communities and the varying levels of precedence accorded to these. However, some authors did continue to call for action suggesting joint efforts towards prevention and better services for these communities: Either there is an epidemic of mental illness among certain Black groups or there are seriously worrying practices that are leading to disproportionate levels of admission. Wherever the answer lies on the spectrum between the two extremes it is essential that we find out as a matter of urgency. (Patel & Heginbotham, 2007, p. 367)* One way forward would be simply to accept that there may be differences in opinion. It may be possible to build a consensus around the assertion that social factors lead to an increased rate of presentation of people of African and Caribbean origin to mental health services and those who come to services have symptoms of mental health problems that require treatment. Prevention strategies often improve more than one problem. (McKenzie, 2010, p. 735)*
Aiming for interdisciplinarity
Interdisciplinarity was one of the most used terms across the most recent papers (i.e., over the last decade). Nevertheless, although many disciplines were considered essential to understand complex processes such as the social causation of psychosis, most concrete examples referred to epidemiological and neuroscience research. At the same time, the broader field of psychiatry witnessed exponential growth, interest and investment in neuroscience and cognitive sciences (Insel et al., 2010) and, as a corollary, their associated foci on objectivism and reductionism (Kirmayer & Crafa, 2014).
These disciplines were progressively seen as the most essential components of research in epidemiology and the social sciences, as a way to align different levels of knowledge, from the social world to the molecular underpinnings of neuronal functioning: There has been a recent upsurge of evidence implicating social experiences and environments in the etiology of psychosis […]. Perhaps most importantly, several plausible biological and psychological mechanisms have been identified […]. Perhaps the most significant recent advance is the realization that genes and environment frequently interact to shape adult outcomes, including psychosis. (Morgan & Hutchinson, 2010a, p. 707)*
Nonetheless, it did not take long for some scholars to caution that an excessive focus on biology was leaving little space for the social, thus significantly compromising the aim of interdisciplinarity: “The prevailing attitude in the North American psychiatric literature continues to be that psychotic disorders arise principally from biological factors; social causes of psychosis remain neglected […]. The lack of North American psychiatric literature on this topic is startling” (Jarvis, 2007b, p. 275)*. Jarvis (2007b) * has also suggested that this “pervasive neglect of social factors in the aetiology of psychosis” could be explained by historical and cultural factors that “encourage scientific inquiry in some domains while limiting work in other areas” (Jarvis, 2007b, p. 275). Perhaps, as mentioned by Selten & Cantor-Graae (2010)*, one explanation for this could be that: Psychiatrists remember the dogma from their textbooks that the rates of schizophrenia do not vary between sites, sexes, ethnic or cultural groups and that the heritability of the disorder is about 80–85%. Consequently, so they believe, there is hardly any room for an environmental effect. (p. 731)
Discussion
The three discursive themes that we identified in the analyzed opinion texts spanning the last 30 years were: institutional racism in psychiatry; psychiatry as a scientific discipline that sees and treats all patients equally; and the social locus of high rates of psychosis. These themes express attempts to make sense of, integrate or choose from among different (and many times divergent) discourses to explain the epidemiological findings around the reported higher psychosis risk (rates of psychotic disorders) among minoritized populations and, at a broader level, to explain psychosis. They also incorporate the struggle that exists within psychiatry to reconcile different explanations, and they show that—typically—explanations that are aligned with the biomedical model tend to dominate and exclude others, even when there is a commitment to interdisciplinarity (Jarvis, 2007a). Although it is possible (and even desirable) for people endorsing different discourses in psychiatry to communicate and work together (Campaner, 2014; Kendler et al., 2011; Murphy, 2006, 2010), including by focusing on pragmatic goals and on what is relevant for practice and policy, professional rivalry and internal imbalances of power have been pointed out as major obstacles for communication between those who offer different explanations and causal theories (Cooper, 2007). Our results highlight that, on the one hand, primacy is placed on the medical model and associated theories that focus on universal entities and essences, detached from their social and cultural trappings. On the other hand, there is the belief that psychiatry and its products (such as diagnosis) are socially constructed and influenced by cultural attitudes and power hierarchies. Therefore, the foundations of psychiatric theory and practice deserve careful critique and questioning.
We argue that several events which were concomitant with the analyzed discourses played a crucial role in shaping and shifting academic talking points. For instance, in the 1990s, the public events raising concern over racism in British institutions prompted an important discussion between scholars, which motivated the development of race equity polices for mental health. Nevertheless, these discussions also fuelled a strong countermovement, as uncovering racism and its effects seemed to elicit deep anxieties and uncertainties, provoking strong reactions. The failure to commit to a reconciliatory perspective may have hindered the implementation of race equity policies and associated intervention programs in the UK (Bhui et al., 2012), as evinced by the scarcity of concrete interventions that target the social determinants of psychosis (either in clinical work or though policy development) in the current literature. Furthermore, in many settings, the emphasis on interventions tackling institutional racism in psychiatry has faded over time or shifted towards a discourse on cultural competence that—despite its enormous value—risks being elusive (especially when unaccompanied by pragmatic guidance) and too often lacks explicit references to racial stratification and institutional racism (Nazroo et al., 2020).
The fact that the discussion of the interplay among issues of race, ethnicity, migration and psychosis nearly disappeared from the mainstream North American literature for several decades is also a manifestation of how historical and socio-political contexts shape professional and academic discourses. In fact, these issues were intensely debated in the USA during the 1960s, 1970s and 1980s (Adebimpe, 1981; De Hoyos & De hoyos, 1965; Neighbors et al., 1989; Simon et al., 1973) when misdiagnosis took precedence, favouring an interpretation of findings that highlighted the weight of racial stereotypes in diagnostic procedures and the ways in which established powers (and psychiatry in particular) perniciously used science to validate social stratification based on race (Jarvis, 2008; Metzl, 2010). The adoption of misdiagnosis over other explanations remains prevalent in North American academic psychiatry (Gara et al., 2019; Hairston et al., 2019; Hampton, 2007; Olbert et al., 2018; Schwartz et al., 2019). Even though this was an important discourse switch in the 1970s after a long legacy of racial oppression and marginalization closely connected with psychiatric practices (Jarvis & Kirmayer, 2021), it may also have had the unintended effect of detracting from discourses on the social determinants of mental health and on how these affect some populations more than others (Gee & Ford, 2011). Meanwhile, the interest in biological psychiatry discourses grew and has been dominating professional conversations and scientific priorities in North America (Compton & Guze, 1995). That kind of focus, in turn, might have had the effect of situating the problem in individuals, disregarding the importance of structural racism in shaping risk for mental disorders and thus reinforcing the otherness and inferiority labels attached to minority populations, especially those with mental illnesses. However, a change of discourses seems to be emerging, notably in North America, at a time when movements such as Black Lives Matter have prompted an increase in references to racism in literature (Krieger et al., 2021). Indeed, new research is being produced looking at how structural racism and its relationship with intersecting aspects of social disadvantage may relate to psychosis development, pathways to care and illness outcomes (Anglin et al., 2021; Jones et al., 2019, 2021; Rosen et al., 2017). At the same time, public acknowledgements of the pervasiveness of racism within academia have also been made (Ben-Cheikh et al., 2021; Canady, 2021).
Importantly, discursive constructions that focus on institutional racism have been more dominant in the USA, while in the UK (and other European countries), there has been greater emphasis on social determinants and migration experiences. This variation should be understood considering the differential historical context of these two nations, a settler society and a colonizer society, and the ways in which otherness is constructed and played out in such contexts. This is reflected, for instance, in the ways that official statistical agencies categorize ethnic groups—along racial categories in the USA and categories based on self-ascribed ethnicity in the UK (as per the country of origin of an individual or their parents/grandparents) (Jarvis, 2008).
The results of this study also show how deeply power dynamics determine which discourses are given voice (Foucault, 1972). For instance, it is worth noting that, over the last 30 years, most editorials, opinion pieces or commentaries on the rates of psychosis in ethnic minorities were written by UK-based (and to a lesser extent USA-based) scholars, most of them psychiatrists and university professors, holding positions of power in renowned institutions and working in the fields of clinical, biological and epidemiological psychiatry and (to a much lesser extent) social sciences (see Table 1). Furthermore, the academic discourses explored in this article seemed to be predominately disconnected from other forms of knowledge. Apart from a few exceptions (Fernando, 1998; Sashidharan, 2001), the opinions of individuals with psychosis belonging to ethnic minorities were not the focus of the discussion but were relegated to the background, or most commonly, completely absent. The fact that lived experience has rarely been sought in this literature has been highlighted by some authors as a major limitation for progress in the field of psychosis (Jones & Shattell, 2016). In fact, publications addressing the lived experience of psychosis in minoritized populations (Ferrari et al., 2015; Jones et al., 2021; Lawrence et al., 2021a,2021b; McCabe & Priebe, 2004; Whitley et al, 2016), and/or assessing their opinions on the topics covered by this paper (Schofield et al., 2019), are scarce.
Several study limitations should be noted. The chosen timeframe as well as document type may have resulted in a restricted collection of materials considered in our analysis. As a critical discourse analysis, we have attempted to situate our findings within a broader understanding of social relations, power structures, and discursive context. As such, in our results, we refer to articles and analyses that were not included in the formal analysis and chosen timeframe. In doing so, we recognize that other contextual features could shift the ways that our discursive themes intersect or could emphasize different aspects of these. Likewise, the choice to restrict the searches to papers published in English excluded a group of discourses from outside the Anglosphere that pertain to different schools of thought, such as those from the Francophone world (Radjack et al., 2012). We chose to analyze editorials, letters, opinion articles and commentaries given their explicit focus on providing an elaborate opinion on a given topic. Nonetheless, a limitation of our study is that it did not include original papers, whose discussions and to a lesser extent abstracts, also contain interpretations and speculations about findings. Furthermore, by browsing documents within mainstream journals and databases, the analyzed data corpus was a priori restricted to discourses that make it into these platforms, which, by a process of epistemic injustice, are typically the ones produced by scholars originating from Euro-American (and mostly Anglophone) countries (Bhakuni & Abimbola, 2021). Moreover, this methodology may have also led us to miss the voices/discourses of individuals with lived experience (or of survivor-researchers). Additionally, we decided to target papers on discourses around the epidemiological findings regarding immigrants and ethnic minorities (in general) and their putative higher risk for psychosis. Had we specified our research terms to, for instance, “refugees”, we may have found a different set of discourses, as the experiences of refugees may differ considerably from those of other migrant or ethnic minority groups.
The discourses portrayed in this study should not be understood in a simplistic manner. The issues approached here are complex and so are peoples’ opinions about them, which translate into multi-layered, sometimes contradictory and often changing views and explanations. While there was an effort to frame most of the excerpts within particular socio-political and scientific environments, an extensive contextual account would undoubtedly provide a more comprehensive, situated and embodied portrait of the various lines of discourse. Nevertheless, we believe that we have described and analyzed in considerable depth the kind of discourses that are accessible to individuals interested in the topics of race, ethnicity, migration and psychosis, and in particular, the findings of higher rates of psychosis among immigrants and ethnic minorities. In so doing, we attempted to highlight important aspects of these discourses, namely their action-prone, active and influential properties, aligned with different perspectives and philosophical standings that have played out across geographies.
A final limitation of this study relates to how its authors work in the fields of social and transcultural psychiatry and early intervention for psychosis without lived experience perspectives. This may have influenced the interpretation of the results towards a particular worldview, one that considers the social and cultural embeddedness of experience, meaning and knowledge systems, while valuing evidence-based practices and epidemiology studies that put forward concrete systemic health inequities. Nonetheless, we believe that the steps taken to enhance the study's rigor (such as the clarification of the authors’ positionality and the consultation with specialists with distinct academic backgrounds) helped attenuate this limitation.
Conclusion
By analyzing scholars’ discourses gathered from psychiatric literature on issues of migration, race, ethnicity and psychosis, this article found evolving perspectives on how sociocultural dynamics are integrated into explanatory models of psychosis. Our work highlights the relevance of historical, social, cultural and political factors in shaping academic knowledge, and the role that hierarchies of power play in influencing the discourses of psychiatric research and practice. The paradigms, subjects, objects and methods of research and the interpretation and use of its results are defined by the beliefs, philosophical commitments and socio-political positions of a few actors, mostly from Anglosphere academia. Despite discourse about the higher rates of psychosis among immigrants and ethnic minorities shifting towards social determinants, the focus remains at the individual level, with limited attention to subjectivity, diversity and social context. The evolution and interplay of, and the varying levels of importance accorded to, explanations for the higher rates of psychosis may have acted as distractions and thus hindered meaningful progress towards concrete solutions for tackling institutional racism and addressing social determinants in prevention and intervention.
Going forward, research in the field of migration, race and psychosis should prioritize the perspectives, wisdom and subjective experiences of persons with psychosis from migrant and ethnic minority groups and view them as unique knowledge producers. This could entail everything from qualitative inquiries to including them in all phases of research development. Finally, what is warranted is a commitment to interdisciplinarity and a broader, intersectional approach to social determinants of mental health that go beyond controlling for individual level variables to take into account local, institutional and larger societal processes. From such an approach, along with a critical posture in the field that engages with the social, historical and political contexts of prevailing discourses, new and creative possibilities could arise, not only to explain and understand psychosis more comprehensively but also to provide solutions that improve mental health at the individual and societal level.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
Xavier is the recipient of a FCT (Fundação para a Ciência e Tecnologia) doctoral fellowship (SFRH/BD/143544/2019). Iyer was supported by the Canada Research Chairs (Tier 1) and the FRQS (Fonds de Recherche du Québec - Santé) Chercheurs-Boursiers programs.
Notes
![]()
