Abstract
Fall-related injuries are a major public health issue for older adults, contributing to mortality, morbidity, decreased functional ability, loss of independence, and increased healthcare costs. Autistic older adults may be at greater risk for falls due to motor coordination difficulties and antipsychotic medication use. This cohort study used multivariable logistic regression to compare the odds of falling and negative binomial regression to compare the rate of fall-related injuries. Data from Medicare Standard Analytical Files (2013–2021) for autistic and non-autistic older adults aged 65+ were analyzed. The sample included 13,732 autistic and 25,497 matched non-autistic older adults. Our dependent variables were (1) falls, (2) unique fall-related injuries, and (3) fall-related hospitalizations. Overall, 47.4% of autistic older adults had a fall compared to 31.5% of non-autistic older adults. Autistic older adults also had more fall-related injuries and hospitalizations. Accounting for duration of observation, autistic older adults had significantly higher odds of any fall (odds ratio = 1.99; 95% confidence interval = 1.89–2.08), rate of fall-related injuries (incidence rate ratio = 1.93; 95% confidence interval = 1.86–2.01), and rate of fall-related hospitalizations (incidence rate ratio = 1.43; 95% confidence interval = 1.35–1.51) than non-autistic older adults. These findings highlight the need for targeted fall prevention strategies for autistic older adults to reduce morbidity and mortality.
Lay Abstract
Falls are a big problem for older adults, often causing injuries and making it hard for them to live independently. Autistic older adults might be at higher risk of falling because of movement difficulties. However, no one has studied how often autistic older adults fall. Our study looked at the difference in fall rates, injuries, and hospitalizations between autistic and non-autistic older adults. We used Medicare data from 2013 to 2021 and included people aged 65 and older. We had 13,732 autistic older adults and 25,497 non-autistic older adults in our study. We matched them based on factors like sex, race, and health status to make sure the comparison was fair. We found that almost half (47.4%) of autistic older adults had a fall, compared to only 31.5% of non-autistic older adults. Autistic older adults also had more injuries and hospitalizations from falls. They had about double the likelihood of falling than non-autistic older adults. The rates of injuries and hospitalizations from falls were more about double for autistic older adults compared to non-autistic older adults. These results suggest that we need special programs to help prevent falls and support the health of autistic older adults.
Introduction
Autism was identified in 1943 and added to the Diagnostic and Statistical Manual of Mental Disorders in 1980 (American Psychiatric Association, 1980; Kanner, 1943). Our knowledge about autism across the lifespan is limited by a lack of epidemiological and prospective studies on adulthood and aging (Lai & Baron-Cohen, 2015). By 2050, there will be about 5.8 million autistic adults in the United States (Dietz et al., 2020), of which approximately 1.2 million will be aged 65 and older. Thus, we are now at the historical point where it is possible and pressing to study autism across the lifespan, including aging-related predictors of morbidity and mortality such as falls.
Autistic older adults may be at elevated risk of falls. Autistic people are more likely than people in the general population to have sensory differences and motor coordination difficulties, including proprioception and postural stability (Hariri et al., 2022), as well as difficulties with executive function (Roestorf et al., 2019), which may contribute to higher incidence of falls. Yet, to our knowledge, no research to date has quantified fall prevalence among autistic older adults. Better understanding fall prevalence among autistic older adults is a necessary first step toward developing fall prevention strategies that have the potential to decrease morbidity and mortality, ultimately contributing to better health and well-being.
Approximately 25% of older adults experience a fall (Centers for Disease Control and Prevention, 2024), and falls are the leading cause of injury-related morbidity and mortality among older adults in the United States (Centers for Disease Control and Prevention, 2022; Nicholson et al., 2024). Falls are associated with decreased functional ability, loss of independence, and increased healthcare costs (Nicholson et al., 2024). Multiple demographic and clinical factors have been linked with increased risk of falls among older adults. For example, fall risk varies as a function of rurality (Yang et al., 2023), sex (Sebastiani et al., 2024), race, and ethnicity (Wehner-Hewson et al., 2022). Clinical factors including frailty (Yang et al., 2023), insomnia, and depression (Gimm & Kitsantas, 2016; Yang et al., 2023) are also associated with increased risk of falling. Understanding the prevalence of and risk factors for falls are crucial for developing effective interventions tailored to meet the needs of clinical populations at the highest risk of falling.
As the population of autistic adults in the United States grows, particularly those aged 65 and older, it is crucial to address the potentially elevated risk of falls among autistic older adults as a part of studying autism across the lifespan. We thus sought to address this gap in the literature by conducting a retrospective study using a large, national sample of Medicare beneficiaries. Because Medicare provides health insurance coverage for 99% of US adults aged 65 and older, these data are highly representative of the older adult population (U.S. Census Bureau, 2025). Specifically, our goals were to compare (1) the odds of experiencing a fall and (2) the rate of fall-related injuries and fall-related inpatient hospitalizations between matched samples of autistic and non-autistic older adults. We hypothesized that autistic adults would have higher odds of experiencing a fall and would experience a higher rate of fall-related injuries and fall-related inpatient hospitalizations compared to non-autistic older adults. In addition, we hypothesized the presence of known fall risk factors would moderate the difference in odds of experiencing a fall and rate of fall-related injuries between autistic and non-autistic older adults.
Methods
Data Source
We used 2013 through 2021 Medicare Standard Analytical Files (SAF), which includes information on 100% of Medicare beneficiaries for these years. Access to Medicare SAF for this project was approved as exempt by The Ohio State University’s Institutional Review Board (2018E0630). We used de-identified encounter-level beneficiary claims data for inpatient, outpatient, and skilled nursing facility records. The outpatient records contain medical billing claims from institutional outpatient providers such as hospital outpatient departments, rural health clinics, renal dialysis facilities, outpatient rehabilitation facilities, Federally Qualified Health Centers, and community mental health centers; they do not include professional service claims from non-institutional providers such as physicians, physician assistants, clinical social workers, or nurse practitioners.
Study Population
We included autistic older adults in this study if they (1) were aged 65 years or older, (2) were enrolled in Medicare Parts A and B for at least 12 months consecutively between 2013 and 2021, and (3) had at least one inpatient or outpatient encounter with a diagnostic code for autism spectrum disorder during 1 January 2013 through 31 December 2021. We identified autism diagnoses using International Classification of Diseases (ICD) codes 299.0, 299.00, 299.01, 299.9, 299.90, 299.91 from the 9th edition (ICD-9) or F84.0, F84.1, F84.5, or F84.9 from the 10th edition (ICD-10). We included beneficiaries with at least one inpatient or outpatient claim with an autism diagnostic code as previous research suggests that Medicare-enrolled autistic adults with more than one claim with an autism diagnostic code are demographically similar to those with a single claim (Benevides et al., 2019).
Our population comparison group of non-autistic older adults met the same inclusion criteria as our autistic group, except these beneficiaries did not have an encounter with an autism diagnosis code during the study period. We used variable ratio propensity score matching to match at most two beneficiaries in the non-autistic older adult sample with one autistic older adult; we matched beneficiaries exactly on sex, race, HMO (Health Maintenance Organization, a type of managed care health insurance plan) status, state of residence, and rurality, and with a caliper of 0.2 on index age, index month and year, duration of observation, and Charlson comorbidity index. Duration of observation was defined as the number of days between the first observation where the beneficiary was at least 65 years or older and the last observation (among non-fallers) or date of first fall (among fallers). Characteristics of the autistic and population comparison groups before matching are displayed in Supplemental Table 1.
Measures
Our dependent variables were (1) any fall, (2) number of unique fall-related injuries, and (3) number of fall-related hospitalizations. We defined any fall as at least one inpatient or outpatient encounter with a diagnosis code of E880-E888.9 (for ICD-9) or W00-W19 (for ICD-10) (Roudsari et al., 2005). We quantified the number of unique fall-related injuries using an established algorithm that identifies fall-related injuries treated in inpatient, outpatient, and skilled nursing home settings (Ganz et al., 2024; Hoffman et al., 2022; Min et al., 2019). We defined fall-related injuries as unique to avoid double-counting multiple claims from the same injury event, ensuring each injury episode was represented once in our analyses. We quantified the number of fall-related hospitalizations with a diagnosis code of E880-E888.9 (for ICD-9) or W00-W19 (for ICD-10), lasting at least one night within 72 h of the index fall encounter (Roudsari et al., 2005). Dependent variables were extracted from 2013 to 2021 Medicare SAF for each included beneficiary from the first observed encounter where the beneficiary was 65 years of age or older through the last observed encounter.
Our primary independent variable was autism diagnosis status. Our secondary independent variables were sex, race, age, rurality, history of depression, history of insomnia, and US Veterans Affairs Frailty Index (VA-FI; Cheng et al., 2021). We obtained the beneficiary’s sex, race, and age from the first observation in the Master Beneficiary Summary File. To determine rurality, we used the beneficiary’s county of residence to create categories of rurality based on US Department of Agriculture (USDA) rural–urban continuum codes (US Department of Agriculture Economic Research Service, 2023). We identified depression and insomnia using the Healthcare Cost and Utilization Project’s Clinical Classifications Software Refined (CCSR) for ICD-10 and General Equivalence Mapping to identify the equivalent ICD-9 codes (Healthcare Cost & Utilization Project, 2024); these codes are shown in Supplemental Table 2. Among those experiencing one or more fall, we defined history of depression or insomnia as one inpatient or two outpatient diagnoses prior to the first fall encounter. Among those who did not experience a fall on record during the study period, we defined history of depression or insomnia as one inpatient or two outpatient encounters for these diagnoses at any time during the study period. The VA-FI identifies 31 health deficits based on diagnosis codes in claims data and calculates a weighted score ranging from 0 to 1 that quantifies the degree of frailty. To capture patients’ frailty status at the study’s onset, we used each patient’s first 3 years of data to assess the presence or absence of the health deficits based on the diagnosis codes indicated in the VA-FI. We included first observed year enrolled in Medicare, US region, and Charlson comorbidity index as covariates (Charlson et al., 1987; Quan et al., 2011).
Statistical Analysis
We summarized characteristics of the beneficiaries using descriptive statistics, using median and interquartile range (IQR) for continuous variables and frequencies and percentages for categorical variables. We used multivariable logistic regression to compare the odds of any fall between autistic and non-autistic older adults, and multivariable negative binomial regression with a log link to compare the incidence rate of unique fall-related injuries and fall-related hospitalizations between autistic and non-autistic older adults (Dicker et al., 2006). All models adjusted for sex, race, age, rurality, history of depression, history of insomnia, VA-FI, HMO status, state of residence, index age, index month and year, and Charlson comorbidity index and included a log-offset of person-years to control for differing durations of observation between matched pairs (Agresti, 2002; Shin & Lee, 2023). Finally, we used a series of interaction models, each including an interaction term between autism and one of our secondary independent variables, to evaluate whether the beneficiary’s sex, race, rurality, age, history of insomnia, history of depression, or VA-FI significantly moderated the difference in odds of experiencing a fall and rate of fall-related injuries between autistic and non-autistic older adults. The significance level was 0.05, and the 95% confidence intervals (CIs) for the odds ratios (ORs) and incidence rate ratios (IRRs) were provided. Authors M.B. and M.N. performed analyses using SAS v9.4, and J.M.H. and B.J.W. consulted on analyses and oversaw the interpretation of results. Results of the multivariable models are reported as ORs, IRRs, and 95% CI. ORs represent the odds of experiencing any fall for autistic and non-autistic older adults, and IRRs compare the rate of unique fall-related injuries and fall-related hospitalizations between autistic and non-autistic older adults. All ORs and IRRs are log-offset by person-years.
Results
This study included 13,732 autistic older adults and 25,497 matched non-autistic older adults (Table 1; Figure 1). Most beneficiaries were male (64.0%) or white (89.3%). Beneficiaries were mostly from metro areas with either a population greater than 1 million people (46.6%) or less than 1 million people (35.1%). Approximately 9.9% of autistic older adults had a history of depression and 5.8% had a history of insomnia compared to 5.9% and 6.0%, respectively, of non-autistic older adults.
Demographics, Clinical Characteristics, and Outcomes for Matched Cohort of Autistic and Non-Autistic Medicare Beneficiaries.
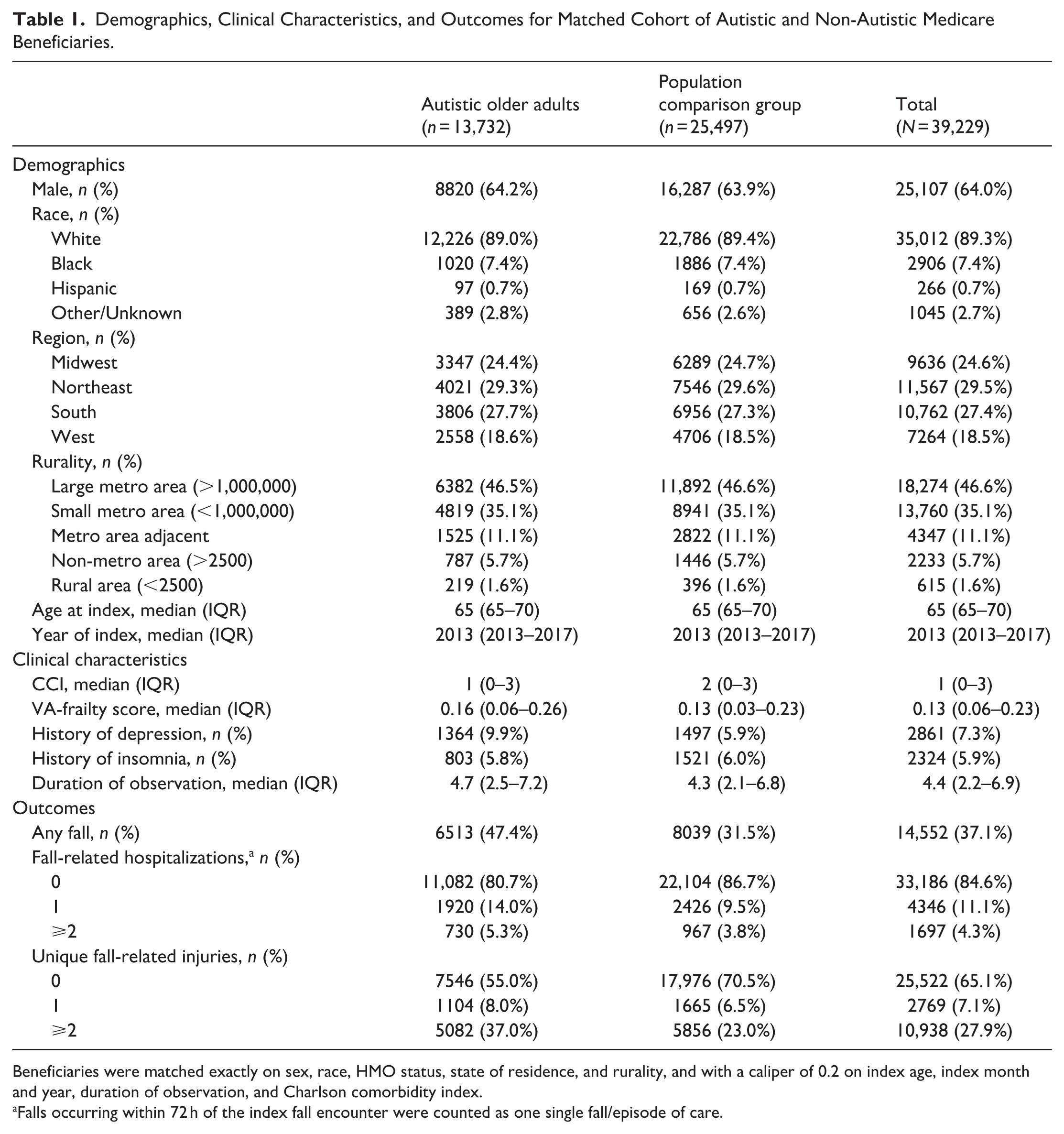
Beneficiaries were matched exactly on sex, race, HMO status, state of residence, and rurality, and with a caliper of 0.2 on index age, index month and year, duration of observation, and Charlson comorbidity index.
Falls occurring within 72 h of the index fall encounter were counted as one single fall/episode of care.
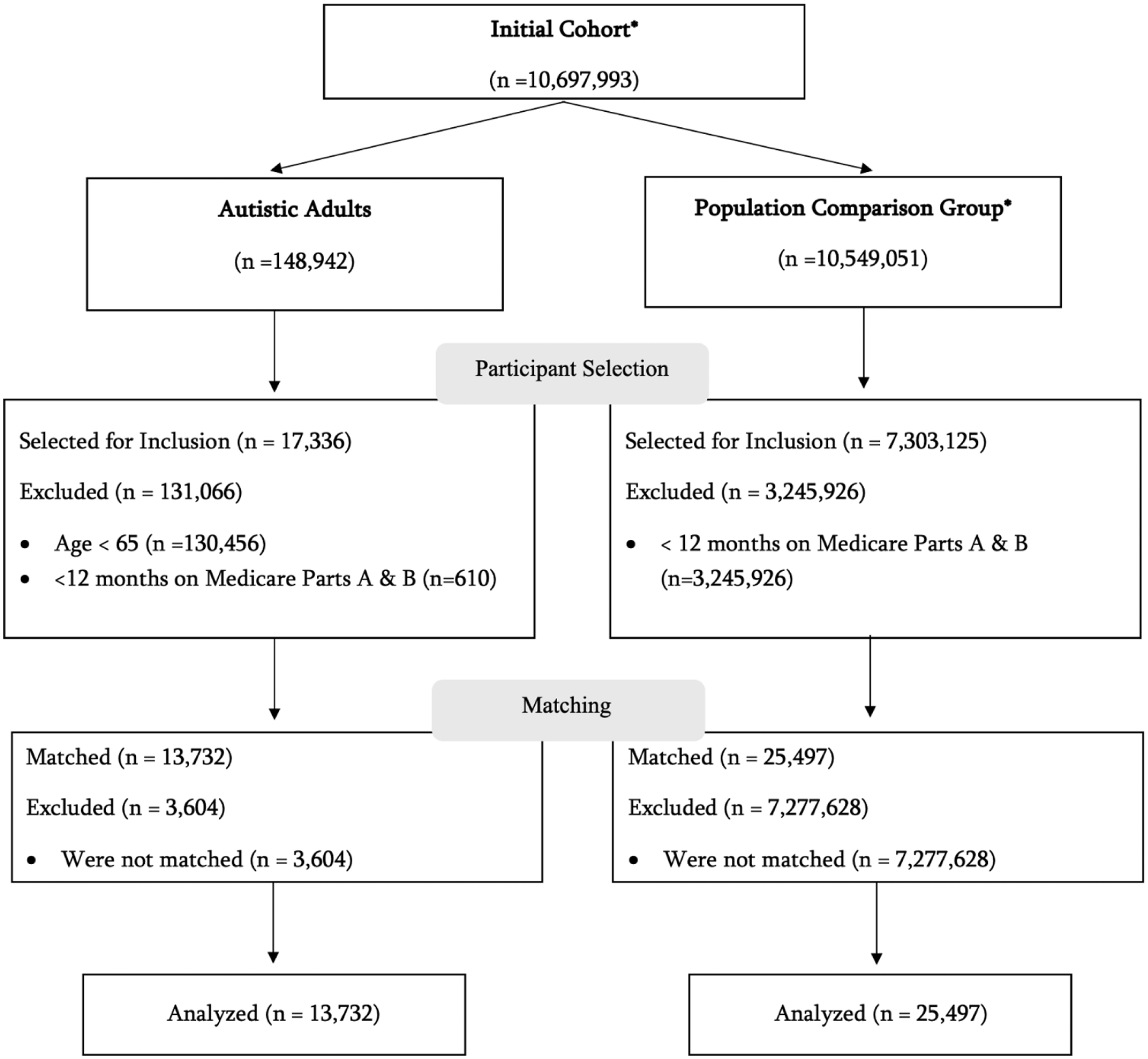
Process Used to Identify Study Population and Analytic Datasets.
Overall, 47.4% (N = 6513) of autistic older adults had a fall compared to 31.5% (N = 8039) of non-autistic older adults. Autistic older adults also had more fall injuries than non-autistic older adults. In total, 8.0% (N = 1104) of autistic older adults had one unique fall injury compared to 6.5% (N = 1665) of non-autistic older adults, and 37.0% (N = 5082) of autistic older adults had two or more fall injuries compared to 23.0% (N = 5856) of non-autistic older adults. Autistic older adults were also more likely than non-autistic older adults to have a fall-related hospitalization, with 14.0% (N = 1920) of autistic older adults having one fall-related hospitalization and 5.3% (N = 730) having two or more fall-related hospitalizations during the study period. In comparison, 9.5% (N = 2426) of non-autistic older adults had one fall-related hospitalization and 3.8% (N = 967) having two or more fall-related hospitalizations during the study period. In our models controlling for duration of observation, autistic older adults had approximately two times greater odds of any fall than non-autistic older adults (OR: 1.99; 95% CI: 1.89, 2.08). In addition, controlling for duration of observation, the incidence rates of unique fall-related injuries (IRR: 1.93; 95% CI: 1.86, 2.01) and fall-related hospitalizations (IRR: 1.43; 95% CI: 1.35, 1.51) for autistic adults were double the corresponding incidence rates among non-autistic older adults. A summary of effect estimates comparing odds of falls, rates of fall-related injuries, and rates of fall-related hospitalizations between autistic adults and non-autistic adults without stratification is displayed in Table 2.
Adjusted and Unadjusted Odds Ratios and Incidence Rate Ratios Comparing Odds of Falls and Fall-Related Hospitalizations, and Rates of Fall-Related Injuries Between Autistic Older Adults and Matched Population Comparison Peers.
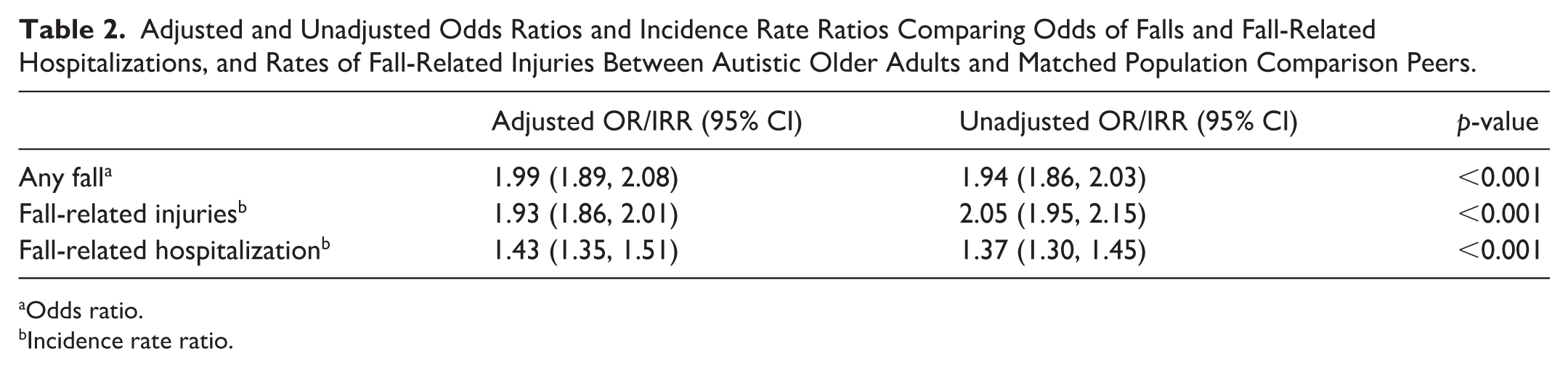

Odds ratio.
Incidence rate ratio.
Results of the multivariable models evaluating the impacts of other known inequities are shown in Table 3. Adjusted fall prevalence estimates derived from these models are provided in Supplemental Table 3. When stratified by sex, the effect of autism diagnostic status on the odds of any fall and incidence rate of fall-related injuries was more pronounced for males than for females. Autistic older adults had higher rates of unique fall-related injuries, and fall-related hospitalizations, but the magnitude of these differences was attenuated in the presence of known fall risk factors such as depression, insomnia, increasing age, and frailty. We did not find significant interactions between autism diagnostic status and race or rurality.
Odds Ratios and Incidence Rate Ratios Comparing Falls, Unique Fall Injuries, and Fall-Related Hospitalizations, Between Autistic Older Adults and Matched Population Comparison Peers Stratified By Sex, Race, Rurality, Depression, Insomnia, Age Group, and Us Veterans Affairs Frailty Index.
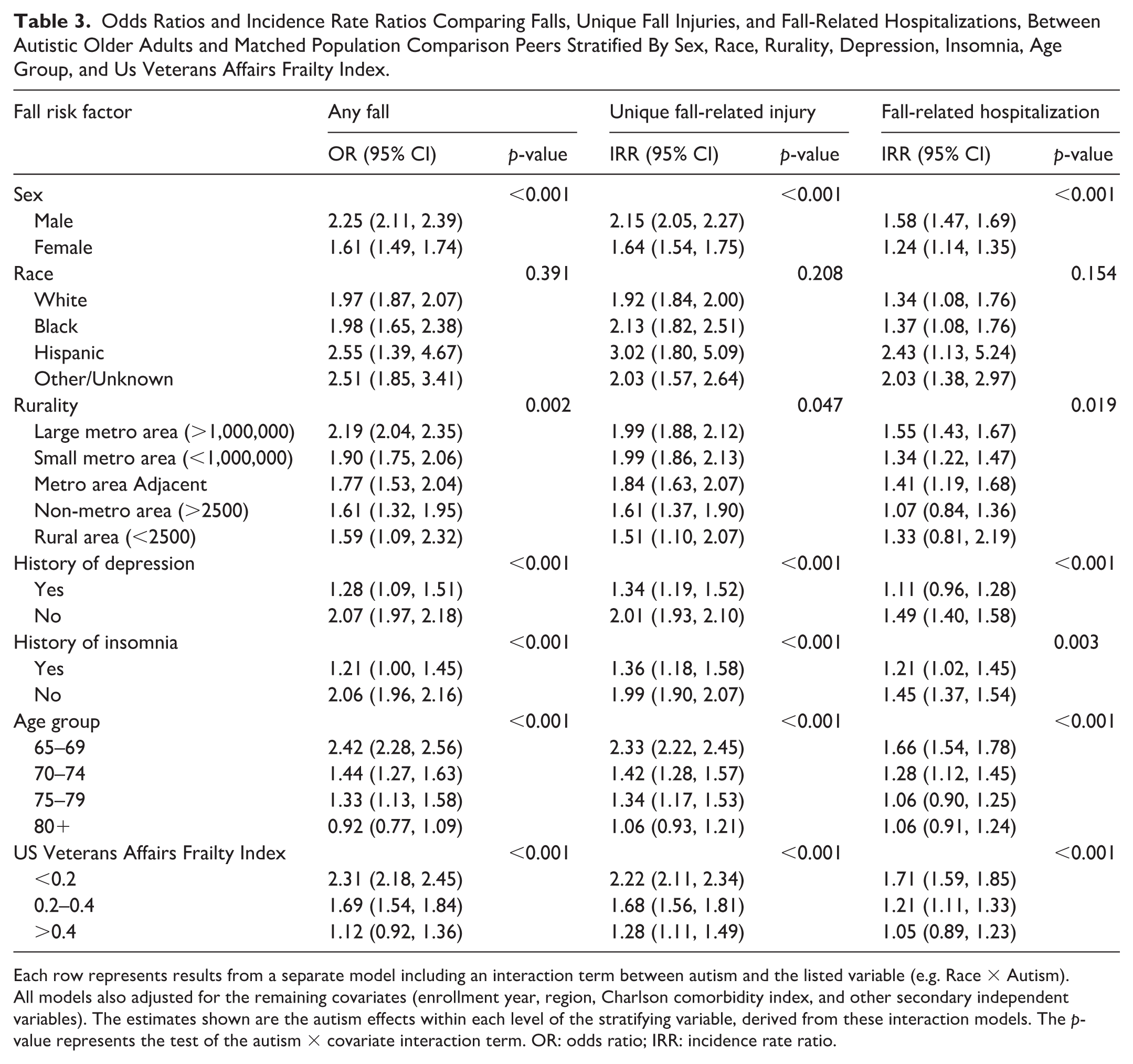
Each row represents results from a separate model including an interaction term between autism and the listed variable (e.g. Race × Autism). All models also adjusted for the remaining covariates (enrollment year, region, Charlson comorbidity index, and other secondary independent variables). The estimates shown are the autism effects within each level of the stratifying variable, derived from these interaction models. The p-value represents the test of the autism × covariate interaction term. OR: odds ratio; IRR: incidence rate ratio.
Discussion
This nested case–control cohort study sought to quantify the odds of falls, rates of unique fall-related injuries, and rates of fall-related hospitalizations among autistic older adult Medicare beneficiaries aged 65+. We found that autistic older adults had significantly higher odds of falling, with nearly half of autistic older adults having at least one fall compared to approximately one-third of adults in our population comparison group. Furthermore, autistic older adults had higher rates of fall-related injuries and hospitalizations compared to non-autistic older adults.
Falls are the most common cause of injury-related morbidity and mortality among adults aged 65+ in the United States (Centers for Disease Control and Prevention, 2022). Our findings suggest that autistic older adults have more than double the odds of falling and rate of unique fall-related injuries and hospitalizations compared to non-autistic older adults. Our results are striking in their magnitude yet unsurprising given that known fall risk factors (e.g. postural instability, proprioceptive difficulties) are prevalent among autistic people. Although this is the first study to characterize fall odds in autistic older adults and more work is needed, results suggest that autistic older adults are at significantly increased odds of falling compared to the general population.
Our stratified analyses (Table 3, Supplemental Table 3) also revealed attenuated magnitude of differences between autistic and non-autistic older adults in the presence of known fall risk factors such as depression, insomnia, increasing age category, and frailty. For example, across age and frailty categories, autistic older adults had an adjusted fall prevalence ranging from about 14.4% to 16.2%, whereas there is considerably more variation in the control group as a function of these risk factors. In other words, in the general population, these known fall risk factors are associated with increased adjusted prevalence of falls, but in autistic older adults, the prevalence of falls is high regardless of the presence or absence of these risk factors. These findings highlight the need for future studies to explore elevated fall risk observed among autistic older adults, with the ultimate goal of informing strategies that promote healthy aging in autistic people.
Fall interventions generally fit into one of three categories, including modifications to living space, exercise interventions, and multifactorial interventions. The US Preventive Services Task Force (USPSTF) recommends that all older adults who are at increased risk of falling participate in exercise interventions, which provide a “moderate net benefit” in preventing falls and resulting fall-related morbidity (Nicholson et al., 2024). Interventions designed for the general population often need to be specifically adapted for autistic people; future research is needed to examine how and to what degree fall risk interventions should be adapted for autistic adults. For example, interventions that enhance postural stability among autistic children (Hariri et al., 2022) or reduce fall risk in the general older adult population (Grossman et al., 2018; Nicholson et al., 2024) could be adapted as fall prevention interventions for autistic older adults. Results of this study suggest the need for universal fall prevention and intervention strategies to help reduce disparities in morbidity and mortality and improve quality of life among autistic older adults.
Limitations and Future Directions
Our study is not without limitations. Findings may not generalize to future populations of autistic older adults due to diagnostic changes over time, and to the unique features of this sample, all of whom were born before autism was added to the Diagnostic and Statistical Manual for Mental Disorders (Gimm & Kitsantas, 2016). Notably, this is a service system-level study that captures all diagnosed autistic Medicare beneficiaries with claims aged 65+. In addition, our autistic sample may exclude people who would qualify for an autism diagnosis but have never been diagnosed. Unlabeled autism cases may mask a larger difference in rates of falls than is reported in this article.
Claims data reflect only diagnoses assigned to patients during healthcare encounters that are directly billed to the payor represented in the data (e.g. Medicare). It is plausible that patients with greater access to care are more likely to both be diagnosed as autistic and have a fall recorded in their claims data. While our propensity score matching approach cannot fully eliminate this bias, matching on variables such as HMO status, state and county of residence, and rurality may help reduce some of the confounding related to healthcare access. In addition, our dataset does not contain data from Medicare Part C or Part D, and we thus cannot examine claims that would have been billed to Medicare Part C or Part D, such as pharmaceutical use. Our data also do not contain professional service claims billed to non-institutional providers, which may lead to us missing some relevant claims. In this study, we did not examine all possible risk factors of falls. For instance, living situation (i.e. group homes or assisted living) may increase the probability of falling or of falls being observed and thus reported in healthcare records (Gimm & Kitsantas, 2016; Grant et al., 2001). Our data do not contain variables detailing living situation and residential settings, so we were unable to delineate risk of falls in these residential care facilities. Future studies will be needed to explore these factors.
Although the fall risk algorithms that we used in this article represent the most rigorous and well-validated algorithms used with claims data, when compared with self-report data, the Ganz et al. (2024) algorithm has moderate sensitivity. However, it has very high specificity, suggesting that a not insignificant number of falls take place without an accompanying medical encounter. As such, our findings are reflective of falls resulting in a medical encounter and may not accurately reflect falls without an encounter. Finally, it is possible that increased fall risk begins in young adulthood or midlife among autistic people; future work that includes younger autistic adults is warranted to estimate the age at which increased fall risk begins among autistic people.
Conclusion
This study found that autistic older adults have significantly elevated odds of falls, rate of unique fall-related injuries, and rate of fall-related hospitalizations. Though preliminary, our findings reveal new directions for future work and underscore the urgent need for targeted fall prevention strategies adapted for autistic older adults. Implementing tailored fall prevention strategies has the potential to reduce morbidity and mortality among autistic older adults.
Supplemental Material
sj-docx-1-aut-10.1177_13623613261433988 – Supplemental material for Falls and Fall-Related Injuries and Hospitalizations in Autistic Older Adults: A Medicare Data Study
Supplemental material, sj-docx-1-aut-10.1177_13623613261433988 for Falls and Fall-Related Injuries and Hospitalizations in Autistic Older Adults: A Medicare Data Study by Lauren Bishop, Madison Blake, Melica Nikahd, J Madison Hyer, Brian W Patterson, Bethany J Wolf and Brittany N Hand in Autism
Footnotes
ORCID iDs
Author contributions
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Research reported in this publication was supported by the National Institute on Aging (NIA) of the National Institutes of Health under award number R01AG082873. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health (NIH).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
