Abstract
To date, no studies have investigated whether disparities in hours of applied behavior analysis (ABA) exist in the Medicaid system. We used multilevel modeling to analyze Medicaid billing claims for 1,028 autistic youth under the age of 21 years to examine the extent to which there were disparities in hours of ABA services for Medicaid-enrolled youth based on race/ethnicity and rurality. Although younger children received more hours of ABA, F(1, 964.63) = 118.28, p < .001, there were no statistically significant differences in hours of ABA based on minoritized race/ethnicity status or sex. On average, youth served in rural areas received significantly less hours of ABA per month than those in non-rural areas, F(1, 122.13) = 7.89, p = .006; youth in rural areas received 10.86 less hours per month than those in non-rural areas. Results suggest that publicly funded service systems like Medicaid may reduce ABA service disparities by race/ethnicity. Policymakers should focus on improving service provision for youth in rural areas.
Lay Abstract
We used Medicaid billing claims from 1,028 autistic youth to see if there were differences in hours of applied behavior analysis (ABA) services per month for youth from different racial/ethnic groups, different service settings (rural or non-rural), different sexes, and different ages. We found that younger autistic youth received more hours of ABA per month compared to older youth, and and youth served in rural areas received about 11 hours less per month compared to youth in non-rural areas. There were no differences among different race/ethnic groups or sexes. Policymakers should focus on improving service availability for autistic youth served in rural areas.
Plain Language Summary
No studies of the Medicaid system have shown whether children of color receive less hours of applied behavior analysis (ABA) than White children or whether children in rural areas receive less services than those in non-rural areas. We used Medicaid billing claims to see if these disparities exist. We found that younger children received more hours of ABA per month, and children from rural areas received an average of 10.86 hr less per month than children in non-rural areas. There were no disparities based on race/ethnicity or sex. Publicly funded service systems like Medicaid may help reduce disparities by race/ethnicity, but policymakers should improve services for children living in rural areas.
Background
Disparities in the age at which children are diagnosed with autism—or whether they are diagnosed at all—are well-documented (Angell et al., 2018; Liptak et al., 2008). Historically, Black and Latine/Hispanic youth, youth from low-income backgrounds, and youth from rural areas are less likely to be identified with autism (Durkin et al., 2010; Mandell et al., 2009) and are diagnosed at a later age than White, middle-/upper-class, and non-rural youth (Barnard-Brak et al., 2021; Mandell et al., 2002; Thomas et al., 2012). Delays in diagnosis ultimately result in delays in service access and utilization, which can result in poorer outcomes over time (Towle et al., 2020).
While the literature on treatment disparities for autistic youth is less robust, a recent systematic review found evidence for disparities in access to acute care and specialized, education and community services for racial and ethnic minority compared to White families (Smith et al., 2020). Black and Latine/Hispanic families also reported lower quality of care. Research has also documented disparities in access and use of allied health services (e.g., occupational therapy), with younger children receiving more services than older children, and youth from minoritized backgrounds and specific geographic regions receiving fewer services than White children (Dallman et al., 2021).
Others have proposed explanations for these treatment disparities, including discrimination, stigma, cost, lack of insurance coverage, poor transportation, geographic barriers, inflexible work schedules, and lower educational attainment and health literacy (Drahota et al., 2020; Pham & Charles, 2023). These factors more commonly affect poorer families, who access services less than those from middle- or upper-class backgrounds (Smith et al., 2020); however, racial and ethnic disparities in treatment access do not fully disappear after controlling for socioeconomic status (Durkin et al., 2017). We need additional research to understand why disparities in service use persist for autistic youth in the same income bracket, particularly among those who are at the highest risk of unmet service needs.
Medicaid is the largest payer of autism-related health care services in the United States (Wang et al., 2013), providing coverage based on low household income, disability, and placement in foster care. Racial disparities in unmet service needs are reduced for autistic youth enrolled in Medicaid’s home and community-based services (HCBS) waiver program (LaClair et al., 2019); we know less about disparities in the Medicaid system outside of this program. One recent study of autism service use among Medicaid-enrolled children documented some racial and ethnic disparities, but findings varied by type of service (Bilaver et al., 2021). Furthermore, there was significant geographic variation, with the disparity in outpatient services for Black youth being driven predominantly by children living in large metropolitan counties.
Applied behavior analysis (ABA) is a common evidence-based intervention for autistic children (ABA; Hyman et al., 2020). ABA is most effective when implemented at a younger age (Smith et al., 2015) and delivered at a high intensity (Virués-Ortega, 2010). Research shows variation in access to ABA providers by county, with higher accessibility in urban and wealthier counties (Yingling et al., 2021). However, no studies have examined whether treatment disparities in ABA are evident based on children’s race/ethnicity or rurality.
In Michigan, Medicaid-enrolled autistic children can receive intensive ABA services covered by the Medicaid Autism Benefit for Behavioral Health Treatment (BHT). Here, we examined whether there were disparities in the BHT program for the number of hours of ABA per month based on race/ethnicity and rurality, controlling for sex and age.
Method
Participatory methods
We developed this research question within the context of a community-academic partnership focused on improving family-centered care within the Michigan Medicaid Autism Benefit. To our knowledge, no autistic people were involved in this analysis.
Medicaid claims data
We obtained de-identified Medicaid claims from April 2017 through March 2018 for 1,028 youth under age 21 with an autism spectrum disorder (ASD) diagnosis modifier (U5) on file from one of 13 regional Prepaid Inpatient Health Plans (PIHP) in Michigan. This PIHP oversees services provided by 12 community mental health (CMH) agencies across 22 counties. Claims data included child date of birth, sex, racial background (White, Black/African American, Asian, American Indian/Alaskan Native, Two or More Races, or Other Single Race), and ethnic background (Hispanic or non-Hispanic), Current Procedural Terminology (CPT) codes, and ABA agency ID. We extracted the total number of units of one-on-one ABA sessions (CPT codes: 0364T, 0365T) for each youth. We categorized agencies as rural based on zip code classifications from the U.S. Department of Health and Human Services.
Participants
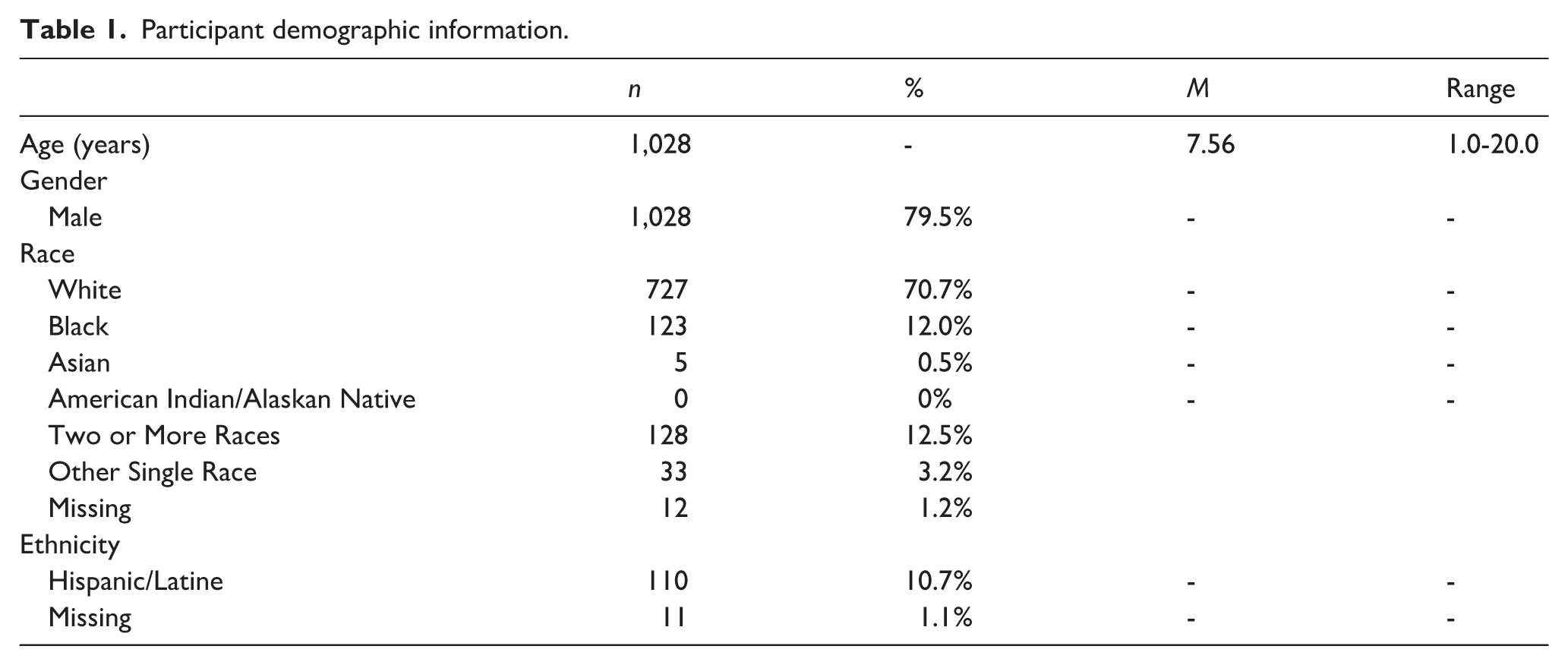
Participants included the 879 youth who had at least one one-on-one ABA session billed to the BHT program. Youth were nested within 69 agencies (42.0% in rural areas). Youth were predominantly White (70.7%), non-Hispanic (88.2%), and male (79.5%), with an average age of 7.56 years (see Table 1).
Participant demographic information.
Data structure
Data were nested within three levels, such that multiple observations across 12 months (Level 1) were nested within each youth (Level 2), and multiple youth were nested within each agency (Level 3). Some youth received services from multiple agencies each month. In those situations, the agency with the most hours of service for that month was used. Preliminary analyses suggested no variability in hours of service across CMH agencies, so they were not included as a level of analysis. Youth who were extreme outliers (e.g., 50+ units of ABA) were noted in ABA agencies within one CMH agency. Our community partners indicated that this agency had difficulties with their electronic medical records system, and claims from that CMH were sometimes submitted in bundles after the service date. As it was impossible to know the true date of each service for these participants, they were removed from the analysis (n = 52 youth).
Racial and ethnic groups in the sample were unevenly distributed; 12.5% of the sample was multiracial without identified specific racial backgrounds, only 0.5% of the sample was Asian, and there were no American Indian/Alaskan Native youth. Given these limitations, a single race/ethnicity variable with four categories was coded: (1) White, non-Hispanic; (2) Black (Hispanic or non-Hispanic); (3) Hispanic (non-Black); or (4) Other Race, non-Hispanic (including multiracial youth, Asian youth, and youth of an unspecified other single race).
Data analytic approach
A series of multilevel models using restricted maximum likelihood was used to predict hours of ABA as a function of either race/ethnicity or agency rurality, controlling for child age and sex. Units of ABA were billed in 30-min increments; analyses were converted to hours for interpretability. Race/ethnicity was treated as a categorical predictor, and age was grand mean centered. Random effects included an intercept variance to account for nonindependence due to agency. Monthly observations were treated as repeated measurements for each youth.
Three models were used. Model 1 predicted hours of ABA as a function of youth race/ethnicity, sex, and age using all agencies. Given the lack of racial/ethnic diversity in the children receiving services from rural agencies (only eight observations of non-White children), we ran a second model (Model 2) that was identical to Model 1 but only included data from non-rural agencies. We hypothesized that youth from racial/ethnic minoritized backgrounds would receive fewer sessions, and younger youth would receive more sessions. Model 3 predicted ABA hours as a function of agency rurality, sex, age, and racial/ethnic minoritized status (effects coded: −1 = White and non-Hispanic, 1 = racial/ethnic minority status). We used a single variable for minoritized status in Model 3 because there were only eight observations of non-White children in rural agencies.
Results
In Model 1, ABA hours were predicted as a function of race/ethnicity group, sex, and age. In terms of random effects, there was significant nonindependence in the data, with significant variation across agencies and a partial intra-class correlation (ICC) = 0.12, Wald Z = 2.83, p = .005. In terms of fixed effects, there was a significant main effect of age, F(1, 964.63) = 118.28, p < .001, but not race/ethnic group, F(3, 924.05) = .69, p = .56, or sex, F(1, 955.37), p = .70. Younger youth received more hours of ABA: each year decrease in age was associated with an increase in 2.14 hr of ABA per month. While hours of ABA did not significantly vary across racial/ethnic groups, estimated marginal means suggest a slight trend in which Hispanic youth received fewer hours per month than the other groups (Table 3 in Supplementary Materials). Model 2 was identical to Model 1 but only included cases in non-rural agencies (n = 35 agencies). Results were consistent with Model 1; that is, there was no evidence of disparities across race/ethnic groups in non-rural agencies, but younger youth received more hours of ABA (Table 4 in Supplementary Materials).
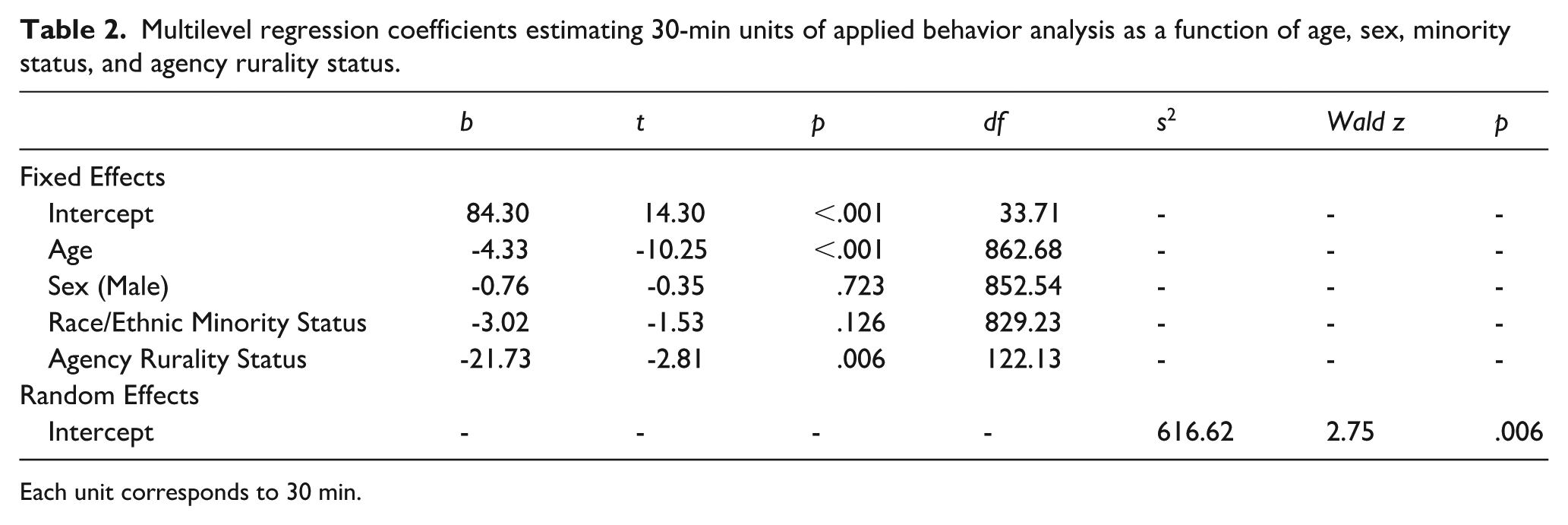
In Model 3, hours of ABA were predicted as a function of age, sex, minority status, and agency rurality. In terms of the random effects, there was significant nonindependence in the data, with significant variation across agencies and a partial intraclass of ICC = 0.13, Wald Z = 2.75, p = .006. There was a significant main effect of age, F(1, 862.68) = 105.12, p < .001 and agency rurality, F(1, 122.13) = 7.89, p = .006, but not for sex, F(1, 852.54) = .13, p = .72 or minoritized status, F(1, 829.23) = 2.34, p = .13 (Table 2). Holding sex, minoritized status, and agency rurality status constant, for every year decrease in age, there was an associated increase in 2.17 hr of ABA per month. Holding sex, minoritized status, and age constant, youth who received services from agencies that were in rural areas received 10.86 hr less of ABA per month compared to those in non-rural areas.
Multilevel regression coefficients estimating 30-min units of applied behavior analysis as a function of age, sex, minority status, and agency rurality status.
Each unit corresponds to 30 min.
Discussion
We examined whether there were disparities in receipt of ABA hours as a function of youth race/ethnicity and rurality, controlling for sex and age. We did not observe sex differences in the number of ABA hours received, but we did observe differences by age, with younger children receiving more hours of ABA than older children. This finding is consistent with recommended ABA practices and has been observed elsewhere (Dallman et al., 2021).
We were surprised to find no racial/ethnic disparities in receipt of ABA hours, although there were some non-significant trends suggesting that Hispanic children received fewer hours than other groups (Model 1). This finding held true when we limited our analyses to non-rural agencies, which were more diverse (Model 2); thus, systematic differences in youth demographics between rural and non-rural agencies did not mask our ability to identify racial/ethnic disparities had they been present.
To our knowledge, only one other study has examined service use disparities for ABA services with Medicaid-enrolled children (Bilaver et al., 2021). They found that racial/ethnic disparities in autism-related service use varied based on the type of service as well as geographic location. For example, although there were racial/ethnic disparities in outpatient services as a whole, disparities were less pronounced for mental health/social skills/behavior modification than for most other outpatient services. While Bilaver and colleagues (2021) collapsed CPT codes for these three service types, our analysis only utilized direct ABA service CPT codes. Thus, it is possible that some of the race/ethnicity disparities may be driven by disparities for other, non-ABA services included in that larger category (e.g., outpatient mental health services).
In addition, in the Bilaver et al. study, disparities for Black (compared to White) autistic children were largely driven by differences in service use among those living in large metro areas (>250,000 people) compared to those in small metro and non-metro areas. Only one of our agencies represented a large metro area; thus, we were not able to examine results at this more nuanced level. In addition, Bilaver and colleagues (2021) also included a larger sample across all 50 states, while we only included one midwestern state. Thus, it is possible that our results would not generalize to the national-level sample.
We found robust evidence of treatment disparities based on rurality; youth served in rural areas received 10.86 hr less of ABA per month compared to those in non-rural areas. Rural areas experience greater geographic barriers, which affect access to both center-based services (e.g., family’s ability to commute to an agency) and home-based services (e.g., provider’s ability to commute to a family's home). Indeed, a recent study found that providers in this system reported difficulty accessing families in rural areas as a significant barrier to the delivery of ABA services (Straiton et al., 2021). These geographic barriers could lead to a higher number of unscheduled or canceled sessions. Furthermore, based on the uneven geographic distribution of autism services, providers in rural areas may need to serve more youth than those in urban and suburban areas (Drahota et al., 2020; Yingling et al., 2022), which limits the number of treatment hours that can be scheduled per child. To improve access to services in rural areas, policymakers and agency leaders should consider targeted recruitment methods and incentive structures for recent graduates to practice in rural locations, provision of flexible supervision models for new graduates, increased use of telehealth service models, and remote consultation services for complex cases (Albright & Williams, 2021; Dew et al., 2013; Mazurek et al., 2017).
Our findings suggest that Medicaid may be a particularly important system for addressing racial and ethnic disparities in ABA services for autistic children. For example, racial disparities in parent-reported service needs for children with special health care needs are reduced when Medicaid coverage is provided (Rose et al., 2010). In addition, increasing Medicaid-funded Home and Community Based Services (HCBS) waivers for autism-related health care costs greatly decreases parent-reported unmet health care needs for families of Black autistic children (LaClair et al., 2019). There are also many other positive benefits of the expansions in Medicaid coverage, such as a positive association with growth in the autism workforce, reducing unmet health needs for individuals with developmental disabilities, and supporting states’ economic development (McBain et al., 2022; McLean et al., 2021).
There are a number of limitations to consider. Our claims data only provided information on the number of hours of ABA that children actually received. We do not know whether the treatment disparities we observed for rural children were due to a higher rate of unscheduled/canceled sessions or fewer hours in the children’s service plan. It is unlikely that differences in hours of ABA are due to level of need but rather systemic inequities in rural areas (e.g., less service providers, travel difficulties). Furthermore, it is unclear whether disparities were due to family preference or provider/agency decisions.
In addition, while we did not observe racial/ethnic disparities in ABA hours, there may have been disparities in children identified and/or enrolled in the Autism Benefit. For example, Autism and Developmental Disabilities Monitoring (ADDM) surveillance data suggest Latine/Hispanic children were less likely to be identified than White children during the time frame of our data collection (Maenner et al., 2021), although this trend has reversed in the most recent surveillance year (Maenner et al., 2023). Moreover, we did not have information on the children’s degree of need. Black children who have an autism diagnosis are more likely to have an intellectual disability than White children (Shenouda et al., 2023), suggesting that Black children without intellectual disability may be less likely to be identified (Maenner et al., 2023). Since a greater intensity of ABA services is likely to be recommended for autistic children with higher support needs, it is possible that the lack of racial/ethnic disparities in our sample may have been due to a higher level of need among minoritized children. Thus, future studies should control for level of need.
Finally, while the sample was quite large, it only represented one region in a single midwestern state and focused exclusively on Medicaid-enrolled children. In addition, due to the low number of participants from some racial/ethnic backgrounds and their uneven distribution across agencies, we were limited in our analyses of racial/ethnic disparities. This limits the conclusions that we can draw regarding disparities for Asian, Native American, and multiracial children. Future research with a larger sample is needed to better understand disparities in ABA services based on race/ethnicity and rurality.
Supplemental Material
sj-docx-1-aut-10.1177_13623613251392495 – Supplemental material for Short report: Disparities in hours of applied behavior analysis services for Medicaid-enrolled autistic youth
Supplemental material, sj-docx-1-aut-10.1177_13623613251392495 for Short report: Disparities in hours of applied behavior analysis services for Medicaid-enrolled autistic youth by Diondra Straiton-Webster and Brooke Ingersoll in Autism
Footnotes
Acknowledgements
The authors would like to acknowledge Dr. Debbie Kashy, a brilliant scientist and mentor who provided statistical consultation for this project. Although Dr. Kashy has passed away, she continues to make a profound impact on our lives and on our science. The authors would also like to acknowledge our community partners at Mid-State Health Network in Lansing, Michigan. In particular, the authors would like to specifically acknowledge Barb Groom for her dedication and support.
Ethical considerations
This study received ethical approval from the Michigan State University IRB. This is an IRB-approved retrospective study; all patient information was de-identified, and patient consent was not required. Patient data will not be shared with third parties.
Author Contributions
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Patient data will not be shared with third parties, given the sensitive and confidential nature of the data (i.e., health care billing claims).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
