Abstract
Weight stigma undermines women’s body image and health through systemic, interpersonal, and intrapersonal pathways, perpetuating maladaptive behaviours and psychological distress. Existing body image resilience models offer limited insights into weight stigma’s challenges. This paper introduces the Promoting Resilience In Women’s Weight Stigma Management (PRISM) model, an approach that novelly integrates psychological resilience, multi-level support, and systemic change to address weight stigma’s impacts on women’s body image. Building on existing models, PRISM operates across three levels: intrapersonal (stigma-resilient self-concept and stigma-specific coping strategies), interpersonal (inclusive support systems), and systemic (policy reform, media representation, and institutional accountability). These components work synergistically to promote robust holistic wellness. By addressing weight bias internalisation and intersecting marginalisation, PRISM positions resilience as a multi-level commitment rather than an individual burden. This approach guides stakeholders in promoting positive body image in women while advocating for systemic change against weight stigma.
Introduction
Poor body image among women represents a significant public health concern and is associated with adverse physical, psychological, and behavioural health outcomes (Rodgers et al., 2023). Weight stigma – a pervasive form of bias and discrimination – is significantly associated with body image distress, particularly for women. Although weight stigma can affect all genders (Pearl and Wadden, 2018), women tend to report more frequent and impactful experiences across the lifespan. For example, girls experience more weight-based teasing than boys in childhood (Puhl et al., 2017; Szwimer et al., 2020) and women continue to experience higher rates of weight stigma than men in adulthood (Sattler et al., 2018; Spahlholz et al., 2016; Timkova et al., 2025; Wijayatunga et al., 2023).
Compared to men, women report higher levels of weight bias internalisation (WBI) (Hughes et al., 2024; Macho et al., 2023; Pearl et al., 2021), greater body dissatisfaction (Macho et al., 2023; Quittkat et al., 2019; Voges et al., 2019), and lower body appreciation (He et al., 2020; Murray et al., 2023). Objectification Theory helps explain these gendered dynamics, highlighting that women are more frequently subjected to appearance-based scrutiny and are more likely to internalise an observer’s perspective of their bodies (Fredrickson and Roberts, 1997). Empirical studies confirm that women experience higher levels of self-objectification, particularly body surveillance, which undermines body image and contributes to gendered disparities in appearance-related outcomes (Murray et al., 2023).
Body image provides a conceptually appropriate focus for weight stigma research as it directly captures the appearance-related dimension of this form of discrimination (Cash et al., 2004; Tylka et al., 2014). Although weight stigma has wide-ranging psychological effects, body image provides a focused lens for examining how appearance-based stigma impacts women’s self-perceptions, making it particularly suited to prevention-oriented frameworks (Zhao et al., 2025).
Weight stigma is embedded across women’s everyday lives, manifesting in policy, healthcare, media, education, and family contexts – where it is routinely enacted and justified through discourses of health and personal responsibility (Brown et al., 2022; Tomiyama, 2014). This stigma is woven into the social regulation of women’s bodies, where appearance is subject to scrutiny and judgment.
Beyond its harmful effects on body image and psychological outcomes, weight stigma presents a broader societal challenge: how can women develop and sustain positive body image in a society where weight bias is so deeply entrenched? Addressing this issue requires more than promoting individual resilience; it demands a shift in the systems and narratives that perpetuate weight stigma – including discriminatory institutional practices, weight-stigmatising social environments, and the pervasive ‘thin-is-good, fat-is-bad’ cultural narrative that equates body size with moral worth (Nutter et al., 2024a). Recognising this complexity, this paper aims to: (1) examine how weight stigma shapes body image across systemic, interpersonal, and intrapersonal pathways, focusing on women as a starting point given the pervasive and disproportionate impact of both weight stigma and body image concerns in this population, while recognising the model’s broader applicability; (2) outline the evidence base for four integrated components that work synergistically to promote resilience in the newly developed Promoting Resilience In Women’s Weight Stigma Management (PRISM) model, a theoretical contribution integrating individual resilience with systemic change to address weight stigma’s multi-level impacts; and (3) provide future research directions to inform the development of body image resilience interventions in weight-stigmatising environments.
Weight stigma operates across three interconnected domains: systemically (across healthcare, workplaces, and media), interpersonally (within family and social relationships), and intrapersonally (through the internalisation of negative societal beliefs) (Nutter et al., 2024a). Although weight stigma affects women of all sizes, those in larger bodies experience more severe and frequent impacts (Spahlholz et al., 2016). Despite its pervasiveness, weight stigma remains largely unchallenged, while overwhelming evidence demonstrates that body weight is shaped by complex biological, environmental, and social determinants beyond individual control (Westbury et al., 2023).
The complexity of weight regulation is particularly evident in women’s health where physiological transitions naturally shape body composition across life stages. For instance, hormonal changes during menstrual cycles lead to natural weight fluctuations; pregnancy requires weight gain to support fetal development; and menopausal transitions alter metabolism and body fat redistribution (Fenton, 2021; Guo et al., 2023; Kanellakis et al., 2023). Yet society routinely disregards these essential biological processes, treating the natural consequences of female physiology as grounds for reduced social value and credibility.
Beyond natural life stage transitions, women’s weight and body composition are influenced by various health conditions and medical interventions. Polycystic ovary syndrome (PCOS), affecting up to 13% of women worldwide, is a prime example where hormonal mechanisms drive weight changes (World Health Organisation, 2025). Common medical interventions also impact women’s bodies. For example, oral contraceptive pills – used by millions of women worldwide – frequently list weight gain as a side effect (Le Guen et al., 2021). Despite the medical basis of these changes, women in these contexts encounter stigma related to managing health conditions or treatments that intersect with the stigma associated with weight-based bias and discrimination. This creates a challenging environment for developing positive body image.
The impact of weight stigma is further complicated for women, through its intersection with other forms of marginalisation. Women from diverse racial and ethnic backgrounds, those experiencing socioeconomic disadvantage, and sexual minority women, face layered prejudices that can compound the effects of weight stigma (Ciciurkaite and Perry, 2018; Deol et al., 2024; Panza et al., 2024). This multiplicity of discrimination not only undermines the development of positive body image but also limits access to supportive resources, underscoring the need for more nuanced and comprehensive approaches.
Towards a new model for body image resilience
Weight stigma operates through a self-reinforcing cycle. External discrimination may trigger psychological distress and internalised shame, which may result in maladaptive coping behaviours, such as comfort eating, and biological stress responses (e.g. cortisol dysregulation) that can contribute to weight gain, potentially increasing vulnerability to further weight stigma (Tomiyama, 2014). This cyclical process is particularly concerning given the widespread framing that weight stigma is ‘beneficial’ or ‘motivational’ despite substantial evidence of its harmful effects on women’s body image and health-promoting behaviours (Pearl and Puhl, 2018; Puhl et al., 2013).
Amid these challenges, body image resilience emerges as a critical underexplored aspiration. Research shows that resilience, the ability to adapt and thrive despite adversity (Joyce et al., 2018), can support positive body image and healthier coping strategies (Snapp et al., 2012). However, existing theoretical models do not fully capture the complexities of weight stigma. Choate’s (2005) foundational body image resilience model provides a valuable starting point. It identifies five protective factors: family-of-origin support, gender role satisfaction, positive physical self-concept, effective coping strategies, and holistic wellness. However, Choate’s model was not explicitly designed to address weight stigma and primarily focuses on intrapersonal and limited interpersonal factors, leaving a critical gap between individual resilience strategies and the broader systemic changes needed to effectively combat weight stigma’s pervasive impacts.
Building on Choate’s work and drawing inspiration from the Health Stigma and Discrimination Framework (HSDF) (Stangl et al., 2019), which conceptualises stigma through a socioecological lens where health-related stigma intersects with other forms of marginalisation, we propose the Promoting Resilience In Women’s Weight Stigma Management (PRISM) model that addresses, for the first time, how weight stigma shapes body image across intrapersonal, interpersonal, and systemic levels. The PRISM model recognises that building body image resilience against weight stigma cannot be achieved through individual efforts alone – it requires inclusive support systems and institutional reforms that challenge weight-centric paradigms. Resilience does not develop in isolation; it is shaped by the environments in which women experience stigma. While intrapersonal and interpersonal strategies provide women with the tools and support necessary to resist stigma, these efforts are limited if broader systems continue to reinforce discriminatory norms (Pearl, 2018). PRISM incorporates systemic strategies to dismantle these structural barriers, ensuring that resilience is cultivated collectively rather than resting solely on the efforts of individual women. Importantly, this model addresses how weight stigma intersects with other forms of marginalisation, including race, socioeconomic status, sexual orientation, gender identity, and health conditions that create unique barriers for many women.
The PRISM model advances our understanding of how to promote body image resilience in weight-stigmatising environments. By integrating theoretical insights with current evidence, PRISM provides guidance for research, practice, and policy. Importantly, we do not position individual resilience as a replacement for comprehensive social reform, but as an essential element in creating environments where resilience can flourish naturally. Through this integrated approach, PRISM contributes to the broader mission of eliminating weight stigma in society while providing immediate support for women navigating its impacts.
Before detailing the specific components of the PRISM model, it is important to establish its theoretical foundation. This includes understanding how weight stigma impacts body image through multiple pathways, conceptualising resilience within the context of body image, and identifying the limitations of existing models. Together, these elements provide the necessary context for understanding why a multi-level model is needed and how each component of PRISM contributes to mitigating weight stigma’s effects on women’s body image and psychological health. The following sections examine these foundational elements before presenting the four integrated components of the PRISM model and their synergistic role in promoting body image resilience in weight-stigmatising contexts.
Weight stigma and body image: Integrated systems of impact
Body image is a multifaceted construct that shapes how women perceive, evaluate, and behave in relation to their physical appearance, and includes two key components: evaluative attitudes (satisfaction or dissatisfaction with appearance) and investment (the importance placed on appearance within one’s self-concept) (Cash et al., 2004).
Weight stigma impacts body image through two primary pathways: direct experiences of discrimination and the internalisation of weight bias – where individuals adopt negative societal attitudes about body size and apply them to themselves (Pearl and Puhl, 2018). While not synonymous with negative body image, weight bias internalisation is a key mechanism through which weight stigma contributes to body image concerns (Bidstrup et al., 2022). This internalisation process can trigger a cascade of maladaptive coping behaviours, including disordered eating, healthcare avoidance, reduced physical activity, extreme dieting practices aimed at rapid weight loss, and compulsive self-monitoring behaviours (Pearl and Puhl, 2018). Indeed, evidence from two comprehensive systematic reviews highlights the significant association between weight bias internalisation, body image concerns, and body dissatisfaction, creating recursive loops between stigma and body image (Bidstrup et al., 2022; Pearl and Puhl, 2018).
These processes are embedded in everyday contexts. Interpersonal relationships, particularly with family and peers, may contribute to weight bias internalisation through negative weight-based comments, reinforcing appearance-focused expectations (Lawrence et al., 2022; Pearl et al., 2018). Consequently, women may develop negative beliefs about their bodies, perceiving themselves as above ‘acceptable’ weight due to prevailing norms favouring thinness (Tylka et al., 2014). In healthcare settings, providers may engage in weight-focused consultations or use stigmatising language, while women may delay or avoid seeking care due to fear of being judged (Puhl et al., 2021a). In workplace environments, weight-based discrimination may limit hiring and promotion opportunities, undermining career progression and job satisfaction (Pearl et al., 2018). Media representations further entrench thin ideals and stigmatise larger bodies, heightening appearance dissatisfaction and fuelling harmful social comparison (Merino et al., 2024).
The institutional landscape further compounds these challenges through a global dearth of protective policies against weight discrimination (Willer, 2024). In the absence of enforceable safeguards, discriminatory practices persist largely unchallenged, reinforcing the misguided notion that women bear full personal responsibility for their weight, and supports the unjustified belief in the legitimacy of weight stigma (Puhl, 2022). As a result, larger-bodied women face widespread social stigmatisation in Western societies, with emerging evidence of similar trends in non-Western countries (Gramaglia et al., 2018). In the absence of legal protections against weight-based discrimination, the message becomes clear: positive body image is portrayed as a privilege reserved for those in smaller bodies, while larger women are expected to maintain a perpetual state of dissatisfaction with their appearance. Therefore, in this context of high weight stigma and low protection, women must navigate complex body image challenges with minimal institutional support. These systemic barriers to positive body image are particularly pronounced for women experiencing multiple forms of marginalisation, as weight stigma intersects with and compounds other forms of systemic oppression (Ciciurkaite and Perry, 2018; Deol et al., 2024; Panza et al., 2024).
Given these pervasive barriers, the relationship between weight stigma and body image resilience poses significant challenges to women’s wellbeing. Understanding how these factors interact to influence health outcomes is essential for developing strategies that strengthen psychological resilience and counter stigmatising narratives. Such understanding is particularly crucial in supporting women in cultivating positive body image, even within systems that often undermine it.
Resilience in the context of body image
The concept of resilience, commonly defined as the ability to adapt effectively in the face of adversity (Joyce et al., 2018) serves as a valuable framework for understanding how some women maintain psychological health despite threats to positive body image. Research identifies several protective factors that underpin body image resilience, including body appreciation (maintaining positive attitudes toward one’s body), body functionality appreciation (valuing what one’s body can do rather than how it looks), and self-compassion (treating oneself with kindness and understanding) (Neff, 2003; Tylka and Wood-Barcalow, 2015a). These factors are associated with greater self-esteem, fewer maladaptive eating behaviours, and improved body satisfaction (Linardon et al., 2022, 2023; McLean and LaGuardia, 2016). Moreover, women who demonstrate higher levels of body image resilience are less influenced by sociocultural appearance pressures (Snapp et al., 2012), underscoring the role these factors play in countering unrealistic and harmful beauty ideals.
However, while these protective factors promote resilience against general appearance-related concerns, weight stigma presents distinct obstacles that exceed the scope of traditional resilience models. Conventional models typically emphasise individual coping strategies, while overlooking broader systemic forces. The socially-sanctioned nature of weight stigma, which operates through institutional discrimination, interpersonal bias, and internalised negative beliefs, suggests that standard resilience approaches may be insufficient. Building resilience against such pervasive prejudice requires an integrated strategy that supports both individual psychological resilience and systemic change. This recognition calls for a specialised model to guide personal resilience development alongside essential environmental reforms.
Adapting Choate’s body image resilience model: Addressing
weight stigma’s unique challenges
Choate’s (2005) theoretical model offers valuable insights for understanding body image resilience through its five components (family-of-origin support, gender role satisfaction, positive physical self-concept, effective coping strategies, and holistic wellness). However, weight stigma presents unique challenges that require a more expansive approach. Three key gaps emerge in applying Choate’s model to weight stigma: limited attention to systemic influences, the need for targeted strategies addressing weight bias internalisation (WBI), and the lack of intersectional considerations.
First, while Choate acknowledges support systems, her model does not capture the bidirectional relationship between individual resilience and systemic change. Women need protection and resources at multiple societal levels to build resilience against weight-based discrimination, with systems serving as both protective factors and catalysts for social reform.
Second, WBI presents distinct psychological challenges that Choate’s general coping strategies do not fully address. An expanded model should address the unique cognitive and emotional impacts of internalised weight stigma, including strategies for maintaining self-worth in the face of persistent societal devaluation and identifying how weight bias becomes embedded in self-perception.
Third, Choate’s original conceptualisation of gender role satisfaction was limited to cisgender women’s experiences and did not account for other social identities including race, socioeconomic status, and sexual orientation. Contemporary research demonstrates that weight stigma intersects with these identities, complicating resilience processes for marginalised groups (Ciciurkaite and Perry, 2018; Deol et al., 2024; Panza et al., 2024).
These limitations highlight the need for an expanded model that can better address body image resilience in the context of weight stigma. The Health Stigma and Discrimination Framework (HSDF) (Stangl et al., 2019) offers valuable constructs that can enhance and modernise Choate’s work. The HSDF emphasises the socioecological nature of stigma, highlighting how stigma drivers and facilitators operate across multiple levels of society. The framework explicitly recognises how different forms of stigma intersect and compound, acknowledging that individuals may simultaneously experience discrimination based on multiple aspects of their identity. By combining Choate’s emphasis on intra- and interpersonal support with the HSDF’s systemic and intersectional perspective, a more robust body image resilience model emerges – one that acknowledges resilience requires not only individual coping skills and supportive family environments but also institutional protections, inclusive social policies, and community-level efforts that actively dismantle stigmatising norms.
The promoting resilience in women’s weight stigma management (PRISM) model:
Enhancing body image resilience
Building upon Choate’s foundational work on body image resilience while addressing its limitations in the context of weight stigma, we present the Promoting Resilience In Women’s Weight Stigma Management (PRISM) model. The PRISM model integrates Choate’s intrapersonal and interpersonal factors with HSDF’s systemic and intersectional perspectives, addressing both the psychological challenges of weight bias internalisation and the structural barriers that perpetuate weight stigma. Operating across individual, interpersonal, and systemic levels, the model aims to reduce weight stigma and create environments where positive body image develops naturally.
As illustrated in Figure 1, PRISM encompasses interconnected components that span multiple levels of influence. At the intrapersonal level, stigma-resilient self-concept and stigma-specific coping strategies form the psychological foundation, equipping women with cognitive and emotional tools to counter weight bias internalisation. These foundational elements are strengthened by inclusive support systems, which function across interpersonal and systemic levels, serving as critical bridges between individual resilience and broader social change. These core components are further reinforced by systemic strategies, which actively dismantle structural barriers to promote inclusive environments. Through the integration of these components, PRISM promotes holistic wellness – a state that represents the synthesis of psychological resilience, social support, and systemic protection against both external weight stigma and its internalisation. Each of these constructs is explored below.
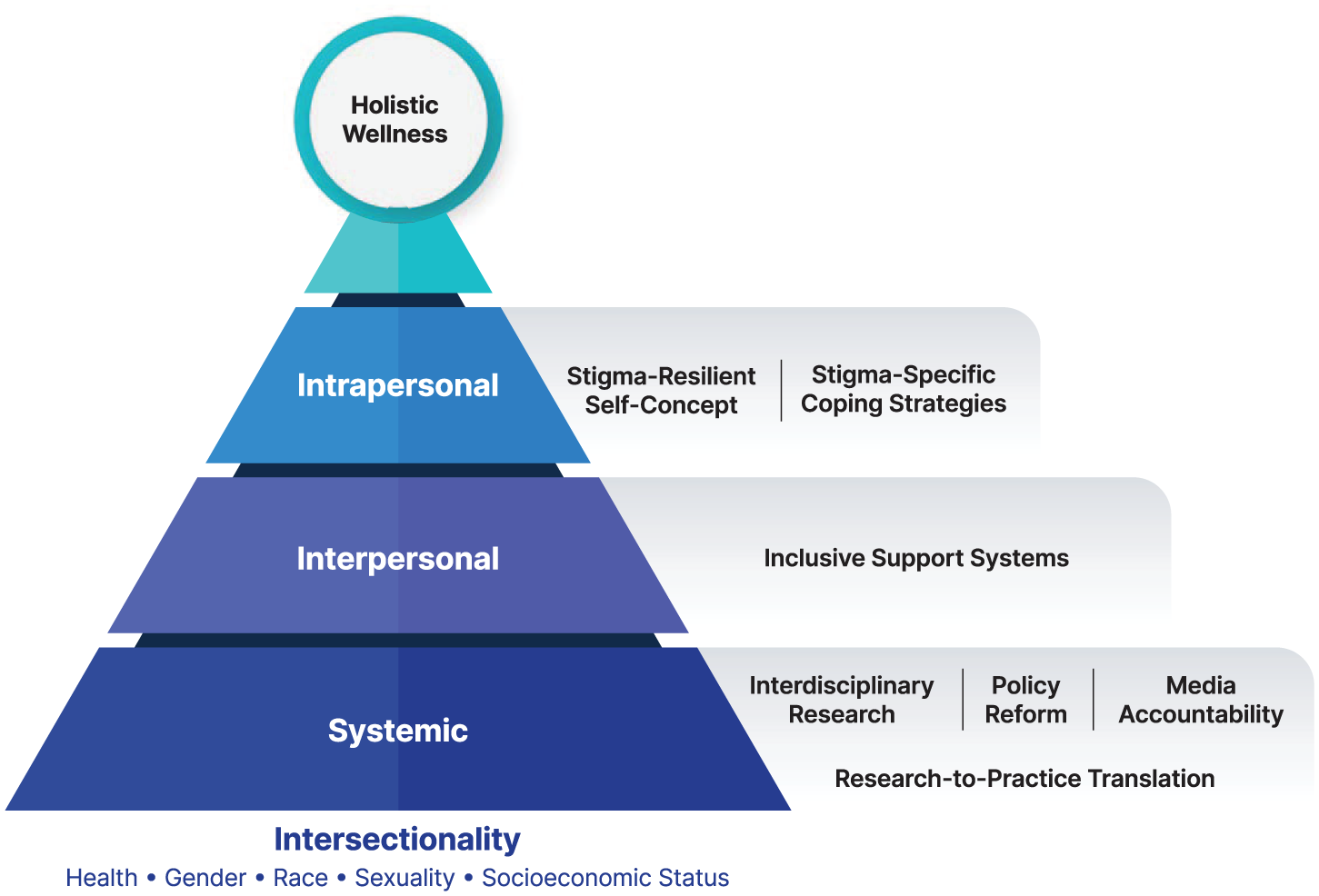
The promoting resilience in women’s weight stigma management (PRISM) model.
The model consists of four integrated components that work synergistically to promote resilience:
Intrapersonal components
At its core, PRISM focuses on equipping women with psychological tools to counter weight stigma’s harmful effects. This component comprises two interrelated elements:
Stigma-resilient self-concept
Drawing on Choate’s (2005) ‘positive physical self-concept’ which focuses on physical fitness, health, and athleticism, this component expands beyond physical capabilities to address the psychological challenges of weight stigma. A stigma-resilient self-concept incorporates elements that help resist weight bias internalisation and affirm self-worth beyond conventional appearance standards.
This resilient self-concept is supported by two interconnected elements, each with growing empirical support for reducing weight bias internalisation (WBI) in women. First, interventions targeting body appreciation show particular promise. Body appreciation involves holding positive views toward one’s body, acknowledging its inherent worth and functionality regardless of appearance (Linardon et al., 2023). For example, Expand Your Horizon (a body gratitude journaling intervention) reported significantly greater reductions in WBI compared to controls, alongside improvements in body functionality appreciation and reduced healthcare anxiety (Davies et al., 2022). Similarly, Webb et al.’s (2022) yoga-based intervention incorporating body gratitude practices led to reductions in internal body shame and increases in body appreciation, functional satisfaction, and body awareness, highlighting the effectiveness of embodied practices that centre capability over aesthetics.
Second, self-compassion interventions demonstrate strong potential in reducing weight bias internalisation. Self-compassion involves treating oneself with kindness during difficult experiences, recognising shared humanity in suffering, and maintaining mindful awareness of thoughts without over-identification (Neff, 2003). These components directly counter the self-criticism, shame, and rumination that characterise body image distress, encouraging a decoupling of self-worth from appearance and cultivating a more flexible and non-judgmental sense of self (Neff, 2003). Supporting this, Haley et al. (2025) found that brief self-compassion training significantly reduced internalised weight bias and body shame compared to controls. Similarly, Nightingale and Cassin (2023) demonstrated that self-compassion letter writing exercises improved adaptive body image and increased self-compassion among women with elevated WBI levels. Such approaches represent viable, low-cost strategies for strengthening psychological resilience in weight-stigmatising contexts.
While preliminary evidence supports body appreciation and self-compassion interventions, developing critical awareness of weight stigma as a societal rather than personal issue may further support stigma-resilient self-concepts. Internalised weight stigma thrives when individuals accept dominant cultural messages about body size as personal truths (Nutter et al., 2024b), suggesting that understanding the broader systemic nature of weight bias could help women maintain resilience against stigmatising messages.
Stigma-specific coping strategies
Expanding on the foundation of a resilient self-concept, this component provides targeted cognitive and emotional strategies to help women navigate and respond to weight stigma. While Choate’s work primarily focused on resisting sociocultural pressures through media literacy, this adaptation extends her approach by addressing both internalised weight bias and external discrimination. Evidence suggests that incorporating cognitive-behavioural techniques can strengthen psychological resilience (Joyce et al., 2018), helping women identify triggering situations and evaluate automatic responses (Pearl et al., 2023). Key techniques include cognitive restructuring, which involves identifying and challenging weight-biased thoughts and developing counter-narratives (Pearl et al., 2023). Studies suggest that cognitive restructuring approaches can reduce WBI and improve body image and psychological resilience (D’Adamo et al., 2024; Pearl and Puhl, 2018). Recent research by Dibb et al. (2025) supports self-affirmation and confronting stigma as cognitive strategies to maintain a positive body image. Assertiveness training may complement these approaches by providing practical tools for navigating stigmatising situations (Yanos et al., 2015). Although no studies have directly examined assertiveness training in weight stigma contexts, evidence from other fields indicates that building communication skills helps individuals navigate social challenges with greater confidence (Yosep et al., 2024).
Inclusive support systems: Bridging multiple levels
A defining feature of PRISM is its emphasis on inclusive support systems that connect individual resilience with systemic change. Extending Choate’s (2005) concept of family-of-origin support, PRISM broadens this to encompass supportive relationships and environments across intrapersonal, interpersonal, and institutional levels. These interconnected support systems reinforce individual resilience by enhancing cognitive and emotional resources while actively challenging structural barriers that sustain weight stigma.
At the interpersonal level, relationships with family, friends, and community networks provide practical and emotional support through multiple protective mechanisms: reducing isolation, providing emotional validation, and strengthening capacity to manage stigmatising encounters effectively (Chronister et al., 2013). Peer-led support groups, for example, provide a sense of belonging and offer safe spaces for authentic dialogue (Burwell and Bias, 2024). Research demonstrates that strong social support may mitigate the negative psychological effects of stigma internalisation across different contexts (Burwell and Bias, 2024; Li et al., 2020). Specifically, Timkova et al. (2025) found that higher social support was associated with lower anxiety, depression, and loneliness among individuals reporting weight stigma, with effects being particularly strong for those experiencing WBI.
At the institutional level, support systems can play a crucial role in developing weight-inclusive environments. Recent research demonstrates potential for institutional approaches to address weight-stigmatising practices through systemic interventions and policy changes (Hill et al., 2024). This multi-level integration distinguishes PRISM’s approach from traditional support models by connecting individual empowerment with systemic change, ensuring that personal resilience both informs and is strengthened by systemic change efforts.
Systemic strategies: Creating environments that support body image resilience
Building upon these multi-level support systems, PRISM incorporates five key systemic strategies that actively challenge structural inequities while reinforcing individual and interpersonal resilience. These strategies complement and extend the HSDF (Stangl et al., 2019) by explicitly addressing the role of media alongside research, policy, implementation, and intersectionality (Stangl et al., 2019). The selection of these domains is based on their potential to comprehensively address weight stigma’s pervasive nature across critical domains that shape individual experiences and societal norms, recognising that sustainable change requires broader social acceptance and engagement.
First, collaborative research across disciplines such as psychology, social sciences, and public health may help establish the empirical foundation for evidence-based resilience interventions. Multidisciplinary initiatives, such as the international consensus statement on weight stigma (Rubino et al., 2020) and the World Obesity Federation’s global working group (Nutter et al., 2024a), demonstrate how diverse expertise can be mobilised to address complex stigma-related challenges across multiple levels. Ideally, such cross-sector collaboration would inform targeted interventions that enhance body appreciation and self-compassion practices, strengthen support networks, and identify institutional practices that protect against weight stigma. This research-practice integration highlights the importance of interventions effectively addressing both individual psychological resilience and systemic barriers.
Second, legal and institutional frameworks shape the environments in which weight stigma operates, yet weight-based discrimination remains largely unprotected by law (Puhl et al., 2021b; Sabharwal et al., 2020). This leaves many women vulnerable to weight bias in workplaces, healthcare settings, and public spaces. The PRISM model advocates for comprehensive anti-discrimination policies providing legal protections against weight-based bias, mirroring existing safeguards for race, gender, and disability.
Beyond legislation, workplace and healthcare policies play pivotal roles in either perpetuating or mitigating weight stigma. Implementing weight-inclusive practices, anti-bias training for employers, and healthcare guidelines that prioritise patient-centred care above weight-centric interventions can transform institutions from places contributing to weight stigma to sources of support (Puhl et al., 2021a, 2021b; McGregor et al., 2022). Mobilising public engagement is equally necessary for influencing policymakers and driving legislative change. Such legislation promotes inclusion, respect, and equal protection under the law (Puhl et al., 2021b), thereby strengthening both individual coping strategies and collective support systems.
Third, the media serve as powerful vehicles for both reinforcing and challenging weight stigma. Weight-stigmatising representations dominate mainstream media, contributing to weight bias internalisation and negative body image (Jiotsa et al., 2021; Moufawad et al., 2024). The PRISM model recognises that systemic change requires a fundamental shift in how women’s bodies are represented and discussed in public discourse. This includes challenging weight-stigmatising portrayals by holding media accountable for biased representations that conflate weight with health, morality, or competence, and promoting body diversity through advocacy efforts (Clark et al., 2021; Merino et al., 2024; Puhl, 2022). Research demonstrates that weight-inclusive media narratives (such as Health at Every Size approach) are perceived as significantly less stigmatising than weight-normative public health campaigns focused on personal responsibility and weight-loss (McGregor et al., 2022).
Social media platforms offer powerful avenues for strengthening support systems through counter-narratives and body-positive communities that validate diverse body experiences (Clark et al., 2021). Such strategies could be implemented through industry self-regulation standards and platform algorithm modifications that de-prioritise weight-stigmatising content, with some platforms like Pinterest already implementing policies that prohibit weight-based discrimination and body shaming (Clark et al., 2021; Pinterest, 2025). These initiatives must be complemented by media literacy programs in educational institutions, particularly during adolescence, when body image concerns are highly formative (Paxton et al., 2022; Tylka et al., 2019). By disrupting media-driven narratives, these strategies strengthen both intrapersonal resilience (by reducing self-stigma) and interpersonal support (by reshaping societal perceptions of body diversity).
Fourth, translating research into practice is essential for creating sustainable change across diverse settings. Effective implementation requires careful attention to delivery methods, intervention design, and evaluation strategies (Fernandez et al., 2019). Current approaches often fail to bridge the gap between research findings and practical strategies that support both individual resilience and systemic transformation. To address this, weight-inclusive training programs for healthcare providers, educators, and employers are essential. These programs should focus on reducing implicit bias and creating support environments that prioritise wellbeing rather than weight. However, while individual-focused approaches are vital for developing coping strategies and positive self-concept, they must be complemented with systemic changes that address the structural drivers of weight stigma. A balanced approach will contribute to translating research findings into meaningful, lasting change.
Intersectional approach: Addressing compounded stigmas
An intersectional perspective is essential when designing interventions that address weight stigma’s diverse impacts on women’s body image. Women who hold multiple marginalised identities, such as experiencing both weight and health stigma, racial discrimination, socioeconomic disadvantage, or biases related to sexual orientation face compounded barriers to resilience. For example, socioeconomically disadvantaged women are more likely to experience mental health harms from weight stigma (Ciciurkaite and Perry, 2018), while sexual minority women report significantly higher levels of weight stigma and internalised bias compared to heterosexual women (Panza et al., 2024). These findings underscore the imperative for an intersectionally informed model that addresses the compounded effects of multiple stigmas on women’s body image resilience.
Holistic wellness
Choate (2005) conceptualised holistic wellness as the culmination of protective factors that promote balance across multiple dimensions, including spiritual, emotional, intellectual, and physical wellbeing. Drawing on the Wheel of Wellness (Myers et al., 2000), she highlights that achieving this balance enables women to develop self-worth beyond weight and shape, making them more resilient to appearance pressures. However, while Choate’s (2005) model recognises multiple protective factors, it was not designed to address weight stigma or the multi-level context in which body image resilience develops. This limitation aligns with our earlier critique regarding the gap between individual resilience strategies and broader systemic changes needed to combat weight stigma effectively. PRISM extends this by positioning holistic wellness as both the outcome and process that emerges when all components work synergistically across multiple levels. In the PRISM model, wellness represents the synthesis of intrapersonal resilience, interpersonal support, and systemic protection against weight stigma – each element reinforcing the others.
To illustrate how these components work together in practice, consider a woman seeking medical care for a non-weight-related condition but encountering weight stigma from her healthcare provider, a common experience (Puhl et al., 2021a). A stigma-resilient self-concept enables recognition that personal worth and health are not defined by weight, reducing internalised bias impacts. Stigma-specific coping strategies provide tools to challenge weight-based assumptions through assertive communication and requests for respectful evidence-based care and treatment options. At the same time, support systems (such as weight-inclusive healthcare networks) provide validation, guidance, and the resources needed to navigate healthcare interactions effectively. On a broader level, systemic strategies, including anti-discrimination legislation, institutional policies and training programs, aim to reduce implicit weight bias among healthcare providers, ensuring that future interactions are both legally protected and clinically appropriate. Together, these components empower women while driving systemic change, illustrating PRISM’s multi-level approach to building resilience in environments that have historically perpetuated weight stigma.
Knowledge gaps and future directions
While PRISM is a novel theoretical model for enhancing body image resilience amid weight stigma for women, realising its full potential requires rigorous empirical validation. A key priority is developing measurement tools that capture both individual and systemic components of resilience. Existing measures, such as the Modified Weight Bias Internalisation Scale (WBIS; Pearl and Puhl, 2014), the Body Appreciation Scale-2 (BAS-2; Tylka and Wood-Barcalow, 2015b), and the Self-Compassion Scale-Short Form (SCS-SF; Raes et al., 2011), provide a foundation for PRISM components. However, measurement tools capturing PRISM’s multi-level components are needed. The Adult Resilience Measure (ARM; Liebenberg and Moore, 2018) offers a socioecological framework consistent with PRISM’s multi-level approach. Adapting or integrating these tools is an important next step for comprehensive assessment aligned with the model.
From a health psychology perspective, PRISM advances conceptualisations of resilience by moving beyond individual-focused models of stigma management toward integrated approaches that recognise reciprocal influences between psychological resources and social environments. To elucidate these processes, mixed-method designs are needed. Qualitative methodologies (e.g. focus groups, in-depth interviews) will map lived resilience experiences and refine theoretical constructs. Longitudinal studies and randomised controlled trials can clarify causal mechanisms and rigorously evaluate the effectiveness of PRISM-informed interventions over time. Implementation science approaches are also needed to guide translation into healthcare, education, and media systems. This includes co-designed interventions that align with the model’s multi-level focus and support systemic change.
Future research should examine how intersectional factors, including race, socioeconomic status, gender identity, and health conditions shape weight stigma and resilience pathways. Exploring the applicability of PRISM to men and gender-diverse individuals, whose experiences and resilience processes may differ, is also needed. These steps will refine and validate the model, informing interventions and policies to promote body image resilience in stigmatising environments. In broader efforts to address weight stigma, theoretical approaches that target other psychosocial factors such as depression and disordered eating in relation to body image should also be considered.
Conclusion
The PRISM model addresses the pervasive impact of weight stigma on body image, using the experiences of women as a defining example to build the model. It integrates key individual-level components such as a stigma-resilient self-concept and stigma-specific coping strategies, with inclusive support systems and systemic strategies that challenge weight-based discrimination at its core. Through interdisciplinary research, policy reform, media accountability, research-to-practice translation, and intersectional approaches tailored to diverse lived experiences, PRISM offers actionable touch points to dismantle weight stigma’s harmful effects. This integrated approach aims to strengthen individual resilience and promote collective advocacy for systemic change. Translating PRISM into effective weight stigma and resilience-building solutions ultimately requires sustained commitment across sectors, from workplaces and healthcare systems to policy makers, media organisations and community advocates, to create environments where women’s bodies are respected rather than stigmatised. Through this coordinated effort, PRISM offers a pathway toward body image resilience through individual empowerment and transformed social environments that support holistic wellbeing and women’s health outcomes across societal layers.
Footnotes
Ethical considerations
Ethics approval was not required for this review article as no data were collected from participants.
Consent to participate
Consent to participate is not applicable to this review article as no data were collected from participants.
Author contributions
MD: Conceptualisation, writing original draft, writing – review & editing. HS: Writing – review & editing, Supervision. ACIR: Writing – review & editing, supervision. BH: Conceptualisation, supervision, writing – review & editing.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: MD is funded by a Monash Graduate Scholarship supported by an Australian Research Council (ARC) Discovery Project (DP220101107) and RTP scholarship. BH is funded by an Australian Research Council (ARC) Discovery Early Career Researcher Award (DE230100704).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All data are available in the manuscript and supplementary materials
