Abstract
The COVID-19 pandemic disrupted breast cancer care, exacerbating disparities among racial and ethnic minority groups. This qualitative study explores the experiences of African American and Latina breast cancer survivors in the Washington, DC, metro area. We conducted semi-structured interviews to examine their experiences during the pandemic and the impact of the pandemic in their wellbeing. We used consensual qualitative analysis to analyze the interviews. Participants (
Introduction
The onset of the COVID-19 pandemic complicated cancer care, resulting in reductions in cancer screenings, diagnoses and altered treatment protocols (Carvalho et al., 2022). A systematic review found that hospital visits and admissions for cancer patients demonstrated a significant reduction during the first 10 months of 2020 (Angelini et al., 2023). Breast cancer biopsies decreased by up to 71% from March to July 2020 (Patt et al., 2020), and many procedures, such as mastectomies to remove malignant tumors, were postponed and reclassified as “elective” due to COVID-19 hospital burden (Martinez Leal et al., 2023). A 2023 systematic review found reductions of greater than 25% in breast cancer diagnoses and a lower proportion of early-stage detection during the pandemic (Li et al., 2023). Other research has predicted an additional 2500 breast cancer deaths as a result of COVID-19 treatment delays, with 30-day mortality almost doubling among breast cancer patients in 2020 (Alagoz et al., 2021; Di Cosimo et al., 2023). In addition to challenges with breast cancer care, the pandemic also led to increased isolation and psychological distress due to fears of cancer progression and increased COVID-19 vulnerability (Martinez Leal et al., 2023) as well as unmet care needs during the pandemic related to the emotional, physical, spiritual, familial, and healthcare realms of daily living, including reduced accessibility and support for cancer symptom management (Legge et al., 2023).
The burden of these negative outcomes was disproportionally experienced by racial and ethnic minoritized cancer survivors (Giaquinto et al., 2022) who already experienced striking disparities in breast cancer outcomes before the pandemic (Giaquinto et al., 2022; Mitchell et al., 2022). Although COVID-19-related breast cancer treatment delays were experienced by all racial and ethnic groups (Mullangi et al., 2022), Black and Latina women were more likely to be affected. Breast cancer patients who self-identified as Latino/Hispanic, Black, Asian, or another race were more likely to experience COVID-19-related treatment delays or changes than those identifying as Non-Hispanic White (Satish et al., 2021). The care delays ranged from 3 to 8 weeks, potentially resulting in a significant increase in breast cancer mortality among minority populations (Satish et al., 2021). Furthermore, from 2019 to 2020, individuals identifying as Hispanic and Black experienced a greater reduction in breast cancer screening (64.2% and 53.9%, respectively) than those identifying as Non-Hispanic White (49.2%; Amram et al., 2021). This reduction in screening rates may result in an increase in later-stage diagnoses among Black and Hispanic women.
Contributing factors to the augmented treatment delays and decrease in screening rates seen in the Black and Latina population include insurance and financial challenges. In a qualitative study of women diagnosed with breast cancer during COVID-19, Black and Latina breast cancer survivors reported experiencing greater care disruption and financial-related challenges than their White peers (Martinez Leal et al., 2023). Black and Latina breast cancer survivors experienced the compounding of pre-pandemic disparities in breast cancer care and disparities in COVID-19 burden. Although evidence demonstrates that COVID-19 caused delays in both cancer care and decreased screening; there is a paucity of qualitative research examining the experiences of Black and Latina breast cancer survivors during the pandemic. This qualitative study aims to examine Black and Latina breast cancer survivors self-reported experiences during the pandemic, as well as the impact of the pandemic on their wellbeing.
Methods
Participants
In order to be eligible, participants recruited for this study had to have been diagnosed with breast cancer at any stage during their lifetime, self-identified as Black/African American or Latina, and speak English or Spanish fluently.
Procedures
An academic institution partnered with two community-based organizations (CBOs) that provide cancer education, support, and navigation to Black/African American and Latina breast cancer survivors. The CBOs were involved in all phases of the project, including protocol development, recruitment, development of study materials, interpretation of study findings, and dissemination. Following IRB approval, CBOs shared study flyers via email and social media with their respective networks. Once CBOs identified potentially eligible participants, they asked the individuals for permission to share their contact information with the research team. Research assistants (RAs) called potentially eligible participants to confirm eligibility and conducted the verbal informed consent by phone. RAs conducting the interviews were in college or had completed college in a science-related discipline such as Biology, Psychology, or Global Health. Out of five the RAs, one was monolingual in English, and four were bilingual in English and Spanish. All RAs were trained in conducting interviews and qualitative analysis by faculty members in the team with expertise in qualitative research.
Once consented to participate, participants completed a survey that included sociodemographic, clinical, and psychosocial outcomes. Participants had the option to complete the survey using an online portal or to have a RA conduct the survey by phone. After completing the survey, RAs asked participants whether they would like to participate in a semi-structured interview to share their experiences with COVID-19, the impact of COVID-19 on their wellbeing, and suggestions for developing educational materials. The interview process lasted approximately between 25 and 45 minutes and was conducted over the phone between the participant and a bilingual trained RA in the participant’s preferred language. All study participants were compensated for their time in completing the surveys, and those who opted to do the semi-structured interview received additional compensation for their time. Telephone interviews were audio-recorded with participant consent, then transcribed verbatim by a professional transcription service. This paper focuses on the qualitative analysis of the interviews.
Measures
Semi-structured interview
The interview focused on women’s experiences during the pandemic while seeking medical care and how COVID-19 impacted them physically, emotionally, financially, and socially.
Analysis
Positionality statement
The authorship team is comprised of academic researchers, undergraduate/graduate students and community partners. Our research team was entirely female and mostly of Hispanic/Latina descent, while the other research team members identified as Non-Hispanic White. Additionally, every member of the research team had a background in behavioral science and public health. The community partners were breast cancer advocates who self-identified as Hispanic/Latina or Black/African American and two of them were breast cancer survivors. The community partners had extensive expertise and experience providing support to breast cancer survivors from Black/African American and Latin American communities. The diverse backgrounds and cultural similarities between the researchers, the community partners, and the participants added nuanced interpretation and a reflective approach to the data.
Results
Sociodemographic and clinical factors
The final sample included 40 participants of which 70% (
Sociodemographic characteristics of the participants (
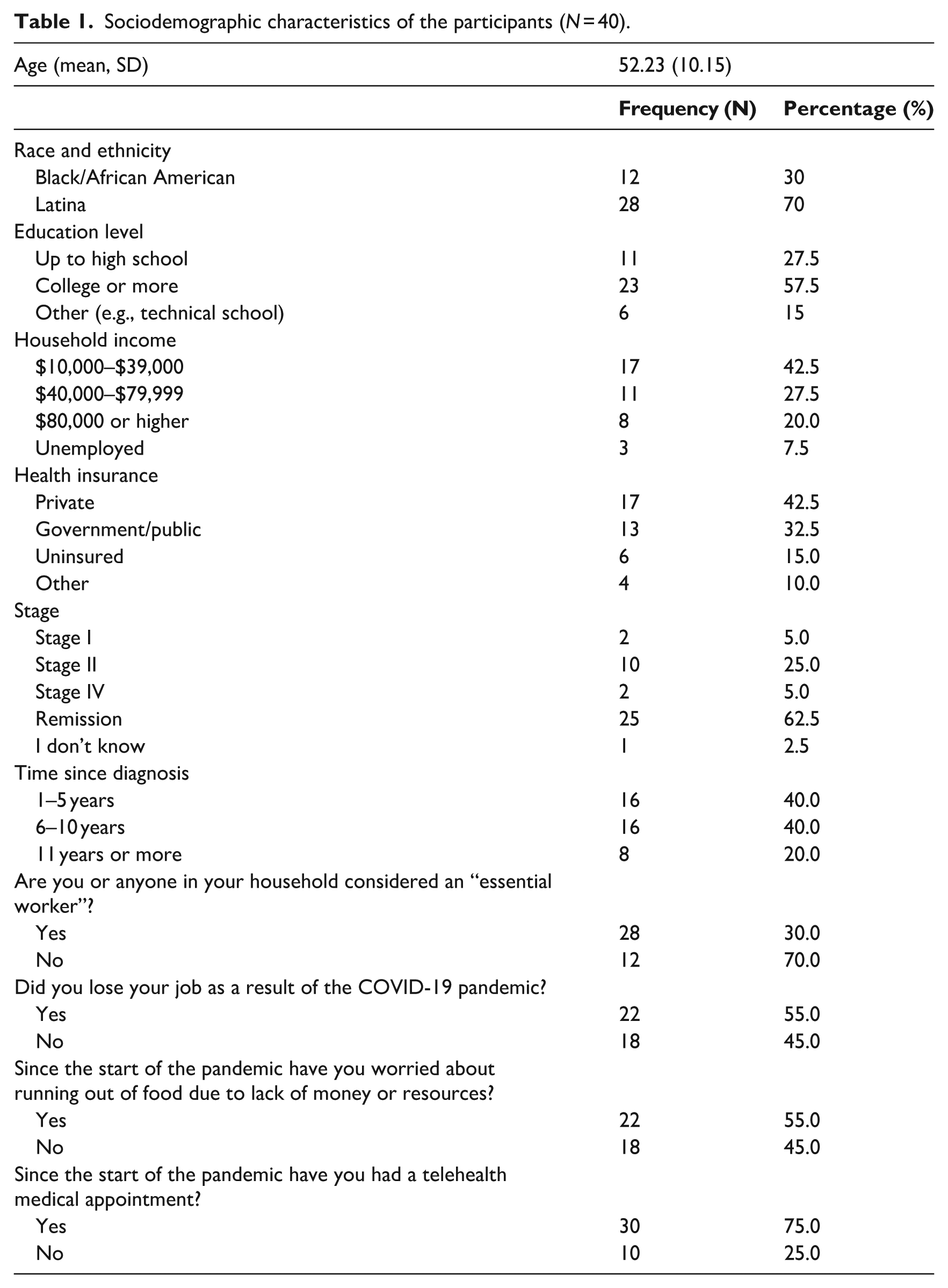
There were various themes that were identified during the interviews. We grouped re-occurring impacts that participants experienced during the pandemic into seven major themes. We selected several quotes that best highlighted participant’s challenges. Bilingual team members translated Spanish quotes into English. See Table 2 for additional quotes.
Additional Exemplary Quotes.

Breast cancer care impact
Women reported experiencing more barriers and difficulties to obtain their cancer care/treatment as a result of the pandemic. Some of the biggest impacts to their cancer care included: harder to schedule appointments, canceled/delayed medical appointments, transitioning from in-person to telehealth appointments, financial struggle, loss of health insurance, suboptimal communication with their providers, and delayed processing times for their medication. As described by one participant: “It was a little harder to schedule my yearly mammogram this year, just because they’re spacing out appointments more, and you had to wait in your car. You couldn’t come in until you’re right before your appointment, those kinds of things. It was a little harder to just schedule the regular things that I try to do as a breast cancer survivor to make sure I’m taking care of myself.” [ID 012, Black/African American]
Participants also faced challenges when they were able to access care. For instance, one participant expressed how stressful it was for her to undergo surgery due to the fear of being infected with COVID-19, and the loneliness she felt due to the COVID-19 restrictions for caregivers to stay at the hospital: “Until they’d take me to the surgery. But this one, it was, it was so much, it was, it was as difficult, like it wasn’t, I’m sorry, it wasn’t more difficult. I just had to get a COVID-19 test a couple of days beforehand, and my mom kind of couldn’t, she had to wait in the lobby, then she found out she couldn’t wait in the lobby, she had to go wait in her car, which was terrifying for her and for me because I was by myself.” [ID 014, Black/African American]
Several women described how they had to transition from in-person to telehealth appointments. While some mentioned the convenience of telehealth appointments, others faced important challenges. For instance, some participants voiced concerns about losing the in-person examinations component.
“It’s an awkward feeling when I had my oncology appointment through the virtual. So there’s no hands-on from my oncologist where she can examine me. So she has to rely on what I tell her.” [ID 010, Black/African American]
Others reported not having a phone due to financial struggles or not being able to attend any calls while working due to the work policies that forbid them to use their phone. This impacted their ability to schedule appointments or receive calls from the medical team.
Women reported undergoing major financial struggles and losing their health insurance, diminishing their possibilities to afford critical cancer screening and medications.
“And with the fact that I didn’t have a job and that they were asking me for about 360 dollars to go for a consultation, and we without having anything, without working, my husband without having a job, without having money – because my children have their own responsibilities and
On the other hand, some women also reported positive outcomes in their cancer care/treatment during the pandemic, such as finding telehealth appointments to be easier and more convenient or reporting no impact in their cancer care as a result of the pandemic.
“If I’m not getting any blood work done, I’ve been just doing video appointments, which I’m fine with. A lot of people are like, “I want to see the doctor in person,” which is fine, too. Everybody has their thing. But if I’m not getting any blood work, why am I gonna bother going?” [ID 042, Black/African American] “I’ve been able to do most of my doctor visits over telemedicine. My doctors are very good about making sure, okay, do I actually really have to have you come into the office for this? Or can we do it over a video call or have a phone call over it instead? So, if I needed to come in, I could, but they were very good about, “I think we could do this over video call and it’s safer for everybody.” [ID 012, Black/African American]
Lifestyle impact
The pandemic imposed an unprecedented change in lifestyle for most participants. Most changes discussed were part of one or more of the following areas: daily routine, job/work, grocery shopping, exercise/fitness routine, socialization/social events, leisure activities, and diet. Additionally, women reporting leaving the home less often, canceling social gatherings/activities, going grocery shopping once a month instead of weekly or not attending places such as restaurants or church compared to before the pandemic.
Perhaps one of the biggest challenges women faced was confinement, and not being able to leave the house frequently or see their loved ones. For instance, one participant describes how she was not able to see her family members and only left the house for necessities, since she was a two-time breast cancer survivor and did not want to get infected with COVID-19: “I didn’t see my daughter and my granddaughter. I pretty much, you know, confined myself except for going to the grocery store and to the doctors. I am somebody who did not want COVID-19 because, you know, a two-time cancer survivor.” [ID 001,Black/African American]
Many women reported having a reduction in work hours/shifts, changes in work schedule, changes in work environment, or a shift from in-person to virtual work. Some ways in which participants had their jobs impacted are highlighted below: “Yes, I work driving a truck. So, I just went, worked and came back. That is, I have worked sporadically. Not like before, every day. If not, the pandemic has also hit us with that, right?” [ID 046, Latina]
Financial impact
As a result of the pandemic, participants in the study experienced substantial financial stress. The most frequently reported challenges were unemployment and work schedule changes that led to decreased income, further exacerbating their financial situations. Consequently, many individuals were not able to access affordable food, healthcare, and housing.
“It affected me financially. Definitely my income. I was on unemployment for several weeks. I had trouble getting unemployment to the point where I didn’t get my first unemployment until I was actually off of furlough and back at work and I had to get it retroactive. So, I was concerned. Can I make my mortgage this month, ‘cause I don’t have my employment? Can I get groceries?” [ID 012, Black/African American]
Additionally, many expressed concern about their ability to provide support for their loved ones residing abroad. The majority of participants who kept their jobs held in-person jobs, increasing their vulnerability to infection.
“I believe that the Hispanic community has been, if not the most affected,
Financial strain and limited healthcare also appeared to cause emotional distress, as expressed by this participant: “My partner got really sick and couldn’t go to work. He was unemployed for over a month. So, when he didn’t work, there was no money coming into the house, and that made me feel really bad. Because I thought, how are we going to manage now? How are we going to eat, pay rent, bills?” [ID 048, Latina]
Social impact
Many individuals expressed a sense of isolation and loneliness due to the lack of social interactions resulting from pandemic restrictions. This isolation affected participants’ mental health, while also causing the loss of many friendships. Participants were unable to visit family, travel to their home countries, attend important events such as graduations, birthdays, and even funerals, which led to feelings of sadness, anxiety, and missed opportunities to create memories with loved ones. Some participants shared that the inability to hug loved ones was particularly difficult to adapt to. The generalized fear of infection further affected social interactions.
“I think the thing that affects me the most is not being able to hug and see my family. I have a grandson that graduated from high school, was not able to attend that. I have missed those types of things and can’t get them back.” [ID 007, Black/African American]
Despite all these difficulties, many individuals found ways to adapt through virtual means and outdoor events. Additionally, parents had the opportunity to spend more time with their children at home, which served as a way to cope with pandemic-related stress.
“Not everything has been bad for me. This has been the only time I’ve had the opportunity to truly spend time with my daughter since I’m working all the time and she’s 13 years old. I had never had the chance to spend so much time with her.” [ID 017, Latina]
Mental health impact
The pandemic impacted the psychological state of participants in different ways, both in the sense of self, and as a result of others’ struggles. On one hand, some people experienced increased anxiety, fear, stress, and depression.
“ I know, like I said, the initial part of
This resulted in several outcomes, with some people turning to “emotional eating,” while others developed a fear of leaving their home. On the other hand, some people experienced increased loss, empathy, and paranoia as a result of struggles other people, or relatives were experiencing.
“We are very paranoid. We have to clean our hands every moment of the day. If we see someone coughing near us, we get nervous thinking they could have the virus.” [ID 043, Latina]
Particularly, in the Hispanic/Latina sample, many of them discussed how family members in their home country were experiencing difficult times as a result of the pandemic, or losses, and they could not travel to be there with them.
Physical impact
As for physical impact, many participants reported having being either diagnosed with COVID-19, or having close family members diagnosed with COVID-19. Additionally, some reported decreased physical activity due to isolation and reporting closures, followed by changes in eating habits (binge-eating/loss of appetite) that ultimately led to reports in weight gain or weight loss among participants.
“I felt like I’ve become an emotional eater. I hate that. This morning I was like, oh my gosh, you gotta drop some pounds. Like it’s made me too still. Now it’s easy if it’s raining or snowing to just lay down and eat whatever you want all day, versus if I had a job, not all jobs are gonna allow you to stay at home. So, yeah, it has affected me physically.” [ID 018, Black/African American]
One participant explained how the stress also had a detrimental impact on her physical health: “Stress always impacts our immune system. I am a cancer survivor and I know that very well, and I worry a lot and I get sick; If I’m sad my defenses go down. And well, during all this time, it has happened to me several times, that is, it has happened to me that I feel too much anxiety, I feel too much stress, and well, I start to feel physically bad.” [ID 015, Latina]
Positive aspects
Participants were also asked to reflect on the positive aspects of the pandemic. Many of the responses provided by participants were geared toward the notion of being able to save time on some aspect of daily life, that allowed them to have more time to do other things. Such as, having more time to exercise, spend with family, learn new skills, clean/organize home, work on unfinished tasks, rest, do leisure activities, etc. The most prominent positive social aspect discussed among all interviews was having more family union and communicating more with friends/family. In terms of financial benefits, many participants described being able to save money on shopping, gas, parking, restaurants, etc. Some women reported minimal disruption to their financial situations and health insurance coverage. Additionally, mentally, many participants described being more mindful about themselves/others, feeling happier/less stressed, practicing self-reflection, feeling closer to God or being more spiritual. In terms of positive physical aspects, some participants described exercising more, being more clean/hygienic, practicing a better diet/lifestyles, losing weight, or feeling in better physical shaped compared to before the pandemic.
“This may sound weird, but time off. Stress associated with work. So, being home, being in my own space. I absolutely do not mind and still don’t to this day going to restaurants. I now prefer to cook my own. Some of those restrictions that are put in place, I kinda hope they carry on.” [ID 020, Black/African American]
Despite these hardships, community members came together to provide support through donations during these difficult times and community-based organizations played a key role to support survivors.
“I have had support from(CBO name) , which is an organization that helps Latinas living with cancer.
Discussion
The pandemic had a nuanced impact on the lives of Black and Latina breast cancer survivors, affecting everything from access to care to spirituality. Women in our study reported leaving the house less often, decreased social interaction, diminished physical activity, and work schedule changes/unemployment resulting in financial hardship. Barriers to care and these negative lifestyle changes contributed to the increased anxiety, fear, stress, and depression participants reported experiencing during the pandemic. To cope, participants highlighted the key role of community-based organizations to provide support via information, emotional support, financial assistance, and community connection. Positively, participants found that the pandemic afforded them more time to spend with family, engage in positive lifestyle behaviors (exercise, learning new skills), save money, and practice more mindfulness and spirituality.
Previous literature has demonstrated that Black and Latina women experienced disparities in breast cancer and COVID-19 outcomes pre-pandemic (Giaquinto et al., 2022; Wang et al., 2021). There is a paucity of research examining how these pre-pandemic disparities affected Black and Latina breast cancer survivors during the COVID-19 pandemic. Our study contributes to understanding the lived experience of Black and Latina breast cancer survivors.
Similar to our findings, in a qualitative study with breast cancer survivors, Martinez Leal et al. found that COVID-19 exacerbated loneliness, financial hardships, insurance challenges, treatment complications, and delays in care, especially among Black and Latina survivors. Patients reported experiencing heightened anxiety due to the failure of healthcare personnel to clearly communicate the reasons for treatment delays (Martinez Leal et al., 2023). In a survey of 1240 cancer survivors, Patel et al. (2022) found that Black and Latinx participants had three times the odds of reporting significant delays in their cancer-care continuum, and greater odds of adverse social and financial effects compared to White respondents. In our study participants reported numerous barriers to obtaining cancer care during the pandemic, including challenges scheduling appointments, appointment cancelations, delayed medication processing, stress during procedures as a result of COVID-19-induced distancing, and challenges communicating with providers and interpreting non-verbal cues due to the use of masks. Taken together, these findings suggest the importance of improving physician communication with breast cancer survivors, and the need for research in improving connection while maintaining social distancing guidelines. Sokas et al. (2021) found that perceived high-quality physician-patient communication increased patient ability to cope and accept delays and altered treatment plans.
To abide social distancing guidelines, many healthcare providers switched to telehealth appointments for routine check-ups. The role of telehealth in cancer care elicited mixed opinions among participants. Some participants found telehealth appointments to be more convenient, also reporting that telehealth helped them save money due to fewer outside excursions. On the other hand, some individuals found telehealth to be challenging due to lack of access to a telehealth platform. These findings are consistent with broader disparities in access to telehealth. Research has found that during the pandemic, low-income and Hispanic populations were less likely to use telehealth, with lower rates of telehealth usage reported by non-White and rural populations (Pierce and Stevermer, 2023; Qian et al., 2022). In our study, the challenges experienced by Black and Latina breast cancer survivors also included lacking access to a phone. This concern was especially salient among Latina women who were not allowed to pick up the phone during work or were not able to pay for the phone due to financial struggles. In addition to lack of access/diminished usage, participants highlighted concerns about losing the in-person aspect of physical examination, and worried that their self-examination reported via telehealth might miss important diagnostic factors. While the switch to telehealth for health care delivery during the pandemic affords increased accessibility and increased safety, there exist barriers in access to telehealth, especially among low-income, minoritized populations. This highlights the importance of implementing strategies to ensure disparities are not exacerbated during shifts in health care delivery modes.
Some studies have shown that the pandemic augmented feelings of anxiety and stress among breast cancer survivors (Martinez Leal et al., 2023). For instance, in a survey study Shah et al. (2023), found that participants undergoing breast cancer treatment during the pandemic or having at least three other comorbidities, reported significantly higher level of COVID-19-related anxiety compared to post-treatment survivors. Additionally, this study found higher levels of anxiety among survivors related to care delays and poorer coping (Shah et al., 2023). Similarly, a systematic literature review Ayubi et al. (2021), found a significant prevalence of depression and anxiety among cancer patients during the COVID-19 pandemic when compared to a non-cancer control. In our study, participants described heightened anxiety, fear, stress, and depression. Participants also reported pandemic-induced changes in eating behaviors, either augmented emotional eating and developing unhealthy eating behaviors due to stress or a loss of appetite. Additionally, 55% of the sample reported experiencing food insecurity. A healthy post-diagnosis diet decreases all-cause mortality and slightly reduces breast cancer-related mortality (Lee et al., 2022). This finding highlights the importance of implementing financial assistance programs to address food insecurity and providing increased counseling on maintaining healthy eating habits during times of unprecedented stress.
In terms of coping with the pandemic, a prior report found that African American breast cancer survivors increasingly turned to religion via increased engagement with religious activities, greater reliance on God, and finding joy and meaning through spirituality to manage psychological distress during the pandemic (Hamilton et al., 2022). In concordance with this finding, participants in our study described that the pandemic allowed them time to practice more mindfulness and self-reflection and helped them feel closer to God. This finding suggests the potential importance of encouraging spirituality and mind body medicine practices as coping mechanisms among breast cancer survivors.
Few studies have examined the positive effects of the pandemic on breast cancer survivors. A quantitative study, Sánchez-Díaz et al. (2025) found that post-pandemic, Hispanic breast cancer survivors reported improved physical and emotional well-being but a lower social well-being. Our study suggests that the beneficial outcomes Sánchez-Díaz et al. (2025) described in the post-pandemic group may be due to the increased time survivors had during the pandemic. For example, some participants highlighted how the pandemic afforded them more time to exercise, clean, maintain their health, learn new skills, complete unfinished tasks, and spend time with family. Some participants reported losing weight, increased connection and creativity. The pandemic allowed participants more free time to engage in wellness practices that may have improved their physical and mental well-being.
Our study has strengths and limitations. In terms of strengths, our paper addresses a gap in literature, using a qualitative lens to examine the positive and negative experiences of Black and Latina breast cancer survivors during the pandemic. Furthermore, the study included strong partnerships with Community Based Organizations. The qualitative, community-based approach of our study allows us to build off existing literature documenting pandemic-imposed disparities in breast cancer care, providing culturally specific perspectives that can inform future interventions. In terms of limitations, our study did not have equal representation of Black and Latina participants, with Latina participants comprising the majority of the sample. Additionally, all participants lived in the Washington DC, Maryland, or Northern Virginia (DMV) area in an urban environment, limiting our study’s generalizability to rural and suburban populations in other U.S. cities.
The pandemic had a multifaceted impact on Black and Latina breast cancer survivors, exacerbating pre-existing disparities in cancer care. Community based organizations play a key role in providing health related information from a trusted source and connecting minoritized populations to health care services, suggesting the benefit of partnerships between CBOs and healthcare providers to meet patient needs. In terms of future directions, more research is needed to continue to understand the effects of the COVID-19 pandemic among minoritized populations, and assess the potential needs in these communities in order to developed culturally-tailored interventions. Findings from this study can inform the development of interventions and policies to reduce disparities and improve post-pandemic care.
Footnotes
Acknowledgements
We are grateful to all the women that participated in our study, and gave us their time and trust to discuss the various challenges they experienced during the pandemic. Furthermore, we would like to thank Eddie Minaya for his assistance in literature review. Lastly, as special thanks to our community partners Nueva Vida and Thelma D. Jones Breast Cancer Fund for their partnership and continuous support and Dr. Erin Speiser, for their continuous support in the research.
Ethical considerations
This study was reviewed and approved by the Institutional Review Board (IRB) at Georgetown University (Study 00002709, 9/1/2020). Study participants gave verbal consent before starting interviews.
Consent to participate
Participants were consented orally and were informed of the voluntary nature of the study and interview and their ability to decline to answer any questions or withdraw from the study at any time, prior to study participation. Permission for interview audio-recording was solicited and granted prior to commencing the research activities.
Consent for publication
All authors of this manuscript have provided written consent for publication.
Author contributions
Dariana Sedeño-Delgado: Data curation, data analysis and writing of original draft
Priyanka Meesa: Writing - original draft preparation
Claudia Campos: Conceptualization, methodology, writing-review and editing.
Thelma D. Jones: Conceptualization, methodology, writing-review and editing.
Jacqueline Beale: Conceptualization, methodology, writing-review and editing.
Julio E. Sanchez Gonzalez: Data analysis and writing of original draft
Jennifer Argueta-Contreras: Data analysis and writing-review and editing.
Jennifer Rodriguez: Data analysis and writing-review and editing.
Natalia Monsalve: Data analysis and writing-review and editing.
Teresa Truong: Data analysis and writing-review and editing.
Annabelle Kim: Data analysis and writing-review and editing.
Kristi D. Graves: Conceptualization, methodology, funding acquisition, writing-review and editing.
Simina Boca: Conceptualization, methodology, funding acquisition, and writing-review and editing.
Alejandra Hurtado-de-Mendoza: Investigation, conceptualization, methodology, funding acquisition, data analysis and writing of original draft.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Georgetown-Howard Universities Center for Clinical and Translational Science (GHUCCTS). Research reported in this publication was supported by the National Center For Advancing Translational Sciences of the National Institutes of Health under Award Number UL1TR001409. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Simina Boca is currently an employee and minor shareholder at AstraZeneca. This work was performed as part of her duties at Georgetown University Medical Center, with no funding coming from AstraZeneca.
Data availability statement
The data collected and presented in the current study are not available publicly or by request due to privacy and ethical concerns.
