Abstract
The use of internet-based cognitive behavioral therapy (ICBT) is gaining traction. It is shown to be effective for pediatric functional abdominal pain disorders (FAPDs), yet little is known about parents’ experiences with this approach. Through nine interviews with 14 parents, we explored their experiences with receiving ICBT alongside their children. We developed two themes through reflexive thematic analysis: “Parental illness understanding,” examining parents’ understandings of their child’s symptoms, and “Redefining various parental roles,” describing how parents navigated and redefined their roles throughout treatment. Parents suspected a psychological component in their child’s symptoms before ICBT, which shaped their perception of ICBT as meaningful. While navigating parental roles was demanding and emotionally taxing, involving feelings of guilt and doubt, parents described a shift from chaos to a more balanced life. To validate these experiences, we recommend integrating a relatable fictional case into parent programs to acknowledge parental emotions.
Keywords
Introduction
Functional abdominal pain disorders (FAPDs), affect up to 15% of children and include functional dyspepsia, irritable bowel syndrome (IBS), abdominal migraine, and functional abdominal pain not otherwise specified (Thapar et al., 2020). FAPDs cause recurrent gastrointestinal symptoms that disrupt children’s daily lives (Boronat et al., 2017; Korterink et al., 2015) and are linked to increased healthcare use and a higher risk of anxiety and IBS in adulthood (Campo et al., 2001; Jarrett et al., 2003). They also significantly impact families, limiting parents’ work opportunities (Lalouni et al., 2019), complicating caregiving (Brekke and Brodwall, 2020), and causing mental strain, highlighting the need for early intervention (McGurgan et al., 2022).
Cognitive behavioral therapy (CBT) is the most evidence-based treatment for childhood FAPDs, addressing symptom-related catastrophic thinking and avoidance behaviors (Bonvanie et al., 2017; Sinopoulou et al., 2025). Parental involvement is crucial, as excessive emotional responses and symptom focus can reinforce the child’s pain (Guite et al., 2009; Walker et al., 2006). Accordingly, reducing parental catastrophizing is shown to alleviate symptoms (Lalouni et al., 2022). In CBT, parents act as co-therapists, supporting tasks like graded exposure while learning to reinforce positive behaviors and identify avoidance patterns (Diamond and Siqueland, 2001; Dowell and Ogles, 2010).
Internet-based CBT (ICBT) is emerging as an effective, accessible intervention for pediatric psychiatric and somatic conditions. It offers flexibility, reduces barriers such as travel and stigma, and allows families to engage in therapy at home (Hedman et al., 2012; Vigerland et al., 2016). Studies confirm its efficacy for FAPDs (Bonnert et al., 2017; Lalouni et al., 2019) and acceptance by parents and children (Lalouni et al., 2017; Levy et al., 2017). However, research on parental involvement remains limited, warranting further investigation (Vigerland et al., 2016). To date, only two studies have examined parental experiences with online FAPD treatment, both focusing on the same self-directed intervention (Nieto et al., 2015, 2019). While parents and children valued the coping strategies, nearly half wanted more professional contact (Nieto et al., 2015, 2019), highlighting the need for further exploration of parents’ perspectives on participating in ICBT alongside their child.
This study aimed to 1) Investigate parents’ overall perceptions of and experiences with an ICBT program for children with FAPDs and 2) Examine the meaning and impact of the treatment on daily life, including its perceived effects and influence on family dynamics.
Methods
We applied a qualitative methodology using semi-structured interviews which are well-suited for exploring parents’ subjective perspectives on ICBT. Unlike quantitative questionnaire studies that rely on predetermined response categories, this approach allows for deeper insights into their lived experiences, motivations, and the significance of various events.
Study context
The study was conducted in the Danish healthcare system, a tax-financed system where managing children with functional disorders follows a stepped-care model. General practitioners and municipalities manage mild cases by focusing on reassurance and normalization of symptoms. In moderate cases psychoeducation is provided in pediatric departments. Finally, children with severe functional disorders receive treatment in close collaboration between pediatric and psychiatry departments, as outpatient or inpatient care (Sundhedsstyrelsen, 2018).
The study was performed at the Department of Child and Adolescent Psychiatry, Aarhus University Hospital Psychiatry, Denmark as an add-on study to The Danish FGID Treatment Study (Skovslund Nielsen et al., 2025), which investigates the feasibility and effect of the Swedish-developed ICBT program in a Danish clinical context for children (8–12 years), adolescents (13–17 years), and their parents. The present study focuses on the younger group (8–12 years), as parents play a more prominent role in their treatment. Children were referred from pediatric departments or private pediatric practitioners to participate in 10 weeks of therapist-guided ICBT, comprising 10 modules for both children and their parents. The child-focused content included psychoeducation, identification of “stomach behavior” (i.e. symptom-related control or avoidance behaviors), exposure exercises, and a mindfulness exercise called “Stop, Observe, and Let go” (SOL). Parent-focused content addressed potential perpetuating behaviors, such as over-attending to symptoms, while emphasizing support for exposure exercises, fostering “Golden moments” (positive shared experiences), and encouraging self-care. Each week, families were expected to dedicate 4–6 hours to the program, divided between online sessions and practical applications in everyday situations. For example, parents should support their child in completing exposure exercises, such as eating pizza. Throughout the treatment, a therapist provided written feedback to support and motivate both children and parents (Lalouni et al., 2021; Skovslund Nielsen et al., 2025).
Study participants and recruitment
Inclusion criteria included parents of children aged 8–12 who completed the program from July 2023 to April 2024. Twelve families completed ICBT within this timeframe, of which eleven provided preliminary consent to participate. Following a 3-month follow-up questionnaire, families were contacted by the first author, LAPD, and invited to participate in the interview study. Nine families consented; one could not be reached, and one was unintentionally not contacted. Participation was based on parental choice, with one or both parents opting to participate. The final sample included 14 parents representing nine children.
Data collection
Through discussions within the research group, we developed a semi-structured interview guide with open-ended questions covering four main topics: everyday life before ICBT, life during ICBT, interactions with the therapist, and treatment effects. All topics collectively aligned with the established research questions. The parents were encouraged to share both positive and negative experiences, underscoring that all input was valuable. A translated version of the interview guide is available in the preregistration on OSF: https://doi.org/10.17605/OSF.IO/9WBDG.
From March to June 2024, LAPD, who was not a part of the original Danish FGID Treatment Study, conducted the interviews. Two pilot interviews were conducted to evaluate the interview guide and provide practice but were included in the final dataset as no significant changes were made. Interviews took place between 112 and 262 days (mean: 156 days) after completion of treatment. They were conducted via video (n = 8) or phone (n = 1), and all were audio recorded (duration: 54–70 minutes; mean: 62 minutes). LAPD consecutively transcribed the interviews verbatim in the original language (Danish).
Data analysis
We used a reflexive approach to thematic analysis (TA) to construct meaning-based themes relevant to understanding parents’ lived experiences with ICBT, ensuring critical, transparent, and considerate reflection throughout all stages of the research project (Braun and Clarke, 2006; Braun et al., 2019). We acknowledge that realities are shaped by and dependent on the individual. Therefore, we actively engaged in the knowledge-production process by drawing on our subjectivity and positions as researchers (Braun and Clarke, 2023; Varpio et al., 2017). We followed Braun and Clarke’s six steps for TA (Braun and Clarke, 2006), here adapted as an iterative and reflexive process, described in Table 1.
Demographics table.

Age when included in the FGID study.
The analysis was conducted in Danish, and selected quotes were translated and gently edited for readability using ChatGPT-3.5.
Ethics
The study was conducted according to the Helsinki Declaration (Association, 2024) and the Danish Code of Conduct for Research Integrity (Ministry of Higher Education and Science, 2014) and registered as part of the Danish FGID Treatment Study at the Central Denmark Region’s records of research projects (Sequential numbers: 769029, Case citation: 1-16-02-101-22) and the Danish Health Research Ethics Committee (Registration numbers: 1-10-72-80-22) without the need for further individual registration (Request journal no. 1-10-72-6-24). Before the interviews, all participants provided informed written and oral consent. Audio recordings, transcripts (pseudo-anonymized), and consent forms were stored in Redcap and MidtX,, a secure database in accordance with the General Data Protection Regulation (GDPR).
Results
The analysis showed that the greatest impact on family dynamics stemmed from the various roles parents had to fulfill. Furthermore, parents’ understanding of the disorder greatly influenced their experience with ICBT. As a result, two main themes were developed: “Parental illness understanding” and Redefining various parental roles,” along with five subthemes presented in Figure 1.
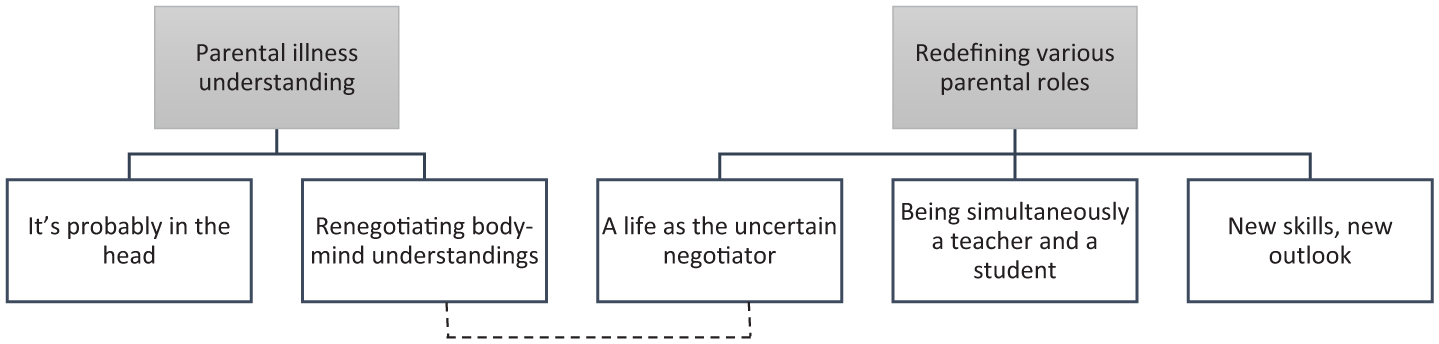
Thematic map with themes (grey boxes) and subthemes (white boxes). Solid lines indicate a connection between themes and subthemes, dashed lines indicate a connection between subthemes.
Before ICBT, the children had experienced stomachaches for an extended period (Table 2). In addition, some also suffered from nausea, vomiting, headache, chest pain, and limb pain. These symptoms significantly impacted the family’s daily life; some children became picky eaters, leading to conflicts during dinner; others struggled to fall asleep, requiring parents to stay in their room all evening; and some stayed home from school, making it challenging for parents to manage their work. Moreover, some children avoided leisure activities, dinners, and/or sleepovers with friends and family, further increasing their parents’ concerns and impacting the whole family life.
Analytical process.

Parental illness understanding
The first theme focuses on parents’ thoughts and understanding of their child’s symptoms and disorder. It also examines how these perceptions influenced their participation in the treatment and how their understandings evolved during ICBT.
It’s probably in the head
This subtheme unfolds the parents’ early thoughts about the cause of the symptoms before starting ICBT.
All parents had some kind of prior understanding of why their child had abdominal symptoms. Even before starting ICBT, most parents considered symptoms to be due to mental challenges. Frida’s mother reflected:
“All along, we talked about, it’s something in her head, something that travels from her mind and into her stomach.”
Likewise, some parents believed that symptoms were related to the child’s mental well-being as they observed a particular pattern in symptom occurrence, e.g., every morning before school.
Other parents talked about the family context and difficult experiences, such as losing a younger sibling or having a parent with a chronic disease, as abdominal symptom “triggers.” Also, in three families, siblings were dealing with psychiatric diagnoses.
The mother of 12-year-old Bertram, who had a younger brother with both psychiatric and somatic illnesses, shared her thoughts on how it might have affected Bertram:
“I suspect that what Bertram has been dealing with has been related to our life circumstances, that his stomachaches have been linked to our situation with a sweet little brother who needs something. . . different.”
In two other families, parents considered school dissatisfaction as the root of their child’s difficulties, noting that their child felt better during holidays. Despite engaging in the treatment and experiencing its positive effects, these parents, in hindsight, still viewed contextual factors as the primary contributors to their child’s struggles.
While most families initially considered the possibility of a psychosocial explanation, Emma’s parents were convinced that the symptoms occurred due to a small stomach.
“We did NOT get the impression that she was upset about coming to school, and consequently her belly hurts in the morning – we simply didn’t have that understanding!” (Father of Emma)
Still, they found the doctor’s suggestion of a functional disorder “interesting” and did not hesitate to join ICBT. Subsequently, they described it as an “eye-opener” to help Emma shift her focus by encouraging her to jump on the trampoline instead of using the toilet as a coping strategy.
Renegotiating body-mind understandings
This subtheme captures the parents’ understanding of their child’s symptoms during and after ICBT, highlighting how this understanding evolved through the interaction between parents and the ICBT program. Although the ICBT program presents an integrative mind-body explanatory model for FAPDs involving both biological and psychosocial factors, parents often wavered between viewing the symptoms as either physical or psychological in nature.
Although most parents suspected that psychosocial factors played a role for their child’s symptoms, their primary concern before ICBT remained the possibility of an underlying physical cause. Rather than giving attention to their intuition about a psychological explanation, they repeatedly considered potential physical causes, such as lactose intolerance, even during the ICBT process.
“Then I think, you know, it pops up again, and I just hope I don’t end up making him believe it’s all just in his head if he’s actually in pain.” (Mother of Bertram)
Like Bertram’s mother, many of the parents continued to express a rather dualistic perspective, that is, either a psychological or physical understanding of FAPDs. However, Hugo’s mother expressed a more integrated understanding:
“I just think it makes sense that it’s a connection between the physical and the psychological. That was probably the feeling we had ourselves as well.”
Likewise, other parents developed a broader understanding of the symptoms through the ICBT and described symptoms as a connection between mind and body, where abdominal signals can trigger alert responses in the brain. Yet some were more skeptical; Gry’s mother, working in the healthcare system, initially expressed reservations:
“My first thought was, ‘damn it’s psychosomatic’, the former term for functional disorders. But after reading about it, it actually made sense that the brain, in some way, overreacts to certain symptoms.”
She described how she initially had some prejudices about functional disorders, thinking of them as “like hypochondria or . . . those nothing-really illnesses”. However, these thoughts changed during ICBT, as she came to realize there was “an explanation for why Gry feels the way she does. And, basically, it’s a condition called miswiring”. Initially, she felt reluctant about being placed “in the psychiatry corner,” but she ultimately gained a deeper understanding of the disorder.
Redefining various parental roles
The second theme captures the different roles parents felt they needed to assume in relation to their child’s disorder and during treatment. Additionally, it examines how parents experienced the evolution of these roles from before starting ICBT to the completion of the treatment.
A life as the uncertain negotiator
This subtheme explores parents’ experiences of their role as caregivers in the period before the initiation of treatment.
Before ICBT, parents described a life characterized by uncertainty. They feared conflicts might arise, were unsure when symptoms would appear, and were uncertain about how the child would react. Daniel’s mother, working with children with special needs, described how she had experienced this time:
“It has been really tough. It’s no fun to get a screaming child out of the house, and you constantly feel guilty about whether you’re doing something wrong or getting angry. As the adult, you shouldn’t, but sometimes you just can’t take it anymore, and then you act out of helplessness.”
Several parents described feeling powerless and frustrated, wanting to help their child but unsure how to do so. They portrayed life before ICBT as a constant state of emergency, always on high alert due to uncertainty about the day’s outcome. This tense atmosphere led to escalating conflicts among siblings, between children and adults, and between parents, while everyday duties - such as encouraging the child to shower - could become a battle. At this point, parents’ lives were characterized by sleepless nights, and some felt overwhelmed by worry and constantly wondered how to help their child. Some parents considered contacting their private health insurance rather than waiting for the public healthcare system, and others sought help from an osteopath, adjusted their diet, or repeatedly visited their general practitioner, all to do their best with the knowledge and resources available to them.
Some parents described a fear that the diagnosis was their fault, that they had overlooked something, or that their parenting approach was incorrect. The mother of 9-year-old Gry described how she had discussed these fears and concerns with her husband:
“We talked a lot about, [. . .] ‘Why?’, ‘What are we missing?’, ‘What have we done wrong?’. We were looking for the fault in ourselves.”
The analysis revealed that some of the parents attributed the symptoms development to their own actions or behaviors.
As described in the subtheme “Renegotiating body-mind understandings” both before, during, and, for some, after ICBT, parents wavered between attributing symptoms to a physical cause or interpreting them as a sign of sadness or apprehensiveness. Since their understanding of the symptoms affected their role as parents before treatment, these subthemes are interconnected, as shown in Figure 1. Parents had to constantly deliberate on how to handle the symptoms without knowing their cause. Thus, parents adopted the role of negotiators. On one hand, thinking symptoms were mainly psychosocial, they aimed to maintain a normal life, encouraging the child to attend school. On the other hand, thinking of symptoms as primarily physical, they constantly feared overlooking a physically treatable disorder and worried that their approach might worsen the situation. The mother of 10-year-old Frida explained this:
“Even though we knew she wasn’t seriously ill, it still lingered in the back of our minds; ‘What if there’s something we’re missing because we’re not pushing hard enough (for a somatic diagnosis)?”
To help, some parents suggested that their child lie down or use the toilet when they experienced symptoms. However, their suggestions for helping remained focused on the symptoms rather than shifting focus, indicating the difficulty of parenting a child with FAPDs.
Being simultaneously a teacher and a student
This subtheme captures parents’ roles during treatment, fulfilling the role of a co-therapist for their child while also balancing their own mixed feelings of uncertainty, relief, and increased confidence.
Most parents accepted ICBT without hesitation and experienced it as relatively straightforward. Despite some parents wishing for increased interaction with the therapist to reduce uncertainty about their performance, the therapy contents were considered logical and “not rocket science.” The exercises were related to familiar everyday activities, making their integration into daily routines manageable. Most parents completed the modules with their child during the weekend and reinforced the program during the week through reminders, such as while driving or during dinner. Although parents found ICBT meaningful and straightforward, the analysis also revealed that its effectiveness relied on their active engagement and ability to take on multiple roles. Thus, ICBT posed challenges beyond the purely practical aspects, placing emotional and cognitive demands on parents.
Parents generally felt relieved when starting ICBT, as they felt that they were now taking actionable steps to address the issue. Additionally, by spending time completing the program, they demonstrated to the child that they cared and took their symptoms seriously:
“She suspected we didn’t believe her, since we couldn’t always say ‘Oh, poor you’ when she had a stomachache. But now, after working on these tasks, she could see that we took it seriously.” (Father of Frida)
While parents felt relieved, they also faced challenges, as they had to adopt the role of the organizer, remembering assignments and planning the week to incorporate them. Some parents experienced this role as stressful. They emphasized that successful participation required support from both parents, particularly in prioritizing tasks and jointly motivating the child. Although parents occasionally struggled to encourage their child, they persevered, recognizing it as essential for success:
“It’s difficult to be the ‘tough one’ and say: ‘Listen, this is how it’s going to be. You can do it’. It doesn’t feel great, but you know it’s necessary.” (Mother of Alfred).
Children’s resistance often stemmed from difficulties understanding the language used in the program, which sometimes included technical terms. To address this, parents also had to act as teachers, reading aloud and providing examples to help the child complete the modules. Moreover, if the child refused to complete an exposure exercise, parents felt they could rely on the program and refer to it as the specialists’ recommendation, providing a sense of authority and reassurance. Thus, despite the challenges, the program helped parents feel less alone in their responsibilities.
A few parents described the program as strenuous, finding it mentally taxing to continually evaluate efforts and consider whether they could do more. Ida’s mother explained why she found participation exhausting:
“It truly requires a lot to critically examine yourself and your parenting; it’s difficult to confront your own mistakes and shortcomings – not just being honest with yourself, but also with a stranger (read: the therapist).”
For some parents, the process felt alienating, as if they were losing their individuality within a larger system. Sharing personal and vulnerable thoughts with a stranger, especially in a program that facilitated communication with the therapist exclusively through written formats, was particularly challenging. Ida’s mother added how this made her feel as if “I was drowning or fading away, like I was more of a number than an actual person.” Despite the limited written contact, most parents regarded the therapist as essential to their experience and outcomes, providing positive support and guidance to help them remain focused and committed to the program despite the demands of their daily lives.
A few parents described uncertainty about their role in the program, feeling unsure whether they met its requirements. Some felt that the insights they gained made them realize that everything they had done before was wrong. Emma’s father described this new, harsh realization:
“During some of the modules, I thought: ‘Okay, we have done everything wrong,!’ because we told her to go to the toilet where she could just sit and think about the stomachache, and it was the complete opposite we were supposed to do!”
Before starting ICBT, parents had already questioned whether they were partly to blame for their child’s symptoms. As they learned more about symptom management, they recognized that some of their earlier behaviors might have unintentionally reinforced the symptoms. This feeling of guilt, as reflected in Emma’s father’s account, highlights the emotional challenges some parents experienced during the program.
New skills, new outlook
This subtheme captures parents’ experiences of their role as parents after completing ICBT, characterized by a sense of optimism and increased knowledge. However, for some, the process also prompted subsequent self-reflection and feelings of guilt.
Parents described an easier daily life as the overwhelming focus on abdominal symptoms subsided. Emma’s father illustrated this transi-tion:
“Actually, I had almost forgotten the program when you contacted us. Now we have the tools we learned in our backpack, and we have implemented them, so now this is just our everyday life.”
Parents were no longer in a constant state of alert, and their prior role as negotiators diminished, as they no longer feared that stomachaches would disrupt their child’s daily life. A sense of powerlessness was replaced with optimism as parents gained a deeper understanding of their child’s disorder and tools they could use for managing it. An enhanced understanding of their child, its symptoms, and their role in symptom management allowed them to handle potential frustrations or conflicts more effectively. As a result, they became more attuned to the child’s needs and more confident in their role as caregivers in general.
The program facilitated the development of a new shared understanding between parents and children. Bertram’s mother highlighted what she considered the most important learning from the program:
“The crucial difference for us is that Bertram has developed a language and an understanding of how to talk about his symptoms, and now, as I was a part of this learning, I also have the tools to talk with him about it.”
As parents and children completed the program together, they learned the same content in parallel, gaining a shared reference frame for understanding and managing the symptoms. They thereby developed a shared language, which they used when something became difficult after completing the program, e.g., parents told the child to try SOL if they complained about stomachaches.
Despite gaining valuable tools for symptom management, a few parents still expressed continuing concern and hesitation. Alfred’s mother reflected on her doubts about their effort:
“Are we really doing the things we learned well enough? We don’t actually know that. I mean, I can see some changes, so I expect we are, but I still have these doubts. Are we just letting it drift?”
For some parents, despite their overall satisfaction with the program and newfound confidence, a persistent sense of uncertainty or even guilt remained as they questioned whether they were managing the symptoms correctly or whether they should be doing more. This state of uncertainty thus persisted as a fundamental condition for some parents.
Discussion
This study explored parents’ experiences with ICBT for their child’s FAPD, including its impact on daily life and family dynamics. Through a reflexive TA, two overarching themes were developed: 1) “Parental illness understanding:” Before ICBT parents often suspected psychological factors but remained preoccupied with excluding potential physical causes rather than trusting their intuition about the impact of such factors. After treatment, some maintained a primarily psychological perspective, while others adopted a more integrative mind-body view. 2) “Redefining various parental roles:” Highlighting how parents balanced multiple roles, supporting their child, managing daily routines, and addressing their own understanding and guilt, but also how these roles evolved during treatment. Thus, despite these challenges, most felt empowered in their caregiving role through ICBT.
Few studies have explored parents’ experiences with psychological interventions, like ICBT, for childhood FAPDs. In the present study, parents found ICBT meaningful and manageable, noting its positive impact on their child’s symptoms, its ease of integration into daily life due to its online format, and its ability to help them support their child. We propose three possible explanations for these positive experiences.
First, the findings from Theme 1, “Parental illness understanding,” reveal how most parents already considered their child’s symptoms to have a psychological component before starting ICBT, which may have facilitated acceptance and engagement in this type of treatment. Existing research indicates that parents of children with FAPDs often initially struggle to accept the diagnosis and understand the pain, but also that psychological interventions can help reframe the pain from “unpredictable” to “predictable,” thereby reducing its impact on families (Nieto et al., 2020; McGurgan et al., 2022). In contrast to studies reporting parental resistance to psychosomatic explanations, our sample showed minimal hesitation, possibly reflecting a self-selected group more open to psychological treatments. Additionally, while some parents maintained a rather one-sided psychological understanding of the symptoms after ICBT, others acquired a more integrative mind-body understanding. One might consider whether there are disadvantages when not adopting such an integrative perspective through the program; however, our findings do not suggest this, as all parents found ICBT helpful regardless of how their symptom perspective evolved.
Second, as described in Theme 2 as part of the subtheme “New skills, new outlook,” the parents developed a shared language around symptoms with their child which facilitated symptom management and an enhanced understanding. This process contributed to a strengthened parent-child relationship, as also shown in previous research on psychological interventions for recurrent abdominal pain (McGurgan et al., 2022). Although McGurgan et al. did not focus on online treatment, parents in their study learned to contain their child’s pain through psychological interventions, and gained an understanding of how their actions could affect the symptoms (McGurgan et al., 2022). Parents valued being actively involved, emphasizing how ICBT helped them move away from a previous sense of being at a loss. These findings suggest that ICBT not only supports symptom management but also provides a unique opportunity for parental empowerment.
Third, participants in our study received weekly written feedback from therapists. While this feedback was appreciated, some parents still wished for more direct contact with a therapist. This aligns with Nieto et al. who examined an online CBT-based treatment for children with FAP and their parents, which, unlike our ICBT, was entirely self-guided. Despite overall satisfaction, parents and children also expressed a desire for professional contact (Nieto et al., 2015). The importance of therapist guidance is further emphasized by strong evidence showing that guided ICBT is more effective than unguided treatment (Palmqvist et al., 2007; Johansson and Andersson, 2012). However, even if some parents in our study wished for more therapist contact, most felt well-supported. The continuous connection with a dedicated therapist may have contributed to parents’ positive experiences with ICBT because it provided them with a feeling of reassurance and a sense of not being alone in the process. Still , incorporating a blended care approach or an initial face-to-face session may further strengthen the sense of support and enhance the overall effectiveness of the ICBT intervention. Blended approaches, combining digital interventions with professional interaction, have been shown to be feasible and to improve treatment outcomes and satisfaction (Erbe et al., 2017). For example, an initial in-person session could help establish rapport, clarify treatment goals, and address individual concerns, thereby enhancing engagement and trust.
The findings of theme 2 highlight the multiple roles parents had to navigate before, during, and after treatment, along with the associated responsibilities that influenced family dynamics. Although demanding, this redefining process was ultimately fruitful for most, transforming daily life from frustration to optimism. Parents’ descriptions of life before ICBT as chaotic and marked by feelings of powerlessness, as reflected in the subtheme “A life as the uncertain negotiator,” align with previous research showing that 60%–70% of parents of children with FAPD report substantial caregiving strain (Calvano and Warschburger, 2018). Parents of children with chronic pain similarly describe their lives as “a never-ending battle” marked by overwhelming demands (Sjögård, 2019). Furthermore, studies suggest that parents often assume the role of a “care coordinator” when navigating the healthcare system (Manderson and Smith-Morris, 2010) and in a qualitative study on parents’ caring for children with functional disorders, parents reported feeling over-responsible, insecure, and overwhelmed when managing symptoms at home (Hulgaard et al., 2019).
Participating in ICBT required parents to assume multiple roles, as captured in the subtheme “Being simultaneously a teacher and a student.” Parents found it meaningful to act as students, learning new skills, and as teachers supporting their child. Although demanding, this active dual role enabled them to support their child effectively. The importance of parental engagement in treatments like ICBT is well known, as it requires parents to support therapeutic efforts at home and adapt their parenting behaviors (Lamparyk et al., 2023). Nevertheless, in contrast to our findings, previous studies suggest that parents experience challenges when taking on an active role as co-therapists. For example, Lundkvist-Houndoumadi et al. found that parents and therapists sometimes had differing role expectations, with parents preferring to remain “just the parent,” while therapists aimed to transfer more responsibility to them (Lundkvist-Houndoumadi et al., 2016). Furthermore, Baker-Ericzén et al. identified barriers such as feelings of blame, judgment, or not being heard by therapists (Baker-Ericzén et al., 2013). This difference between our findings and prior research may be partly explained by the online format of ICBT, which requires substantial parental involvement from the outset. Rather than viewing this responsibility as a burden, parents in the present study perceived it as natural and empowering due to the program’s clear and accessible content, which aligned well with their needs. A key advantage of the ICBT format may be that the material can be revisited repeatedly, allowing parents to refresh their understanding as needed—unlike face-to-face sessions, where parents rely more on remembering the contents presented at the time. By offering a structured approach, ICBT can thus bridge the gap between professional treatment and parental involvement, helping parents feel less overwhelmed by transforming their frustrations into manageable tasks.
A potential challenge during ICBT was the emergence or intensification of parental guilt and self-blame. This was particularly reflected in the subthemes “A life as the uncertain negotiator” and “Being simultaneously a teacher and a student.” Some parents expressed guilt over their perceived inability to support their child before treatment or questioned whether they had fully adhered to the program. Others came to realize that earlier well-intentioned efforts may have inadvertently hindered their child’s progress, raising fears that they had contributed to the persistence or worsening of symptoms. These experiences align with findings from research on parents of children with chronic pain and FAPDs. For instance, Le et al. reported parental guilt and sadness over not being able to alleviate their child’s suffering (Le et al., 2019). Bradshaw et al. highlighted the emotional strain caused by diagnostic uncertainty (Bradshaw et al., 2022) while Brodwall et al. noted that some parents blamed themselves in the absence of an somatic explanation (Brodwall et al., 2018). Our study highlights the risk of inducing or worsening already experienced feelings of guilt in some parents. While ICBT is designed to empower families, it may unintentionally elicit guilt as parents reflect on past actions. These insights underscore the importance of explicitly addressing such emotional responses within ICBT content and therapist feedback to help normalize these feelings, reduce distress, and support ongoing parental engagement and well-being.
Strengths and limitations
Participants likely represented a selected group as they had all accepted psychological treatment and completed the ICBT program. This limits insights from families who rejected the treatment and from dropouts, and future studies could focus on exploring these families’ perspectives. We acknowledge that the results are not generalizable quantitatively, nor are they intended to be. However, as the developed themes are transferable to similar contexts, they may enhance our understanding of parents’ experiences when engaging in internet-based psychological treatments for various child conditions.
A key strength of this study was the recruitment of participants until adequate information power (IP) was estimated to have been achieved, ensuring a robust analysis (Malterud et al., 2016). We successfully recruited participants who had recently completed the program and thus could recall their experiences in detail. At the same time, they had the opportunity to reflect on their experiences and apply the tools in their daily lives. Furthermore, LAPDs status as a junior researcher did not compromise IP, as she received continuous supervision from senior researchers (SL and CUR). Finally, ongoing discussions within the interdisciplinary research team ensured researcher triangulation and focus on critical reflexivity throughout the process. Moreover, a strength of the data collection was that parents were encouraged to share both positive and negative aspects, without filtering their experience. Additionally, LAPD’s non-involvement in the original Danish FGID treatment study helped ensure that their perspectives were unbiased.
Implications for practice
Our qualitative findings highlight important considerations for enhancing the clinical application of ICBT. A key implication is the need to acknowledge and validate parents’ potential feelings of guilt and self-blame related to their child’s symptoms, while also affirming their dedication and efforts. Incorporating a fictional case example into the parent modules—featuring a caregiver with similar experiences—could help normalize these emotions and foster a sense of being understood. Therapists should also address such feelings directly in their written feedback, reassuring parents that their contributions are meaningful and valued. A blended care model, or an initial face-to-face session, may further strengthen parents’ sense of support and enhance treatment engagement. In addition, while our qualitative approach offers deep insights into parents’ lived experiences, complementary quantitative research is needed. Future studies should explore changes in illness perceptions, parenting competences, and family dynamics over time, as well as the long-term effects of ICBT participation.
Conclusion
This qualitative study provides insights into how parents experience caring for a child with FAPDs and their experiences participating in therapist-supported ICBT. The findings deepen our understanding of how parents’ interpret functional symptoms, their beliefs about underlying causes, and how these perspectives evolve through treatment. Additionally, the study highlights how parents can acquire new skills to better manage their child’s symptoms.
Despite the challenges parents faced when navigating multiple roles before, during, and after ICBT, they remained highly confident in the program and did not express feeling overburdened by responsibility. While ICBT requires parents to develop multiple roles, potentially stirring up guilt and self-blame, it also provides tools to fulfill these roles and a structured framework that alleviates frustration and transforms chaos into order. This support empowered parents to fulfill their caregiving roles more effectively, alleviating the feeling of shouldering the responsibility alone.
Footnotes
Acknowledgements
We want to thank all parents who willingly participated and generously shared their experiences. The study was preregistered at Open Science Framework (OSF: ![]() ). The manuscript was edited for proper English language, grammar, punctuation, spelling and overall style by a professional language editing service ( Vidkom).
). The manuscript was edited for proper English language, grammar, punctuation, spelling and overall style by a professional language editing service ( Vidkom).
Ethical considerations
The study was conducted according to the Helsinki Declaration and the Danish Code of Conduct for Research Integrity. It was registered as a part of “The Danish FGID Treatment Study” at the Central Denmark Region’s records of research projects (Sequential number: 769029, Case citation: 1-16-02-101-22). The study was further registered as a part of “The Danish FGID Treatment Study” (Registration number 1-10-72-80-22) at the Danish Health Research Ethics Committee. Following Danish legislation, they declared that it did not need separate approval (request with journal no. 1-10-72-6-24).
Consent to participate
All participants received written and verbal information about the study before providing written and verbal consent for participating.
Consent for publication
Consent for publication is not applicable to this article as it does not contain any identifiable data.
Author contributions
Conceptualization: LAPD, SL, ESN, KHK, and CUR. Methodology: LAPD, SL, and CUR. Writing – Original draft preparation: LAPD. Writing – Review and Editing: LAPD, SL, HSS, KHK, ESN, MB, ML, and CUR. Supervision: SL and CUR. Project administration: LAPD, KHK, ESN, and CUR. Funding Acquisition: LAPD and CUR. All authors have read and agreed on the published version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Lundbeck Foundation [Grant number R432-2023-94]; The Central Region Denmark, Psychiatry Research Foundation [No grant number]; Mrs. C. Hermansen’s memorial fund [No grant number]. Associate Professor Maria Lalouni was supported by the Kamprad Family Foundation [Grant number 20223238]. The funding sources did not affect the study design, collection, analysis, or interpretation of data, neither in the report’s writing nor the decision to submit the article for publication.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
To protect the participants’ anonymity, the interview transcripts for this qualitative study are not freely available.
