Abstract
Perceived birth trauma can disrupt parent-infant bonding and affect family dynamics. This study examined the impact of perceived birth trauma on maternal and paternal attachment using path analysis. An analytical cross-sectional study was conducted with 134 mother-father pairs in Turkey, 6 months postpartum, following planned cesarean sections. Data were collected using the Traumatic Childbirth Perception Scale, Mother-to-Infant Bonding Scale, and Paternal-Infant Attachment Scale. Descriptive statistics and reliability analyses were conducted using R software. Path analysis was performed with the R package “lavaan” to assess direct and indirect relationships. Higher perceived birth trauma was significantly associated with increased maternal bonding difficulties and decreased paternal bonding. A significant negative covariance between maternal and paternal bonding scores indicated interdependent bonding dynamics. The model explained 6% of the variance in maternal bonding and 3.7% in paternal bonding. These findings underscore the need for family-centered, trauma-informed postpartum care to support healthy parent-infant attachment.
Keywords
Introduction
Pregnancy and childbirth are transformative life experiences, often celebrated as milestones. However, these processes can also bring significant physiological and psychological challenges, sometimes leading to postpartum mood disorders. Research indicates that 20%–48% of women perceive childbirth as a traumatic experience (Simpson and Catling, 2016). This perception of birth trauma has been linked to the development of birth-related posttraumatic stress disorder (PTSD), a chronic mental health condition characterized by persistent re-experiencing of the traumatic event, avoidance of related memories, emotional numbing, and hyperarousal (American Psychiatric Association, 2013). Recent meta-analyses reveal that approximately 4.7% of mothers experience birth-related PTSD (Heyne et al., 2022). Such psychological challenges can profoundly affect maternal mental health, significantly influencing early parenthood experiences. One of the most critical consequences of birth trauma is its potential impact on parent–infant attachment. However, attachment is a complex and multifaceted process shaped not only by birth-related experiences but also by various psychological, social, environmental, and infant-related factors (Döblin et al., 2023; Golubitsky et al., 2024; Provasi, 2019; Scism and Cobb, 2017; Seefeld et al., 2023). Maternal mental health conditions such as postpartum depression, anxiety, and symptoms of post-traumatic stress disorder can adversely affect maternal–infant bonding (Song et al., 2017). Paternal attachment, on the other hand, may be influenced by maternal psychological distress, fathers’ perceived role in caregiving, and their level of involvement in infant care (Scism and Cobb, 2017). Infant characteristics such as prematurity, low birth weight, prolonged hospitalization, or difficult temperament may also pose challenges to the development of secure attachment (Provasi, 2019). Moreover, the presence of social support and the quality of the parental relationship are key determinants in shaping early attachment dynamics (Wells et al., 2024).
Cesarean sections may negatively impact maternal-infant bonding due to delayed skin-to-skin contact, increased postpartum pain, and feelings of detachment (Cetisli et al., 2018). Unlike vaginal birth, C-section often involves separation due to medical procedures, potentially disrupting early bonding. Additionally, post-surgical discomfort and reduced mobility may further hinder maternal responsiveness (van Reenen and van Rensburg, 2013). While some studies report no significant association between mode of delivery and parent-infant bonding (Figueiredo et al., 2009; Selcuki et al., 2022), others link C-section to weaker bonding (Cetisli et al., 2018; Song et al., 2017; Zanardo et al., 2016). Women undergoing planned cesarean sections may experience a sense of loss of control, fear regarding their own or their baby’s well-being, or disappointment if the surgical birth deviates from their expectations (Blüml et al., 2012). Unlike emergency cesarean sections, which are typically marked by urgency and limited emotional processing (Ma et al., 2025), planned procedures allow for anticipatory reflection, which may heighten emotional responses before and after birth (Blüml et al., 2012). These psychological responses, even in the absence of acute complications, may pose a risk to maternal mental health and interfere with the development of secure attachment during the early postpartum period (Sharma et al., 2018). Importantly, these dynamics may also influence paternal attachment. Recent studies suggest that fathers’ bonding with their infants after cesarean sections—both planned and unplanned—may be shaped by their partner’s emotional state, the degree of early involvement in infant care, and the psychological processing of the birth experience (Döblin et al., 2023; Fägerskiöld, 2008; Nishimura et al., 2023). These findings highlight the importance of viewing parent–infant attachment as a relational and systemic process, rather than one limited to maternal factors alone.
When attachment is weak or insecure, it can lead to long-term emotional and developmental challenges for both parents and infants. Research has shown that infants who experience poor attachment are at greater risk for behavioral problems, emotional dysregulation, and difficulties in forming relationships later in life (Cook et al., 2018). Additionally, low maternal attachment has been associated with an increased likelihood of postpartum depression and decreased maternal sensitivity to infant cues, further exacerbating difficulties in caregiving (Song et al., 2017). Similarly, fathers who struggle with attachment may feel disengaged or inadequate in their parental role, impacting overall family dynamics (Seefeld et al., 2023). For newborns, insecure attachment can disrupt early emotional regulation and stress response mechanisms, increasing the risk of feeding and sleeping difficulties, excessive crying, and reduced social engagement (Feldman, 2017). Infants who do not experience consistent and responsive caregiving may also show altered cortisol levels, which can affect their physiological stress adaptation and overall neurodevelopment (Gunnar and Quevedo, 2007). These consequences highlight the importance of addressing attachment-related challenges early to promote healthy parent-infant relationships and foster optimal newborn development.
Recognizing the centrality of secure attachment for both infants and parents, it is crucial to explore further the specific factors that may disrupt this process, among which birth-related trauma has received increasing scholarly attention. Although some studies have identified a clear link between birth trauma and impaired attachment (Döblin et al., 2023; Nystedt and Hildingsson, 2018), the relationship is not universally consistent. Some research suggests that despite experiencing birth-related trauma, certain mothers maintain secure attachment to their infants, especially when supported by protective factors such as high-quality postpartum care, strong social support networks, and effective coping mechanisms (Chen et al., 2024; Shorey and Wong, 2022). Furthermore, recent prospective findings indicate that the impact of childbirth-related posttraumatic stress disorder (CB-PTSD) on parent-infant bonding may be shaped by concurrent psychological distress, particularly in mothers. For instance, maternal psychological distress at 1 month postpartum was found to mediate the relationship between CB-PTSD symptoms and mother-infant bonding at 3 months, while no such associations were observed for fathers (Stuijfzand et al., 2020). These results underscore the nuanced nature of trauma and bonding, suggesting that the presence of CB-PTSD symptoms alone does not inevitably lead to impaired bonding, but rather interacts with other psychological and contextual factors to influence outcomes.
To better conceptualize these varied outcomes and underlying mechanisms, it is essential to consider them within a robust theoretical framework such as Attachment Theory. Attachment Theory, introduced by John Bowlby, serves as a critical framework for understanding how maternal perceived birth trauma affects parent-infant relationships. Secure attachment, which is essential for a child’s cognitive, emotional, and social development, depends on sensitive and responsive caregiver interactions (Bowlby, 1973). Maternal birth trauma can disrupt this process, as PTSD symptoms—such as avoidance, emotional numbing, and hyperarousal—may impair a mother’s ability to engage emotionally and responsively with her infant (Cook et al., 2018). This disruption can hinder the development of secure attachment, leaving infants vulnerable to long-term cognitive and emotional challenges (Döblin et al., 2023; Seefeld et al., 2023). While much of the focus has been on mothers, fathers may also be indirectly affected by maternal birth trauma. The emotional and psychological struggles stemming from their partner’s trauma can impact their own ability to bond with the infant. Fathers may experience anxiety, detachment, or feelings of inadequacy, which negatively influence the father-infant relationship (Etheridge and Slade, 2017).
To explore these dynamics, this study utilizes path analysis to examine the relationships between maternal perceived birth trauma, maternal attachment, and paternal attachment. Path analysis provides a statistical framework to evaluate how maternal trauma perceptions directly influence attachment processes for both parents and identifies the interconnectedness of family relationships. This approach highlights the significant influence of maternal psychological experiences on family dynamics and attachment patterns. By focusing on planned C-sections, the study emphasizes a unique context where the psychological impacts of birth trauma may differ from other delivery modes, shedding light on underexplored aspects of parental attachment. Through this framework, the research seeks to understand the psychological and relational consequences of maternal perceived birth trauma and underscores the importance of comprehensive postpartum mental health support for both parents.
Purpose of the study and hypotheses
The purpose of this study was to use path analysis to examine the impact of perceived birth trauma on maternal and paternal attachment within a psychological and relational framework.
Hypotheses
Methods
Design
An analytical cross-sectional study, reported in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist, was conducted to examine the effect of birth trauma on maternal and paternal attachment in the postpartum period using path analysis.
Settings and participants
The study was conducted in a public university hospital in the Central Anatolia region of Turkey. All births included in the study occurred in this hospital, which provides secondary- and tertiary-level obstetric care under the national health system. The sample was formed using convenience sampling from women who gave birth in the obstetrics and gynecology unit of the hospital between January 2023 and May 2024. Inclusion criteria: Mothers aged 18 and older, in their sixth postpartum month, who had a planned cesarean section, have a live singleton baby, can speak and understand Turkish, are literate, and have voluntarily agreed to participate in the study. “Planned cesarean section” in this context refers to non-emergency procedures that may have been medically indicated (e.g. breech presentation, previous cesarean sections, maternal request) but were not associated with high-risk pregnancy conditions. Inclusion criteria for fathers: Fathers who are willing to participate in the study voluntarily, can speak and understand Turkish, and are literate. Exclusion criteria included women with medically diagnosed high-risk pregnancies (e.g. preeclampsia, gestational diabetes, placenta previa, or multiple pregnancy), as well as mothers or fathers with a known psychiatric diagnosis, recent trauma or bereavement, substance or behavioral addiction, use of assisted reproductive technologies (ART), serious physical or cognitive impairments, or unwillingness to participate. ART-conceived pregnancies were excluded because they are clinically associated with increased risk for obstetric and neonatal complications, even when singleton and non-complicated, and often require special monitoring. This exclusion aimed to ensure a low-risk sample and reduce confounding effects on psychological outcomes related to perceived birth trauma and parent–infant attachment. These criteria were defined to reduce potential influences on psychological well-being and parent–infant attachment. The study utilized multiple regression analysis with one predictor; the sample size was 89, with a medium effect size (0.15), a power level of 95%, and a significance level of 0.05. A total of 154 mother-father pairs were evaluated for eligibility; 15 pairs did not volunteer to participate, and 5 mothers were illiterate. The study was completed with 134 mother-father pairs. Based on the post hoc power analysis conducted at the end of the study, the research achieved a 99% power level.
Measures
The study instruments included a Semi-Structural Sociodemographic Information, Traumatic Childbirth Perception Scale, Mother-to Infant Bonding Scale, and Paternal-Infant Attachment Scale.
Semi-structural sociodemographic information
This form, which was prepared by researchers using the literature (Alaçam, 2019; Chabbert et al., 2021; Dekel et al., 2017; Işik and Egeli̇oğlu Ceti̇şli̇, 2020; Karakoç et al., 2022). The form includes questions about the mother’s age, father’s age, number of pregnancies, number of births, mother’s education level, father’s education level, mother’s employment status, father’s employment status, and their perception of income status.
Traumatic Childbirth Perception Scale (TCPS)
Developed by Yalnız et al. in 2016, this 11-point Likert-type scale measures a single dimension (Yalnız et al., 2016). Each item is rated on a scale from 0 to 10. The total score ranges from 0 to 130, with the following interpretations: 0–26 indicates a very low perception of traumatic birth, 27–52 indicates a low perception, 53–78 indicates a moderate perception, 79–104 indicates a high perception, and 105–130 indicates a very high perception of traumatic birth. The scale has demonstrated strong internal consistency, with a Cronbach’s alpha coefficient of 0.89. In our study, the Cronbach’s alpha coefficient was calculated as 0.93.
Mother-to Infant Bonding Scale (MIBS)
The Mother-to-Infant Bonding Scale was developed by Taylor et al. in 2005 (Taylor et al., 2005). The Turkish validity and reliability study was conducted by Karakulak and Alparslan in 2016 (Karakulak and Alparslan, 2016). This scale allows mothers to express their feelings toward their baby with a single word and can be administered from the first day postpartum. The scale consists of 8 items using a 4-point Likert format, scored from 0 to 3. The total score ranges from 0 to 24 (Karakulak and Alparslan, 2016). Higher scores indicate greater challenges in mother-to-infant bonding. In the study conducted by Karakulak and Alparslan, the Cronbach’s alpha coefficient of the scale was found to be 0.69 on the first day postpartum and 0.68 within 8–12 weeks postpartum. In our study, the Cronbach’s alpha coefficient was calculated as 0.83.
Paternal-Infant Attachment Scale (PIAS)
The scale was developed by Condon in 2008 (Condon et al., 2008), and its Turkish validity and reliability were established by Güleç and Kavlak in 2013 (Güleç and Kavlak, 2013). It comprises 19 items and includes three subdimensions: “patience and tolerance,” “ pleasure in interaction” and “love and pride.” The scale’s total scores range from 19 (minimum) to 95 (maximum). There is no cut-off point of the scale. Higher scores indicate stronger attachment, and the scale is evaluated based on total scores. In the study by Güleç and Kavlak, the Cronbach’s alpha coefficient of the scale was reported as 0.76. In our study, the Cronbach’s alpha coefficient was calculated as 0.77.
Data collection
The purpose of the study was explained to postpartum mother-father pairs staying in the obstetrics unit who met the inclusion criteria. Those who agreed to participate signed an informed consent form, after which their contact information and home addresses were collected. A home visit was scheduled during the sixth month postpartum on a day convenient for both the mother and father.
During the home visit, the parents independently completed all questionnaires. A semi-structured sociodemographic information form was filled out by both the mother and father. Mothers completed the Traumatic Childbirth Perception Scale (TCPS) and the Mother-to-Infant Bonding Scale (MIBS), while fathers completed the Paternal-Infant Attachment Scale (PIAS). Participants finished the data collection tools within 25–35 minutes, and all items were checked to ensure no missing data.
Ethical consideration of research
Ethics approval for this study was obtained from the Human Research Ethics Committee of the University in Ankara (Approval No. E-59394181–604.01.02-33844). Additionally, institutional approval was granted by the hospital’s The study adhered to the Declaration of Helsinki and relevant guidelines and regulations. Written informed consent was obtained from each participant after they were informed about the study’s risks and benefits. Participants were free to withdraw from the study at any time without providing an explanation. All data were stored securely and treated confidentially, with access restricted to the research team.
Data analyses
Data analyses were conducted using R software. Descriptive statistics (mean, standard deviation, range, frequency, and percentage) were used to describe the study sample and main variables. The internal consistency reliabilities of the instruments were assessed. Path analysis was performed to examine the model and hypotheses. This method allows for estimating both the magnitude and significance of causal relationships (Crossman, 2019). The structural equation modeling (SEM) approach was employed to develop the model, and path analysis was conducted using the R package “lavaan” (Rosseel et al., 2019). Visualizations of the model and its relationships were generated using the R package “lavaanPlot” (Lishinski, 2021).
Results
A total of 134 participants were included in the study. The mean age of participants was 30.55 ± 4.15 years, while the mean age of fathers was 32.84 ± 4.61 years. Participants had an average of 1.90 ± 1.08 pregnancies and 1.49 ± 0.65 births. In terms of educational attainment, 65.7% of participants had a university degree, 11.2% had postgraduate education, 14.2% completed high school, and 9% had primary or secondary education. Employment status showed that 46.3% of participants were employed, while 53.7% were unemployed. For the fathers’ education, 56% held a university degree, 30.6% completed high school, 9% had primary or secondary education, and 4.5% had postgraduate qualifications. Most fathers (98.5%) were employed, with only 1.5% unemployed. Regarding income status, 28.4% of participants reported that their income was less than their expenses, 53.7% said their income was equal to their expenses, and 17.9% stated that their income exceeded their expenses (Table 1).
Distribution of participants’ sociodemographic characteristics (n = 134).
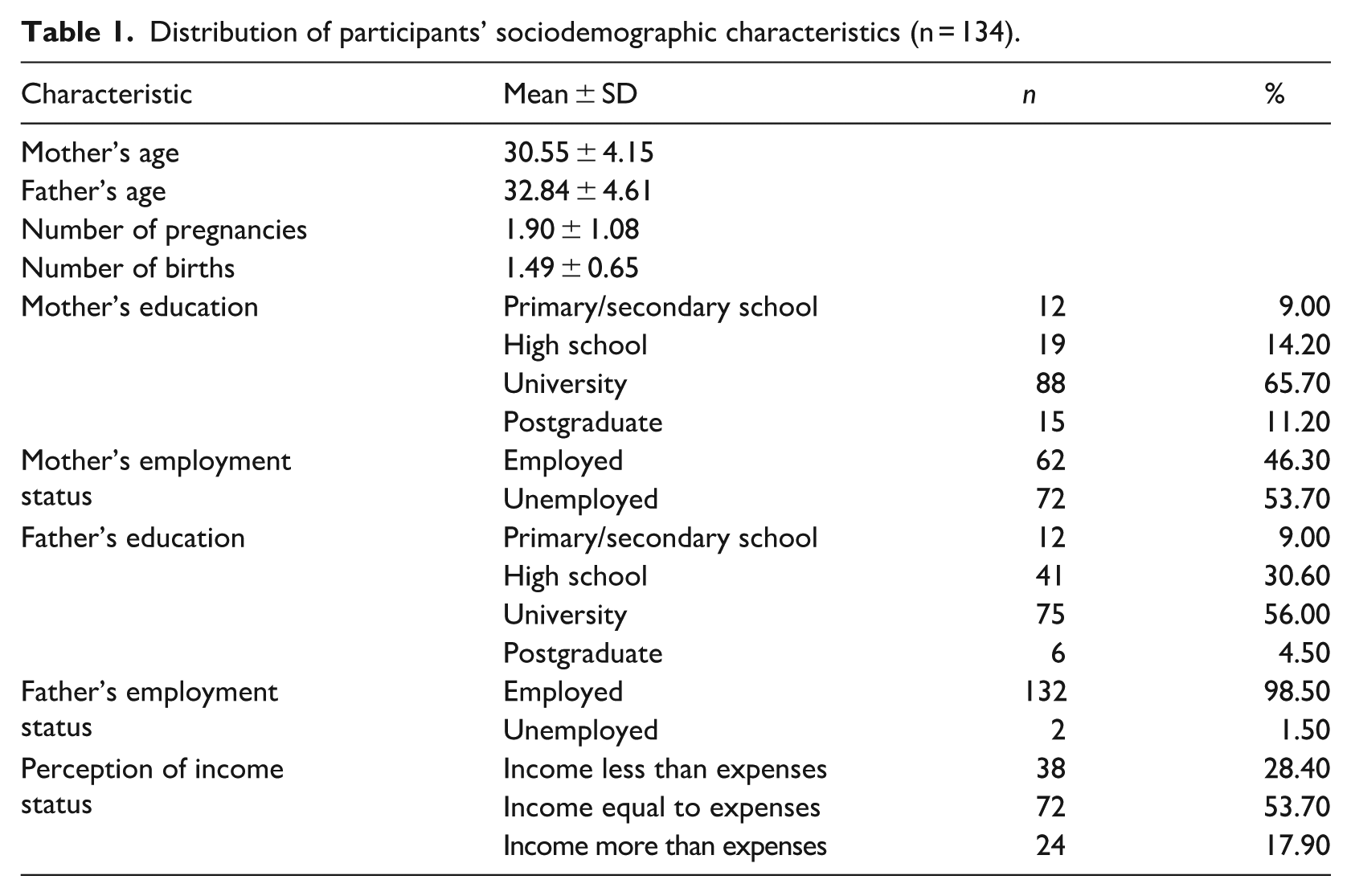
Table 2 provides the descriptive statistics and reliability coefficients for the study variables. The mean score for the PIAS was 83.78 ± 6.07, with skewness (−0.682) and kurtosis (0.052) values indicating normal distribution. The Cronbach’s alpha coefficient for the PIAS scale was 0.77, reflecting acceptable internal consistency. The MIBS had a mean score of 0.69 ± 1.18, with skewness (1.673) and kurtosis (1.937) values suggesting a slightly skewed distribution. The Cronbach’s alpha for the MIBS scale was 0.83, indicating good internal consistency. The TCPS had a mean score of 53.37 ± 29.82, with skewness (0.531) and kurtosis (−0.808) values demonstrating normal distribution. The Cronbach’s alpha coefficient for the TCPS scale was 0.93, indicating excellent internal consistency. Given the total score range of 0–130, the mean TCPS score of 53.37 corresponds to a moderate level of perceived traumatic childbirth. According to the scale’s interpretation thresholds, scores between 53 and 78 indicate moderate trauma perception, while scores of 79 and above reflect high or very high levels of perceived trauma.
Descriptive statistics of the study variables.

PIAS: Paternal-Infant Attachment Scale; MIBS: Traumatic Childbirth Perception Scale; TCPS: Traumatic Childbirth Perception Scale; M: mean; SD: standard deviation; Sk: skewness; Kt: kurtosis; α: Cronbach’s alpha.
Table 3 presents the path analysis results for the effect of Perception of Traumatic Birth (TCPS) on Mother-Baby Bonding (MIBS) and Father-Baby Bonding (PIAS). The model included one predictor variable (TCPS) and two outcome variables (MIBS and PIAS). In addition, the model tested the covariance between MIBS and PIAS to evaluate the interdependence of maternal and paternal bonding experiences. The path analysis diagram for the relational structure is shown in Figure 1. According to the fit indices calculated from the path analysis (χ² = 0.000, df = 0, CFI = 1, GFI = 1, AGFI = 1, RMSEA = 0.000), the model created is well-saturated and demonstrates excellent fit. The regression analysis revealed that perceived traumatic birth (TCPS) had a significant positive effect on mother-to-infant bonding (MIBS) scores (B = 0.010, SE = 0.003, z = 3.112, p = 0.002), indicating that higher TCPS scores are associated with greater challenges in mother-to-infant bonding. In contrast, TCPS had a significant negative effect on father-to-infant bonding (PIAS) scores (B = −0.039, SE = 0.017, z = −2.333, p = 0.020), suggesting that increased TCPS perception is linked to weaker father-to-infant bonding. Additionally, a significant negative covariance was found between MIBS and PIAS (B = −2.948, SE = 0.888, z = −3.320, p = 0.001), indicating an inverse relationship between the bonding experiences of mothers and fathers. The model explained 6% of the variance in MIBS (R² = 0.060) and 3.7% of the variance in PIAS (R² = 0.037). These findings highlight the complex and interdependent dynamics of parental bonding in the context of perceived birth trauma.
Path analysis for the effect of perceived birth trauma on maternal and paternal attachment.
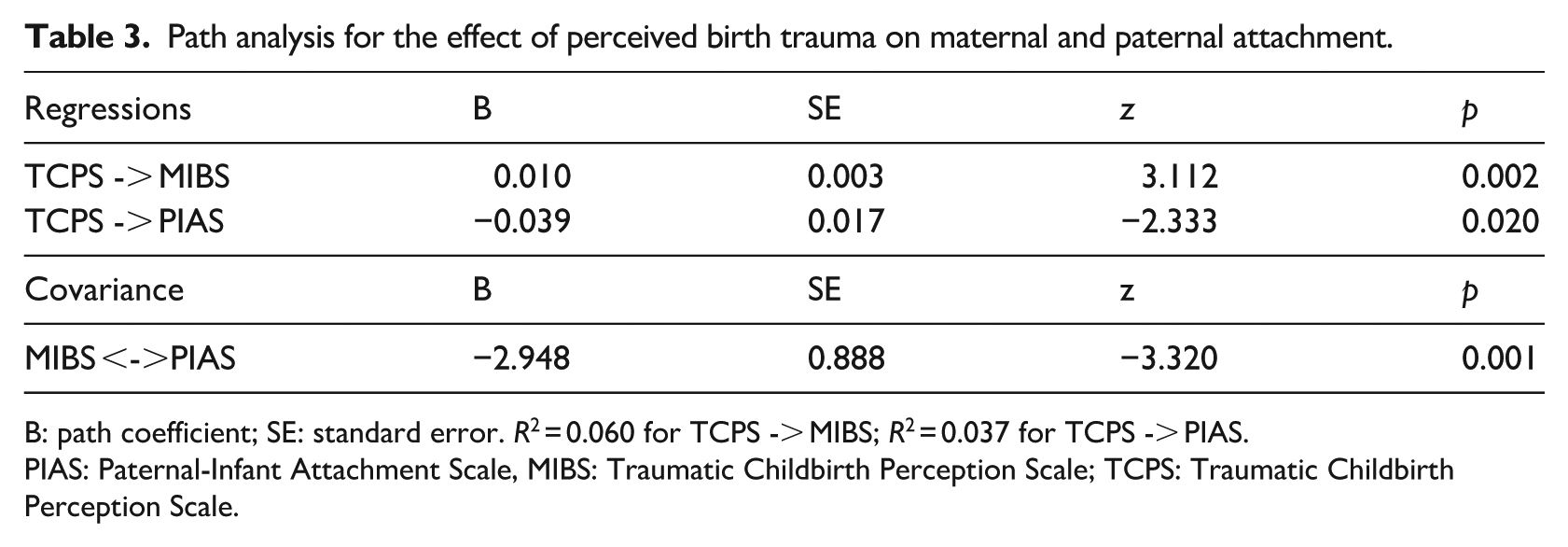
B: path coefficient; SE: standard error. R2 = 0.060 for TCPS -> MIBS; R2 = 0.037 for TCPS -> PIAS.
PIAS: Paternal-Infant Attachment Scale, MIBS: Traumatic Childbirth Perception Scale; TCPS: Traumatic Childbirth Perception Scale.
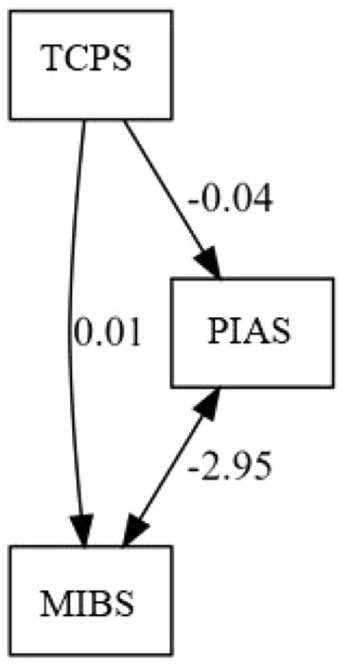
The effect of perceived birth trauma in women with planned cesarean section on maternal and paternal attachment: path analysis model.
Discussion
This study examined the effect of perceived birth trauma in planned cesarean sections on both maternal and paternal attachment using a path analysis model. The results underline the complex, interactive process of parental bonding and point to how maternal psychological experiences are at the core of shaping the relationships between the parents and the infant. The findings also showed low levels of maternal bonding difficulties and high levels of paternal attachment on average, as reflected by MIBS and PIAS scores, respectively.
This study showed a moderate level of perceived traumatic childbirth, with a mean TCPS score of 53.37 ± 29.82, consistent with the defined range for moderate perceptions of trauma (53–78). This finding is consistent with prior research that highlights moderate to high levels of perceived traumatic birth experiences among women (Altuntuğ et al., 2024; Şahin and Erbil, 2024; Yalnız et al., 2016; Yalnız Dilcen et al., 2021). The multifaceted nature of perceived traumatic childbirth is influenced by various variables. Factors such as expectations about childbirth, previous traumatic experiences, insufficient support during delivery, and a lack of effective communication with healthcare providers play critical roles in shaping these perceptions (Aksu and Serçekuş, 2023). Recent research highlights that women’s perceptions of childbirth as traumatic or empowering are shaped not only by individual psychological preparedness but also by broader factors such as cultural identity, bodily autonomy, and access to culturally affirming care (Aksu and Serçekuş, 2023; Kuipers et al., 2024; Lawrie et al., 2024). Given the moderate scores observed in this study, it is evident that even in planned cesarean sections, where perceived control and predictability are often assumed, women are still vulnerable to experiencing childbirth as traumatic. This emphasizes the necessity for healthcare systems to adopt more patient-centered approaches, fostering supportive environments that address both physical and emotional well-being. Future studies could further explore the interplay of individual, societal, and healthcare-related factors in shaping perceptions of traumatic childbirth, contributing to the development of targeted interventions.
Our study revealed a significant positive association between perceived birth trauma and challenges in mother-to-infant bonding. These findings highlight the profound impact that perceived traumatic childbirth can have on a woman’s psychological well-being and her ability to form a secure and responsive bond with her infant. This underscores the interconnected nature of childbirth experiences and early parent-infant relationships. Similarly, Karakoç et al. (2022) emphasized the psychological dimensions of childbirth experiences by examining the relationship between mothers’ birth memories and their attachment styles. The research identified a moderate positive correlation between insecure attachment styles and negative birth memories, particularly in aspects such as memory centrality, coherence, sensory memory, and recall (Karakoç et al., 2022). Women who perceive their childbirth as traumatic or recall it negatively may experience heightened feelings of distress and inadequacy, further hindering their ability to engage emotionally and responsively with their infant.
The findings of Döblin et al. (2023) highlight that all modes of delivery, including planned and unplanned cesarean sections, were associated with more negative birth experiences compared to spontaneous vaginal delivery. However, mothers who delivered via cesarean sections reported stronger parent-infant bonding at both 8 weeks and 14 months postpartum (Döblin et al., 2023). In our study, maternal-infant bonding was assessed at 6 months postpartum, providing a mid-point perspective between the early (8 weeks) and later (14 months) assessments in Döblin et al.’s research. While Döblin et al. found birth experiences to mediate the relationship between all modes of delivery and bonding, our study focuses specifically on planned cesarean sections and demonstrates that perceptions of trauma can persist and continue to affect bonding outcomes at 6 months postpartum. This highlights the critical need to address the psychological impacts of childbirth through supportive interventions that help mothers process their experiences and foster secure maternal-infant bonds.
This interplay between maternal perceptions of traumatic childbirth and bonding dynamics extends beyond the mother-infant relationship, influencing the emotional and psychological well-being of fathers and their ability to bond with the infant. Our study found a significant negative association between maternal perceptions of traumatic childbirth and father-to-infant bonding. Although fathers are often viewed as secondary stakeholders in the childbirth process, their emotional and psychological well-being can be profoundly impacted by their partner’s traumatic experiences (Etheridge and Slade, 2017). When fathers perceive their partner’s distress, they may experience heightened anxiety, helplessness, or emotional detachment, which can diminish their ability to form a secure and responsive bond with their infant. Recent findings by Golubitsky et al. (2024) further underscore the vulnerability of fathers in the context of childbirth. Approximately 6% of fathers in their study reported symptoms consistent with probable PTSD in the first year postpartum, and negative cognitions mediated the association between an emergency cesarean section and paternal PTSD. Moreover, fear of childbirth was found to be related to emergency cesarean sections and insufficient information provided by the medical team (Golubitsky et al., 2024). These results align with our findings by emphasizing that the psychological impacts of childbirth also affect fathers and that the birth experience can profoundly influence paternal outcomes. Taken together, this evidence underscores the need to consider the family unit as a whole when addressing the psychological impacts of childbirth trauma. Both mothers and fathers require adequate emotional support and resources to process their experiences, adapt to their new roles, and establish strong bonds with their infants. Encouraging active paternal involvement during childbirth and the postpartum period, ensuring clear and consistent communication from healthcare professionals, and offering psychological counseling when needed may collectively mitigate the negative effects of maternal trauma on paternal bonding. Such a family-centered approach has the potential to foster healthier parent-infant relationships and promote long-term well-being for all family members.
Our findings reveal a significant negative covariance between maternal and paternal bonding scores, highlighting the interdependence of family dynamics in parent-infant attachment. Higher scores on the Mother-to-Infant Bonding Scale (MIBS) indicate greater maternal bonding challenges, while higher Paternal-Infant Attachment Scale (PIAS) scores reflect stronger paternal bonding. As maternal bonding difficulties rise, paternal bonding often decreases, suggesting that one parent’s emotional state can influence the other’s bonding capacity. Seefeld et al. (2023) further show that a parent’s negative birth experience weakens their own bond with the child 14 months postpartum, with a stronger impact on partners than mothers, mediated by postpartum psychiatric symptoms. However, one parent’s experience does not significantly affect the other parent’s long-term bond (Seefeld et al., 2023).
These findings underscore the importance of a holistic, family-centered approach to postpartum care, addressing each parent’s emotional needs and fostering supportive interventions to promote secure parent-child attachments. This study highlights that perceived birth trauma can significantly influence both maternal and paternal attachment. Even in planned cesarean sections, where a sense of control may be presumed, parents remain susceptible to psychological distress that can undermine their ability to bond with their infants. Recognizing the interplay of maternal and paternal experiences emphasizes the importance of a holistic, family-centered approach to postpartum care. Healthcare professionals should offer emotional support, clear communication, and interventions tailored to the individual needs of both mothers and fathers. By helping parents process their birth experiences and adjust to their new roles, such strategies ultimately foster secure, responsive parent-infant bonds and promote healthier long-term family dynamics.
Limitations and future research
This study has several limitations that should be addressed in future research. The sample was limited to a single state hospital in Turkey, which may restrict the generalizability of the findings to other cultural and healthcare contexts. Additionally, the cross-sectional design does not allow for causal inferences or the examination of changes in attachment over time. Future studies should consider longitudinal designs to explore the long-term impacts of perceived birth trauma on parent-infant relationships. Furthermore, while the study focused on planned cesarean sections, comparative studies involving different modes of delivery, including emergency cesarean sections and vaginal births, could provide a broader understanding of how delivery experiences influence parental bonding. Finally, although the study does not evaluate the structural causes or policy implications of cesarean section rates in Turkey, we acknowledge that high national cesarean section prevalence reflects systemic, cultural, and institutional dynamics that may shape birth perceptions and parental experiences. Future research should consider integrating qualitative or policy-oriented approaches to better understand the broader sociocultural and institutional factors influencing planned cesarean sections and their psychological outcomes. As the study aimed to examine maternal perceived trauma related to the most recent planned cesarean birth, variables such as the number of previous cesarean sections were not included in the model. Future research may consider incorporating this and other obstetric history variables to provide a more comprehensive perspective on factors influencing psychological responses and parental attachment.
Conclusion
This study offers valuable insights into the psychological and relational consequences of perceived birth trauma within the context of planned cesarean sections. While the study does not evaluate health system performance directly, the findings underscore the importance of maternal psychological well-being and a supportive family environment in shaping early parent–infant relationships. The results point to a critical need for the development and implementation of more family-centered, trauma-informed approaches in postpartum care, especially in healthcare contexts where such practices are currently limited or inconsistently applied. Implementing such strategies has the potential to enhance parental attachment, improve outcomes for both parents and infants, and ultimately foster healthier long-term family dynamics.
Footnotes
Acknowledgements
We would like to thank all the mothers and fathers for their cooperation and contribution to this study.
Ethical consideration
Official permissions for this study were obtained from the Human Research Ethics Committee of the University in Ankara (No. E-59394181–604.01.02-33844), and institutional approval was granted by the hospital’s board.
Consent to participate
All participants provided informed consent prior to their inclusion in the study.
Consent for publication
Participants consented to the publication of anonymized data.
Author contributions
Merve Mert-Karadas: Conceptualization; Data curation; Formal analysis; Investigation; Methodology; Project administration; Resources; Supervision; Visualization; Writing—original draft; and Writing —review & editing. Cansu Akdag Topal: Conceptualization; Data curation; Formal analysis; Investigation; Methodology; Supervision; Visualization; Writing—original draft; and Writing—review & editing. Irem Karakurt: Conceptualization; Data curation; Investigation; Methodology; Supervision; Writing—original draft; and Writing—review & editing. Handan Boztepe: Conceptualization; Data curation; Investigation; Methodology; Supervision; Writing—original draft; and Writing—review & editing.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
