Abstract
Pain invalidation (e.g., having pain discounted) is a risk factor for depression among people with chronic pain, but the mechanisms remain unclear. Shame is a common, yet understudied, aspect of the pain experience. This study investigated whether pain-related shame helps explain the relationship between pain discounting and heightened depressive symptoms. The secondary aim was to examine whether social support can protect against the harmful effects of discounting. Patients with chronic pain (N = 305) were recruited from outpatient pain clinics. Participants completed an online cross-sectional survey and data were analyzed using moderated mediation analysis. Greater discounting was associated with greater depressive symptoms, and pain-related shame significantly mediated this relationship. Perceived social support attenuated the relationship between discounting and depressive symptoms. Greater attention towards pain-related shame as a treatment target is needed. Individual- and system-level interventions are required to address pain invalidation and bolster support for this population.
Introduction
Chronic pain affects approximately 25% of Canadian adults (Canadian Pain Task Force, 2020) and is a leading cause of disability worldwide (Vos et al., 2020). An estimated 30–60% of people with chronic pain experience depression. This co-occurrence results in worse health outcomes, compared to those with chronic pain or depression alone (Bair et al., 2003). Chronic pain is considered an invisible illness because it often lacks external markers to indicate the presence of a chronic condition. As such, it is highly contestable and susceptible to social stigma (De Ruddere and Craig, 2016), including invalidating responses (Kool et al., 2010). The overarching goal of the current study was to investigate the relationship between pain invalidation and depressive symptoms in a community-dwelling sample of adults with chronic pain. We examined pain-related shame as a potential mediator in this relationship, and the extent to which a supportive social network may weaken the relationship between pain invalidation and pain-related shame and depressive symptoms.
Invalidation is a common stigmatizing response to chronic pain that is associated with worse health outcomes (Kool et al., 2010). Pain discounting is an especially harmful form of invalidation that denies the legitimacy of a person’s pain (Kool et al., 2010) and can contribute to increased pain severity, loneliness, and depressive symptoms in chronic pain samples (Ghavidel-Parsa et al., 2015; Kool et al., 2010, 2013; Molzof et al., 2020). These findings are consistent with social status theory, which suggests that disruptions in social status due to stigma can lead to negative mental health outcomes (Gruenewald et al., 2007). Findings also align with the minority stress model (Meyer, 2003), which posits that individuals who are socially categorized in marginalized groups, including those with stigmatized chronic illness (Rendina et al., 2017), are at risk of greater stress and consequent worse health outcomes.
Surprisingly limited attention has been given to the mechanisms through which invalidating social encounters are related to health and wellbeing among people with chronic pain. Recent research highlights the need to integrate affective science into studies of mechanisms linking social relationships and health (Sbarra and Coan, 2018). One potential affective mediator that may link the social environment to mental health outcomes is shame. Shame is a painful, self-conscious moral emotion characterized by a global negative evaluation of the self, formulated in response to the perceived or anticipated actions or thoughts of others. Shame often ascribes blame to oneself for a perceived or actual moral failing (Tangney and Tracy, 2011). Studies show that shame is a common emotional response to stigmatizing and de-legitimizing health-related experiences (Bennett et al., 2016; Luoma and Platt, 2015) and is a strong predictor of depression and worse health outcomes across multiple contexts and health conditions (Kim et al., 2011). The theory of self-stigma suggests that negative social judgments lead to worse outcomes through internalization processes that apply stigmatizing social beliefs to oneself (Watson et al., 2007). This is supported by empirical evidence, with a recent study finding that feelings of internalized shame mediated the relationship between pain invalidation and depressive symptoms among university students with current or prior acute, not chronic, pain (Boring et al., 2021).
Research has yet to examine the potential mediating role of shame in the association between invalidation and depressive symptoms among people living with chronic pain. Despite shame consistently emerging as a theme in qualitative studies of the chronic pain experience (Gustafsson et al., 2004; Honkasalo, 2001), very few quantitative studies have examined shame in the context of chronic pain. Two studies have investigated whether shame proneness (i.e., the general tendency to feel shame across various circumstances) is elevated within chronic pain populations compared to normal controls, with conflicting results (Ten Klooster et al., 2014; Turner-Cobb et al., 2015). Notably, this focus on shame proneness fails to capture actual present levels of shame stemming from the pain experience.
Although the social environment can be a source of stress and invalidation for people with persistent pain, ample research highlights the health benefits of positive social relationships. Patients who are satisfied with their social support report less pain interference (Penn et al., 2019), more adaptive coping strategies (Holtzman et al., 2004), lower pain catastrophizing (Cano et al., 2009; Holtzman and DeLongis, 2007), and lower depressive symptoms (McKillop et al., 2017). Within the stress-buffering model of social support, perceptions of support can attenuate harmful effects of stress on health and wellbeing (Cohen and Wills, 1985). Indeed, a survey of patients with rheumatic diseases demonstrated that social support may protect against the mental health harms of invalidation from family members (Kool et al., 2013). Outside the pain literature, studies have found that greater social support can weaken the relationship between perceived stigma and depression (Casale et al., 2019; Rao et al., 2012). More research is needed to clarify the potential buffering effect of social support on chronic pain invalidation and depression, and to identify whether social support protects against pain-related shame.
The current study addressed gaps in the literature regarding the role of pain-related shame and pain invalidation in the experience of depressive symptoms and the potentially protective role of perceived support in this process. Study hypotheses and methods were pre-registered with Open Science Framework (OSF; osf.io/xvpu8). The first aim was to determine whether pain-related discounting is associated with depressive symptoms among patients with chronic pain and to examine pain-related shame as a potential mediator of this relationship.
The second aim was to examine whether perceived availability of support weakens the relationship between pain discounting and pain-related shame and depressive symptoms.
Materials and methods
Participants
Participants were recruited from a network of four outpatient medical clinics in Western Canada specializing in the treatment of chronic pain. Data were collected between November 2020 and March 2021. Eligible participants had chronic pain (i.e., pain for at least 12 weeks), were at least 18 years old, and were fluent in English. There were no exclusion criteria.
Procedure
After providing informed consent, participants completed a cross-sectional survey comprised of demographic and medical questions and standardized, validated psychosocial questionnaires. Participants were given the option to complete a version of the survey online (n = 301) or using paper-and-pencil (n = 4). Upon completion of the survey, participants could enter a draw for one of three $100 CAD Amazon gift cards.
Measures
Outcome variable: Depressive symptoms
The Beck Depression Inventory II (BDI-II) is a 21-item self-report inventory of symptoms of depression (e.g., hopelessness, fatigue, and concentration difficulties; Beck et al., 1996). Items are rated on a scale of 0 (absence of a symptom) to 3 (most severe possible level of a symptom). The BDI-II is widely used and has demonstrated strong psychometric properties across diverse populations (Wang and Gorenstein, 2013). Cronbach’s α was 0.93 in the current study.
Independent variable: Pain invalidation (discounting)
The Illness Invalidation Inventory (3*I) measures perceptions of invalidating social responses to a person’s illness (Kool et al., 2010). It contains two subscales: discounting and lack of understanding. The measure is intended to be applicable across a wide range of medical conditions, but it was developed and validated using chronic pain populations. It is a 40-item measure, with 8 items each identifying illness invalidation from spouses, family, medical professionals, work environment, and social services (participants are instructed to skip subscales that do not apply). Participants rate perceived frequency of invalidating experiences on a Likert scale from 1 (never) to 5 (very often).
The current study used the discounting subscale of the 3*I, which captures perceptions of responses that actively deny or doubt the legitimacy of a person’s pain experience (e.g., “. . . makes me feel like I am an exaggerator” and “. . . thinks I can work more than I do.”). This study focused on the discounting subscale, as it was expected that discounting a person’s pain is an especially shaming form of invalidation, since discounting implies that the problem lies with the person (i.e., the pain is not real) and shame reflects a critical view of the self as flawed or failing (Tangney and Tracy, 2011). Although previous studies have required completion of at least three social source subscales (Cameron et al., 2018) this would have disproportionately excluded unmarried individuals from our sample. Therefore, we created mean scores for participants who reported at least two sources of discounting. Studies show that the 3*I demonstrates good reliability and excellent construct validity (Kool et al., 2014; Molzof et al., 2020). Cronbach’s α was 0.93 for the discounting subscale.
Mediator: Pain-related shame
The Chronic Illness-Related Shame Scale (CISS) is a 7-item self-report measure that captures feelings of shame specifically related to chronic illness (e.g., “I’m ashamed of talking with others about my illness or symptoms,” “I feel inadequate because of my illness and symptoms”; Trindade et al., 2017). For the purposes of this study, wording of items was altered to refer to shame about chronic pain (e.g., “I feel inadequate because of my chronic pain”). Items are rated on a Likert scale from 0 (never true) to 4 (always true). The CISS has shown strong reliability across samples and good convergent validity (Trindade et al., 2017). Cronbach’s α was 0.93 in the current study.
Moderator: Perceived social support
The Multidimensional Scale of Perceived Social Support (MSPSS) is a commonly used measure of perceived social support (Zimet et al., 1988). Participants rate levels of social support from their family, friends, and significant other. Twelve items (four for each support source, e.g., “I get the emotional help and support I need from my family”) are rated on a 7-point Likert scale ranging from 1 (very strongly disagree) to 7 (very strongly agree). The MSPSS has strong psychometric properties (Zimet et al., 1990) and demonstrated a Cronbach’s α of 0.93 in the current study.
Demographic and medical factors
Participants reported their demographics (e.g., age, gender, employment status) and medical situation (e.g., pain condition, cause of pain). Pain severity and gender were considered as potential covariates given past research demonstrating a link with our main study variables (e.g., Mok and Lee, 2008; Munce and Stewart, 2007). Pain severity was assessed using the pain severity subscale of the Brief Pain Inventory—Short Form (BPI-SF) which asks about worst, least, and average levels of pain within the past week, as well as respondents’ current pain, rated from 0 (no pain at all) to 10 (worst pain imaginable). Cronbach’s α was 0.88.
Statistical analysis
The statistical analysis plan was pre-registered with OSF (osf.io/xvpu8). To test Hypotheses 1 and 2, a simple mediation analysis was conducted in SPSS using PROCESS (Model 4; Hayes, 2018) with discounting as the predictor, pain-related shame as the mediator, and depressive symptoms as the outcome. To test Hypotheses 3 and 4, moderated mediation was conducted using PROCESS in SPSS (Model 8; Hayes, 2018). Moderation analysis tested whether the strength of the relationship between discounting and depressive symptoms varied as a function of perceived support (conditional direct effect) and whether the strength of the relationship between discounting and pain-related shame varied as a function of perceived support (conditional indirect effect). To explore potential differences in the effects of invalidation from specific sources, an exploratory set of analyses was run with each of the five sources of invalidation serving as the independent variable. Although the focus of this pre-registered study was on pain discounting, we ran an additional set of exploratory analyses to determine whether results were similar when using the “lack of understanding” subscale of the 3*I (see Supplemental Online Materials).
Results
Sample characteristics
A total of 335 patients responded to the study advertisements, met criteria for inclusion, and provided informed consent. A total of 305 (91%) provided sufficient data to be included in the present analyses. Participants identified as female (74.1%), male (24.9%), and non-binary (1.0%), and the average age was 55.64 (SD = 13.59, range 18–89). Participants were predominantly White (92.8%) and retired (29.8%) or on medical leave/disability (26.2%). The average pain severity was 5.56 (SD = 1.73). Participants attributed their chronic pain to a variety of causes, with 49% of participants selecting multiple causes. Almost two-thirds of the sample attributed their pain to one or more injuries or accidents, including motor vehicle accidents (22.6%), workplace injuries (18.4%), and other accidents/injuries (21.6%; e.g., sports-related injuries). Other causes of pain included (non-malignant) chronic health conditions (e.g., arthritis, fibromyalgia; 31.8%), post-surgical pain (15.1%), cancer-related pain (3.3%), and other causes (e.g., stress, abuse; 8.5%). Almost one-third (30.5%) of respondents indicated that the cause of their pain is unknown.
Descriptive statistics and bivariate correlations
Descriptive statistics and bivariate correlations can be found in Table 1. Discounting responses were reported to be highest from social services (M = 2.62, SD = 1.19), followed by work colleagues (M = 2.50, SD = 1.09), family (M = 2.27, SD = 0.94), spouse (M = 2.25, SD = 0.88), and medical professionals (M = 2.06, SD = 0.89). Correlations between discounting, pain-related shame, depressive symptoms, and perceived social support were all significant (p < .001) and in the expected direction. Pain severity was significantly and positively associated with discounting, pain-related shame, and depressive symptoms, but not perceived social support. Female (versus male) gender was significantly associated with greater levels of pain-related shame. However, because gender was not significantly associated with depressive symptoms at the bivariate level, only pain severity was retained as a covariate.
Means, standard deviations, and bivariate correlations of study variables.
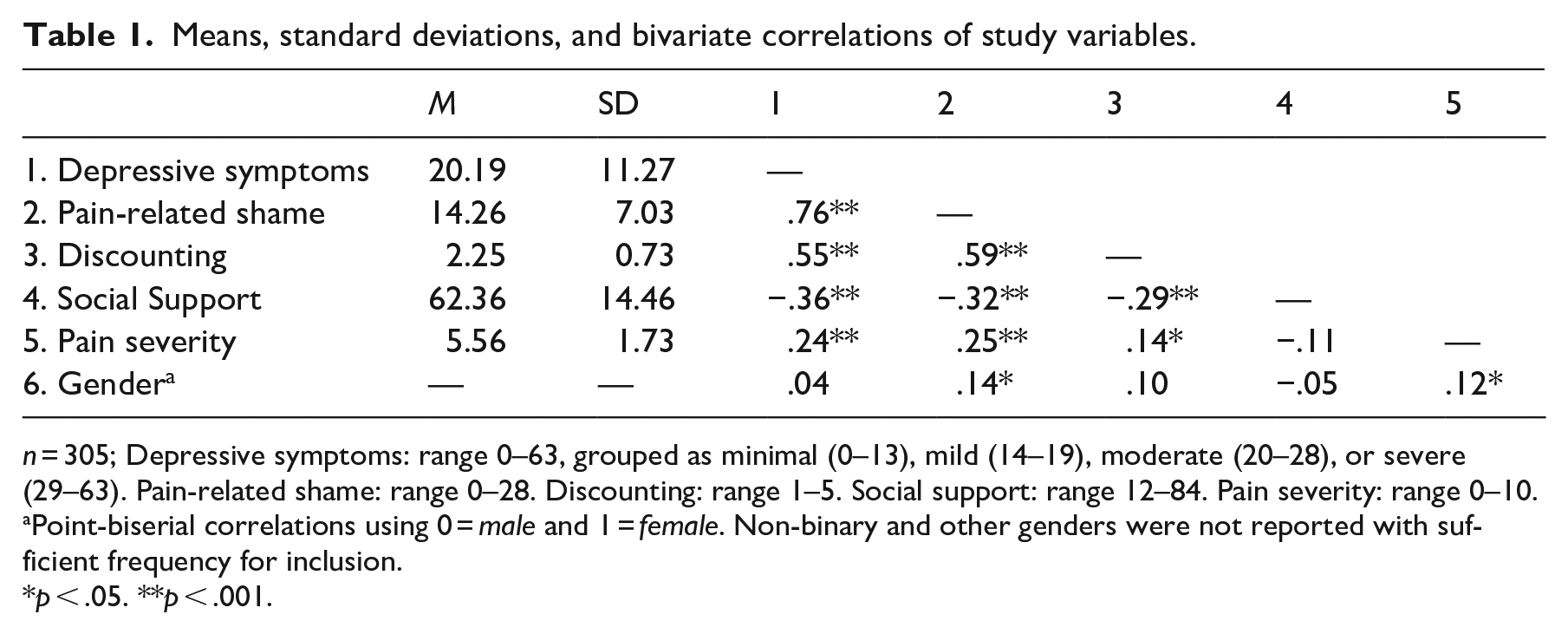
n = 305; Depressive symptoms: range 0–63, grouped as minimal (0–13), mild (14–19), moderate (20–28), or severe (29–63). Pain-related shame: range 0–28. Discounting: range 1–5. Social support: range 12–84. Pain severity: range 0–10.
Point-biserial correlations using 0 =male and 1 =female. Non-binary and other genders were not reported with sufficient frequency for inclusion.
p < .05. **p < .001.
Simple mediation analysis
Consistent with Hypothesis 1, the total effect of discounting on depressive symptoms was significant, β = 0.55, b = 8.43, 95% CI [7.00, 9.86], p < .001. Higher levels of discounting were associated with higher levels of pain-related shame, β = 0.58, b = 5.58, 95% CI [4.72, 6.44], p < .001, which were in turn associated with greater depressive symptoms, β = 0.64, b = 1.03, 95% CI [0.88, 1.17], p < .001. The indirect effect of discounting on depressive symptoms through pain-related shame was significant, β = 0.37, b = 5.73, 95% CI [4.55, 7.03], p < .001, supporting Hypothesis 2. The direct effect of discounting on depressive symptoms remained significant, β = 0.18, b = 2.71, 95% CI [1.31, 4.10], p < .001. The magnitude of the indirect effect was moderate (β = 0.37), while the magnitude of the direct effect was small (β = 0.18), indicating that the impact of discounting on depressive symptoms was larger when indirectly related through pain-related shame.
Moderated mediation analysis
Hypotheses 3 and 4 were tested using a moderated mediation model (see Table 2). A significant moderation of the direct effect of discounting on depressive symptoms was identified, as perceived social support weakened the strength of the relationship between discounting and depressive symptoms, supporting Hypothesis 3. Specifically, at low (−1 SD) and mean levels of social support, higher discounting was significantly related to higher depressive symptoms, b = 3.66, 95% CI [1.96, 5.36], p < .001, and b = 2.22, 95% CI [0.83, 3.62], p = .002, respectively. At high (+1 SD) levels of perceived support, discounting was not significantly associated with depressive symptoms, b = 0.79, 95% CI [−1.10, 2.68], p = .41.
Results of moderated mediation (PROCESS Model 8) examining moderating effects of perceived social support (SS) on relationship of discounting with depressive symptoms and pain-related shame.
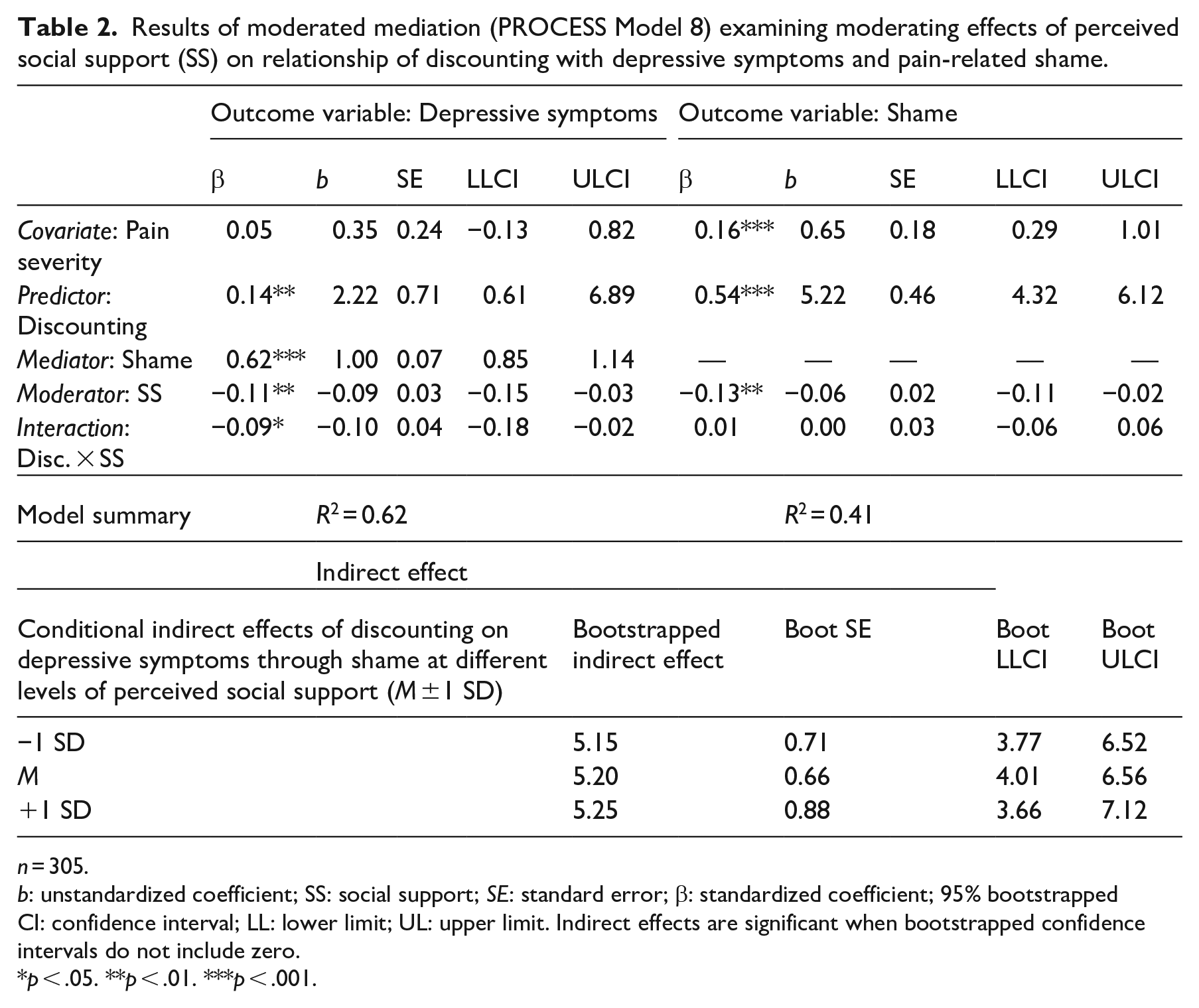
n = 305.
b: unstandardized coefficient; SS: social support; SE: standard error; β: standardized coefficient; 95% bootstrapped CI: confidence interval; LL: lower limit; UL: upper limit. Indirect effects are significant when bootstrapped confidence intervals do not include zero.
p < .05. **p < .01. ***p < .001.
The moderating effect of perceived social support on the association between discounting and pain-related shame was non-significant. Thus, Hypothesis 4 was not supported. However, there was a significant direct association between greater perceived social support and lower pain-related shame.
Supplemental analyses
The current study assessed the relationship between shame specific to the chronic pain experience and global depressive symptoms. However, to ensure that our study findings were not due to measurement overlap between shame and depressive symptoms, analyses were re-run using a modified version of the BDI-II that omitted five items capturing shame-related concerns (failure, guilty feelings, self-dislike, self-criticalness, worthlessness). Pain-related shame remained strongly correlated with scores on the modified BDI-II, r = .71 (vs 0.76), p < .001. The simple mediation analysis and moderated mediation analysis were also re-run with the modified BDI-II scale, and all significant results held (see Supplemental Online Materials; Tables S1 and S2).
We conducted exploratory analyses to test whether the source of discounting (spouse, family, work, medical professionals, and social services) influenced the hypothesized relationships (see Supplemental Online Materials). Results were largely similar to the primary analyses including discounting from all sources combined. We also ran the same analyses using the lack of understanding subscale from the 3*I. Results were similar to the primary model for lack of understanding from all sources combined, as well as specifically from spouses, family, work, and medical professionals (see Supplemental Online Materials).
Discussion
Chronic pain and depression commonly co-occur in the general population (Bair et al., 2003). Findings from the current pre-registered study revealed that perceptions of discounting from others are associated with significantly higher levels of depressive symptoms in a community-based sample of people with chronic pain. Perhaps most notably, this work identified a key pathway through which pain invalidation may contribute to depressive symptoms—pain-related shame. To date, the vast majority of research examining the emotional experience of chronic pain has focused on depression, anxiety, and (sometimes) anger or irritability (Holtzman et al., 2015; Lumley et al., 2011). However, the current research highlights the need for researchers and clinicians to broaden their lens when considering emotional aspects of pain to include moral emotions, such as shame. Findings from this study also contribute to understanding the ways in which supportive social relationships can serve as a protective factor in the context of chronic pain and pain-related invalidation.
The significant association between higher reports of discounting and higher depressive symptoms found in this study adds to a growing body of empirical literature suggesting that perceptions of discounting are directly related to poorer mental health for people with chronic pain (Kool et al., 2010, 2013; Molzof et al., 2020). These findings support social status theory (Gruenewald et al., 2007) and the minority stress model (Meyer, 2003), which give central importance to the impact of negative social judgments on the mental health of stigmatized populations. Perceptions of discounting and pain-related shame were also associated with depressive symptoms over and above the effects of pain severity. In fact, once discounting and shame were accounted for in the mediation model, pain severity was no longer a significant predictor of depressive symptoms. This is in line with past chronic pain research indicating that psychosocial factors are stronger predictors of emotional and physical functioning than pain intensity itself (Sullivan and Ballantyne, 2016).
Results from the current study also support the theory of self-stigma (Watson et al., 2007), indicating that pain-related shame may be an important pathway through which the social stigma of chronic pain is internalized to contribute to depressive symptoms. The magnitude of the indirect effect was substantial (β = 0.37), and our model accounted for an impressive 60% of variance in depressive symptoms. Our findings most closely relate to a recent study that identified shame as a mediator between pain invalidation and depressive symptoms among undergraduate students without chronic pain (Boring et al., 2021). The current study is the first to demonstrate the mediating role of shame in a large sample of people with chronic pain and to do so by measuring shame specifically related to one’s pain condition. Supplementary analyses showed that this study’s findings were not merely due to an overlap in the measurement of shame and depression. Although people with depression commonly experience shame, results held even when depressive symptoms related to shame were removed from the BDI-II, indicating that pain-related shame is strongly and significantly related to the broader cluster of depressive symptoms.
This research further extended previous work by examining the protective role of social support in the context of pain-related invalidation and shame. As hypothesized, perceived social support weakened the relationship between discounting and depressive symptoms, such that the association between discounting and depressive symptoms became nonsignificant at high levels of perceived support. To our knowledge, only one previous study has tested the stress buffering effects of social support specifically for invalidation of chronic pain, with similar results (Kool et al., 2013). More broadly, results add to the extant body of literature demonstrating the stress buffering effects and coping benefits afforded by social support for people with chronic pain (Holtzman et al., 2004; Matos et al., 2017), and the value of social support in protecting against the harms of stigma (Meyer, 2003).
Contrary to study hypotheses, perceived social support did not moderate the association between discounting and pain-related shame. However lower levels of support were directly related to higher levels of pain-related shame. This is consistent with research showing that lower levels of social support are associated with higher levels of negative affect in general (Dour et al., 2013) and that illness-related shame is linked with social withdrawal and diminished quality of social relationships (Trindade et al., 2018). Yet it remains unclear why social support did not specifically protect against the effects of invalidation on pain-related shame in the same way it did for depressive symptoms. Further research is needed to better understand the protective role of social support in the face of shame and various sources of pain invalidation. In sum, the relationship between social support, invalidation, and feelings of shame are complex and further research is needed.
Clinical implications
The current study highlights the vital need to address invalidation of chronic pain at the societal level in order to mitigate psychosocial harms. Education for the public as well as for formal and informal care providers, physicians, employers, and social services on the challenges of invisible illnesses and injurious impacts of invalidation may help to improve understanding of chronic pain and associated challenges. Enhancing validating responses to a person’s pain will likely help improve patient outcomes (Edmond and Keefe, 2015). Additionally, there is some evidence that fostering effective strategies for coping at the individual level, such as improving self-efficacy and pain acceptance, may protect against negative outcomes associated with invalidation (Cameron et al., 2018). Perceived social support emerged in the current study as a protective factor for depressive symptoms related to discounting, adding to existing evidence that enhancing supportive social networks for people with chronic pain can help to ameliorate symptoms of depression (McKillop et al., 2017).
Current evidence-based psychological treatments for chronic pain and comorbid mental health conditions include cognitive behavioral therapy and mindfulness- and acceptance-based interventions (Darnall, 2019). However, the small to medium effect sizes for these treatments suggests that there is significant room for improvement (Ehde et al., 2014; Hughes et al., 2017). Results of the present study indicate that targeting pain-related shame may provide a novel avenue for improving treatment outcomes for those with comorbid chronic pain and depression. As highlighted by intersectionality theory, shame may be a transdiagnostic factor exacerbated by the intersecting stigmatized nature of both chronic pain and depression (Oexle and Corrigan, 2018). Yet shame has received minimal recognition as a treatment target in chronic pain populations (c.f. Gustafsson et al., 2004), despite emerging literature highlighting the importance of shame and other self-conscious moral emotions, such as pain-related guilt (Serbic et al., 2022; Turner-Cobb et al., 2015).
Although shame presents unique challenges in psychotherapy, such as increased likelihood of non-disclosure or cessation of treatment (Dearing and Tangney, 2011), a recent systematic review demonstrated that shame is highly treatable across a range of psychiatric conditions (Goffnett et al., 2020). In fact, 90% of reviewed studies demonstrated significant reductions in shame, and shame was responsive to a wide range of treatment modalities, including acceptance and commitment therapy, cognitive behavioral therapy, and mindfulness-based interventions (Goffnett et al., 2020). None of the interventions in the systematic review addressed chronic illness- or chronic pain-related shame. However, current findings highlight shame as a promising target that could be addressed within the framework of already existing mindfulness- and acceptance-based interventions for chronic pain (Darnall, 2019).
Results from the current study suggest that patients with high levels of social support may be protected against the harmful effects of discounting social responses. This finding is yet another testament to the powerful role of support from family and friends in this population. This study is also the first to demonstrate an association between lower levels of support and higher levels of shame in a chronic pain sample. Health care providers may need to enhance informal supports for those who experience pain-related shame and to consider whether shame may be a barrier to seeking support (Trindade et al., 2018).
Limitations and future directions
There were several limitations to the current study. This study employed a cross-sectional design and there are likely bidirectional relationships between the study variables. For example, higher levels of depressive symptoms may also influence perceptions of support availability and heighten subjective feelings of invalidation (Naushad et al., 2018). Although results from a cross-sectional study cannot be used to draw conclusions about causality (Maxwell and Cole, 2007), findings can inform causal arguments with empirical and theoretical backing (Hayes and Rockwood, 2017). Future research should investigate bidirectionality and the mechanistic role of pain-related shame for people living with chronic pain through daily process and longitudinal research designs that can better isolate and clarify the temporal ordering of study variables.
Participants were predominantly White and living in Western Canada, and thus results may not generalize to other racial or ethnic groups or cultural settings. Cultural differences and context are an important consideration in shame research, as the experience and expression of this social emotion is highly dependent on cultural values and social norms (Honkasalo, 2001; Wong and Tsai, 2007). Further, minority racial and ethnic groups have been shown to have greater undertreatment and underestimation of chronic pain compared to White patients (Paulson et al., 2007). Patients who face multiple forms of stigma (e.g., stigmatized illness and racial prejudice) may be at increased risk of pain-related invalidation and shame, which may in turn differentially impact pain-related health outcomes (Goodin et al., 2018). Indeed, people experiencing stigma and social marginalization are at risk of not receiving adequate healthcare and pain management services (Craig et al., 2020). Future research can expand upon current findings by exploring sociodemographic and cultural factors that predict increased likelihood of pain-related shame and experiences of pain invalidation.
Relatedly, research regarding the role of gender on experiences of invalidation is mixed. Some studies suggest that women may experience more discounting or doubt about the legitimacy of their pain symptoms than men (Werner and Malterud, 2003), while recent research, including the current study, shows that women do not differ from men in reports of invalidation of pain (Kool et al., 2010). However, results suggest that women may be more likely to experience pain-related shame, consistent with previous research (Ludwig et al., 2017). Future studies are needed to investigate factors that may be driving gender-related differences in the experience of invalidation and shame among those living with chronic pain.
This study addressed social support as a potential moderator of the effects of invalidation. Yet invalidation is influenced by numerous factors and varies across chronic pain conditions (Kool et al., 2010). Additional research is needed to understand specific risk and protective factors related to experiences of invalidation. For example, age (Orth et al., 2010), pain diagnosis (Kool et al., 2010), and the extent to which participants’ chronic pain has a medical explanation may all affect the likelihood of invalidation (De Ruddere et al., 2016) and subsequent experiences of pain-related shame and depression. The current sample was highly heterogeneous in terms of the cause(s) of patients’ pain, and future research is needed to investigate whether rates of shame vary across diverse pain conditions and causes due to different rates of invalidation. Research may then be able to identify subgroups of pain populations that are more vulnerable to experiencing the cluster of discounting, pain-related shame, and depressive symptoms demonstrated in this study.
Conclusion
The current study contributes to the broader literature on the harms of social stigma and invalidation on the mental health and wellbeing of people with chronic pain. Pain-related shame is a prominent emotional experience among chronic pain populations but, to date, has remained relatively understudied. Results from the current study demonstrate a powerful link between pain-related shame and depressive symptoms and show, for the first time, that shame about one’s pain may be a key mechanism linking pain discounting to depressive symptoms among people with chronic pain. The finding that discounting was not significantly related to depressive symptoms among patients with the highest levels of perceived support further highlights the benefits of fostering supportive social relationships in this vulnerable population. Overall, findings suggest that pain-related shame may be a beneficial treatment target for addressing depressive symptoms in this population, in addition to bolstering social support and reducing invalidation of chronic pain at all levels of our society.
Supplemental Material
sj-docx-1-hpq-10.1177_13591053231191919 – Supplemental material for Understanding the link between pain invalidation and depressive symptoms: The role of shame and social support in people with chronic pain
Supplemental material, sj-docx-1-hpq-10.1177_13591053231191919 for Understanding the link between pain invalidation and depressive symptoms: The role of shame and social support in people with chronic pain by Alanna Coady, Rebecca Godard and Susan Holtzman in Journal of Health Psychology
Footnotes
Acknowledgements
Thanks to Dr. Brian O’Connor, Professor and statistician within the Psychology Department of the University of British Columbia Okanagan campus, for providing statistical consultation on the methods used in this study.
Data sharing statement
The current article is accompanied by the relevant raw data generated during and/or analysed during the study, including files detailing the analyses and either the complete database or other relevant raw data. These files are available in the Figshare repository and accessible as Supplemental Material via the Sage Journals platform. Ethics approval, participant permissions, and all other relevant approvals were granted for this data sharing.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by a research fellowship to the first author from the Social Sciences and Humanities Research Council of Canada.
Ethics approval
Ethics approval through the University of British Columbia Board of Research Ethics was received September 24, 2020 (study number H20-02449).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
