Abstract
Introduction
Trauma-informed care (TIC) has been promoted as a way for services to be aware and respond to the potential impact of trauma. Although professionals are encouraged to adopt it in routine practice, understanding of TIC is often unclear. A TIC training provider sought advice how to improve training for professionals working with children and adolescents.
Method
This qualitative study explored participants’ understanding of TIC after being trained, experiences of barriers and facilitators to implementing TIC, and recommendations to improve training. Nine professionals from health, social and education services completed semi-structured interviews. Participants varied in age and experience but lacked ethnic and gender diversity.
Results
A model of behavior change (COM-B: capabilities, opportunities, motivation, behavior) guided analysis. Participants described an understanding of TIC consistent with current guidelines, with some divergence regarding responsibility for using TIC and the conceptualization of trauma. Facilitators and barriers to TIC implementation were shaped by these perceptions. Some barriers could be addressed through training, while others require more systemic change, (e.g. shared TIC language; increased resources). Suggested training improvements included clarifying definitions and roles, increasing hands-on practice, and training of supervisors.
Discussion
Findings offer theory-driven contributions to the evidence-base of TIC understanding, facilitators and training improvement.
Plain Language Summary
Traumatic events, such as abuse, can negatively affect mental and physical health. Individuals who have experienced trauma are vulnerable to distress or re-traumatization as a result of healthcare experiences. Understanding this, led to the development of trauma-informed care, which encourages service providers to respond to clients’ needs by being “aware, sensitive, and responsive to the potential impact of trauma.” Trauma-informed care is intended for use by all professionals, from administrators to therapists and teachers, across mental health services, hospitals and schools. In the UK, services are advised to adopt trauma-informed care and train staff accordingly. However, staff often remain confused about what trauma-informed care actually means, how to put it into practice, and how trainings can be improved. A service providing trauma-informed care training for professionals working with children and young people sought advice on how to improve their trainings. The study explored professionals’ understanding of trauma-informed care after training, what helps and hinders their use of trauma-informed care in practice, and recommendations to improve training. Interviews were completed with 9 professionals across young people’s health, social and education services. A psychological model of behavior change guided the analyses of these interviews. Participants generally understood trauma-informed care, with minor differences on who is responsible for using it and what trauma means. Depending on how they understood trauma-informed care, they described different things that helped or stood in the way of using it. Based on this learning, this paper makes recommendations on how to improve trauma-informed care trainings.
Childhood trauma and adversity can have a significant psychosocial impact across the lifespan (Brown et al., 2009; Burke et al., 2011; Kiesel et al., 2016) and is associated with elevated risk of psychopathology, risk events (including self-harm, suicide and violent offences), and functional impairment. Individuals with a history of trauma are particularly vulnerable to becoming distressed or re-traumatized as a result of healthcare experiences (Coles & Jones, 2009). Understanding this led to the development of ‘trauma-informed care’ (TIC), for service providers to better equip themselves to respond to clients’ needs by being ‘aware, sensitive, and responsive to the potential impact of trauma’ (Hanson & Lang, 2016). TIC is an orientation shift from asking clients “what’s wrong with you”, to considering “what happened to you” (Sweeney & Taggart, 2018). It focuses not only on clinical delivery but considers how trauma impacts staff and how systems respond to trauma, across services and levels of staff (Sweeney et al., 2016; Wilson et al., 2013). While there is no universal definition of TIC (Bendall et al., 2020; Berring et al., 2024), there is widespread use of the principles described by the US Substance Abuse and Mental Health Services Administration (Substance Abuse and Mental Health Services Administration (SAMHSA), 2014), which were adopted by the official UK governmental website (gov.uk; Office for Health Improvement & Disparities, 2022) as working definition in light of lacking consensus. They describe four key assumptions of TIC (“4Rs”): realizing the impact of trauma on service users, staff, communities and healthcare systems, recognizing the signs and symptoms of trauma, responding by integrating knowledge about trauma into practice and policy, and resisting re-traumatization.
Increasing TIC Use Through Staff Training
In recent years, TIC has gained popularity across sectors (Becker-Blease, 2017; Purtle, 2020), however, there is limited evidence on what may facilitate or hinder TIC implementation and lead to behavior change (Berring et al., 2024; Hanson & Lang, 2016). TIC guidance suggests that TIC can be implemented at multiple levels, including changes to policy, care environment and through staff training (NHS Education for Scotland, 2017, Substance Abuse and Mental Health Services Administration (SAMHSA), 2014). Staff training is recommended as a first, fast, and feasible way for services to become trauma-informed (Purtle, 2020). Some evidence suggests that staff training in TIC leads to beneficial outcomes including reduced practices that can lead to re-traumatization such as isolation and confinement (Azeem et al., 2017; Borckardt et al., 2011; Elwyn et al., 2015). For patients, some staff training led to decreased juvenile misconduct and assaults (Elwyn et al., 2015) and reduced days spent in treatment in psychiatric hospital (Greenwald et al., 2012). For staff, TIC training was reported to improve attitudes towards trauma, increase TIC knowledge and confidence working with TIC, self-reported skills implementing TIC practices, and perception of safety (Chin et al., 2024; Kenny et al., 2017; Kramer et al., 2013; Purtle, 2020; Shoptaugh et al., 2025). However, multiple studies also found that training had no significant impact on practice or staff’s trauma sensitivity (Borckardt et al., 2011; Crable et al., 2013; Green et al., 2016). TIC training may be especially important for staff working with children (an under-researched area; Kramer et al., 2013), and mitigate the impact of adversity early on (Atkinson et al., 2023). TIC staff trainings vary in definitions, content, aims, length and implementation of TIC (Jackson & Jewell, 2021). Trainings often teach the tenets of trauma-informed practice with the aim of “increasing staff knowledge, improving attitudes, and changing behavior” (Purtle, 2020) however, without clear training aims or theory of how to facilitate TIC implementation and behavior change (Weiss et al., 2017). A scoping review concluded no ‘best practice’ on how to train TIC (Jackson & Jewell, 2021).
A Behavior Change Approach
Psychological theories can guide, structure and inform behavioral change, such as increased TIC use, in an evidence-based way. The widely used COM-B model (Michie et al., 2011) posits that the three factors of capabilities (C), opportunities (O) and motivations (M) are essential for behavior (B) change to occur. See Figure 1. The model can be used to identify facilitators of behavior change. The current study defines behavior as the way an individual or group conducts oneself in response to the environment (Merriam-Webster n.d.) which includes awareness, responses and inhibited responses. The COM-B framework. Note. ‘The COM-B system - a framework for understanding behavior’ (Michie et al., 2011). Capabilities includes physical (skills, training, practice) and psychological capabilities (knowledge, understanding, awareness, memory); opportunities consist of physical (resources, environmental context) and social opportunities (culture, social norms); and motivation incorporates reflective (thoughts, beliefs about capabilities) and automatic motivation (emotions)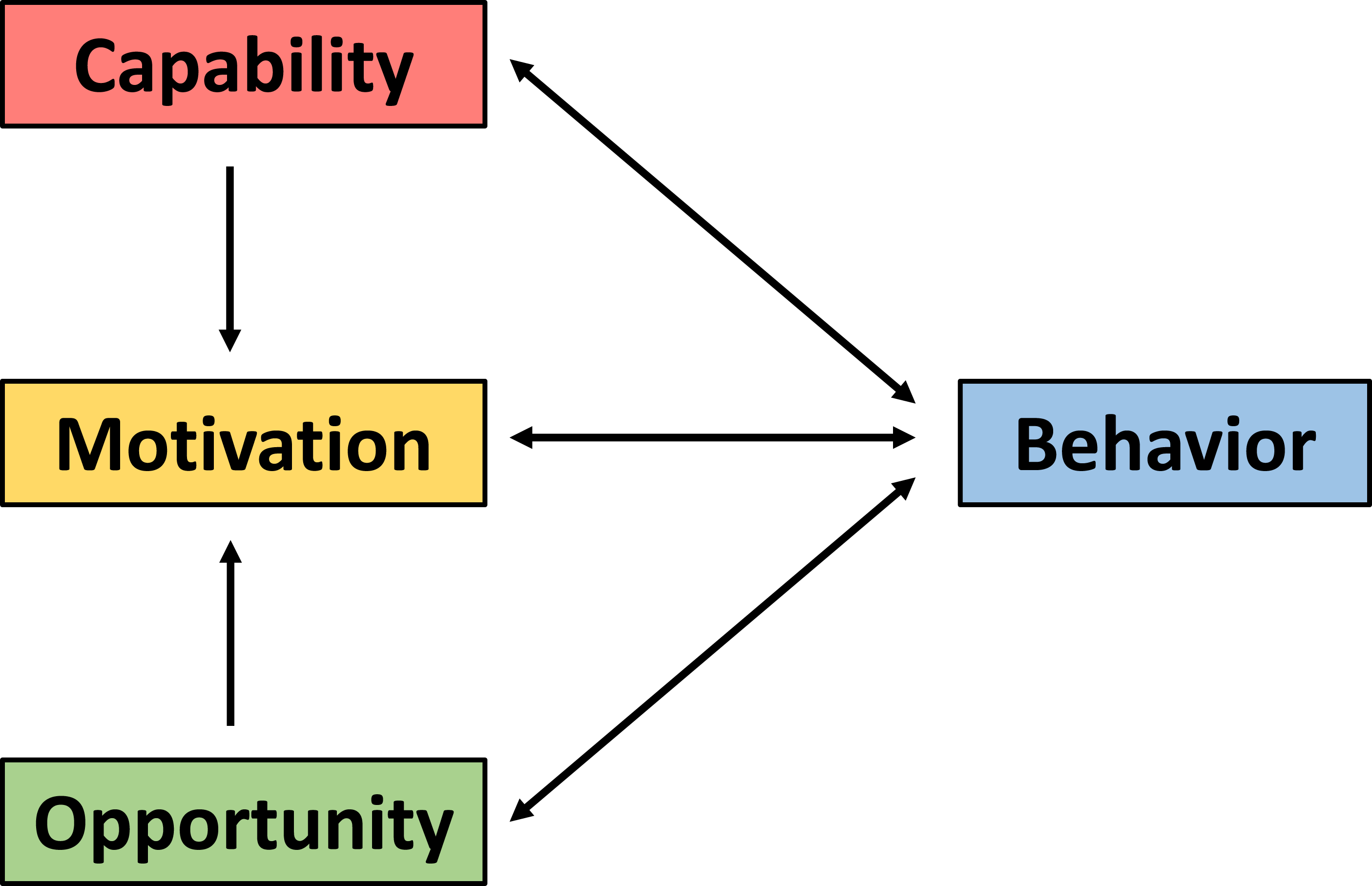
Services across the United Kingdom (UK), including child and adolescent mental health service, social services and schools, have been encouraged to use TIC and train their staff (Office for Health Improvement & Disparities, 2022). A recent review of mental health trusts in England found that a majority (70% of respondents) do not offer any TIC training despite recommendations to do so (McNally et al., 2023). The current study was initiated by an English NHS trust seeking to improve their TIC training for professionals working with children and young people, as anecdotal feedback suggested that TIC understanding remained unclear and TIC was not implemented after training.
The study aimed to explore (1) participants’ understanding of TIC after being trained, (2) participants’ experience of barriers and facilitators to implementing/using TIC, and (3) how TIC training can be improved to aid participants’ understanding and use of TIC.
Method
Participants
Participant Characteristics
Demographic Characteristics of all Analyzed Participants (N = 9)

Note. M = mean; SD = standard deviation; CAMHS = Child and Adolescent Mental Health Service.
Design
The study used a qualitative research design. Reflexive Thematic Analysis (Braun & Clarke, 2006, 2021) was used to explore participants’ understanding of TIC after being trained, their experience of facilitators and barriers to implementing TIC, and recommendations to improve training.
Philosophical Stance
The study is situated within constructivist epistemology, which assumes that knowledge is co-constructed through interactions between participants, researchers, and the broader social context, thus, meaning is produced through engagement with participants’ accounts and the researcher’s own reflexive insights.
Materials
Trauma-Informed Care Training
A 2-hr training was facilitated online, via Microsoft Teams, by a Clinical Psychologist (CC) who had co-developed the training based on current literature and professional, clinical experience, and refined through participant feedback and discussion with young people. The training did not use a specific formal training model. The content covered values and principles of TIC, including SAMHSA’s 4Rs (2014), understanding the psychosocial impact of adverse childhood experiences on children, secondary trauma impact on staff, importance of staff self-care, factors for organizational change, and TIC implementation at all levels of service. This content was accompanied by visuals, case examples and group discussions.
Demographic Questions
Demographic questions asked about age, gender, ethnicity, profession, service, number of years qualified in core profession, amount of direct client contact, and hours of TIC training during and post-qualification.
Topic Guide
To explore participant’s understanding of TIC (aim 1), questions built on the 4R’s definition of TIC (Substance Abuse and Mental Health Services Administration (SAMHSA), 2014). Open ended questions explored participants’ experience of barriers and facilitators to using TIC (aim 2) and recommendations for improvement of the TIC training (aim 3). See Supplemental Material. A focus group of previous TIC training participants, consisting of a mental health nurse and a social workers/cognitive behavioral therapist, helped develop and review the interview questions.
Procedure
The study was approved by the Oxford Health NHS Foundation Trust Quality and Audit Team as service evaluation. Individuals who attended the TIC training were invited to a 45-min interview. Individuals all provided written electronic consent and completed brief demographic questions via the online system Qualtrics. Semi-structured interviews were conducted via Microsoft Teams by the lead researcher.
Analysis
Exclusion
One participant was excluded. During the interview it became clear that they were not able to refer to the training in question but confused it with others and appeared unable to understand questions after prompting.
Thematic Analysis
Interviews were audio recorded. Transcripts were subsequently analyzed using Reflexive Thematic Analysis (Braun & Clarke, 2006, 2021) using NVivo12 (International QSR, 1999). The lead author reviewed each transcript several times to ensure familiarization before conducting the initial coding and generating themes. All authors reviewed the final themes and interpretation of the data to ensure credibility and coherence.
Initially, an inductive coding approach was employed to allow themes to be developed from the data without imposing any pre-existing frameworks. In the second phase, a deductive approach was used to map themes onto the COM-B model, to interpret the data within an established theoretical framework. The analysis takes a predominantly semantic approach, focusing on the explicit content expressed by participants, while acknowledging that these meaning are situated within broader social contexts.
Reflexivity
In line with the analytic approach of Reflexive Thematic Analysis, I, the lead author, acknowledge my role in co-constructing meaning with participants. I have no lived experience of the British settings participants work in (e.g., schools, social care, CAMHS), which likely limited my insight and may have influenced my interpretation of participants’ contexts and experiences. While I share the predominant gender and may be perceived as ethnically similar to professionals in the study, my accent may have shaped how participants perceived me and responded to my interview questions.
My professional background is in quantitative research and diagnosis-focused work with posttraumatic stress disorder, which shaped my initial approach to the research questions and made the shift to qualitative methods a significant learning process. I began with a critical stance toward trauma-informed care, viewing it as a vague concept often used as a ‘buzzword’. My aim was to contribute to its clarification, guided by a personal and professional commitment to improving support for individuals affected by trauma.
Results
Overview of Themes and Subthemes
Six key themes were set by the COM-B model corresponding to capability, opportunity and motivational components which impact behavior change. Twelve subthemes were generated from the participant interviews which impact the behavior of trauma-informed care. For an overview see Figure 2. Schematic of themes and subthemes following the COM-B model. Note. The COM-B model (Michie, van Stralen, & West, 2011Michie et al., 2011) was expanded with current subthemes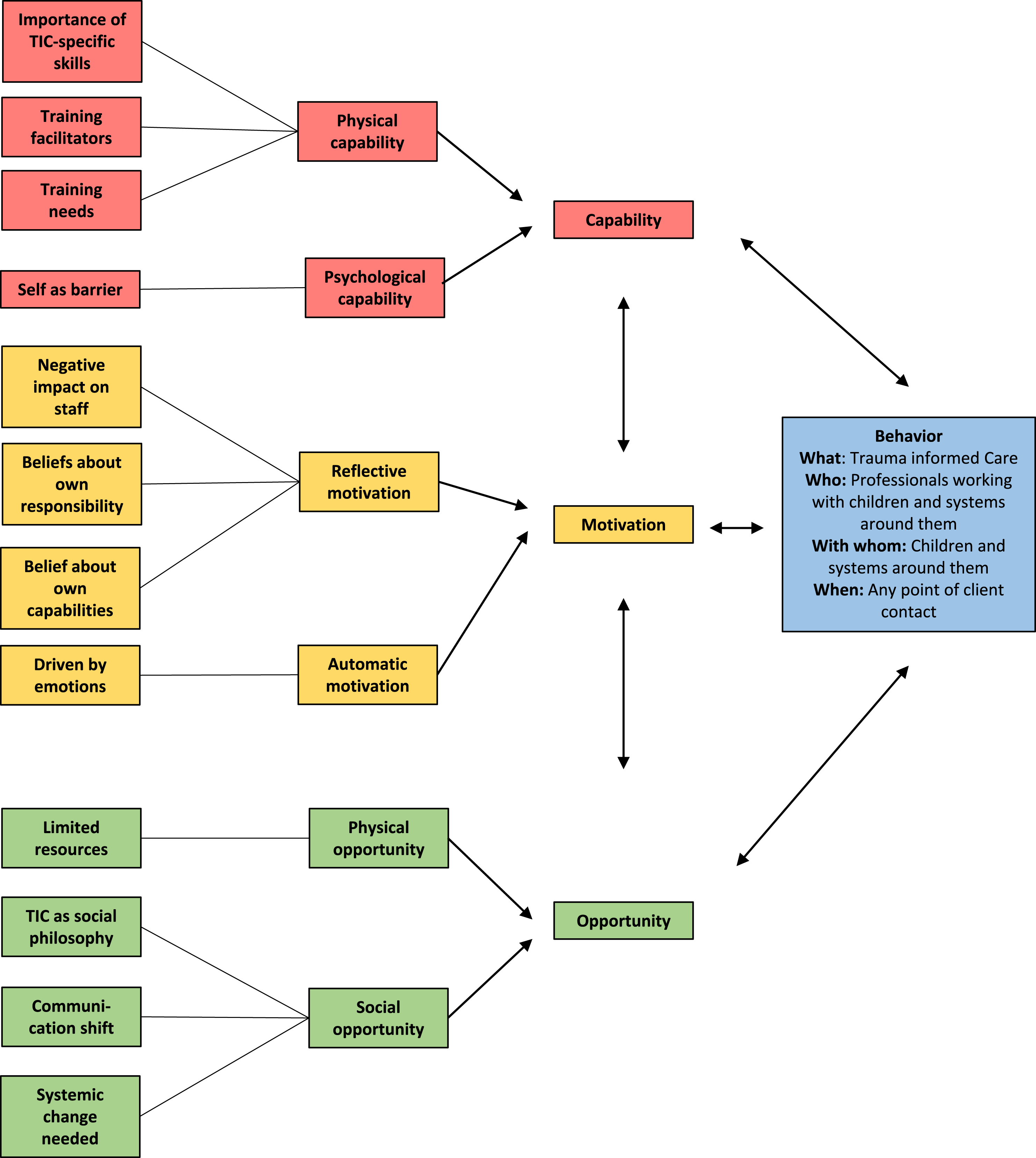
Capability: Physical Capability
Importance of TIC-Specific Skills
Participants varied in their understanding of what TIC should look like in practice. Some listed specific trauma-informed skills, such as “looking for adverse childhood experiences… anything they felt that happened, that had a big impact on them” (P5 1 ). One team used a “trauma crib sheet” as “a prompt, what to ask and what to look for when going through those… tricky conversations.” (P9). One emphasized trying to prevent re-traumatization by “checking out with the person what distresses them so you can make sure that it's not a trigger” and not unnecessarily asking people to retell their trauma (P4, P8, P9).
There was a pattern of TIC-specific behaviors of empowering clients and being client-led (P7). This included “getting permission for beginning that conversation and… understanding what… they want to do next after sharing something like that” (P4), “giving some control back to that child” (P5).
Others described their TIC understanding and implementation in ways that could be construed as standard best practice, such as validating client’s experiences (P1), normalizing (P7), empathizing (P8), offering reassurance, not blaming the child (P7), and not making assumptions (P1) but asking questions when unsure (P1). TIC was described as all-encompassing approach “putting the young person first and making sure all their needs are met” (P2).
Training Facilitators
Specifics of the training format were highlighted as helpful, especially interactive “discussion and hearing other people’s point of view” (P4) and case studies to benefit from the multidisciplinary perspectives “if you had a teacher, a youth worker, a CAMHS worker, a statutory social worker, then me, and we’re all looking at the same case study but everyone’s got different views because of their… different training” (P7).
Participants highlighted particular content they found helpful, such as specific metaphors, “that ‘window of tolerance’… either you’re hypervigilant…, but on the other end of the spectrum you completely shut down,” or stress visualized as “a cup being filled” (P10). Participants emphasized their new understanding of “different levels of [trauma] interventions” (P1) and “trauma not just being about traumatic experiences and formal PTSD as an entity” (P8). One particularly valued how “[the facilitator] went back to basics… and explained what trauma was, what it might look like, what being informed means” (P9).
Participants unanimously agreed on the need for top-up trainings or to “have like a check in session, maybe a couple of months later, just to see… have you had the opportunity to try anything new and how’s it going?” (P9). Participants suggested “online resources… to go to independently to look at that are… clinically sound information and link to what you’ve learned” (P1) as well as “workbooks/sheets” (P4,P7), “infographics “(P2,P6), one noting that printouts were “a discussion point for a good week amongst all the staff” (P2). Participants suggested reminders, “newsletters” (P6,P10), “or a mailing list of any updates” (P6).
Individual attributes of the training facilitator were highlighted as positively contributing to the training, especially the facilitator’s expertise (P1,P5), “infectious passion” (P5) and way of communicating (P2) and encouraging questions (P6).
Training Needs
Participants noted specific staff groups who didn’t attend the training but would benefit from it, such as “ensuring that managers are singing off the same song sheet as you” (P4), “clinical supervisors within the team who do the caseload and clinical supervision” (P6), and “particularly for my admin team…they have such limited training… around trying to understand and manage sometimes very difficult interactions with parents or others” (P12).
Clinicians working in specialist services were keen to receive training around their specific client group (P2) and “how they might present differently, like our autistic or ADHD population, if there were adaptations we’d want to make around that” (P1).
A few participants noted that that the TIC training lacked implementation skills, with one stating “I struggled to know what I could take from the training to implement with the wider team” (P9), while another had not used TIC since the training (P6).
Capability: Psychological Capability
Self as Barrier
While participants widely agreed that they had the capability to use TIC, some saw themselves as barrier to using it, noting “I don’t think I’m perfect at recognizing trauma” (P4), “recognizing… there are limitations for myself… in how to manage [trauma]” (P1) and seeing trauma as something complicated and complex, where “trying to implement that is always tricky, ‘cause it’s about kind of where you pitch things and when to do that” (P1). Multiple pronounced their poor memory as a barrier to TIC (P4,P8,P9) where “it’s really hard to remember specifics” (P8) from the training.
Motivation: Reflective Motivation
Negative Impact on Staff
Participants voiced concerns over the negative emotional impact of trauma on themselves and other staff (P1, P8, P10) and the potential for it to “trigger own trauma” (P6), describing: “some days if somebody is ringing me upset, I… sometimes don’t want to talk about [trauma]… I do, but I don’t want to … it’s a lot to take on some days” (P4). Proposed solutions included broaching this topic in trainings and team conversation, exemplified by their recent TIC training: “we spoke about… the impact of trauma on the practitioner… about stress and burnout and… ways that we deal with that feeling in our practice…it’s something that we don’t talk about enough, especially when we’re starting to feel burnout as practitioners” (P4). Others suggested utilizing self-reflection (P1,P6): “if you come away from a situation like taking on some of the emotion of the person you are speaking to… I think that can be really reflective of how that person is in it as well” (P4).
Beliefs About Own Role and Responsibility
A central theme was the question of who was responsible for using trauma-informed care. Some saw it as a significant barrier that they didn’t have better access to TIC “experts”, someone “more specialized” (P4) where children with trauma would “normally be referred on” (P7). A few merged this with their understanding of TIC as a specialist topic and not within their job: “we have to be clear what our remit is within our service and providing trauma work… isn’t really something that we’re set up to do” (P1), setting TIC equivalent to trauma work which “isn’t ours to deal with” (P1).
Others viewed TIC as a topic everyone is responsible. The majority suggested that that therefore “everyone should attend the training” (P2, P3, P8, P10), arguing that it’d be really helpful for us to all be at the same training and learning about the same topics so then we have that shared knowledge. ‘Cause often there’s like four people sometimes working with one person, so I think consistency is really helpful” (P4) and indicating a shared responsibility to know and use TIC and prevent re-traumatization (P4). One criticized that only individuals who were already interested in TIC attended the training (P5), placing the responsibility of using TIC on those with personal interests in the area, to which others suggested that training should be mandatory (P1,P7).
To facilitate shared responsibility, participants proposed building TIC skills within their own teams (P8) to decrease the need to refer to experts. Ideas included bringing TIC-related questions to managers meetings (P9), having trauma-informed supervision (P5), “weekly consult” or “having a “trauma-informed champion” (P8), asking questions within the team such as “have you considered trauma? How significant is that event?” (P6), and sharing and displaying TIC resources (P10).
Beliefs About Own Capabilities
Some described questioning their capabilities and skills in “opening that box” of trauma (P4). For multiple participants, the TIC training increased confidence (P1, P5) and comfort with the topic (P1), reassured and validated their existing skills and knowledge, and gave them “the language around [TIC] to evidence it and to feel confident that that’s what I’m doing” (P5).
Motivation: Automatic Motivation
Driven by Emotions
Participants’ fears impeded TIC use. For example, “people are reluctant to name things… even saying the T word in that fear” (P1), and worries about retraumatizing were the “hardest thing” (P9) where “the natural urge would perhaps be to not go anywhere near [the trauma]” (P5). In contrast, TIC learning was facilitated by positive emotions (P9) such as interest in TIC (P1, P7, P8) and experiencing the training as enjoyable (P2, P4, P5, P6).
Opportunity: Physical Opportunity
Limited Resources
Systemic barriers were highlighted across sectors as impeding TIC usage, with “workers and services being really stretched” and “understaffed” (P5), making TIC use “really difficult” (P5), with one explaining: “I think, pressures are so high on people within services… that sometimes the focus can be on the problem at hand and not thinking wider” (P10). Time pressures (P2, P4, P9) were highlighted as a major factor limiting TIC use, based on the belief that “it takes time to talk about [trauma]…I don’t want to… open that box then quickly shut it and it be more damaging to our family than if I’m just keeping it shut. So I think that’s always a challenge” (P4) and balancing time demands: “when you’ve got a really long list of people to see… I’d love to be really trauma-informed for every single person we see, but I know in reality we’re up against it.” (P5).
Opportunity: Social Opportunity
TIC as Social Philosophy
Many participants described TIC as a general mindset or perspective (P1), rather than specific behavior. This included being aware and mindful of trauma (P5), recognizing potential trauma and its impact on the young person or their system (P1, P6) and how trauma should be considered within next steps of care (P5). Emphasis was given to “holding in mind” the young person and family’s experience (P9, 10), their story, environment and context (P5,P10). In addition, TIC included being “incredibly mindful” (P8) of potential triggers for re-traumatization (P6, P8).
Communication Shift
TIC was experienced across participants as a change of narrative (P5,P8) around the young person, which included TIC-specific language (P2,P8) as a way of demonstrating that change of perspective and to “reframe what traumatic experience is” (P8). A TIC-narrative should de-blame and emphasize that the trauma “shouldn’t have happened and wasn’t their fault” (P5) and “lend itself to be more client-centered” (P8).
TIC also recognizes behavior as a way for young people to communicate (P1,P7) or respond to trauma (P2,P4), for example, reframing “young people who are ‘naughty’ or ‘aggressive’,” to recognize “a child that’s in distress” (P5), and describe behaviors as “attachment seeking, not an attention seeking” (P10), in short, using what is known about the child’s experience (P4) to understand their behavior (P2, P4, P5, P7, P10). One pronounced that TIC also meant encouraging others to change their language away from “negative labels” and “helping the young person understand their behavior differently” (P5).
Systemic Change Needed
Most participants emphasized that, for TIC to work, implementation needed to be systemic, across professionals, teams, services, agencies (P9) and “everyone around that young person” (P5), with some calling for a culture change towards becoming more trauma-informed (P8, P10). There was agreement that a joint approach across services was essential (P5, P9, P10), drawing on all resources around the young person (P9), such as parents, family, carers, school, social workers (P5) and “making sure that everyone around that child is aware of what’s happened… aware of where we are now and what the plan is moving forward, and that we’re all doing the same thing” (P9). Participants noted barriers to systemic change: “I think the biggest barrier is individuals, whether in my team or in the system, not being aware of the training” (P8) and “at different levels of being trauma-informed” (P10). To facilitate systemic change in services, many noted that TIC should be modelled and encouraged ‘top down’ (P5, P8, P10): “if it’s something that we want embedded then it has to come from the top down and it has to be reflected across all levels of the management team, through our supervision with staff and also how everybody treats each other within the team” (P5).
Interrelated Results
All three research aims were captured within one model as they are closely interrelated: How participants understood TIC (aim 1) shaped what they saw as facilitators or barriers to behavior change (aim 2). For example, participants’ understanding of who is responsible for using TIC, influenced whether they noted “increasing access to experts” or “increasing expertise within their own team” as possible facilitators. Many of the described facilitators and barriers to TIC (aim 2), could be increased or mitigated, respectively, through improved training (aim 3), for example, “belief in own capabilities” can be increased through training and practice, and understanding of TIC (aim 1) as a “communication shift” encourages de-blaming narratives around trauma.
Discussion
The current study aimed to evaluate trauma-informed care trainings of professionals working with children and young people and make recommendations for training improvement. It did so by exploring participants’ understanding of TIC after being trained, participants’ experience of barriers and facilitators to using TIC, and drawing out how TIC training can be improved to aid participants’ understanding and use of TIC. Themes that were constructed from semi-structured interviews were mapped onto a psychological model of behavior change (COM-B) to understand factors leading to increased TIC behavior.
TIC Understanding
Participants’ TIC understanding was largely in line with the existing evidence base (SAMHSA, 2014), suggesting that the training effectively conveyed the conceptual foundations of TIC. Participants realized the impact of trauma on service users and highlighted how it can impact staff themselves (e.g. inducing fears and negative emotions). This demonstrates an awareness of the emotional labor inherent in their roles, with underlying worries that this could be amplified when being exposed to more trauma-related topics. Participants’ description of TIC as a social philosophy or mindset suggests that they see it as more than a set of techniques but a way of thinking that shapes everyday interactions. For example, participants noted that they were able to recognize signs and symptoms of trauma, for example in behaviors (e.g. “the naughty child”) in response to trauma and advocate for a communication shift (changed language, narrative) in response. This illustrates professionals’ ability to translate learning and interpret children’s behaviors through a trauma-informed lese in their daily work. Going beyond the shift in mindset and perspective, participants critiqued the lack of concrete implementation skills in training on how to respond. This highlights a mismatch of training set up (theoretical, knowledge-based) and organizational need (practical, skills-based). However, they also described practicing some TIC-specific skills to respond to trauma and to resist re-traumatization such as trauma-specific questions and client empowerment through choice, indicating active use of TIC skills.
Some participants’ understanding of TIC was different to the dominant evidence-base, for example, believing it necessary to know details of the trauma to apply TIC (P6), while TIC principles only include a general ‘awareness of the impact of potential trauma’ (Substance Abuse and Mental Health Services Administration (SAMHSA), 2014), or that TIC should only be done by specialists or needs extensive time, rather than being a general mindset shared by everyone, as the literature describes. These responses demonstrate assumptions about professional roles, responsibility and expertise that are not in line with the intended TIC learning and suggest the need for more explicit clarification of these issues. A critique of TIC is that it is simply a new label for best-practice person-centered care (Berliner & Kolko, 2016) or gets misunderstood as such. This understanding was shared by some participants who defined TIC as practices common to standard best practice such as consent, empathy, validation, and safeguarding. Future trainings should clarify the definition and boundaries of TIC, so participants have a shared understanding. These differing interpretations underscore the potential for ambiguity in practice and suggest that TIC trainings need to clarify the scope and application of TIC to foster a consistent, collective understanding among staff.
Facilitators and Barriers to TIC Use
Participants highlighted specific facilitators and barriers to behavior change. In line with the COM-B model (Michie et al., 2011), results showed how their physical capabilities to use TIC behavior were facilitated by good training (interactive format, facilitator qualities, repetition) and knowledge of TIC-specific skills, while individuals saw their psychological capabilities diminished by personal shortcomings (poor memory and skills), demonstrating how capabilities are not only based on skill acquisition but shaped by self-perception. Reflective motivation encouraged TIC behavior where individuals had a strong belief in their own capabilities and felt responsibility to use TIC, emphasizing how confidence and professional commitment can drive behavior. However, beliefs that TIC was not within their job remit, or experiencing negative impacts of trauma work on themselves created reflective and automatic motivations against the use of TIC. Limited resources (understaffing, lack of time) were consistently described as limiting physical opportunity to use TIC, demonstrating that structural constraints can undermine even motivated, capable practitioners. Therefore, systemic change was requested to create social opportunity to use TIC. This included joint approaches of the systems around a child, a communication shift towards using TIC language and non-blaming narrative, and having a shared social philosophy/mindset of TIC. These insights illustrate that behavior change in TIC is not solely an individual challenge, but deeply embedded in organizational culture, norms, and resource allocation.
Multiple of these findings match aspects needed to implement TIC, as described in other studies, including the need for leadership ‘buy in’ (Weiss et al., 2017), a conceptual mind-set shift (Nikopaschos et al., 2025), a common language regarding TIC (Bartlett & Rushovich, 2018), more in-depth training (Choi & Seng, 2015; Novilla et al., 2024), need for specific TIC strategies (Chudzik et al., 2025), training to increased confidence in TIC (Dueweke et al., 2019), the need for a “cultural shift” across all levels of a system (Chudzik et al., 2025; Stokes et al., 2024), and resources, time, and administrative support in stretched and stressed settings (Novilla et al., 2024). Other findings match theoretical principles of TIC, such as increasing client choice and empowerment (Substance Abuse and Mental Health Services Administration (SAMHSA), 2014).
Recommendations for TIC Training
Recommendations to Improve TIC Training

Reflexivity
My (HL) training as a Clinical Psychologist may have influenced my interpretation of participants’ descriptions of trauma-informed care (TIC), potentially leading me to align TIC practices with my understanding of broader principles of good practice and person-centered care. To mitigate this bias, I maintained a reflective log throughout the study to track shifts in my thinking and ensure that the themes remained closely aligned with participants’ perspectives.
Strengths and Limitations
A strength of the current study is its theory-driven approach using a psychological model to guide analysis and recommendations for behavior change. Results illustrate how inter-related and mutually influencing the answers to TIC understanding, TIC barriers/facilitators and training improvement are, highlighting the strength of capturing them within one model. Especially in a field that offers largely descriptive research (Hanson & Lang, 2014; Reeves, 2015), this study offers an evidence-based contribution to the discourse. The qualitative approach allowed for exploration of a topic where there is not yet established consensus of the understanding of TIC by professionals using it. The study incorporated a wide range of professionals working with children and young people allowing a broader impression of professionals’ TIC understanding and implementation across services and sectors than if a professionally homogenous sample had been interviewed.
Key limitations must also be noted. Participation was likely biased by self-selection through a personal interest in TIC. The sample notably lacked diversity of gender and ethnicity (predominantly White, female). Unfortunately, this is largely representative of the professions included, but means experiences from more diverse backgrounds or minority groups were not captured. A strength of the sample was its variation in age and years of experience, reducing the likelihood that perspectives on TIC understanding and training were skewed toward either novice or highly experienced professionals. The study grouped together professionals from a wide range of services, reflecting the multidisciplinary nature of TIC and realistic training set-up in this context. Future research could explore differences in understanding and facilitators of TIC by profession and provide training recommendations specific for professions or contexts (e.g., schools vs neuropsychology services). As is expected with qualitative research, the study cannot claim that results generalize to other settings or contexts but findings could provide a starting point for improving TIC trainings and guiding further research.
In conclusion, in the context of increased popularity of TIC but dearth evidence on its training and implementation, the current study contributes to the evidence-base of TIC understanding, training and implementation using a theory-driven approach.
Supplemental Material
Supplemental Material - Trauma Informed Care Training: A Theory-Driven Qualitative Evaluation and Recommendations for Improvement
Supplemental Material for Trauma Informed Care Training: A Theory-Driven Qualitative Evaluation and Recommendations for Improvement by Hjördis Lorenz, Carmen Chan and Ciorsdan Anderson in Clinical Child Psychology and Psychiatry
Footnotes
Acknowledgements
We are grateful for all participants of the focus group and interviews.
Ethical Considerations
The project was approved and registered by Oxford Health NHS Foundation Trust Quality and Audit Team as service evaluation, and thus no ethical approval was needed.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The first author, HL, was funded by the Oxford Health NHS Foundation Trust for a Doctorate in Clinical Psychology. This project fell within the scope of this doctorate.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data can be made available upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
