Abstract

A 23-year-old man with right great saphenous vein (GSV) insufficiency and dermatitis underwent staged segmental radiofrequency ablation (RFA) using the ClosureFast device (Medtronic, Minneapolis, MN, USA). Following intense physical exertion involving heavy lifting, he developed a painful right inguinal mass. Duplex ultrasonography demonstrated a large, thrombosed aneurysm arising from the proximal GSV stump (Panel A-1: arrow). Computed tomography (CT) venography confirmed an aneurysm (5.6 × 4.0 × 1.9 cm) without arterial communication (Panel A-2: arrows). Surgical excision was performed (Panel B-1), and the specimen was removed en-bloc (Panel B-2). Histopathological examination (using hematoxylin and eosin) revealed medial degeneration and elastic fiber fragmentation (Panel C-1: arrows and arrowhead, respectively), as well as smooth muscle degeneration and reactive lymphoid hyperplasia ( Panel C-2: arrows and arrowhead, respectively) — features consistent with a primary venous aneurysm rather than reflux-induced degeneration.
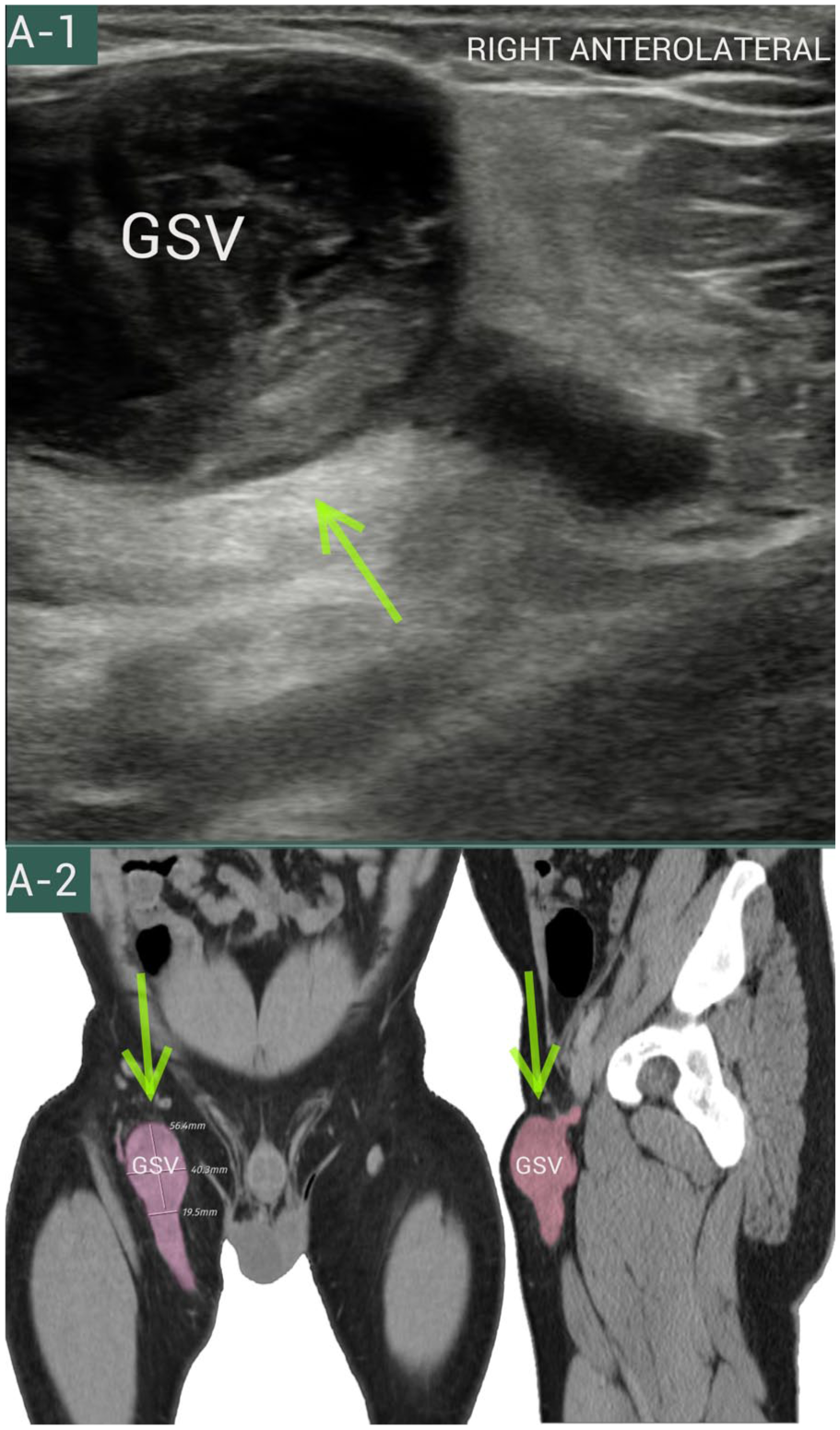
Ultrasound demonstrated a large thrombosed saccular dilation at the proximal right GSV stump, and CT venography confirmed a non-opacified aneurysm without tributary inflow.
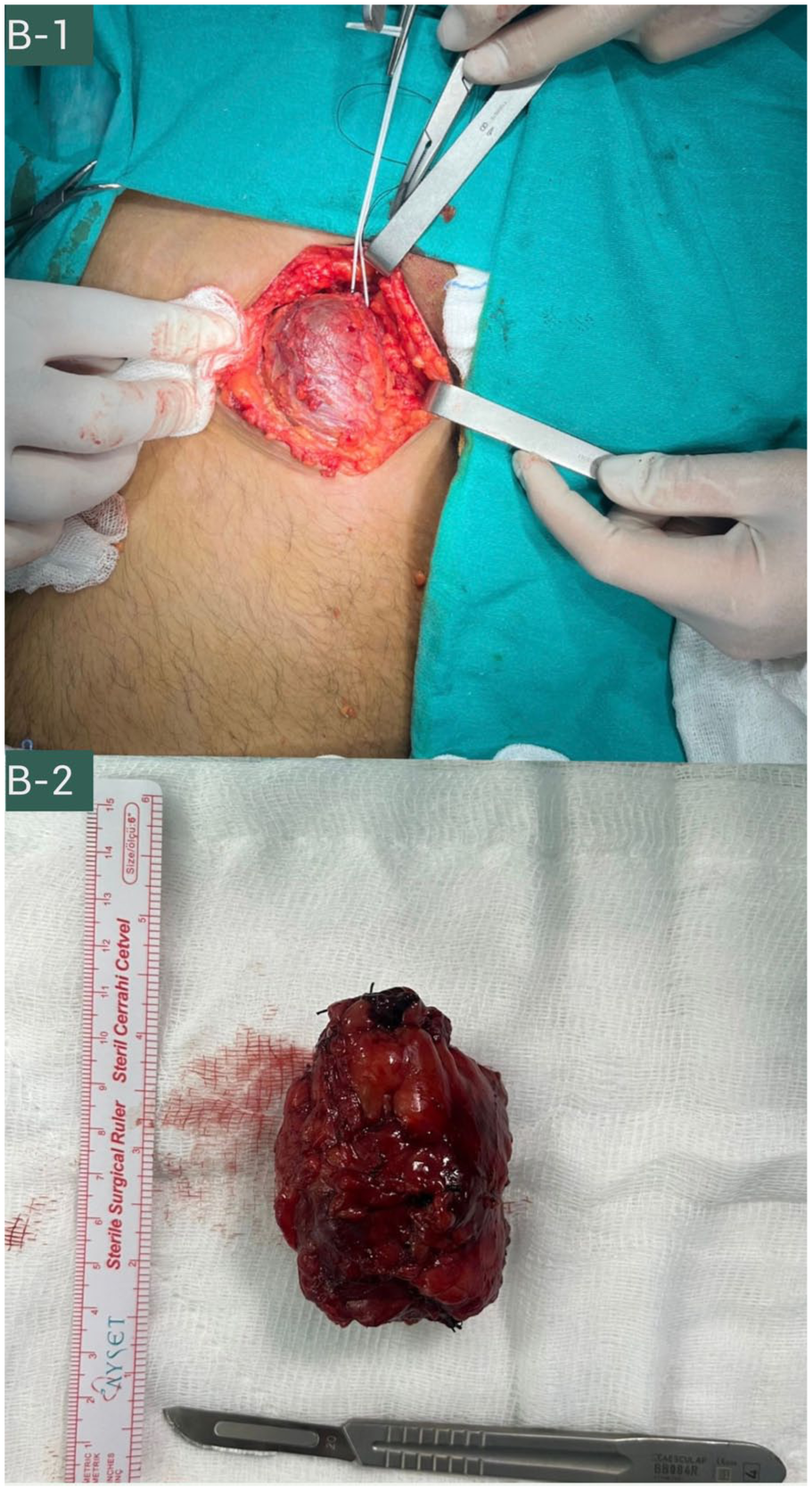
Intraoperatively, a well-encapsulated thrombosed sac was exposed and excised en bloc; the gross specimen showed a completely thrombosed aneurysm.
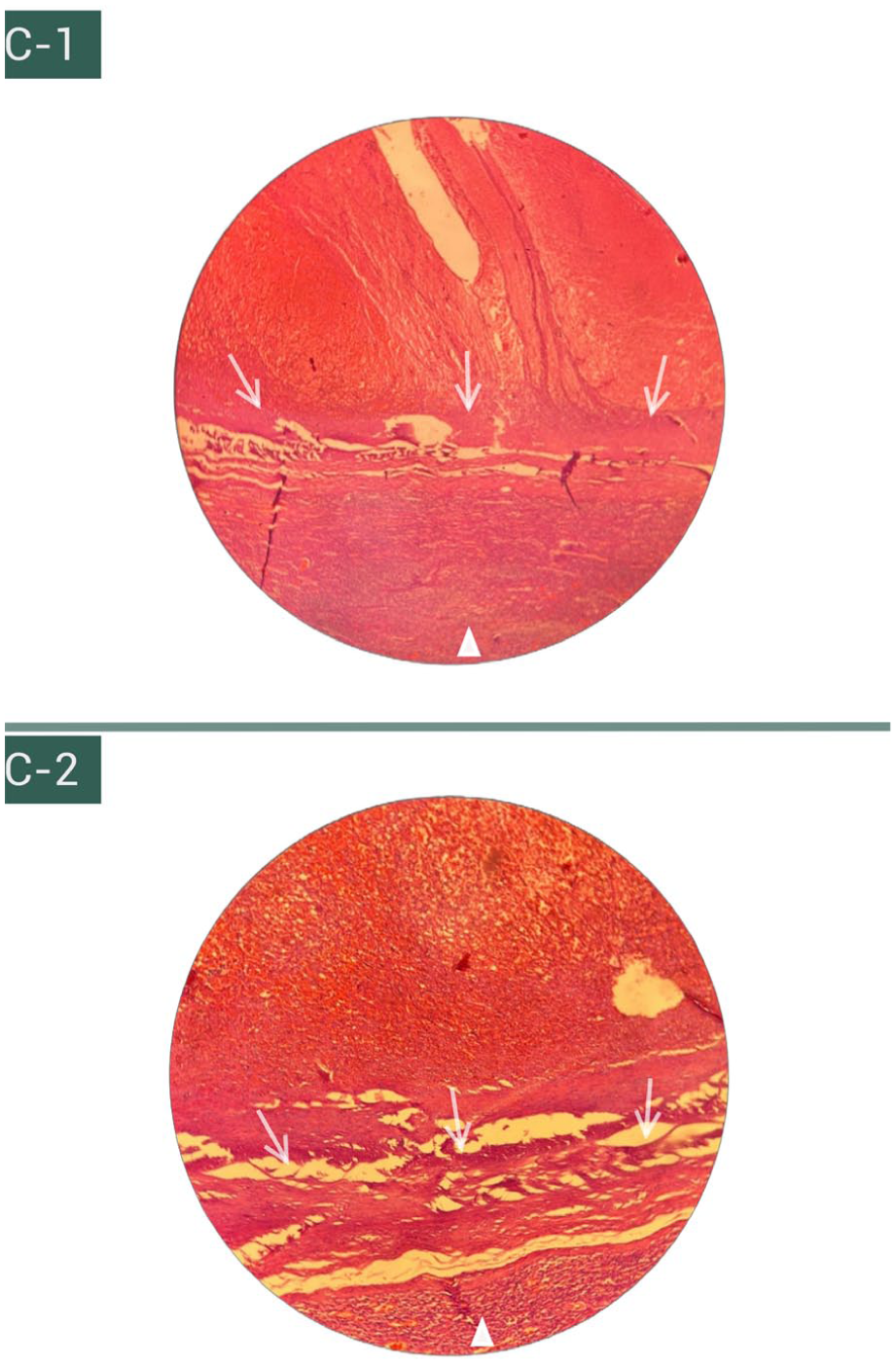
Histopathology (H&E) revealed medial degeneration with smooth muscle loss, elastic lamina fragmentation, and adventitial thickening with adherent organized thrombus, consistent with a primary venous aneurysm.
Venous aneurysms of the GSV are rare and often overlooked. Classified as primary (idiopathic) or secondary to venous hypertension, trauma, or postphlebitic. Chronic reflux in GSV may promote aneurysmal change via wall stress. 1 Aneurysmal dilatation of a thrombosed GSV stump following endovenous ablation has not previously been documented. Only one previous case has been linked to arteriovenous fistula formation. 2 In contrast, we describe a thrombosed, nonfistulized aneurysm that occurred shortly after technically successful RFA. This raises questions about the interaction between procedural success, wall fragility, and postoperative stress.
Medial disruption is typical of nonvaricose venous aneurysms, where intrinsic wall weakness predominates. 3 The absence of reflux, tributary inflow, or systemic disease, combined with complete thrombosis, suggests aneurysmal transformation within a hemodynamically isolated yet structurally vulnerable segment.
Endovenous thermal ablation is the preferred treatment for truncal reflux due to its safety and efficacy. 4 Guidelines diverge on postoperative surveillance. The European Society for Vascular Surgery (ESVS) recommends ultrasound at 1–4 weeks postablation (Class IIa, Level-C), 4 whereas the 2023 American Venous Forum (AVF) advises against routine imaging in asymptomatic patients (Class I, Level-B). 5 Our case illustrates how intense early exertion may reveal latent wall weakness, supporting selective early surveillance in patients at higher mechanical risk.
Footnotes
Acknowledgements
The clinical management of this case was performed during the corresponding author’s tenure at Şırnak State Hospital, Türkiye.
Author Contributions
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
