Abstract

Physicians and other healthcare professionals attracted to vascular medicine are passionate about addressing the complexities of vascular conditions collaboratively and comprehensively. Vascular medicine is a multifaceted specialty that intersects with a multitude of disciplines, including: cardiology, vascular surgery, internal medicine, family medicine, interventional radiology, wound care, hematology (clinical thrombosis and antithrombotic therapy), oncology, and neurology, among others. The broad scope of this field presents opportunities and challenges for those who practice vascular medicine. In contrast to other medical and surgical specialties that typically work within a narrower scope, collaboration with numerous disciplines is necessary for success in providing vascular care. Vascular medicine specialists are devoted to delivering comprehensive, holistic, patient-centered care that integrates medical, interventional, and surgical modalities.
This Blue Page edition explores the opportunities and significance of collaboration in vascular medicine along with providing insights into how professionals can navigate this intricate landscape throughout their careers to gain professional fulfillment.
Embarking on the journey: Opportunities and challenges for early career professionals
Early career vascular medicine specialists encounter numerous opportunities as they launch their professional journey. Commitment to patient-centered care, equitable resource allocation, and advocacy for dedicated interdisciplinary teams are essential. This includes the incorporation of advance practice providers who have been increasingly integrated into the vascular medical team in a variety of roles and settings. 1 However, limited training programs, territorial boundaries, and restricted resources can heighten the scarcity of opportunities, making it imperative for aspiring vascular medicine specialists to navigate this terrain strategically. 2
Given the relative scarcity of vascular medicine training programs at the present time, early career professionals must meticulously research available programs and be prepared to relocate for advanced training opportunities to meet the requirements and full array of vascular medicine competencies. 3 The demand for vascular medicine specialists often exceeds the supply, leading to competition for open positions among the facilities. Realizing the value of institutional support and mentorship, trainees may prioritize employment possibilities at institutions with established vascular medicine divisions or programs. Training institutions often serve as hubs for employment opportunities, offering appointments ranging from clinical faculty positions to research and administrative roles. Early career professionals can capitalize on these opportunities by completing fellowship training and establishing themselves as leaders within their respective departments. Working alongside like-minded colleagues and mentors who understand the significance of the specialty can provide a supportive atmosphere for professional growth and collaboration. Because of this, many people acquire jobs within the organization where they completed their training program. Some individuals may consider transitioning to other specialties, such as pursuing fellowship in cardiology, where the management of vascular disorders is included. Although this may present a more established career path due to the sheer number of those in the profession, it may only partially align with their passion to provide comprehensive vascular care. This may lead some individuals to focus their time on cardiology alone and bring about potential professional dissatisfaction.
Moreover, concerns may arise from fellows on visas as they cannot be sponsored at all institutions. Many fellows who have pursued cardiology fellowship after a vascular medicine training year have cited concerns regarding employment in their home country where vascular medicine is not recognized or there are no established vascular medicine centers. They may subsequently be marketed as a cardiologist and their knowledge in the vascular arena is under-utilized; or they are unable to build a practice of ‘vascular’ patients due to lack of awareness of what this specialty provides. In addition, corporatization of medicine at many institutions may not allow distinction among subtle specialty differences. This in turn limits the ability to attract well-trained vascular medicine specialists to geographic areas where patients could most benefit from their services.
Though not impossible, securing a vascular medicine attending position outside of a training institution can be challenging, necessitating proactive leverage, networking, and relationship building. Creating a new interdisciplinary vascular medicine clinic or program requires developing relationships that share common goals and cultivating comprehensive patient care, but the effort can unlock new leadership opportunities for early career professionals in vascular medicine. This gives early career professionals a unique advantage as they can mold their career trajectory from its inception—exemplifying their vision of themselves as a catalyst for change and their passion for comprehensive vascular care. Aspiring vascular medicine specialists can lay a substantial foundation for future success by actively pursuing mentorship from seasoned professionals.1,4
Whichever path the early career vascular specialist chooses, navigating this terrain demands strategic planning and proactive engagement. Networking is vital for uncovering job opportunities and advancing one’s profession in any field, and vascular medicine is no exception. Partaking in professional organizations, including SVM, attending conferences, and engaging in collaborative research projects are effective ways to extend professional networks and grow strong, enduring relationships within the field. By strategically leveraging connections with colleagues at training institutions and proactively engaging in networking activities, vascular medicine specialists can overcome challenges associated with job availability or poor visibility of the specialty. Being able to fill a void despite not fitting inside the ‘box’ can lead to long-term success and fulfillment in vascular medicine. It is not unusual to consider dual department appointments to meet the needs of the vascular medicine specialist and the institution.
Navigating the mid-career terrain: Balancing expertise and collaboration
Mid-career vascular medicine specialists experience unique opportunities as they grow their careers and make meaningful contributions to the field. A delicate harmony between fostering collaboration and deepening expertise distinguishes this stage for mid-career professionals (e.g., 10–20 years removed from initial training). Key opportunities include interdisciplinary communication, career advancement, and strengthening practice balance. Practice balance herein encompasses individuals with dual training in cardiology and vascular medicine, for example. They may become increasingly drawn to either discipline, potentially diminishing their focus and passion for one specialty over the other. Similarly, practice balance in individuals specializing solely in vascular medicine may concentrate intensely on one aspect, such as thrombosis, creating an asymmetry in clinical practice. Both, if not well managed, can result in mid-career dissatisfaction.
In reaction to these challenges, individuals may examine alternative avenues to maintain their devotion to vascular medicine and advance their careers. Some may seek to assimilate new roles or responsibilities within their existing positions, such as leadership roles in interdisciplinary teams or involvement in research and education endeavors. By expanding their scope of professional involvement with the subspecialty outside of their clinical practice, mid-career professionals can enhance their professional satisfaction and contribute to advancing vascular medicine.
Progressing from early career roles to positions of leadership and influence demands proactive career planning and skill maturation. Mid-career professionals must take opportunities for continuing education, research, and leadership positions within their organizations and beyond—such as at national and international societal levels. 5 Effective collaboration with colleagues from specialties such as cardiology, interventional vascular radiology, and vascular surgery is fundamental for optimizing patient care and can support this practice balance. Navigating differing viewpoints and communication styles can pose challenges, requiring strong interpersonal skills and an open collaborative mindset among the interdisciplinary team of vascular experts.
To ensure professional satisfaction, avoid burnout, and mitigate the need to pursue new employment, individuals encountering challenges related to focus, balance, and dissatisfaction in vascular medicine can implement several proactive solutions. 6 Time management, delegation, and boundary-setting are important for long-term sustainability. This can assist in maintaining interest and passion by offering various invigorating challenges, such as engaging in ongoing professional growth to augment skills and knowledge across various aspects of vascular medicine. Pursuing additional training, attending conferences, and participating in continuing medical education activities can enhance expertise and foster a sense of fulfillment. 6 In addition, collaboration with colleagues from other specialties like interdisciplinary consultations for unique complex clinical scenarios (e.g., pulmonary embolism multidisciplinary response teams [PERTs]), joint case discussions, and collaborative research projects to leverage collective expertise and address complex cases comprehensively can deliver professional satisfaction, and moreover, better patient-centered outcomes. 7 Seeking mentorship from experienced vascular medicine experts or leaders within the field to gain insights, guidance, and support is important. Mentorship connections can provide invaluable perspective, encouragement, and guidance for navigating challenges and growing professionally. 6 Advocating for resources and support within one’s employment organization to promote balanced practice and professional growth may be necessary and often involves asking for dedicated research or education time or securing additional funding. Regular assessment of career fulfillment and alignment with personal and professional pursuits is crucial. This may require intermittent negotiation with employers to build a work atmosphere that supports particular needs and preferences to avoid burnout and promote long-term job satisfaction. 6
The demands of a career in vascular medicine can be all-consuming, making it essential for mid-career professionals to prioritize self-care and support a healthy work–life balance. Despite these demands, mid-career professionals are well positioned to leverage their expertise to drive excellence in vascular medicine. By promoting collaboration, pursuing ongoing professional development, and prioritizing personal well-being, mid-career specialists can successfully navigate this phase and continue making meaningful contributions to the field.
Mastering the art of leadership: Perspectives from senior career professionals
Senior career vascular medicine professionals have assembled a wealth of experience and expertise throughout their careers, positioning themselves as leaders within their organizations and the broader medical community. As mentors and role models, senior professionals play a crucial part in shaping the future of vascular medicine. Critical insights from observing senior career specialists from a mid-career perspective include mentorship, advocacy, strategic leadership, legacy, and impact.8–10
Senior professionals have a responsibility to mentor and advocate for the next generation of vascular medicine specialists, providing guidance, support, and opportunities for professional growth. Mentorship programs within institutions and professional organizations can promote these relationships and ensure continuity within the field.8–10 Effective leadership in vascular medicine requires a strategic vision for advancing patient care, research, and education. Senior professionals must navigate complex institutional dynamics, advocate for resources and support, and champion initiatives that promote excellence and innovation. Senior professionals have the opportunity to consider their legacy and the impact they have had on the field of vascular medicine. Senior professionals have the important responsibility to advocate for the advancement of the field as a whole, including promoting subspecialty recognition, accreditation of training programs, and securing funding for these programs. 11
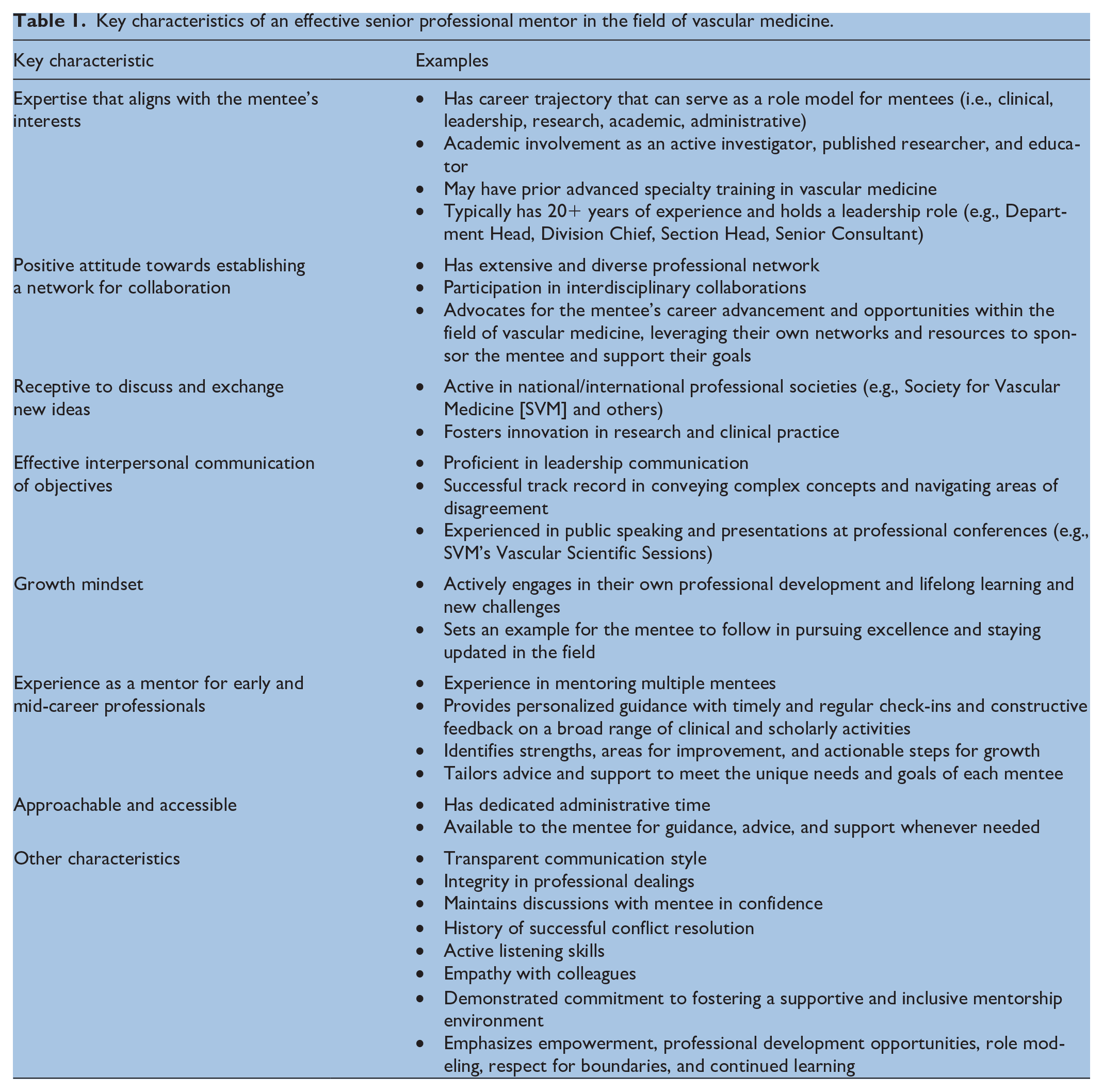
Whether through clinical innovation, research discoveries, or mentorship of future leaders, senior specialists can leave an everlasting imprint on the specialty and inspire generations to come.8–10 Senior professionals can secure vascular medicine’s continued advancement and evolution by assuming their roles as mentors, thought leaders, and advocates for excellence within the field and across disciplines. Key characteristics of an effective senior professional mentor in vascular medicine are described in Table 1.
Key characteristics of an effective senior professional mentor in the field of vascular medicine.
Summary
Like many specialists, becoming a vascular medicine specialist demands perseverance, relentless efforts, dedication, and a willingness to navigate opportunities with resilience and creativity. From the early career stage to senior leadership roles, professionals in this field encounter unique obstacles and opportunities, each shaping their journey and contributions to the specialty. Despite the challenges, such as the lack of recognition at some institutions, by adopting strategies for success through interdisciplinary collaboration, prioritizing ongoing professional development, and leveraging strategic networks and opportunities, specialists can develop a pathway of excellence and make a lasting impact on patient care, research, and education in vascular medicine.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
