Abstract
Infective native aneurysms (INA) of the infrapopliteal arteries are rare and have previously been poorly described. This systematic review aims to provide an overview of the literature of this entity. Furthermore, two case reports of our own clinical experience are presented. PubMed, ScienceDirect, Cochrane, Ovid Embase, Ovid MEDLINE, and Web of Science were searched for articles on INAs of the infrapopliteal segment from January 1990 to September 2023. Article screening and selection were performed adhering to PRISMA guidelines. A total of 98 articles were screened and 20 were eligible for inclusion, of which all were case reports. In total, 22 patients with 28 infrapopliteal INAs were identified. The majority of INAs were located in the tibioperoneal trunk (n = 10, 36%) followed by the posterior tibial artery (n = 7, 25%). A current, or history of, infective endocarditis (IE) was described in 18 out of 22 patients (82%). Two patients died during hospitalization and one patient required a transfemoral amputation. A conservative antibiotic-only approach was chosen in three out of 28 INAs, two of which were the case reports described in this article; surgical or endovascular intervention was performed in 19 out of 28 aneurysms. No complications occurred in the conservative group, but one complication (transfemoral amputation) occurred in the interventional group. Infrapopliteal INA is a rare entity, and most described cases are precipitated by IE. Surgery or endovascular treatment might be indicated, but more research is warranted to define which patient would benefit and by what surgical approach.
Background
Infective native aneurysms (INAs) of the infrapopliteal arteries are rare, and their epidemiology, pathophysiology, microbiology, and management have previously been poorly described.1 –6 INAs of the infrapopliteal segment are considered to develop most often in patients diagnosed with infective endocarditis (IE) as a vascular phenomenon. A proposed theory considers that the aneurysm formation is caused by septic emboli, infecting the arterial wall and leading to destruction of the intima and media layer with subsequent aneurysm formation. 7 INAs of the infrapopliteal arteries can result in both bleeding and ischemia of the lower extremity, which can lead to amputation of the limb, as well as being a continuous source of further infection. The diagnosis is based on a combination of clinical presentation, laboratory findings including culture results, and imaging features on computed tomography (CT) with angiography. 8 This diagnostic algorithm was developed for infective native aortic aneurysms (INAAs) but has also been adopted for peripheral arteries. The ‘Clinical Practice Guidelines on the Management of Abdominal Aorto-iliac Artery Aneurysms’ provided by the European Society for Vascular Surgery recommends treatment for INAs to be constituted by both aggressive antibiotic therapy and surgical repair. 9 For INAs of the infrapopliteal arteries, optimal treatment management is unknown, and due to its rarity the disease is not mentioned in any guidelines. In a review about nontraumatic infrapopliteal aneurysms, 10 cases with an infective origin were identified, where surgical treatment with either ligation and/or bypass grafting was performed in the majority of patients. 1 Since then, several articles have been published about INAs of the infrapopliteal segment; however, not beyond the scope of case reports or narrative reviews.10 –13 We describe two cases of infrapopliteal INAs from our own experience in which a conservative approach was chosen, as opposed to most cases described in current literature. Both patients reported in this study provided formal consent for the information described in the presented case reports. Furthermore, we performed a systematic literature review to provide an overview of the epidemiology of infrapopliteal INAs regarding pathophysiology, microbiology, and details on management and respective outcome.
Case report #1
A 42-year-old male patient with a history of previous cryptogenic cerebral bleeding, a known bicuspid aortic valve, and active smoking presented with a 1-month history of generalized joint pain, insomnia, night sweats, and weight loss. On physical examination, the patient was pale, but without fever. Laboratory results demonstrated leukocytosis of 13.1*109/L, C-reactive protein of 89 mg/L, and a hemoglobin value of 6.8 mmol/L. On day 1 following hospital admission, he complained about pain in the right calf, which was already present 2 months earlier but duplex ultrasound at the time did not provide a diagnosis. On physical examination, there was severe tenderness in the calf region, which was warmer compared to the left side. Repeated ultrasound of the right leg was performed and demonstrated deep venous thrombosis of the fibular vein. On the third day, blood cultures were positive for Streptococcus mutans, and benzylpenicillin and gentamycin intravenously were started. Transesophageal echocardiography demonstrated both mitral and aortic valve vegetations. A positron emission tomography scan was performed, showing signs of a possible infected hematoma in the right calf. Subsequent computed tomography angiography (CTA) of the right leg demonstrated an aneurysmatic dilation of the tibioperoneal trunk of up to 9 mm, with patent posterior tibial and peroneal arteries (Figure 1). Physical examination of the foot revealed good perfusion with a palpable posterior tibial artery and an ankle–brachial index (ABI) of 1.30. Since the symptoms of the leg had been present for 2 months without deterioration, conservative management of the INA was chosen. The patient had a fast recovery following antibiotic treatment, which was terminated after 6 weeks. Duplex ultrasound of the leg 3 weeks and 5 months after discharge demonstrated no signs of aneurysm growth. Three months following discharge, the patient had made a full recovery and had returned to work.
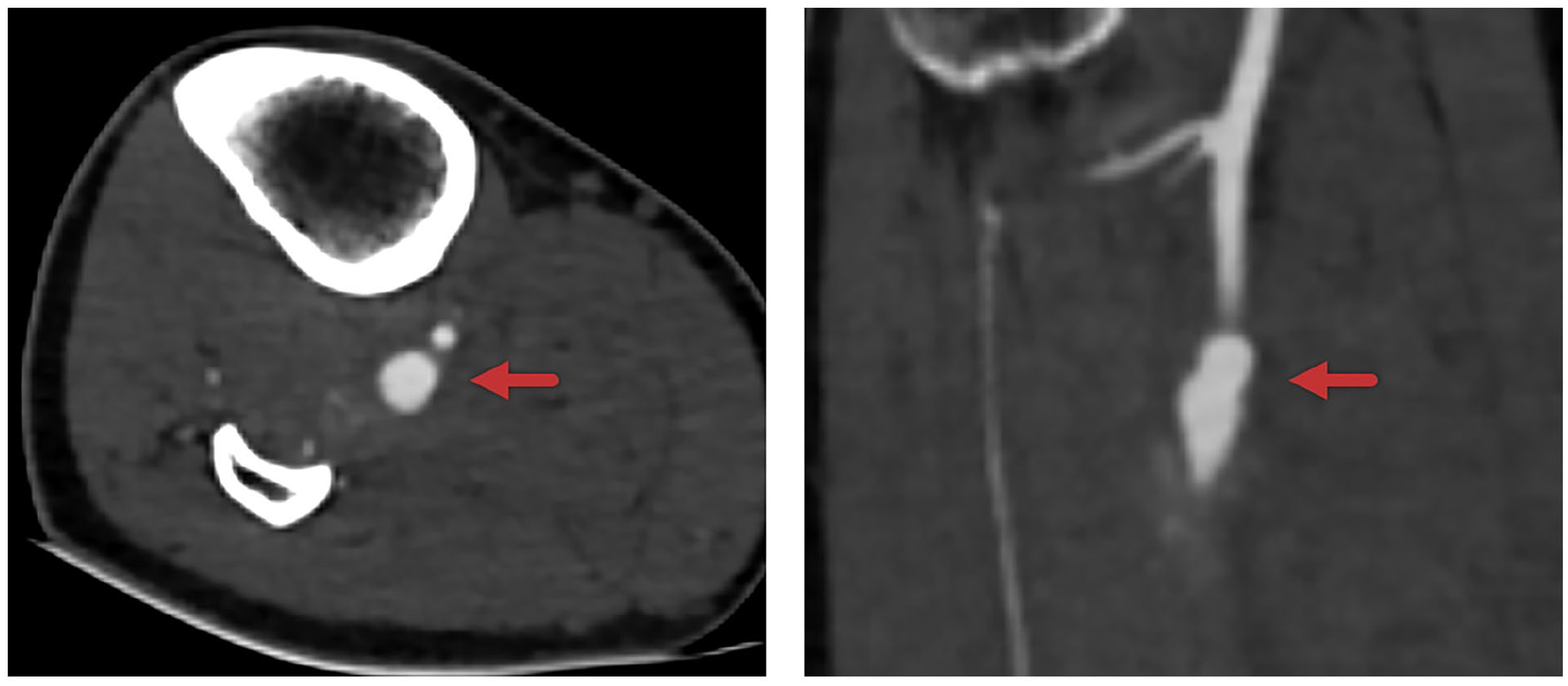
Case #1: Computed tomography angiography demonstrating the transverse (left panel) and coronary (right panel) views of the tibioperoneal trunk aneurysm (arrows) on the right side.
Case report #2
A 55-year-old man with a history of Brugada syndrome, paroxysmal atrial fibrillation and a recent arthroscopy of the knee was admitted to the hospital with fever, cough, and pain in both shoulders. Physical examination revealed no abnormalities. Leukocyte count and C-reactive protein (CRP) were 10.9 × 109/L and 191 mg/dL, respectively. Since there was no focus for his fever, empiric intravenous antibiotic therapy with piperacillin and tazobactam was started. One out of three blood cultures retrieved at admission revealed growth of Staphylococcus aureus. Initially, there was good clinical response on antibiotic treatment, which was withdrawn after 5 days. Five days after this the patient was readmitted with a high fever and increasing pain, during which a transthoracic echocardiography demonstrated vegetation of the mitral valve. Piperacillin and tazobactam were started again, and switched to cefuroxime and rifampicin the same day. Three weeks into treatment the patient experienced a sudden onset of pain in his left lower leg. On physical examination, there were no signs of swelling and the foot was clinically well perfused with palpable pulses on the posterior tibial and dorsal pedis arteries. Duplex ultrasound showed no signs of deep venous thrombosis. A CTA was performed to rule out septic emboli, and showed an aneurysmatic dilatation of the proximal peroneal artery of 15 mm (Figure 2). There was adequate outflow distally. Since there were no signs of ischemia or bleeding, a conservative approach was considered appropriate. The pain in his leg gradually improved, and a CTA 9 days later demonstrated no signs of aneurysm enlargement. The antibiotic treatment was terminated after 6 weeks. Duplex ultrasound 4 months following diagnosis demonstrated no signs of aneurysm growth. The patient remains free from symptoms at 1 year following discharge and has fully recovered.
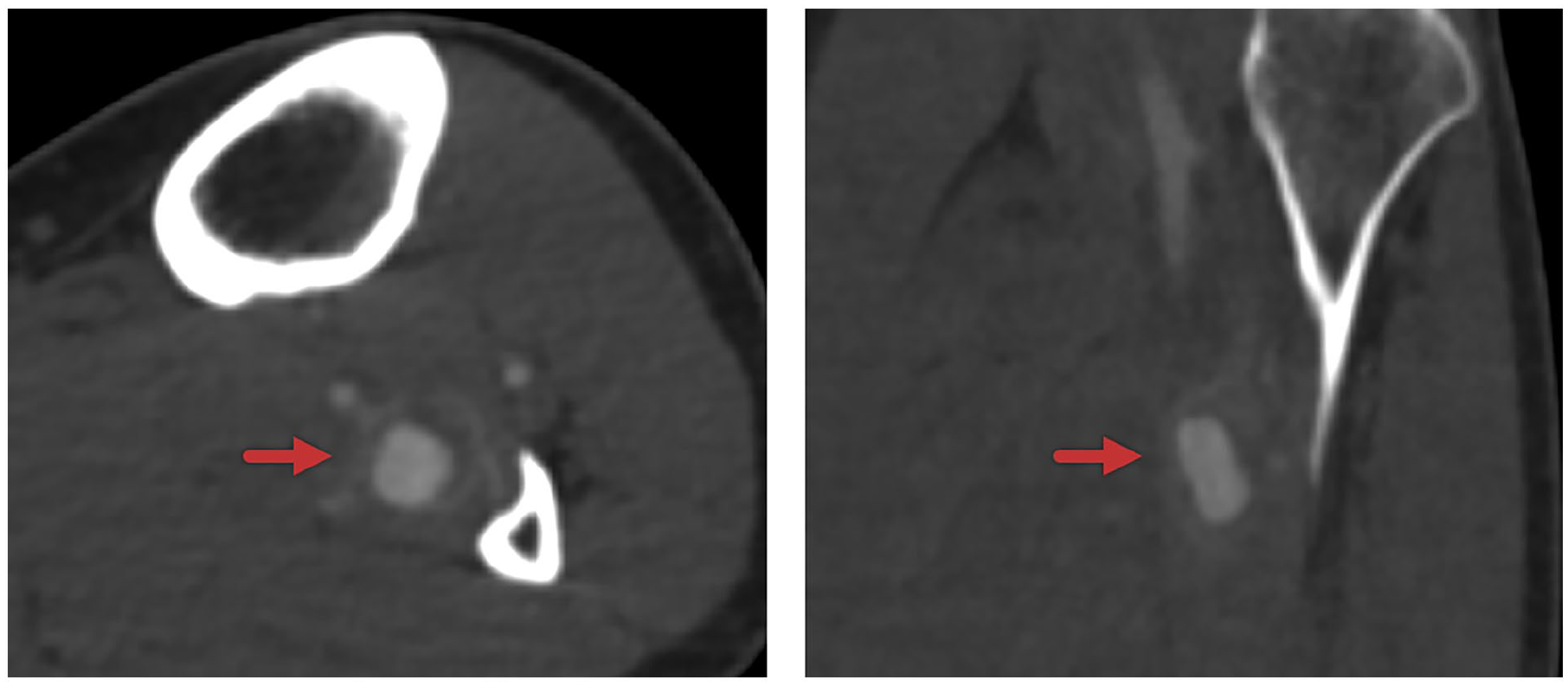
Case #2: Computed tomography angiography demonstrating the transverse (left panel) and coronary (right panel) views of the peroneal artery aneurysm (arrows) on the left side.
Methods
Search strategy
A systematic review of the literature was performed, adhering to PRISMA guidelines for the report on systematic review. 14 PubMed, ScienceDirect, Cochrane, Ovid Embase, Ovid MEDLINE, and Web of Science were searched for articles on infrapopliteal INAs from January 1990 to September 2023. The search strategy included ‘infected aneurysm’ or synonyms (infective aneurysm, bacterial aneurysm, mycotic aneurysm) in combination with arterial localization (online supplementary material: Appendix A). The term INA was introduced in an international consensus Delphi study published in 2023, which is why this term was not used in the literature search, only older synonyms and misnomers. 8 Only full text articles in English were included. Reference lists of included studies were scrutinized to identify additional literature that fulfilled the inclusion criteria and could be included. Articles were screened for eligibility according to the PRISMA guidelines. The article search was conducted by one researcher (PH) and was validated by another researcher (KS). Quality assessment of included articles was performed by PH and KS using the methodological index for non-randomized studies (MINORS) score. 15 Each article was given a grade according to the final score: low < 12; medium 12–15, and high = 16. Quality assessment was not used as exclusion criteria.
Article selection, data extraction, and aims
Article selection and assessment of articles rendered by the search was carried out by two researchers (PH and KS). In case of disagreement between investigators, this was resolved by discussion with other co-authors (EF and OL) until a consensus could be reached. Articles describing the clinical experience with an infrapopliteal infective native aneurysm were included. Studies or case reports on infected grafts of the lower limb were excluded, since this is another disease entity. Review articles were excluded after scrutiny, unless there was a description of a patient with an infective infrapopliteal aneurysm. Article data were extracted following a predefined protocol on patient characteristics: age, sex, symptoms (pain, fever, swelling, other), recent or ongoing concomitant infection, laboratory results (white cell blood count, CRP, and culture results), and imaging results (ultrasound, computed tomography with angiography), aneurysm anatomical localization and characterization including rupture, details on surgical and antibiotic treatment, and outcome (survival, development of infection-related complications [IRC; sepsis, new infective aneurysm, graft infection, or fistulation], amputation, bleeding, need for revised management plan). The aims of the study were to describe the epidemiology, pathophysiology, microbiology, and anatomical location of INA of the infrapopliteal arteries, and to report management with respective outcome, as well as report our experience with a conservative management approach. Both the cases rendered with the systematic literature search as well as the two case reports from our own clinical experience were included in the analysis.
Statistics
Data were assessed for normality with histograms, and continuous data were summarized as median (IQR) or mean (SD) and categorical variables as proportions (%). Age was described as median with IQR.
Results
Search results, quality assessment, and patient characteristics
The literature search rendered a total of 98 articles, of which 20 were eligible for inclusion in this systematic literature review (for details see Figure 3 and Table 1). All the included studies were case reports, each describing a single patient either with single or multiple infrapopliteal infective native aneurysms. The median MINORS score was 1, which ranged from 1 to 3. Together with the two patients from our own clinical center, a total of 22 patients were thus identified as having at least one INA of the infrapopliteal segment (Table 2). The total cohort had a median age of 50.5 years (25th and 75th percentile, 42 and 59 respectively) and three were female patients (14%). Follow up ranged from 0 to 138 weeks (median 21 weeks). Concomitant or recent infection was present in all patients; IE in 18 (82%), localized foot infection in two (9%), knee prosthesis infection in one (5%), and fever with unknown origin in one (5%). The most frequently reported symptoms included pain (n = 16, 73%) and swelling (n = 16, 73%). Three patients (14%) suffered from aneurysm rupture. Multiple infective infrapopliteal artery aneurysms were reported in four patients (18%), resulting in a total report of 28 INAs in 22 patients.
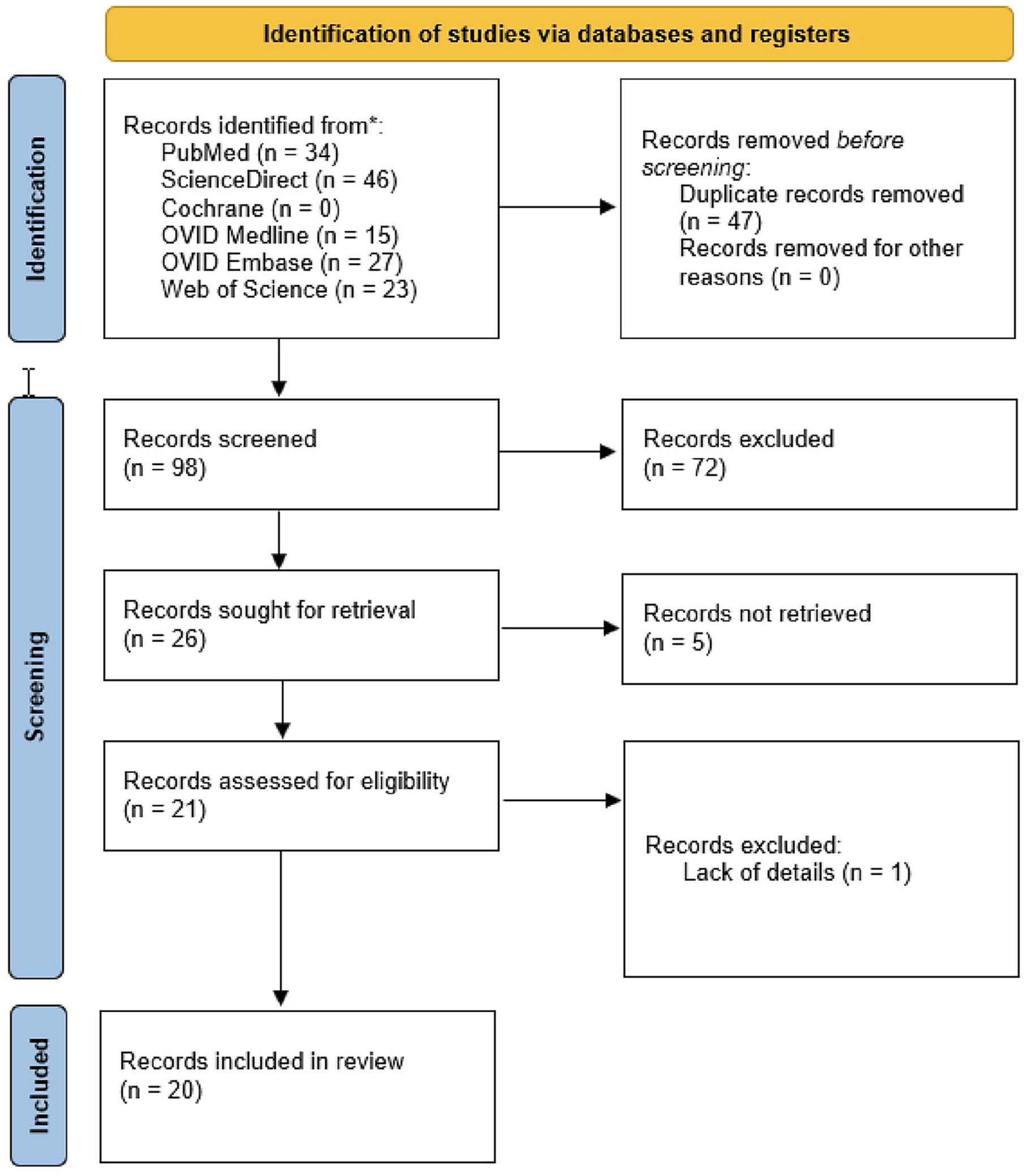
Flowchart of study selection according to PRISMA guidelines.
List of included studies with respective quality assessment.
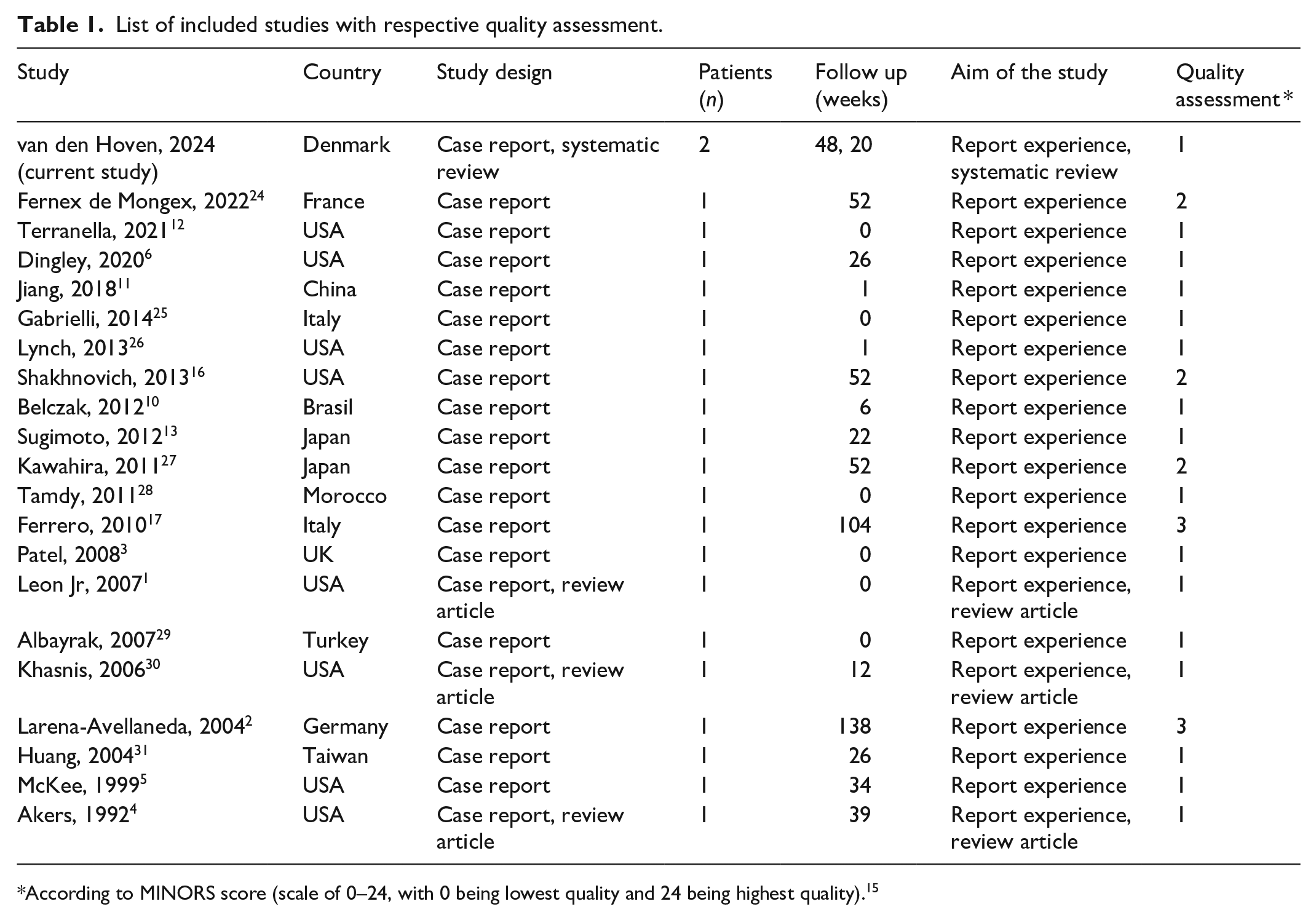
*According to MINORS score (scale of 0–24, with 0 being lowest quality and 24 being highest quality). 15
Patient characteristics, culture results, and anatomical location of the infective native aneurysms.

INA, infective native aneurysm.
Anatomical location and microbiology
Of the 28 reported INAs, the most common localization was the tibioperoneal trunk (n = 10; 36%), then the posterior tibial artery (n = 7, 25%) and a pedal artery (n = 4, 14%). Diagnosis was confirmed mostly using CTA, followed by magnetic resonance angiography (MRA), duplex ultrasound, and angiography (Table 2). These aneurysms were diagnosed during an episode of active infection in 16 out of 22 patients (73%). The remaining six patients presenting without an active infection all reported a history of IE in the years precipitating the INA diagnosis, ranging from 5 months to 8 years. Staphylococcus aureus and Streptococcus sp. were the most commonly identified micro-organisms in blood cultures taken at the time of the suspected precipitating infection (Table 2). Other isolated micro-organisms in blood cultures were predominantly bacterial, with only one case of fungus, Candida albicans. Local cultures taken from the aneurysm site during surgery were negative in more than half of cases, three of which had already started antibiotic treatment prior to surgery, whereas the other two cases had no signs of active infection.
Treatment and outcome
An intervention was performed in 19 out of 28 INAs (68%) (Table 3). Intervention consisted of either ligation with or without excision in nine (32%) INAs, excision with reconstructive bypass in eight (29%), coiling of the aneurysm in one (4%), and thrombin injection in one (4%). The six patients without active infection were all treated surgically, without any complications during follow up. Indications for repair in these six patients included rupture (n = 2, 7%), pain (n = 3, 11%), and marked swelling (n = 1, 4%). The patient who was successfully treated with thrombin injection presented with an INA of the dorsal pedis artery and had an uncomplicated course without need for further intervention. Two patients were not treated surgically due to severe IE, both of whom died due to their infections. Above the knee amputation was necessary in one patient who had a ruptured INA of the posterior tibial artery, caused by a lengthy, complicated course of an infected prosthetic knee joint. No limb loss or mortality was encountered in all other reported cases. Antibiotic treatment management was documented in 15 out of 22 patients (68%). In five out of the 16 patients with an active systemic infection, information about antibiotic treatment was absent.
Description of different treatments and respective outcome for infective native aneurysms of the infrapopliteal arteries described in the literature.
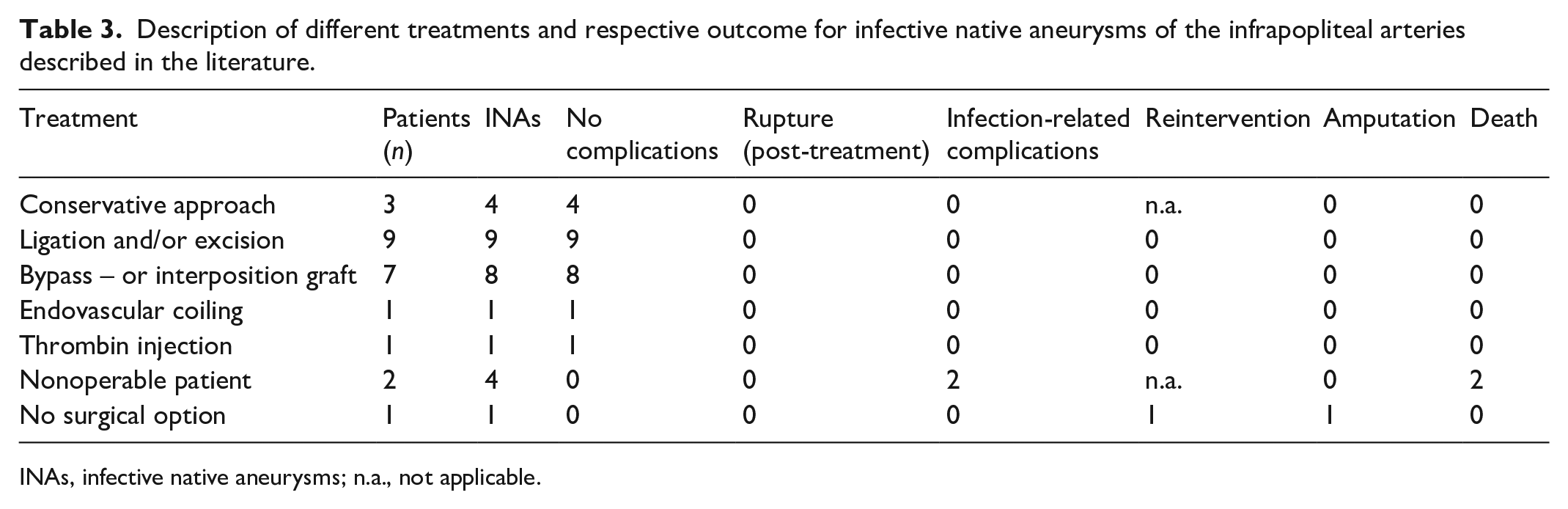
INAs, infective native aneurysms; n.a., not applicable.
Discussion
This is the first systematic review on INA of the infrapopliteal segment, demonstrating several important findings. First, the vast majority of INAs of the infrapopliteal segment predominantly affect men and are precipitated by infective endocarditis. Second, it underlines the low evidence on this entity or at least its low reporting in the literature with only 21 previously reported cases. Third, a significant number of patients presented with a delay in clinical diagnosis, which could indicate that aneurysm progression occurs despite active infection.3,4,6,16,17 Therefore, patients with a history of IE presenting with lower-extremity symptoms including pain and swelling should be carefully examined with INAs in mind. Last, documented surgical treatment consisted mostly of aneurysm ligation, in which nearly half of the patients had no indication for vascular reconstruction due to intact collateral circulation of the foot. Consequently, conservative management of INAs of the infrapopliteal segment with antibiotic treatment only (without surgery), under strict surveillance, seems appealing. Key to successful management is probably to manage these patients in a multidisciplinary team, including cardiologists, vascular surgeons, and specialists in either infectious disease and/or microbiology. Our findings reveal that INA of the infrapopliteal segment are associated with a significant morbidity burden. Out of the 22 patients included in the study, two patients died during hospitalization and one patient required a transfemoral amputation due to aneurysm rupture. Both patients who succumbed due to their infections were diagnosed with IE, which is associated with considerable mortality rates. 18 The anatomical localization most commonly affected was the tibioperoneal trunk, even though the entire infrapopliteal arterial circulation is at risk of being affected. This finding supports the theory that emboli most commonly follow the straight circulation, and lodges in narrowings such as bifurcations. 13 Although various methods for diagnosis were utilized, it is known that MRA yields the highest sensitivity for imaging of the infrapopliteal arteries, and therefore seems preferable. 19 INA of the infrapopliteal segment may be caused by a variety of microorganisms, almost exclusively by Gram-positive bacteria. Staphylococci and Streptococci were predominant in this study, which is in accordance with the microbiological etiology of native and prosthetic IE. In IE, however, Enterococcus are also frequently encountered, which was not found as an etiology of INA of the infrapopliteal segment. 20 Overall, patients with an infrapopliteal INA in combination with active IE were treated with intravenous antibiotics, most commonly with a duration of 6 weeks which adheres to current clinical guidelines on infective endocarditis. 21 Whether treatment should be prolonged in the presence of a peripheral INA is unclear; however, no extended antibiotic regimens were reported in the present study, and no patient developed any late IRCs. However, one patient with a blood culture positive for C. albicans received prolonged antifungal treatment. 2 Indications for surgery differed among patients, but mainly symptomatic INAs – including rupture – or INAs with active systemic infection were treated surgically. In the case of a rupture and uncontrolled bleeding, surgical treatment is imperative. Interestingly, only one patient was treated with endovascular coiling. An endovascular strategy should be kept in mind, especially since a considerable number of the patients in the current study were successfully treated with ligation without need for revascularization or amputation. Compared with INAs of the femoral artery, it is arguable that the bacterial load in an INA of the infrapopliteal segment is significantly lower.22,23 Therefore, as long as collateralized distal perfusion is assured, endovascular occlusion of an infrapopliteal artery aneurysm might be a considerable alternative. In the two cases presented by the authors, there were no signs of ischemia or rupture. A conservative management with antibiotic treatment only in these patients was chosen, but with close follow up – including duplex ultrasound imaging. Although limited by a short follow up, both remain free from symptoms, and none has developed any signs of aneurysm progression or has needed a revision of treatment plan.
Limitations for the present systematic review are inevitably present, the foremost being the low number of reported cases, and the low quality of included studies, precluding a comparative analysis and meta-analysis. Furthermore, documentation on follow up was often scarce and, therefore, long-term outcomes could not be reliably assessed. This could be overcome by adhering to a systematic reporting of INAs at any anatomical location to provide further insights of the disease, including information about patient demographics, microbiological pathogens, overall management including surgical treatment and antimicrobial treatment, and detailed follow up including aneurysm size, progression, IRCs, amputation, and bleeding. The reporting standards proposed for INAs of the aorta could be used and amended for this purpose.
Conclusion
Infrapopliteal infective native aneurysm is a rare entity, and most described cases seem to be precipitated by infective endocarditis. Management should be tailor-made for each individual patient. Surgery or endovascular treatment might be indicated in some cases, but more research is warranted to define which patient would benefit and by what surgical approach.
Supplemental Material
sj-pdf-1-vmj-10.1177_1358863X241245417 – Supplemental material for Infective native aneurysms of the infrapopliteal arteries – A systematic literature review and report of two cases
Supplemental material, sj-pdf-1-vmj-10.1177_1358863X241245417 for Infective native aneurysms of the infrapopliteal arteries – A systematic literature review and report of two cases by Pim van den Hoven, Emil Fosbøl, Oskar Ljungquist and Karl Sörelius in Vascular Medicine
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplementary material
The supplementary material is available online with the article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
