Abstract

A 63-year-old man with a history of hypertension, hyperlipidemia, and dyslipidemia was admitted to our hospital, complaining of intermittent claudication of the right lower limb while walking within a distance of 100 meters, which was consistent with a Rutherford classification of grade I-2. Computed tomographic angiography (CTA) showed chronic total occlusion in his right superficial femoral artery. We performed femoropopliteal bypass with the autologous saphenous vein. One week after surgery, CTA revealed a heart-shaped pseudoaneurysm in the saphenous vein graft (Panel A).
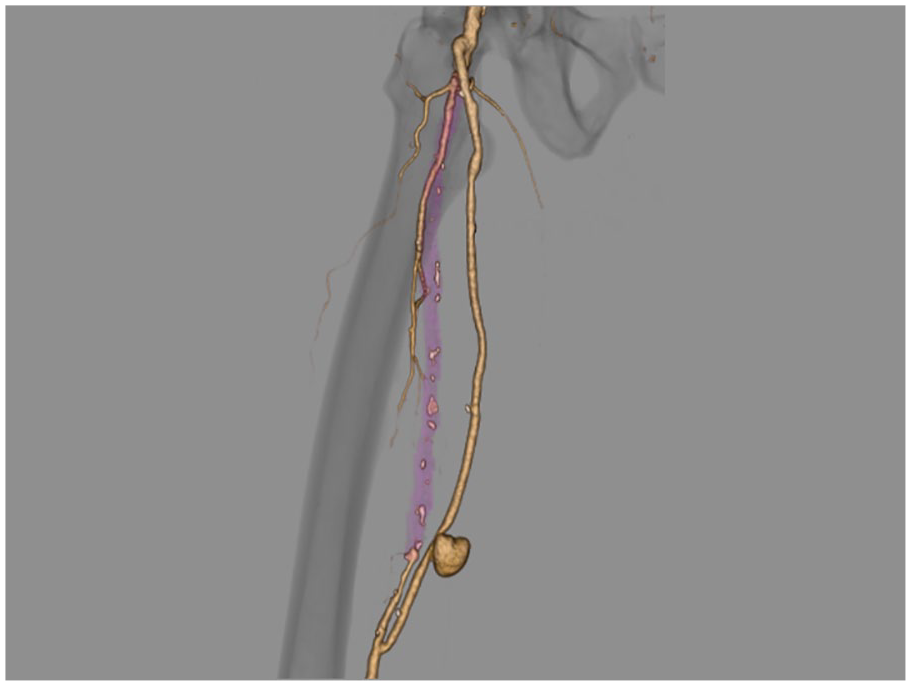
The patient refused to undergo open surgical repair; therefore, we performed percutaneous transluminal angioplasty. We deployed a GORE VIABAHN 5 × 10 cm covered stent (W. L. Gore & Associates, Flagstaff, AZ, USA), which provided coverage of the heart-shaped pseudoaneurysm (Panel B-1). The final angiogram showed excellent results of the bypass graft, without endoleaks (Panel B-2). After the procedure, CTA demonstrated the heart-shaped pseudoaneurysm had disappeared (Panel C). Three years after the operation, the GORE VIABAHN stent and vein graft remained patent.
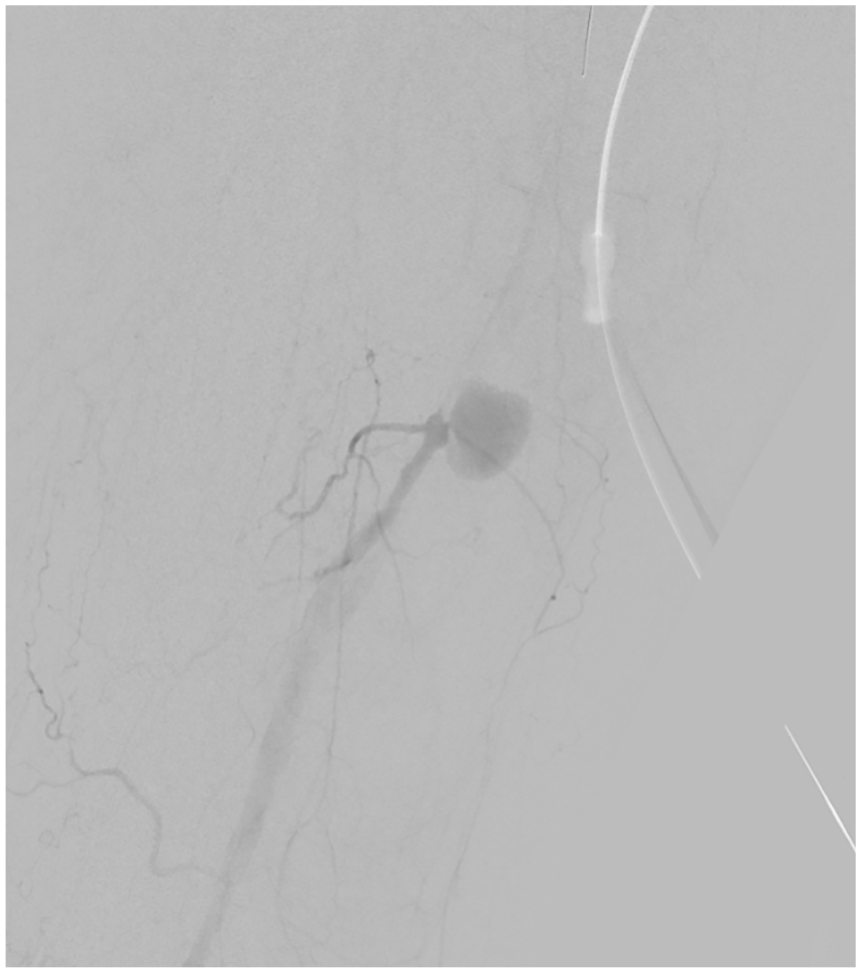
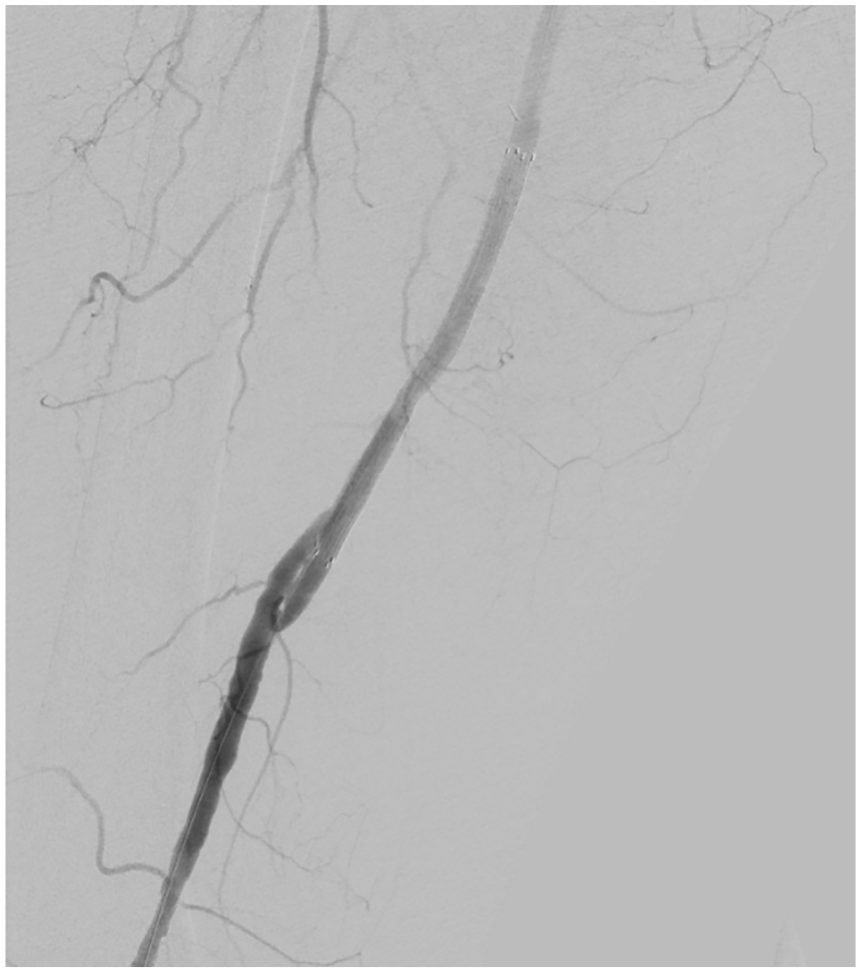
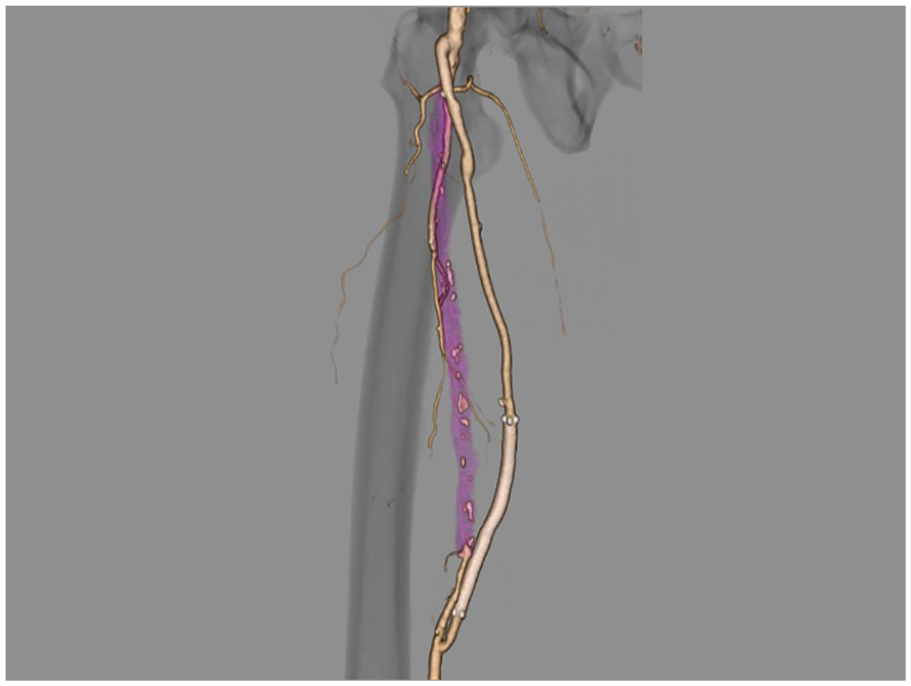
Previous studies have demonstrated that endovascular revascularization of infrainguinal graft stenosis is safe and associated with acceptable early and medium-term patency rates. 1 According to another report, placing a GORE VIABAHN stent inside the occluded prosthetic bypass graft appears to be effective in the treatment of prosthetic above-knee femoropopliteal bypass occlusion. 2 In contrast, very few studies have demonstrated the utility of endovascular therapy for vein bypass graft pseudoaneurysm. 3 The clinical usefulness of stents in infrainguinal vein grafts is not yet established, and their safety and efficacy remain unclear. However, the case we have described, as evidenced in Panel C, demonstrates the utility of such a stent in the infrainguinal region, even for pseudoaneurysms with unusual shapes.
‘Images in vascular medicine’ is a regular feature of Vascular Medicine. Readers may submit original, unpublished images related to clinical vascular medicine. Submissions may be sent to: Heather Gornik, Editor in Chief, Vascular Medicine, via the web-based submission system at http://mc.manuscriptcentral.com/vascular-medicine
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
