Abstract

A 75-year-old woman presented to our department with a 9-month history of resistant grade 3 hypertension and progressive intermittent claudication of the lower limbs. Despite triple therapy, a recent 24-hour outpatient blood pressure monitor showed high daytime (143/88 mmHg) and night-time (131/81 mmHg) averages. Her history was significant for chronic obstructive pulmonary disease in an active smoker. Physical examination showed weakened femoral pulses and the ankle–brachial index was 0.5. Laboratory tests revealed worsening renal function: blood creatinine value of 2 mg/dL and estimated glomerular filtration rate of 24.3 mL/min/1.73 m2. The electrocardiogram demonstrated sinus rhythm with no pathological findings relevant at echocardiography.
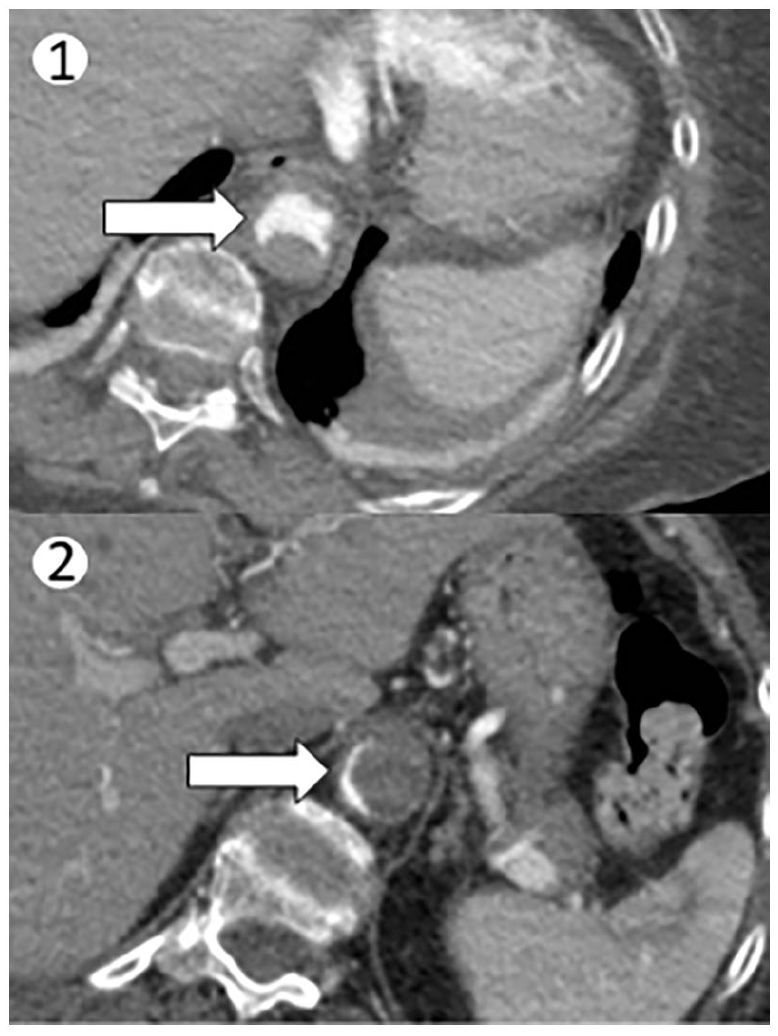
Suspecting secondary hypertension, a computed tomography angiogram (CTA) of chest (Panel A-1) and abdomen (Panel A-2) was performed, revealing ectasia of thoracic aorta with extensive thrombotic apposition. These findings involved the descending tract of the aorta and extended up above the emergence of the celiac tripod, showing a severely ulcerated wall causing subtotal vessel occlusion with opacification of the residual lumen (Panel A: arrow) in the filiform posterior marginal site (Panel A: arrows). The superior mesenteric, celiac axis, renal, and inferior mesenteric arteries were atheromatous but patent.
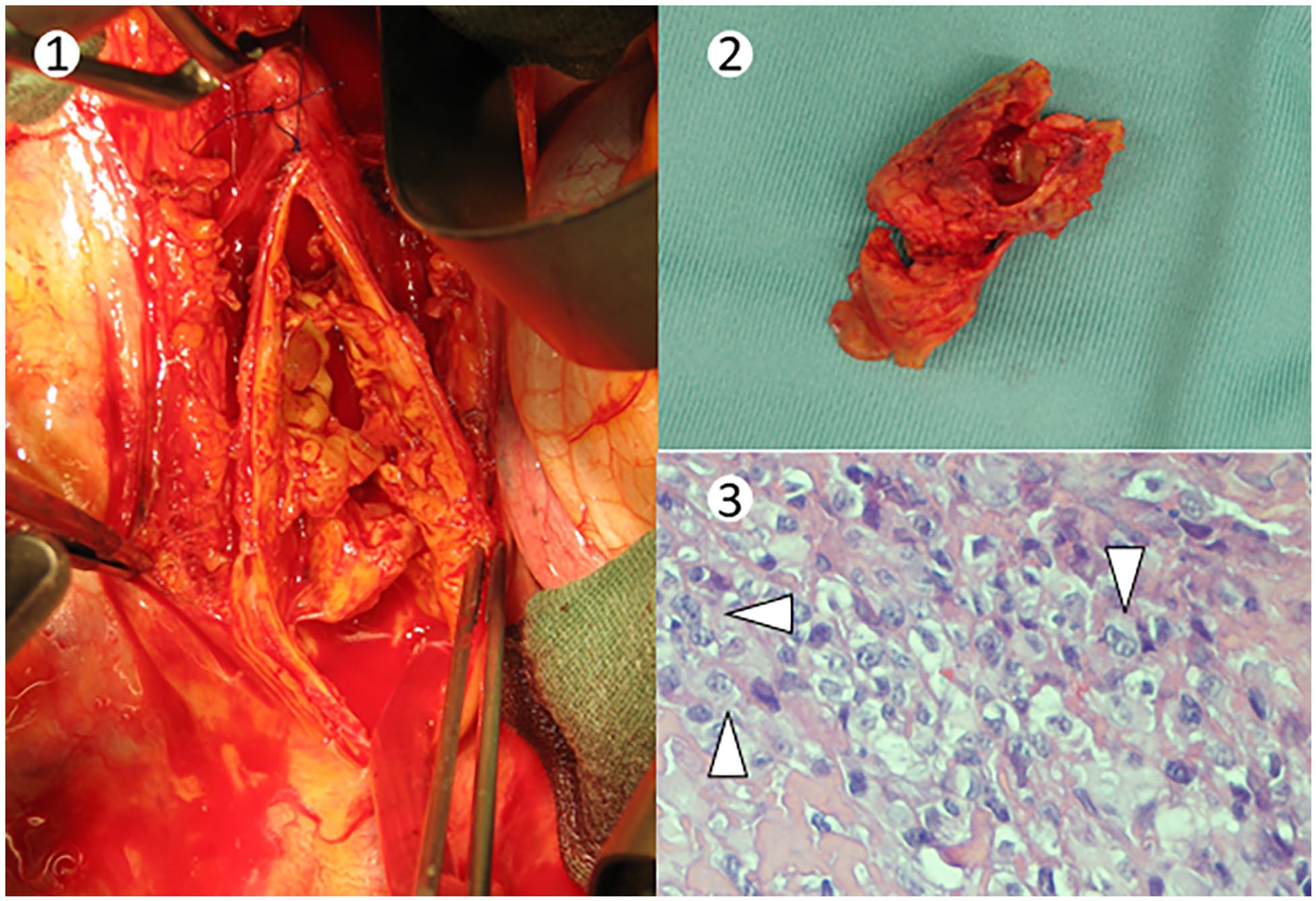
Catheter-directed thrombolytic therapy was attempted, with no significant clinical improvement; therefore, a surgical thoracotomy was required. During surgery (Panel B-1), the occluding material was not compatible with thrombosis: a hyaline and lipoid membranous material was removed (Panel B-2). Examination of the specimen diagnosed epithelioid angiosarcoma. Histological examination showed neoplastic cells with large nuclei and prominent nucleoli (Panel B-3: arrowheads; original magnification ×40), occasional intracytoplasmic lumens, and scattered mitotic figures. After surgery, hypertension was within limits and medications were reduced; after rehabilitation, the claudication disappeared.
Mid-aortic syndrome is uncommon and is caused by a narrowing of the abdominal and/or thoracic segment of the aorta. 1 It is found more frequently in children and young adults, with underlying structural malformations of the aortic wall; patients develop resistant hypertension associated with claudication or intestinal signs of ischemia. Primary tumors of the aorta, such as angiosarcomas, are also rare, and diagnosis is challenging, especially in elderly patients with concomitant atherosclerotic disease; besides the suspicion, histopathological confirmation is mandatory. 2 As in the case described, thrombosis plays a crucial role: it could be a mimic, a local complication, or both, and requires tailored management. 3
‘Images in vascular medicine’ is a regular feature of Vascular Medicine. Readers may submit original, unpublished images related to clinical vascular medicine. Submissions may be sent to: Heather Gornik, Editor in Chief, Vascular Medicine, via the web-based submission system at http://mc.manuscriptcentral.com/vascular-medicine
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
