Abstract

A 60-year-old male was admitted to our department due to a painful right lower limb, associated with pulsatile edema from the mid-thigh to proximal leg, fever and rapid clinical deterioration. He had had a recent hospitalization due to diarrhea, which improved after hydration and intravenous empirical antibiotic therapy. His medical history was notable for chronic heart failure, hypertension, smoking, hypercholesterolemia, and diabetes mellitus type 2, which was poorly controlled. Duplex ultrasonography showed arterial dilatation above and below the right knee. A computed tomography (CT) angiography scan displayed a ruptured popliteal aneurysm (Panel A, arrow) with extravasation into the soft tissues and massive local emphysema (Panels A and B) within the right popliteal fossa and distal femur (Panel C, arrowhead). The maximum diameter was 2.7 cm. The 3D reconstruction identified the exact point of rupture with plaque disruption (Panel D, arrow). The patient underwent a surgical procedure where the distal superficial femoral artery was ligated, the aneurysm was excluded and the affected artery resected. Blood flow was restored through an internal saphenous vein bypass. The patient died due to acute myocardial infarction on the eighth postoperative day. Blood culture was positive for Salmonella sp., as well as the culture of thrombus and aneurysm wall. These findings indicated a probable relation of his prior diarrhea to Salmonella and the subsequent aneurysm infection and rupture.
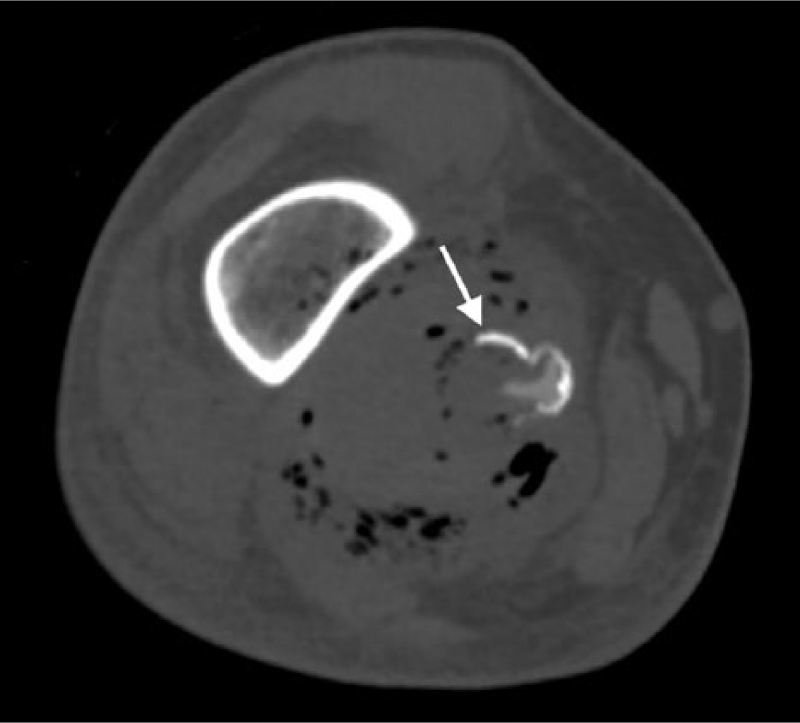
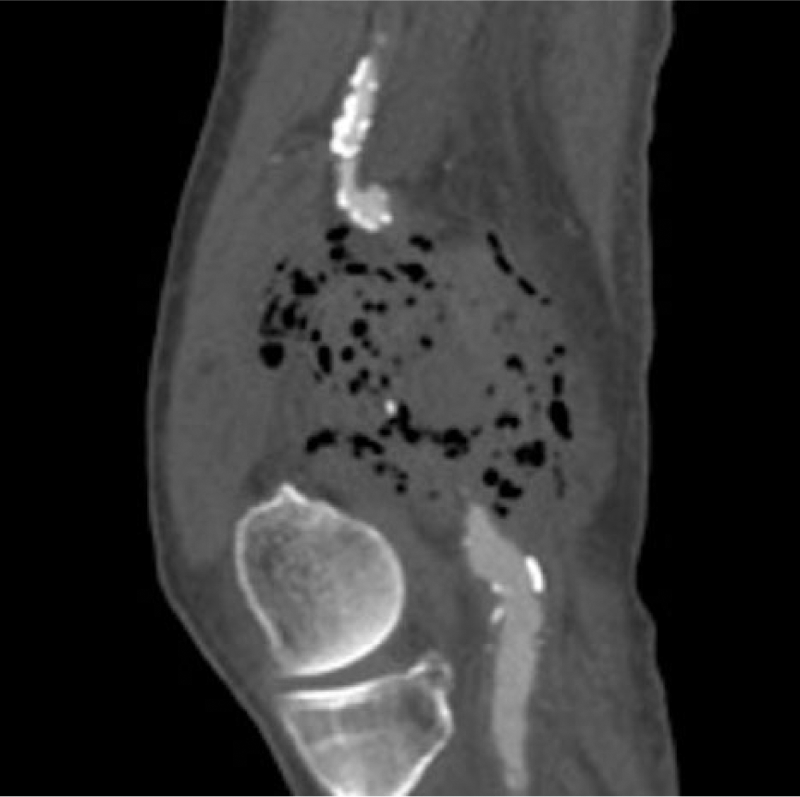
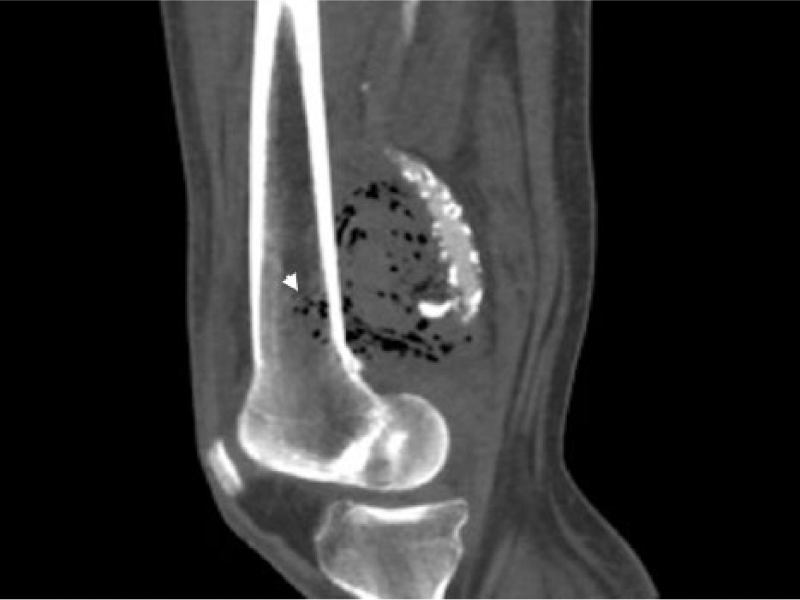
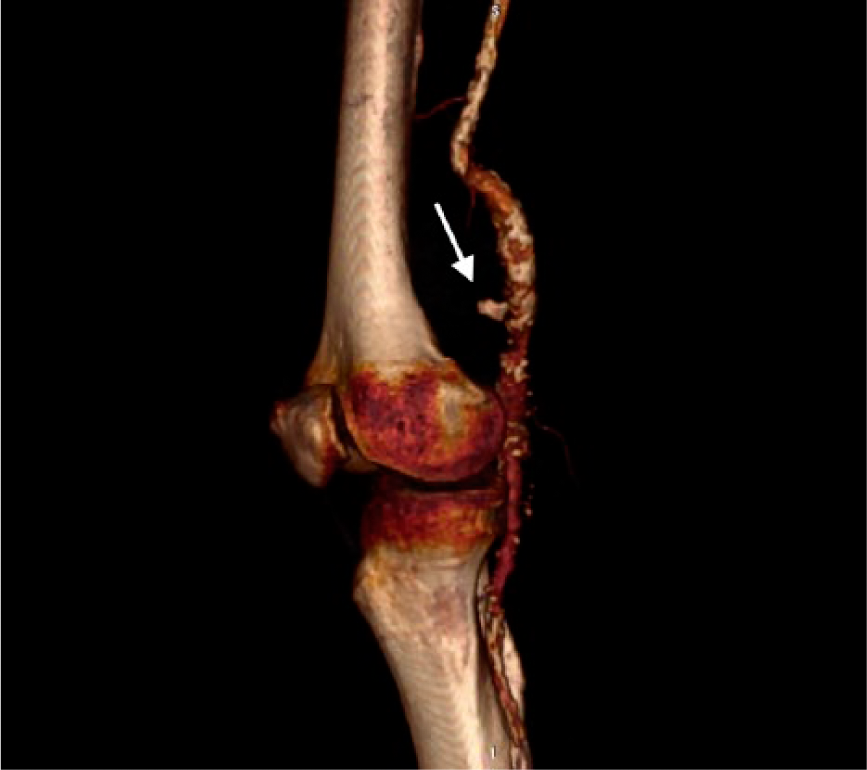
Popliteal artery aneurysms are the most prevalent peripheral aneurysms. 1 The most common complications are thromboembolic followed by compression of adjacent structures and rupture; 2 rupture caused by infection is an even rarer event 3 (a few cases have been reported in aneurysmal popliteal arteries and one case in a non-aneurysmal artery). However, a case with extensive emphysema has not been described to date.
‘Images in vascular medicine’ is a regular feature of Vascular Medicine. Readers may submit original, unpublished images related to clinical vascular medicine. Submissions may be sent to: Heather Gornik, Editor in Chief, Vascular Medicine, via the web-based submission system at http://mc.manuscriptcentral.com/vascular-medicine
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
