Abstract
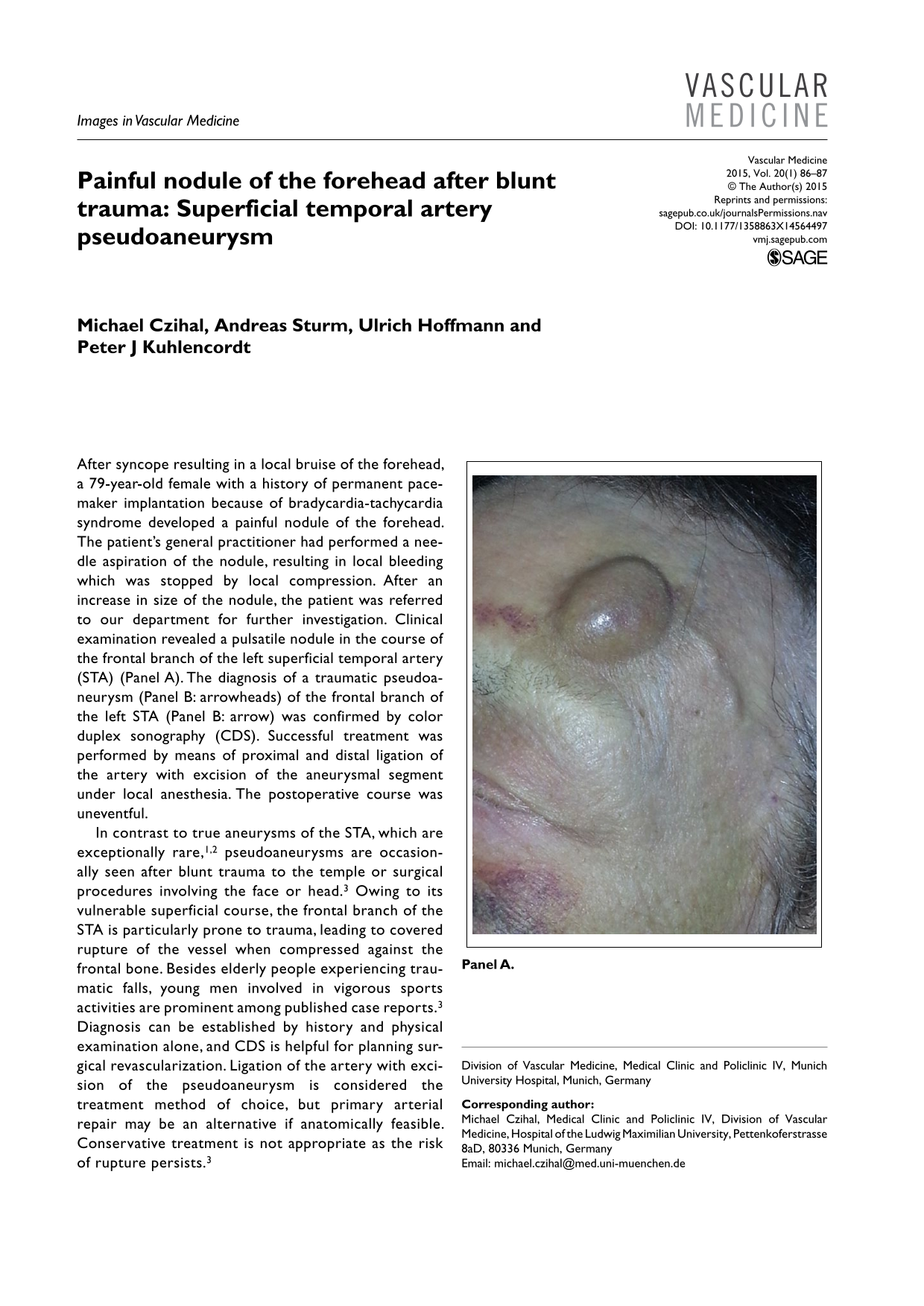
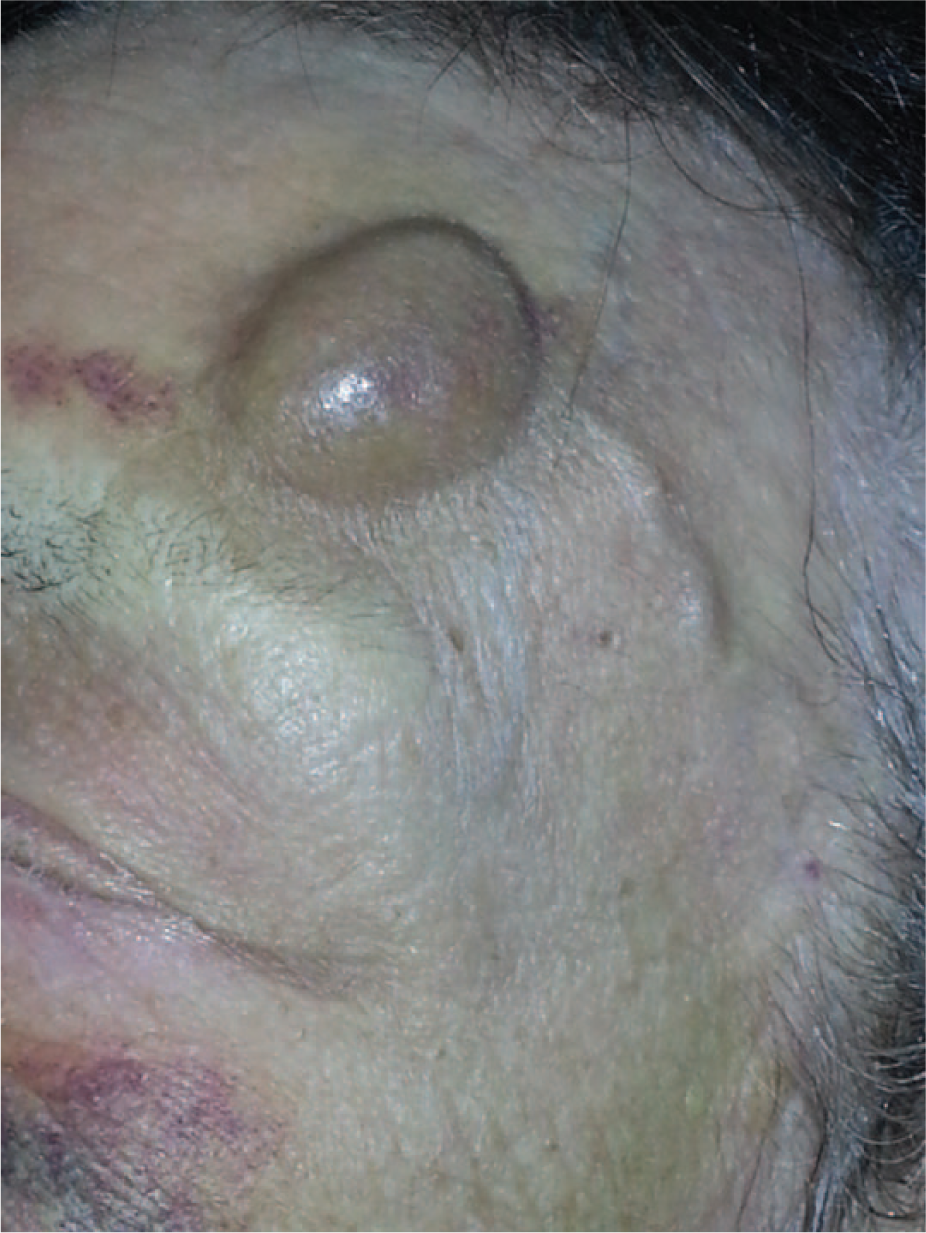
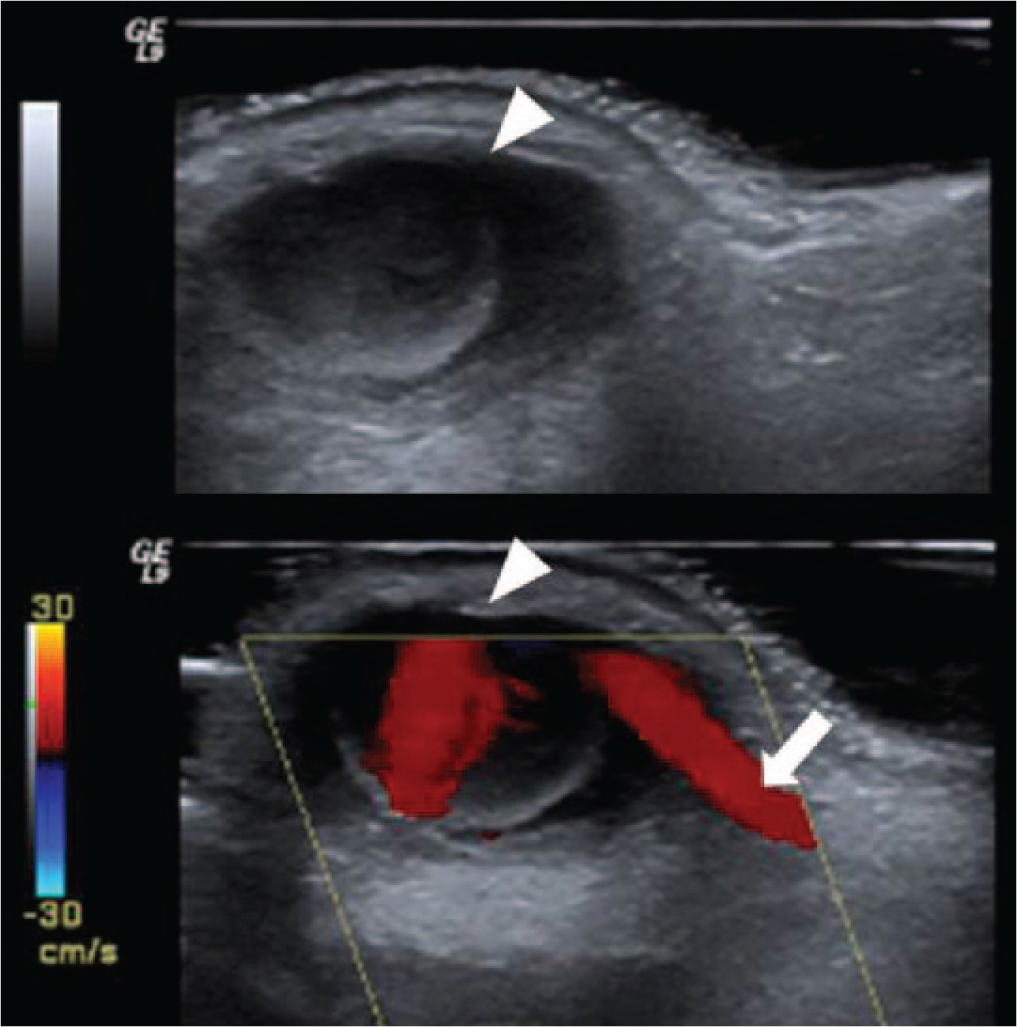
After syncope resulting in a local bruise of the forehead, a 79-year-old female with a history of permanent pacemaker implantation because of bradycardia-tachycardia syndrome developed a painful nodule of the forehead. The patient’s general practitioner had performed a needle aspiration of the nodule, resulting in local bleeding which was stopped by local compression. After an increase in size of the nodule, the patient was referred to our department for further investigation. Clinical examination revealed a pulsatile nodule in the course of the frontal branch of the left superficial temporal artery (STA) (Panel A). The diagnosis of a traumatic pseudoaneurysm (Panel B: arrowheads) of the frontal branch of the left STA (Panel B: arrow) was confirmed by color duplex sonography (CDS). Successful treatment was performed by means of proximal and distal ligation of the artery with excision of the aneurysmal segment under local anesthesia. The postoperative course was uneventful.
In contrast to true aneurysms of the STA, which are exceptionally rare,1,2 pseudoaneurysms are occasionally seen after blunt trauma to the temple or surgical procedures involving the face or head. 3 Owing to its vulnerable superficial course, the frontal branch of the STA is particularly prone to trauma, leading to covered rupture of the vessel when compressed against the frontal bone. Besides elderly people experiencing traumatic falls, young men involved in vigorous sports activities are prominent among published case reports. 3 Diagnosis can be established by history and physical examination alone, and CDS is helpful for planning surgical revascularization. Ligation of the artery with excision of the pseudoaneurysm is considered the treatment method of choice, but primary arterial repair may be an alternative if anatomically feasible. Conservative treatment is not appropriate as the risk of rupture persists. 3
‘Images in vascular medicine’ is a regular feature of Vascular Medicine. Readers may submit original, unpublished images related to clinical vascular medicine. Submissions may be sent to: Heather Gornik, Editor in Chief, Vascular Medicine, via the web-based submission system at http://mc.manuscriptcentral.com/vascular-medicine
Footnotes
Informed consent
The patient provided written informed consent for publication of the photograph.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
