Abstract
Background and Objectives
Driven by the rising demand for telerehabilitation (TR) services and digital transformations in the healthcare management of people with facial palsy (FP), studies on TR programs in this specific population are steadily increasing. Our scoping review aimed to provide an overview of the current state of knowledge on TR for people with FP by addressing three subquestions regarding the types of studies conducted, the technologies used, and the potential existing technologies that could be adapted for TR in this context.
Study Design and Methods
We followed the Joanna Briggs Institute methodology for scoping reviews. Between January and February 2024, two authors performed a literature search on Medline, Cochrane, PEDro, and Scopus databases, while two additional authors conducted a gray literature search using the “Grey Matters” tool, repositories, and Google.
Results
A total of 10,804 reports were initially considered in this scoping review. After the screening process, we included and analyzed 39 results. We found 18 studies with 11 different study designs or types related to TR in FP, 14 technologies projected or already used for TR purposes with a variety of delivery methods or rehabilitative treatments, and 18 additional digital instruments suitable for different TR stages.
Conclusions
Our findings indicate a growing interest in and development of TR instruments, aligning with the broader expansion of telemedicine services across healthcare. We have identified a diverse range of delivery methods, rehabilitative treatments, and digital tools utilized in TR for FP. Additionally, our comprehensive overview provides healthcare providers with practical insights to improve their approach to managing patients with FP in TR contexts.
Introduction
The facial nerve is a complex structure composed of efferent (motor and autonomic) and afferent (sensory) nerve fibers. 1 It plays a crucial role in controlling various aspects of our individuality, particularly the facial expressions unique to each person. 2 Peripheral facial paralysis is a condition characterized by the loss of functionality of the facial nerve due to various causes.3,4 Although considered a benign condition 5 with spontaneous and complete recovery within 3 months for 80% to 85% of patients, 6 it can still present with either transient or persistent motor dysfunction, which is associated with functional, 7 psychological,8,9 and social impairments, 9 with an impact on quality of life regardless of the severity of the condition. 10 Different rehabilitative interventions have been proposed for patients suffering from facial palsy (FP),11–13 with effective results in reducing nonrecovery and improving functional outcomes, even though studies of high quality are lacking. 14 Telerehabilitation (TR) is a branch of telemedicine, and refers to the delivery of rehabilitation services (including evaluation, assessment, monitoring, prevention, intervention, supervision, education, consultation, and coaching) through different technologies. 15 Following the COVID-19 pandemic, a multitude of TR studies have surfaced among various rehabilitation domains.16,17 These studies frequently demonstrate outcomes similar to traditional in-person therapy,18,19 accompanied by elevated levels of satisfaction. 20 However, there is a consensus that studies must enhance methodological rigor. 21 The digital transformation in healthcare has significantly contributed to the advancement of managing patients with facial impairments.22–24. It is acknowledged that digital technologies are employed in facial recognition25,26; however, a substantial implementation has been achieved even in their clinical application.27,28 These technologies have facilitated a more precise clinical assessment of facial lesions 29 and expressions, 30 as well as early diagnosis of facial nerve paralysis through contralateral comparison. 31 In the field of interventional procedures, they support the preparation of advanced techniques in facial plastic and reconstructive surgery.32,33 Moreover, their support extends to preventive measures for monitoring iatrogenic lesions,34,35 and offering potential customized contributions for developing functional devices tailored to specific needs. 36 Machine learning algorithms have shown some potential utility in predicting the likelihood of synkinesis development subsequent to Bell's palsy. 37 In accordance with the widespread adoption of TR services in a variety of conditions, 18 a recent narrative review 22 has highlighted how telemedicine could represent an opportunity in plastic surgery and treatment of FP, even though this field lacks high-quality studies. For instance, Khan et al., 38 in a systematic review aimed at supporting the use of facial rehabilitation to enable TR services for this population, did not find any trial conducted in TR. Moreover, to our knowledge, there are no other scoping reviews, systematic reviews of randomized clinical trials (RCTs), or any RCTs conducted in the area of TR in peripheral FP. Despite this, several articles on the topic exist, employing various methodological designs. Therefore, this scoping review aims to summarize the information about the actual use and potential of TR in peripheral FP, in order to promote further studies regarding feasibility, acceptability, and/or efficacy of TR programs in this population. Hence, the main question is: What is the current state of knowledge of TR in people with FP? To address this, the authors will explore three subquestions: first, what types of studies have been conducted to date about TR in individuals with FP? Second, what technologies (including software, apps, websites, and instruments) have been projected or already used for TR services in patients with FP? Lastly, which existing technologies, developed or used for FP but not specifically designed for TR, could potentially be adapted for use in this context?
Methods
Protocol and registration
The protocol for this scoping review was developed following the “Joanna Briggs Institute (JBI) Manual for Evidence Synthesis” 39 and relevant best practices 40 and was registered on the “Centre for Open Science Framework.” 41 This study was conducted in accordance with the “JBI Manual for Evidence Synthesis” 39 and its updates. 42 We used the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) checklist to guide the reporting. 43
Eligibility criteria
Population
We included studies or contents focused on adult patients (18 years and older) with peripheral facial nerve palsy, including Bell's palsy. The inclusion criteria encompassed all degrees of palsy severity and any underlying etiology. Studies investigating patients under 18 years old of age or those with central facial nerve palsy were excluded from this study.
Concept
All relevant information about PCC inclusion criteria is reported in the protocol Table 1. 41 To answer the first and second subquestions we focused on TR services provided to people with FP. For a more comprehensive description about what is meant by TR services and its applications, please refer to the study protocol. 41 In this review, both synchronous and asynchronous TR services delivered through various modalities (videoconferencing, tele-support, use of platforms, websites, applications) were included. 15 Briefly, synchronous TR involves real-time interaction between the patient and clinician, while asynchronous TR involves nonsimultaneous (“store and forward”) exchange of information, such as clinical data, question, digital media, etc. Both modalities require the use of information and communication technologies. Studies that reported rehabilitation treatments carried autonomously and remotely by patients, even via technologies (i.e. digital platform, websites, etc.), but without providing any clinical data to the therapist through information and communication technologies, were excluded. However, whenever such technologies appeared to be suitable for a TR service, they were included if they met our inclusion criteria for the third sub-question. 41 To describe this potential TR technology, we included the first study in which it has been used or tested on a FP population. Technologies that presented barriers to accessibility or usability for clinicians or patients were excluded. This encompassed technologies that were not user-friendly (defined as “easy to operate or understand, without the need for special training”), 44 required specialized skills or additional equipment, or were not yet available in a fully functional state.
Context
For the first two sub-questions, we restricted our research to a rehabilitative context (physical therapy, speech therapy, etc.), without any geographical or setting limitations. For the third sub-question, we considered a more comprehensive clinical context, excluding technologies that focus on facial features for other purposes (e.g. facial recognition systems for security purposes).
Types of evidence sources
We included every type of publication (primary and secondary research, quantitative, qualitative and mixed-method studies, gray literature, protocols, letters to the editor, and guidelines) that was available as full-text and focused on digital technologies directly or potentially related to TR for FP. We also included content from websites whenever technologies directly or potentially related to TR for FP were found. We excluded website content in case TR or digital solution for the FP population were addressed in a generic way, without focusing on a specific instrument. Studies or website contents in English and Italian were considered.
Search strategy
The search strategy was developed by one author (DG) in collaboration with the entire research team, based on a three-step approach. 39 The literature search was carried out up to 1 February 2024, including the articles published up to the end of January, in the following databases: MEDLINE (via PubMed), Cochrane Central Register of Controlled Trials, Physiotherapy Evidence Database (PEDro), and Scopus. Furthermore, additional content on relevant or potential technologies for FP TR was identified through key words via Google, and a supplemental search of the gray literature was conducted following the “Grey Matters: a practical tool for searching health related grey literature” 43 in every source in accordance with PCC. Clinical trials registries, such as ClinicalTrials.gov, International Clinical Trials Registry Platform (ICTRP), or Australian New Zealand Clinical Trials Registry (ANZCTR), plus the sources listed on “Grey Matters” tool, were analyzed. The web and gray literature searches were carried out up to 18 February 2024. When needed, authors of primary sources or web contents were contacted for further information. The search strategies for each data source can be found in “A” Supplemental material—Tables A1 and A2.
Study selection
During the literature search process, two independent reviewers (DG and SV) screened titles and abstracts for relevance and eligibility for the review. Articles selected for full-text review were read and assessed by the same two independent researchers (DG and SV). Any disagreement that arose at each stage of the study selection was resolved through a group discussion (DG, SV, GO, MC, IG, and GC). The web and gray literature searches were conducted by two independent reviewers (GO and GC) and any divergences were resolved through consultation with a third author (DG).
Data charting process
A data-charting table was jointly developed by five reviewers (DG, SF, MZ, BC, and PK) in accordance with our review questions and the PCC framework, 45 to extract all relevant variables (see Table 1 in the protocol section 41 ). Three authors (GO, MC, and IG) conducted data extraction and subsequently, a fourth author (DG) independently reviewed charted data. When needed, disagreements were resolved by group discussion (DG, GO, MC, IG, GC, and PK).
Data items
We selected specific variables to address each of the three subquestions in addition to basic report characteristics (author, year, and country). For the first subquestion, we collected information on the “source” and “study design.” The “population” variable indicates which FP etiology the study or technology was tested or designed for. The “technology” variable specifies the type or name of the digital instrument, if reported. The “description” provides further details about the study or technology, while “availability” covers the terms of access to the technology, if mentioned. To answer the second subquestion, we used our TR concept to define “type of TR,” indicating whether the TR technology is useful synchronously or asynchronously. 15 “TR usage” addresses the clinical context (e.g. physical therapy, speech therapy, and psychotherapy), and “stage of TR” focuses on the different steps of the rehabilitation process (assessment, intervention, and monitoring) in which the TR technology could be implemented. 46 For the third subquestion, “field of application” refers to the clinical context in which the instrument was originally tested, used, or designed for, distinct from TR usage. “Suitable TR application” refers to the potential type and usage of the technology for TR purposes.
Results
Selection of results
The overall number of sources identified was 10,804. The literature search yielded a total of 6753 articles, including 4857 from MEDLINE (PubMed), 177 from the Cochrane Central Register of Controlled Trials, 1414 from Scopus and 292 from PEDro. Additionally, 18 records were identified through cross-reference sources. The gray literature search resulted in 4033 items, including 1116 from Google, 5 from ClinicalTrials.gov, 100 from ICTRP, 21 from ANZCTR, and 2791 using “Grey Matters” list. The initial screening process eliminated 887 duplicates and 122 non-English results, leaving 5744 articles for review. Title and abstract screening further reduced this to 97 full-text articles for eligibility assessment, with 2 unavailable for retrieval. From the remaining articles, 73 were excluded due to various reasons: 21 did not pertain to TR on people with FP or technologies suitable for this purpose; 13 were about technologies that were not user-friendly in their application; 29 were about technologies that needed extra equipment or user skills to be used; 1 focused on a different population; 7 cited suitable technologies already included; 1 was about technologies not already available; 1 needed clinician based calculation of facial data (not automatically). The remaining 22 studies were considered eligible for this review. Of the 18 studies obtained through citation searching, 2 were not retrieved, 5 were about technologies that needed extra equipment or user skills, 3 were about technologies that were not user-friendly and 1 cited an already included technology, leaving 7 remaining studies considered eligible. The screening stage of the gray literature search resulted in 20 reports. Of these, 7 were removed because they were not focused on TR or suitable technologies; 2 were about a different population; 1 was about a technology that was not available. The overall screening stage resulted in 39 contents eligible for this review. The selection process is detailed in the PRISMA flowchart, 43 presented in Figure 1. The list of excluded full-text citations with reasons for exclusion, as well as studies that were not retrieved, can be found in “B” Supplemental material—Tables B1, B2, and B3.
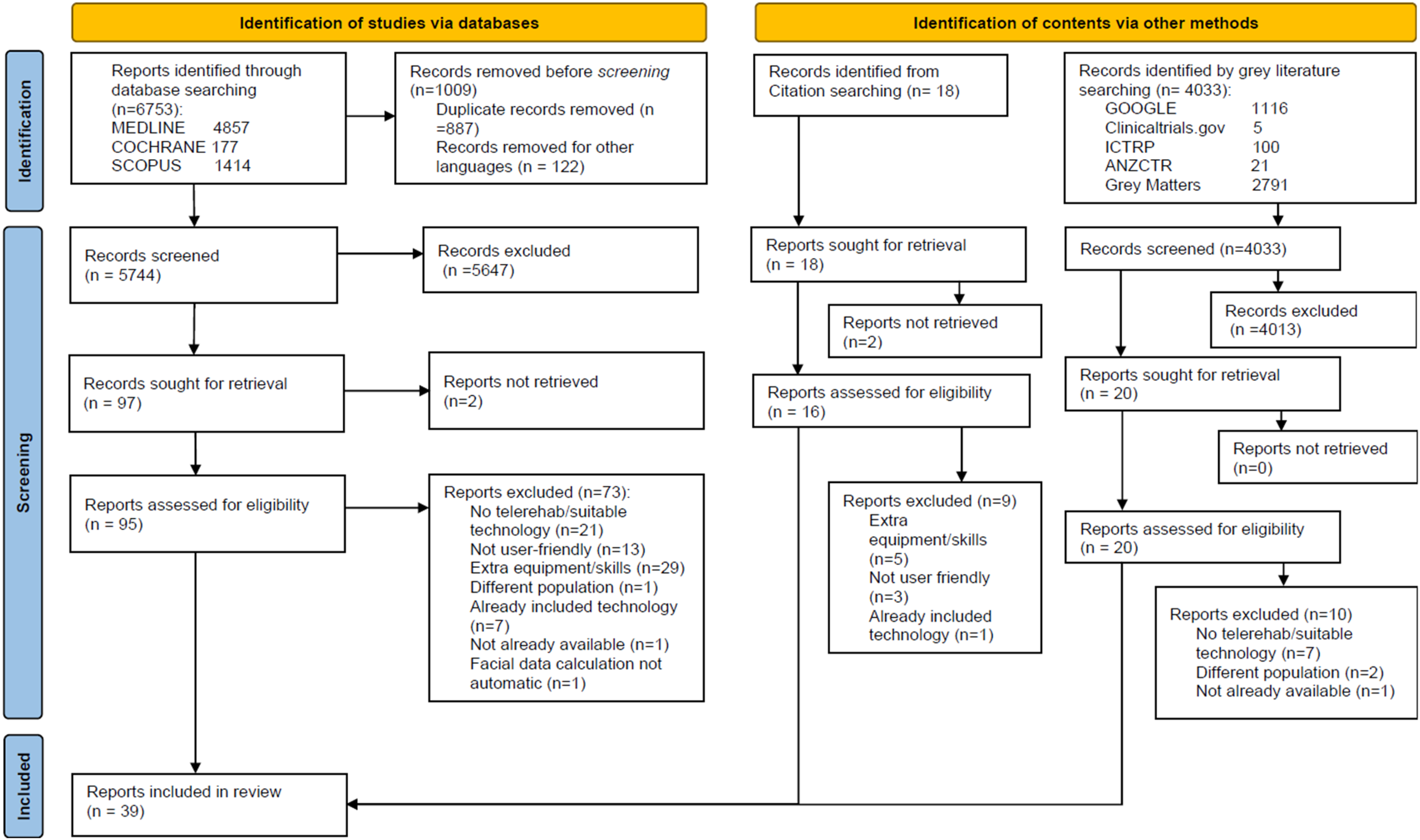
PRISMA study flow diagram.
Report characteristics
Of the 39 results included, 33 are research papers, 1 is a conference abstract, and 5 are website contents. Regarding research papers, the study countries of origin, based on the corresponding authors’ affiliations, span 16 different countries. Authors from Italy produced the highest number of publications (n = 6; 33.3%), followed by the United Kingdom (n = 5; 27.7%), and the United Kingdom and Canada (n = 4; 22.2%). Other countries with fewer than three studies include: Germany, Australia, China, Spain, Japan, Austria, Brazil, United Arab Emirate, Pakistan, Thailand, Turkey, and France. The 33 research papers were published between 2010 and 2023. The origins of protocol authors are Canada, France, and Turkey, with publications between 2016 and 2023. The conference abstract is from the United Kingdom. The countries of origin for the five website contents are the United Kingdom, Sweden, Denmark, Belgium, and Slovakia.
Synthesis of results
From the initial pool of 10,804 resources identified during the screening process, a total of 39 met the inclusion criteria for our review. In summary, 18 studies from 16 countries have been published about TR in FP population since 2010. The selected reports involved 18 different types of technologies projected or already used for TR services for this population. Additionally, we identified 17 more technologies suitable for a TR purpose, according to our third subquestion.
Study designs in TR research on FP
Of the 39 reports included, 18 studies (46.1%) focused on TR services in FP population. These include 11 research papers, 4 RCT protocols, 2 graduation theses, and 1 letter to the editor. The main findings regarding study designs, types of technologies and suitable TR application are reported in Table 1.
Summary of key findings.
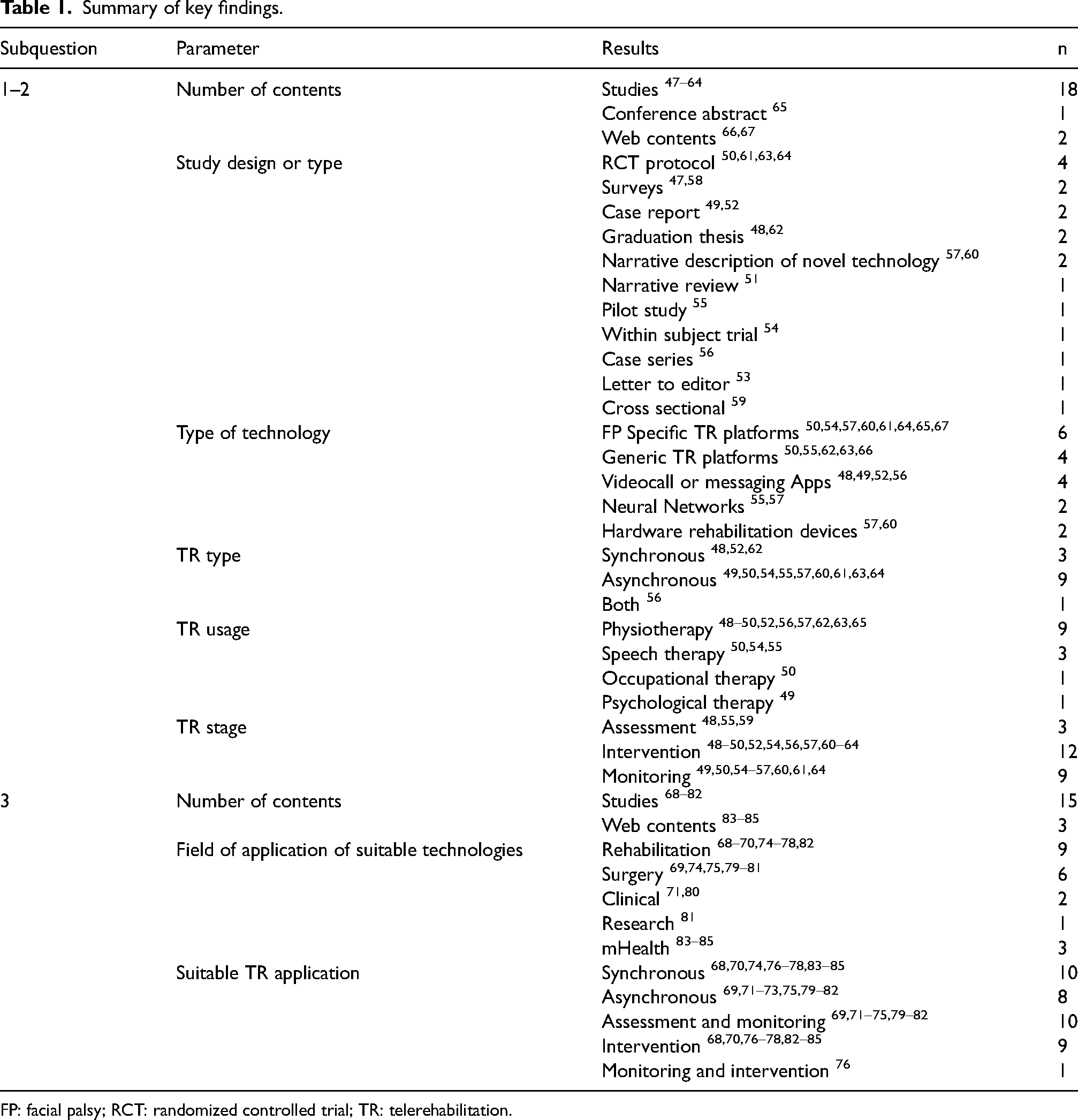

FP: facial palsy; RCT: randomized controlled trial; TR: telerehabilitation.
Identified technologies for TR services in FP
Regarding the technologies to provide or support TR services for the FP population, we included 17 reports (43.5%) of which 14 are research papers, 1 is a conference abstract, and 2 are web contents. The synoptic table containing the extracted extended information is available in Supplemental C, Table C1, where the contents are initially organized by subquestion number and subsequently in chronological order. To summarize the key findings, we grouped these technologies into five different categories:
– “FP Specific TR platforms” are digital platforms specially created for FP rehabilitation. They are accessible via smartphone or PC, allowing clinicians to monitor and guide patients’ exercise programs and progress. The specific platforms identified include MEPP 2.0,50,61 MEPP 1.0,54,61 FRAME,60,65 FaceRehab®,
67
and other two additional specific platforms57,64; – “Generic TR platforms” are technologies designed for more comprehensive TR services. These include the Phystrack® app,50,66 Homely Care,
55
Pagine Mediche®,
62
and an unspecified online platform
63
; – “Videocall or messaging apps” are existing and widely used applications that were not originally developed for TR purposes. They allow therapists and patients to schedule synchronous video TR sessions or exchange information about the rehabilitation process asynchronously. The apps used include Zoom®,
48
Skype®,
52
WhatsApp®,48,49 and an unspecified messaging app
56
; – “Neural networks” were trained and used to identify specific facial points through patients’ video recordings or camera layouts,55,57 which are useful for analysis purposes; – “Hardware rehabilitation devices” were specifically designed to provide FP rehabilitation treatments. These devices include a “flexible massaging headgear”
57
and “EMG biofeedback goggles”,
60
both of which are supported by one of the previously mentioned specific TR platforms.
The TR typology of the included studies was as follows: synchronous in 3 studies,48,52,62 asynchronous in 9 studies,49,50,54,55,57,60,61,63,64 and both synchronous and asynchronous in 1 study. 56 Regarding the two web content technologies, one utilized an asynchronous modality, 67 while the other employed both synchronous and asynchronous approaches. 66 In the included studies, the TR was primarily utilized by physiotherapists.48–50,52,56,57,62,63,65 One study reported that patients were provided with additional psychological support. 49 In addition to physiotherapists, one study included both speech and occupational therapists, 50 two studies involved only speech therapists,54,55 and two studies did not specify which type of rehabilitation specialists supervised the treatments.61,64
Suitable technologies for TR aim in FP
According to our inclusion criteria, the literature and web search conducted for the third subquestion identified 18 items (46.1%), comprising 15 studies, and 3 web contents. As mentioned earlier, the synoptic table containing the extracted extended information is available in Supplemental C, Table C1. We grouped the included technologies based on their suitability for different TR stages:
– “Intervention technologies” were described in five articles and three web contents. Of the eight digital technologies, “Face mirroring system,”
68
“Specular Face Software,”
70
“IDIBELL software®,”
76
“Webcam Toy®,”
77
and “Face2Face Facial Palsy®
83
” used mirroring software to duplicate the healthy side of the face for mirror therapy. “FaraPy”
78
and “Facial Paralysis®”
85
used real-time feedback on exercise performance, while “Face It! Bell's palsy-Training®”
84
provided exercises and educational content. – “Assessment and monitoring technologies” for defining the grade of FP were described in 10 studies. Five instruments use facial automatic landmarks: the two version of “Emotrics”73,80 compute a set of relevant facial measurements in FP, while “Auto-eFace,”
69
“SBface application,”
72
and “real-time facial asymmetry analysis”
74
assign scores based on ratios of the facial marks. Three technologies use specific algorithms on photos or videos to evaluate facial movements (“TrueDepth camera” based-app
71
) or emotions (“FaceReader®”
75
and “SmileCheck”
79
). Additionally, one program produces a “Facogram”
81
and a “Computer Application”
82
works by analyzing pixel changes in photos.
Notably, some of the cited instruments could be used for both intervention and assessment or monitoring stages.74,82
Discussion
Summary of evidence
This scoping review aimed to synthesize existing knowledge about TR in FP population. The review included studies that directly addressed TR services for patients with FP, as well as those that indirectly discussed related symptoms. Additionally, we examined technologies with potential applications in TR for this specific population, broadening the scope to include emerging tools and methods that could enhance remote care delivery for patients with FP. Among the 21 studies selected to address our first and second subquestions, only 9 (42.8%) explicitly mentioned TR.47–49,52,53,56,58,62,63 This is attributable to the heterogeneity of digital health-related terms and the overlapping concepts within their definitions. 86 However, it's worth noting that all the technologies described in the included studies aligned with our definition and criteria for TR services, even if not explicitly labeled as such. The selected reports involved different types of technologies, including specific and generic TR platforms, as well as messaging apps, which is consistent with the variety found in studies for other populations.87,88 Olsen et al. 89 found that rehabilitation technology factors, such as patient engagement features (e.g. monitoring, reminders, and rewards) or personalization tailored to patient needs, can positively influence their adoption and sustained use. These features are usually embedded in TR platforms, given that their development, as a best practice, requires the involvement and iterative assessments of potential users. 90 Despite lacking these elements, our findings confirm the vast utilization of messaging or video-calling apps, such as WhatsApp®,91–93 Zoom®,94,95 or Skype®,96,97 in telemedicine.
Through our literature search, we identified at least 15 subjects with FP who received a TR treatment,16,47–49,56,62 as well as 1 survey that revealed therapists’ perspectives on TR in FP. Furthermore, we found several specific technologies designed for providing TR services.50,54,57,60,61,65,67 Hence, this research revealed a gap: while there is a growth in TR services and technologies for FP, we found no RCTs confirming their efficacy, 98 as previously noted by some authors. 53 To address this issue, our search of clinical trial repositories uncovered two ongoing RCTs50,63 and one completed RCT with no study results available yet. 64 Studies on user experience for specific platforms are either available 54 or currently underway. 61 The two included surveys have provided some qualitative input on the perception of TR instruments. Szczepura et al. 58 found a positive attitude toward digital technology in managing FP among both clinicians (favorable for TR) and patients, consistent with results from studies in a broader context99–101. Despite the generally positive reception, some concerns have been noted in the literature, especially due to the hands-off nature of TR. 102 In a related study, Buckingham et al. observed favorable views towards TR among UK rehabilitation practitioners. 47 However, the researchers were unable to provide the raw survey data specifically pertaining to FP tele-treatment as reported by one participant. In their update of the evidence for facial exercise therapy, including for a TR purpose, Khan et al. 38 reported considerable heterogeneity among the interventions included. To a lesser extent, our findings reflect similar considerations among the rehabilitation interventions. Some authors performed the MEPP protocol, which consists of counseling, motor imagery, and facial retraining through modified visual biofeedback and neuromuscular retraining components.50,54,61 Others provided cognitive and sensory tasks mixed with facial expression exercises but with different time sequences.48,49,62 Additional proposals involved active and specific facial muscle exercises, either alone 52 or combined with education, auto-massage, and other app functions. 67 Facial muscle massages using a peripheral device, 57 auto-stretch and facial massage with smartphone application guidance,60,65 neuromuscular retraining alone 52 or with educational content, 84 virtual smile exercises, 64 and mime therapy 66 were also reported. As mentioned above, some included instruments are suitable for providing mirror therapy68,70,76,77,83 or obtaining visual feedback during the exercises.78,85 Some rehabilitation programs were not reported in detail.56,85 Several identified instruments have potential for the assessment stage. However, only a few have been validated, such as “Emotrics” 103 and “SmileCheck,” 79 with further details about this topic available in other sources. 104 We assumed that suitable technologies for assessing the degree of FP through photo69,72,73,80 or video analysis71,74,75,79,81 could align with asynchronous stages of TR, which allows for an exchange of data (such as digital media or clinical statistics) between patient and clinician. Technologies useful for performing exercises, such as mirror therapy,68,70,76,77 visual feedback,74,78 or app-based approaches,83–85 were considered appropriate for supporting synchronous sessions. Tan et al. 59 provided further details about the potential for conducting asynchronous FP assessment using House-Brackmann, Sydney, and Sunnybrook systems through recorded video, finding good reliability, although it was poor in measuring synkinesis.
Driven by the global digital transformation of healthcare systems, 105 the diverse technologies developed to address FP have the potential to significantly extend digital health delivery models 106 for this population. Hence, new remote care pathways are emerging even for the rehabilitation of FP, confirming a trend observed for other conditions20,107,108 and a lasting interest in this field.17,109
Strengths and limitations
Our research methodology incorporated two key strengths: strict adherence to the “JBI group” guidelines for conducting and documenting our study, and a thorough literature review encompassing various electronic databases and gray literature sources. However, there are limitations. Firstly, due to the variety of nomenclature in the digital health field (eHealth, mHealth, telehealth, etc.), we included some studies based on our criteria even when TR purpose was not explicitly declared in the report. For the same reason, there is a risk that some relevant studies were not detected by our search strings, despite our efforts to make them adequately sensitive. Regarding the third subquestion, our research group initially selected specific characteristics (user-friendliness, no extra equipment or skills required, and immediate availability) for suitable TR technologies at the protocol stage. This was done to enhance generalizability and applicability in broader research or clinical contexts. However, excluding studies without these features may have precluded the inclusion of other potentially relevant instruments in the TR field. In two specific cases, we decided to include studies about a beta version 72 and a prototype 71 of assessment technologies, despite our inclusion criteria of immediate availability. This decision was made because both instruments were in an advanced stage of development and had already been tested for reliability. Additionally, we included some assessment instruments69,73,75 that work with photos taken in a laboratory context using specific digital cameras, assuming that these digital media could likely be replicated using accessible instruments (e.g. smartphone cameras) in a home setting. However, this assumption should be confirmed in specific studies. It is important to note that every identified suitable technology should be tested in proper research consistent with the relative clinical question before their implementation in a clinical TR context. Our opinions on the TR stage of suitable technologies were based on our experience and knowledge of the TR field, but this does not preclude potential and different application in further works. Finally, the absence of critical appraisal of the included reports did not allow us to provide further information about the quality of the studies and, consequently, the described technologies.
Deviations from the protocol
We performed the gray literature search until 18 February 2024 and not in January 2024 as declared in our protocol. This is due the fact the research toward “Grey Matters” and Google resulted in more reports than expected, requiring additional time for the screening stage. Similarly, due to the larger volume of included resources compared to our expectations, three authors extracted data for the Supplemental C, Table C1 instead of the authors stated in our protocol.
Future implications
In our protocol, 41 we assumed that our research could reveal the need for RCTs to evaluate the efficacy of TR in people with FP, as well as further studies on the feasibility and acceptability of TR platforms for this population. Our findings confirmed these hypotheses, showing the current state of TR services and instruments, both in the literature and in the market. A Delphi survey 110 on research priorities in FP management that involved patients, researchers, clinicians, and carers did not highlight any TR needs to be addressed. However, this research dates back to 2018, before the COVID-19 pandemic, after which an increased interest in this topic was reported. 17 Despite this, no other emerging needs in the digital management of people with FP were raised in recent studies,111,112 except in Szczepura et al. 58 Nevertheless, researchers can take advantage of our results to address the gap between actual usage and research. They can establish which TR programs, instruments, delivery methods, dosage, and types of treatments could be effective or feasible through further studies, such as clinical trials or feasibility studies. Furthermore, they will have the chance to test additional instruments potentially useful for the TR context. Our work can support clinicians currently involved in TR services, providing some valuable insights regarding the remote management of this population using the described technologies.
Conclusion
In conclusion, this review provides a comprehensive understanding of TR programs for individuals with FP. Our findings reveal a growing interest in and development of TR instruments, aligning with the broader expansion of telemedicine services across healthcare. We have identified a diverse range of delivery methods, rehabilitative treatments, and digital tools utilized in TR for FP. These findings present opportunities for researchers to conduct in-depth studies on the feasibility and efficacy of these approaches. Additionally, our summary provides clinicians with practical information to enhance their management of patients with FP in the TR setting.
Supplemental Material
sj-docx-1-jtt-10.1177_1357633X251342335 - Supplemental material for Telerehabilitation for peripheral facial palsy: A scoping review
Supplemental material, sj-docx-1-jtt-10.1177_1357633X251342335 for Telerehabilitation for peripheral facial palsy: A scoping review by Davide Grillo, Gianluca Ossola, Mattia Cecconi, Stefano Vania, Ignazio Geraci, Gianluca Calò, Sara Federico, Mirko Zitti, Błażej Cieślik, Silvia Zangarini and Pawel Kiper in Journal of Telemedicine and Telecare
Supplemental Material
sj-docx-2-jtt-10.1177_1357633X251342335 - Supplemental material for Telerehabilitation for peripheral facial palsy: A scoping review
Supplemental material, sj-docx-2-jtt-10.1177_1357633X251342335 for Telerehabilitation for peripheral facial palsy: A scoping review by Davide Grillo, Gianluca Ossola, Mattia Cecconi, Stefano Vania, Ignazio Geraci, Gianluca Calò, Sara Federico, Mirko Zitti, Błażej Cieślik, Silvia Zangarini and Pawel Kiper in Journal of Telemedicine and Telecare
Supplemental Material
sj-docx-3-jtt-10.1177_1357633X251342335 - Supplemental material for Telerehabilitation for peripheral facial palsy: A scoping review
Supplemental material, sj-docx-3-jtt-10.1177_1357633X251342335 for Telerehabilitation for peripheral facial palsy: A scoping review by Davide Grillo, Gianluca Ossola, Mattia Cecconi, Stefano Vania, Ignazio Geraci, Gianluca Calò, Sara Federico, Mirko Zitti, Błażej Cieślik, Silvia Zangarini and Pawel Kiper in Journal of Telemedicine and Telecare
Footnotes
Acknowledgments
The authors would like to thank all the contacted researchers who took the time to provide us detailed explanations about their studies: Ms. Liesbet Desmet, Dr Sarah Martineau, Dr Sarah Buckingham, Dr Diego L. Guarin and Dr Fatih Ozden. We acknowledge the use of Gemini (Google AI) for writing assistance.
Author contributions
DG was involved in conceptualization, methodology, investigation, writing—original draft, supervision, and project administration; GO, MC, SV, IG, and GC in conceptualization, methodology, and investigation; SF, MZ, BC, and SZ in conceptualization, methodology, and writing—review and editing; and PK in conceptualization, methodology, supervision, and project administration.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This work was supported by the Italian Ministry of Health (Ricerca Corrente).
Supplemental material
Supplemental material for this article is available online.
Data availability statement
The example text of a data statement as provided by the author. All data generated or analyzed during this study are included in this published article [and its supplementary information files].
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
