Abstract
Background
To determine (a) the effect of mHealth-based physiotherapy for patients with chronic non-specific low back pain (CNLBP) on fear, anxiety, depression, and self-efficacy; (b) which is the most effective on improving individuals’ pain intensity and physical disability through the comparison of the efficacy of mHealth-based physiotherapy with outpatient-based physiotherapy, home-based physiotherapy with simple supervision or unsupervision, and waiting-list group.
Methods
The systematic review and meta-analysis of randomized controlled trials (RCTs) was conducted in PubMed, MEDLINE (via Ovid), Scopus, Embase, the Physiotherapy Evidence Database (PEDro), Web of Science, and the Cochrane Central Register of Controlled Trials (CENTRAL) until September 20, 2024. Two independent reviewers (LQ and CZW) extracted information about origin, characteristics of study participants, eligibility criteria, characteristics of interventions, outcome measures and main results.
Results
A total of 37 RCTs involving 5832 participants were included. The risk of bias was generally low in the included studies. The results indicated that mHealth-based physiotherapy for individuals’ CNLBP was more effective in reducing pain intensity (standardized mean difference [SMD] −0.32, 95% CI −0.48 to −0.17; P < 0.001), improving physical disability (SMD −0.30, 95% CI −0.42 to −0.18; P < 0.001), and decreasing fear-avoidance (SMD −0.28, 95% CI −0.47 to −0.09; P = 0.004). However, the mHealth-based physiotherapy was less effective on decreasing anxiety (SMD 0.29, 95% CI 0.06–0.52; P = 0.01) and remained unclear in decreasing depression (SMD 0.13, 95% CI −0.05 to 0.31; P = 0.16) and improving self-efficacy (SMD 0.14, 95% CI −0.06 to 0.34; P = 0.18). In subgroup analyses of pain intensity and physical disability, mHealth-based physiotherapy for individual with CNLBP was more effective than outpatient-based physiotherapy, home-based physiotherapy with simple supervision or unsupervision and waiting-list groups.
Conclusion
Our meta-analysis suggested that mHealth-based physiotherapy holds significant potential for reducing pain intensity and fear-avoidance, and improving physical disability in individuals with CNLBP compared to traditional physiotherapy model. However, its effect was less on reducing anxiety and depression, and improving self-efficacy.
Introduction
Low back pain (LBP) is a condition characterized by discomfort, muscular strain, or inflexibility in the lumbosacral region, which may occasionally extends down the lower extremities.1,2 The Global Burden of Disease (GBD) study reports that by 2020, the global prevalence of LBP will exceed 619 million people, a 60% increase from 1990, and is expected to reach 843 million by 2050. 3 Studies showed 85% to 90% of individuals with LBP has unclear triggering factors, and these cases were referred to as non-specific LBP (NLBP). 2 LBP is classified as acute (less than 6 weeks), subacute (6–12 weeks), and chronic (more than 12 weeks) based on pain duration. 4
Previous studies indicated that individuals with chronic NLBP (CNLBP) would develop depression, anxiety and fear-avoidance due to repeated pain and physical disability, and long-term psychological dysfunction might further exacerbate pain intensity and physical dysfunction, forming a vicious circle. 5 Lim et al. showed that exercise, education and cognitive behavioral therapy (CBT) are the first-line treatment for CNLBP based on their summary and analysis of 30 global clinical practice guidelines (CPGs) related to LBP. 6 However, the efficacy of physiotherapy for patients with CNLBP has been underestimated under traditional physiotherapy models, which necessitate that patients receive qualified physiotherapy at outpatient clinics or specialized orthopedic institutions. 7 This may be due to the fact that a large number of individuals with CNLBP do not have access to receive professional physiotherapy services due to time restriction, the high expense of treatment and traveling, and transportation inconvenience. 8 Moreover, The CPGs showed that the crucial role of home-based exercises and daily self-management for patients with CNLBP is often undermined due to lack of supervision and guidance.8,9 Therefore, it is both urgent and critical for individuals with CNLBP to explore innovative physiotherapy approaches.
The advent of mobile health (mHealth) technologies offers a promising solution to these challenge.9,10 Nowadays, mHealth technologies, including smartphone applications, wearable devices, and online platforms, are extensively used to provide remote guidance and supervision for home-based exercise protocols and education in individuals with CNLBP. 11 Previous systematic reviews have demonstrated the effects of app-based physiotherapy on pain intensity reduction and physical function improvement in individuals with CNLBP.12–14 However, the outcomes of previous research varied according to the different interventions of control group.15–18
Psychological factors have a strong association to the pain and physical disability of individuals with CNLBP. 5 Nevertheless, the effect of mHealth-based physiotherapy is still unclear on improving depression, anxiety, and fear-avoidance. So far, previous studies has reported conflicting results on the mental health benefits of mHealth-based physiotherapy.15,16 Additionally, although studies have shown that the effect of mHealth-based physiotherapy is strongly associated with individuals’ self-efficacy, which reflects their perceptions and confidence in their ability to exercise,17,18 the efficacy of mHealth-based physiotherapy in enhancing self-efficacy has not been thoroughly investigated.
Based on previous research findings,5,12–14 the objective of this systematic review and meta-analysis was to explore the efficacy of mHealth-based physiotherapy for patients with CNLBP in terms of psychological outcomes, including depression, anxiety, self-efficacy and fear-avoidance. Furthermore, our research team explored the efficacy of mHealth-based physiotherapy in reducing individuals’ pain intensity and improving physical disability compared with outpatient-based physiotherapy, home-based physiotherapy with simple supervision or unsupervision, and waiting-list groups.
Methods
Registration and approval
This review has been registered with PROSPERO (CRD4202458173). The literature search, reporting guidelines, and research implementation process all adhered to the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. 19
Search strategy
Randomized controlled trials (RCTs) meeting the inclusion criteria were included in this review. The inclusion criteria are defined according to the “Population, Intervention, Comparison, and Outcomes” (PICO) model, as outlined in Table 1. There were no restrictions on publication year or language.
Inclusion criteria defined by PICOS.
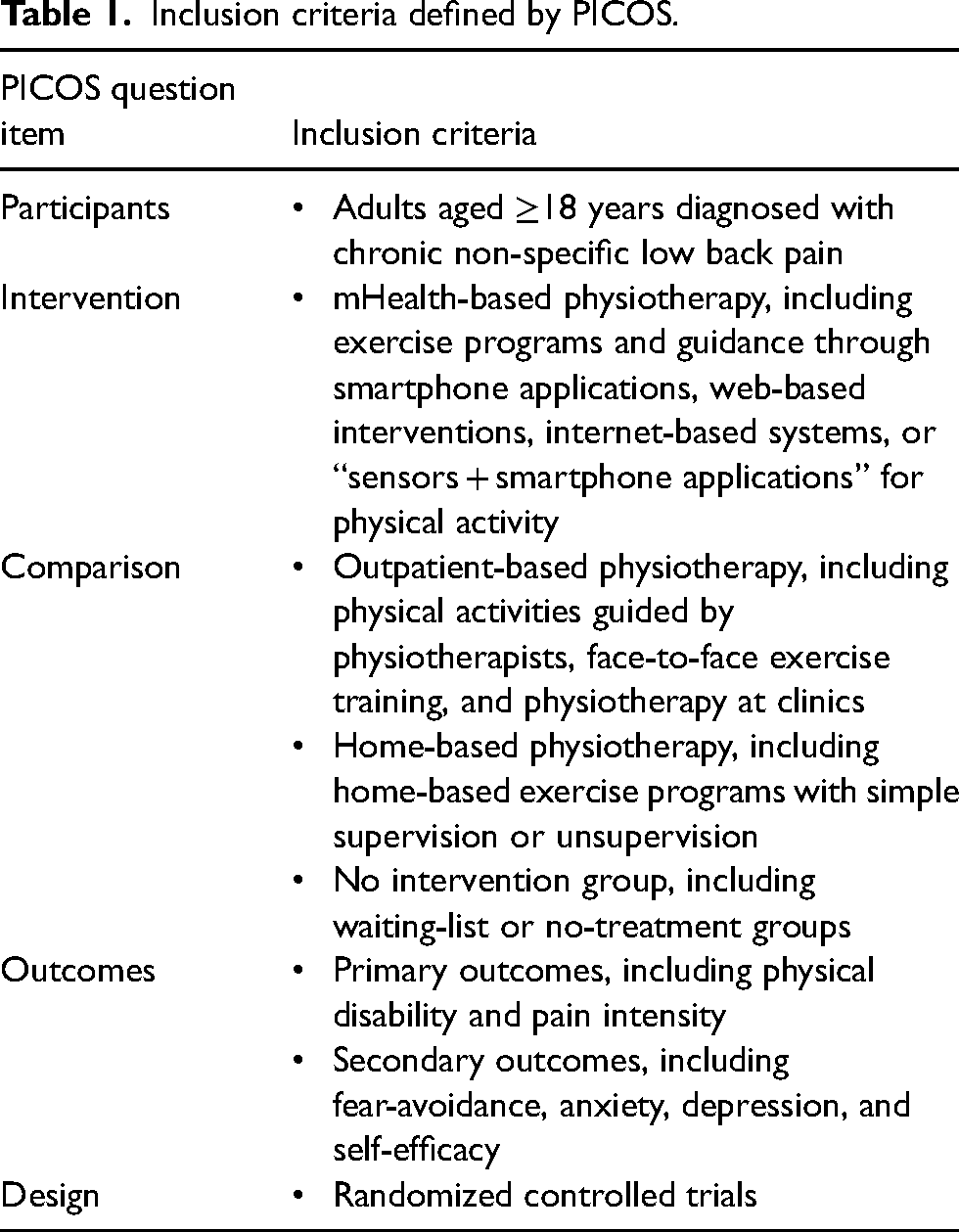
Information sources
Our research team has identified relevant RCTs up to September 20, 2024 in the following databases: PubMed, MEDLINE (via Ovid), Scopus, Embase, the Physiotherapy Evidence Database (PEDro), Web of Science, and the Cochrane Central Register of Controlled Trials (CENTRAL). The reference lists of the included studies were also screened. The entire search process, including risk of bias assessment, data extraction and analysis, and completion of writing this article, was carried out until October 20, 2024.
Search strategy
The search strategy consisted of controlled vocabulary and keywords tailored to each database's requirements. The exact research terms used were as follows: (“low back pain” or “back pain” or “Backache”) and (“Mobile Applications” or “mobile health” or “digital health” or “telerehabilitation”) and (“Randomized controlled trial” or “systematic review” or “meta-analysis”). A detailed search strategy for PubMed can be found in Supplement 1. The research team selected updated searches from the initially used databases to refine the study results. Additionally, reference lists from prior reviews were consulted to identify other relevant studies.
Screening process
The studies obtained from the search were uploaded to Endnote X9 (Thomson Research Soft). After removing duplicates, two researchers (SWH and ZYH) independently screened the titles and abstracts to identify relevant trials. Full texts of potentially relevant studies were retrieved and independently reviewed by two assessors, who evaluated whether they met the inclusion criteria according to the predefined standards. In case of any disagreement between the assessors regarding inclusion, a third reviewer (ZHQ) acted as an arbitrator until a consensus was reached. For trials with unclear intervention or design, further clarification was sought from the corresponding author.
Risk of bias assessment
The quality of individual trials was assessed using the PEDro scale. 20 The PEDro scale consists of 11 items designed to score the methodological quality of RCTs. Each item, except for the first (whether inclusion criteria and sources are stated), contributes one point, for a total score of 10. Items 2 to 9 assess internal validity concerning random allocation, allocation concealment, baseline comparability, blinding, adequate follow-up and intention-to-treat analysis. Items 10 and 11 evaluate the completeness of statistical reporting. Published PEDro scores were extracted from the PEDro database, and trials without a PEDro score were assessed by two independent reviewers (SWH and ZYH), both trained in the PEDro scale.
Data collection process
Two reviewers (LQ and CZW) independently extracted all data using standardized forms developed for this review. The extracted data included basic information (e.g. author, publication year, country, and study type), characteristics of the study population (e.g. age, gender, sample size), methodological details (e.g. study design, participant characteristics, interventions, outcome measures), and results (e.g. data format, pre- and post-intervention scores, change scores).
Statistical analysis
If fewer than three studies were included, a systematic review was conducted. If a sufficient number of studies were included, a meta-analysis was performed using RevMan 5.4 (Nordic Cochrane Center) and Stata 17.0 (StataCorp) to estimate effect sizes, conduct subgroup analyses, and perform sensitivity analysis. Weighted mean differences (WMD) with 95% confidence intervals (95% CI) were used as effect sizes when the same measurement methods were employed; standardized mean differences (SMD) with 95% CI were used when measurement methods differed. 21 The interpretation of SMD is as follows: SMD < 0.2 is small; 0.2 ≤ SMD < 0.5 is moderate; 0.5 ≤ SMD < 0.8 is large; SMD ≥ 0.8 is very large.
For studies reporting means and standard deviations (SDs) indirectly, mean differences (MD) and SMD were calculated according to the Cochrane Handbook. Heterogeneity was assessed by visually inspecting point estimates and overlapping confidence intervals, as well as using χ2 tests and I2 statistics. If I2 > 50% and P < 0.01, a random-effects model was used for the meta-analysis; otherwise, if I2 ≤ 50% and P > 0.01, a fixed-effects model was applied. Subgroup analyses based on different control groups were conducted to explore sources of heterogeneity. Sensitivity analysis was performed to assess the robustness of the results, and funnel plots and Egger's test were used to evaluate publication bias, using Stata 17.0 (StataCorp) as the analysis tool.
Results
Study selection process
A total of 3445 potentially relevant studies were identified, including PubMed (639), MEDLINE (via Ovid) (123), CENTRAL (1020), Embase (191), Web of Science (1296), Scopus (176), and PEDro (134). After removing duplicates and screening titles and abstracts, 176 articles met the criteria for full-text review based on the inclusion and exclusion criteria. Subsequently, 37 studies were selected for final inclusion in the analysis (see Figure 1).
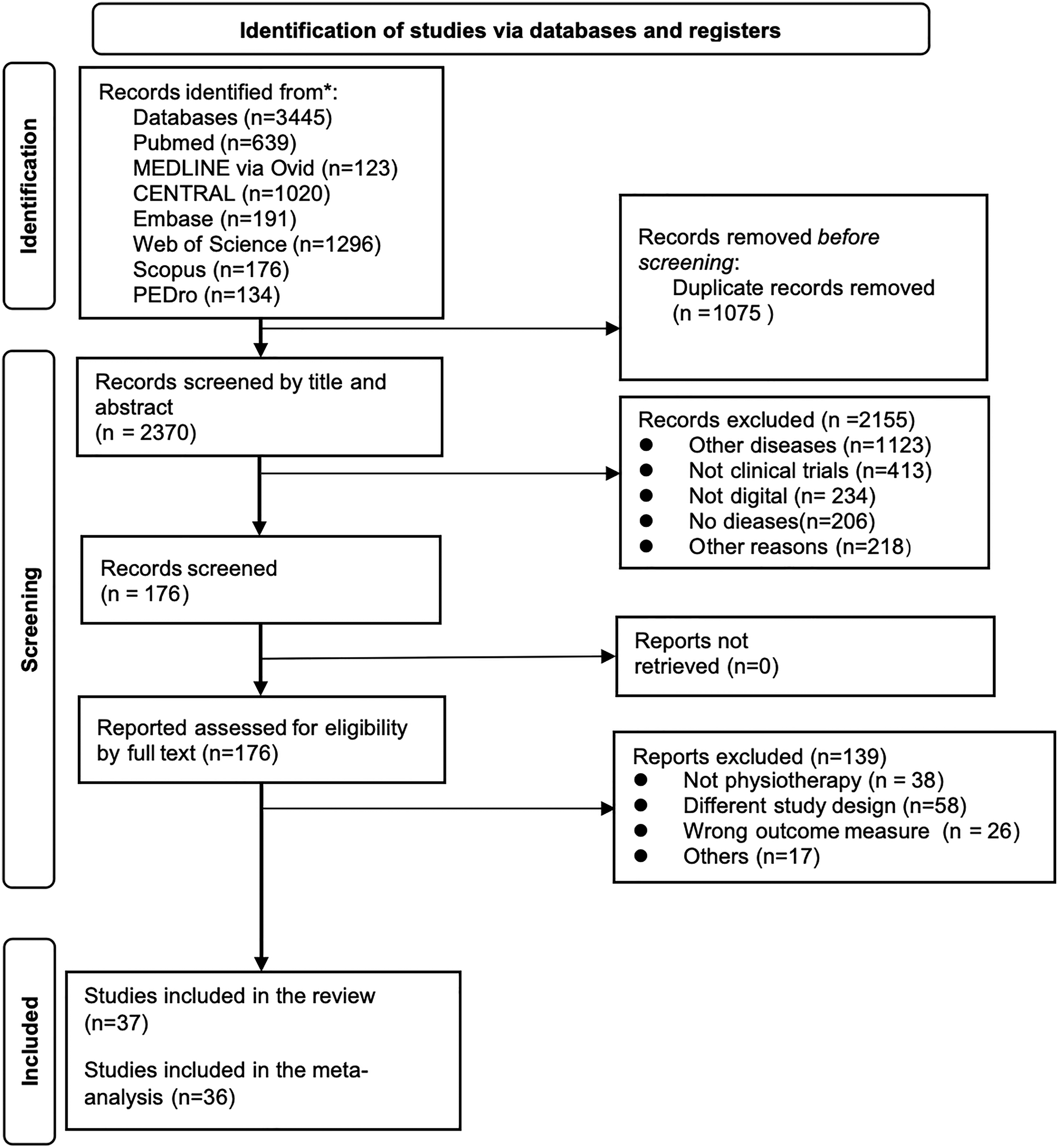
Flowchart of studies selection.
Characteristics of included studies
This review included 37 articles, all of which were RCTs published between 2004 and 2024. The total sample size across the studies was 5832 participants (3541 in the experimental group and 2291 in the control group). These studies primarily compared mHealth-based physiotherapy with outpatient-based physiotherapy (13/37, 35.2%), home-based physiotherapy with simple or no supervision (12/37, 32.4%), and waiting-list groups (12/37, 32.4%). The studies were conducted in the following regions: Europe (17/37, 45.9%), Asia (9/37, 24.3%), Africa (2/37, 5.4%), Oceania (4/37, 10.8%), North America (4/37, 10.8%), and South America (1/37, 2.7%). The follow-up periods across the studies ranged from 8 weeks to 4 months (see Tables 2 to 4). The primary and secondary outcome measures included pain intensity, physical disability, fear, anxiety, depression, and self-efficacy.
Summary of the intervention characteristic of the included studies (mHealth-based physiotherapy vs. outpatient-based physiotherapy).

VAS: Visual Analog Scale.
PSEQ: Pain Self-efficacy Questionnaire.
RMDQ: Roland–Morris Disability Questionnaire.
SF-36: 36-item Short Form.
NPRS: Numerical Pain Rating Scale.
TSK: Tampa scale for kinesiophobia.
HFAQ: Hannover Functional Ability Questionnaire.
VR-12-PCS: Veterans RAND 12-Item Health Survey-Physical component summary score.
VR-12-MCS: Veterans RAND 12-Item Health Survey-Mental component summary score.
ODI: Owestry Disability Index.
FABQ: Fear-Avoidance Beliefs Questionnaire.
DASS: Depression Anxiety Stress Scale.
SF-12-MH: 12-item Short-Form Health Survey-Mental Health.
PCS: Pain Catastrophizing Scale.
GSES: General Self-Efficacy Scale.
GAD-7: 7-item Generalized Anxiety Disorder Scale.
PHQ-9: Patient Health Questionnaire-9.
Summary of the intervention characteristic of the included studies (mHealth-based physiotherapy vs. home-based physiotherapy with simple supervision or unsupervision).
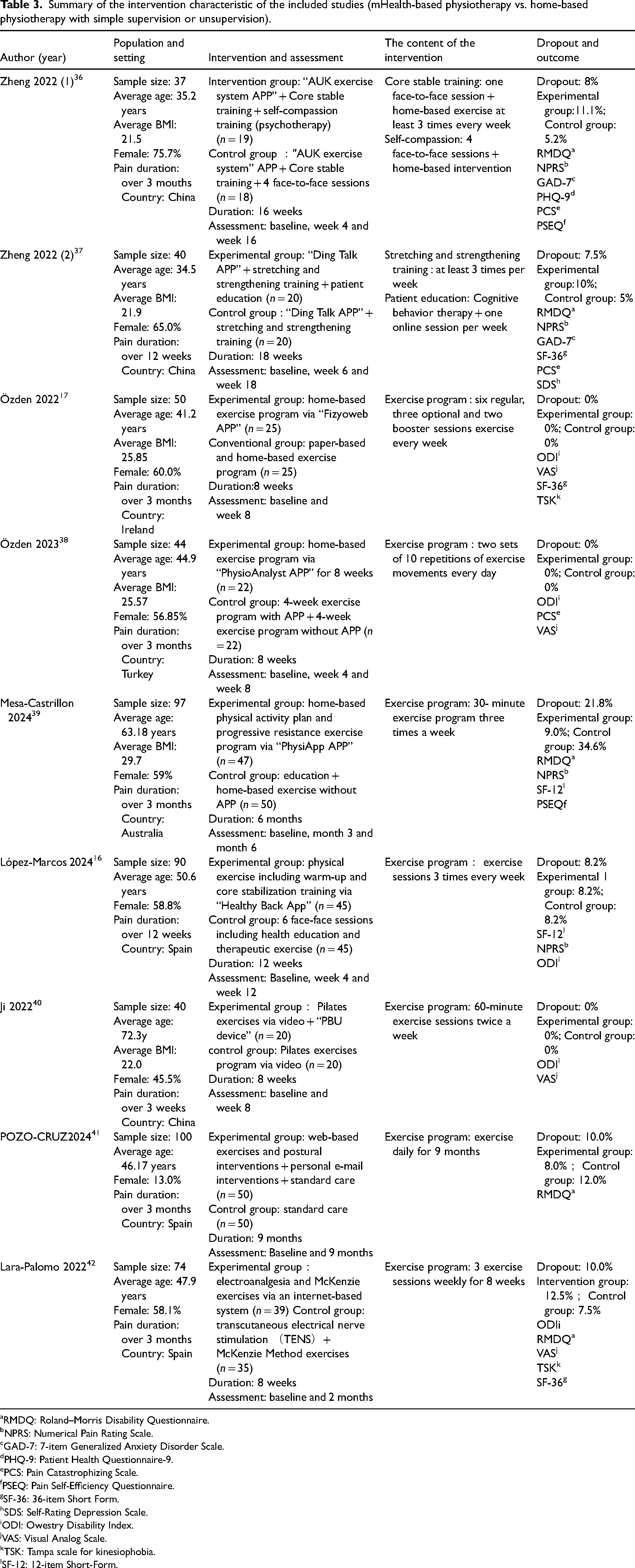
RMDQ: Roland–Morris Disability Questionnaire.
NPRS: Numerical Pain Rating Scale.
GAD-7: 7-item Generalized Anxiety Disorder Scale.
PHQ-9: Patient Health Questionnaire-9.
PCS: Pain Catastrophizing Scale.
PSEQ: Pain Self-Efficiency Questionnaire.
SF-36: 36-item Short Form.
SDS: Self-Rating Depression Scale.
ODI: Owestry Disability Index.
VAS: Visual Analog Scale.
TSK: Tampa scale for kinesiophobia.
SF-12: 12-item Short-Form.
Summary of the intervention characteristic of the included studies (mHealth-based physiotherapy vs. waitlist group).
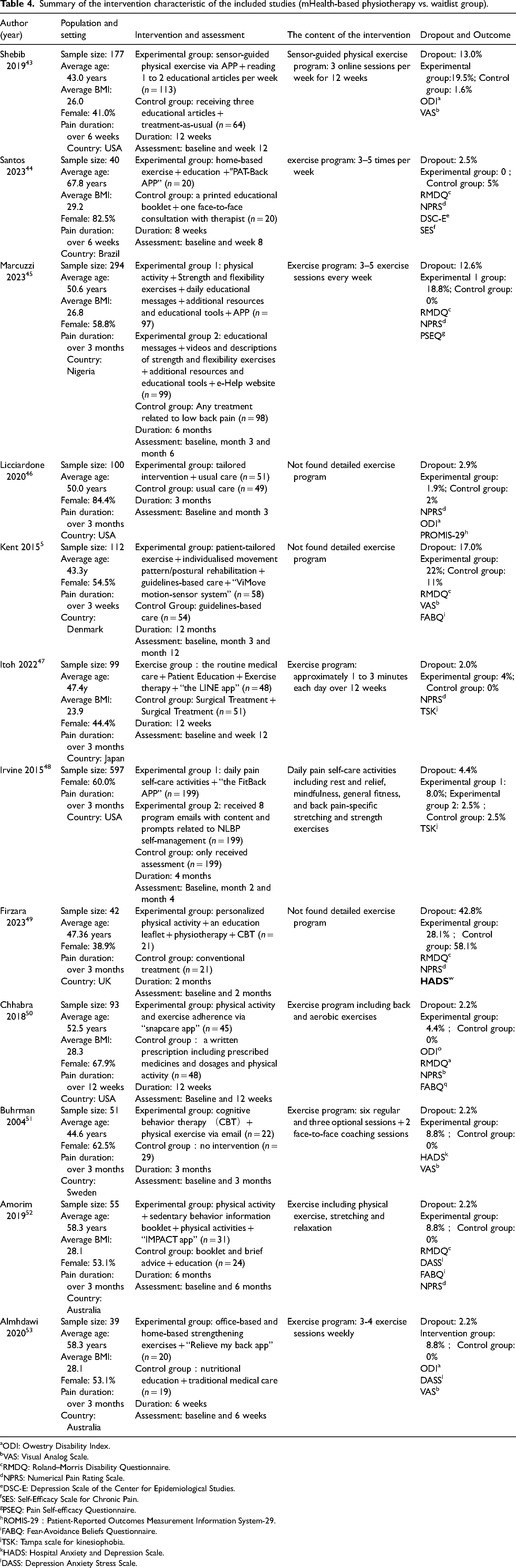
ODI: Owestry Disability Index.
VAS: Visual Analog Scale.
RMDQ: Roland–Morris Disability Questionnaire.
NPRS: Numerical Pain Rating Scale.
DSC-E: Depression Scale of the Center for Epidemiological Studies.
SES: Self-Efficacy Scale for Chronic Pain.
PSEQ: Pain Self-efficacy Questionnaire.
ROMIS-29:Patient-Reported Outcomes Measurement Information System-29.
FABQ: Fear-Avoidance Beliefs Questionnaire.
TSK: Tampa scale for kinesiophobia.
HADS: Hospital Anxiety and Depression Scale.
DASS: Depression Anxiety Stress Scale.
Risk of bias assessment
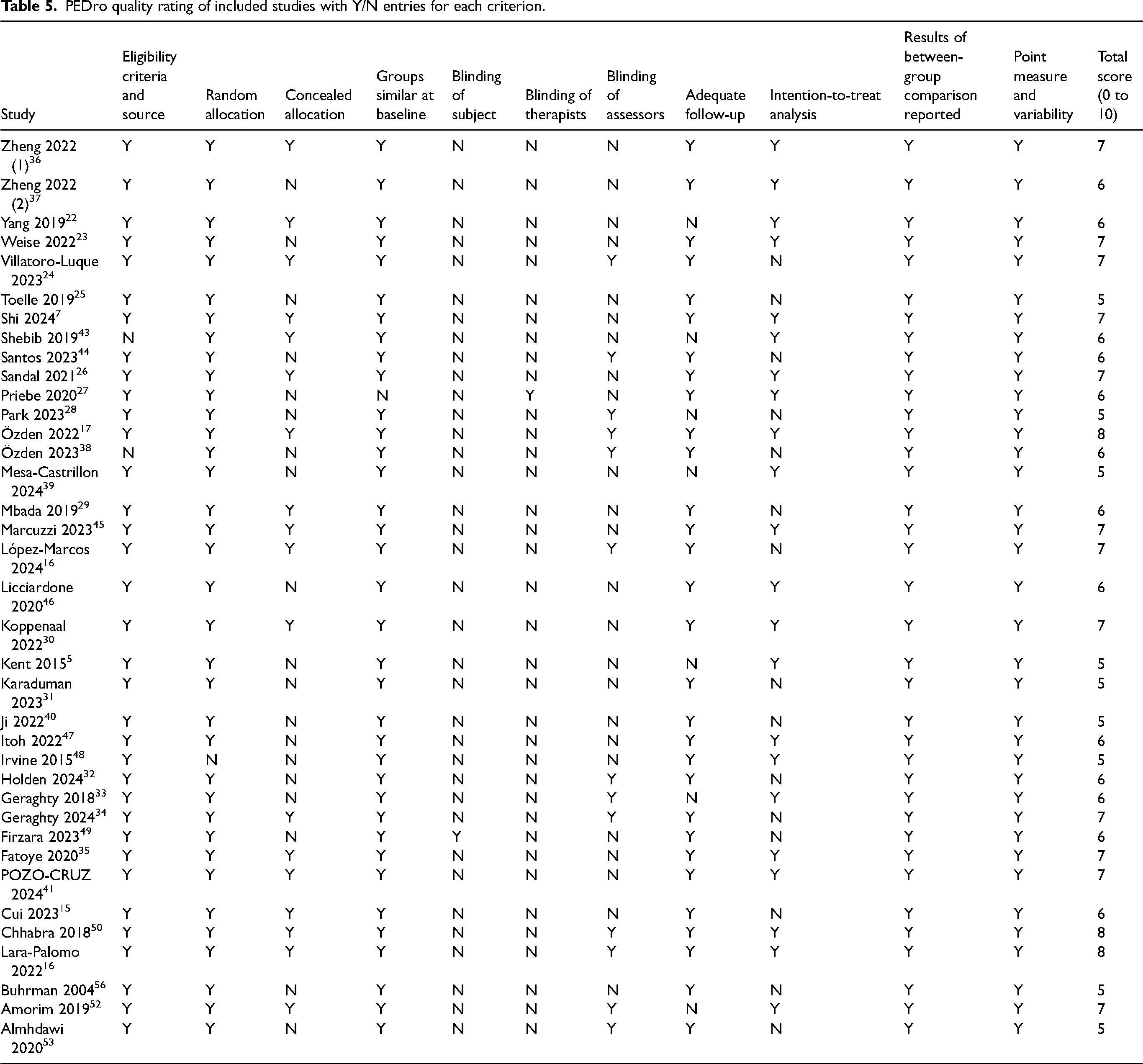
Among the 37 studies, the PEDro scores ranged from 5 to 8 points: 24.3% of the studies scored 5, 35.1% scored 6, 32.4% scored 7, and 8.1% scored 8 (see Table 5). The studies met the following PEDro criteria: random allocation (100%), allocation concealment (48.6%), baseline group comparability (97.3%), assessor blinding (35.1%), adequate follow-up (81.1%), intention-to-treat analysis, reporting of between-group comparison results (100%), and reporting of point estimates and feasibility (100%). One trial implemented blinding for participants, while another blinded the therapists, as this type of intervention is challenging to blind.
PEDro quality rating of included studies with Y/N entries for each criterion.
Meta-analysis results
Effect of mHealth-based physiotherapy on pain intensity
Among the 37 studies, 33 (89.2%) were included in the evaluation of the effect of mHealth-based physiotherapy on pain intensity.5,7,15–18,22–30,33,34,36–40,42–47,49–53 Twenty-three studies used the Numeric Pain Rating Scale (NPRS),7,15,16,23,25–28,30–34,36,37,39,44–47,49,50,53 and 10 studies used the Visual Analog Scale (VAS).5,16,17,22,29,38,40,42,43,51 The heterogeneity test revealed significant heterogeneity between the studies (I2 = 83%, P < 0.001), therefore a random-effects model was used for the analysis. The meta-analysis results indicated that, compared with the control group, mHealth-based physiotherapy had a moderate benefit in reducing pain intensity (SMD −0.32, 95% CI −0.48 to −0.17; P < 0.001; see Figure 27,15,17,18,22–30,33,34,36,37,39,40,42–47,49–53). Besides, the mHealth-based physiotherapy has a superior effect than the outpatient-based physiotherapy (SMD −0.25, 95% CI −0.49 to −0.01; P = 0.04; see Figure 27,15,22–34), home-based physiotherapy with simple supervision or without supervision (SMD −0.43, 95% CI −0.85 to −0.01; P = 0.05; see Figure 217,18,33,34,36–40,42), waitlist group (SMD −0.35, 95% CI −0.59 to −0.10; P < 0.001; see Figure 215,31,43–47,49–53).
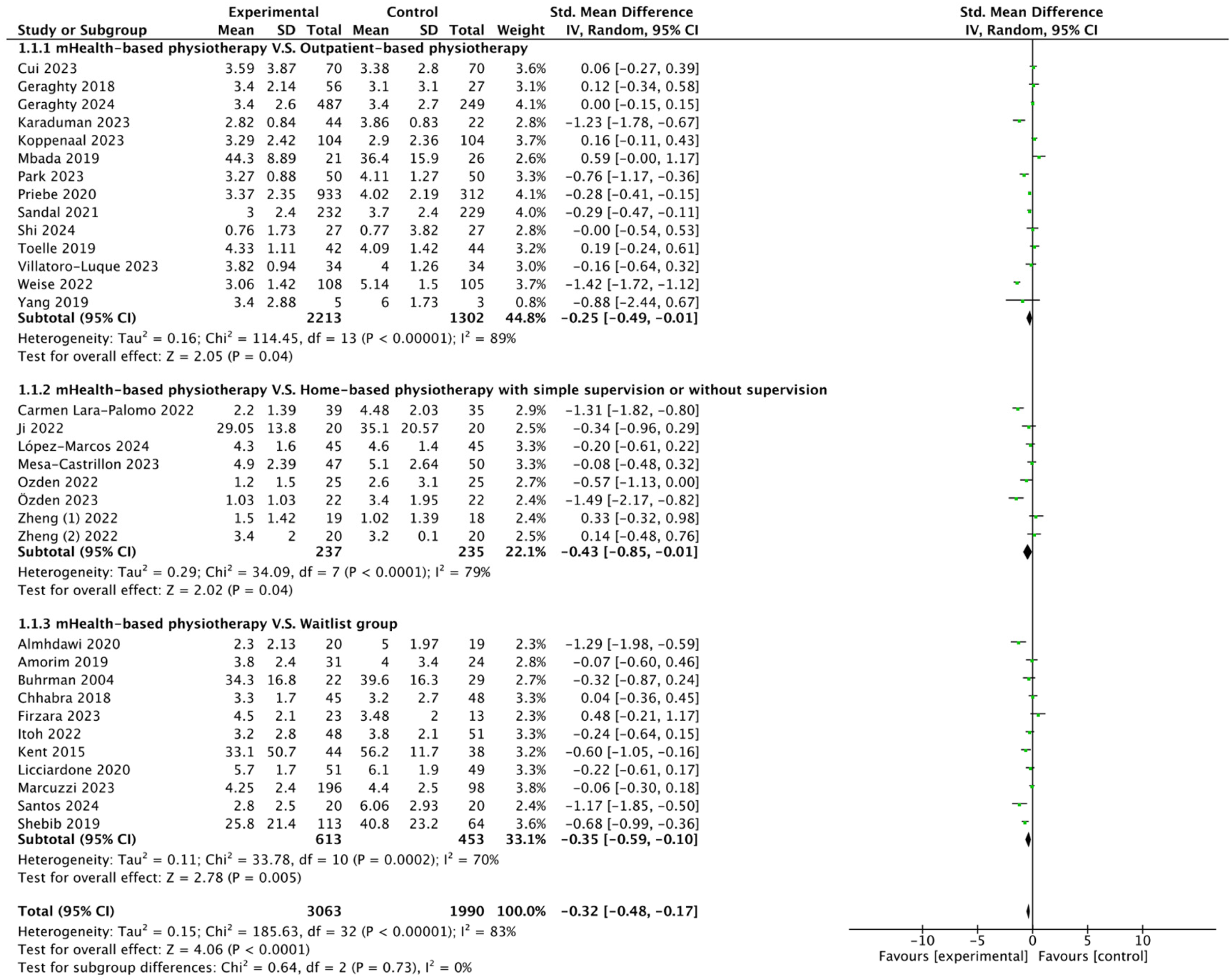
Forest plot of the effect of mHealth-based physiotherapy on the improvement of pain intensity.
Effect of mHealth-based physiotherapy on physical disability
Among the 37 studies, 32 (86.5%) were included in the evaluation of the effect of mHealth-based physiotherapy on physical disability.5,7,15,17,18,22,25–40,42–47,49,50,52,53 Fifteen studies used the Roland–Morris Disability Questionnaire (RMDQ),5,15,22,26,29,33,34,36,37,39,44,45,47,49,50,52 15 studies used the Oswestry Disability Index (ODI),7,15,17,18,28,30–32,35,38,40,42,43,46,53 and 2 studies used the Veterans RAND 12-Item Health Survey–Physical Component Summary Score (VR-12-PCS).25,27 The heterogeneity test revealed significant heterogeneity between the studies (I2 = 67%, P < 0.001), therefore a random-effects model was used for the analysis. The meta-analysis results showed that, compared with the control group, mHealth-based physiotherapy had a moderate benefit in improving physical disability (SMD −0.30, 95% CI −0.42 to −0.18; P < 0.001; see Figure 37,15,17,18,22,25–40,42–50,52,53). Besides, the mHealth-based physiotherapy has a superior effect than the outpatient-based physiotherapy (SMD −0.15, 95% CI −0.28 to −0.02; P = 0.007; see Figure 37,15,22,25–35), home-based physiotherapy with simple supervision or without supervision (SMD −0.57, 95% CI −1.02 to −0.12; P = 0.02; see Figure 317,18,36–40,42), waitlist group (SMD −0.32, 95% CI −0.51 to −0.14; P < 0.001; see Figure 35,31,43–47,49,52,53).
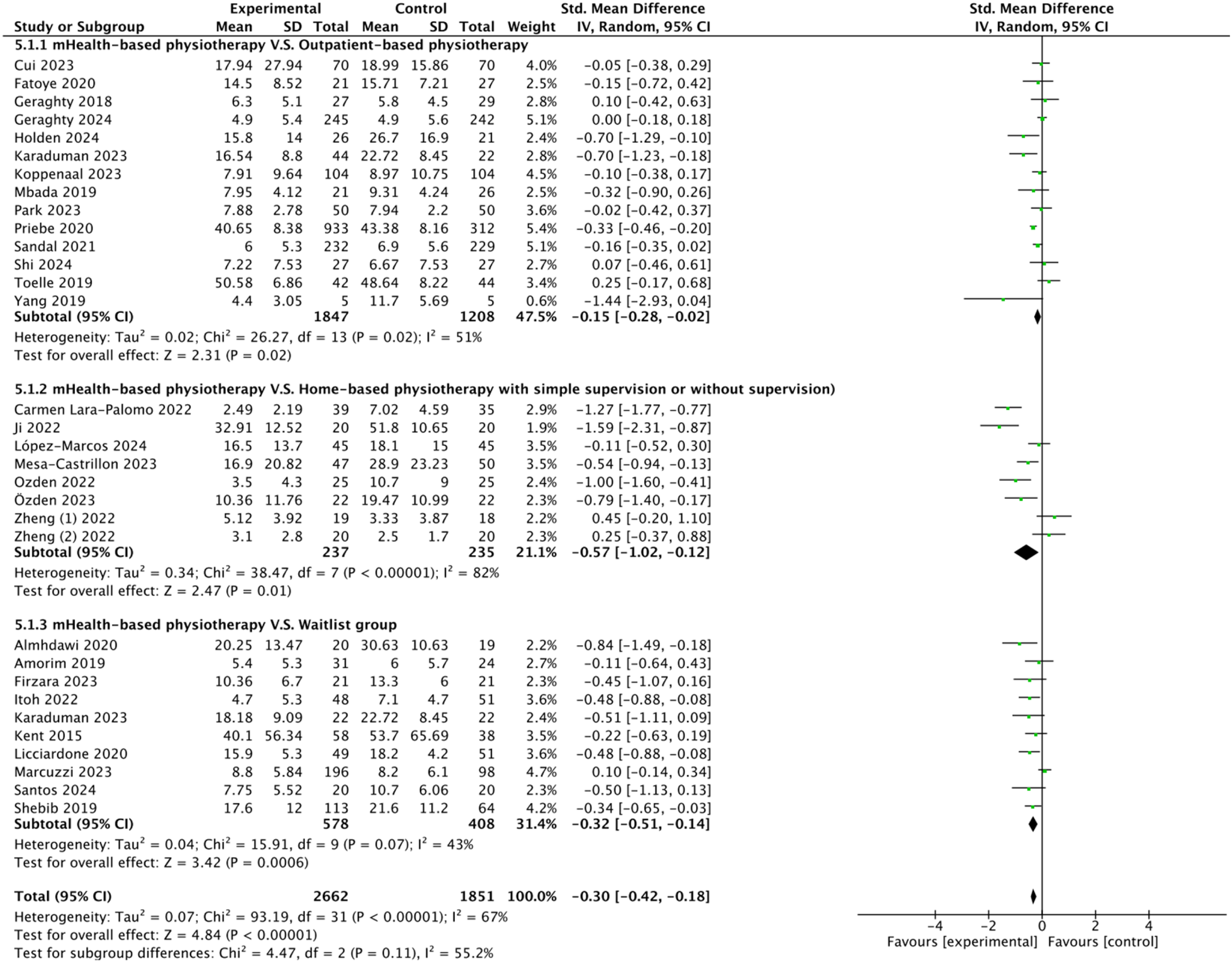
Forest plot of the effect of digital-based physiotherapy on the improvement of physical disability.
Effect of mHealth-based physiotherapy on depression, anxiety, fear-avoidance, and self-efficacy
Among the 37 studies, 17 (45.9%) were included in the evaluation of the effect of mHealth-based physiotherapy on depression7,15,17,18,22,25,27,36–39,42,44,46,49,51,52 The heterogeneity test revealed significant heterogeneity between the studies (I2 = 62%, P < 0.001), therefore a random-effects model was used for the analysis. No significant difference was found between the intervention group and the control group (SMD 0.18, 95% CI 0.01–0.31; P = 0.16; see Figure 47,15,17,18,22,25,27,36–39,42,44,46,49,51,52).
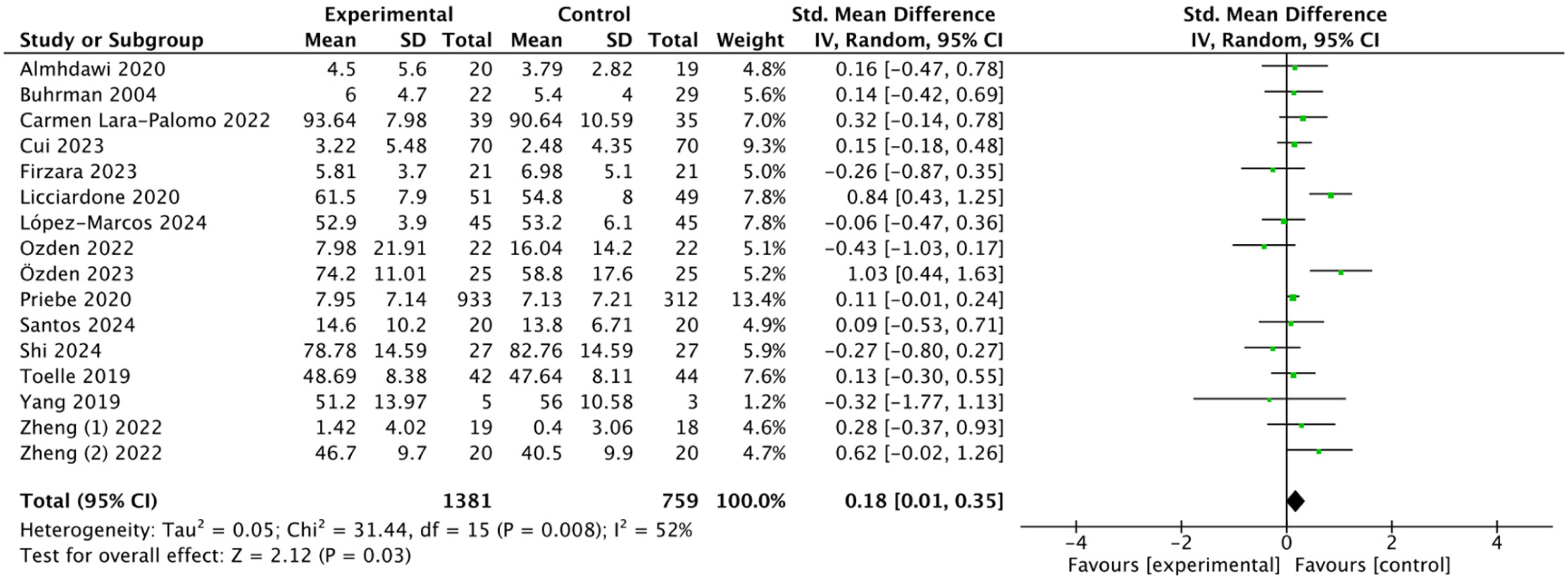
Forest plot of the effect of mHealth-based physiotherapy on decreasing depression.
Among the 37 studies, 8 (21.6%) were included in the evaluation of the effect of mHealth-based physiotherapy on anxiety.15,27,36,37,46,49,51,52 The heterogeneity test revealed significant heterogeneity between the studies (I2 = 57%, P = 0.02), therefore a random-effects model was used for the analysis. The meta-analysis results indicated that mHealth-based physiotherapy was less effective than the control group in reducing anxiety (SMD 0.29, 95% CI 0.06–0.52; P = 0.01; see Figure 515,27,36,37,46,49,51,52).
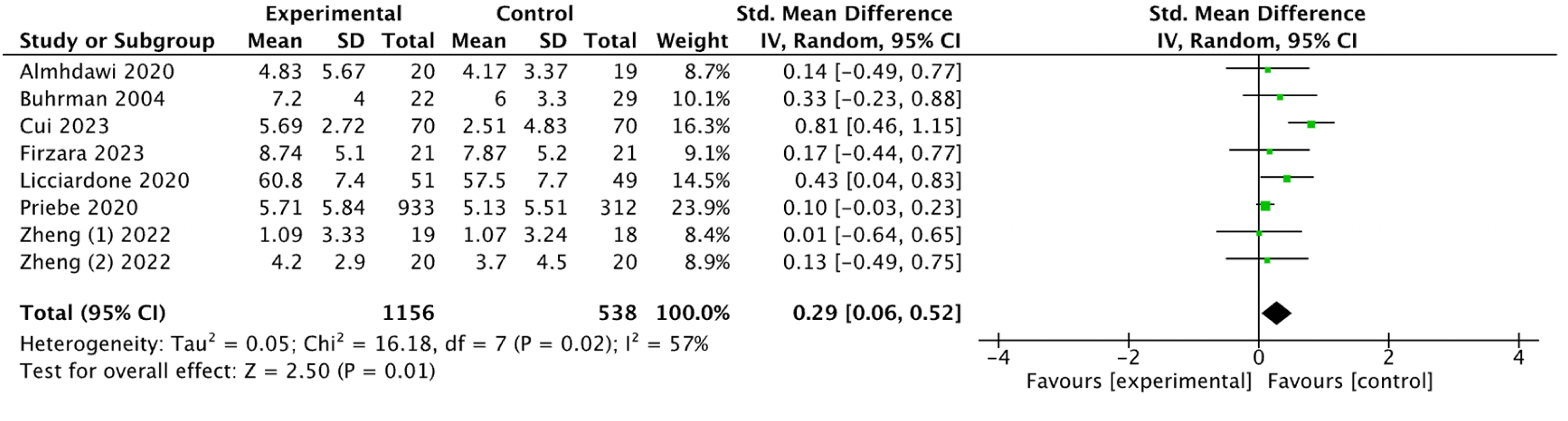
Forest plot of the effect of mHealth-based physiotherapy on decreasing anxiety.
Among the 37 studies, 13 (35.1%) were included in the evaluation of the effect of mHealth-based physiotherapy on fear-avoidance.7,15,17,18,24,30,31,33,34,36,37,47,48 The heterogeneity test revealed significant heterogeneity between the studies (I2 = 71%, P < 0.001), therefore a random-effects model was used for the analysis. The meta-analysis results indicated that, compared with the control group, mHealth-based physiotherapy had a moderate benefit in reducing fear (SMD −0.28, 95% CI −0.47 to −0.09; P < 0.001; see Figure 67,15,17,18,24,30,31,33,34,36,37,47,48).
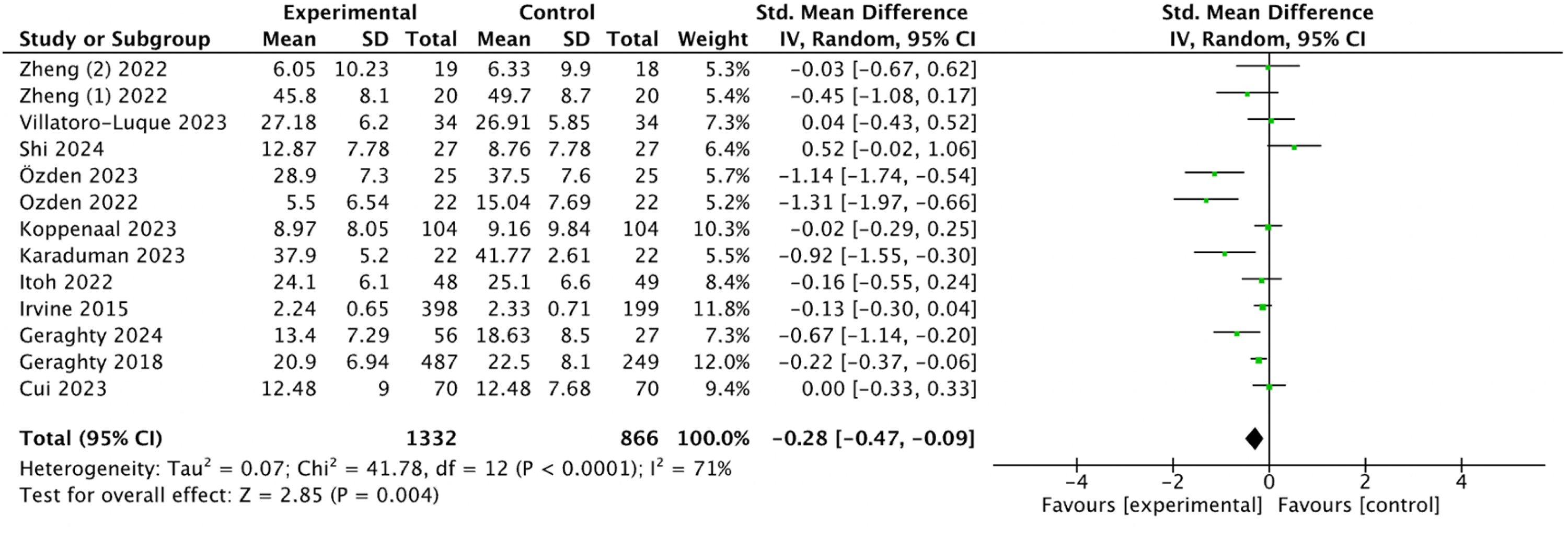
Forest plot of the effect of mHealth-based physiotherapy on reducing fear-avoidance..
Among the 37 studies, 8 (21.6%) were included in the evaluation of the effect of mHealth-based physiotherapy on self-efficacy.22,26,30,32,34,36,44,45 The heterogeneity test revealed significant heterogeneity between the studies (I2 = 66%, P < 0.001), therefore a random-effects model was used for the analysis. No significant difference was found between the intervention group and the control group (SMD 0.14, 95% CI −0.06 to 0.34; P = 0.18; see Figure 722,26,30,32,34,36,44,45).
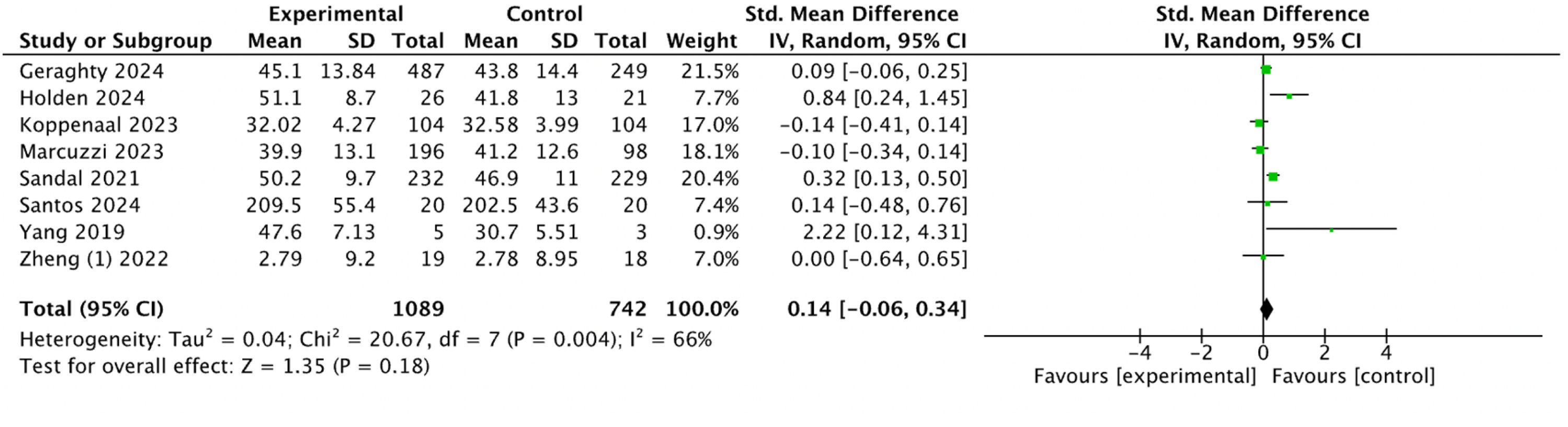
Forest plot of the effect of mHealth-based physiotherapy on the improvement of self-efficacy.
Sensitivity analysis
In this study, Stata 16.0 was used to conduct sensitivity analysis on pain intensity for evaluating the robustness and reliability of the results. The sensitivity analysis results demonstrated that excluding any single study did not impact the effect size of the mHealth-based physiotherapy on pain intensity (eFigure 1 in the Appendix 1), physical disability (eFigure 2 in the Appendix 1), depression (eFigure 3 in the Appendix 1), anxiety (eFigure 4 in the Appendix 1), fear-avoidance (eFigure 5 in the Appendix 1), and self-efficacy (eFigure 6 in the Appendix 1).
Publication bias
Funnel plots were used to assess publication bias in the effects of mHealth-based physiotherapy on pain intensity, physical disability, depression, anxiety, fear and self-efficacy and their funnel plots exhibited symmetrical patterns. In addition, our research team conduct Egger test for pain intensity (t33= −1.09, P = 0.286; eFigure 7 in the Appendix 1), physical disability (t32=-1.83, P = 0.077; eFigure 8 in the supplement 1), depression (t17 = 0.07, P = 0.946; eFigure 9 in the Appendix 1), anxiety (t8 = 0.93, P = 0.388; eFigure 10 in the Appendix 1), fear-avoidance (t13= −1.26, P = 0.388; eFigure 11 in the Appendix 1) and self-efficacy (t8 = 0.96, P = 0.375; eFigure 12 in the Appendix 1), and this results suggested no significant bias.
Discussion
Main findings
The aim of this systematic review and meta-analysis was to evaluate the effectiveness of mHealth-based physiotherapy for individuals with CNLBP in reducing pain intensity, improving physical disability, addressing psychological outcomes such as depression, anxiety, fear-avoidance and improving self-efficacy. In this research, mHealth-based physiotherapy demonstrated moderate benefits in reducing pain intensity (SMD −0.32, 95% CI −0.48 to −0.17; P < 0.001), improving physical disability (SMD −0.30, 95% CI −0.42 to −0.18; P < 0.001), and reducing fear-avoidance (SMD −0.28, 95% CI −0.47 to −0.09; P < 0.001) when compared to the control group. However, its impact remains unclear on improving individuals’ self-efficacy (SMD 0.14, 95% CI −0.06 to 0.34; P = 0.18) and decreasing depression (SMD 0.13, 95% CI −0.05 to 0.31; P = 0.16). In contrast, the effects of mHealth-based physiotherapy on decreasing anxiety (SMD 0.29, 95% CI 0.06–0.52; P = 0.01) were not as pronounced.
Effectiveness of mHealth-based physiotherapy for CNLBP patients
This review demonstrates that mHealth-based physiotherapy is more effective than outpatient-based physiotherapy, home-based physiotherapy with simple supervision or unsupervision and waiting-list groups in reducing pain intensity and improving physical disability, which is consistent with previous research findings.9,10 This suggests that mHealth-based Physiotherapy may offer a more effective approach for individuals with NCLBP compared to the traditional physiotherapy. Furthermore, mHealth-based physiotherapy can address common barriers, such as cost, time, and transportation issues and improve work production and adherence, allowing NLBP patients to consistently and correctly follow home-based exercise protocol, ensuring exercise quality while providing qualified guidance to a larger number of patients.9,10 Cui et al. found that mHealth-based technologies helps establish a strong alliance between patients and physical therapists, fosters frequent communication, and enhances patients’ understanding of LBP. 15
As is known to us, individuals with CNLBP always develop depression, anxiety, and fear-avoidance due to long-term pain and physical disability, and these psychological factors further make a negative impact on pain intensity and physical disability, and quality of life.54,55 The result of our research found the effect of mHealth-based physiotherapy has a moderate effect superior to the control group. However, mHealth-based physiotherapy did not show better effects in improving depression and anxiety. This may be due to the fact that the primary outcomes of studies included in this research were physical disability and pain intensity, and these studies more focused on reducing pain intensity and improving physical disability in individuals with CNLBP, not on alleviating depression and anxiety.17,25,36,38 However, previous studies has shown that mHealth-based psychological interventions for individuals with CNLBP and depression can effectively decrease individuals’ anxiety and depression compared to usual care group, but the interventions of these studies did not lead to significant improvements in individuals’ pain intensity and physical disability, due to the absence of mHealth-based physiotherapy components.55–58 For example, Baumeister et al. found after six months of mHealth-based psychological interventions, individuals with CNLBP and depression experience a more significant reduction of depression compared to the usual care group, but there was no notable improvement in their physical disability. 58 In the future, we could further explore the physical and psychological effect of mHealth-based physiotherapy combined with psychological interventions for individuals with CNLBP.
Previous research mostly concentrated on the effect of mHealth-based physiotherapy for individuals with CNLBP after short-term interval. For long-term follow-up, Sandal et al. found that app-based physiotherapy was more effective than outpatient-based physiotherapy in improving physical disability of NLBP patients after 9 months. 26 However, Geraghty et al. showed that there is no statistical difference between internet-based physiotherapy and outpatient-based physiotherapy, whether or not physiotherapist support was provided, in reducing pain intensity and improving physical disability. 34 These findings suggest that individuals with NLBP can effectively engage in self-management with the guidance of mHealth-based technologies.
Advantages and limitations
The advantages of mHealth-based physiotherapy have been identified. Initially, previous studies have shown that individuals with CNLBP who experienced mHealth-based physiotherapy had better adherence and engagement compared to those receiving traditional physiotherapy model.7,23,24 This may be due to the fact that mHealth-based technologies allow individuals with CNLBP to follow a flexible schedule for completing home-based exercise protocols, which undoubtedly offers convenience. Additionally, mHealth-based physiotherapy saves individuals’ time and expenses on traveling and treatment, thereby reducing their financial burden. 25
However, the widespread adoption of mHealth-based physiotherapy faces certain limitations, particularly in remote areas where many patients with CNLBP have limited internet access, preventing them from receiving mHealth-based physiotherapy. Besides, a large number of individuals with CNLBP are not aware of the importance of mHealth-based physiotherapy and find it challenging to accept this innovative model of physiotherapy.8,9
From the methodological perspective, this study has several strengths. First, we included 37 relevant studies, providing a robust dataset to evaluate the physical and psychological effectiveness of mHealth-based physiotherapy. Besides, our research team minimized bias by having at least two independent reviewers assess the study inclusion criteria, data extraction, risk of bias, and certainty of the evidence. Nevertheless, there are several limitations to consider. First, there is some clinical heterogeneity in the interventions across the studies, but we have defined mHealth-based physiotherapy as home-based exercise programs guided by smartphone apps, internet-based systems, web interventions, and “app + sensors.” Additionally, our literature search was limited to English-language studies, which may have introduced language bias, potentially affecting the generalizability of the findings. Furthermore, due to the nature of the interventions, some studies may have been susceptible to bias, such as the lack of blinding for participants and therapists.
Conclusion
The results of this systematic review and meta-analysis strongly suggested that mHealth-based physiotherapy is more effective in reducing pain intensity and improving physical disability for patients with CNLBP than traditional physiotherapy model, especially outpatient-based physiotherapy, which means that mHealth-based physiotherapy can provide opportunities for individuals who lack access to professional physiotherapy services. Compared to traditional physiotherapy, this studies found that mHealth-based physiotherapy has a better effect in reducing individuals’ fear-avoidance, but it was less effective in alleviating depression and anxiety, and improving self-efficacy, which might be due to the fact that mHealth-based physiotherapy of studies included in this review did not combined with the psychological interventions.
Supplemental Material
sj-docx-1-jtt-10.1177_1357633X251340037 - Supplemental material for The physical and psychological effectiveness of mHealth-based physiotherapy for patients with chronic non-specific low back pain: A systematic review and meta-analysis
Supplemental material, sj-docx-1-jtt-10.1177_1357633X251340037 for The physical and psychological effectiveness of mHealth-based physiotherapy for patients with chronic non-specific low back pain: A systematic review and meta-analysis by Weihong Shi, Lixia Chen, Yuhang Zhang, Wangshu Yuan, Qing Li, Zhengwei Chen, Houqiang Zhang, Qiyang Feng, Yingshan Gan, Huiling Zhang, Di Liu and Ye Lin in Journal of Telemedicine and Telecare
Footnotes
Author contributions
The inception of the study was facilitated through the collaborative efforts of Weihong Shi, Lixia Chen and Wangshu Yuan. Di Liu, Yingshan Gan and Weihong Shi undertook the experimental procedures and were responsible for the composition of the manuscript. The quality of papers was evaluated by Weihong Shi and Yuhang Zhang. The data extraction of papers was conducted by Zhengwei Chen and Qing Li. Substantial contributions to the analysis and preparation of the manuscript were made by Qing Li, Houqiang Zhang and Huiling Zhang. Qiyang Feng executed the data analyses, and Zhengwei Chen played a crucial role in the analytical process through constructive discussions.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: National High-Level Hospital Clinical Research Funding (grant number 2022-PUMCH-B-053).
Data availability statement
The data generated during this study are available from the corresponding author upon reasonable request. All data supporting the findings of this study are included within this published article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
