Abstract
Objectives
The introduction of medical revalidation in 2012 has been a controversial and radical change to medical regulation in the UK. It involved changes to the way organizations manage medical performance, and to the relationships between doctors, their employers and the professional regulatory body. In this paper, we explore the implementation of medical revalidation, analysing the change process and its consequences for doctors and organizations.
Methods
We conducted a qualitative investigation of the implementation of revalidation in 15 case study organizations in 2016–2017, collecting documents and undertaking a total of 80 interviews with medical and non-medical staff. We used Normalization Process Theory to frame and structure the analysis.
Results
Revalidation reforms were largely implemented successfully within and across our case study organizations, with evidence of growing acceptance of the purpose and processes of revalidation. There was an emergent shift from securing doctors’ compliance towards the use of revalidation to strengthen clinical governance, and towards evaluating revalidation processes and seeking to make them more effective. However, there was substantial variation in the implementation and impact of revalidation; it was still not fully understood by many doctors, and revalidation processes were highly reliant on a few key individuals in each organization. The changes brought about by revalidation have had consequences for the way in which doctors construct their identity and the way they relate to the organizations in which they work.
Conclusion
Despite considerable early scepticism and overt opposition in the medical profession, revalidation has become gradually accepted, embedded and even valued over time. Its impact and effectiveness are still questioned by many stakeholders, and the focus of attention has now shifted towards revising and improving the way revalidation works in practice.
Keywords
Introduction
Medical revalidation requires all licensed doctors to demonstrate they are up to date and fit to practise. Introduced in the UK in 2012, 1 it involved changes to the way organizations manage medical performance, and to the relationships between doctors, their employers and the professional regulatory body. Extending regulatory oversight of doctors’ practice throughout their post-qualification careers, revalidation has brought professional regulatory activity and oversight formally into the organizational sphere for the first time, providing considerable statutory legal powers and duties which fall upon doctors’ employers. Revalidation has repositioned where regulatory practices occur, now taking place in contexts in which complex and varied managerial and governance systems exist.
Before the introduction of revalidation, the UK General Medical Council (GMC) mainly regulated doctors’ practice and behaviour after qualification and admission to the register through its fitness to practise procedures in instances of alleged misconduct. 2 Employers in the National Health Service (NHS) mostly dealt with performance concerns informally, and their links to the professional regulator were limited. 3 This form of regulation became increasingly challenged, which resulted in debate over regulatory reform 4 that was further shaped by a series of high-profile incidents of gross medical misconduct in England.5,6 In response, the governance of the GMC was reformed while fitness to practise proceedings were also changed, along with the introduction of arrangements for independent adjudication and appeals against unduly lenient decisions.7–9 In parallel, and after an extended period of contentious policy development, a new system of medical revalidation was introduced, representing the most significant and far-reaching element of these regulatory reforms.
Revalidation is a continuing competency system carried out in five yearly cycles. All licensed doctors who are not in training must take part in the annual appraisal for which they need to provide and reflect on, among other things, continuing professional development (CPD), significant events, review of complaints and compliments, quality improvement activity and feedback from colleagues and patients. They have to be connected to one organization (‘designated body’), a ‘Suitable Person’ or report back to the GMC directly. Designated bodies have to provide a senior doctor as Responsible Officer (RO) who ensures that every doctor has a regular appraisal, is supported by an up to date appraisal system with sufficient trained appraisers, and that clinical governance systems are in place that provide supporting information, policies and systems for identifying and responding to concerns about doctors. Organizations have to link with other organizations where their doctors also work, so that information about their practice can be shared. The RO can make one of three possible revalidation recommendations to the GMC: revalidation, deferral (requesting the GMC to give more time for a recommendation to be made) or non-engagement (which can lead to the doctor losing their licence to practise). 10
Our earlier work on the initial stages of the implementation of revalidation suggested that senior leaders gradually recognized the benefits of revalidation and became more accepting of it, but that revalidation had yet to be fully embedded, and scepticism about its value remained. 11 Little is known about the experience of those operationalizing revalidation ‘on the ground’, however, with formal evaluations of the introduction of revalidation in organizations lacking. Also, at the time of our earlier study, not all doctors had experienced revalidation. Indeed, the first full five-year cycle of revalidation was completed in 2017 only, making this paper, which analyses the implementation of how doctors and organizations experienced revalidation, particularly timely.
As in our previous study, 11 we used Normalization Process Theory (NPT) to help understand the implementation process through analysing interventions in relation to the work people do to implement them. 12 NPT has been successfully used to examine a wide range of clinical working practices, making it particularly applicable to the study of revalidation. 13 We used NPT to assess the implementation of revalidation across a wide range of organizations, and from the perspective of those people, clinical and non-clinical, operationalizing and ‘doing’ revalidation on the ground. Revalidation is a practice, and the medical profession’s acceptance and attitude towards it is crucial for implementation. NPT provides a lens to investigate the acceptability of this change and gain an understanding of how willing people are to engage in and adapt the practice of revalidation both in the medical profession and the organizations in which they work. We thus extend the existing use of NPT, which has predominantly been used to study the introduction of new clinical techniques, guidelines or practices at a micro level, by applying the theory to an organizational intervention introduced as a result of national health policy and legislation.14,15
Methods
This study draws on qualitative data to understand how revalidation has been implemented during the first five years. Ethical approval for this study was awarded by the University of Manchester Ethics Committee (REC 15028). Fifteen health care organizations were recruited through purposeful sampling following a national survey of ROs, to ensure coverage across types, settings, performance (appraisal rates; self-assessment) and geography. 16 In contrast to our previous study, which focused on policymakers and senior national professional leaders, this study centred on clinical and non-clinical staff who were directly involved in, or who experienced impact from, the implementation of revalidation in their organization. 11 We generated a list of potential interview participants based on information from organizational policies, board reports and role descriptions relating to revalidation or the management of medical work, resulting in 80 interviews with 79 participants, with one participant interviewed twice. Very few participants declined to be interviewed; when this did occur it was because individuals understood their role to not be relevant to the study, and predominantly coincided with the individual in question referring us to a more appropriate colleague. Roles held by participants included those with specific or obvious revalidation duties such as ROs, appraisal leads and appraisers, but participant recruitment also extended across wider organizational management structures including directors of fitness to practise, human resources, and professional practice, complaints managers, practice managers and medical directors. Twenty-one participants worked in primary care organizations and 58 in secondary care. The recruitment of participants varied according to organization type and size; it was guided by reviewing organizational structures and policies and drew on a snowball strategy or referrals from other interview participants. Participants were approached either via email or phone, depending on the contact details provided by gate keepers in each organization. The study and nature of data collection were fully explained and a participant information sheet and consent form provided in order to ensure participants could make an informed decision on whether or not to part take in the research. All participants provided written informed consent.
Interviews were carried out between 2016 and 2017 by seven researchers. Initially interviews were conducted in pairs to help provide consistency as well as an interview schedule being used by all researchers. Following this a combination of individual and paired researcher interviews were carried out with regular debriefing and discussion meetings to reflect on interviews and the interviewing experience. The research team developed an initial interview guide based on reviewing organizational policy and job description documents and from reviewing literature on the management of medical performance. Having conducted initial analysis on the first round of interviews, we developed a second interview guide to further explore emerging themes and to fill gaps in the data to reach a point of apparent data saturation. 17 Interviews were conducted in person or by telephone, according to participants’ preferences. All interviews were digitally recorded, transcribed and imported into Dedoose qualitative analysis software. 18
We developed a coding framework from the four domains and sub-domains of NPT (Table 1), using an adapted version of the NoMAD instrument, which was developed to assess implementation processes. 13 This instrument was then applied to transcripts by coding evidence of the sub-domains. Four researchers analysed the transcripts independently. Dedoose was used to enable blind coding verification of code application to check consistency of analysis. Coding and interpretations were discussed at regular intervals throughout the analysis phase of the study during collaborative meetings with all authors.
Adapted NoMAD instrument.
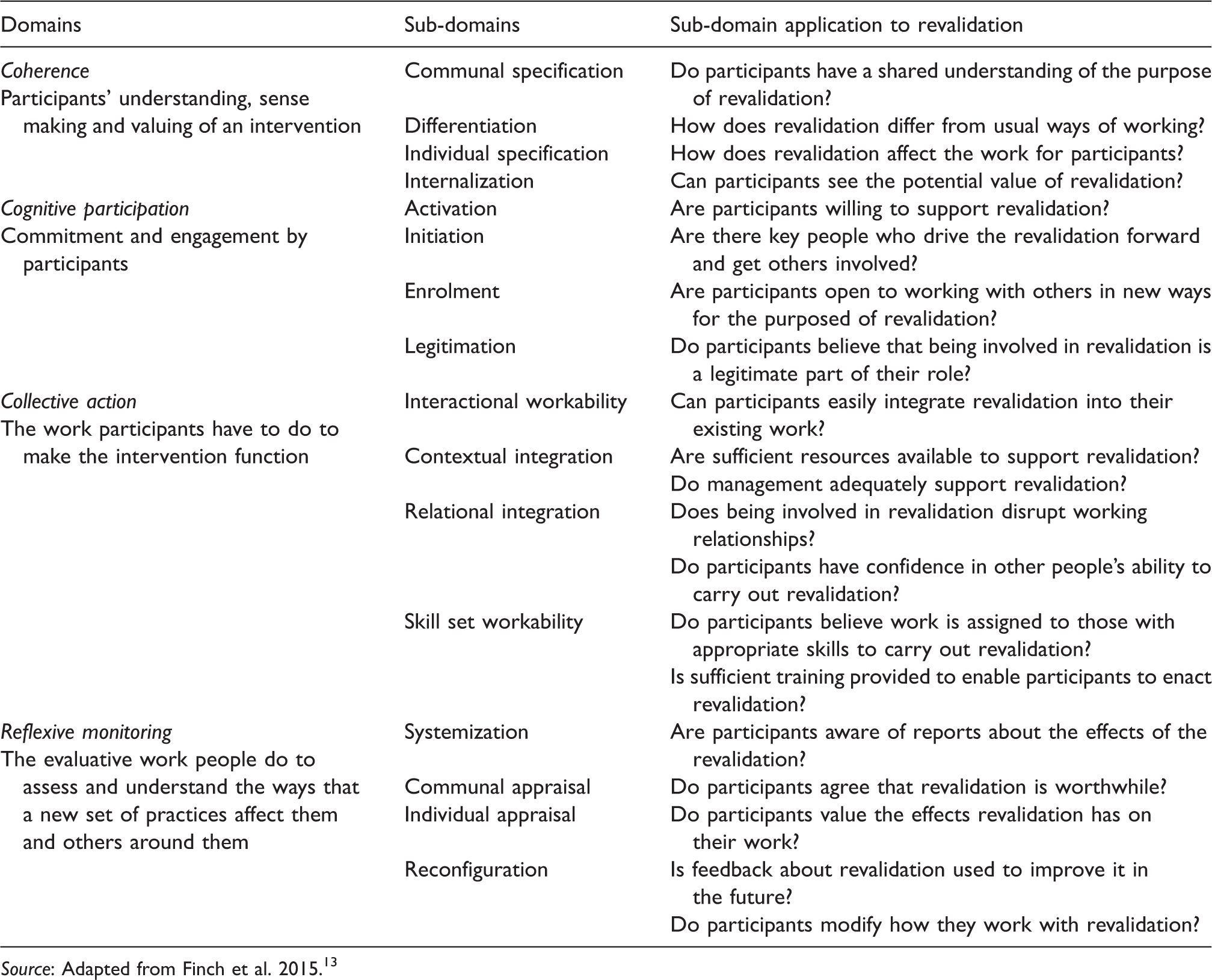
Source: Adapted from Finch et al. 2015.13
Results
We found evidence of all the NPT domains in our data. The degree and form of each domain’s presence provided insight into how the implementation of revalidation was experienced and operationalized in practice. It also highlighted how successful or not the organizations we investigated were at embedding the policy and securing acceptance of revalidation within the medical profession. Table 2 provides a selection of interview excerpts to illustrate and evidence the presence of each domain.
Analysis of interview data by Normalization Process Theory (NPT) domains: sample excerpts.

RO: responsible officer; HR: human relations; AMD: assistant medical director; CQC: Care Quality Commission..
The following four sections explore our findings further, covering each of the NPT domains and subdomains as set out in Table 2.
Coherence
Participants on the whole held a shared understanding of the objectives of revalidation. It was understood by most as a necessary form of regulation that aims to improve patient safety through ensuring doctors are up to date and fit to practise, and to identify and offer support for struggling doctors. There was less consensus in understandings of the outcomes of revalidation, especially deferral. Doctors in non-standard roles such as locum doctors (doctors who work short term in the place of the regular doctor when that doctor is absent or when a hospital or practice is short staffed), whose way of working conflicted with the formalized requirements of revalidation, were noted to be more likely to lack a full understanding of the process. Overall, however, knowledge had increased as people had gained experience of the revalidation process.
When differentiating the changes revalidation brought to ways of working, participants focused on the formalization of clinical governance systems, such as the linking or integration of previously separate areas of clinical governance. This was seen to have facilitated the collection of information for clinical governance and communication between teams, which positively impacted participants’ work. The introduction of the RO role in particular was stated to have significantly increased these connections. Participants also indicated that revalidation helped to clarify quality improvement activities, by creating a clear structure for them to function within.
Participants expressed a general acceptance of the need for greater scrutiny of the medical workforce and of medical revalidation as a legitimate means to achieve this. The value of revalidation was demonstrated through explicit comments and reports of engagement with the policy (Table 2). Positive perceptions of revalidation were understood to have increased over time as the profession and others involved in the policy gained greater clarity through having to operationalize it.
Not all valued revalidation, however, for two main reasons. Firstly, there was scepticism that it would identify poor performance or impact clinical practice. Participants expressing these views tended to see revalidation as purely administrative in function. A minority stated that revalidation would not deal effectively with very poor or dangerous practice by doctors who actively sought to conceal problems. Secondly, some thought that revalidation was simply duplicating other areas of clinical governance, making it unnecessary as its goals could be reached by existing systems or regulatory bodies.
Cognitive participation
All case study organizations had implemented a system of revalidation and revalidated the majority of their doctors. The compulsory nature of the policy meant that ‘willingness’ to support revalidation was in part because doctors and organizations had no choice. At an organizational level, support was evident through a willingness to appoint new posts, restructure ways of working and provide resources (to varying degrees). At an individual doctor level, most were reported to be willing to comply with this requirement, and increasingly so.
Although the majority of doctors were reported to engage willingly with revalidation, an ongoing push was still identified as necessary. Chasing was required, described as an ongoing task for revalidation teams, especially administrative staff. Non-engagement became being less tolerated and more directly challenged. Organizations were described as becoming stricter in their approach to engagement and being more likely to take action, and there was a perception that the GMC did so, too.
Key individuals driving revalidation forward were identified and described as pivotal to initial implementation, changing attitudes and the continued successful running of revalidation. ROs and their support staff (most frequently a medical staffing and revalidation team) were identified as those occupying these driving roles. Having strong leadership by an individual or team understood to be knowledgeable and supportive seemed to contribute to engagement levels. Those able to effectively communicate with their doctors and allay concerns appeared to be successful in ensuring engagement, making the process less onerous for all involved.
Revalidation was seen to have brought change to the way doctors and other staff worked with others both internally and externally. People were reorganizing themselves, new groups had been put in place to manage the requirements of the revalidation process alongside some new appointments. These changes were reported as being positively received and responded to, but this perception varied between organizations.
Change had also occurred in the ways that designated bodies worked with external partners. The passing of information between organizations as doctors moved was stated to occur to a better standard than previously and more frequently. At the same time, the ability to share information was seen to be hampered by inconsistent use of IT systems across organizations.
Revalidation and the changes it brought were perceived to be most legitimate by those involved in running the process, in particular ROs and revalidation teams. This is perhaps unsurprising given the individual investment in the policy that their roles required. While many doctors on the ground were said by participants to have accepted revalidation, for some it was seen as a bureaucratic, tick box exercise which detracted from their clinical role. There was also a perception by a small number of participants that some senior doctors were unwilling to or displeased about being appraised by others. Further, not all doctors accepted the disclosure of private practice as part of the appraisal process, which some viewed to be outside the remit of NHS designated bodies. This is despite appraisal requiring to cover doctors’ full scope of practice. A generational difference was also reported, which was seen to be the result of differences in training, with younger doctors identified as more accepting of such oversight than older doctors.
Collective action
Our data revealed that there had been some initial difficulty in setting up and integrating revalidation into existing work patterns, with four main reasons identified: initial resistance; the newness of the policy; poor existing clinical governance systems and preparation for the introduction of revalidation, and lack of resources. Integration became easier and more successful over time, but this was largely dependent on an organization’s preparation and planning for revalidation as well as organizational culture. Those for whom it meant the biggest change to existing ways of working found integration of revalidation most challenging, in particular those in poorly resourced or less supportive organizations. Similarly, doctors whose working context meant that they were distant from their organization, transient or did not work within an organization found integrating revalidation difficult due to the lack of organizational support they could access.
The availability of resources and management support for revalidation was key to how easily individual doctors were able to integrate it into their existing work, in particular protected time, IT systems and administrative support. Time was one of the most under-resourced areas and numerous individuals highlighted that their organization had not provided protected time for revalidation roles, or provided administrative support to operate the policy. This meant that the preparation revalidation required of individual doctors, those being appraised and those conducting appraisals, was experienced as a burden requiring work in personal time outside of formal working hours. Poor organizational and IT systems were also identified as problematic, making it difficult to gather the data doctors needed for their appraisal and revalidation. It was argued that if these systems were improved it would make undertaking appraisal and revalidation more straight forwarded. Lack of resources was not always within local control however; issues such as an inability to recruit the required staff were understood as challenges facing the health care system in England more broadly.
Many of those involved in operationalizing revalidation noted to lack confidence in the ability of others to carry out its requirements appropriately, referring both to doctors going through the system and those running it. This was mostly seen as an indication of adapting to the newness of the policy rather than specifically about revalidation itself. Lack of confidence was for example commonly noted to result from individuals being unable to fit training into their work, or that training opportunities provided by organizations were inadequate. However, confidence was seen to be ‘restored’ once identified training needs had been addressed and indeed, confidence in the ability of those assigned tasks to fulfil them was, for the majority, high. Concerns remained in regards to succession planning, with participants noting that knowledge and ability to run revalidation within organizations was held by and reliant on a few ‘in the know’. With the exception of succession planning, once the necessary systems had been put in place and training delivered, revalidation was described as running smoothly for most.
Reflexive monitoring
At the time of this study, the organizations being studied had revalidation systems up and running, with most of their doctors having completed the first five-year cycle of revalidation. Many organizations had undertaken audits of the quality and effectiveness of revalidation systems or these were underway, while formal assessments of the impact of revalidation on performance and patient care were, on the whole, yet to be undertaken.
Many participants spoke of the effects and impacts of revalidation on practice and the organizations in which they worked, based on their own informal assessment of the system as individuals and communally with colleagues. Most believed revalidation to be worthwhile, with different explanations provided. Revalidation was believed, for example, to have improved continued professional development and keeping doctors up to date; reflection, leading to improvements in patient safety; the quality of appraisal and the appraisal process (record keeping, formalization); doctors’ behaviour to other staff and the likelihood of concerns about or behavioural difficulties of a doctor being dealt with.
The majority of those interviewed spoke of the impact of revalidation at a distance from themselves, highlighting changes of the profession at large or at an organizational level rather than their own practices. Perceived impacts depended on the role of the individual. Those in management saw revalidation as offering them a better oversight of other doctors’ practices and more authority, enabling them to better perform management duties. But this also meant an increased workload. At the individual level, revalidation was mostly seen to have increased and improved reflection, as noted, and some identified this as improving practice although many did not make this link. Non-clinical staff involved in revalidation within organizations reported significant changes to roles, increased ability to get doctors to engage and more authority to ensure compliance.
We noted earlier that there was a minority of those interviewed who did not perceive revalidation to be worthwhile. Further, some participants noted an awareness of others in the profession who did not view revalidation to be of value, highlighting that negative views were discussed by colleagues across organizations. Questions about the effectiveness of revalidation were further fuelled by the observation in some organizations that revalidation had failed to pick up serious patient safety concerns.
The requirements of revalidation are uniform for doctors nationally, but organizations approached it differently, adapting it to fit best with existing systems, agendas and ways of working. The tailoring of revalidation in this way was often a practical approach to resource constraints and a result of ongoing assessments of revalidation systems both formally and informally. In most organizations, this came following an initial phase of ‘getting it in’. Once this point had been reached, a gradual increase of feedback was said to occur and was used to improve the efficiency and quality of revalidation systems. Interview participants spoke of an increased focus on the quality of systems in place and the information and material used for revalidation. This was most evident in relation to appraisal, particularly supporting information and appraisal reports. Work was also described as beginning in terms of strengthening the triangulation of information and better connecting revalidation to wider clinical governance systems to support organizations in their clinical governance and ability to monitor doctors and patient safety.
Discussion
In this paper, we have assessed the implementation of revalidation across a range of organizations using NPT as a framework for analysis. We found that, overall, in NPT terms, coherence was achieved by most organizations, although not completely. Much of the impact on organizations and doctors’ practice occurred as an indirect result of the work that revalidation required organizations to do on their existing systems. There remained a lack of coherence in terms of participants’ understanding of the revalidation process and its requirements.
Cognitive participation had also been achieved to a degree and it had enabled implementation, although this was in places limited. We found that all the organizations included in this study had sufficient support from clinical and non-clinical staff to get revalidation up and running. The mandatory requirement for revalidation was seen as essential to its implementation, especially since support and acceptance of it was gradually acquired via experience rather than in the initial stages. This suggests that if the process had been voluntary, it would have been unlikely to have been taken up or supported to the same degree.
Organizational context was the most significant factor determining doctors’ and non-clinical staffs’ experience of revalidation and the likelihood of successful collective action. Context here refers to organizational size and type, resourcing, culture and organizational history. These findings echo those of Spendlove’s recent research on revalidation, which focused on a single organization. 19 Reflexive monitoring had begun to take place, too. Organizational systems were planned to be appraised and audited by most organizations. There were informal discussions on the impact of revalidation on practice and performance but none of the organizations studied had formally assessed the impacts of revalidation as yet. Most, but not all, participants believed that revalidation was worthwhile due to perceived improvements since its introduction.
Approaches to revalidation varied across organizations, which were described as tailored to the needs, agendas and resources of each. There was thus limited consistency in the experience and delivery of revalidation. Given that many of the issues faced by organizations in the implementation of revalidation were seen to be the result of newness and unfamiliarity with systems, this multiplicity raises questions about what is legitimate variation and what is inconsistency. Variation between organizational approaches could be interpreted as revalidation being used by organizations to fit their own agendas, or as a consequence of the medical profession shaping revalidation in a way that might avoid the full scrutiny of the policy. 19 At the same time, a ‘one-size fits all approach’ of revalidation may be inappropriate, given that individual doctors’ practice and working circumstances vastly differ as do the organizations in which they work.11,16 From this perspective, the tailoring of revalidation can be understood to be necessary for its implementation and potentially contributing to existing acceptance, while also beneficial to its chances of long term acceptance and embedding in everyday work.
Overall, our findings suggest that nationally developed and led policy initiatives such as revalidation need to be sufficiently flexible to allow organizations to implement them in a way which capitalizes on existing systems, and be appropriate for the specific organizational context. The success and ease of implementation of organizational change depend on a number of local factors, notably the existence of relevant organizational policies and processes, which means that a better understanding of such policies and processes would be beneficial to inform policy development. There is a particular need to better address the challenges faced by those groups of doctors for which revalidation has been identified as particularly problematic, such as locums and those with a portfolio career. In addition, organizations that experience tension between revalidation and the running of business, such as private agencies, require further attention. By changing the relationship between doctor and organization, revalidation has implications for professional identity in medicine and how it is enacted and performed. 20
The use of NPT to explore the implementation of revalidation in this study has extended the usual parameters of the theory. We have noted earlier that existing work that has used NPT in health care has explored implementation of clinical and behavioural practices at an individual level rather than those at an organizational level.15,21,22 Our use of NPT in this study demonstrates its value for exploring and analysing the implementation of interventions within the health care setting at organization and system levels and perhaps of other complex social interventions and policies outside of this setting.
Conclusion
This study explored the implementation of medical revalidation, which was introduced in the UK in 2012, analysing the change process and its consequences for doctors and organizations. We found that despite considerable early scepticism and overt opposition in the medical profession, revalidation has become gradually accepted, embedded and even valued over time. Its impact and effectiveness are still questioned by many stakeholders, and the focus of attention has now shifted towards revising and improving the way revalidation works in practice.
Footnotes
Acknowledgements
The authors would like to thank all the interviewees for taking part.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
Ethical approval for this study was awarded by the University of Manchester ethics committee (REC 15028). All participants provided informed consent for themselves prior to being interviewed.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study is an output from independent research commissioned and funded by the Department of Health Policy Research Programme (PR-R9-0114–11002) Evaluating the development of medical revalidation in England and its impact on organizational performance and medical practice.
