Abstract
Background:
Higher levels of physical activity (PA) among youth with multiple sclerosis (MS) associate with lower levels of disease activity, and better psychosocial outcomes. Yet, youth with MS remain inactive. Built-environment features may explain low PA and inform intervention design.
Objectives:
This cross-sectional study examined associations between built-environment features and PA levels among youth with MS.
Methods:
Youth (⩽18 years) with MS completed the Godin Leisure-Time Exercise Questionnaire (GLTEQ) for overall PA and a health contribution score (HCS; moderate & vigorous PA) in metabolic equivalents (METs). Built-environment features (intersections, green space, Walk/Transit Score) were linked to postal codes using the CANUE repository. Associations were analyzed using Spearman’s correlation.
Result:
Our sample included 59 youth (median age 15 ± 3 years; 61% female). Median GLTEQ and HCS scores were 43 ± 44 and 35 ± 42 METs/minutes/week. Greater greenspace at 500 m positively associated with GLTEQ and HCS (rs = 0.33, p = 0.012; rs = 0.30, p = 0.020). Number of Intersections at 1000 m negatively correlated with GLTEQ and HCS (rs = –0.39, p = 0.002; rs = –0.35, p = 0.006). Walk and Transit Score were not significantly associated with PA (p > 0.05).
Conclusion:
We found associations between PA levels and greenspace and intersection density. Reasons for this require further investigation.
Keywords
Introduction
Individuals with pediatric-onset multiple sclerosis (POMS) experience high levels of disease activity, depression, and fatigue.1 –3 Importantly, higher levels of vigorous physical activity (PA) associate with lower magnetic resonance imaging (MRI) brain activity and lower levels of fatigue and depression; thus, PA may confer benefits in POMS.1,4,5 However, youth with MS are physically inactive, engaging in less than 10% of recommended levels of PA. 4 Therefore, identifying facilitators and barriers to PA participation in this population is paramount to improving outcomes.
The social ecological model is a framework that can help understand relationships between PA and built-environment features. Following this model, the physical built environment (e.g. access to facilities, equipment, proximity to parks), together with the macro-environment (e.g. community and urban planning policies), is noted to shape human behavior, including PA behavior.6,7 In support of this theory, studies of healthy youth have identified positive associations between safety of neighborhoods, access to facilities, and PA levels.8 –10 Additional research has identified positive associations of PA levels in healthy youth with walkability metrics, residential density, proximity to recreation facilities, and negative associations with traffic density. 11
Understanding features of the built environment may be of specific importance in POMS, given their baseline low levels of PA and relapses, which may affect gait, vision, and cognition. 4 We previously found that greater distance to recreation facilities was associated with lower moderate PA (r = –0.40, p = 0.01) in youth with MS. 12 Moreover, youth with MS have also identified proximity to gyms, schools, backyards, and malls as important for supporting participation in PA. 13 Finally, in adults with MS, the presence of shops, transit stops and low-cost recreation facilities within walking distance associate with daily step counts and PA levels.14 –16
However, known associations between PA and built environment among healthy youth may not directly translate to POMS. In addition to the aforementioned depression, fatigue and high levels of disease activity, individuals with POMS may experience residual motor or sensory deficits, are embarking on a lifetime of intervention, and face the specter of possible irreversible disability. 17 Furthermore, youth with POMS are in a critical development period. Their interactions with the environment may shape their PA behaviors differently from adults, highlighting the need to understand these associations specifically in POMS.18,19 With this in mind, we evaluated associations of PA with built-environment features such as green space, number of intersections, walkability, and transit access in youth with POMS, hypothesizing that higher levels of these features would associate with higher levels of PA.
Methods
This observational study recruited youth attending a specialized Neuroinflammatory Disorders Clinic at a quaternary pediatric hospital, The Hospital for Sick Children, Toronto, Canada (2015–2023). Inclusion criteria included: (1) individuals ⩽ 18 years old; (2) confirmed diagnosis of MS as per the 2017 McDonald diagnostic criteria; and (3) a valid residential postal code. 20
The study protocol was approved by the SickKids Research Ethics Board (REB#1000042743). Informed consent was collected from the participants or their legal parents/ guardians at the end of their clinic visits. See study flowsheet for participant recruitment details (Figure 1). Demographic data (sex, race, age, postal code), medical history, and clinical data (date of diagnosis, relapses, disease duration) were collected using standardized case report forms.
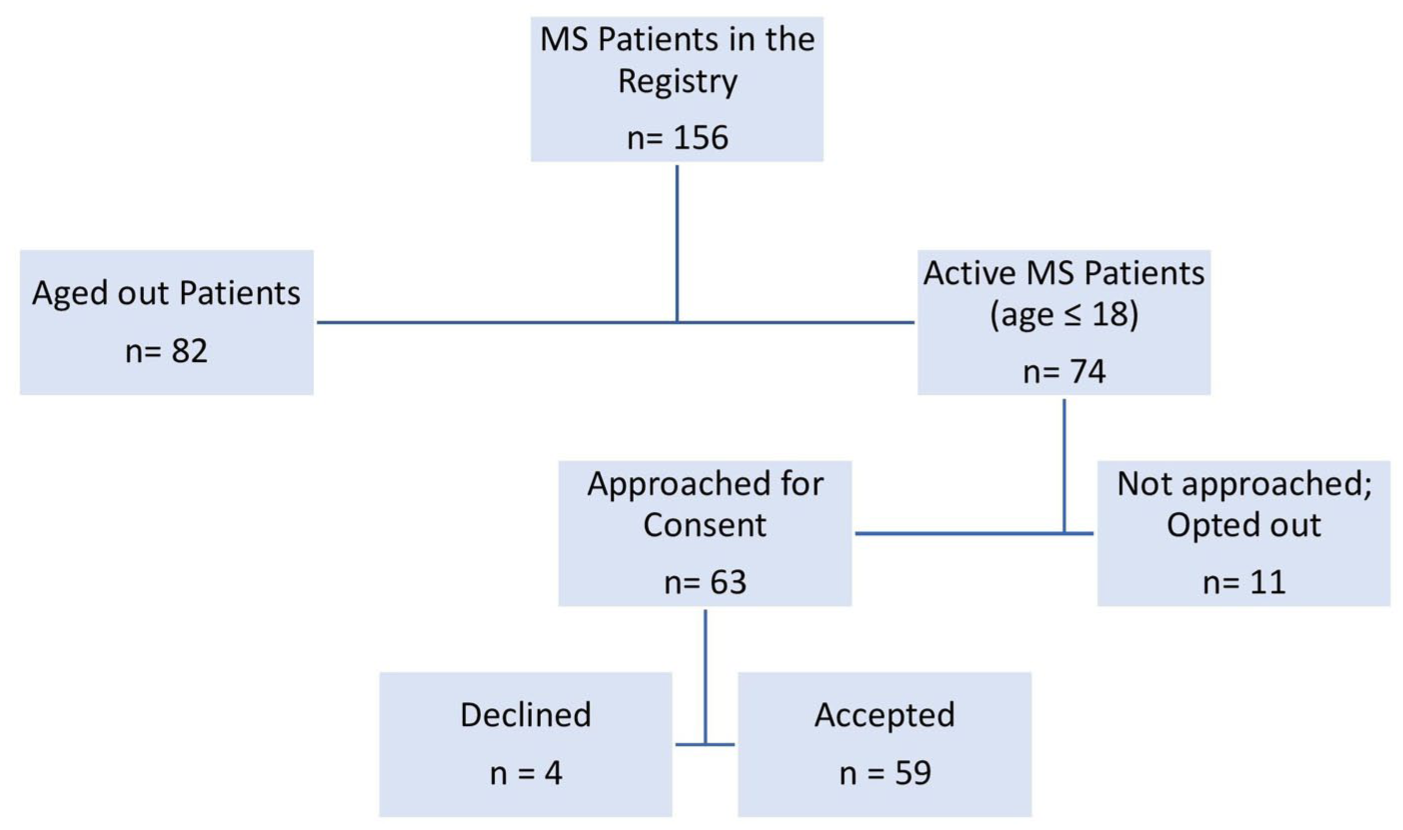
Study flowsheet (The neuroinflammatory registry consisted of 156 people with MS, of whom 82 were over the age of 18. Eleven patients were not approached due to prior opt-out in the registry. All active participants were approached for consent; four declined due to lack of time/interest. The final sample comprised 59 patients).
Disability scores (Expanded Disability Status Scale (EDSS); range 0 = normal neurological functioning to 10 = death) were collected from a single visit via chart review. 21 All assessments were conducted by neurologists certified in the administration of the EDSS. PA data was collected using REDCap electronic data capture tools hosted at SickKids, and the built-environment data was imported through an open database, The Canadian Urban Environmental Health Research Consortium (CANUE).22,23
Outcome variable: PA
The Godin Leisure-Time Exercise Questionnaire
The Godin Leisure-Time Exercise Questionnaire (GLTEQ) is a self-reported PA questionnaire designed to estimate frequency and intensity of PA levels. 24 Participants report the number of times they engaged in 15 minute bouts of strenuous, moderate, and light PA in the last seven days (range 1–7/week). The total score represents an estimate of metabolic equivalents of tasks (METs) (range 0 -119) 24 (1 MET = appx. 3.5 ml O2/kg/min (1.2 kcal/min for a 70 kg person)). 25 The health contribution score (HCS) (range 0–98) classification is: insufficiently active (score < 14 units), moderately active (14–23 units), and active (score ⩾ 24). 24 HCS correlates with accelerometer-measured MVPA in POMS and adults with MS.26,27
Independent variables: built-environment variables
The built-environment data were extracted from the publicly available database, CANUE, and linked to individual variables using postal code. 22 This large repository contains standardized measures of environmental factors. A summary of all environmental variables used in this study is presented in Table 3 below. The built-environment variables included:
Growing season max
Normalized difference vegetation index (NDVI) data was used to estimate green space and is a validated measure of residential greenspace. NDVI has been previously used for evaluating associations between greenspace and post-menopausal breast cancer and pediatric inflammatory bowel disease.28,29 This continuous measure (range -1 to 1) uses satellite imaging. Positive values represent a greater presence of healthy green vegetation in the area. 30 The variable growing season max value at 1000 m and 500 m represent the max NDVI within 1000 m and 500 m of postal code, respectively. 30 We selected 500 m and 1000 m buffers, approximating distances youth cover in 6–12 minutes of walking. 31
Number of intersections
The number of intersections in a buffer area of 1000 m around a postal code represents the area’s street connectivity. Only street intersections with more than one street segment joining were counted — no dead ends were included. A higher value indicates more intersections and a greater degree of connectivity enabling more direct travel between two points using existing streets. 32
Walk Score®
Walk Score® (range 0–100) estimates the pedestrian friendliness around a postal code based on population density and road metrics. 33 Scores reflect walking routes to nearby amenities, with maximum points for those within a 5 minute walk (.25 miles) . 33 Walk Scores of 0–49 are considered “car-dependent,” 50–69 “somewhat walkable,” 70–89 “very walkable,” and 90–100 “walker’s paradise” (no car needed for daily errands).
Transit Score®
Transit Score® (range 0–100) estimates ease of access to transit around a postal code. 34 It is based on the frequency, type of route (train, subway, bus, ferry, and other transport modes), and distance from postal code to the nearest stop. The “usefulness” of the nearby routes is summed and normalized into a score. 34 Classification includes: 0–24, “minimal transit,” 25–49 “some transit,” 50–69 “good transit,” 70–89 “excellent transit,” and 90–100 “Rider’s paradise” with world-class public transportation.
Statistical analyses
All statistical analyses were performed using Jeffrey’s Amazing Statistics Program (JASP) version 0.17.3. Statistical significance was defined, at p < 0.05. 35 The Shapiro-Wilk test was used to assess the normality of all variables. Given the small sample size and skewness of the dependent variable (GLTEQ score), non-parametric tests were used to provide valid inferences. Spearman’s Rho was used to measure the correlation between PA and built-environment variables. The correlations were interpreted using the following magnitude thresholds: 0.10–0.39 as small, 0.40–0.69 as moderate, and ⩾ 0.70 as strong. 36
Results
Baseline demographics and clinical characteristics
Fifty-nine youth with MS (36F) were included (median age of disease onset in our sample was 14 (interquartile range (IQR) 12.0–15.0), annual relapse rate was 2 (IQR 1.0–2.25), median EDSS score was 1.5 (IQR 1.0–2.0), 21 and median disease duration was 2 years (IQR 1.0–3.0). See Table 1 for demographic and clinical characteristics.
Baseline demographic and clinical characteristics of recruited participants with MS.
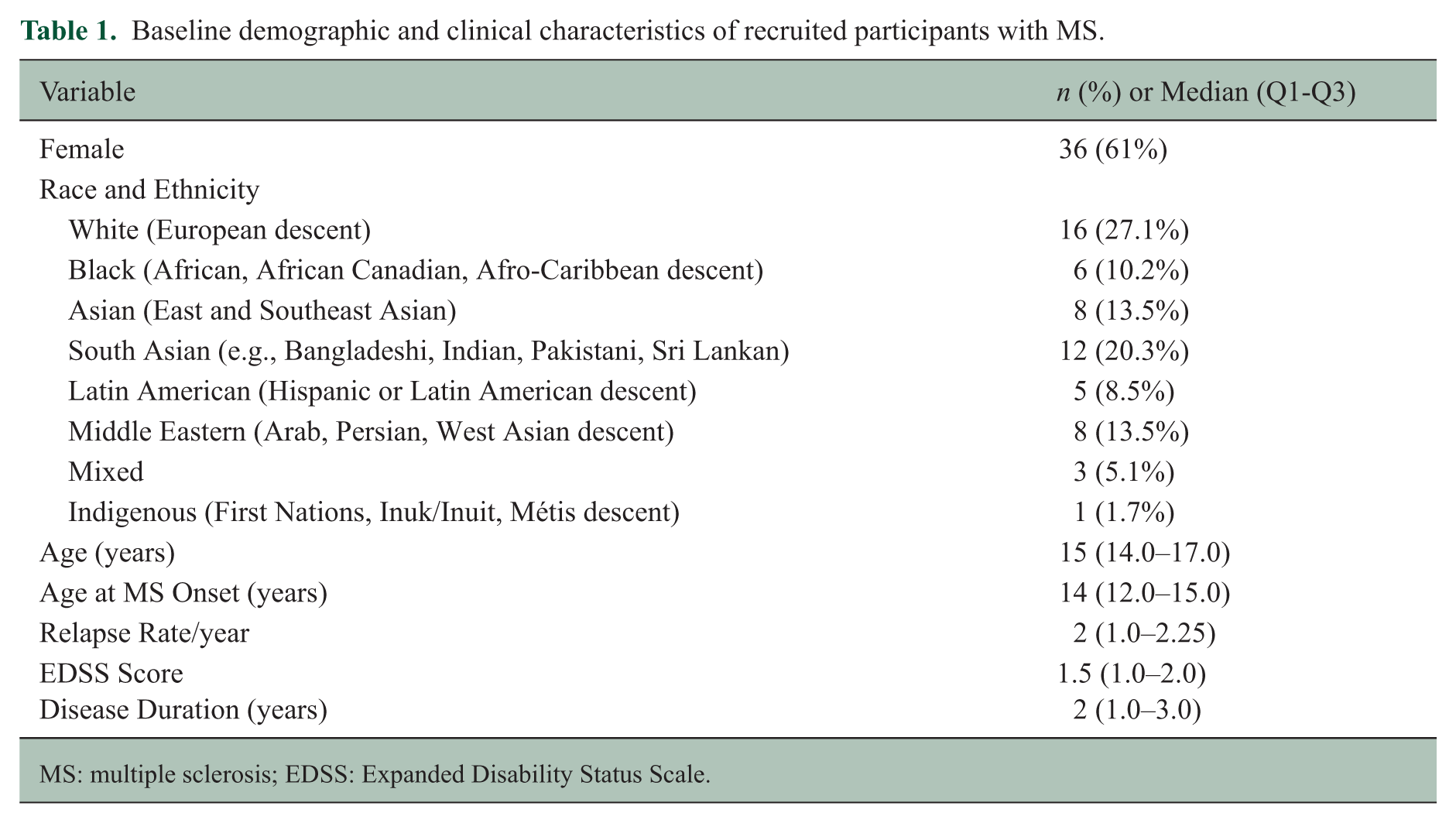

MS: multiple sclerosis; EDSS: Expanded Disability Status Scale.
GLTEQ characteristics
A summary of GLTEQ characteristics is presented in Table 2. The median total GLTEQ was 43 (range 0–119, IQR 23.5–67.5) and median HCS 35 (range 0–98, IQR 14.5–56.5). 61% (n = 36) of our sample was physically active and 39% (n = 23) was insufficiently active (HCS cut-offs (score < 24 = inactive)).
Physical activity (PA) levels of the recruited participants.
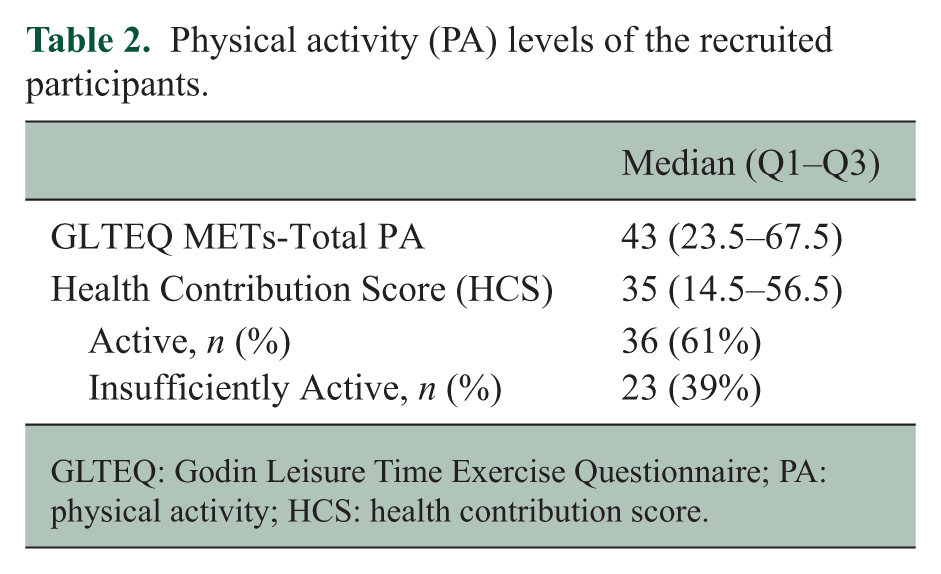
GLTEQ: Godin Leisure Time Exercise Questionnaire; PA: physical activity; HCS: health contribution score.
As per Mann–Whitney U test, there were no significant differences in GLTEQ and HCS between males and females (Supplementary Table 2).
Characteristics of built-environment variables
The median (IQR), minimum and maximum values of all built-environment variables are summarized in Table 3.
Characteristics of built-environment features.
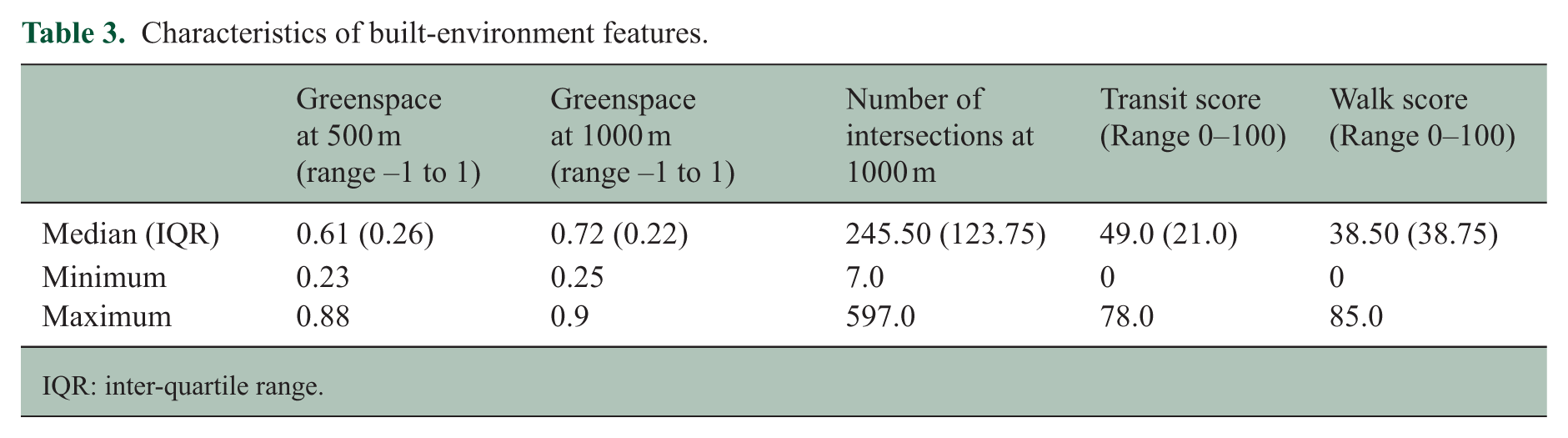
IQR: inter-quartile range.
Associations of built-environment variables with GLTEQ and MVPA
Table 4 shows associations between built-environment variables and GLTEQ score (METs). Increased greenspace at 500 m correlated with increased GLTEQ (METs) in the positive direction (rs = 0.33, confidence interval (CI) (0.075, 0.537), p = 0.012). We did not observe a statistically significant correlation between greenspace at 1000 m and GLTEQ score (METs) (rs = 0.25, CI (–0.09, 0.474), p = 0.058). Similarly, greenspace at 500 m was positively correlated with MVPA (HCS score) with a small effect size (rs = 0.301, CI (0.049, 0.518), p = 0.020); higher level of greenspace at 500 m was associated with higher (HCS) MVPA METs. However, greenspace at 1000 m was not significantly associated with MVPA (rs = 0.204, CI (–0.055, 0.437), p = 0.121). Intersections at 1000 m were negatively associated with GLTEQ score (METs) (rs = –0.39, CI (–0.590, –0.152), p = 0.002); more intersections at 1000 m radius were associated with lower GLTEQ score. Similarly, a negative association with a small effect size was observed between MVPA and intersections at 1000 m (rs = –0.351, CI (–0.557, –0.104), p = 0.006). Transit Score and Walk Score were not associated with GLTEQ score and MVPA (HCS).
Spearman’s Rho correlation matrix of all built-environmental variables and PA.
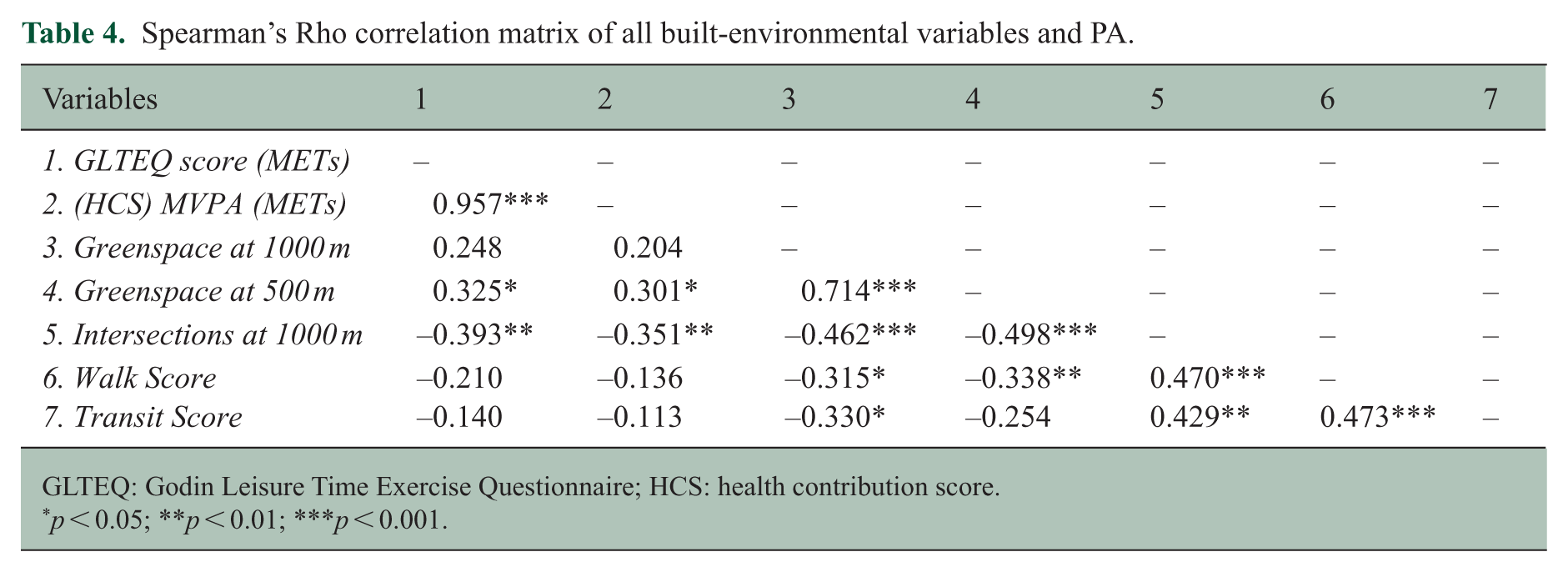
GLTEQ: Godin Leisure Time Exercise Questionnaire; HCS: health contribution score.
p < 0.05; **p < 0.01; ***p < 0.001.
Discussion
We evaluated associations between PA and built-environment features, including greenspace, number of intersections, Walk Score, and Transit Score, in individuals with POMS. Consistent with our hypothesis, we found an association between higher levels of greenspace at 500 m and higher PA levels, and no association at greater distances. In contrast to expectations, higher urban density was associated with lower PA levels. We found no associations between PA and Walk Score or Transit Score.
The significant associations of total PA and MVPA levels with greenspace at 500 m but not 1000 m highlight the importance of the presence of greenspace in close proximity to one’s home. These findings are consistent with previous research conducted among non-MS youth. For example, a cross-sectional Turkish study surveyed 384 youth aged 13 to 19 and found that an increase in distance from greenspaces was associated with a decrease in frequency of outdoor PA (β = –0.117, p ⩽ 0.01). 37 Similarly, an accelerometry-based study conducted with 902 children observed that time spent in greenspaces accounted for 33.6% of children’s outdoor MVPA on weekdays, increasing up to 60% on weekends. 38 Results from a Canadian study with youth suggest that with every 5% increase in treed area, there was a 5% increase in the odds of engaging in PA. 39 Finally, features of the greenspaces, such as increased trees, play equipment, and sports facilities/courts, have been associated with higher duration and frequency of PA among youth. 37
The presence of infrastructure for play and sport alone may not explain the relationship we found. It is possible that spaces that promote congregation and active play can increase social ties — crucial to supporting PA behavior in children.40–45 Socialization with peers, such as “hanging out” in public greenspaces contributes to shaping social identity, which can influence engagement in health-promoting activities. In a mixed-methods Dutch study (n = 618), participants described social interactions in urban green spaces as fostering the development of social networks, particularly among immigrant groups. 46 Another study of impoverished older adults in urban settings found associations between higher levels of social integration and sense of local community and the presence of green spaces. Among pediatric populations, an Iranian cross-sectional study of 11,000 youth found longer time in greenspaces associated with higher levels of self-satisfaction and social contacts. 47 Finally, a study of urban youth in the Netherlands identified that greater proportions of greenspace within 1 to 3 km of one’s home were associated with lower feelings of loneliness and greater greenspace within 1 km was strongly associated with higher perceived social support. 48 This may be of specific relevance to youth with MS, as recent studies have identified the importance of social connectedness for promoting PA behaviors.13,49 Further work including granular assessments of possible contributing factors is needed to understand the reasons for the associations we found. Although the associations were statistically significant, the small correlation coefficients suggest cautious interpretation. P-values were not adjusted for multiple comparisons, as this exploratory study aimed to identify environmental trends to guide future research.
Contrary to our hypothesis, higher street connectivity—number of intersections at 1000 m—is associated with lower PA and MVPA. On the surface, our finding appears to diverge from the results of a previous study, which identified that greater intersection density at 1 km was associated with higher MVPA in healthy children. 50 However, differences between urban and non-urban settings distinguished this relationship. A higher link: node ratio (more street segments vs intersections, including dead ends) was associated with lower MVPA among females in urban areas, but with higher MVPA among females in non-urban areas. 50 Our sample, of 61% female and urban residents, aligns with Boone-Heinonen’s study subgroup that demonstrated lower MVPA in highly connected urban settings. These results emphasize the need to account for the interplay between the social normative constructs (i.e. gendered perceptions of safety and mobility) and urbanicity when examining built-environment influences on youth PA with MS.
An alternative explanation may be parental safety concerns, as parental perceptions of barriers may have a greater influence on children’s PA than the children’s perceptions. 51 Parents of children living in areas of higher street connectivity may perceive these areas to have safety issues such as having higher rates of crime and dense automobile traffic, both potential barriers to PA. For example, higher violent crime within a half mile of one’s home is associated with decreased outdoor PA among Mexican American girls, whereas perceived neighborhood safety is associated with higher outdoor PA among girls but not boys. 52 Specifically, younger females report more fear of crime compared to males, which is relevant as our study’s sample was majority female youth. 53
Differing from our hypothesis, PA levels did not associate with either Transit or Walk Scores. These scores represent the ability to use public transit or walk to complete everyday tasks. Other studies have shown associations of higher PA with access to transit in non-MS youth. For example, a cross-sectional study conducted with healthy children reported that those who utilized public transit achieved one-third of the daily recommended PA from transit use alone. 54 In addition, an Australian study of healthy youth demonstrated that accessibility to public transport near schools was associated with over 20 minutes of active travel. 55 The lack of association may stem from overall poor access to transit and amenities among our participants, who had a median Transit Score of 49, with 65% scoring below 60. 34 Similarly, the average Walk Score was 35.64, and 63% had a Walk Score below 50. These low scores suggest that most participants lived in car-dependent areas with lack of amenities within walking distance. 33 The lack of expected associations may stem from limited variability in scores or the fact that the scores were so low that there were minimal practical differences, even if the scores differed.
Finally, we emphasize that using walkability scores are only meaningful for understanding PA–built environment associations when there is adequate variability in the range of scores in co-occurring features—proximity to recreational facilities—that can improve PA. 56 As noted above, walkability and transit scores likely serve as surrogate measures of amenity access, which may be shaped by the relative neighborhood socio-economic status (SES). For example, children from high SES neighborhoods with more facilities had increased odds of achieving ⩾ 5 bouts of MVPA/week compared to children from low-income neighborhoods. 57 Youth residing in low-income and marginalized Ontario neighborhoods may lack options for PA, especially in colder seasons when parks are inaccessible. Future work including a detailed evaluation of low-cost recreational facilities, proximity to parking, and accessible transit stops could provide more clarity regarding these associations.
Limitations of our study include the cross-sectional methodology which limits causal inference. Sampling bias may also exist, as 61% of our sample was physically active, a departure from previous reports which found most children with MS to be inactive. Moreover, a limited number of participants were from rural areas, as our study only collected data at one center. However, given ongoing urbanization—with 90% of Ontario’s population and 83% of Canada’s population living in urban settings — these findings are relevant to most North American settings. In addition, the lack of device-based measures of PA (e.g. accelerometry) and a control group may limit generalizability of results. Future work using device-based PA measures may provide insights into how subcategories of GLTEQ associate with these factors. Finally, due to limited data and exploratory nature of our study only preliminary analyses were included without controlling for confounders or adjusting for multiple comparisons.
Our study provides a strong framework for understanding the associations of greenspace, intersections, transit and walk score with PA among youth with MS. Clinicians and families can encourage youth to identify greenspaces in local proximity for engaging in PA. On a broader level, our findings have the potential to serve as the basis for changes in practice and policy through greater use of greenspaces in urban design, schools, clinics, and community settings. Larger multi-site studies are needed to confirm our findings. Safety is an important built-environment feature to consider for future studies, especially for children and youth with MS. In addition, perceived built-environment in combination with objective measures of built-environment may be useful in understanding usage of facilities and transit. Finally, objective PA measures such as GPS mapping could provide precise insights regarding location, intensity, and timing of PA.
Conclusion
Youth with MS participating in this study had poor access to facilities and transit. Greater greenspace within 500 m was associated with higher levels of PA and MVPA, while more densely populated areas associated with lower PA. Although these findings are specific to our sample, they suggest that features of the built-environment may improve PA levels among youth with MS. Our findings highlight the importance of urban planning to improve accessibility for managing MS through modifications of the local environments. Future studies with larger and diverse samples are needed to confirm our findings. The interactions between built-environment and individual-level factors need to be evaluated to better understand their collective influence on PA and inform targeted interventions for youth with MS.
Supplemental Material
sj-docx-1-msj-10.1177_13524585251407505 – Supplemental material for Built-environment correlates of physical activity in youth with multiple sclerosis
Supplemental material, sj-docx-1-msj-10.1177_13524585251407505 for Built-environment correlates of physical activity in youth with multiple sclerosis by Sonika Kumari, Samantha Stephens, Paul Yejong Yoo, Kelly P Arbour-Nicitopoulos, Brian M Feldman, Marcia L Finlayson, Ruth Ann Marrie, Robert Motl, Teresa To and E Ann Yeh in Multiple Sclerosis Journal
Footnotes
Acknowledgements
Author Contributions
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: E.A. Yeh has received research funding from NMSS, CMSC, CIHR, NIH, OIRM, SCN, CBMH Chase an Idea, SickKids Foundation, Rare Diseases Foundation, MS Scientific Foundation, McLaughlin Centre, Leong Center, Peterson Foundation, Gary Hurvitz Centre for Brain and Mental Health. She holds the Garry Hurvitz Chair in Neurology (The Hospital for Sick Children). Investigator initiated research funding from Biogen. Scientific advisory: Hoffman-LaRoche, Alexion. DSMB: Pipeline Therapeutics. Speaker honoraria: Biogen, JHU, Saudi Epilepsy Society, NYU, MS-ATL; ACRS, PRIME, CNPS. Co-Editor in Chief, MSARD. Governing Council: CANTRAIN. Steering Committee: Rare-Kids CAN. R.A. Marrie receives research funding from: CIHR, MS Canada, Crohn’s and Colitis Canada, National Multiple Sclerosis Society, CMSC, the Arthritis Society, Public Health Agency of Canada, Brain Canada, Children’s Hospital Research Institute of Manitoba, Pfizer Foundation and the US Department of Defense, is a co-investigator on studies receiving funding from Biogen Idec and Roche Canada and holds the Multiple Sclerosis Clinical Research Chair (Dalhousie University). All other authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Canadian Institutes of Health Research, Edwin S.H. Leong Center for Healthy Children, and Gary Hurvitz Centre for Brain and Mental Health.
Ethical Considerations
The study protocol was approved by the SickKids Research Ethics Board (REB#1000042743) on October 8, 2013. Informed consent was collected from the participants or their legal parents or guardians at the end of their clinic visits. Clinical and demographic data were collected from the program’s registry, a prospectively collected registry containing clinical and demographic information on consecutive children with neuroinflammatory disorders (Hospital for Sick Children REB#1000005356).
Consent to Participate
The study was approved by the SickKids Research Ethics Board (REB#1000042743) on October 08, 2013. All participants or their legal parents or guardians provided written informed consent prior to participating.
Consent for Publication
Written informed consent was obtained from a legally authorized representative for anonymized patient information to be published in this article.
ORCID iDs
Data Availability
The participants of this study did not give written consent for their data to be shared publicly, so due to the sensitive nature of the research, supporting data is not available.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
