Abstract
Topical photodynamic therapy is a widely approved therapy for actinic keratoses and low-risk nonmelanoma skin cancers with a rapidly growing range of emerging indications for other cutaneous diseases. This review summarizes the best-available evidence to provide a clinical update for dermatologists on the approved and emerging indications of photodynamic therapy. The body of evidence suggests that photodynamic therapy is superior or noninferior to other available treatment modalities for actinic keratoses, low-risk basal cell carcinomas, Bowen’s disease, skin field cancerization, chemoprevention of keratinocyte carcinomas in organ transplant recipients, photoaging, acne vulgaris, and cutaneous infections including verrucae, onychomycosis, and cutaneous leishmaniasis. There is emerging evidence that photodynamic therapy plays a role in the management of actinic cheilitis, early-stage mycosis fungoides, extramammary Paget disease, lichen sclerosis, and folliculitis decalvans but there are no comparative studies with other active treatment modalities. Common barriers to topical photodynamic therapy include procedural pain, costs, and the time required for treatment delivery. There is significant heterogeneity in the photodynamic therapy protocols reported in the literature, including different photosensitizers, light sources, number of treatments, time between treatments, and use of procedural analgesia. Topical photodynamic therapy should be considered in the management of a spectrum of inflammatory, neoplastic, and infectious dermatoses. However, more comparative research is required to determine its role in the treatment algorithm for these dermatologic conditions and more methodological research is required to optimize photodynamic therapy protocols to improve the tolerability of the procedure for patients.
Introduction
Topical photodynamic therapy (PDT) is centred on the interaction between a photosensitizer, the appropriate activating wavelength of light, and oxygen. The resulting photochemical reaction generates singlet oxygen, a highly-reactive chemical species that initiates a series of cellular reactions that culminate in necrosis, apoptosis, and a host immunologic response. 1 The main topical photosensitizers used for PDT are 5-aminolevulinic acid or its ester, methyl aminolevulinate (MAL). These photosensitizers preferentially bind with low density lipoproteins (LDLs), and the resulting complexes are subsequently internalized by LDL receptor-mediated endocytosis and are metabolized into the photoactive protoporphyrin IX (PpIX) within the mitochondria. 2 Premalignant and malignant cells accumulate PpIX due to higher rates of LDL uptake from increased LDL receptor expression to supply these rapidly dividing cells with cholesterol to create membranes for cell division, and increased mitochondrial PpIX synthesis.3,4 Numerous clinical guidelines have approved topical PDT for the treatment of actinic keratoses (AKs) and low-risk nonmelanoma skin cancers (NMSCs).5,6 There is a rapidly expanding number of studies exploring the utility of topical PDT for a spectrum of dermatological conditions. However, topical PDT continues to be underutilized in Canada. Therefore, a review is necessary to update dermatologists on the latest evidence about the clinical applications of topical PDT, with a focus on high-quality comparative studies with other first-line treatment modalities.
This review explores the approved and emerging clinical applications of topical PDT in dermatology to evaluate its role in the treatment algorithm of cutaneous diseases and the barriers to its use. The literature comparing topical PDT and other accepted treatment modalities for the established and emerging dermatological clinical indications for topical PDT are summarized in Table 1. This review preferentially included randomized-controlled trials (RCTs) and meta-analyses of RCTs with quantitative primary outcomes. In the absence of published RCTs and meta-analyses in the context of emerging clinical applications of topical PDT, prospective and retrospective cohort studies as well as case studies and series with quantitative primary outcomes were included. All descriptive studies were excluded.
Efficacy Comparisons Between PDT and Other Accepted Treatment Modalities for the Established and Emerging Clinical Indications for Topical PDT.
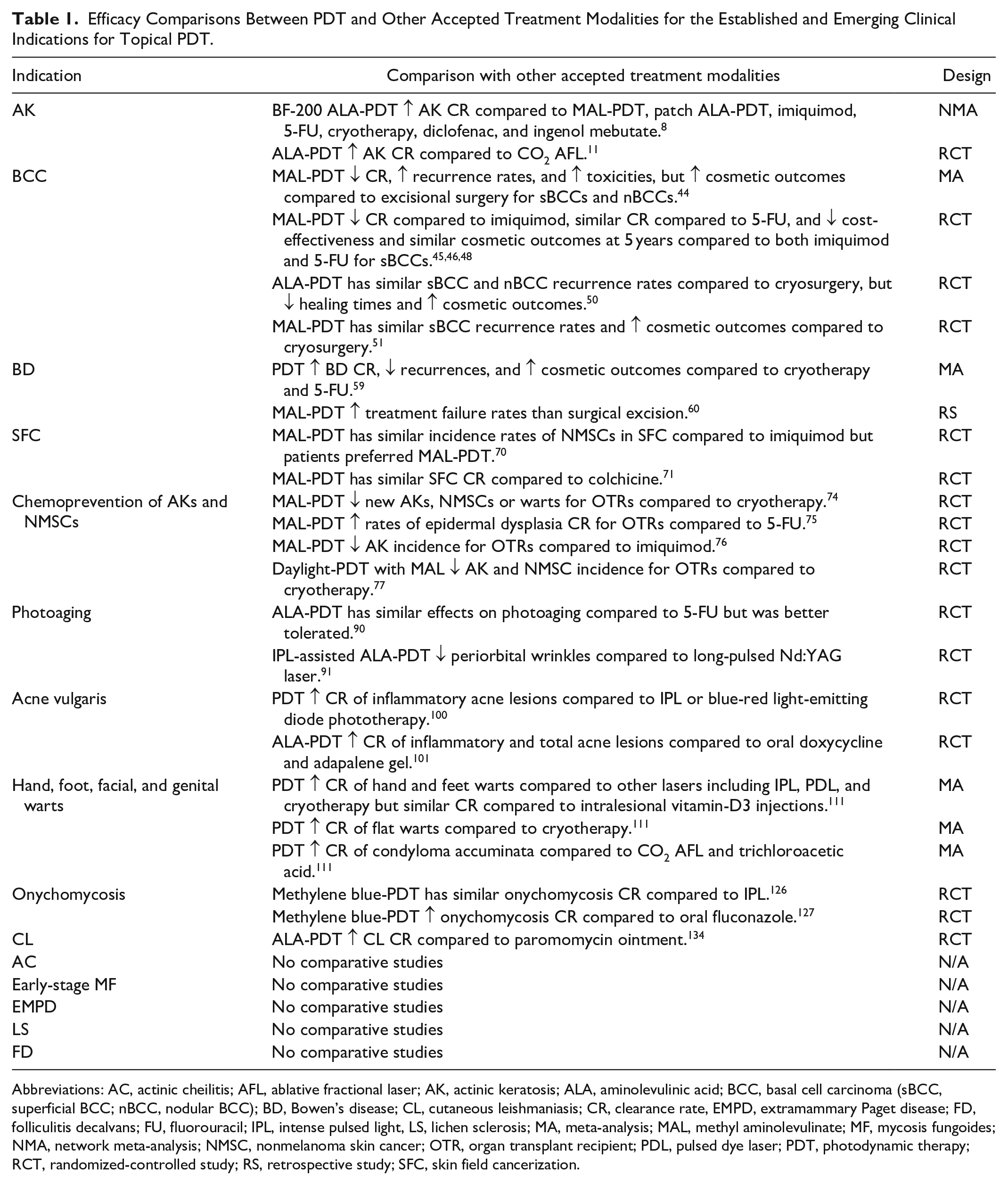

Abbreviations: AC, actinic cheilitis; AFL, ablative fractional laser; AK, actinic keratosis; ALA, aminolevulinic acid; BCC, basal cell carcinoma (sBCC, superficial BCC; nBCC, nodular BCC); BD, Bowen’s disease; CL, cutaneous leishmaniasis; CR, clearance rate, EMPD, extramammary Paget disease; FD, folliculitis decalvans; FU, fluorouracil; IPL, intense pulsed light, LS, lichen sclerosis; MA, meta-analysis; MAL, methyl aminolevulinate; MF, mycosis fungoides; NMA, network meta-analysis; NMSC, nonmelanoma skin cancer; OTR, organ transplant recipient; PDL, pulsed dye laser; PDT, photodynamic therapy; RCT, randomized-controlled study; RS, retrospective study; SFC, skin field cancerization.
Currently Approved Indications
Actinic Keratoses
Topical PDT has been established as an effective approach to treat AKs, common precancerous skin lesions that develop from cumulative sun exposure and may progress to squamous cell carcinomas (SCCs). There are numerous treatment modalities for AKs. Lesion-directed therapies include cryotherapy, lasers, and curettage. Field-directed therapies include topical 5-fluorouracil (FU), imiquimod, and diclofenac.
7
In a network meta-analysis of 25 RCTs of 5562 participants, topical PDT with a nanoscale-lipid vesicle formulation of aminolevulinic acid (ALA; BF-200 ALA-PDT), showed the highest AK clearance rates (75.8%) compared to topical PDT with MAL (MAL-PDT), patch ALA-PDT, cryotherapy, diclofenac, 5-FU, ingenol mebutate, and various imiquimod treatment protocols.
8
Another network meta-analysis of 15 RCTs of 4252 patients with at least 12 months of follow-up found that ALA-PDT had the highest AK clearance rates compared to placebo (Risk Ratio (RR): 8.05; 95% CI: 2.07-31.37), followed by imiquimod 5%, MAL-PDT, and cryotherapy.
9
In a meta-analysis of 4 RCTs with a total of 641 participants, PDT with either ALA or MAL increased AK clearance rates at 3 months compared to cryotherapy (RR: 1.14; 95% CI: 1.11-1.18).
10
ALA-PDT reduced AK quantity at 3 months compared to CO2 ablative fractional laser (AFL) (80% vs 66.7%;
Daylight-PDT, where natural daylight exposure is used instead of an artificial light source, addresses many of the limitations of conventional PDT by reducing clinic visit times associated with the illumination procedure and minimizing procedural pain. Of course, the effectiveness of daylight-PDT is dependent on weather conditions, as limited sunlight could be insufficient to activate the photosensitizer, and cold ambient temperatures may preclude patients from tolerating the necessary time outdoors to receive the optimal dose of daylight exposure. It was found that there was generally sufficient natural sunlight (>8 J/cm2 for at least 2 hours) and a comfortable temperature (minimum temperature of at least 10°C) for outdoor sunlight exposure to treat patients with AKs effectively with daylight-PDT until the middle of September, even in countries in Northern latitudes.
27
This threshold of 8 J/cm2 for at least 2 hours was based on a study that found similar AK clearance rates after daylight-PDT with MAL at light doses of 8 to 70 J/cm2 and that 1.5 and 2.5 hours of daylight exposure resulted in similar AK clearance rates.28,29 From our experience in an Eastern Canadian climate, daylight-PDT remained effective well into the month of October with temperatures remaining above 10°C. Daylight-PDT was noninferior to conventional PDT for grade I to II AKs (RR: 0.97; 95% CI: 0.91-1.04) but was less effective for thick and hyperkeratotic grade III AK lesions (RR: 0.87; 95% CI: 0.81-0.94) in a meta-analysis of 6 RCTs with a total of 369 patients.
30
This meta-analysis also showed that daylight-PDT reduced maximal pain scores (mean difference: 4.51; 95% CI: 3.89-5.12) and lowered the risk of adverse events (RR: 0.7; 95% CI: 0.58-0.85) compared to conventional PDT. More patients were satisfied with daylight-PDT compared to conventional PDT (RR: 4.001; 95% CI: 2.017-7.938) in a meta-analysis of 5 RCTs with a total of 318 patients.
31
These findings align with our experience treating a 72-year-old male with chronic facial actinic damage and AKs with 4 repeated sessions of daylight-PDT with MAL (Figure 1). There have been some methodological studies to guide the selection of a daylight-PDT AK treatment protocol. Patients undergoing pre-treatment curettage, which is thought to enhance photosensitizer penetration, had similar AK clearance rates at 3 months compared to the non-curettage group.
32
Comparisons between the ALA and MAL photosensitizers found that daylight-PDT with BF-200 ALA improved AK clearance rates at 3 months and at 12 months.33-35 No difference in AK clearance rates were found in a study comparing a single treatment and 2 treatments of daylight-PDT with MAL; however, the second treatment increased pain (
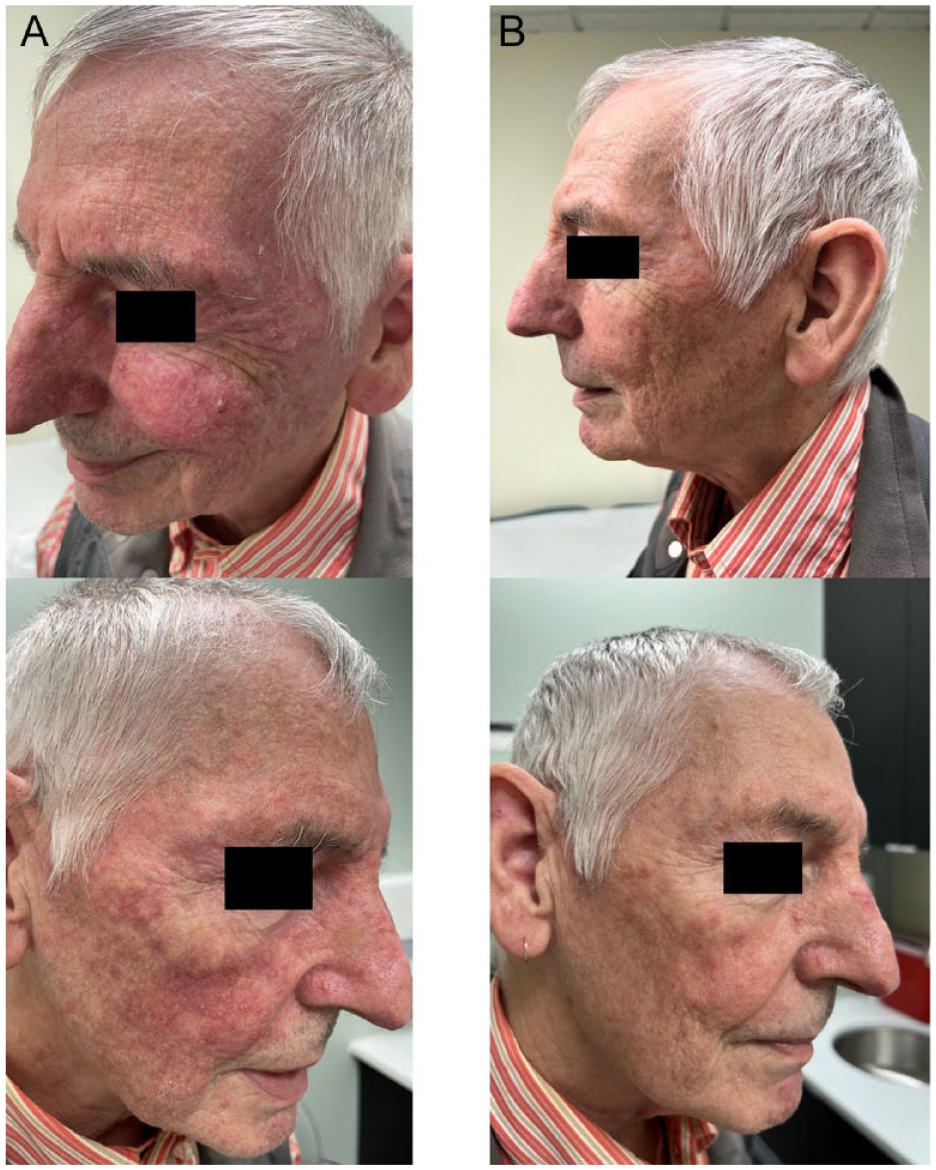
Facial photographs (A) pre- and (B) post-daylight MAL-PDT for a 72-year-old male with chronic actinic damage and numerous AKs on the bilateral cheeks, forehead, and nose. After 4 treatments with daylight MAL-PDT, marked improvement was noted with no significant procedural side effects. AKs, actinic keratoses; MAL-PDT, methyl aminolevulinate photodynamic therapy.
There is evidence that treatment modalities to improve photosensitizer penetration such as micro-needling and lasers enhances the efficiency of PDT. In a meta-analysis of 4 RCTs with a total of 240 participants, laser-assisted PDT with CO2 or Er:Yag AFL improved AK clearance rates compared to PDT monotherapy (RR: 1.33; 95% CI: 1.24-1.42) with no increased procedural pain. 38 In a meta-analysis of 5 RCTs with a total of 213 participants, the combination of micro-needling and ALA-PDT increased AK clearance rates compared to ALA-PDT monotherapy (mean difference: 6.01; 95% CI: 0.84-11.17), with no increased procedural pain. 39
Pre-treatment with topical treatments may improve photosensitizer accumulation and enhance PDT treatment outcomes. Similar AK clearance rates were reported for patients undergoing 1 session of MAL-PDT pretreated with 40% urea (60.8%), 10% salicylic acid (61.4%), or curettage (68.5%), but pre-treatment with urea and salicylic acid increased procedural pain in comparison to curettage (
Basal Cell Carcinomas
Basal cell carcinomas (BCCs) are keratinocytes malignancies and are the most common cancers worldwide.
43
Surgical excision definitively manages BCCs, but these procedures are time consuming, and may be associated with significant cosmetic and functional limitations. There are different subtypes of BCCs, including superficial, nodular, morpheaform, infundibulocystic, pigmented, and fibroepithelioma of Pinkus BCCs. PDT is approved for the treatment of low-risk, superficial BCCs (sBCCs). A meta-analysis of 7 RCTs involving 1339 patients and 1568 BCCs and 1 retrospective study involving 108 BCCs found that MAL-PDT has inferior 3-month (RR: 0.93; 95% CI: 0.89-0.97) and 12-month (RR: 0.90; 95% CI: 0.85-0.95) clearance rates compared to surgery, with an increased 12-month recurrence rate (RR: 10.43; 95% CI: 1.98-55.03) and more toxicities (RR: 2.12; 95% CI: 1.46-3.09).
44
However, MAL-PDT had superior cosmetic outcomes compared to excisional surgery (RR: 1.99; 95% CI: 1.5-2.63). It is important to note that excisional surgery is rarely employed in the clinical management of sBCCs. The more common treatment options for sBCCs include 5-FU, imiquimod, and cryosurgery. Imiquimod was superior to 2 sessions of MAL-PDT and 5-FU was noninferior to MAL-PDT in a RCT of 601 patients with sBCCs after 1 and 3 years.45,46 A follow-up cost-effectiveness analysis of this study cohort showed that imiquimod and 5-FU were more cost-effective than MAL-PDT for sBCC management.
47
A follow-up analysis of the cosmetic outcomes 5 years post-treatment showed modest improvements in the number of recurrence-free patients with good and excellent cosmetic outcomes after MAL-PDT when compared to imiquimod and 5-FU. However, due to the increased risk of sBCC recurrence in the MAL-PDT treatment group that may have required re-treatment with surgical excision, there were ultimately no statistically significant differences in cosmetic outcomes between the 3 treatment groups.
48
However, a subgroup analysis of this study cohort showed that MAL-PDT was superior to imiquimod in 1 subgroup of lower extremity sBCCs on patients > 60 years, which may be explained by functional barriers that elderly patients experience when applying topical medications on the lower extremities.
49
ALA-PDT had similar rates of histological recurrence of sBCCs at 12 months compared to cryosurgery (25% vs 15.4%;
Some studies have demonstrated value for PDT in the treatment of nodular BCCs (nBCCs).
52
Though MAL-PDT has inferior sustained nBCC complete response rates at 5 years compared to excisional surgery (76% vs 96%;
Bowen’s Disease
Cutaneous SCC is the second-most common form of skin cancer, with an increasing worldwide incidence.
58
PDT -in some instances- can be used for the treatment of SCC in situ, otherwise known as Bowen’s disease (BD). Other treatment options for BD include surgical excision, 5-FU, imiquimod, and cryotherapy. In a meta-analysis of 4 RCTs with 292 patients, PDT had higher complete response rates (RR: 1.36; 95% CI: 1.01-1.84), reduced recurrence (RR 0.53; 95% CI 0.3-0.95), and improved cosmetic outcomes (RR 1.34; 95% CI: 1.15-1.56) compared to cryotherapy and 5-FU.
59
However, in comparison with surgical excision with a 5 mm safety margin, PDT has higher rates of treatment failure in a retrospective study of 608 patients with a median follow-up of 18 months (Hazard Ratio (HR): 2.71; 95% CI: 1.52-4.83).
60
It should also be noted that in a long-term follow-up study of MAL-PDT outcomes for BD, a sizeable recurrence rate of 71% at 5 years was noted and risk factors for recurrence included tumour size >300 mm2, upper extremity location, and age <70 years old.
61
There is some evidence that laser-assisted PDT enhances PDT therapeutic efficacy for BD. Pre-treatment with CO2 or Er:YAG AFLs improved BD clearance rates and reduced recurrence rates at 1 year (6.7% vs 31.6%;
Emerging Indications
Skin Field Cancerization
Skin field cancerization (SFC) is a process that occurs in areas of the skin that have undergone genomic alterations induced by ultraviolet radiation, with AKs being the product of this environment. PDT has shown promise in treating SFC. In a placebo-controlled RCT of patients with AKs and a history of NMSC, ALA-PDT delayed the mean time of appearance (9.86 months vs 7.14 months) and reduced the total number of new AK lesions at 12 months (14 vs 30;
Chemoprevention of AKs and NMSCs
There is growing interest in PDT to prevent AKs and NMSCs in high-risk immunosuppressed organ transplant recipients (OTRs). OTRs have a 65 to 140 times greater risk of developing SCCs, which account for 5% of all-cause mortality in OTRs.
73
PDT showed promise for the primary prevention and treatment of SCCs in OTRs; a meta-analysis of 3 RCTs with a total of 148 solid OTRs found that PDT reduced the incidence of AKs/SCCs (risk difference: 0.14; 95% CI: 0.08-0.19) and a separate analysis of 4 RCTs with 78 solid OTRs showed that PDT increased AK/SCC complete response rates (risk difference: 0.5; 95% CI: 0.22-0.79).
74
Numerous RCTs have compared PDT to other lesion or field treatment options including cryotherapy, 5-FU, and imiquimod. A RCT of OTRs showed that 2 MAL-PDT treatments, 1 week apart, reduced the incidence of new AK, NMSC, or wart lesions (65 vs 103;
Photoaging
Chronic prolonged sun exposure induces photoaging, a process by which the skin undergoes changes that can manifest as rhytids, telangiectasias, increased skin laxity, hyperpigmentation, lentigines, ephelides, volume loss, poikiloderma, and cutaneous dysplasia. Prevention of photoaging is centred around sun protection, and treatment options for photoaging include topical retinoids, 5-FU cream, chemical peels, micro-needling, neuromodulators, and laser resurfacing procedures. PDT is an emerging treatment modality in photorejuvenation. A placebo-controlled RCT showed that 2 treatments of MAL-PDT, 2 to 3 weeks apart, improved fine lines, course lines, mottled pigmentation, tactile roughness, sallowness, erythema, and sebaceous hyperplasia at 1 month post-treatment (
Acne Vulgaris
Acne vulgaris is a common inflammatory disorder of the pilosebaceous unit. Early studies have demonstrated that photosensitizer preferentially accumulates in the pilosebaceous unit due to their lipidic cytoplasms and involvement in skin lipid and hormone control that facilitate uptake of the hydrophobic photosensitizer molecule, which facilitates the selective phototoxicity, anti-bacterial and anti-inflammatory effects of PDT at the culprit site of acne vulgaris.
92
In a meta-analysis of 13 RCTs involving a total of 701 subjects, PDT with ALA, MAL, and liposomal methylene blue significantly reduced inflammatory acne lesion counts (15.97%,
A comparative RCT found that ALA-PDT resulted in superior clearance rates of inflammatory acne lesions compared to IPL or blue-red LED light-based therapies (92% vs 58% or 44%;
Hand, Foot, Facial, and Genital Warts
Verrucae, or cutaneous warts, are a common skin condition caused by epidermal infection with human papilloma virus (HPV). Treatments for verrucae include topical keratolytics, cryotherapy, electrosurgery, laser therapy, cantharidin, imiquimod, sinecatechins, and intralesional treatments such as bleomycin and
Condyloma acuminata (CA) is a sexually transmitted cutaneous infection of the anogenital region caused by certain variants of HPV. A number of studies have demonstrated that PDT improves outcomes in CA treatment. Traditional treatment for CA include topical trichloroacetic acid, imiquimod, cryotherapy, CO2 AFL, and surgical excision, but cure rates are around 50% with high recurrence rates.
110
In a meta-analysis of 6 RCTs, PDT had similar CA clearance rates to CO2 AFL (RR: 0.98; 95% CI: 0.95-1.00) and trichloroacetic acid (RR: 1.04; 95% CI: 0.59-1.83).
105
Another meta-analysis of 20 RCTs found that ALA-PDT reduced the recurrence rate of CA at 2 weeks compared to CO2 AFL (RR: 0.26; 95% CI: 0.2-0.35) and cryotherapy (RR: 0.49; 95% CI: 0.28-0.87).
111
There is also evidence that the combination of PDT with locally destructive therapies such as cryotherapy or CO2 AFL enhances CA clearance rates. The utility of PDT as an adjunct to cryotherapy was demonstrated in a RCT that showed that ALA-PDT immediately after cryotherapy in 2 treatment sessions separated by 7 days increased CA clearance rates in the urethral meatus (100% vs 54.5%;
Onychomycosis
Onychomycosis is a fungal nail infection that can be difficult to treat and often requires the protracted administration of systemic antifungals which have important side effects such as hepatotoxicity.
117
In vitro studies have demonstrated that
Cutaneous Leishmaniasis
Old world cutaneous leishmaniasis (CL) results from cutaneous parasitic infection of dermal macrophages with
Actinic Cheilitis
Actinic cheilitis (AC) is a premalignant lesion of the lip that requires early treatment to terminate its progression into lip SCC. Traditional treatment strategies include cryotherapy, surgical or CO2 laser vermilionectomy, and topical treatments with 5-FU, imiquimod, or topical diclofenac in hyaluronic acid. To date, there are no comparative studies between PDT and other AC treatment strategies. However, in a systematic review of 49 studies, PDT had lower AC complete response rates (68.9%) in comparison with the 100%, 93.8%, and 75% overall complete response rates reported with surgical, laser, and topical 5-FU treatments, respectively.
137
There is evidence that daylight-PDT is as efficacious as conventional PDT for AC with a better adverse event profile. In a systematic review of 19 studies, daylight-PDT had comparable AC clinical response rates (76.7%) to conventional PDT (80%) and ALA patch-PDT (65.1%), but is better tolerated with more painless patients (daylight-PDT: 87.1%; conventional PDT: 31.25%) and reduced rates of moderate and severe local phototoxic reactions (daylight-PDT: 0%; conventional PDT: 47.78%; ALA patch-PDT: 21%).
138
There has also been some emerging research on combination PDT treatment options for AC. The combination of MAL-PDT followed by a 4-week course of 5% imiquimod cream 3 days per week showed an AC complete response rate of 80%, with only 2 recurrences in a single-armed study of 34 patients.
139
One session of Er:YAG AFL-assisted MAL-PDT showed superior AC complete response rates at 3 months (92% vs 59%;
Early-Stage Mycosis Fungoides
Mycosis fungoides (MF) is a monoclonal proliferation of CD4+ or CD8+ mature T lymphocytes and is the most common type of cutaneous T-cell lymphoma. MF presents as localized patches or plaques in early stages and often has an indolent course, but may progress to more aggressive tumours and become erythrodermic or metastasize in advance stages. PDT has shown promise in the treatment of early-stage MF; however, there are no placebo-controlled studies exploring the efficacy of PDT with MAL or ALA. In a systematic review of 8 case reports/series with a total of 44 patients found that 67.3% with Stage 1A MF affecting a wide range of body surface areas from 1 to 154 cm2 achieved complete response after PDT (MAL was used in 97.7% of the cases) with a mean of 9.5 treatment cycles. 141 ALA-PDT may be less effective than MAL-PDT for the treatment of early-stage MF. Objective response rates to ALA-PDT every week for up to 6 cycles were only found in 36.4% of patients with refractory MF, defined by failure of at least 2 skin-directed therapies or 1 systemic therapy, with no patients achieving complete remission. 142 A case series showed that 4 to 12 treatments of CO2 AFL-assisted MAL-PDT resulted in complete remission of all 4 patients with Stage 1A MF affecting a body surface area of 8 to 154 cm2 on various sites of the body including the inguinal region, buttocks, cheek, and thigh. 143
Hypericin is an emerging photosensitizer for PDT that is preferentially absorbed by malignant cells and inhibits the proliferation and induces the apoptosis of malignant T lymphocytes.
144
In a phase II placebo-controlled study of patients with patch or plaque MF, twice-weekly hypericin-PDT treatments for 6 weeks resulted in a response rate at 41.7% and 55.6%, with 0.1% and 0.25% hypericin, respectively.
145
In a phase III RCT of patients with Stage 1A or 1B MF, 6 weeks of hypericin-PDT improved index lesion response rates of at least 50% relative to placebo (16% vs 4%;
Extramammary Paget Disease
Extramammary Paget disease (EMPD) is a rare intraepithelial neoplasm that classically presents as erythematous, ill-defined, pruritic, scaly plaques in the anogenital region. The accepted standard of care for EMPD is surgery with either wide-local excision or Mohs micrographic surgery, and non-surgical approaches including laser therapy, topical imiquimod, 5-FU, and radiotherapy have also been utilized. EMPD has a high local recurrence rate even after the gold-standard surgical approaches. A systematic review and meta-analysis of 27 studies, reported recurrence rates of 7.3% and 26.6% after Mohs micrographic surgery and wide-local excision, respectively. 148 A recent systematic review of 30 case series and reports of 177 patients with 211 EMPD lesions found that ALA-PDT and MAL-PDT have complete response rates of 57.7% and 27.4%, respectively; however, they had high recurrence rates of 40% and 35%, respectively. 149 PDT was found to be a valuable adjunct to imiquimod, laser, and surgical therapeutic strategies, with complete response rates of 100%, 60%, and 100% and recurrence rates of 0%, 8.3%, and 25.6% respectively. Since the publication of that systematic review, a case report showed that 6 sessions of MAL-PDT at 4-week intervals followed by topical 5% imiquimod every other day for 4 months resulted in the sustained remission of perianal EMPD during a 2-year surveillance period. 150 Another case series reported that photodynamic diagnosis, which also uses a photo-excitable compound, was valuable to guide tumour excision by forecasting the EMPD tumour margins and that 2 to 4 cycles of ALA-PDT intra- and post-operatively resulted in no local reoccurrences in a mean follow-up of 2.9 years. 151 There is some preliminary evidence that PDT should be considered for patients with EMPD who are poor surgical candidates or as an adjunct to surgical excision, but there is need for comparative studies between PDT and other treatment modalities for EMPD.
Lichen Sclerosis
Lichen sclerosis (LS) is a chronic inflammatory skin disease that typically involves the anogenital areas of postmenopausal women, with the main symptoms being vulvar itch, pain, and dyspareunia. Various treatment modalities have been described in the management of LS including topical corticosteroids, calcineurin inhibitors, estrogens, retinoids, and cryotherapy. Numerous case reports and series have supported the role of ALA-PDT in the treatment of recalcitrant LS of the vulva and penis, with gradual resolution of the burning, pruritis and pain, improved DLQI scores, and reduced lesion sizes.152-155 These findings were concordant with observational studies with a total of 213 patients with LS. Treatment with PDT resulted in LS clinical remission rates of 51% to 100%.156-159 One of the primary limitations of PDT for LS is the significant procedural pain. In 1 case report, the patient refused to be re-treated with MAL-PDT after clinical relapse of her vulvar LS due to the intense pain during the illumination sessions and the distressing experience of local anaesthetic administration. 160 One potential approach to reduce PDT procedural pain is to illuminate with a green light instead of the standard red light source. In a case series of 11 patients, ALA-PDT with green light illumination was efficacious for LS with complete resolution of erosions in all 5 patients who previously had visible vulvar LS erosions and pruritis in 81.8% of patients at 2 months after topical PDT; in addition, no patients complained of severe pain during the sessions that required analgesia or stopping the illumination. 161 A small number of case studies have explored the utility of laser-assisted PDT. The combination of 1927 nm thulium fibre laser followed by MAL-PDT resulted in the complete clearance of recalcitrant LS of the penis in 2 patients and PDL-assisted MAL-PDT improved clearance of extragenital LS lesions compared to PDL alone.162,163 There is evidence that PDT has a role in the management of LS, but there is a need for studies that compare the efficacy of PDT with other accepted treatment approaches for LS.
Folliculitis Decalvans
Folliculitis decalvans (FD) is a rare primary scarring alopecia characterized by painful, recurrent perifollicular pustules resulting from neutrophilic inflammation of the scalp. Combined topical and oral antibiotics, topical and intralesional steroids and oral retinoids are used to manage FD; however, relapses are frequent. 164 PDT has shown some efficacy in the management of FD. Two case reports reported that 3 cycles of MAL-PDT and 4 cycles of ALA-PDT resulted in sustained remission of FD for 1 year without any adjunctive therapy.165,166 These encouraging findings were corroborated by a prospective study showing that 4 sessions of MAL-PDT resulted in a clinical response for 9/10 patients with FD, with 6 patients exhibiting disease remission, and a retrospective study showing that 9/13 patients with FD undergoing 3 sessions of ALA-PDT were well-controlled with no recurrence at 12 months.167,168 However, the literature includes some conflicting results, with 1 case series reporting treatment failure for 3 patients with recalcitrant FD treated with a mean number of 11 MAL-PDT sessions. 169 The evidence suggests that PDT should be considered for refractory FD, but the available studies had small sample sizes and lacked control groups and thus comparative research is required to establish the role of PDT amongst the other treatment options for FD.
Conclusion
Topical PDT is a widely approved therapy for AKs and low-risk NMSCs with a rapidly growing range of emerging indications for other neoplastic, infectious, and inflammatory cutaneous diseases. There is evidence that PDT is superior or noninferior to many other available treatment modalities for AKs, low-risk BCCs, BD, SFC, the chemoprevention of AKs and NMSCs in OTRs, photoaging, acne vulgaris, and cutaneous infections including verrucae, onychomycosis, and CL. There is emerging evidence that PDT plays a role in the management of AC, early-stage MF, EMPD, LS, and FD but there are no comparative studies with other accepted treatment modalities for these conditions. More high-quality, larger-scale RCTs are required to compare topical PDT with active comparators for all approved and emerging indications to support and guide evidence-based clinical decision-making. There is significant heterogeneity in the topical PDT protocols reported in the literature, and more methodological research is required to address the commonly observed barriers to PDT including procedural pain, postprocedural skin reactions, cost of the procedure, and the time spent in the office to complete the PDT therapy.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Consent
Consent was obtained for publication of the images.
