Abstract

To the Editor,
In Canada, teledermatology (TD) offers a promising solution for enhancing dermatological care in rural and remote communities. 1 -3 There are noted discrepancies in rural and remote geographical access to dermatological care that highlight a severe and urgent inequity in Canada. Additionally, Indigenous peoples are more likely to be in rural and remote areas compared to the general population, adding to further inequity. 4 Effective implementation of TD also depends on high-speed broadband internet availability, critical for real-time video consultations and the store-and-forward transmission of high-resolution images. 1,5 The relationship between accessing regional dermatological care and the prevalence of high-speed broadband internet remains unclear.
We performed an analysis using publicly available Canadian geospatial data. With an ecological design, we first assessed the association between the distribution of dermatologists and the presence of high-speed broadband internet within Ontario. All dermatologist practice location data from the College of Physicians and Surgeons of Ontario (CPSO) was extracted on January 3, 2023, and overlapped using publicly available 2021 population data provided by the Canadian Radio-television and Telecommunications Commission (CRTC). CRTC’s 2021 Broadband Coverage in Canada report provided data on broadband speeds and accessibility. Download speeds of ≥25 megabits (Mbit)/s (25+) were used, as the current minimum broadband threshold for video telemedicine per the American Federal Communications Commission’s Mapping Broadband Health. Higher speeds may be required depending on additional requirements. First Nation (FN) reserve communities with and without 25 + internet access were identified. Numerous areas of northern Ontario, when overlapped with dermatologist practice location data, have no access to TD and in-person dermatological care (Supplemental Figure 1).
After review of the distribution of dermatologists and high-speed bandwidth in Ontario, we then investigated availability of high-speed bandwidth across Canada. In total, 633 of 907 (69.7%) of the CRTC reported FN reserve communities in Canada had access to 25 + internet, the minimum speed required for video telemedicine (Figure 1). Smaller provinces such as Prince Edward Island (PEI) and New Brunswick, had the highest 25 + internet coverage (>97%), while provinces such as Newfoundland and Labrador (25.92%), Manitoba (36.46%), and Saskatchewan (43.42%) had the lowest (Supplementary Table 1).
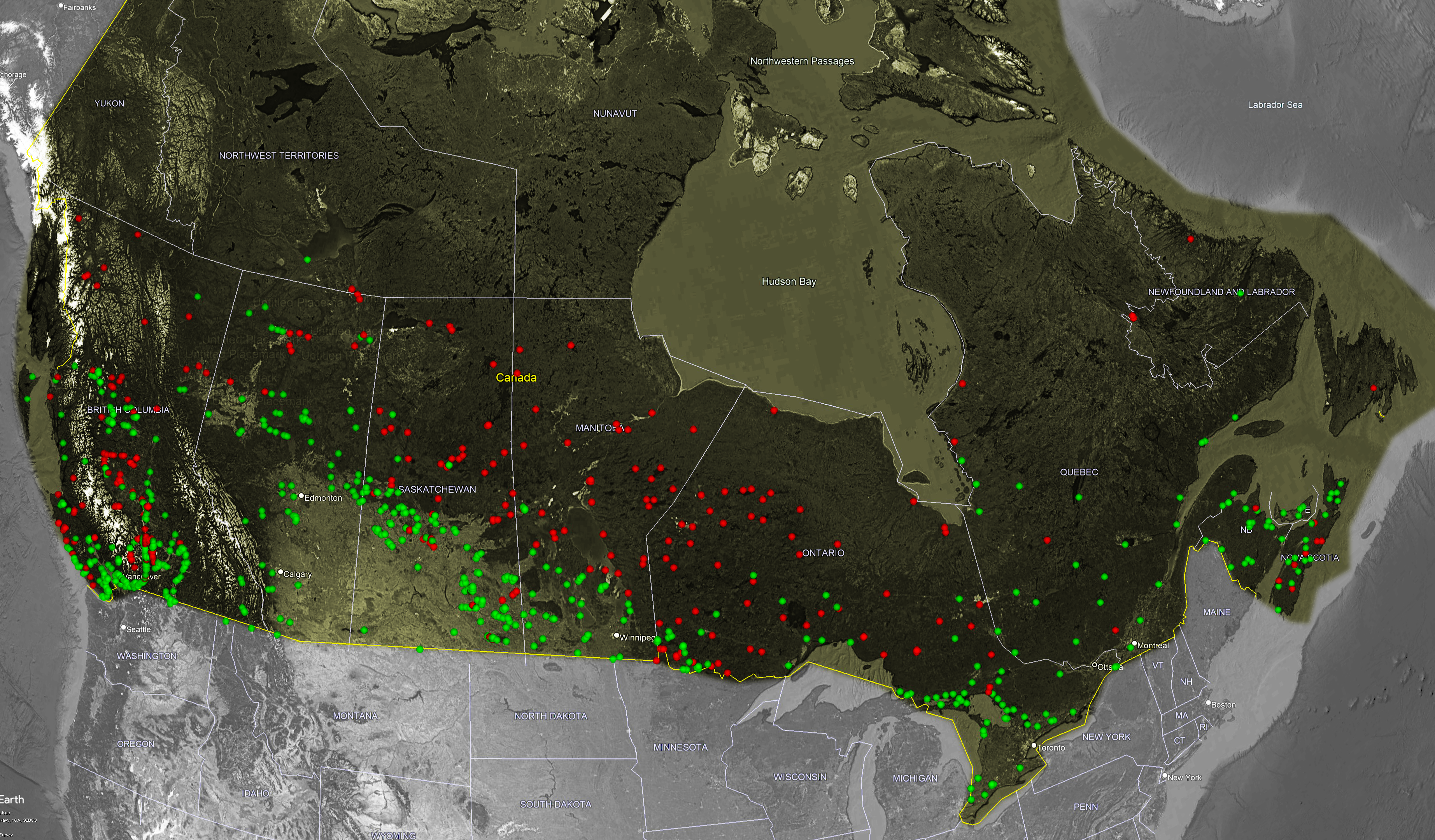
Distribution of FN reserve communities across Canada with access to 25 + broadband internet access. Green, FN reserve community with access to 25 + broadband internet; Red, FN reserve community without access to 25 + broadband internet access.
Initiatives for telemedicine and virtual care solutions exist and may help address barriers. The Real-Time Virtual Support dermatology program with Interior Health in British Columbia, is a virtual program administered via Zoom that connects healthcare professionals in remote and rural areas to a dermatologist in a time-efficient manner. Patients without sufficient internet connection may complete their virtual appointments at a clinic with fast-wired internet, alleviating broadband internet challenges. This innovative program can help address existing gaps, but demands coordination, and introduces challenges related to travel and weather compared to direct TD visits. Since TD requires adequate broadband internet connection, direct care requires improvements in rural and remote areas across many Canadian provinces and territories. 3 Future research should address the efficacy of such programming to alleviate barriers to dermatological care. Limitations of the present study include the binary definitions of adequate broadband internet access, no data in Yukon, and a lack of nationwide dermatologist practice location data.
Supplemental Material
online supplementary file 1 - Supplemental material for Broadband Internet Access in First Nation Reserve Communities and Maldistribution of Canadian Dermatologists: An Ecologic Study
Supplemental material, online supplementary file 1, for Broadband Internet Access in First Nation Reserve Communities and Maldistribution of Canadian Dermatologists: An Ecologic Study by Eric McMullen, Kyle Storm, Mahan Maazi, Jordanna Roesler, Rachel Asiniwasis and Wingfield Rehmus in Journal of Cutaneous Medicine and Surgery
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
