Abstract
Purpose:
Idiopathic orbital myositis, a rare disease of unknown cause, presents a diagnostic puzzle because the diagnosis is based on the exclusion of other diseases. This study aims at elucidating its long-term outcome to answer a clinical question whether idiopathic orbital myositis would be a distinct clinical entity.
Methods:
Retrospective review was made on 7 consecutive patients (6 men and 1 woman) with the age at the initial visit ranging from 33 to 69 years (mean, 45.8 years) who were diagnosed with idiopathic orbital myositis and followed for 5 years or more (mean, 9.2 years) at a referral-based hospital.
Results:
Chief complaint at the initial visit was diplopia in 4 patients, blurred vision in 2 patients, and proptosis in 1 patient. On magnetic resonance imaging, 4 patients showed enlargement of a single extraocular muscle on unilateral side while 3 patients showed enlargement of multiple extraocular muscles on unilateral side or bilateral sides. No patient developed systemic diseases or other orbital lesions in the long-term follow-up. All patients at the last visit were free from symptoms, including diplopia, after tapering of prednisolone at the initial dose of 20 to 60 mg daily.
Conclusion:
Idiopathic orbital myositis had a favorable long-term outcome with corticosteroid administration and appears to be a distinct clinical entity without systemic involvement.
Idiopathic orbital myositis is a rare disease of unknown cause which shows enlargement of one or more extraocular muscles either in unilateral orbit or in bilateral orbits.1–11 The diagnosis is based on orbital imaging, mainly magnetic resonance imaging, and is established only after other causes for extraocular muscle enlargement, such as lymphoma, sarcoidosis, and thyroid disease, have been excluded. Therefore, idiopathic orbital myositis is a kind of wastebasket diagnosis. In this study, we reviewed long-term outcome of 7 patients diagnosed with idiopathic orbital myositis to know whether or not a clinical entity of idiopathic orbital myositis would be reasonable in the present way of diagnosis.
Methods
Retrospective review was made on 7 consecutive patients diagnosed with idiopathic orbital myositis who were followed for 5 years or more at Okayama University Hospital in the 22-year period from January 1996 to September 2018. Patients with other orbital lesions such as lacrimal gland enlargement at the initial visit were excluded from the study. Serum free triiodothyronine (T3) and thyroxine (T4), thyroid-stimulating hormone (TSH), thyroid autoantibodies, and angiotensin-converting enzyme (ACE) activity were measured to exclude thyroid orbitopathy and sarcoidosis as common diseases. The study conformed to the tenets of the Declaration of Helsinki and was approved as a retrospective study by ethics committee of Okayama University Graduate School of Medicine, Dentistry, and Pharmaceutical Sciences (identifier, 1507-012).
Results
The age of 7 patients (6 men and 1 woman) at the initial visit ranged from 33 to 69 years (mean, 45.8 years), and the follow-up period ranged from 5 to 13.5 years (mean, 9.2 years). Chief complaint at the initial visit was diplopia in 4 patients, blurred vision in 2 patients, and proptosis in 1 patient (Table 1). In the follow-up with magnetic resonance imaging (Figure 1), 4 patients showed enlargement of a single extraocular muscle on unilateral side: medial rectus muscle (Figure 1E and F) in 2 patients and lateral rectus muscle (Figure 1A, B, I and J) in 2 patients, 2 patients (Case 2 and 5) showed enlargement of 3 or 4 extraocular muscles on unilateral side (Figure 1C, D, G and H), and the remaining 1 patient (Case 7) showed enlargement of 1 extraocular muscle on one side, together with enlargement of 2 extraocular muscles on the other side. Decreased visual acuity in a patient (Case 6) resulted from compression of the optic nerve by the enlarged muscle (Figure 1I and J).
Summary of 7 consecutive patients with idiopathic orbital myositis.
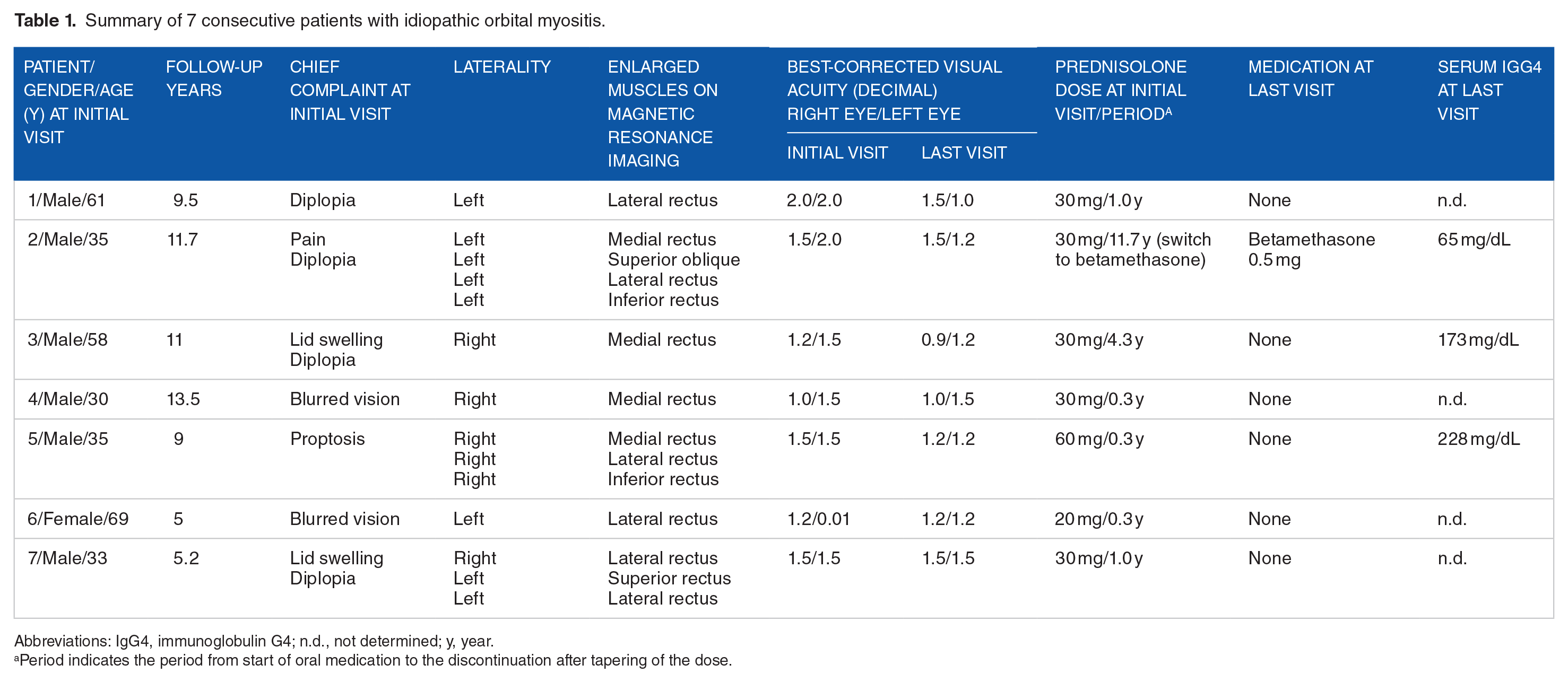
Abbreviations: IgG4, immunoglobulin G4; n.d., not determined; y, year.
Period indicates the period from start of oral medication to the discontinuation after tapering of the dose.
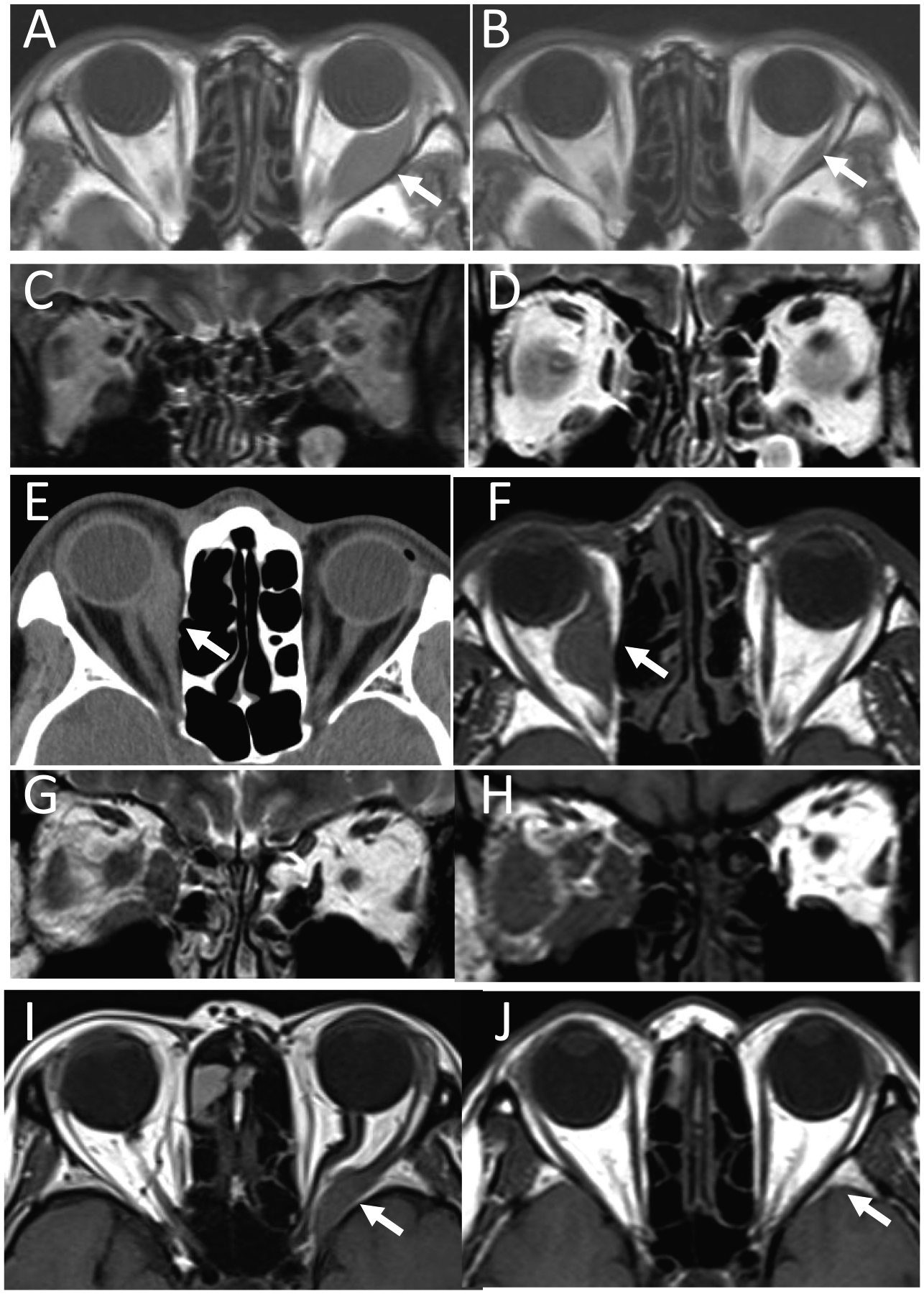
Magnetic resonance imaging or computed tomographic scan of the orbit. Case 1: A 68-year-old man, 7 years after initial visit, showing enlarged lateral rectus muscle on left side (arrow, A), which reduced in size 3 years later at last visit (arrow, B). Case 2: A 35-year-old man at initial visit, showing medial rectus, inferior rectus, lateral rectus, and superior oblique muscle enlargement on left side (C), which became less thickened 7 years later (D). Case 3: A 59-year-old man, 1 year after initial visit, showing enlarged medial rectus muscle on right side (arrow, E, computed tomographic scan), which became further thickened a little bit 1 year later (arrow, F, magnetic resonance imaging). Case 5: A 35-year-old man at initial visit, showing medial rectus, inferior rectus, and lateral rectus muscle enlargement on right side (G), which became further thickened 5 years later (H). This patient used oral corticosteroids only for 4 months at the initial presentation based on his wish. Case 6: A 69-year-old woman at initial visit, showing enlarged posterior part of lateral rectus muscle on left side (arrow, I), which became normal 5 years later (arrow, J). Note that the enlarged muscle compressed the optic nerve (arrow, I), leading to reduction of visual acuity.
Oral corticosteroids were given in all 7 patients to alleviate symptoms (Table 1). Prednisolone was continued in all patients except for one (Case 2) who had a switch to betamethasone because prednisolone did not have an effect on eye pain in this patient. The duration of corticosteroid administration from the start to the discontinuation after tapering of the dose ranged from 0.3 to 11.7 years. Four patients with diplopia as a main symptom took oral corticosteroids for a longer period of the time, 1 year or longer. In contrast, the other 3 patients with blurred vision or proptosis took the drug only for 4 months (0.3 years). The extraocular muscle enlargement became less thickened in the follow-up of all patients except for one patient (Case 5) who only used oral corticosteroids for 4 months in the initial phase of the disease based on his wish. Of the 3 patients with short-term corticosteroid administration, the visual acuity in one woman (Case 6) dramatically returned to 1.2 from 0.01 in a short period, in concordance with the muscle size normalization (Figure 1I and J).
No patient developed systemic diseases or other orbital lesions in the follow-up. All patients at the last visit were free from symptoms with no medication, except for one (Case 2) who continued to use betamethasone 0.5 mg daily. Four patients with diplopia at the initial visit, including Case 2 on continuous oral betamethasone, did not complain of diplopia at the last visit.
Serum immunoglobulin G4 (IgG4) was measured in 3 patients. One patient (Case 2) with multiple extraocular muscle involvement still on corticosteroid use showed a normal level of serum IgG4 at 65 mg/dL at the final visit of this study. Another patient (Case 5) with multiple extraocular muscle involvement under no medication showed serum IgG4 which was elevated to 242 and 228 mg/dL, 1 year before the final visit and at the final visit of this study, respectively. The third patient (Case 3) in subsidence of single extraocular muscle involvement under no medication showed serum IgG4 which was elevated to 173 mg/dL at the final visit.
Discussion
The goal of this study is to elucidate long-term outcome of idiopathic orbital myositis and the role of oral corticosteroids as standard therapy. In addition, a clinical question in this study is whether or not idiopathic orbital myositis would be a distinct clinical entity without systemic involvement. The outcome in the present 7 patients was favorable from the standpoint of no symptoms at the last visit. It should be noted that the patients were largely divided into 2 groups, those with long-term corticosteroid use and those with the short-term use. The patients who presented diplopia as a main symptom had to take corticosteroids 1 year or more. In contrast, corticosteroids were tapered and discontinued in 4 months in the remaining patients because the symptoms such as blurred vision and proptosis had disappeared rapidly. It is understandable that diplopia caused by extraocular muscle enlargement would naturally take time to resolve.
Idiopathic orbital myositis is part of a clinical entity designated as idiopathic orbital inflammation or orbital inflammatory disease which has been previously called orbital pseudotumor.12–16 Idiopathic orbital inflammation is a non-infectious benign inflammatory disease and shows a mass or masses involving any part of the orbit including lacrimal gland, lacrimal sac, eyelid, soft tissue, or extraocular muscles. In the case that only extraocular muscles are involved, the term “idiopathic orbital myositis” is used.
Idiopathic orbital myositis is usually diagnosed clinically based on the exclusion of other inflammatory or neoplastic diseases involving extraocular muscles.1-11 Excisional or needle biopsy of the extraocular muscle is usually not performed because of the difficulty in approaching thin extraocular muscles which pass in close contact with the eye globe along the anteroposterior curvature. Thus, therapeutic diagnosis with oral corticosteroids still remains to be the standard at the setting of clinical ophthalmology. A clinical question as regards to the diagnosis is whether other orbital or systemic diseases would happen to be detected in the process of long-term observation in patients with idiopathic orbital myositis. In the present series of patients, no other orbital or systemic diseases were noted in the long-term follow-up, and thus, the diagnosis of idiopathic orbital myositis appeared to be correct.
The cause for inflammation in idiopathic orbital myositis remains unknown mainly because biopsy has not been done in extraocular muscles. A key for understanding the inflammation in idiopathic orbital myositis would be IgG4. Serum IgG4 measurement has been recently covered by national health insurance reimbursement in Japan. IgG4-related disease frequently involves orbital tissues such as lacrimal glands and inferior orbital nerve. In addition, serum IgG4 has been reported to be elevated in some patients who were diagnosed as orbital myositis.17–19
In the present series of patients, serum IgG4 in 2 patients with multiple extraocular muscle involvement gave contradictory results: a normal IgG4 level in one patient who was still on corticosteroid use, and in contrast, elevated IgG4 levels in another patient with no medication. The third patient with preceding single extraocular muscle involvement showed an elevated IgG4 level under no medication long after the subsidence of myositis. Corticosteroid administration might influence the serum IgG4 level, but the role of IgG4 remains undetermined in the present series of patients with idiopathic orbital myositis. The elevation of serum IgG4 would be otherwise a non-specific finding because tissue staining with IgG4 was not available in these patients.
The exclusion of lymphoma is most difficult at the diagnosis of idiopathic orbital myositis. I previously encountered a patient with medial rectus muscle enlargement on unilateral side who happened to have metastasis of neuroendocrine tumor (carcinoid) to the extraocular muscle. 20 Idiopathic orbital myositis is difficult to be differentiated from extraocular muscle metastasis and lymphoma from the standpoint of orbital imaging. Natural course of the extraocular muscle enlargement as well as the response to corticosteroids should be carefully observed in long-term follow-up. The enlarged muscle would remain in the same size or would become less thickened in the long-term time course in the present series of patients with idiopathic orbital myositis. The response to corticosteroids would be also assessed on the basis of other symptoms or signs such as lid swelling or pain.
In conclusion, the 7 present patients with idiopathic orbital myositis who were diagnosed on clinical basis did not show any other orbital lesions or systemic manifestations in years of the long-term observation. Thus, idiopathic orbital myositis appears as a distinct clinical entity. Oral corticosteroids have an effect on reducing the extraocular muscle thickening and thus on alleviating the symptoms. There is, of course, a limitation in the clinical diagnosis of idiopathic orbital myositis which is not based on the pathological diagnosis. Although the patients in the present series have been followed up and have not manifested any sign of systemic involvement, still a question remains unanswered as to whether these cases would be truly idiopathic.
Footnotes
Author Contributions
TM followed up all patients; had conception and design; did data collection, analysis, and interpretation; and wrote the manuscript.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
