Abstract
Objective:
Although safety concerns still remain among patients undergoing unanticipated noncardiac surgery after prior percutaneous coronary intervention (PCI), it has not been directly compared with coronary artery bypass grafting (CABG). The objective of this study was to compare clinical outcomes after noncardiac surgery in patients with prior (>6 months) coronary revascularization by PCI or CABG.
Methods:
From February 2010 to December 2015, 413 patients with a history of coronary revascularization, scheduled for noncardiac surgery were identified. Patients were divided into PCI group and CABG group and postoperative clinical outcome was compared between 2 groups. The primary outcome was composite of all-cause death, myocardial infarction, and stroke in 1-year follow-up.
Results:
The 413 patients were divided according to prior coronary revascularization types: 236 (57.1%) into PCI and 177 (42.9%) into CABG group. In multivariate analysis within 1-year follow-up, there was no significant difference in clinical outcome which was composite of all-cause death, myocardial infarction, and stroke (hazard ratio [HR]: 1.50; 95% confidence interval [CI]: 0.76-2.93; P = .24). The same result was present in propensity-matched population analysis (HR: 1.43; 95% CI: 0.68-3.0; P = .34).
Conclusions:
In patients undergoing noncardiac surgery with prior coronary revascularization by PCI or CABG performed on an average of 42 months after PCI and 50 months after CABG, postoperative clinical outcome at 1-year follow-up is comparable.
Introduction
The advancements in various techniques and devices have reduced mortality of coronary heart disease (CHD). Two distinct revascularization strategies in CHD have been compared not only in survival rates but also in many aspects including angina frequency and physical limitations. In general, coronary artery bypass graft surgery (CABG) provided slightly better intermediate-term health status and quality of life than percutaneous coronary intervention (PCI) in most of the studies. 1
Noncardiac surgery after coronary revascularization is another issue. In asymptomatic patients, prophylactic coronary revascularization before noncardiac surgery is not recommended by either CABG or PCI, whereas CABG has traditionally been suggested in symptomatic patients because noncardiac surgery shortly after CABG carries relatively low risk of cardiac complication.2–5 Although many studies have also shown the perioperative cardiovascular stability of prior PCI in patients undergoing noncardiac surgery, debate still exists, and most of the former studies have compared PCI with medical therapy.6–8 This study is aimed to compare the impact of prior PCI with CABG on clinical outcomes of noncardiac surgery.
Methods
Study population and data collection
This study was a single-center retrospective study from February 2010 to December 2015. The inclusion criteria were as follows: (1) patients who had a history of coronary revascularization by either PCI or CABG and (2) patients who underwent noncardiac surgery. The exclusion criteria were as follows: (1) patients with less than 6 months of duration after coronary revascularization, (2) patients who underwent both PCI and CABG, and (3) patients who underwent prophylactic PCI or CABG due to CHD incidentally diagnosed during preoperative evaluation. In patients with multiple noncardiac surgeries, only the first surgery after coronary revascularization was enrolled in the analysis. Clinical, laboratory, and outcome data of 1-year follow-up were collected by a trained study coordinator using a standardized case report form and protocol. The study protocol was approved by the Institutional Review Board of our hospital.
Definition and outcomes
Surgery was defined as the procedures performed under general or regional anesthesia. Risk stratification of surgery was according to 2014 European Society of Cardiology/Anaesthesiology (ESC/ESA) guideline. 9 Clinical characteristics and history of medications were collected at the time of surgery. Diabetes mellitus was defined as having a history of type 1 or type 2 diabetes mellitus, with history of treatment by medication or dietary changes. Hypertension was self-reported by patient or systolic blood pressure >140 mm Hg at rest. Stroke was defined as brain hemorrhage, transient ischemic attack, and cerebral infarction.
The primary outcome was defined as composite of all-cause death, myocardial infarction, and stroke during 1-year follow-up. The secondary outcomes were as composite of all-cause death, myocardial infarction, and stroke during in-hospital stay and repeat revascularization during 1-year follow-up and in-hospital stay. Each composite of primary outcomes was also analyzed.
Statistical analysis
For continuous variables, differences between each group were compared using the t test or the Wilcoxon rank sum test and presented as mean ± SD or median and interquartile range (IQR) when applicable. The χ2 test or Fisher exact test was used for categorical data. Survival curves were constructed using Kaplan-Meier estimates and compared with the log-rank test. For clinical outcomes in 1-year follow-up, adjusted hazard ratio (HR) was compared using Cox regression based on the following covariates: age, male, multivessel coronary disease, valvular heart disease, peripheral arterial disease, and left ventricular ejection fraction <50%. The same covariates were adjusted in logistic regression analysis to compare odds ratio (OR) of clinical outcomes during in-hospital stay. To reduce treatment selection bias for revascularization types and potential confounding factors, we performed rigorous adjustments for patients’ baseline and preoperative characteristics using their propensity scores estimated using multiple logistic regression analyses. An absolute standardized difference <10% for the measured covariate suggested an appropriate balance between the groups. In the propensity score–matched populations, we compared HR for clinical outcomes in 1-year follow-up using a Cox regression model with a robust variance estimate and OR for clinical outcomes during in-hospital stay using logistic regression analysis. Statistical analyses were performed with SAS 9.4 (SAS Institute Inc., Cary, NC, USA). All tests were 2-tailed and P < .05 was considered statistically significant.
Results
A total of 561 patients were initially enrolled. In all, 67 patients were excluded due with less than 6 months of duration after coronary revascularization, 74 patients due to both PCI and CABG, and 7 patients due to prophylactic revascularization during preoperative evaluation. A total of 413 patients who met criteria were remained for analysis. The flowchart of patients is summarized in Figure 1. The median duration from coronary revascularization to surgery was 42 months (IQR: 18-88) in PCI group and 50 months (IQR: 23-101) in CABG group (P = .07).
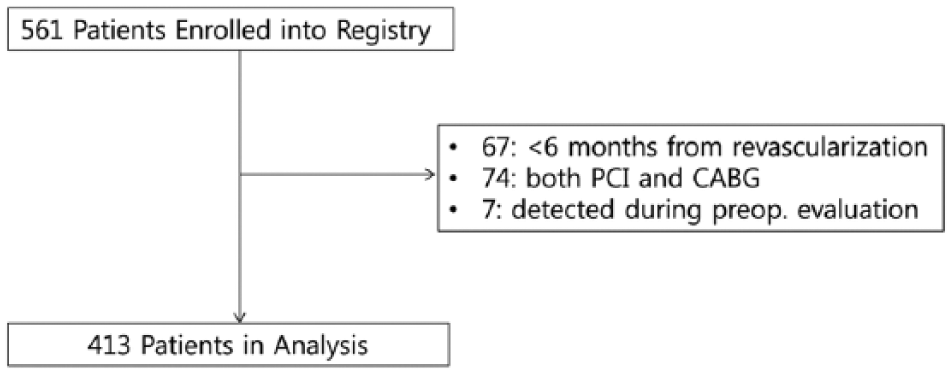
The flowchart of patients. CABG indicates coronary artery bypass grafting; PCI, percutaneous coronary intervention.
Baseline characteristics
Patients were divided into 2 groups: 236 (57.1%) in PCI group and 177 (42.9%) in CABG group. The median follow-up periods were 365 days (341-365) in PCI group and 365 days (282-365) in CABG group (P = .47). The baseline characteristics are summarized in Table 1. Valvular heart disease, history of peripheral arterial disease, multivessel coronary disease, and left ventricular ejection fraction <50% were more frequently present in CABG group. Table 2 shows preoperative characteristics of each group. After performing propensity score matching for the entire population, a total of 142 pairs of matched data sets were generated by 1:1 individual matching without replacement. We found no significant imbalance in the baseline characteristics between the PCI and the CABG groups for the propensity-matched subjects (Tables 1 and 2).
Baseline characteristics.
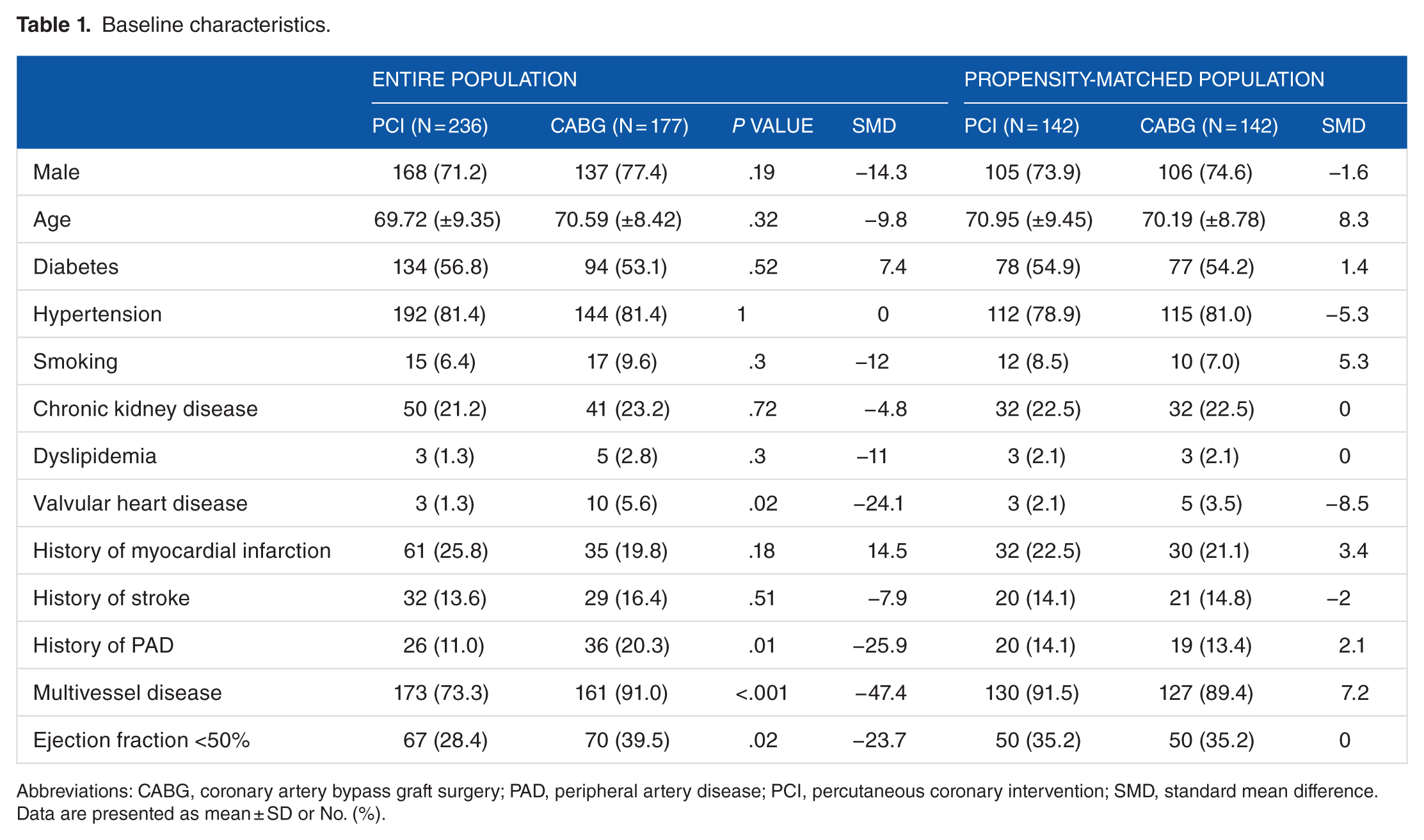
Abbreviations: CABG, coronary artery bypass graft surgery; PAD, peripheral artery disease; PCI, percutaneous coronary intervention; SMD, standard mean difference.
Data are presented as mean ± SD or No. (%).
Preoperative characteristics.
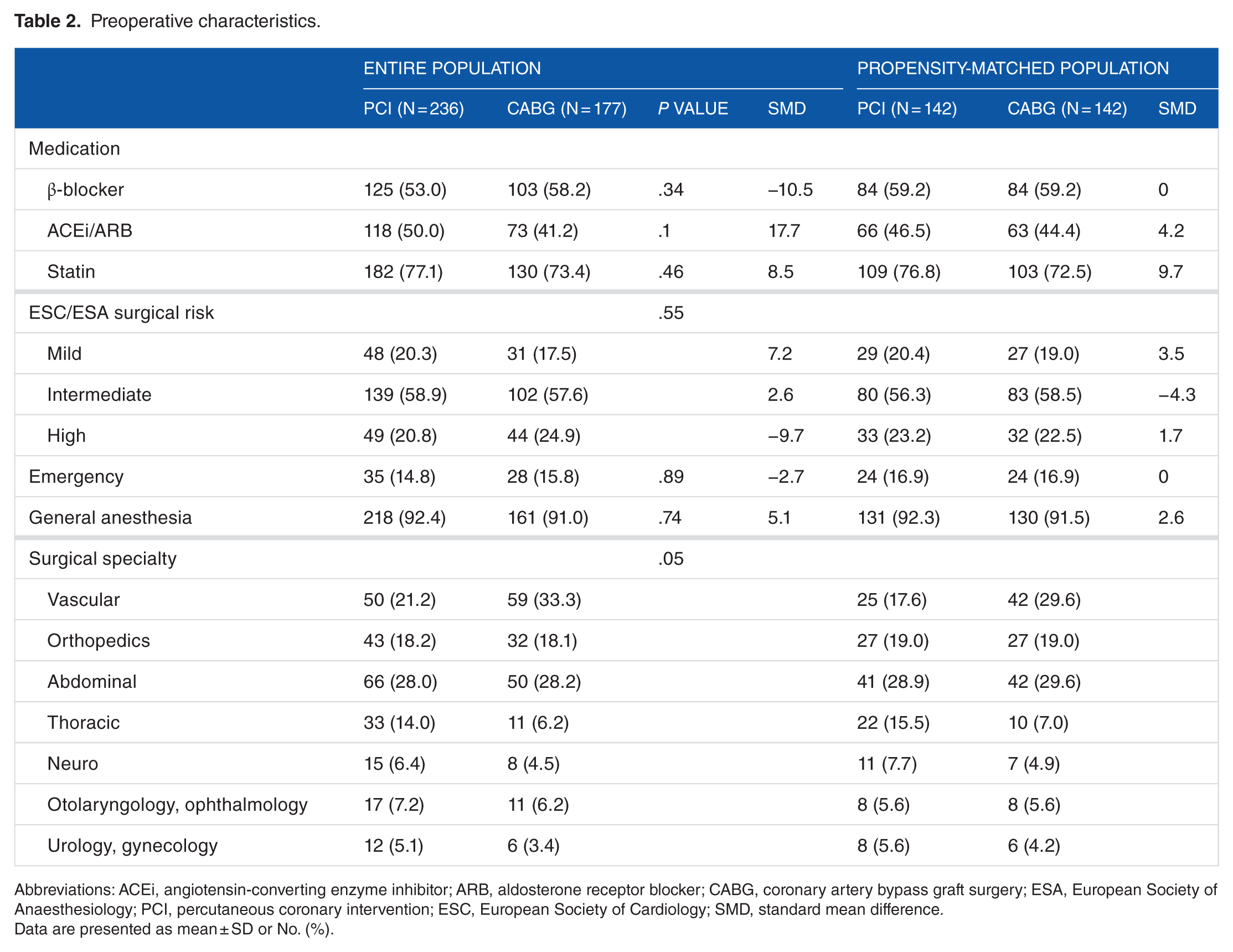
Abbreviations: ACEi, angiotensin-converting enzyme inhibitor; ARB, aldosterone receptor blocker; CABG, coronary artery bypass graft surgery; ESA, European Society of Anaesthesiology; PCI, percutaneous coronary intervention; ESC, European Society of Cardiology; SMD, standard mean difference.
Data are presented as mean ± SD or No. (%).
Clinical Outcomes
The clinical outcomes during in-hospital stay showed no difference in both entire and propensity-matched populations (Tables 3 and 4). In multivariate analysis, the incidence of composite of all-cause death, myocardial infarction, and stroke in 1-year follow-up was not significantly different (HR: 1.50; 95% confidence interval [CI]: 0.76-2.93; P = .24). In propensity-matched population, the results were also not significant (HR: 1.43; 95% CI: 0.68-3.0; P = .34). The clinical outcomes in 1-year follow-up are summarized in Tables 5 and 6. Survival curves for entire and propensity-matched population are shown in Figure 2.
In-hospital clinical outcomes in entire population.
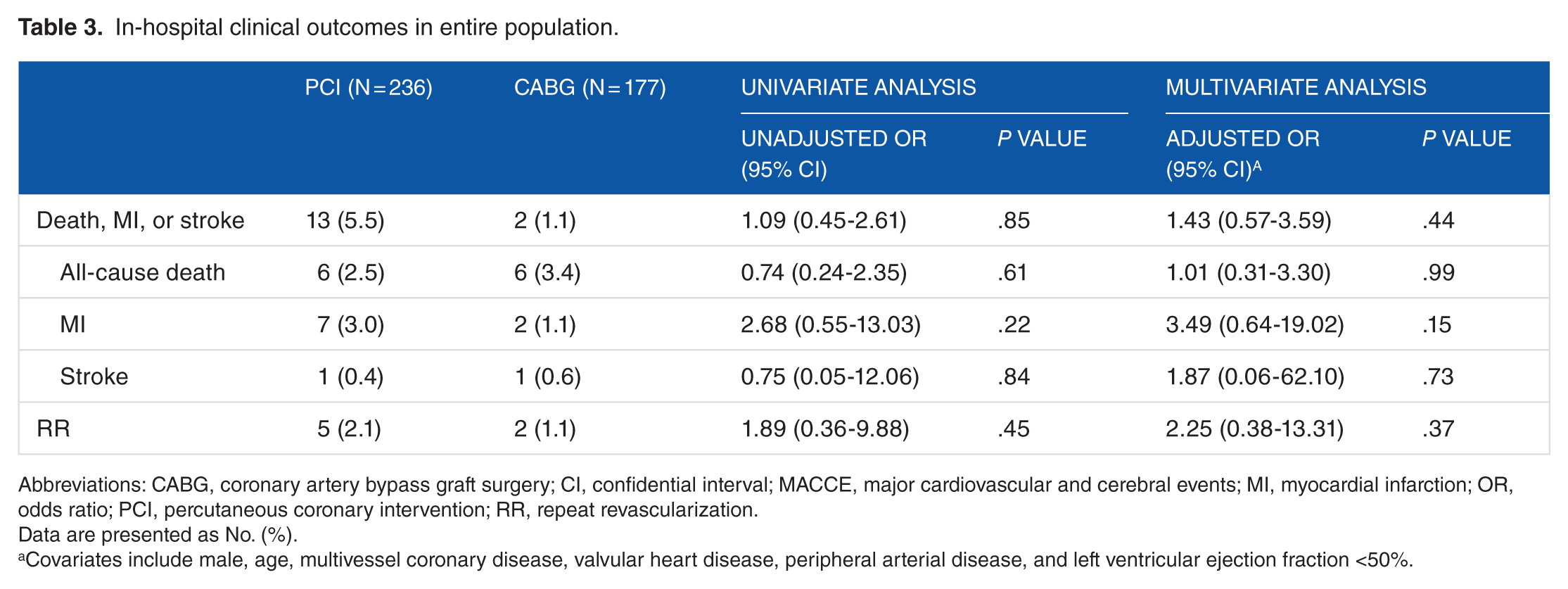
Abbreviations: CABG, coronary artery bypass graft surgery; CI, confidential interval; MACCE, major cardiovascular and cerebral events; MI, myocardial infarction; OR, odds ratio; PCI, percutaneous coronary intervention; RR, repeat revascularization.
Data are presented as No. (%).
Covariates include male, age, multivessel coronary disease, valvular heart disease, peripheral arterial disease, and left ventricular ejection fraction <50%.
In-hospital clinical outcomes in propensity-matched population.
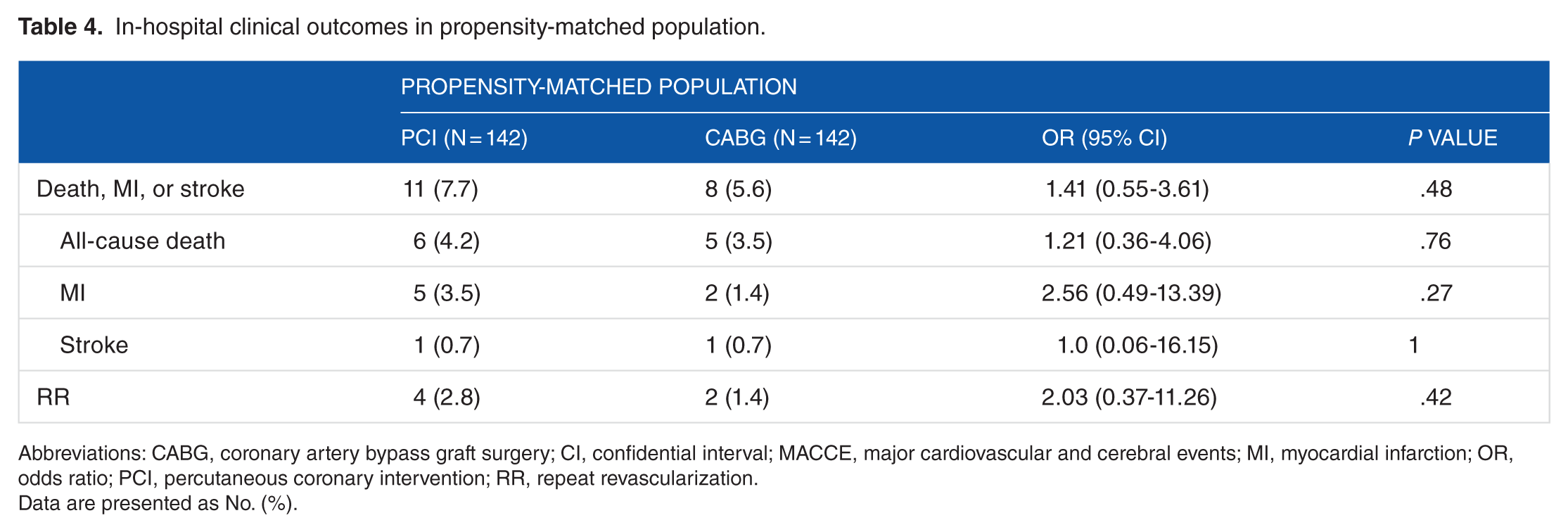
Abbreviations: CABG, coronary artery bypass graft surgery; CI, confidential interval; MACCE, major cardiovascular and cerebral events; MI, myocardial infarction; OR, odds ratio; PCI, percutaneous coronary intervention; RR, repeat revascularization.
Data are presented as No. (%).
One-year clinical outcomes in entire population.
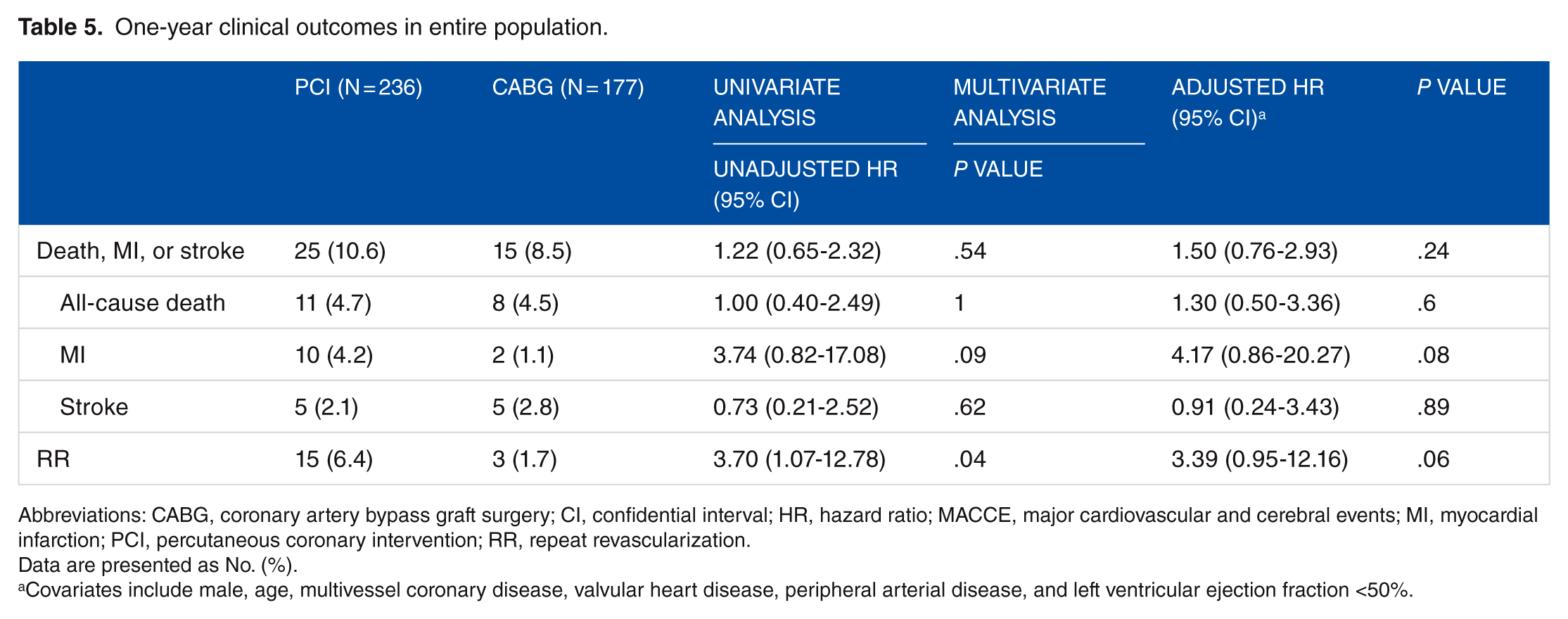
Abbreviations: CABG, coronary artery bypass graft surgery; CI, confidential interval; HR, hazard ratio; MACCE, major cardiovascular and cerebral events; MI, myocardial infarction; PCI, percutaneous coronary intervention; RR, repeat revascularization.
Data are presented as No. (%).
Covariates include male, age, multivessel coronary disease, valvular heart disease, peripheral arterial disease, and left ventricular ejection fraction <50%.
One-year clinical outcomes in propensity-matched population.
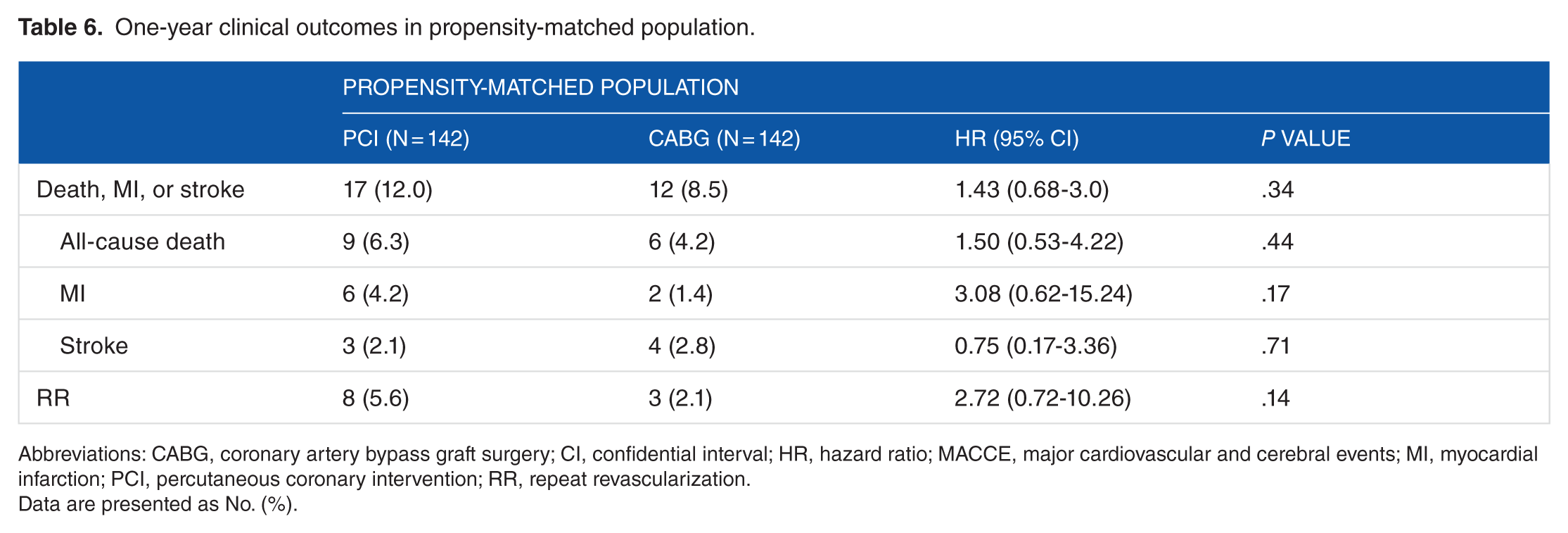
Abbreviations: CABG, coronary artery bypass graft surgery; CI, confidential interval; HR, hazard ratio; MACCE, major cardiovascular and cerebral events; MI, myocardial infarction; PCI, percutaneous coronary intervention; RR, repeat revascularization.
Data are presented as No. (%).
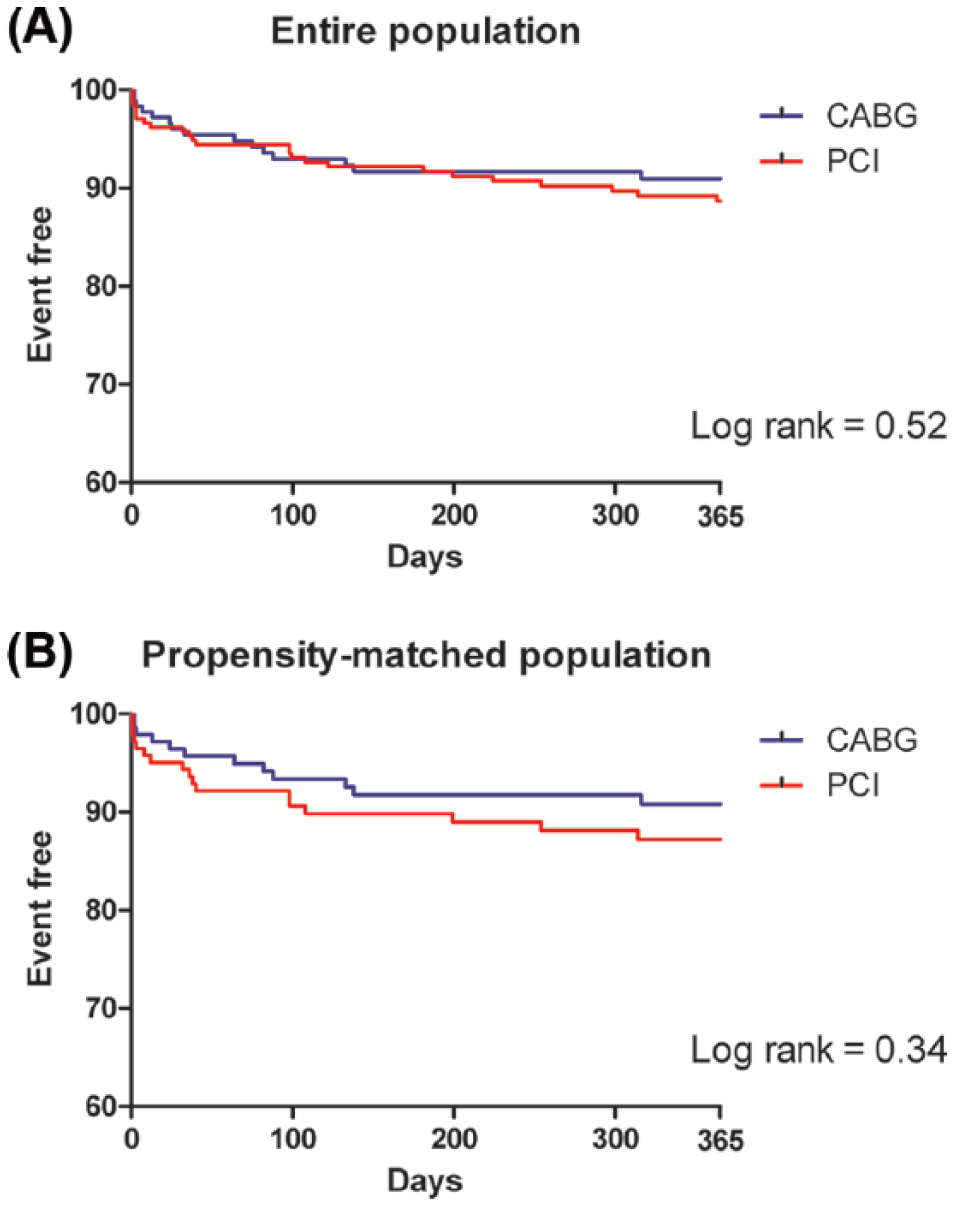
The Kaplan-Meier curves of all-cause death, myocardial infarction, or stroke in (A) entire population and (B) propensity-matched population. CABG indicates coronary artery bypass grafting; PCI, percutaneous coronary intervention.
Discussion
This study shows that in patients undergoing noncardiac surgery with prior coronary revascularization by PCI or CABG performed on an average of 42 months after PCI and 50 months after CABG, postoperative clinical outcome at 1-year follow-up is comparable.
The advancements in various techniques and devices have reduced mortality of patients who were treated with coronary revascularization by either PCI or CABG. In addition, this reduction in mortality rate was not only in patients with acute coronary syndrome but also in patients with stable coronary disease. 10 Hence, average life expectancy of patients with CHD has also increased leading to higher chance of other pathologic conditions which may require surgical treatment. 11
Coronary heart disease still remains as a well-known risk factor of surgery. Noncardiac surgery is associated with an average overall annual mortality rate of 0.8% to 1.5% and up to 42% of these are caused by cardiac complications. 9 During a perioperative period, many patients who would not require revascularization undergo revascularization prophylactically. A current guideline on perioperative cardiac evaluation suggests that coronary revascularization should be reserved for patients with unstable symptoms who are indicated independent of surgery. 12 The answers to question of which patients would benefit from preoperative revascularization are still debatable calling for further studies. And whether PCI provides the same degree of protection for future noncardiac surgery is unanswered. In this study, prophylactic coronary revascularization on lesions detected during preoperative evaluation was excluded to focus on long-term effect of coronary revascularization on postoperative outcome of noncardiac surgery.
Percutaneous coronary intervention has become a reasonable treatment option for CHD and shows comparable outcomes with CABG in many aspects. However, some evidence still indicate that CABG may be superior to PCI under specific conditions with a potential benefit in patients with diabetes and multivessel disease with complex lesions.13–17 Coronary artery bypass graft surgery has also traditionally been chosen over PCI for prophylactic revascularization before noncardiac surgery in patients with significant coronary artery disease with unstable symptoms.2–5 Moreover, a recent ESC/ESA guideline does not recommend a routine angiography in patients with history of CABG in the past 6 years based on the analysis showing prominent protective effect of CABG.9,18 However, safety concerns still exist for prior PCI. Postoperative risk is considered to decrease over time but the minimal safety duration required after PCI is still debated. The most recent study has reported that increased risk was only present within the first month after PCI. 19 However, most studies have shown increased risk of adverse events in patients undergoing noncardiac surgery within minimum of 6 months after PCI.6,8,20,21 Patients with less than 6 months of duration after coronary revascularization were excluded from this study.
A previous study compared postoperative outcome of patients with preceding PCI to medical therapy without stent and showed no difference in mortality but an increased risk of myocardial infarction and revascularization during a year after PCI. 22 In this study, clinical outcome of noncardiac surgery after PCI was compared with CABG and showed comparable result. The incidence of repeat revascularization was numerically higher in PCI group, which was partly consistent with previous studies on quality of life after coronary revascularization.15,22 However, this difference was not statistically significant after adjustment. The assumed reasons for insignificance are as follows. First, this study was only done among 1-year follow-up which may be insufficient duration for events to occur. Second, this study was done on relatively small number of patients.
As, number of patients with prior coronary revascularization increases with improved survival rate, clinicians more commonly encounter noncardiac surgeries in patients with prior coronary revascularization. This study has advantages over previous studies on noncardiac surgery after coronary revascularization. Traditional studies on cardiac risk of noncardiac surgery compared medical treatment with PCI or CABG and showed a benefit of coronary revascularization especially in patients with unstable symptoms.6–8,23,24 And recent studies mostly focus on types of stent and safety duration.6,8,20,21 However, despite shared benefit and risk among coronary revascularization types, there are also factors unique to each type of revascularization. In this regard, this study directly compared postoperative clinical outcome of PCI with CABG to better evaluate relative risk of noncardiac surgery. In addition, unlike previous studies focusing on prophylactic revascularization, this study limited participants to unanticipated noncardiac surgeries at the point of coronary revascularization in which randomized trial is not feasible.
The limitations of this study are that it is a single-center, observational study. The number of patients analyzed is small. Confounding factors could have significantly affected the results. Although a propensity score–matched analysis was performed to adjust for these potential confounding factors, unmeasured ones were not able to be corrected. Another limitation is an insufficiency of detailed medical information in patients with coronary revascularization performed other than our medical center. Although transferred with former medical chart, detailed information of coronary revascularization such as vessel number, stent type and complete revascularization may not fully available in every patients. Also, as a nature of retrospective study, an accurate functional status was not available in every patients, therefore could not be analyzed. We excluded patients with PCI or CABG performed less than 6 months before the noncardiac surgery. No conclusion can be drawn on the management of patients during this time frame. Despite these limitations, this is the first study analyzing the outcomes after noncardiac surgery in patients revascularized by either PCI or CABG. A better understanding of the relative risk for noncardiac surgery after PCI compared with CABG is necessary for further evaluating quality of life after coronary revascularization.
Conclusions
In patients undergoing noncardiac surgery with prior coronary revascularization by PCI or CABG performed on an average of 42 months after PCI and 50 months after CABG, postoperative clinical outcome at 1-year follow-up is comparable. Larger registries are necessary to confirm these results.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration Of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
JP and SHL has equally contributed to this work; designed the study and wrote the manuscript. JK and MP collected the data. HCG and YTL analyzed the data. SML critically reviewed the manuscript and supervised the whole study process. All authors read and approved the final manuscript.
