Abstract
There are powerful demographic, political, and environmental trends shaping women’s health. Increases in life expectancy, literacy, and empowerment are fueling expansions in education and advocacy. Research and development focuses on women’s health and fertility across an expanded age spectrum. There is also a cultural emphasis on antiaging and aesthetics. In parallel, the digital revolution is changing how health care is accessed by and delivered to women. A women’s journey through menopause is at the crossroads of these transformations. Medical and social platforms encourage women to embrace menopause as a pivotal life stage. Yet, many women are reticent to discuss “the transition” due to embarrassment about its symptoms, lack of awareness of its physical manifestations, or fear of aging. We introduce a patient-centric framework to support patient-provider engagement on menopause: prevention, anxiety, urogenital symptoms, vasomotor symptoms, and education. Although not comprehensive, PAUSE represents an acronym and reminder to focus a portion of the medical interaction on menopause.
Introduction
Menopause care is at the epicenter of multiple transformations affecting women’s health. From research and development advances and the digital revolution to shifting cultural attitudes, dimensions of care including education, selection, utilization, and perception are in flux. The menopause hormone therapy paradigm has dramatically evolved over time due to the landmark 2002 Women’s Health Initiative (WHI) which is still debated 15 years later.1,2 Open questions pervade menopause care delivery: Who should deliver care within a multidisciplinary system? What evaluations such as gynecologic examinations are required and at what frequency? How do providers and patients make appropriate benefit-risk decisions regarding therapeutic interventions? Dynamic answers reflect changing primary and gynecologic care guidelines and economic realities affecting access and utilization. There is a consequent need and opportunity for concentrated and consistent discourse between patient and provider on menopause.
PAUSE Framework Defined
To support an effective and efficient focus on menopause in the patient-provider interaction, we introduce the PAUSE framework to highlight 5 areas of care: prevention, anxiety, urogenital symptoms, vasomotor symptoms (VMS), and education (Figure 1). Each element of the framework represents a menopause topic area and trigger question.
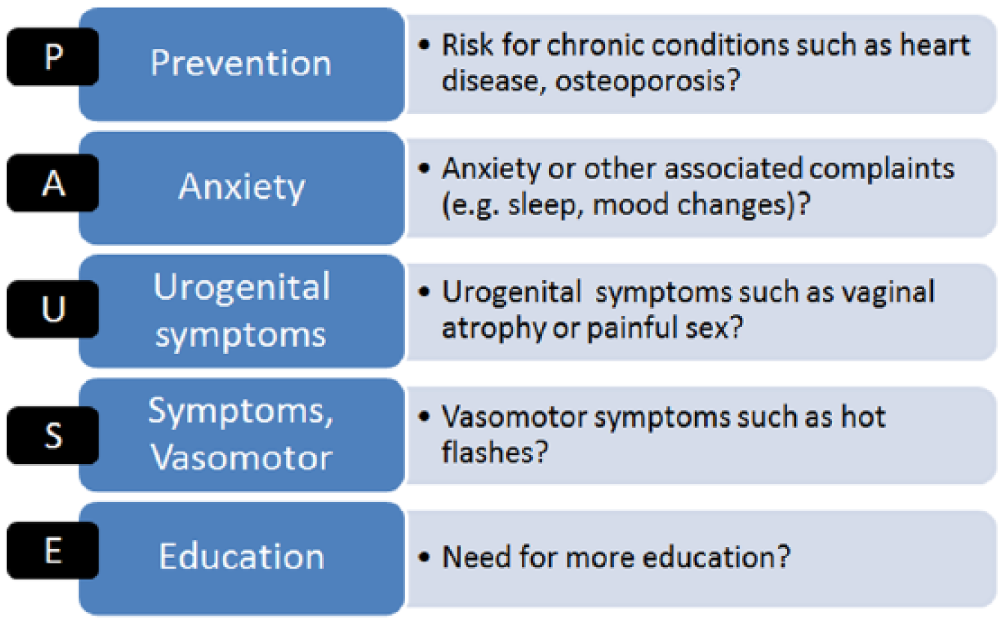
PAUSE framework: 5 elements and questions.
Prevention
Menopause is associated with increased risk of certain chronic diseases including cardiovascular disease and osteoporosis. The first and arguable most important element of the PAUSE framework is Prevention to assess and address a patient’s risk for these conditions. For example, for heart disease prevention, lifestyle-based recommendations including eating a healthy diet and maintaining a normal weight and physical activity such as walking are critical recommendations. 3 As metabolism slows through aging and menopause, weight management becomes more challenging and there is a need to continually engage on the topic and discuss strategies for weight loss. Blood pressure and cholesterol control may be necessary. For patients at risk for osteoporosis, lifestyle management recommendations including weight bearing exercise, vitamin D supplementation, and intake of adequate calcium should be reviewed. In some instances, prescription medications are a consideration for osteoporosis prevention. 4
Anxiety
Women may experience mood swings, difficulty concentrating, and stress through menopause. The Anxiety element called out in the PAUSE framework refers to anxiety or potential psychiatric symptoms such as mood disorder which tend to occur at higher rates in perimenopausal and postmenopausal women.5,6 Anxiety is a broad term that may manifest as nervousness, sleeplessness or frequent waking during the night, difficulty concentrating, and/or irritability. It may be seen concurrently with depression. This topic area is highlighted because it often goes unrecognized and it is important to make a distinction between general anxiousness and an anxiety disorder which interferes with a women’s ability to function. Also, the potential impact of menopause on sleep should be addressed.
Urogenital symptoms
The loss of estrogen through menopause may result in vulvar and vaginal atrophy (VVA) and the PAUSE framework focuses on identifying associated Urogenital Symptoms. In 2014, the term genitourinary syndrome of menopause was introduced to encompass a multitude of urogenital symptoms such as genital dryness, dyspareunia, irritation and itching of vulva or vagina, urinary frequency/urgency, and urinary tract infections. 7 First-line treatment for mild VVA symptoms includes over-the-counter vaginal moisturizers and lubricants. For moderate to severe VVA symptoms, prescription treatments include vaginal estrogen therapy which is available as creams, tablets, or rings. Product innovations in this arena include new doses, products, and administration options for VVA-associated indications such as dyspareunia.8,9 For urinary symptoms including stress and urge incontinence, behavioral or medical therapy may be appropriate.
Symptoms, vasomotor
Vasomotor symptoms, referred to as hot flashes or flushes, are the most common menopausal symptoms. The fourth element of the PAUSE framework assesses for the presence and impact of Vasomotor Symptoms. The ways these symptoms manifest and how women experience them is highly variable. In clinical trials, they are often characterized by their degree of severity. Symptoms are described as minor for the sensation of heat without sweating, moderate for the sensation of heat with sweating and the ability to continue activity, and severe for the sensation of heat with sweating and disruption of activity. 10 Newer tools to assess vasomotor symptoms incorporate physical symptoms and quality of life impacts.
Before 2002, most of the postmenopausal women were treated with menopausal hormone therapy until data from WHI showcased certain health risks associated with their use and the Food and Drug Administration encouraged manufacturers to update their labels with boxed warnings. Since then, the number of women using menopausal hormone therapy has decreased significantly. 11 Provider education to patients on this topic is critical. The North American Menopause Society (NAMS) MenoPro app is one of several tools available to support discussions of benefit-risk and individual treatment selection. 12 Behavioral changes may help with mild symptoms. For treatment of moderate to severe symptoms, approved prescription medical options include estrogen-only therapy for postmenopausal women without a uterus. For those women with a uterus, options include estrogens in combination with progestational agents or estrogens with a selective estrogen receptor modulator. Nonhormonal options may also be appropriate. Other considerations include various modes of administration for these products and patient preference.
Education
Menopause conversations may be challenging for patients and providers. The final step of the PAUSE framework focuses on Education to ensure patients have their questions answered with evidence-based content. Women often use online resources and social communities to obtain menopause information, the quality of which is highly variable. Also, patient education may be influenced by information on compounded “bioidentical” hormonal products, a practice which multiple health professional organizations warn against save for particular situations.13–15 To address this PAUSE element, in addition to one-on-one interactions, the provider may sponsor menopause counseling in a private or group setting. Patients may be directed to reviewed resources such as the Office on Women’s Health at https://www.womenshealth.gov/menopause/. 16 Numerous health professional organizations also have patient portals.
PAUSE Framework Implementation
The PAUSE framework may be initiated during any patient interaction or integrated into annual or wellness visits. Any caregiver involved in menopause care may use the framework. Although not comprehensive, it can serve as a mechanism to initiate a sometimes difficult conversation or drive health literacy. Given the ease of the acronym, the framework may be raised by the patient herself, her partner, or an involved caretaker.
Conclusions
Menopause represents a medical journey that women experience differently but which all will undergo. Here, we use the term PAUSE, to our knowledge for the first time, as an acronym and framework to support the patient-provider conversation on menopause. It is intended to be holistic, multidisciplinary, and to include prevention, treatment, and education elements to support appropriate evidence-based interactions. Taking a PAUSE literally and figuratively during the patient-provider interaction can support menopause care.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests:
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: R.A. is Pfizer employee and stockholder. M.E.P. has no disclosures.
Author Contributions
RA wrote the first draft of the manuscript. RA and MEP contributed to the writing of the manuscript, agree with manuscript results and conclusions, jointly developed the structure and arguments for the paper, made critical revisions and approved final version, and reviewed and approved the final manuscript.
Disclosures and Ethics
As a requirement of publication, authors have provided to the publisher signed confirmation of compliance with legal and ethical obligations including but not limited to the following: authorship and contributorship, conflicts of interest, privacy and confidentiality, and (where applicable) protection of human and animal research subjects. The authors have read and confirmed their agreement with the ICMJE authorship and conflict of interest criteria. The authors have also confirmed that this article is unique and not under consideration or published in any other publication, and that they have permission from rights holders to reproduce any copyrighted material. The external blind peer reviewers report no conflicts of interest.
