Abstract
Objective:
We investigated the efficacy and safety of retrograde intrarenal surgery (RIRS) as a primary treatment for staghorn calculi.
Methods:
From 2012 to 2016, we identified 39 patients with staghorn calculi who received RIRS as a primary treatment. During the study period, no staghorn calculi were treated primarily with percutaneous nephrolithotomy or any other modality. A stone-free status after RIRS was defined as no detectable stone fragments on X-rays or computed tomography scans.
Results:
Of 39 patients who received 134 procedures (median 3 procedures per patient; range: 1-11; mean stone length: 60.5 ± 23.0 mm), 18 (46%) and 21 (54%) had staghorn calculi <60 and >60 mm in maximum length, respectively. The stone-free rates after the first and final procedures were 21% (8 of 39) and 62% (24 of 39), respectively; overall, 39% (7 of 18) and 78% (14 of 18), respectively, for the 18 patients with <60 mm staghorn calculi; and 5% (1 of 21) and 48% (10 of 21), respectively, for the 21 patients with >60 mm calculi. Multivariate analysis revealed a maximum stone length >60 mm to be the only independent predictor of a stone-free status after the first and final procedures. During the treatment series, perioperative complications occurred in 16 (41%) patients. Only one patient presented with a Clavien-Dindo grade III complication (malposition of a ureteral stent).
Conclusions:
RIRS is a safe and effective treatment option for staghorn calculi.
Keywords
Introduction
Staghorn calculi are branched kidney stones that occupy all or part of the renal pelvis and branch into several or all of the calyces. 1 A newly diagnosed staghorn calculi represents a standard indication for active management.2,3 The American Urological Association and European Association of Urology guidelines recommend that staghorn calculi should be treated primarily with percutaneous nephrolithotomy (PCNL).1,4 Although the efficacy of PCNL is well-established, serious complications can occur, such as massive hemorrhage or injury to surrounding organs. 5
Retrograde intrarenal surgery (RIRS), which involves holmium:yttrium-aluminum-garnet (YAG) laser lithotripsy with flexible ureteroscopy, is an alternative to PCNL. Retrograde intrarenal surgery is superior to PCNL due to its lower morbidity rate and shorter admission time. 6 With advances in instruments, such as miniaturization of the flexible ureteroscope and improved visualization, the indications for RIRS have been expanding to larger renal stones while maintaining lower morbidity rates. 7 A recent meta-analysis comparing RIRS to PCNL for treatment of kidney stones recommends that RIRS should be considered as standard therapy for stones <2 cm in diameter. 5
Few studies have investigated the safety and efficacy of RIRS as the primary treatment for staghorn calculi. Mariani et al 7 demonstrated that staged ureteroscopic nephrolithotripsy is feasible with low morbidity and high stone clearance rates in 16 patients with 17 branched renal calculi. Only a small number of patients were included in the study, and electrohydraulic lithotripsy was used mainly for fragmentation of stones. Current urological guidelines indicate that holmium:YAG laser therapy is the gold standard modality for intracorporeal lithotripsy due to its high efficacy. 4
At our hospital, nearly all patients with large renal stones, including staghorn calculi, have been treated primarily with RIRS, and PCNL is performed only in patients with renal stones that cannot be accessed via retrograde ureteroscopy. We investigated the efficacy and safety of contemporary RIRS as a primary treatment for staghorn calculi.
Methods
A total of 68 patients with staghorn calculi were treated primarily with RIRS at International University of Health and Welfare Mita Hospital between April 2012 and March 2016. Among them, 14 patients who received ongoing stone treatment and 15 whose stones were not evaluated preoperatively by computed tomography (CT) were excluded from this study. We conducted a retrospective study for the remaining 39 patients to investigate the efficacy and safety of RIRS as a primary treatment for staghorn calculi. During the study period, no patients with staghorn calculi were treated primarily with PCNL and extracorporeal shock wave lithotripsy (SWL) at our hospital. This study was approved by the institutional review board of the International University of Health and Welfare Mita Hospital.
RIRS Technique
Patients were given intravenous antibiotics preoperatively according to their preoperative urine culture. Patients with a negative urine culture were given cephazolin, and those with a positive urine culture were given an appropriate antibiotic susceptible to bacteria isolated from the urine. Under general anesthesia, the patient was placed in the lithotomy position and prepared and draped in a sterile fashion. A lubricated 22-French rigid cystoscope (Olympus, Tokyo, Japan) was inserted transurethrally into the bladder to visualize the ureteral orifice. Then, a 0.038-in hydrophilic guidewire was advanced from the ureteral orifice into the renal pelvis under fluoroscopic guidance. A 6-French rigid ureteroscope (Richard Wolf GmbH, Knittlingen, Germany) was advanced over the guidewire to the proximal ureter, and retrograde ureteropyelography was performed. Through these procedures, we assessed ureteral compliance and passively dilated the entire ureter, as well as selected the appropriate ureteral access sheath size and length and determined the best position for the ureteral access sheath tip. 6 Next, the ureteral access sheath (12 of 14-French or 14 of 16-French, 35 or 45 cm; Cook Medical, Bloomington, IN, USA) was advanced over the guidewire under fluoroscopic guidance. We used a digital flexible ureteroscope (URF-V; Olympus) or a fiberoptic flexible ureteroscope (URF-P5 or URF-P6; Olympus), according to the ureteral access sheath size and the extent of ureteropelvic junction narrowing. Lithotripsy was performed using a reusable holmium:YAG laser fiber (SlimLine 200; Lumenis, Santa Clara, CA, USA). If ureteral access sheath insertion failed, a 6-French (Boston Scientific, Natick, MA, USA) or 7-French (Bard Medical, Covington, GA, USA) double-J stent was placed, and RIRS was postponed for approximately 1 month. The holmium:YAG laser was set at 0.5-1.0 J energy and firing a rate of 5-20 Hz. When stone fragment extraction was deemed necessary, a 1.5-French nitinol tipless basket (Cook Medical) was used. At the end of the procedure, retrograde ureteropyelography was performed again through the flexible ureteroscope, the ureteral access sheath was removed, and a 6- or 7-French double-J stent was placed under fluoroscopic guidance.
Preoperative and Postoperative Management
Preoperatively, all staghorn calculi were evaluated by CT and, if necessary, a kidney, ureter, and bladder X-ray (KUB) or intravenous pyelography (IVP) was performed. Initial postoperative stone assessment was based on intraoperative endoscopic findings and a KUB film taken on the first postoperative day. Patients with no fever or other severe symptoms were discharged from the hospital on the first postoperative day. At 3 to 4 weeks postoperatively, a KUB film was taken again. If a patient had residual stones in the upper or middle pole of the renal pelvis and had no primary ureteral stricture, RIRS was repeated. If a patient had only residual stones in the lower pole of the renal pelvis, whether or not treatment of the residual stones was decided by discussion between the patient and attending physician, RIRS or SWL was repeated, if necessary. If the residual stones were not treated by repeat RIRS, the double-J ureteral stent was removed at the outpatient clinic. Final stone status was assessed 3 months after the last RIRS session by KUB, IVP, or CT. A stone-free status was defined as complete clearance of the staghorn calculus with no fragments detectable by imaging.
The following preoperative clinical factors were assessed: age, sex, affected kidney (right or left), stone length, and involvement of the lower renal pole. Stone length was defined as the maximum diameter on an axial, sagittal, or coronal CT scan. Postoperative complications were evaluated according to the Clavien-Dindo classification. 8 Macroscopic hematuria and ureteral stent-related symptoms were always associated with RIRS or postprocedural ureteral stenting. Therefore, the complication rate was calculated after excluding macroscopic hematuria that did not require medical management and stent-related symptoms relieved by nonsteroidal anti-inflammatory drugs.
Statistical Analysis
Demographic and clinical characteristics were compared using the chi-square or Mann–Whitney U test as appropriate. Multivariate logistic regression models were used to assess the predictors of a stone-free status or postoperative complications after RIRS. Statistical analyses were performed using the SPSS Version 22.0 statistical software package (IBM, Armonk, NY, USA). All P values were 2-tailed, and P < .05 was considered significant.
Results
The mean ± standard deviation stone length was 60.5 ± 23.0 mm. A total of 134 procedures were performed in 39 patients (median 3 procedures; range: 1-11). Stone composition information was available in 92% (36 of 39) of all patients. Calcium oxalate (monohydrate or dehydrate) was found in 20 (51%) patients, struvite in 10 (26%), uric acid in 2 (5%), cysteine in 2 (5%), calcium phosphate in 1 (3%), and 2,8-dihydroxyadenine in 1 (3%).
The stone-free rates after the first, second, third, fourth, and final procedures were 21% (8 of 39), 31% (12 of 39), 36% (14 of 39), 46% (18 of 39), and 62% (24 of 39), respectively. Clinical characteristics of the subjects are summarized in Table 1. There were no significant differences in age (⩽60 vs >60 years), sex (male vs female), affected kidney (right vs left), stone length (<60 vs >60 mm), or lower renal pole involvement (yes vs no) between patients who became stone-free and those with residual stones. Univariate and multivariate analyses revealed that a stone length >60 mm was the only independent predictor of a stone-free status after the first (P = .03; hazard ratio [HR], 12.73; Table 2) and final (P = .03; HR, 6.59; Table 3) procedures.
Clinical and stone characteristics of the patients with staghorn calculi treated by RIRS.
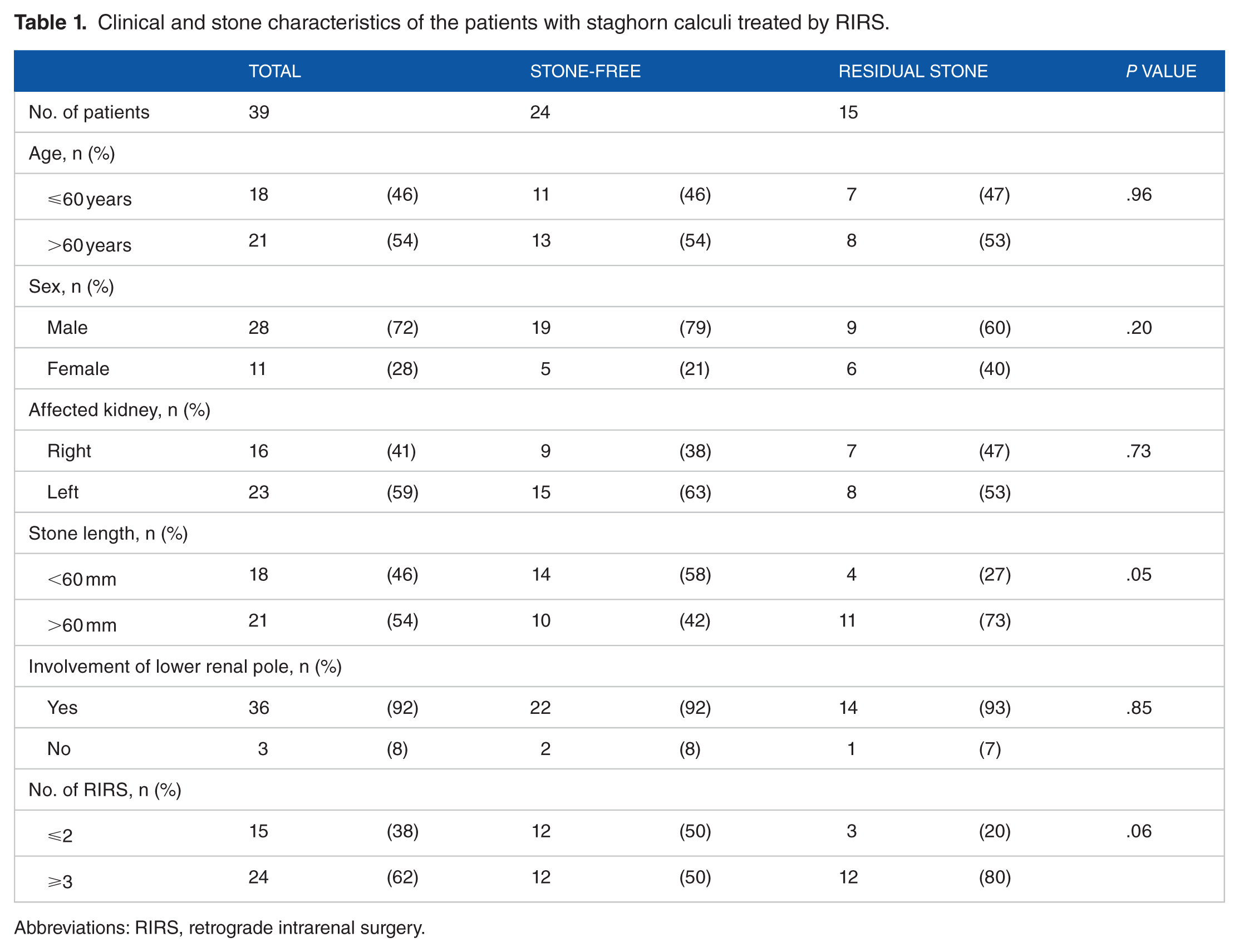
Abbreviations: RIRS, retrograde intrarenal surgery.
Univariate and multivariate logistic regression analyses of clinical and stone variables predicting a stone-free status after the first RIRS procedure.
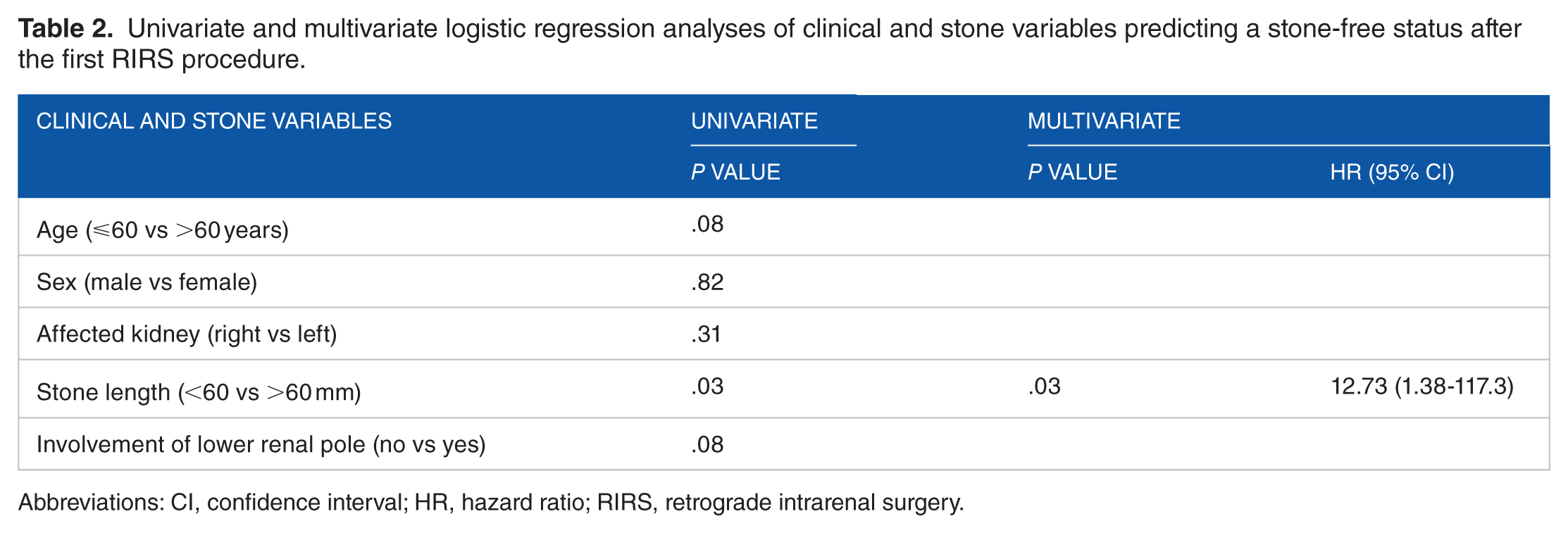
Abbreviations: CI, confidence interval; HR, hazard ratio; RIRS, retrograde intrarenal surgery.
Univariate and multivariate logistic regression analyses of clinical and stone variables predicting a stone-free status after the final RIRS procedure.
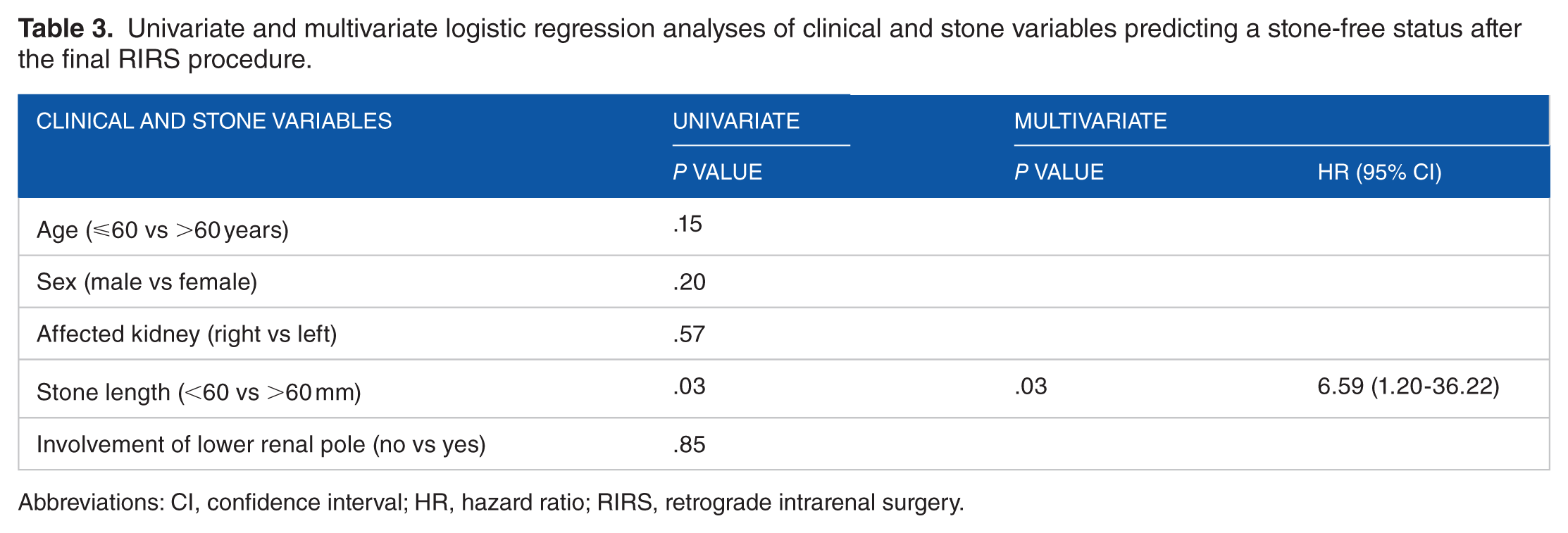
Abbreviations: CI, confidence interval; HR, hazard ratio; RIRS, retrograde intrarenal surgery.
Of the 39 patients, 18 (46%) and 21 (54%) presented with staghorn calculi <60 and >60 mm long, respectively. The median number of RIRS in these patients was 1 (range: 1-6) and 4 (range: 1-11), respectively (significant difference, P < .01). The median total operative time was also significantly longer in patients with staghorn calculi >60 mm (286 minutes; interquartile ratio [IQR]: 218-395) than those with calculi <60 mm (80 minutes; IQR: 48-195; P < .01). Stone-free rates stratified according to the number of RIRS procedures are shown in Table 4 and Figure 1. The stone-free rates after the first, second, third, fourth, and final procedures were 39% (7 of 11), 50% (9 of 18), 61% (11 of 18), 72% (13 of 18), and 78% (14 of 18), respectively, for patients with staghorn calculi <60 mm and 5% (1 of 21), 14% (3 of 21), 14% (3 of 21), 24% (5 of 21), and 48% (10 of 21), respectively, for those with calculi >60 mm. Of 15 patients with residual stones after the final RIRS, 2 had primary severe ureteral stenosis or ureteropelvic junction stricture that prevented a retrograde approach and required other treatment (PCNL or SWL). The remaining 13 patients presented with residual stones in the lower pole of the kidney or embedded in the renal parenchyma.
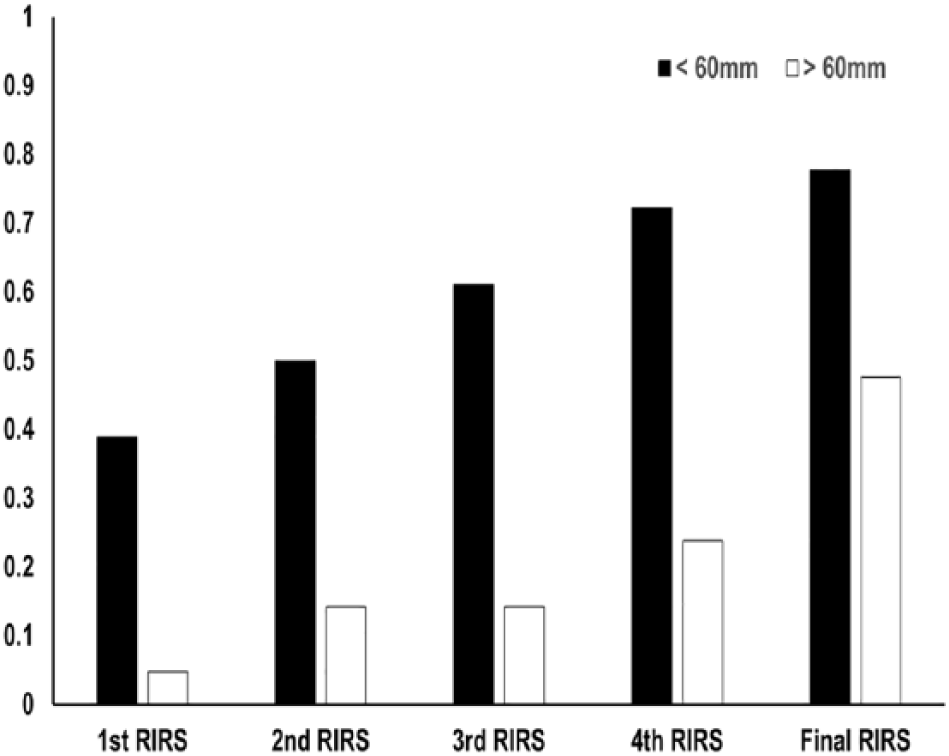
Stone-free rate stratified according to stone length and number of retrograde intrarenal surgical procedures. RIRS indicates retrograde intrarenal surgery.
Stone-free rates stratified according to stone length and the number of RIRS procedures.
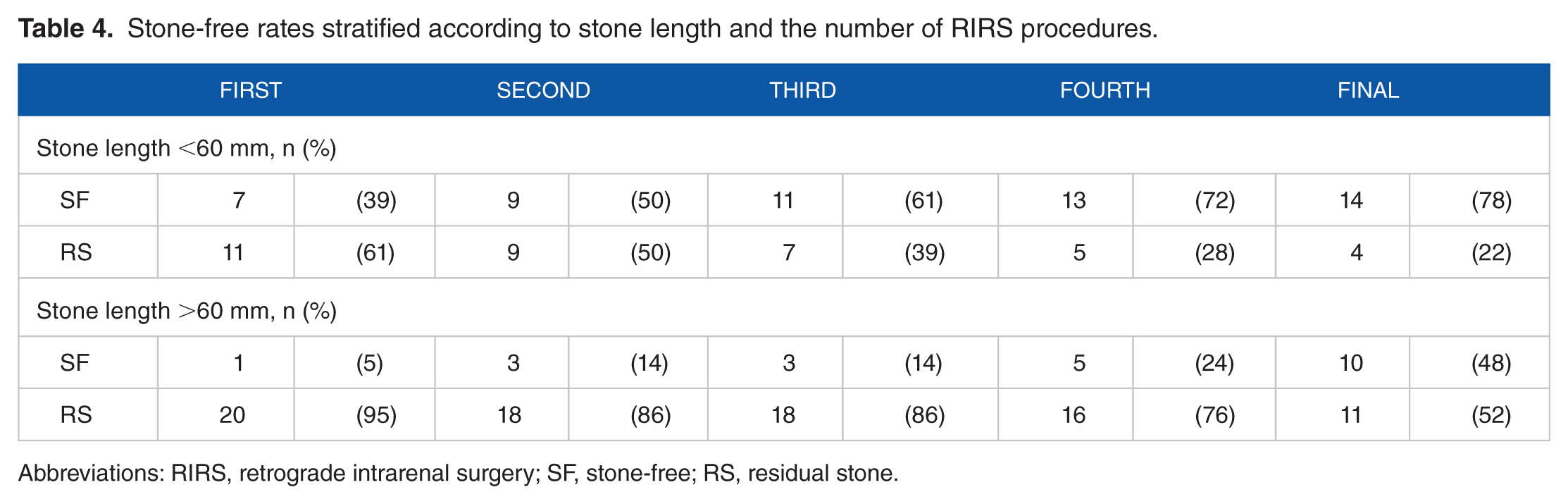
Abbreviations: RIRS, retrograde intrarenal surgery; SF, stone-free; RS, residual stone.
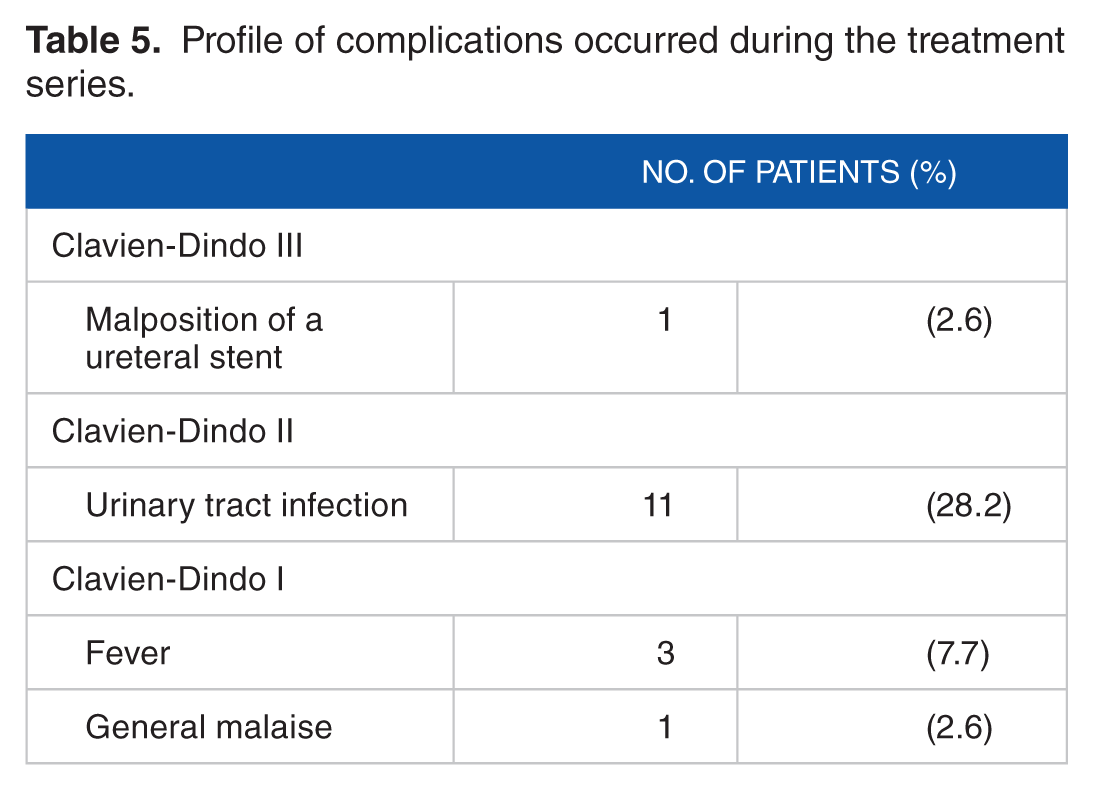
During the treatment series, complications occurred in 16 (41%) patients, with Clavien-Dindo grades I, II, and III occurring in 4, 11, and 1, respectively (Table 5). All 11 Clavien-Dindo grade II complications were urinary tract infections (UTIs). The incidence of UTI was significantly higher in patients with struvite (70%, 7 of 10) than in those with other (15%, 4 of 26, P < .01) stones. The grade III complication was malposition of a ureteral stent that required endoscopic ureteral stent exchange on postoperative day 1.
Profile of complications occurred during the treatment series.
Discussion
Recently, the indications for RIRS have been expanding, and RIRS has been used increasingly as a primary treatment for patients with larger renal stones.9–13 However, few studies have evaluated clinical outcomes of RIRS as a primary treatment for staghorn calculi. Mariani et al 7 previously evaluated the clinical outcomes of staged ureteroscopic nephrolithotripsy for patients with branched renal calculi. In the study, lithotripsy using the holmium:YAG laser, which has been the gold standard lithotrite for contemporary RIRS, 4 was performed in only 4 patients. To the best of our knowledge, this is the first study to evaluate the clinical efficacy and safety of contemporary RIRS using the holmium:YAG laser as a primary treatment for staghorn calculi. We demonstrated that approximately 40% of patients with staghorn calculi <60 mm became stone free after one RIRS procedure, and approximately 60% became stone free within 3 procedures. However, only one-fourth of patients with staghorn calculi >60 mm became stone free within 4 procedures, although approximately 50% eventually became stone free at last. During the treatment series, 40% of patients presented with a complication; however, most complications were minor and only one patient presented with a severe complication (malposition of a ureteral stent, Clavien-Dindo grade III).
The overall stone-free rates after the first and final RIRS procedures were 21% and 62%, respectively. Previous studies reported that the stone-free rates for patients with staghorn calculi after the first and final PCNL procedures were 54%-77% and 70%-86%, respectively.14–17 Comparing the results of these studies with our results, RIRS seems to be inferior to PCNL in terms of complete stone clearance. Teichman et al 18 conducted a retrospective study of 177 patients with staghorn calculus treated with PCNL and suggested that asymptomatic patients who presented with residual stones after PCNL without urinary tract obstruction or infection are less likely to seek additional treatment. In our study, excluding 2 patients whose stones could not be managed via a retrograde approach, all remaining residual stones were asymptomatic. Our results suggested that RIRS is clinically useful to prevent renal function deterioration or UTI complicated by staghorn calculi.
The most important advantage of RIRS over PCNL is its lower morbidity. Armitage et al 19 investigated the postoperative outcomes of PCNL at English National Health Service hospitals, and they revealed 0.2% (13 of 5750) in-hospital deaths within 30 days after PCNL. Ghani et al 20 investigated recent trends in the perioperative outcomes of PCNL in the United States in a nationwide inpatient sample, and they reported that the mortality rate of PCNL remains 0.0% to 0.4%. However, to date, only a few cases of death after RIRS have been reported in the English literature.21,22 Cindolo et al 21 conducted a survey asking 11 skilled endourologists to review their RIRS series and reported a total of 6 deaths after RIRS: one patient died of a hemorrhagic complication associated with additional nephrostomy during RIRS, one died of a fulminant untreatable cardiac arrest at induction of general anesthesia, and only true fatal complications associated with RIRS occurred in the remaining 4. As cases of mortality after RIRS are underreported, we can estimate that fatal complications associated with RIRS are much less frequent than those with PCNL. Of course, there was no life-threatening complication in this study. Other severe complications are specific to PCNL, such as injury to adjacent organs or severe bleeding associated with renal puncture. 23 The overall complication rate of PCNL for staghorn calculi was reported to be 24%-43%.14,16,17,24 A blood transfusion was given in >10% of patients during the perioperative period.17,24 In our study, no patient required blood transfusion. The results of previous studies and our study suggest that the morbidity associated with repeated RIRS for staghorn calculi is much lower than that for PCNL.
There were 2 interesting findings of our study. First, the overall stone-free rate was higher in patients with staghorn calculi of <60 mm than in those with calculi >60 mm (78% vs 48%, P = .05). A previous meta-analysis suggested that RIRS should be considered as the standard of care for the treatment of renal stones <20 mm. 5 In addition, a prospective randomized study to compare the safety and efficacy of RIRS and PCNL for patients with renal stones >20 mm demonstrated that RIRS was less effective than PCNL but caused less morbidity. 16 Emphasizing the favorable morbidity after RIRS, the investigators proposed that RIRS be considered as an alternative treatment option for larger stones. Other studies have suggested that RIRS achieves acceptable clinical efficacy with lower morbidity than PCNL when treating renal stones with a diameter >20 mm, 17 >25 mm, 9 15 to 30 mm, 18 or 20 to 35 mm. 20 Our results supported these previous studies and expansion of the indication for RIRS for larger renal stones.
Second, our study also suggested that repeated RIRS may be safe and tolerable for patients with staghorn calculi. While 40% of our patients presented with a complication during the treatment series, no complications were associated with repeated RIRS, such as ureteral or urethral stricture. Delvecchio reported that only 1 of 71 patients who received ureteroscopic procedures using a ureteral access sheath suffered a ureteral stricture. 25 Komori reported that increased surgeon experience can decrease the risk of severe complications of flexible ureteroscopic lithotripsy. 26 Our hospital is a high-volume center for flexible ureteroscopic lithotripsy including RIRS, with >200 cases per year. The low complication rate, including no case of postoperative ureteral stricture, may partly depend on our experience.
This study had several limitations, including potential selection bias due to its retrospective nature and the small number of patients assessed. However, no patient with staghorn calculi received primarily PCNL or SWL at our hospital during the study period, suggesting that selection bias may be minimal. Another limitation is that the stone-free status of patients was determined from KUB films, which is an inferior method to unenhanced CT in detecting urinary tract stones. However, KUB films are obtained more frequently for postoperative imaging than CT scans in routine clinical practice, 24 suggesting that our retrospective study reflects the real-world setting.
In conclusion, to our knowledge, this is the first study to evaluate efficacy and safety of contemporary RIRS using the holmium:YAG laser as a primary treatment for staghorn calculi. We demonstrated that RIRS is safe and effective for patients with staghorn calculi, particularly those with comparatively small stones. Retrograde intrarenal surgery could be an alternative to PCNL for selected patients with staghorn calculi.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
NN, KM, and TA designed the study. NN, AK, and MK performed the acquisition, analysis, and interpretation of data. NN and KM wrote the original manuscript. NN, KM, TO, HB, and TA reviewed and commented on the manuscript.
