Abstract
Recently, the development of antiangiogenic drugs has changed the therapy for metastatic renal cell carcinoma (RCC). As a result, the survival of individuals with advanced RCC has more than doubled. The median overall survival improved from 12 months during the cytokines era to near 30 months with antiangiogenic drugs. In this decade, the advent of immune checkpoint inhibitors showed enthusiastic results and is the new standard of care for patients with metastatic RCC previously treated with antiangiogenic drugs. The combination of immune checkpoint inhibitors plus antiangiogenic drugs may have a synergistic activity. As a result, current studies investigate the combination for treatment-naïve patients. This may potentially change clinical practice. In this article, we will highlight new therapeutic options available and agents or combinations that are being investigated for metastatic RCC.
Background
Renal cell carcinoma (RCC) is the most common primary renal malignancy. Renal cell carcinoma accounts for 4 of 5 of all kidney tumors and 2% to 3% of all types of cancer in adults. 1 In the United States, 63 990 new cases and 14 400 deaths may occur in 2017. 2
One out of every 5 cases is diagnosed in the advanced stage; in addition, there is a high risk of recurrence after nephrectomy. 1 Classically, the standard of care for advanced disease was cytokines with low response rates and significant toxicity.3,4
The clarification of carcinogenesis’ mechanisms in RCC led to the identification of some targets for therapeutic intervention, which started the era of molecularly targeted therapy in kidney cancer. One of the most studied targets is the vascular endothelial growth factor (VEGF) pathway that is related to tumor angiogenesis and growth. 1 Several VEGF inhibitors were developed since then (sorafenib, pazopanib, bevacizumab, and axitinib), with overall survival (OS) improvement for patients previously untreated or cytokine pretreated when compared with interferon or placebo in many pivotal trials.4–6
Other important mechanism involved in pathogenesis of RCCs is the mechanistic target of rapamycin (mTOR) pathway. 1 Temsirolimus and everolimus were developed and approved for RCC treatment.7,8 New tyrosine kinase inhibitors (TKIs) are under development for later lines or for patients with known mutations in the downstream of mTOR pathway.
In the past 2 years, new options for treatment of RCC received approbation in the US by Food and Drug Administration (FDA), including multitargeted TKIs (cabozantinib and levatininib), and immune checkpoint inhibitors (nivolumab).
This development was a paradigm shift for the advanced RCC treatment and the survival of patients has more than doubled. The median OS more than doubled (from 12 months with cytokines to more than 26 months with antiangiogenic drug). 6
We will review below recent findings and future directions for the treatment of advanced RCC.
RCC-Targeted Therapy Evidence
Sunitinib
Sunitinib is a multikinase inhibitor that inhibits both the VEGF receptor (VEGFR) and the platelet-derived growth factor receptor (PDGFR). A randomized clinical trial enrolled 750 treatment-naïve patients with RCC to sunitinib or interferon alfa. 5 The overall response rate (ORR) was higher with sunitinib compared with interferon alfa (47% versus 12%), as well as progression-free survival (PFS) (median: 11 months versus 5 months), and OS (median: 26.4 months versus 21.8 months). Sunitinib had also a better toxicity profile and became the standard of care for treatment-naïve patients with RCC.
Pazopanib
Pazopanib targets VEGFR, PDGFR, and c-Kit. A randomized clinical trial compared pazopanib with placebo. 9 This study enrolled 435 patients with RCC previously untreated or after failed on cytokine. In the overall population, PFS improved (9.2 months with pazopanib versus 4.2 months with placebo) and the benefit was greater among previously untreated patients (11.1 months versus 2.8 months, respectively).
A phase 3 study enrolled 1100 untreated patients with metastatic RCC to receive sunitinib or pazopanib. 6 Both agents showed similar efficacy in terms of PFS and OS, although pazopanib might be better tolerated than sunitinib.
Sorafenib
Sorafenib is also a multikinase inhibitor approved for the second-line treatment of advanced RCC. A phase 3 trial compared sorafenib with placebo for previously treated patients which showed an improvement of the median PFS (5.5 months versus 2.8 months), although there was not any improvement in OS compared with placebo. 10 Sorafenib was compared with interferon alfa for previously untreated patients in a phase 2 trial; nevertheless, this study was negative. 11
Cabozantinib
The rationale for cabozantinib development is to target multiple tyrosine kinase receptors to overcome resistance to classical VEGFR inhibitors. Cabozantinib targets MET, VEGFR, and AXL. METEOR is a phase 3 study that compared cabozantinib with everolimus for RCC second-line therapy. 12 The study included 658 patients and demonstrated cabozantinib superiority. The reduction in the risk of progression was 42% (PFS: median: 7.4 months versus 3.8 months). Cabozantinib also improved ORR (21% versus 5%) and OS (median: 21.4 months versus 16.5 months). 13 Recently, a phase 2 trial (CABOSUN) compared cabozantinib with sunitinib for previously untreated patients and showed an improvement in PFS (8.2 months versus 5.6 months) and ORR (46% versus 18%). 14 Overall survival was not the end point of the study and was immature when the study was published.
Axitinib
Axitinib is a second-generation antiangiogenic drug that was studied for patients with RCC who had disease progression on first-generation TKIs. 15 AXIS study enrolled 723 patients to axitinib or sorafenib. The median PFS was 6.7 months with axitinib compared with 4.7 months with sorafenib. No differences were observed in terms of OS and patient-reported outcomes. After AXIS trial, another study compared axitinib with sorafenib for treatment-naïve patients with RCC and failed to show any improvement in terms of PFS, which was the primary end point. 16
Lenvatinib
Lenvatinib is a multitargeted TKI (VEGFR, RET, and fibroblast growth factor receptor kinases 1 to 4) tested in combination with everolimus for the second-line therapy in an international phase 2 trial. 17 A total of 153 patients were randomized in a 1:1:1 ratio to lenvatinib, everolimus, or lenvatinib plus everolimus. The combination improved PFS compared with everolimus alone. Even though, there are no randomized trials comparing lenvatinib plus everolimus innovative drugs, such as nivolumab, cabozantinib, and axitinib.
Table 1 summarizes clinical data of most relevant drugs for advanced RCC treatment.
Summary of all recommended treatments for advanced renal cell carcinoma.
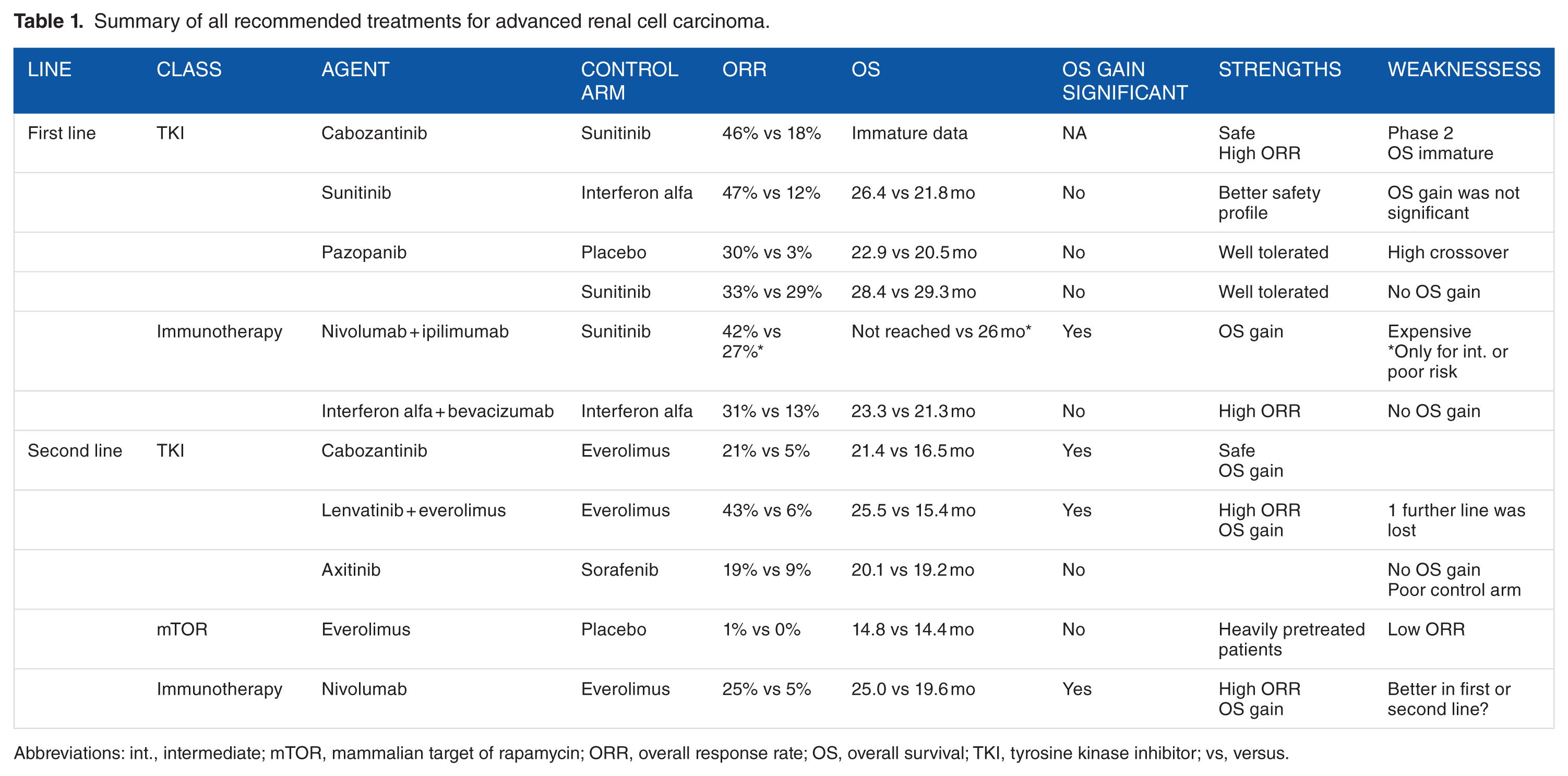
Abbreviations: int., intermediate; mTOR, mammalian target of rapamycin; ORR, overall response rate; OS, overall survival; TKI, tyrosine kinase inhibitor; vs, versus.
mTOR Inhibitors
Temsirolimus
Temsirolimus was the first mTOR inhibitor studied for the treatment of advanced RCC. In a multicenter phase 3 trial, 626 untreated patients classified as poor prognosis were randomly assigned to temsirolimus alone or interferon alfa alone or combination therapy. 7 The mTOR inhibition improved OS compared with interferon alone, although there were no benefits observed for this combination. 7
Everolimus
Everolimus is another mTOR inhibitor that improved PFS in a randomized phase 3 trial compared with placebo after failure of sunitinib or sorafenib. 8 Recent studies demonstrated that everolimus is inferior to innovative drugs, such as lenvatinib plus everolimus, cabozantinib, and nivolumab.13,17,18 Nevertheless, everolimus is still an option when cabozantinib, nivolumab, or lenvatinib is not available. 19
Table 1 summarizes clinical data of most relevant drugs for advanced RCC treatment.
Targeted Therapy Combos
As cited above, the combination of everolimus with lenvatinib had favorable results for the second-line setting compared with everolimus monotherapy. 17
Bevacizumab is a monoclonal antibody against circulating VEGF that was combined with temsirolimus or sorafenib or both in a phase 3 study (BEST trial). 20 The combination did not improve PFS compared with bevacizumab monotherapy and was associated with a worse profile of toxicity when compared with monotherapy.
RCC Immunotherapy Evidence
Background of RCC immunotherapy
The rationale for RCC started with the observation of spontaneous remissions in metastasis after kidney removal. 21 In addition, 2 classic immunotherapy agents showed activity for RCC treatment. High-dose interleukin 2 (IL-2) achieved durable tumor response in a small proportion of patients and is indicated only for patients with good performance status who have access to a facility able to manage the harmful toxicity associated with IL-2 high dose. 22 Then, several large trials showed the activity of interferon alfa in metastatic RCC as monotherapy or in combination with IL-2 and bevacizumab.3,4 Although interferon alfa had less adverse events (AEs) than IL-2, a small proportion of patients responded to both of them. 3
During the 2000s, the knowledge of cancer immune tolerance improved and this may have led to the development of the modern immunotherapy. 23 Programmed cell death protein 1 (PD-1) is the immune checkpoint most implicated in clinical practice. 24 Activated T cells and B cells express PD-1, and PD-1 binds to 2 ligands, PD-L1 and PD-L2. The interaction between PD-1 and its ligands inhibits the lymphocytes and is used by tumor cells to avoid the immune system. 24 A high expression of PD-L1 was seen in one-third of RCC tumors and was related to advanced tumor stage, higher Fuhrman grade, sarcomatoid differentiation, and in turn poorer survival. 25
Nivolumab
Nivolumab is fully human IgG4 monoclonal antibody that binds PD-1 and stimulates T lymphocytes against cancer cells. CheckMate 025 was a phase 3 trial that randomized 821 previously treated patients to receive nivolumab 3 mg/kg every 2 weeks or everolimus 10 mg/d. 18 The risk of death was 27% lower with nivolumab compared with everolimus and the median OS improved from 19.6 to 25.0 months. The OS benefit occurred among all risk groups and irrespective of the number of prior antiangiogenic therapies. PD-L1 expression was not a predictor factor of nivolumab effectiveness.
Nivolumab also improved the ORR compared with everolimus (25% versus 5%; odds ratio: 5.98, 95% confidence interval [CI]: 3.68-9.72). As previously seen in other neoplasms, nivolumab did not improve PFS compared with everolimus (median: 4.6 months versus 4.4 months; hazard ratio [HR]: 0.88, 95% CI: 0.75-1.03).
Fatigue occurred in one-third of patients treated with nivolumab. Other common AEs were nausea (14%) and pruritus (14%). All AEs were manageable. Severe AEs (grade 3 or 4) were less common with nivolumab compared with everolimus (19% versus 37%). Nivolumab also improved quality of life compared with everolimus (P < .05). 18
The FDA approved nivolumab for RCC second-line treatment in November 2015. European Medicines Agency (EMA) approved nivolumab in February 2016.
Other immune checkpoint inhibitors
Atezolizumab is a humanized anti-PDL1 antibody that acts in the same pathway PD-1/PD-L1 as nivolumab. A phase 1 study included 70 previously treated patients and showed enthusiastic results. 26 The ORR was 15%. The median PFS was near 6 months (95% CI: 3.9 to 8.2 months), and the median OS was 28.9 months (95% CI: 20.0 months to not reached [NR]). The most common AE was grade I rash (20%). These results led to the development of robust ongoing studies with atezolizumab for advanced RCC presented in the next section.
The cytotoxic T lymphocyte–associated protein 4 (CTLA-4) is another checkpoint largely studied. The antigen-presenting cell (APC) recognizes pathogens and tumors as non-self and stimulates lymphocytes against pathogens and tumors antigens by the binding of APC’s surface proteins B7.1 and B7.2 to lymphocytes’ CD28. When activated, the lymphocytes express CTLA-4 that binds B7.1 and B7.2 to inhibit the lymphocyte.
Ipilimumab and tremelimumab are monoclonal antibodies against CTLA-4. A phase 2 trial studied the activity of ipilimumab and included 61 patients with metastatic RCC. 27 Ipilimumab was given in a dose escalation ranging from 1 to 3 mg/kg every 3 weeks. Several autoimmune-mediated AEs occurred, the most common was enterocolitis (18%) followed by hypophysitis (7%) and dermatitis (4%). Interestingly, AEs were predictors of efficacy. Interestingly, ORR was higher among patients who developed immune-mediated AEs compared with patients who did not (30% versus 0%; P = .0007).
A phase 1 trial assessed tremelimumab in combination with sunitinib regardless of previous treatments for metastatic RCC. 28 The authors enrolled 28 patients. The ORR was 43% among evaluable patients (n = 21); however, the toxicity related to the treatment was unexpectedly high and severe. One patient had a sudden death related to the treatment, and up to 50% had to stop the treatment because of dose-limiting toxicity.
Current Sequential Therapies for Metastatic RCC
The improvement in OS observed with these 3 new second-line treatment options (nivolumab, cabozantinib, lenvatinib plus everolimus) changed the landscape of advanced RCC. 19 Axitinib and everolimus are also options for second-line therapy. 19 Figure 1 summarizes current options recommended by European Society of Medical Oncology (ESMO) guideline for metastatic RCC. 19 Table 1 summarizes clinical data of most relevant drugs for advanced RCC treatment.
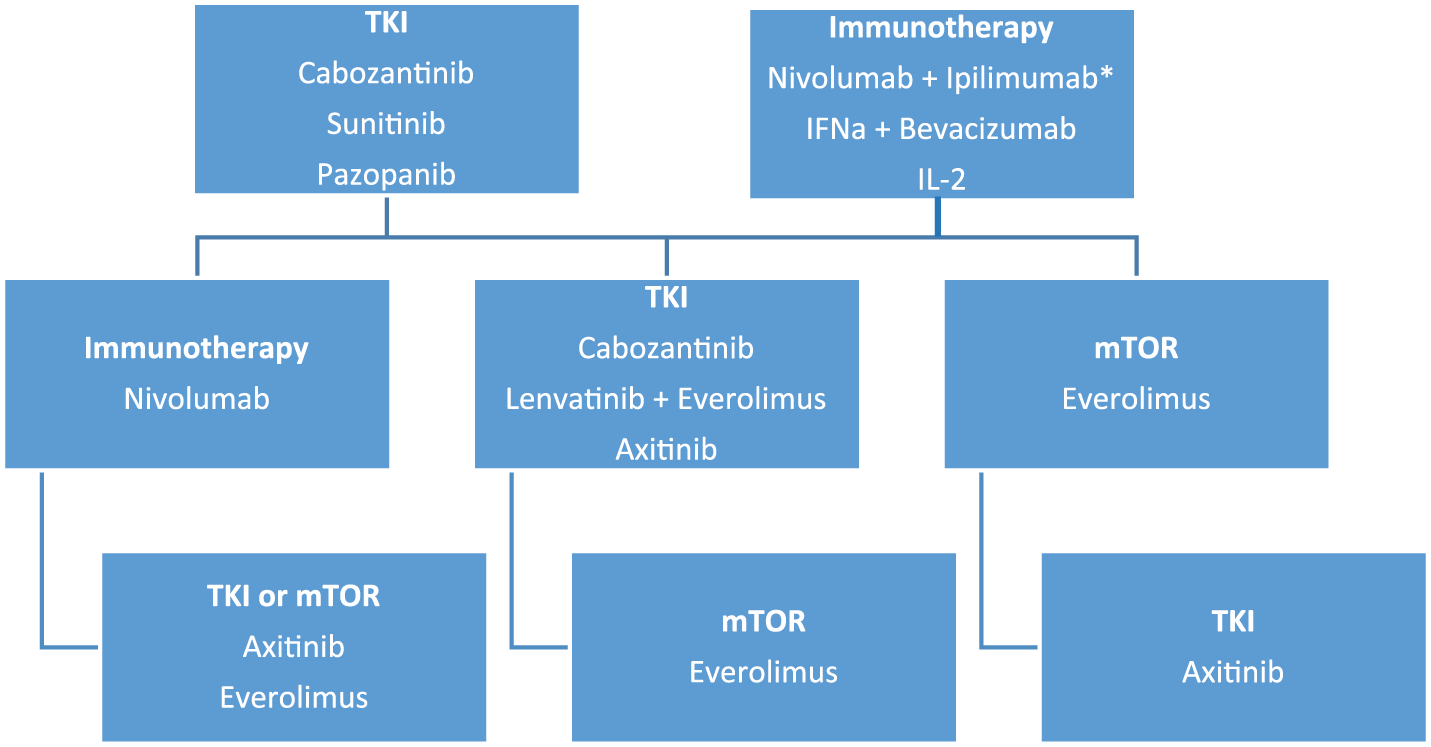
European Society of Medical Oncology (ESMO) guideline for advanced renal cell carcinoma.
RCC Immunotherapy Future Perspectives
Immune checkpoint inhibitors plus VEGF inhibitors
Nivolumab showed enthusiastic results as cited above; nevertheless, most patients’ disease was still progressive. 18 The complete response rate was only 1%, and only one-third of patients had a durable response. 18 Several studies assessing drugs combinations are ongoing to improve patients’ outcomes. Scientists hypothesized that VEGF pathway inhibition enhances immune responses 29 by increasing infiltration of T cells into tumor,30,31 inhibiting anti-inflammatory cytokines and Treg lymphocytes. 32 Table 2 summarizes the ORR among recent trials for previously untreated patients.
Overall response rate for immunotherapy plus TKI combos under investigation.

Abbreviations: TKI, tyrosine kinase inhibitor; VEGF, vascular endothelial growth factor.
Nivolumab plus sunitinib or pazopanib
A phase 1 study assessed the combination of nivolumab plus sunitinib or pazopanib for previously treated patients with RCC. 33
Most of the patients (80%) had any AE, although the most common grade 3 or 4 AEs were seen in 20% of the patients (elevated transaminases and diarrhea in the pazopanib arm and hypertension in the sunitinib arm). In the sunitinib arm, the ORR was 52%. In the pazopanib arm, the ORR was 45%.
Consequently, recent studies changed the combination of immune checkpoint inhibitors with bevacizumab or axitinib instead of sunitinib or pazopanib to improve safety.
Atezolizumab plus bevacizumab
A total of 305 previously untreated patients with RCC were randomized to 1 of 3 arms, atezolizumab alone, atezolizumab plus bevacizumab, or sunitinib. After progression, patients were allowed to crossover from the single-agent arms to the combination of atezolizumab plus bevacizumab. 34
After a median follow-up of 20.7 months, preliminary results were presented at 2017 ASCO (American Society of Clinical Oncology) Annual Meeting. 34 The ORR for atezolizumab plus bevacizumab, atezolizumab alone, and sunitinib was 32%, 25%, and 29%, respectively. PD-L1 expression ≥1% improved the response only in the combination arm (ORR: 46%). Neither atezolizumab nor the combination improved the PFS compared with sunitinib. The OS data are immature. As expected, the combination had a favorable safety profile compared with sunitinib. A phase 3 study (IMmotion 151) compared atezolizumab plus bevacizumab versus sunitinib for previously untreated patients. The results of IMmotion 151 was presented at the 2018 Genitourinary Cancers Symposium and showed that atezolizumab plus bevacizumab improved outcomes compared to sunitinib. The ORR was 37% versus 33% and the median PFS was 11,2 months versus 8,4 months (HR 0.83 [95% CI: 0.70, 0.97]). Overall survival data was immature as both arms have not reached the median OS (NCT02420821).
Pembrolizumab plus axitinib
In a phase 1 study with an expansion cohort, 52 previously untreated patients received the combination of pembrolizumab, an anti-PD1 antibody, and axitinib. 35
The authors presented at the 2016 ESMO Annual Meeting an impressive ORR of 71%, including 3 complete and 34 partial responses. Survival data were immature; nevertheless, it was at a minimum median PFS of 15.1 months. The combination was well tolerated and only a small proportion (3.8%) experienced severe immune-related AEs.
An ongoing phase 3 trial will compare this combination with sunitinib (NCT02853331, KEYNOTE-426).
Avelumab plus axitinib
Avelumab is an anti-PDL1 monoclonal antibody evaluated in a phase 1 study that included 55 patients previously untreated with favorable or intermediate-risk advanced RCC. Initial results were presented at the 2017 ASCO Annual Meeting. 36
The ORR was 58%, including 3 complete responses and 29 partial responses. The median PFS was 6.7 months. The combination was safe, and the most common immune-related toxicity was hypothyroidism manifested in 21.8% of the patients. The combination of avelumab plus axitinib is being compared with sunitinib in a phase 3 trial (NCT02684006).
Immune checkpoint inhibitors’ combos
After limited activity and severe AEs of CTLA-4 inhibitors’ monotherapy, they are now under investigation in combination with PD-1 or PD-L1 inhibitors based on the enthusiastic results achieved in malignant melanoma. 37
Nivolumab plus ipilimumab
This combination was first assessed in a dose-escalation phase 1 study. 38 The ORR was 40% and the 24-week PFS rate was 65%. The 2-year OS rate was nearly 70% for both arms. A phase 3 trial (CheckMate 214) presented at 2017 ESMO Annual Meeting compared nivolumab plus ipilimumab versus sunitinib for previously untreated RCC. 39 CheckMate 214 enrolled 1096 patients of whom 847 had intermediate- or poor-risk disease. The ORR in the intention-to-treat population was 39% for immunotherapy combo and 32% for sunitinib. Among patients with intermediate- or poor-risk disease, the ORR was 42% versus 27%, respectively. Interestingly, among favorable risk patients, the ORR was 29% and 52%, respectively. Nivolumab plus ipilimumab improved OS significantly compared with sunitinib among intermediate- or poor-risk patients (median OS: NR versus 26 months; HR: 0.63, 95% CI: 0.44-0.89). 39 These results were impressive as it was the first study that showed an OS gain compared with sunitinib.
Vaccines
As immunotherapy showed enthusiastic results in the treatment of RCC, different agents are being tested to find the most effective treatment. In this context, vaccines should also be considered when studying combination immunotherapies.
Novel approaches to reengage immune recognition of tumor through autologous cellular immunotherapy are under active development in patients with advanced RCC.
A phase 2 study assessed that AGS-003, an autologous immunotherapy prepared from dendritic cells, has been studied in combination with sunitinib for previously untreated patients with RCC with intermediate- and poor-risk disease. 40 A total of 21 patients were included in the study and assessed for tumor response after 5 doses of AGS-003. Most of the patients (62%) experienced clinical benefit, although there were no complete responses. As a result, the enrollment terminated early. The median PFS was 11.2 months and the median OS was 30.2 months. The survival rate at 4.5 years was 33%. The most common AEs were mild injection site reactions. Other AEs were related to sunitinib. There were a correlation between T cells circulating in plasma and OS.
The phase 3 ADAPT study (NCT01582672) is ongoing but not recruiting participants. Patients with metastatic RCC after nephrectomy were randomized to sunitinib or sunitinib plus AGS-003. Both arms received standard sunitinib at standard dose; patients in the sunitinib plus AGS-003 arm received 8 intradermal injections in the first year followed by boosters every 3 months. Accrual completed in 2015 and the primary end point is OS.
Another example is the cancer vaccine IMA901 based on tumor-associated peptides which was administered as first-line therapy to patients with metastatic RCC who were HLA-A02 positive. This was given as an intradermal vaccination for up to 10 doses, each in conjunction with 75 µg of granulocyte macrophage colony-stimulating factor (GM-CSF).
A phase 3 study (IMPRINT) randomized 339 treatment-naïve patients to sunitinib alone or sunitinib plus IMA901 and GM-CSF. 41 The study fails to improve OS, its primary end point (HR: 1.34, 95% CI: 0.96-1.86, P = .08).
Conclusions
In conclusion, several new agents have been proven to be efficient for RCC and became new treatment options. Even though, new studies are needed to improve new agents’ efficacy through treatment combinations and to find the best treatment sequencing after all this development.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: P.A. Jr received honoraria from BMS, AstraZeneca, and Novartis and speaker funding from MSD and Roche/Genentech. T.C.d.P., C.M.N.B., and A.d.G. do not have any conflicts to disclosure.
Author Contributions
PAJ wrote the text and developed the review. TCP reviewed targeted-therapy and wrote the text. CMNB reviewed immunotherapy and wrote the text. AG developed the review and made final edits in the text.
