Abstract
Numerous studies have been conducted in the past few decades on obstructive sleep apnea (OSA) as an independent risk factor for the development and progression of cardiac arrhythmia. Treatment with continuous positive airway pressure (CPAP) therapy lowers blood pressure, improves ejection fraction in patients with heart failure, and decreases the need of revascularization procedures in patients with coronary artery disease. However, there has been little published discussion regarding the effect of CPAP treatment on cardiac arrhythmia in patients with OSA. We aimed to summarize scientific evidence regarding the utility of CPAP treatment in managing the recurrence and severity of different types of cardiac arrhythmia. We retrieved articles published in English before December 2016, through database search of PubMed, CENTRAL, and Embase. All peer-reviewed experimental, comparative, and other observational studies focused on adults were considered eligible. Several studies documented positive changes in arrhythmia frequency and severity with CPAP application, irrespective of type of arrhythmia, study methodology, or setting. However, the available evidence on the impact of CPAP treatment on the frequency and severity of cardiac arrhythmia is limited by heterogeneity of data. The duration of CPAP application, compliance with treatment, and baseline severity of OSA and cardiac pathology are important confounding factors that influence the effect of CPAP treatment. We emphasize the need for agreement on a core set of relevant predictors of the magnitude of the effect. Future research should carefully address these factors and their influence on the potential therapeutic ability of CPAP treatment to improve cardiac outcomes and reduce the risks of adverse cardiac and noncardiac effects associated with untreated OSA.
Keywords
Introduction
Obstructive sleep apnea (OSA) is characterized by recurrent obstruction of the upper airways during sleep which causes cessation of breathing despite continuous respiratory drive. 1 Obstructive sleep apnea is prevalent in 9% of middle-aged women and 25% of middle-aged men, 2 and associated with substantial human and economic costs.3,4 Obstructive sleep apnea has been recognized as an independent risk factor for hypertension, 5 heart failure, 6 cardiac arrhythmia, 7 coronary artery disease, 8 stroke, 9 sudden cardiac death, 10 and mortality in general and from cardiac causes specifically.11,12 Recently, OSA has been highlighted as a risk factor for increased complications postcardiac surgery. 13
Furthermore, several studies found that OSA increases susceptibility of individuals to potentially life-threatening atrial and ventricular arrhythmia.7,14 Obstructive sleep apnea has been found to increase the odds of arrhythmias occurrence 18-fold over normal breathing. 15 The mechanism for such adverse effects is not entirely clear; however, it has been proposed that OSA creates an imbalance between sympathetic and vagal activity during sleep which plays a major role in generating or exacerbating cardiac rhythm disturbance. 16 Obstructive events also bring on hypoxia17,18 which, in the presence of obstruction, induces a reflex bradycardia and elevates blood pressure. 19 In addition, hypoxia is associated with increased oxidative stress and generation of reactive oxygen species, 20 which result in cellular injury, ischemia, and abnormal excitability of the myocardium. 21 These changes in turn may induce atrial and ventricular arrhythmia. 21 Moreover, increased negative intrathoracic pressure causes acute stretch of myocardial wall and intrathoracic vessels evident by proximal aortic dilation and increased left ventricular volumes. 17 These structural changes along with an increase in transmural gradients may create an arrhythmogenic milieu that triggers atrial and ventricular arrhythmia.18,22 Finally, nocturnal obstructive events are frequently terminated by arousals that are accompanied by a surge of the sympathetic nervous system activity, which results in considerable rise in blood pressure 23 and heart rate 24 as well as coronary vasoconstriction and micro-ischemia. 17 Consequently, sympathetic hyperstimulation can induce various tachyarrhythmia and myocardial repolarization disturbances.17,18
Several approaches to the treatment of OSA have been promoted based on our current understanding of the mechanism underlying the disorder. Although milder cases of OSA can be managed by weight reduction, avoidance of muscle relaxants, improvement of nasal patency, oral appliances, and avoidance of sleeping in a supine position, 25 in more severe cases continuous positive airway pressure (CPAP), a treatment that delivers positive pressure through a mask to maintain the opening of the upper airways during sleep, are recommended. 26 Earlier research has shown that despite the efficacy of CPAP treatment in OSA, clinicians and researchers face significant problems with its adherence and compliance in patients. 27 The main reasons for poor adherence to CPAP treatment are suggested to be skin irritation due to mask application and difficulty dealing with the equipment. 28 However, understanding all facets of application of CPAP treatment including that of the physician, the health care system, and the CPAP distributors suggests that advocating for its continuous use is desirable. Similarly, categorizing the benefits of CPAP treatment in the context of several types of cardiac arrhythmia might help in developing clinical guidelines so that patients with cardiac arrhythmia will be screened for OSA and treated with CPAP therapy to optimize outcomes. Consequently, it is essential that information regarding the application of CPAP treatment in patients with OSA and cardiac arrhythmia be comprehensively reviewed to inform more rigorous and ethical clinical decision making.
To date, 2 meta-analytic reviews29,30 have been published to provide insight into the topic of effect of CPAP intervention on cardiac arrhythmia. Although both reviews provide a solid launching point for our review, they, unfortunately, implausibly assumed homogeneity of risk within numerous categories relevant to the topic (age, sex, type, and severity of arrhythmia, compliance with CPAP, type of intervention, etc) and focused on the effect of CPAP treatment only on atrial fibrillation (AF) recurrence after catheter ablation procedures. Keeping in mind these limitations, we undertook an updated review of the literature on CPAP application in patients with OSA and any type of cardiac arrhythmia to accomplish the following purposes: (1) to examine scientific evidence regarding efficacy of CPAP toward frequency and severity of different types of cardiac arrhythmia and (2) to categorize benefits in the application of CPAP intervention for patients with OSA and cardiac arrhythmia.
Methods
Data sources
We searched PubMed, CENTRAL, and Embase databases using the search terms “exp sleep*” or “sleep apnea” or “exp sleep related breathing disorder,” along with “exp arrhythmia, “bradycardia, “arrest,” “block,” “ectopy,” “ventricular fibrillation,” “atrial fibrillation,” or “exp atrial flutter,” and “exp continuous positive airway pressure.” The appropriate truncations were included. The databases were searched up to December, 2016. The complete searches can be found in Supplementary file 1. Furthermore, publications identified from bibliographies of identified articles and reviews were considered eligible. We emphasized prospective studies and nonrandomized and randomized trials that applied CPAP to manage any type of cardiac arrhythmia in adult (>18 years old) patients with OSA of any severity.
Study selection
The search procedure yielded 331 abstracts (Figure 1 and Supplementary file 1). The title and abstract of the papers were scanned to determine whether they fit the inclusion criteria. Peer-reviewed, English language studies were included if they focused on the effect of CPAP treatment and identified any specific arrhythmia outcome: heart rate, frequency, and/or severity of episodes of specific arrhythmia. Case reports, pediatric studies, dissertations, and articles with no primary data were also excluded.
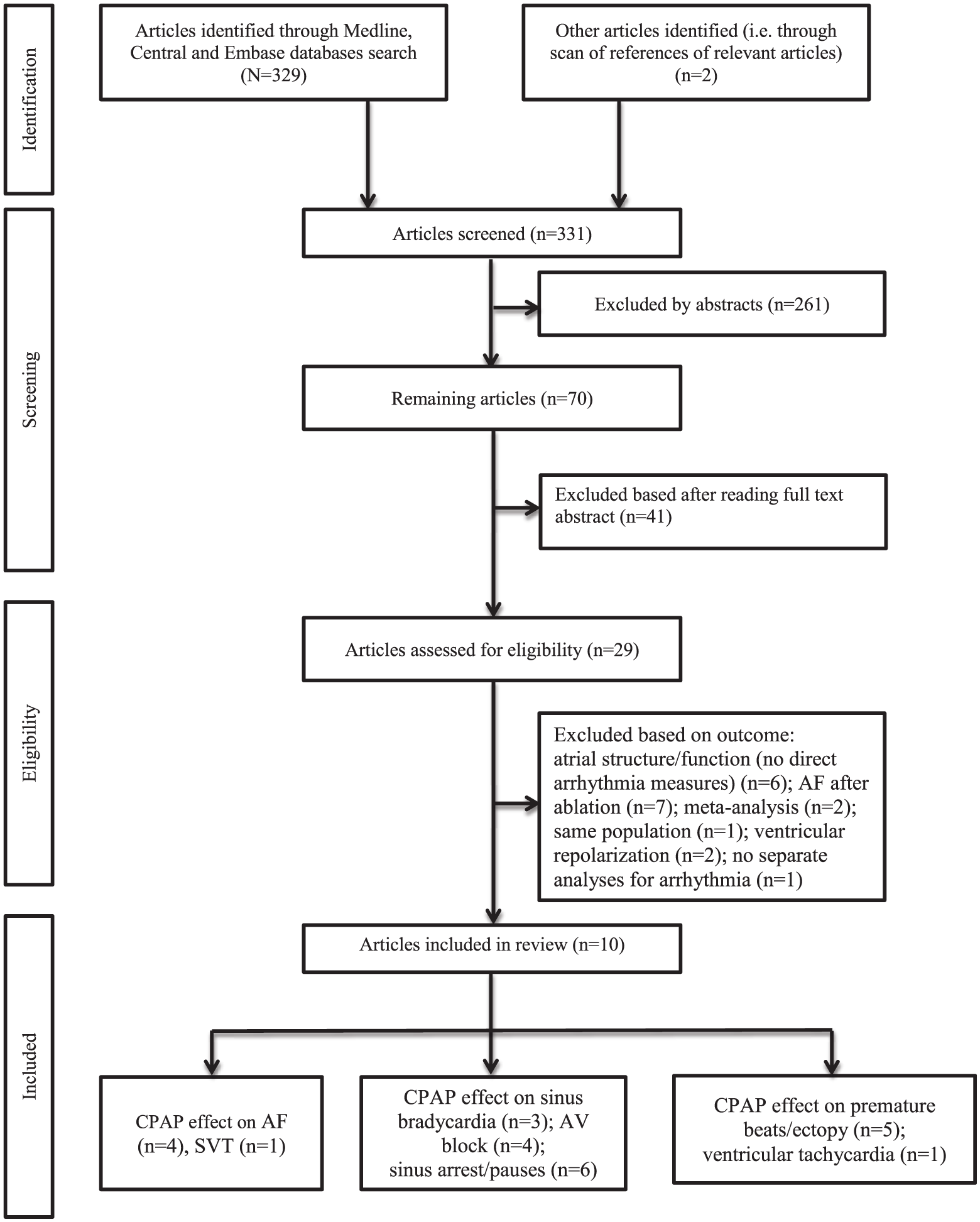
Flowchart documenting process of article selection for review. AF indicates atrial fibrillation; CPAP, continuous positive airway pressure; SVT, supraventricular tachycardia.
Data extraction
After screening the titles, abstracts, and full texts where necessary, 29 full-text articles were considered relevant and were downloaded for full review (Figure 1). Studies that focused on a different but concurrent topic in cardiology (ie, CPAP effects on atrial remodeling, AF recurrence after ablation, etc) were excluded. After reading the full text of the articles selected in the first stage, 19 articles were excluded because they did not meet the inclusion criteria. The reasons for exclusion are listed in Supplementary file 2. The remaining 10 articles were selected for data synthesis.
Data synthesis
Selected articles were appraised and categorized based on the category of cardiac arrhythmia. The information abstracted from the articles included study details (ie, author names, publication year, setting, country), study characteristics (ie, objective, design, inclusion/exclusion criteria, sample size), participant characteristics (mean age, sex, comorbid disorders), severity of OSA and arrhythmia, methods of assessment, characteristics of CPAP intervention (ie, duration, limitations, adherence, etc), and outcome measure preintervention and postintervention. We followed Elsevier’s Evidence for Primary Research Question 31 criteria to assign the level of evidence to each study.
Results
Table 1 summarizes characteristics and key findings of the reviewed studies. Sample size varied from 17 to 10 132 patients with any type of cardiac arrhythmia. Primary outcomes were generally limited to measures of effectiveness in alleviating cardiac arrhythmia or reducing its severity. Three types of cardiac arrhythmia were identified: (1) supraventricular tachyarrhythmia: AF and supraventricular tachycardia (SVT); (2) bradyarrhythmia: sinus bradycardia, atrioventricular (AV) block and sinus pauses/arrest; and (3) ventricular arrhythmia: ventricular premature beats (VPBs)/extrasysoles/ectopy and ventricular tachycardia (VT).
Studies that have examined the efficacy of continuous positive airway pressure treatment in patients with cardiac arrhythmia and obstructive sleep apnea: summary of studies’ characteristics and findings.
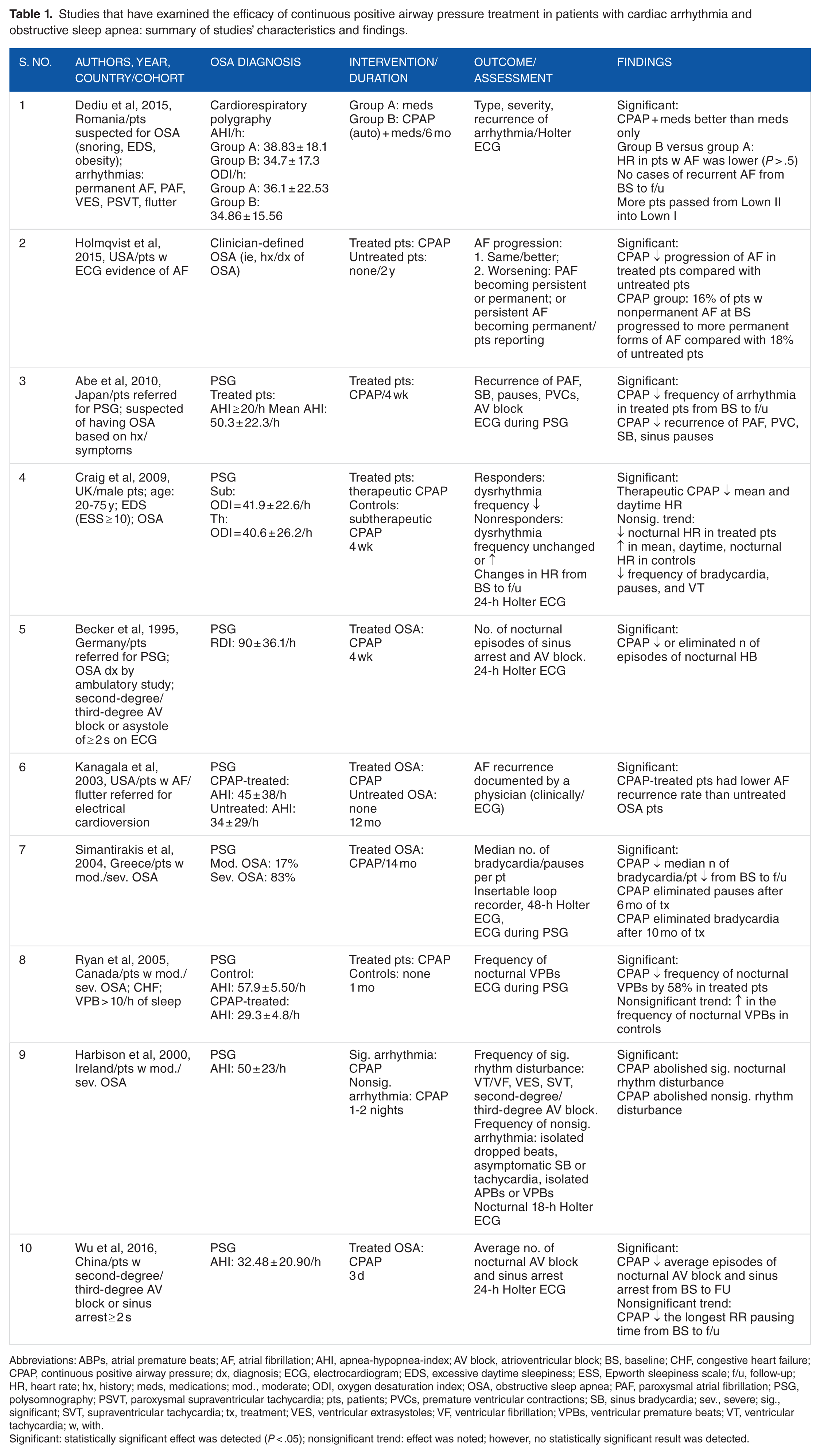
Abbreviations: ABPs, atrial premature beats; AF, atrial fibrillation; AHI, apnea-hypopnea-index; AV block, atrioventricular block; BS, baseline; CHF, congestive heart failure; CPAP, continuous positive airway pressure; dx, diagnosis; ECG, electrocardiogram; EDS, excessive daytime sleepiness; ESS, Epworth sleepiness scale; f/u, follow-up; HR, heart rate; hx, history; meds, medications; mod., moderate; ODI, oxygen desaturation index; OSA, obstructive sleep apnea; PAF, paroxysmal atrial fibrillation; PSG, polysomnography; PSVT, paroxysmal supraventricular tachycardia; pts, patients; PVCs, premature ventricular contractions; SB, sinus bradycardia; sev., severe; sig., significant; SVT, supraventricular tachycardia; tx, treatment; VES, ventricular extrasystoles; VF, ventricular fibrillation; VPBs, ventricular premature beats; VT, ventricular tachycardia; w, with.
Significant: statistically significant effect was detected (P < .05); nonsignificant trend: effect was noted; however, no statistically significant result was detected.
Supraventricular tachyarrhythmia
Atrial fibrillation
Four studies32–35 focused on controlling AF with the use of a CPAP device. Studies involved patients with mild to severe OSA. All 4 studies, involving patients (n = 2041) with AF (paroxysmal, persistent, permanent), differed in the duration of application of CPAP treatment from baseline testing to follow-up assessment, the level of sleep studies that reported on CPAP efficacy (level 1 [ie, in-auto-titration sleep study with a portable monitoring device]), diagnostic definition of obstructive apnea or hypopnea applied in each study, and the rate of adherence/compliance with CPAP application. General improvements of AF parameters (ie, mean heart rate, frequency/recurrence of AF episodes) have been reported in all 4 studies from baseline to follow-up. Also, in CPAP-treated patients, there was less progression to more permanent forms of AF compared with untreated patients (for more information, please refer to Table 1 and Supplementary file 3).
Supraventricular tachycardia
One study 36 evaluated SVT between 2 groups of subtherapeutic (n = 40) and therapeutic (n = 43) CPAP. The study defined SVT as a heart rate over 125 bpm with narrow complexes not preceded by normal sinus P wave (including AF) for more than 3 consecutive beats. There was 1 patient with AF in each group. However, the study did not report data regarding outcome measures of AF frequency/severity within the SVT category. The prevalence of SVT per 24 hour was 35% in the subtherapeutic group and 32.6% in the therapeutic CPAP group at baseline. There was no significant change in SVT frequency (daytime or nocturnal) from baseline to follow-up in the 2 groups.
Bradyarrhythmia
Three studies32,36,37 investigated the effect of CPAP treatment on sinus bradycardia in 119 patients. Four studies32,38–40 evaluated second-degree and third-degree AV block in 74 patients in total. Six studies32,36–40 included 194 patients with sinus pauses/arrest. Outcome measures included the total number of episodes, the average number of episodes per 24 hour, and the number of episodes per patient. Several studies reported that CPAP treatment significantly decreased or totally prevented the recurrence of nocturnal sinus bradycardia, AV block, and sinus arrest.32,37–40 In one study, 36 researchers found a positive trend in favor of therapeutic CPAP decreasing nocturnal sinus bradycardia and pauses. However, this result did not reach a level of statistical significance (for more information, please refer to Table 1 and Supplementary file 3).
Ventricular arrhythmia
Five studies32,33,36,39,41 investigated the effect of CPAP treatment on VPBs in 132 patients in total. A randomized controlled trial (RCT) 36 evaluated VT events among therapeutic (n = 43) and subtherapeutic (n = 40) CPAP groups. Assessed outcomes included the recurrence and severity of VPBs classified by the Lown classification. Three studies32,39,41 reported a significant reduction in the frequency of nocturnal VPBs. Fourth study 33 reported improvement in severity of VPBs by categorizing patients in a lower level of the Lown classification after CPAP treatment. Still another study (the RCT) failed to detect a statistically significant reduction in VPBs frequency (daytime or nocturnal) while still observing a trend toward a fewer daytime VT events 36 (for more information, please refer to Table 1 and Supplementary file 3).
Discussion
In this study, we have summarized evidence regarding CPAP application in patients with OSA and cardiac arrhythmia and highlighted potentially essential effect of improved nocturnal breathing with CPAP application on altered cardiac impulse formation and impulse conduction, involved in the mechanism of cardiac arrhythmia. Despite the general clinical and methodological differences between studies (ie, type and severity of cardiac arrhythmia, patients’ medication regime, age, sex, OSA severity, period of CPAP application, etc), the observed results point to the promising improvements in studied cardiac pathology in OSA with CPAP application overall and support feasibility of CPAP intervention in patients with both atrial and ventricular arrhythmia.
Atrial fibrillation
Results from studies included in this review show positive effects of CPAP treatment on the frequency32,34 and severity of AF episodes. 33 Proposed mechanisms of CPAP effects on decreasing the frequency of AF episodes include a reduction in sympathetic nervous system activity,42,43 nocturnal hypoxemia, and hemodynamic stress, 44 all of which play a crucial role in the development of AF and other arrhythmias. In addition, the reversibility of OSA-induced atrial electrical remodeling in response to CPAP application has been discussed.45–47 For instance, signal-averaged P-wave (SAPW) duration, which is regarded as a marker of atrial electrical remodeling, has shown to be longer in patients with severe OSA compared with patients with less severe OSA. 45 Furthermore, 4 weeks of CPAP treatment resulted in a significant decrease in SAPW duration compared with controls with no CPAP treatment.45,47 Furthermore, CPAP treatment reduced the electromechanical delays between and within the atria and decreased P-wave dispersion with 6 months of therapy application. 46
Regarding the structural remodeling, the results of included studies were not uniformly consistent. In an RCT, CPAP treatment was found to improve left atrial passive emptying and functional performance, with no significant changes in atrial structure from baseline to 24-week follow-up. 48 Likewise, a decrease in left atrial volume and volume index found in patients compliant with CPAP treatment after 12 months was not significantly different from pretreatment values. 49 However, a significant increase in both measures was reported in noncompliant patients. 49 Therefore, improvement in atrial performance and potentially reversing atrial electrical and/or structural changes may help explain putative improvements in AF associated with CPAP application. Nonetheless, further research is needed to evaluate CPAP effects on atrial structural and functional measures in patients with AF. Further understanding of the mechanism by which OSA induces remodeling and evaluating patients for incident AF may provide a better knowledge around the clinical implications of CPAP treatment, for example, in patients with OSA of milder severity. It is also important to determine the duration of CPAP therapy that is required to induce positive changes and possible reversal effect. Although an electrical disturbance seems to be reversed within a short duration of CPAP application (ie, 1 month), 47 structural remodeling seems to be more resistant to positive changes with CPAP treatment. 48 Despite inability to infer a protective role of CPAP against structural remodeling, taken together, the results support the hypothesis that CPAP application in patients with OSA along with compliance with treatment confers a reduced risk of AF frequency and severity.
Supraventricular tachycardia
One study 36 included in this review reported a significant reduction in daytime heart rate (but not nocturnal) and changes in the frequency of SVT with 4 weeks of CPAP application, which, however, did not reach a level of statistical significance from baseline to follow-up. 36 Researchers attributed the reduction in daytime heart rate to reduced sleep fragmentation and reduced sympathetic activity associated with OSA following CPAP application. The reasons for the reduction in SVT frequency in response to CPAP treatment application not reaching the level of statistical significance from baseline to follow-up could be attributed to insufficient sample size that allows detection of differences, limited follow-up time, and/or short-term electrocardiogram (ECG) monitoring. In addition, the study population did not include patients with heart failure or myocardial infarction, who generally have a higher prevalence of arrhythmia due to associated ventricular dysfunction, and thus changes of arrhythmia prevalence could be less evident with the exclusion of this population. Nevertheless, changes observed in SVT frequency with CPAP application from baseline to follow-up were clinically relevant and, therefore, should be considered when designing larger clinical trials.
Bradyarrhythmia
Obstructive sleep apnea–induced hypoxia increases the carotid chemoreceptor activity which, in the presence of obstruction, increases vagal stimulation of the heart and consequently triggers bradyarrhythmia. 19 It has been observed that about 87% of OSA-associated nocturnal bradyarrhythmias occur during rapid eye movement (REM) stage of sleep 50 due to autonomic instability. Continuous positive airway pressure treatment, by restoring normal breathing, eliminates the adverse effects of hypoxia and autonomic changes during obstructive events and hence prevents the occurrence of OSA-induced bradyarrhythmia. Several studies32,37–40 reported a decrease in the frequency of nocturnal sinus bradycardia, AV block, and sinus arrest even after a short duration of CPAP use (ie, 2 nights). 39 Interestingly, 2 studies37,40 excluded patients with an abnormal electrophysiological studies thereby eradicating the presence of sinoatrial node or AV node dysfunction. Simantirakis et al 37 applied an insertable loop recorder for long-term cardiac rhythm monitoring in addition to the 48-hour ECG Holter. Importantly, the weekly analysis of the insertable loop recorder detected that 22% of patients experienced cardiac rhythm disturbances, whereas the 48-hour Holter revealed that only 13% of patients experienced cardiac arrhythmia. 37 Most of the detected episodes of bradycardia and pauses were nocturnal and showed a significant night-to-night variability in individual patients. In CPAP-treated patients, Craig et al 36 reported a trend toward a reduction in the frequency of nocturnal bradycardia and pauses, which did not reach the level of statistical significance. The conventional short-term ECG monitoring and lack of assessment of SA/AV-node function may contribute to these nonsignificant results. Likewise, in light of previous research that revealed that bradycardia and pauses are more prevalent in patients with severe OSA, 51 concomitant heart failure, 52 longer obstructive events, 53 and higher degrees of oxygen desaturation, 50 the population characteristics might constitute a confounder of the nonsignificant results in Craig et al 36 study and should be accounted for in future research on the topic.
Ventricular arrhythmia
A significant reduction in the frequency of nocturnal VPBs immediately after the application of CPAP treatment has been observed in the study by Harbison et al. 39 Likewise, a decrease in the severity of VPBs was reported within 6 months of CPAP initiation in the study by Dediu et al 33 . In contrast, Craig et al 36 did not observe a significant reduction in the prevalence of Ventricular Ectopy (VE) but showed that daytime VT events tended to decrease after 4 weeks of CPAP treatment. 36 Although the reason for conflicting findings between studies remains unclear, it is expected that CPAP would decrease the occurrence/recurrence of VPBs by providing more homogeneous conduction and improving ventricular repolarization. Earlier evidence showed that OSA causes a prolongation of ventricular repolarization and dispersion measures (including QT interval) at the onset of an apneic event and a sudden shortening of these indices at the end of apneas. 54 In addition, a significant positive correlation between repolarization changes and measures of sympathetic function such as heart rate and urinary adrenaline levels has been detected. 54 Thus, increased sympathetic stimulation in OSA may contribute to the underlying mechanism of increased cardiac dispersion and consequent ventricular arrhythmia. Furthermore, withdrawal of CPAP treatment has previously shown a prolongation of ventricular repolarization measures 55 —a precursor of ventricular arrhythmia and sudden cardiac death. 56 Conversely, CPAP treatment of moderate to severe OSA provided a significant reduction in ventricular dispersion. 57 Taken together, in the context of clinical details on OSA severity, CPAP treatment is likely to hold more benefits for patients with more severe OSA, whereas preventive role of CPAP in ventricular arrhythmia appear to have less apparent effect in studies of milder forms of OSA. These findings suggest that clinicians should not view OSA and cardiac arrhythmia in vacuum but instead consider these markers and the utility of CPAP treatment in combination with other clinical details to make decisions.
Limitations
Assessment of the quality of the included studies was not formally reported due to the heterogeneous study methodology (ie, cohort, case-control, RCT) of included studies. Furthermore, the population of interest was heterogeneous in terms of age, sex, OSA severity, medication regime, etc, as well as severity and type of cardiac arrhythmia. This heterogeneity at multiple levels precluded us from performing a meaningful formal assessment of the quality of the included studies. To minimize bias and maximize internal and external validity, we included studies published only in peer-reviewed journals, screened articles for potential risk of biases (excluding those with insufficient information), and extracted and reported all information about the studies (ie, intervention, population, context, sample sizes, outcomes, and the level of evidence on the hierarchy of scientific evidence). Supplementary file 3 is structured such that it allows observing the similarities and differences between characteristics and outcomes of the included studies. Another limitation concerns inclusion of only peer-reviewed studies published in English thereby omitting publications in other languages and their possibly relevant results. We also eliminated possibly relevant studies which evaluated CPAP effects on arrhythmia frequency after catheter ablation procedures,58–62 as it was not possible to separate the effect of the ablation procedure from the effect of CPAP treatment and in light of a previously published meta-analytic reviews on that topic.29,30 Despite these limitations, our review represents a first step in summarizing the evidence on the role of OSA treatment in different types of cardiac arrhythmia, and in understanding how normalization of nocturnal breathing through CPAP application affects altered impulse formation and conduction (Figure 2), particularly relevant should clinicians attempt to identify preclinical OSA cases in patients with arrhythmia.
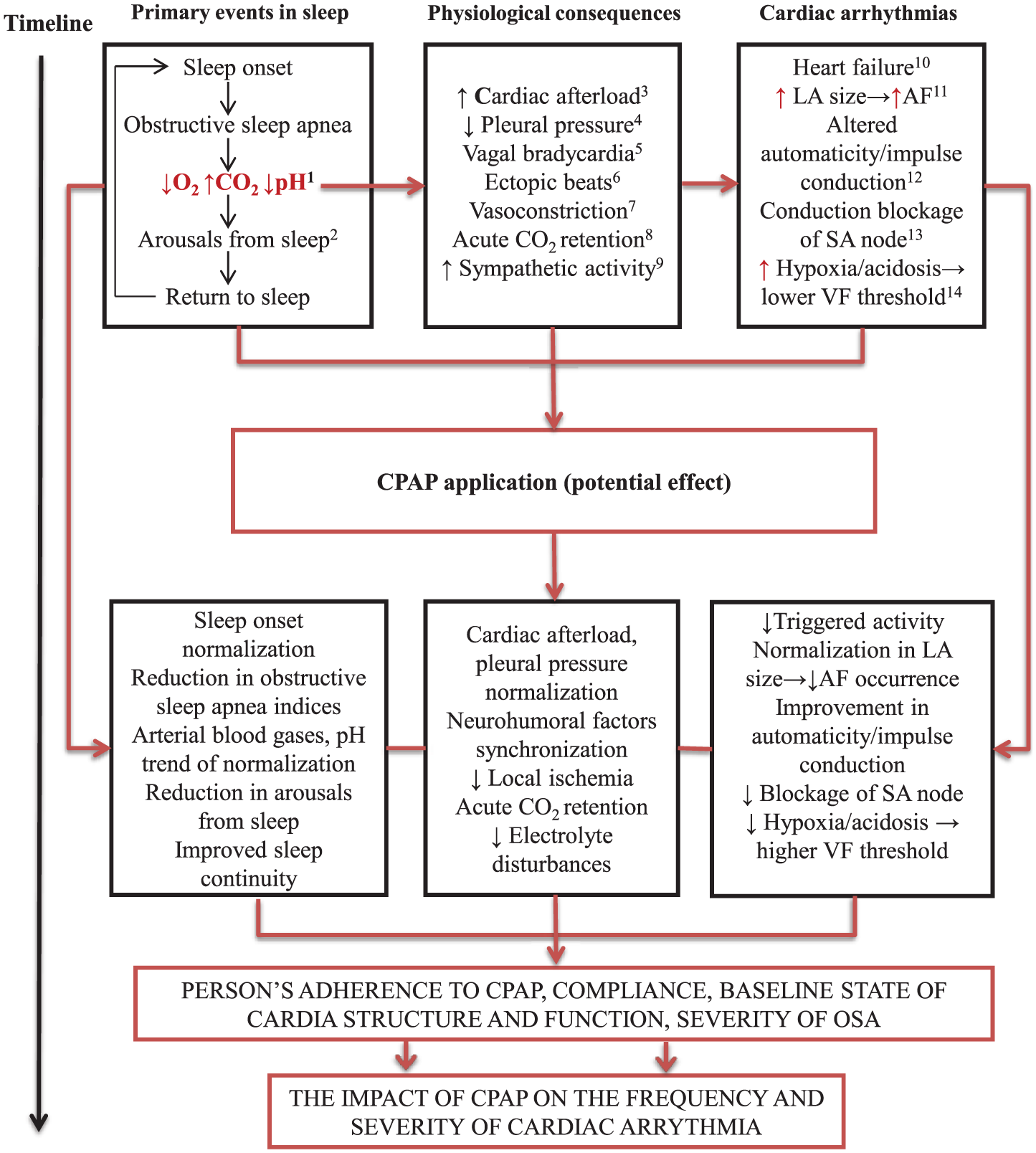
Schematic representation of the longitudinal associations in OSA informing CPAP application in patients with cardiac arrhythmia. AF indicates atrial fibrillation; CPAP, continuous positive airway pressure; SVT, supraventricular tachycardia; VF, ventricular fibrillation. References 1 to 25 to support the figure are provided in Supplementary file 3.
General Discussion and Future Directions
Obstructive sleep apnea is associated with various forms of atrial and ventricular arrhythmia, and the severity of OSA is linked to the progression of these arrhythmias. Reviewed evidence from observational and nonrandomized studies has consistently shown significant positive effects of CPAP treatment in patients with cardiac arrhythmia from the baseline to follow-up. These effects included a statistically significant (1) reduction in mean heart rate and in the frequency and progression of AF episodes; (2) reduction in nocturnal bradyarrhythmia including sinus bradycardia, second-degree and third-degree AV blocks, and sinus pauses; and (3) functional improvements in measures of ventricular repolarization and reduction in the frequency of nocturnal ventricular ectopy. The results have also highlighted improvement of electrical and structural remodeling of the atria with CPAP administration, which may decrease the risk of occurrence and/or recurrence of atrial arrhythmia. The results from a single randomized trial in male patients aged 20-75 years confirmed a significant reduction in the average and daytime heart rate after 4 weeks of CPAP administration compared with a group of male patients who received a subtherapeutic CPAP treatment, however, did not detect statistically significant changes of the frequency of arrhythmia including SVT, sinus bradycardia, sinus pauses, ventricular ectopy, and ventricular tachycardic events from pretreatment to posttreatment administration. These inconsistencies between results could be due to differences in the methodology, sample size, or selection of patients (eg, unmatched controls or small samples). In addition, positive effects of CPAP therapy are clearly linked to the duration of nightly use and its use during REM sleep, 63 in which unopposed sympathetic activity creates a favorable milieu for occurrence of arrhythmic events. After a myocardial injury, there is loss of physiological vagal response during sleep, which may explain the higher risk of complications during sleep, including lethal arrhythmias and sudden cardiac death. In addition, decreased motor output to pharyngeal muscles during REM sleep results in an increase in the upper airway resistance and periods of hypoventilation.64,65 Therefore, severe respiratory events during REM sleep (period of which increases as the night progresses) emphasize the importance of the continuous application of CPAP across study period (ie, overnight compliance), the topic which has not been received significant attention in studies we included in this review. The issue of CPAP compliance falls beyond the scope of this review; however, it is important to note that 29% to 83% of patients use the CPAP devices for less than 4 h/night, 66 often at the beginning of the night only, which may be responsible for differences in the magnitude (or lack) of treatment effect. For example, a recent study (SAVE trial) 67 has shown that CPAP treatment, in addition to usual care, has failed to cause a statistically significant reduction in the occurrence of cardiovascular events in patients with moderate to severe OSA, a conclusion that may be biased by low level of compliance (on average 3.5 h/night on first year). Such level of compliance would not allow to accurately assess the efficacy of the treatment on long-term cardiovascular events and, therefore, should be taken into account when interpreting results.
In the context of arrhythmia burden, the exact mechanism and timeline for induction of arrhythmia in patients with OSA are yet to be explained. Although OSA may constitute an extra factor in inducing arrhythmia, other factors possibly related to the comorbid conditions such as hypertension 68 and obesity69,70 may play a role in arrhythmia occurrence. Moreover, the baseline severity of OSA may affect the response to CPAP treatment. With the progression of severity of OSA, it is expected that electrical and structural remodeling of the atria are more resistant to CPAP therapy or may require longer duration for reversal. A recent study showed that CPAP treatment improved gene expression of circulating potassium channels in patients with moderate OSA but not in those with severe OSA. 71 Downregulation of potassium channels in patients with OSA may explain prolonged QT interval and increased risk of ventricular arrhythmia and sudden cardiac death. 71 Hence, CPAP treatment may not reverse long-term structural remodeling which triggers arrhythmia; however, it may decrease further progression of such events. Therefore, treatment of OSA with CPAP therapy should be considered as an adjunct to the medical therapy for arrhythmia and/or other related conditions and not as a sole treatment. Finally, it remains to be determined whether early screening of OSA in patients with arrhythmia and subsequent treatment administration is protective in terms of long-term cardiovascular morbidity and mortality.
Conclusions
The available evidence on the effect of CPAP treatment on the recurrence and severity of cardiac arrhythmia is currently insufficient, as we found variability in the magnitude of the effect in studies of variable methodology addressing these issues. More research is needed to establish associations between the duration of CPAP treatment, patients’ characteristics, severity of baseline OSA, primary versus secondary nature of cardiac arrhythmia, general health status (ie, comorbidity load), response to/and compliance with antiarrhythmic medications, medication effects with impact on smooth muscle, and the magnitude of CPAP treatment effect. Development in future studies should entail a clear monitoring of CPAP adherence across the sleep period, calculate adequate sample size for detection of statistical difference, and focus on clinically meaningful effects of CPAP treatment in patients with cardiac pathology. Future research, considering the above-mentioned points, may lead to scientific and clinical progress in the understanding of and appreciation for the complexity of factors influencing the magnitude of the effect in response to CPAP treatment administration.
Footnotes
Peer review:
Three peer reviewers contributed to the peer review report. Reviewers’ reports totaled 903 words, excluding any confidential comments to the academic editor.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
