Abstract
Chronic obstructive pulmonary disease (COPD), a common, preventable, and treatable disease characterized by persistent respiratory symptoms and airflow limitation, is rapidly becoming a global healthcare challenge. Chronic obstructive pulmonary disease is the third leading cause of death in the United States and has been ranked fourth worldwide. Its current therapies improve symptom relief but do not alter the natural history of the disease. Therefore, as COPD is a progressive condition, novel treatment strategies, and alternative therapies are desperately needed. There are now multiple lines of evidence suggesting that changes to the pulmonary vasculature are important to the development and progression of COPD, independent of pulmonary hypertension. Hence, we hypothesize that a vascular-targeted therapy can be a potent and reliable way of monitoring and possibly changing the course of COPD progression. This review focuses on the potency and promise, as well as challenges, of developing vascular-targeted therapy in alleviating the early onset of COPD signs and symptoms.
Introduction
Chronic obstructive pulmonary disease (COPD) is a complicated disease of the lower respiratory system that is posing a major challenge to the health care and scientific communities with its complex clinical manifestations and comorbidities. Presently, COPD is the third leading cause of death in the United States and the fourth leading cause of death worldwide.1,2 Also, in the year 2000, COPD was responsible for 8 million physician office and hospital outpatient visits, 1.5 million emergency department visits, 726 000 hospitalizations, and 119 000 deaths. 3 In 2010, there were more than 3 million COPD deaths recorded worldwide 1 and among US adults, an estimated 15.7 million adults had been told by a physician or other health care professional that they have COPD. 4
Recently, the 2017 Global Initiative for Chronic Obstructive Lung Disease executive report defined COPD as a common, preventable, and treatable disease characterized by persistent respiratory symptoms and airflow limitation that is due to airway and/or alveolar abnormalities. 5 There are several different components of COPD definition and the clinical syndromes that make up COPD which require additional clarification, including the extent of airflow limitation and reversibility of this limitation, classification of disease severity, respiratory symptoms, chronic bronchitis, emphysema, and asthma. 6 These clinical syndromes and comorbidities make the treatment of COPD complicated.
Bacterial and viral infections, environmental pollution, and genetic makeup (for example, alpha-1 antitrypsin deficiency) are classified as risk factors; however, cigarette smoking remains the most common risk factor for COPD. 7 Continued irritation of the lung tissue by noxious particles induces epithelial and endothelial changes and causes weakened compliance of the lungs. These irritants impede the proper functioning of the pulmonary blood vessels which facilitate the exchange of oxygen and carbon dioxide between pulmonary and systemic circulations. Airflow limitation in patients with COPD is usually progressive and associated with a chronic inflammatory response of the lungs to noxious particles or gases. 8 Chronic dyspnea and persistent inflammation of the airways and lung tissues are major contributors to the pathophysiology of COPD.
This review will selectively emphasize on the potency and promise of vascular-targeted therapy in alleviating the early onset of COPD signs and symptoms.
Current treatment options for COPD
Many clinical and translational research studies are increasingly focusing on finding more alternative therapies for combating the growing epidemic of COPD. More than half a century ago, the only therapies available for COPD treatment were antibiotics for pneumonia, potassium iodide used as mucus thinner, and combination products containing ephedrine, a small amount of theophylline, and a minor amount of sedative to deal with the side effects of ephedrine. 9 Presently, there is a broader spectrum of COPD therapies and they are mainly categorized as either anti-inflammatory agents or bronchodilators. However, current medications are focused on symptom relief and do not conclusively alter the natural history of the disease. As COPD is a progressive condition, novel treatment strategies are needed.
Smoking cessation and air quality control
Over the past 30 years, there has been a reasonable decrease in tobacco consumption in many developed countries, but in others, smoking rates remain alarmingly high. 10 Consequently, smoking cessation remains the best intervention for slowing lung function decline and is one of the few interventions in COPD to improve survival. Many environmental pollutants are natural risk factors for COPD development. Research has shown that the most common environmental pollutants linked to COPD include traffic pollutants and wood smoke. 6 Therefore, adequate air quality control management is critical to the gradual increase or decrease in COPD prevalence over time.
Anti-inflammatory agents
Chronic inflammation in COPD causes narrowing of the airways and eventual destruction of lung parenchyma. These adverse effects can be improved using anti-inflammatory agents to counter the dysfunction of immune cells. Some of the clinical benefits of anti-inflammatory agents include improved lung function and symptoms, reduction in exacerbation, and improved health status. 5 Of the many anti-inflammatory agents currently available, only corticosteroids and phosphodiesterase 4 (PDE4) inhibitors are used clinically. This is partly because of the potential side effects associated with other agents. 5 The PDE4 inhibitors can improve peak expiratory flow, forced expiratory volume in 1 second (FEV1), and forced vital capacity, as well as reduce exacerbations. 11 Although beneficial clinically, regular treatment with inhaled corticosteroids could, over a period of time, lead to an increased risk for pneumonia. 5
Bronchodilators
Therapies in this group relax the smooth muscles in the lung airways, resulting in bronchodilation and improvements in shortness of breath. The duration of bronchodilators, when inhaled or administered orally, can be short term or long term depending on the mechanism of action of the drug used. Short-term bronchodilators can be classified as short-acting beta agonists and/or short-acting muscarinic antagonists, whereas long-term bronchodilators can also be classified as long-acting beta2 agonists and/or long-acting muscarinic antagonists. Clinically, bronchodilators improve lung function, FEV1, and enhance symptom management. 5
The promise of vascular-targeted therapy
Because bronchodilators and anti-inflammatory therapies mostly focus on symptom relief and not on the progression of the disease, there is an urgent need for more alternative therapies. Hitherto, there is still a paucity of therapies that can modify the early onset of COPD pathogenesis. Thus, the central aim of this review is to highlight the need for vascular therapies to be considered and explored in targeting the course of COPD symptoms. We hypothesize that a vascular-targeted therapy can be a potent and reliable way of monitoring and possibly changing the course of COPD progression. First, we will review a common pulmonary vascular manifestation of COPD, pulmonary hypertension (PH), and close with a discussion of the “vascular hypothesis” of COPD development and progression.
Pulmonary hypertension and chronic obstructive pulmonary disease
Overview
Pulmonary hypertension, defined as a mean pulmonary artery pressure (mPAP) ⩾ 25 mm Hg on right heart catheterization (RHC), is a common manifestation of COPD which is classified as group 3 PH by the World Health Organization. 12 Pulmonary hypertension portends a poor prognosis in patients with COPD, but no specific treatments have been proven to be beneficial for long-term use in this condition.
Prevalence
The overall prevalence of PH in patients with COPD has been difficult to elucidate, with estimates ranging from 18% to 90%. This large range of prevalence rates is reflective of varying mPAP cut points (⩾20 or ⩾25 mm Hg) and different patient populations (Table 1). The highest prevalence estimates come from studies investigating advanced patients with COPD undergoing workup for lung volume reduction surgery (LVRS) or lung transplant. Using the now standard definition of mPAP ⩾ 25 mm Hg as a cutoff for diagnosing PH, 30% to 50% of these patients had PH.13–15 In stable outpatients with less advanced disease, estimates range from 18% to 27%.16,17 In patients with COPD without PH at rest, >50% have an abnormal increase in pulmonary artery (PA) pressure during maximal exercise,16,17 which corresponds to a decreased functional capacity. 17 Therefore, most of the patients with COPD have increases in PA pressure, either at rest or during exercise.
Prevalence of PH in COPD.
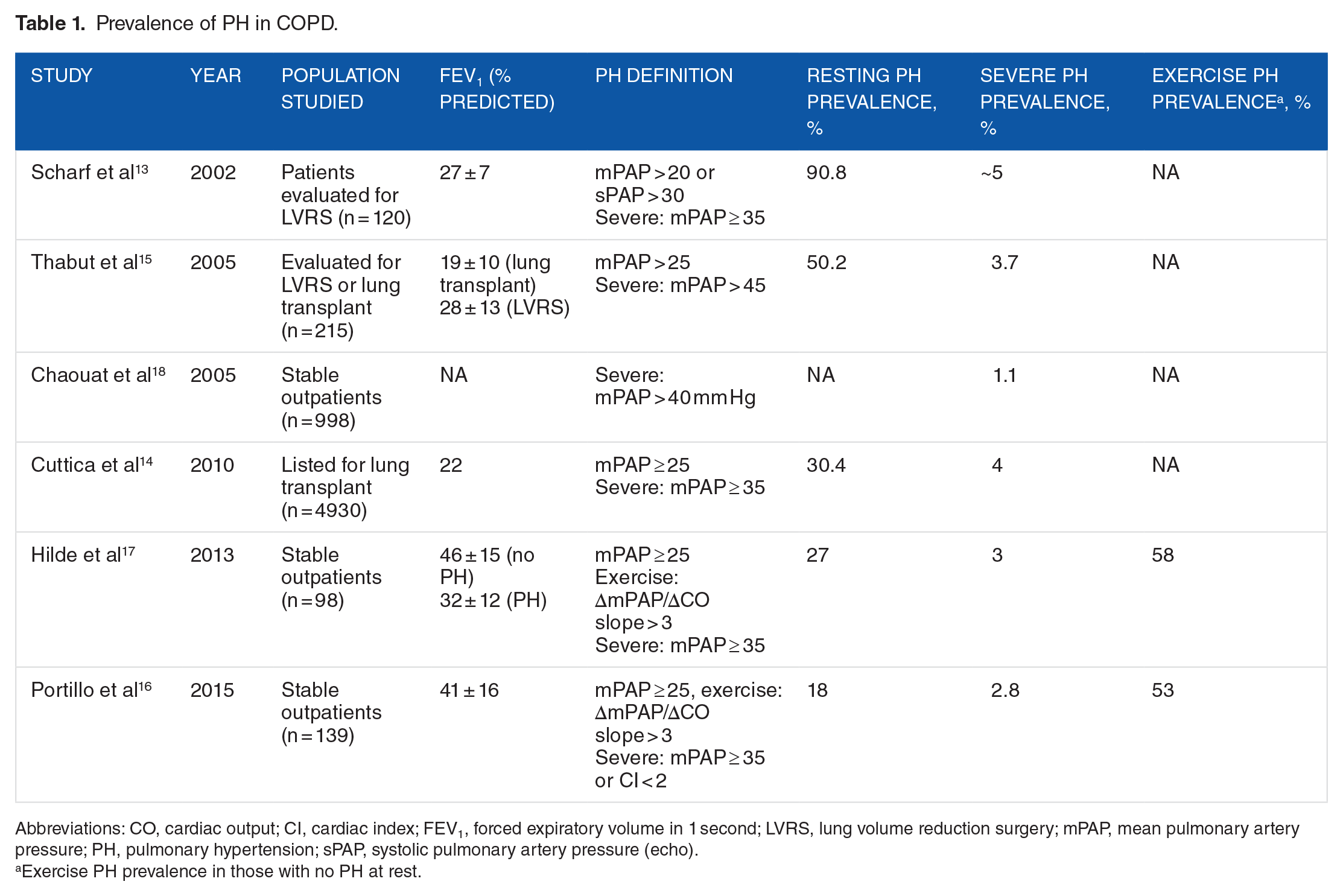
Abbreviations: CO, cardiac output; CI, cardiac index; FEV1, forced expiratory volume in 1 second; LVRS, lung volume reduction surgery; mPAP, mean pulmonary artery pressure; PH, pulmonary hypertension; sPAP, systolic pulmonary artery pressure (echo).
Exercise PH prevalence in those with no PH at rest.
Although most COPD patients with PH have mild-moderate increases in their PA pressure at rest, there is a small but significant subgroup of patients who appear to have severe PH, which is often out of proportion to their degree of lung function impairment. Prevalence of severe PH in COPD is as high as 5% 13 in those with advanced disease, but the best estimate is likely the 1.1% found in stable outpatients by Chaouat et al. Out of 998 patients with COPD who underwent RHC as part of their routine clinical evaluation, 27 had severe PH defined as a mPAP ⩾ 40 mm Hg. Of these, 16 patients had at least one other disease associated with PH (eg, left heart disease, human immunodeficiency virus, etc), whereas 11 (1.1%) had severe PH only caused by their COPD. 18 Although this number appears small, when taking into consideration how common COPD is, the number of patients with severe COPD-PH likely outnumbers those with idiopathic pulmonary arterial hypertension (PAH). COPD patients with severe increases in PA pressure appear to have a unique phenotype characterized by only moderate airflow obstruction, low carbon dioxide levels, and a severe reduction in diffusion capacity and oxygenation. 18 This was further confirmed in a cluster analysis by Thabut et al. 15 As outlined below, trials investigating specific drug therapy for COPD-PH have generally been negative, but this unique subgroup deserves further study, as their pulmonary vascular involvement appears to be different from other patients with COPD-PH.
Impact/prognosis
Patients with COPD-PH tend to have worse functional status and a greater degree of hypoxemia compared with patients with COPD without PH. In patients being evaluated for lung transplant, mPAP was an independent predictor of low 6-minute walk distance (6MWD).
14
This is also true for stable outpatients with COPD-PH; every 1 mm Hg increase in mPAP is associated with a 9.5-m decline in 6MWD.
17
In those with severe COPD-PH, there is a moderate negative correlation (r = −0.66) between mPAP and partial pressure of oxygen (Pa
The natural history of positive airway pressure change in COPD has been studied using RHC. In a study investigating patients with COPD without PH at baseline who had an RHC repeated (6.8 ± 2.9 years between RHCs), 33/131 (25%) developed PH, which was generally mild in severity. 19 For the entire group, the annual progression of mPAP was +0.4 mm Hg/y. Presence of PH has been consistently shown to be one of the strongest determinants of prognosis in patients with COPD. In patients with advanced COPD, presence of PH increased the risk for death while awaiting transplant by 27% to 40%. 14 Survival also depends on the degree of PH in patients with COPD. In those with severe PH-COPD, 1- and 3-year survivals were 70% and 33%, significantly worse than those with mild-moderate PH-COPD (83% and 55%, respectively). 20 Another study by Kessler et al 21 demonstrated that an mPAP > 18 mm Hg is one of the best predictors of increased risk for hospitalization due to acute exacerbations of COPD, a highly important clinical outcome.
Pathophysiology
The pathophysiology of PH is complex and multifactorial. As detailed below (section “vascular hypothesis of COPD development and progression”), a pulmonary vasculopathy exists throughout the spectrum of COPD severity, both in patients with and without PH (Figure 1). It is poorly understood why some patients with COPD develop PH and why some do not. Endothelial dysfunction and inflammation play an important role in the development of pulmonary vascular dysfunction (and resultant PH) in patients with COPD. These changes are likely triggered by the toxic effect of cigarette smoke and are further propagated despite smoking cessation. There have been a few studies that have shown differential levels of systemic inflammation in patients with COPD with and without PH, with patients with COPD-PH having an interleukin 6 (IL-6) gene polymorphism 22 and higher levels of c-reactive protein and tumor necrosis factor α. 23
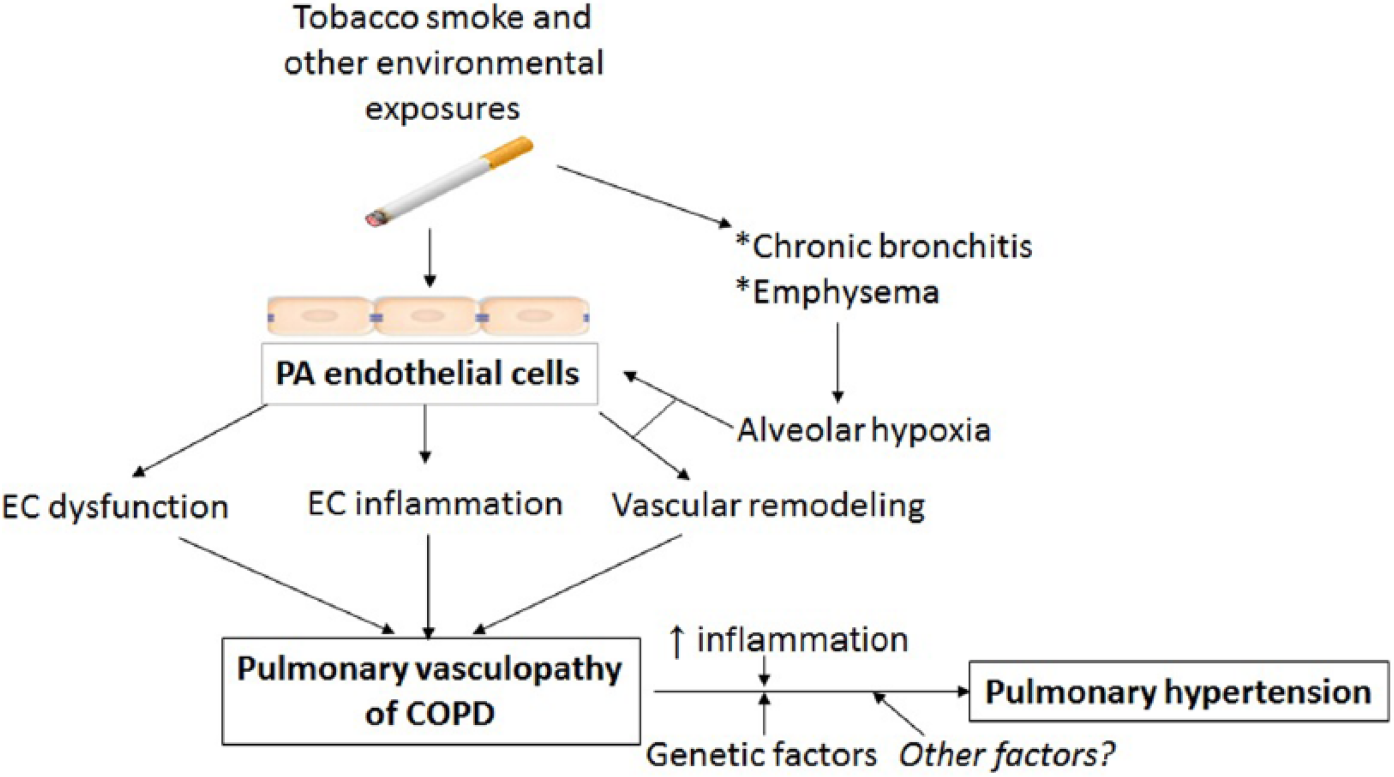
Vascular hypothesis of COPD development and progression. COPD indicates chronic obstructive pulmonary disease; EC, endothelial cell; PA, pulmonary artery.
Although alveolar and systemic hypoxia are contributing factors to the development of PH in COPD, it clearly is not the only factor, as endothelial changes occur early in the pathogenesis of mild COPD24,25 and, in one study, Pa
Evaluation
Pulmonary hypertension remains a hemodynamic definition and requires RHC for confident diagnosis. Pulmonary hypertension may be suspected clinically when patients with COPD have dyspnea out of proportion to their degree of airflow obstruction or if there are severe reductions in diffusion capacity for carbon monoxide or significant impairment in oxygenation. Echocardiography is generally advocated as the screening test of choice and allows for determination of right-sided chamber size and function, right atrial pressure assessment, and estimation of systolic PA pressure (sPAP). However, there are technical challenges in performing echocardiography in patients with COPD due to lung hyperinflation and rotation of the heart. For example, in 141 patients with advanced COPD, sPAP could be estimated in only 38% of patients. 28 Although there is a mild-moderate correlation between sPAP on echo and RHC in patients with COPD,20,28 echo can significantly overestimate or underestimate the presence of PH. In an analysis of patients with severe emphysema, 35% of echo estimates differed by more than 10 mm Hg from invasively determined PA pressures, 28 which can lead to erroneous assessment of the presence or absence of PH. Computed tomographic scans can also be used to screen patients for COPD-PH. A ratio of PA to aorta size > 1 outperformed echocardiography in identifying COPD patients with PH, with a diagnostic accuracy of 83%. 29 Ultimately, a diagnosis of PH must be made on RHC, defined as a resting mPAP ⩾ 25 mm Hg and PA wedge pressure of ⩽15 mm Hg, used. 12 In general, RHC should be reserved for patients with COPD undergoing workup for LVRS or lung transplant, as part of a clinical trial, or if off-label use of PH-specific medications is considered (see details below). Treating patients with COPD with PH-specific medications without first confirming the diagnosis invasively is strongly discouraged.
Treatment
There are no Food and Drug Administration–approved or guideline-recommended specific therapies for PH in patients with COPD. 30 Oxygen supplementation is indicated for patients with COPD with severe resting hypoxemia. Long-term oxygen therapy (LTOT) was shown in the seminal Nocturnal Oxygen Therapy Trial study to reduce pulmonary vascular resistance (PVR) in COPD patients with severe hypoxemia, in addition to having a mortality benefit. 31 Another report demonstrated that LTOT for 15 to 18 h/d can cause reverse progression of PH, but normalization of PA pressures rarely occurs. 32 Nonspecific vasodilators are not recommended as treatments for COPD-PH. Extensive investigations of calcium channel blockers in patients with COPD-PH concluded that these medications significantly impair hypoxic pulmonary vasoconstriction and oxygenation33,34 without reducing PA pressures with long-term use.35,36
Pulmonary hypertension–specific medications targeting the endothelin, nitric oxide/soluble guanylate cyclase, and prostacyclin pathways have been investigated without conclusive benefit. Phosphodiesterase-5 inhibitors have been studied extensively in COPD-PH. Acutely, sildenafil given to COPD patients with mild PH not only results in significant reductions in mPAP and PVR both at rest and during exercise but also worsens ventilation-perfusion (V/Q) mismatching and arterial oxygenation without altering oxygen delivery. 37 In a small randomized study in severe patients with COPD with moderate PH, 3 months of sildenafil treatment did not improve exercise capacity or quality of life. 38 Similar results were found in a larger randomized study of tadalafil in COPD-PH. 39 Both of these studies included patients with mild-moderate elevations in PA pressures, which may not be the population who could benefit most from PH therapy. A small pilot study enrolling 28 patients with more severe PH randomized patients to sildenafil or placebo (2:1) for 16 weeks found a significant reduction in PVR (mean placebo difference −1.4 Wood units), as well as improvements in diffusion capacity and quality of life without impairing oxygenation. 40 The acute effect of riociguat, a more recently developed medication targeting the soluble guanylate cyclase pathway, was tested on 23 patients with COPD with mild to severe PH. Riociguat acutely decreased mPAP and PVR, along with an increase in cardiac output. 41 Long-term studies of riociguat in COPD-PH are needed.
The dual endothelin antagonist bosentan has also been investigated in COPD-PH. In a small randomized, nonblinded study of 18 months of bosentan in patients with moderate-severe COPD-PH, treatment resulted in improvements in mPAP, PVR, and 6MWD without affecting systemic oxygenation. 42 Another study of bosentan in patients with severe COPD did not show any improvements in exercise capacity but did demonstrate significant worsening of oxygenation and quality of life. However, this study did not specifically include patients with COPD-PH, and PA pressures were estimated by echocardiogram. 43
Epoprostenol, a potent pulmonary vasodilator targeting the prostacyclin pathway, was investigated in severe patients with COPD with elevated PA pressures in the setting of respiratory failure from an acute exacerbation of COPD. Patients received epoprostenol for 2 days and had an initial improvement in mPAP, but this effect waned after 24 hours; more concerning was a substantial decrease in Pa
As is clear from these studies (Table 2), there is no conclusive evidence from large randomized studies that PH-specific medications lead to clinically meaningful benefit in COPD patients with PH. There are 3 potential reasons why PH-specific medications have, in general, failed in patients with COPD: (1) the pathogenesis of PH in COPD is different from group 1 PH (idiopathic PAH, drug-induced PAH, connective tissue disease, etc) and therefore targeted therapy may not be beneficial in this subgroup; (2) beneficial effects on hemodynamics are counterbalanced by negative effects on gas exchange, which could lead to an overall neutral clinical effect; or (3) the wrong group of patients with COPD-PH has been studied, and future studies should target the subgroup of patients with COPD-PH with out of proportion disease (ie, high PA pressure, moderate obstruction, very low diffusion capacity).
Randomized clinical studies of PH-specific medications in patients with PH.
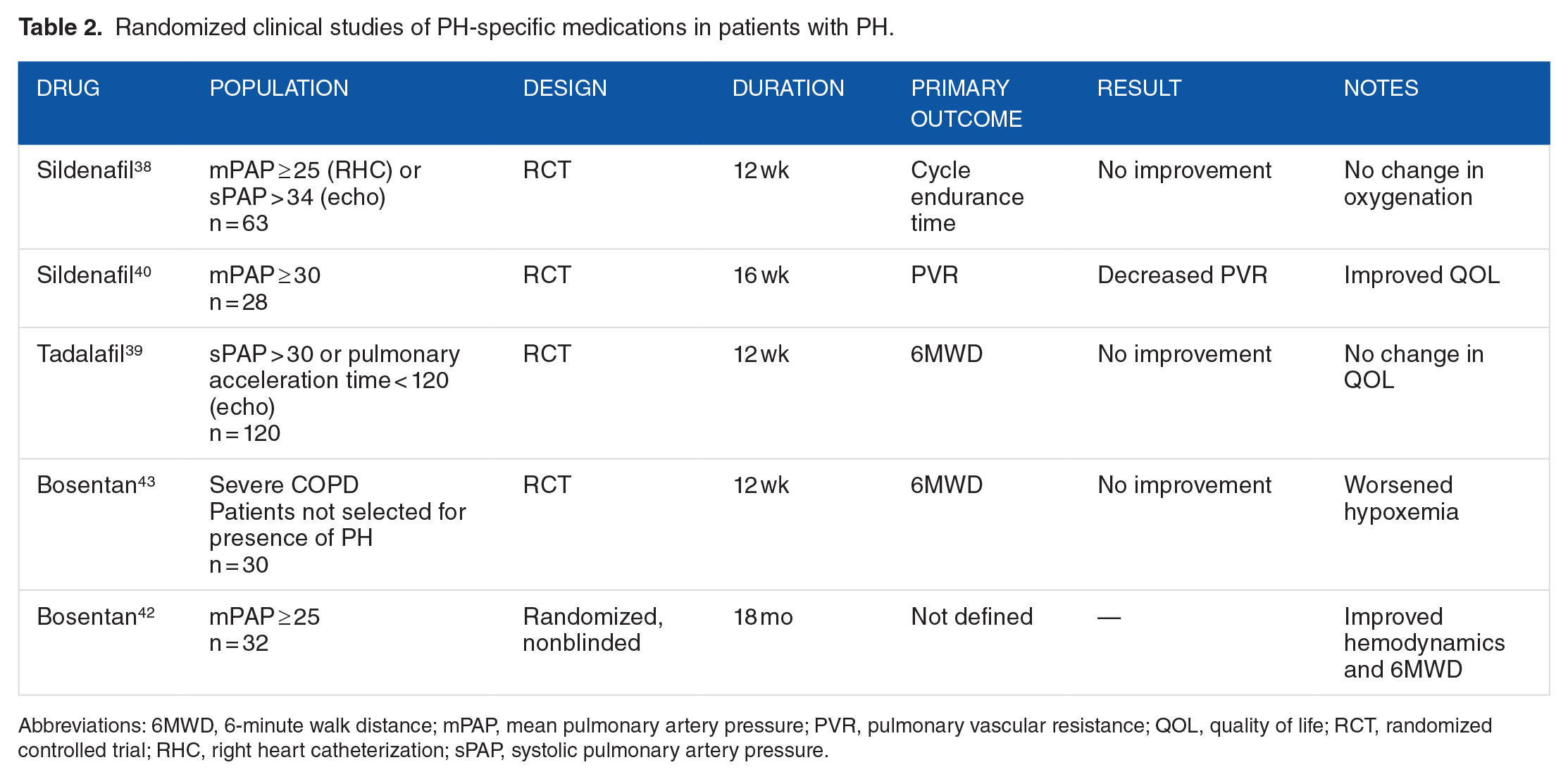
Abbreviations: 6MWD, 6-minute walk distance; mPAP, mean pulmonary artery pressure; PVR, pulmonary vascular resistance; QOL, quality of life; RCT, randomized controlled trial; RHC, right heart catheterization; sPAP, systolic pulmonary artery pressure.
Vascular hypothesis of COPD development and progression
There are now multiple lines of evidence that changes to the pulmonary vasculature are important to the development and progression of COPD, independent of PH (Figure 1). Due to strong preclinical data (detailed below), vascular-targeted therapies may be a novel treatment approach for patients with COPD, although this hypothesis remains to be proven. As mentioned earlier, pulmonary vascular changes are not simply the result of chronic hypoxemia, as an abnormal pulmonary endothelium is demonstrable in mild patients with COPD as well as healthy smokers. Peinado et al 47 studied 41 patients who underwent lung resection (7 nonsmokers, 13 smokers with normal lung function, and 21 mild COPD subjects). They found that the patients with COPD and smokers with normal lung function had thickened intima in their pulmonary arteries, and the mild COPD subjects also had endothelial dysfunction. The same group of investigators discovered that smokers without lung disease and normoxic patients with COPD had an inflammatory infiltrate in their pulmonary arteries. 24 In cigarette smoke animal models of COPD, it is clear that pulmonary vascular changes actually precede the development of emphysema, highlighting that the vasculature is involved early in the pathogenesis of COPD.48,49 Pulmonary vasculopathy developed by 3 months, whereas it took 6 months for histologic changes of emphysema to become apparent. More provocatively, preclinical studies have suggested that insults to the pulmonary vasculature may contribute to COPD development. Chronic vascular endothelial growth factor (VEGF) receptor inhibition in rats led to alveolar septal apoptosis and subsequent emphysema. 50 This is relevant to humans, as emphysema patients have significantly lower VEGF levels compared with normal controls. 51 Finally, targeted induction of endothelial cell apoptosis led to airspace enlargement and inflammation consistent with emphysema. 52
Animal studies of vascular-targeted therapies
Due to the strong preclinical evidence that pulmonary vascular changes occur early in the disease pathogenesis of COPD and may contribute to the development of emphysema and inflammation, multiple groups have investigated vascular-targeted therapies in animal models either to prevent or treat COPD-like manifestations. Use of soluble guanylate cyclase stimulators prevented PH and emphysema development in animals exposed to cigarette smoke, seemingly by preventing alveolar and endothelial apoptosis and attenuating inflammation. 49 Dominguez-Fandos et al 53 studied a cigarette smoke guinea pig model of COPD and found that pretreatment with sildenafil prevented development of PH but did not affect histologic emphysema. An orally available prostacyclin analogue, beraprost, also was demonstrated to prevent inflammation, oxidative stress, alveolar cell apoptosis, and emphysema when given prior to cigarette smoke. 54 Our group was the first to find that intratracheal iloprost, when given chronically in a treatment fashion after COPD model induction, had beneficial effects on systemic inflammation and oxidative stress, as well as airway hyperresponsiveness. 55 Finally, Seimetz et al 48 demonstrated that an inducible nitric oxide synthase (iNOS) inhibitor actually reversed emphysema in a mouse model; it appeared that the drug was causing its effect by inhibiting iNOS derived from lung vascular cells.
Human studies
Despite the excitement generated from these preclinical experiments, no human study has proven that vascular-targeted treatment for patients with COPD is beneficial in the absence of concomitant PH. A small randomized crossover study of 10 patients with COPD who did not have PH found no effect of 4 weeks of sildenafil on 6MWD, but did show worsened oxygenation and quality of life. 56 For future studies of pulmonary vascular therapies for patients with COPD without PH, patient selection will be critical and attention will be needed to issues of V/Q mismatching. As the pulmonary vasculature may be most modifiable early in the course of disease,24,47 patients with mild COPD may be an appropriate patient population, in an attempt to disrupt progression of disease.
Conclusions
In conclusion, pulmonary vascular pathology clearly occurs in the early stages of COPD and may indeed participate in the development and progression of disease in this condition. Pulmonary hypertension is a common manifestation in COPD which is tightly associated with functional limitations and poor prognosis, although specific treatment for COPD-PH has not yet proven to be beneficial. Future studies should focus on the unique phenotype of patients with COPD with out of proportion PH. Experiments in animal models of COPD have demonstrated that vascular-targeted therapies prevent49,54 and treat 55 disease manifestations, but whether this can be translated to patients with COPD, particularly those with mild disease, remains an exciting avenue of research that needs to be proven.
Footnotes
Acknowledgements
The authors are thankful to Professor A Hamid Boulares (Louisiana Cancer Research Center/LSU Health Sciences Center, New Orleans) for his moral support and contribution to the training of the authors of this article.
Peer review:
Three peer reviewers contributed to the peer review report. Reviewers’ reports totaled 352 words, excluding any confidential comments to the academic editor.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study is supported in part by the National Institutes of General Medical Sciences of the National Institutes of Health under award numbers U54 GM104940 (M.R.L.) and 1P30GM106392 (M.R.L.).
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
All the authors contributed equally to the design and writing of this article.
