Abstract
The primary aim of suicidology is to understand the phenomenon of suicide by increasing its predictability and prevention to reduce the suicide rate. However, the rate of suicide remained obstinately high. This phenomenological study explored the different perspectives of 5 suicide attempt survivors and 7 mental health professionals on suicide recovery and its process. Phenomenological methods were used to analyze the participants' lived experiences through reduction, description, and finding the essence. Four essential emergent elements elucidate these perspectives, implying the general status of the current suicide healthcare system, vital in understanding suicide and suicide recovery, namely: (1)
Keywords
Introduction
The primary aim of suicidology is to study and investigate the phenomenon of suicide. Suicidology research increases predictability and prevention of suicidality, reducing the suicide rate. However, despite the large body of literature on suicide, full integration of the different findings about this concept is still difficult, and its complexity and intricacies remain unfathomable despite the existing theoretical models. 1 As such, the rate of suicide remained obstinately high, and predicting suicide behavior stays difficult. 2 According to the World Health Organization (WHO) (2019), suicide adamantly remains a serious global public health issue, as it causes more deaths than malaria, breast cancer, war, and homicide. As suicide attempt is considered one of the major predictive factors of suicide, it is alarming to note that WHO 3 reported 10-25 additional attempts for every suicide death.
The existing measures or models do not have the specificity and sensibility to ensure effective prediction of suicide behaviors. 4 Based on the Lancet Commission’s research studies, it is still observed that the quality of mental health services remains worse than that of those for physical health. The government allots pitiful monetary and developmental assistance for mental health. 5 Yet, WHO 6 has prioritized the reduction of suicide mortality, included as an indicator, of target 3.4.2, in the United Nations Sustainable Development Goals (SDGs), the WHO 13th General Programme of Work 2019-2023, and the WHO Mental Health Action Plan 2013-2030. Attaining these SDGs is a mission that should be shared by all nations. 5 Even though there were efforts made in the previous decades to understand suicide, there is still a wide gap in developing and implementing suicide management programs that are systemic and collaborative.
Conversely, it is believed that suicidal behavior is preventable.7,8 However, the only data-proven preventive measure against suicide is to make deadly tools, firearms, and poisons inaccessible. 7 Other criteria used for suicide prevention generally lack sufficient evidence. 9 Further, persons suffering from suicidality often slip through the cracks of the healthcare systems, with suicide management strategies and interventions not strongly integrated and well-established. 10
By and large, suicidology literature needs to wholistically see the phenomenon. Rather than the treatment being solely focused on reducing symptoms, the recovery-focused movement promotes a more holistic and client-centered approach that upholds and advocates establishing a meaningful life for the clients. 11 Yet, suicidology literature focusing on suicide recovery is scarce but is essential in suicide prevention practices 12 and treatment programs. 13 Relatively few studies likewise deal with the lived experiences of those who, after a suicide attempt, went through recovery, 14 and most of these were conducted in psychiatric and hospital settings which limits their generalizability. 15 Moreover, Bledsoe et al 16 posited that while recovery is generally for mental health treatment, suicide interventions can be strengthened with the core elements of the recovery construct. Thus, like a missing piece in the puzzle, the study of suicide recovery may give form and provide a broader picture to suicidology literature and unearth other information to make suicidality more preventable and manageable.
Inflorescence Model of Suicide Recovery
The present study is anchored on Bautista and colleagues’ Inflorescence Model of Suicide Recovery (IMSR) (2022), which elucidates the suicide recovery process that suicide attempt survivors go through. It is the process of traversing the path, from the state of wanting to die (or the state of brokenness or “buriedness”) to the state of flourishing in life (or the state of sustaining recovery), by which crises, manifested by suicidality behaviors, were overcame through taking recovery actions to allow the needed values to surface and attain recovery. The whole process of suicide recovery in the Inflorescence Model suggests the foci and targets of a recovery-focused suicide management program. As such, this phenomenological study was primarily conducted to develop and propose this suicide management program as a means to improve the existing suicide healthcare system. This program, in turn, emphasizes the value of addressing the identified fragmentation or gap in the suicide healthcare system since the collective failure of this system results in the immense cost of “losing human capabilities and experiencing avoidable suffering”. 5
Method
Design
Our study used Moustakas’ 17 method of transcendental or psychological phenomenology to describe the participants’ lived experiences of the phenomenon of suicide recovery and its process. The overall essence of this phenomenon is based on the textural description of the participants’ experiences, the structural description of their experiences, and the triangulation of both the perspectives of suicide attempt survivors and mental health professionals. 18
Participants
A total of 12 participants were interviewed to explore their perceptions about the phenomenon of suicide recovery to conceptualize a recovery-focused suicide management program. The 12 participants are 5 suicide attempt survivors and 7 mental health professionals consisting of 2 guidance counselors, 3 clinical psychologists, and 2 psychiatrists. All participants secured informed consent and, without remuneration, participants voluntarily joined in the interviews. Table 1 shows the descriptive characteristics of the participants.
Descriptive Characteristics of Study Participants (N = 12).
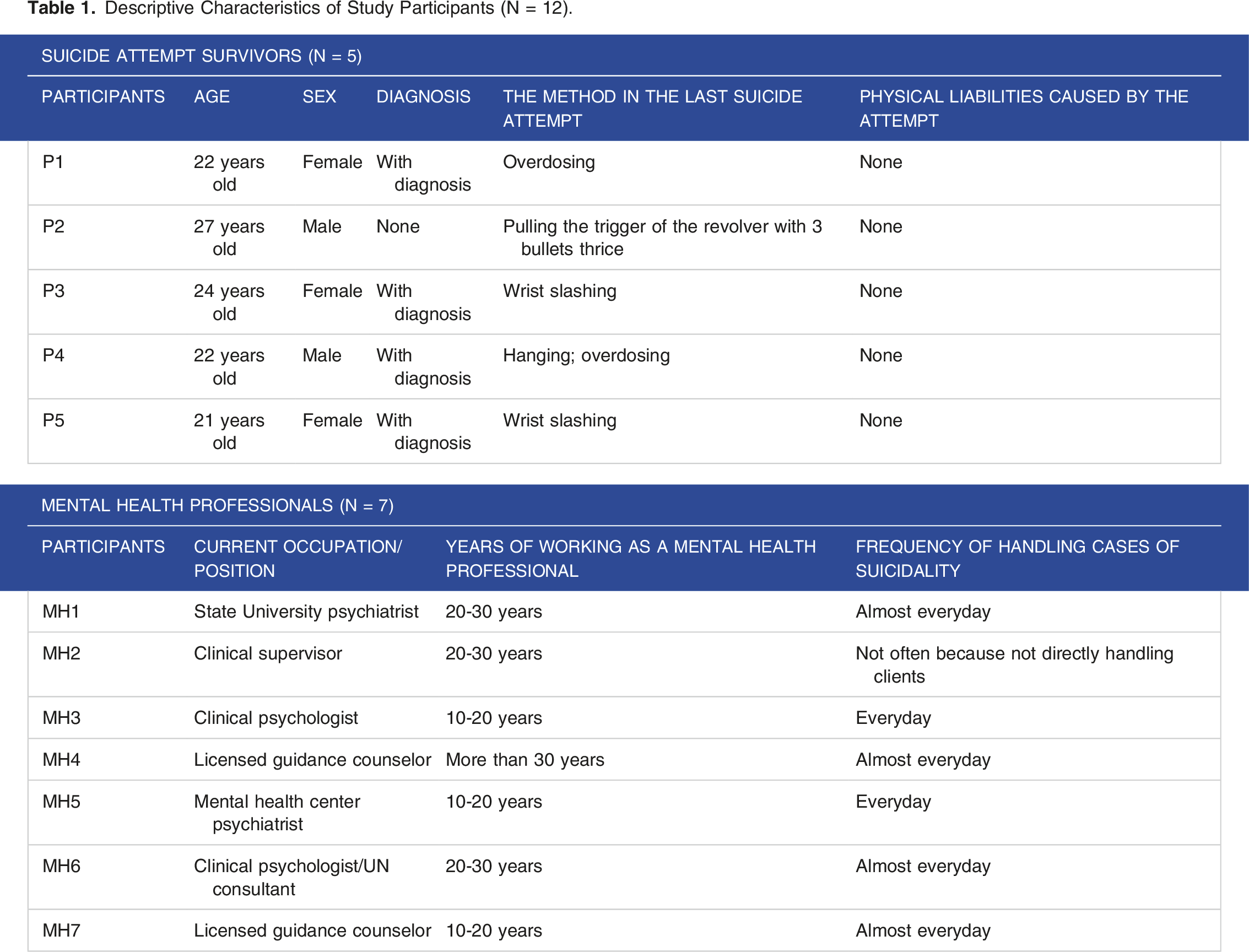
Research instruments
Robofoto
The Personal Information Sheet (PIS) obtained participants’ socio-demographic information. Specifically, it asked to know the age, sex, mental health diagnosis, method used in the last suicide attempt, and physical liability caused by the attempt from suicide attempt survivors; and for current occupation/position, years of working as a mental health professional, and frequency of handling cases of suicidality from mental health professionals.
Aide Memoire
The present study developed and utilized a semi-structured interview guide to probe into the participants' lived experiences of suicide recovery. On the one hand, for suicide attempt survivors, it tried to explore 5 elements or layers of human experience that pertain to their suicide recovery, namely: (1) suicide behaviors before and after a suicide attempt; (2) experienced changes that characterize suicide recovery; (3) experiences and perception about the process of suicide recovery; (4) psychiatric and psychological interventions and treatment; and (5) factors that contribute and hinder their engagement in their unique recovery process. On the other hand, the aide-memoire for mental health professionals explored: (1) their experiences with clients' suicide attempt/s; (2) their experiences with clients’ suicide attempt aftermath; (3) factors that lead to their clients’ suicide recovery; (4) their experiences with clients’ suicide recovery; and (5) their perception of suicide recovery.
Suicide Recovery Ability Scale
The SRAS developed by Sun et al 19 has satisfactory psychometric properties in measuring suicide recovery ability. It is a 15-item questionnaire that measures 3 factors of suicide recovery, namely: (1) Self-awareness of the value of life; (2) Utilization of coping strategies; and (3) Efforts being exerted to live a normal and satisfying life. It also includes a global scale to show an overall picture of such an experience. Item-total correlations were greater than .3 and Cronbach’s alpha and the test-retest reliability scores for the global scale and the SRAS subscales were all above .7.
Suicide Probability Scale
SPS was developed by Cull and Gill 20 and is a 36-item self-report that measures suicide risk designed to be used with adolescents and adults. It has 4 sub-scales, namely, Hopelessness, Suicide Ideation, Negative Self-Evaluation, and Hostility. It makes use of a 4-point Likert scale ranging from “None or little of the time” to “Most or all of the time.” A high suicide probability score reflects a high risk of suicide. SPS was found to have a high level of test-retest reliability, which had coefficient scores of .92 and .94 over 3-week and 10-day intervals, respectively. The internal consistency of the subscales falls within the ranges from .62 to .98. The validity of the instrument is considered to be good. 21 The SPS was also used as a screening tool in selecting the participants.
Procedure
Data collection started after securing ethics approval from the University of Santo Tomas Graduate School Ethics Review Committee. The robofoto was used to gather the participants' socio-demographic profiles and warrant that our study follows the set inclusion criteria. Standardized screening instruments (SRAS, SPS) were also administered to assess prospective participants’ suicide recovery ability and suicidal probability. Those who scored high in SRAS and low in SPS were qualified. However, from a sample pool of 25 suicide attempt survivors, only 5 participants were randomly chosen and were invited to be interviewed in this phenomenological study. Seven of ten identified mental health experts accepted the invitation, which was based on their expertise, years of experience, and recognition in the mental health field, were interviewed for this phenomenological inquiry. Before starting the interview sessions conducted virtually during the pandemic, informed consent was sought. Each interview lasted for an average of an hour.
The aide-memoire was used to guide the interview, but prioritized spontaneous conversation; clarifying and asking for additional information were made to facilitate the discussion.
Data analysis
Data were managed and organized by converting transcripts into text data. Reading the whole database and memoing were done to identify anchors and phenomenal referents. Data were analyzed by using the processes of reduction, description, and finding the essence. 17 In the process of epoche, or reduction, the participants’ narratives were scrutinized and analyzed to form codes or categories. Building detailed descriptions presents the essence or meaning of the phenomenon as narrated by the participants. Lebenswelt, or finding the essence, refers to the analytical processing of themes and uncovering the core meaning of the participants' lived experiences. Dendrograms, or clustering of themes, were through cool analysis (culling out, sorting, and categorizing) and warm analysis (thematizing and finding essence) of the gathered data. Inductive and deductive methods were used for appropriate thematization.
Moreover, the triangulation of data from suicide attempt survivors and mental health professionals allowed the exploration of different perspectives on suicide recovery. It provided a basis for a recovery-focused suicide management program. Peer debriefing and member validation were employed for consistency and to ensure the truthfulness and trustworthiness of the theory.
Findings
Data analysis yielded recognizable features that collectively characterize the different perspectives of the participants. Four essential elements emerged that elucidate these perspectives, vital in understanding suicide recovery, namely, (1)
Figure 1 is the simulacrum showing the elements that emerged in this phenomenological study were plotted to show their interplay with suicide recovery. The simulacrum illustrates that central to the suicide management program is its procedural elements. One integral element is suicide recovery rehabilitation, which encompasses techniques and strategies that target to address the suicidality behaviors and facilitate suicide recovery actions through enhancement of recovery values to be able to resolve crises identified in the suicide recovery process, thereby overcoming suicidality. Phenomenological model of the different perspectives on suicide recovery phenomenon.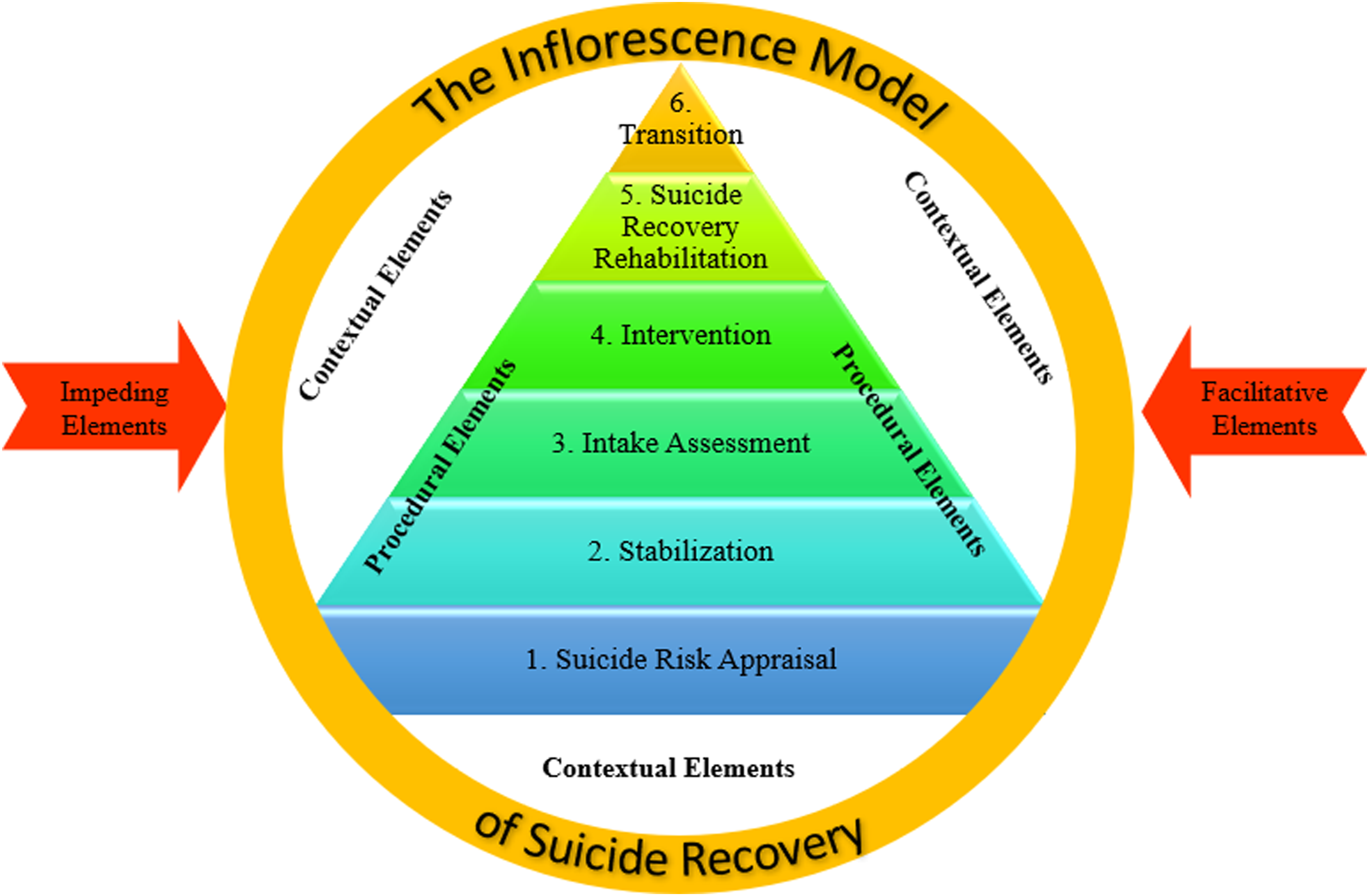
Contextual Elements
As one of the conditions for further study in the Diagnostic and Statistical Manual of Mental Disorder (DSM)-5-TR; 22 still, suicide behavior disorder (SBD) continued to be a puzzle. Hence, the contextualization of the phenomenon of suicide recovery is deemed essential for better understanding the concept and establishing or clarifying its constructs. Such contextualization is integral in viewing suicidality wholistically.
However, if the 2 groups of participants, namely, the suicide attempt survivors, and the mental health professionals, differ in their understanding of suicidality, depending on their own experiences, exposures, and specializations, suicide management or treatment may not be responsive or effective. Thus, the findings on the contextual elements are all about the participants' perception of (1) suicidality; (2) characteristics of suicidality; and (3) suicide recovery.
On suicidality
Both suicide attempt survivors and mental health professionals view suicidality as (a) a pattern of overthinking, intense emotionality, and destructive behaviors; (b) an escape from painful experiences, translating the emotional pain into a physical one; (c) a cry for help or a means to get the attention of the people around them without considering the fatality of their suicide acts; and (d) an expression of hopelessness. As narrativized: I bottled it up, and, after a year, I exploded. I realized that when I did these during the lowest time or I was in a negative state, I interpreted it differently, which consumed me. When I get hurt, I overthink to the extent of getting drowned with my thoughts. I got so frustrated with myself that I needed to turn to physical means. (P2)
However, suicide attempt survivors disagree that suicidality is solely a symptom of a mental health disorder; yet, most mental health professionals, particularly psychiatrists, perceive otherwise. As the participants expressed: I was diagnosed with a mental health disorder. The medications helped me in the stabilization of my symptoms. However, I felt that this treatment was not adequate to understand the factors that caused my mental illness. (P1) Probably because I'm a psychiatrist, I look at it from the health side. As a phenomenon, it's, for me, the worst complication of any mental health problem. Even though there are a lot of studies that say not all suicidal behaviors are due to a mental health problem, I still believe that much of it is due to mental distress. For me, it's the worst complication, but there are also several factors; research has always said the lack of connectedness has always been a factor… but for me, it's a health issue; it's a complication of a health issue. (MH1)
Suicide attempt survivors believe that suicidality means more than just a symptom of any other mental health disorder; however, most mental health professionals believe that it is solely a symptom.
On the characteristics of suicidality
How the participants perceive the attributes of suicidality contributes to how they contextualize suicide recovery and its process. How they characterize or describe the manifestations of suicidality influences their conceptualization of specific suicide management programs. For mental health professionals, suicidality is an expression of worthlessness, hopelessness, and helplessness, and a manifestation of a mental health disorder, as described in the narration: The typical thought processes of youths suffering from suicidality are affected by feelings of worthlessness, feelings of hopelessness, feelings that they can't go on, or being stuck wherever they may be in life. Suicide risk assessment usually finds manifestations of depression or sadness, a sense of hopelessness, and helplessness. (MH6)
Furthermore, mental health professionals cannot agree on some characteristics of suicidality in the current milieu. As they narrated their different perspectives: Actually, at this point, my observations of these youths have diversified over time. Before, the youths suffering from suicidality were those who went to the clinic, typically looking down and sad. They were the ones who were crying and not doing well academically or already failing. Or, when working, they were not functioning as they were doing. Now, some clients enter the clinic dressed very well and even look happy. I even encountered clients who, at the start of the session, were very jolly; then, as the session progressed, they suddenly disclosed their ideations. For me, there is diversity already. Suicidality is experienced across ages, genders, socioeconomic positions, and religions. Before, those who exhibited suicidality were those who lost faith, but now even those who are believers or devoutly religious suffer from it. They even prayed to God to forgive them. So, I use the term diverse to describe this. (MH7) There is not much difference between then and now in terms of outpatient consultations. But in terms of suicidal thoughts and attempts, like post-hospitalization, they are increasing. But I don't think it's because the cases are increasing. I don’t have proof of this. I also think because the services are available and are free, therefore, they consult. But I cannot say that they are increasing in number because before they didn't get referred or they didn’t seek consultation because they thought that it was okay. After all, they thought it was non-suicidal anyway. (MH1)
Overall, the participants unanimously agreed that suicide is still not fully understood. As the participants verbalized: … it’s also because we don’t do a lot of psychological autopsies with people who die of suicide. There are already good signs, but we have yet to do a longitudinal study regarding repeated suicidal behaviors because we don’t know when it’s going to relapse. (MH1)
In this context, suicide is yet to be fully understood because both suicide attempt survivors and mental health professionals expressed varying perspectives on suicidality. More so, mental health professionals do not have a general basis on the trends of the characteristics of suicidality.
On suicide recovery
The participants’ stances about suicide recovery are important in how they execute and follow its process in suicide treatment and management. Suicide attempt survivors view suicide recovery as a unique process for each person, as narrativized: Progress isn’t linear. Everyone has their way of recovery but we have to remind ourselves that we need to stick with our choices... My concept of recovery is it depends on the person. You open up yourself to recover… It’s a choice. It’s like spiritual. It's a choice. It’s responsibility. (P25)
Both suicide attempt survivors and mental health professionals were less aware of suicide recovery and its process. Mental health professionals conceded that suicide recovery is not a popular concept, particularly in managing suicidality. All of them observed that it is in their practice to monitor improvements and keep track of the progress; however, the process of suicide recovery or specific suicide management plan is not being followed. More so, suicide recovery is not explicitly part of the treatment goal or focus. A mental health professional expressed their unfamiliarity with the construct as they expressed: In the professional circle, I seldom encountered suicide recovery being talked about. What is often talked about is suicide, interventions, and even first aid, but not recovery. I don’t hear about it often. I mean, we do it, we practice it, we take care of our patients toward recovery, but it’s not usually discussed in the circle. It’s something that has been missing in practice. When asked if there are suicide recovery programs being implemented, my answer is none because we are into first aid, suicide intervention, safety plans, mental health treatment, and other management strategies, but we never really have recovery planning. I can see now that suicide recovery is something that hasn't been talked about, something that is missing in the puzzle. It seems that we stopped at addressing suicide or providing first aid. Again, we do it, we do it in different ways, and we've been practicing it, but I think we haven't focused so much on it; we need to pay more attention to it; and I agree that we need to have an approach, a model, or even a course of practice to do it. We even need to advocate for it because, in our society, we don't talk much about suicide, and perhaps this is the reason why we fail to see this aspect, which is suicide recovery… Suicide recovery is a reinforcement of life, and I realized that others, not only mental health professionals, should see recovery. I think things would change a great deal in terms of their perception and management of suicide, particularly those that are help-seeking behaviors. I think it would have a big influence on that. (MH3)
By and large, the contextual elements describe how the participants perceive the phenomena of suicide and suicide recovery. Putting these elements in one picture may aid us in seeing where the participants come from and identifying the gaps among these perceptions. Moreover, suicide recovery is not very clear even for mental health professionals. Yet, pertinent to this study are the contextual conditions of the youths who suffered from suicide and went through recovery. Thus, mental health professionals need to consider these youths’ perspectives about their suicidality rather than view it solely as a symptom of mental health illnesses.
Furthermore, if suicide recovery is not apparent, or worse, a concept that mental health professionals do not believe in, interventions will only revolve around reducing suicide risks, and suicide recovery will remain unexplored and unknown in managing suicidality. What is lost in the healthcare system without suicide recovery are the opportunities to be fully aware and hopefully grasp the concepts of suicide recovery action to make the specific phases of suicide recovery targets or foci of suicide interventions.
Facilitative Elements
Knowing the various factors that facilitate or lead to suicide recovery not only helps to understand its phenomenon better but also helps conceptualize the unique recovery path for each client. The suicide recovery process can be achieved by reconciling the dilemma experienced in each step. These dilemmas are better coped with when these facilitative elements are identified. To wit, the facilitative elements or factors leading to suicide recovery should be recognized to assist the youths in attaining their inflorescence. They were unanimous in identifying these conditions to be integral in recovering, namely, (a.) social and emotional support; (b.) resilience; (c.) help-seeking behaviors; and (d.) keen observation of and objective awareness of suicide recovery behaviors to implement a safety plan.
It was found that an integral facilitative element in suicide recovery is the social and emotional support provided to suicide attempt survivors. One of the clinical psychologists shared: I'll go back to emotional support. It is a big help that they could feel that there are other people out there who are willing to help. The feeling of intense helplessness is alarming, but when they start realizing and seeing that there are other people for them or even having their friends, it is a big driving force towards healing, recovering, or even stopping them from attempting again. When they seek therapy and they have someone to speak with, they feel lighter. In some cases, when they have thoughts of suicide, and they can talk about it, their emotions de-intensify, and the risk disappears. So, I think a big factor is social support, which is an external factor. (MH3)
Focus on building resilience was found to be a facilitative element essential in bouncing back from brokenness and starting the recovery process. The participant emphasized: Being resilient helped me exert efforts to be fully mindful of what I felt. Before, when I looked at the problem, it was like the end of the world. Now, it's like going through it only, and the problem will also end. It's always baby steps because appreciating the little things can make you like what is innate in you. When there is a problem, there are times when I just let it be, or I try to find other ways to solve it positively or do it more proactively. It’s against yourself, and you have to train yourself every day. (P3)
Asking for help or seeking professional help was found to be a protective factor from suicide and leads to suicide recovery. As a mental health professional said: When they realized that they already needed professional help, that was when they decided to start their recovery. (MH6)
Most significant is when the suicide attempt survivors initiate to implement their safety plan, by increasing their coping means, enhancing faith, and complying with treatment and follow-ups. As a mental health professional expressed: It is already clear that he wants to recover, so he initiates his suicide safety plan. The early thoughts, early attempts, or early plans do not have a suicide safety plan. It changes every so often. It does not stay that way all the time. There are instances when a person will consult that he has already changed his suicide safety plan. But even if they have the thoughts that they have recovered, the indicator is that they want to get out of that thought. So, they do their safety plan, and they come to figure out how to implement their safety plan. So, the point is, even if they are thinking… I don’t label this person as if they still with the disease; yes, I mean, he is still at risk, but I would still see something positive there in the fact that he has a safety plan. For me, that is an indicator of recovery, but this is not a full recovery yet; this is only the start, but at least you have a chance. (MH1)
Thus, as unanimously reported by all participants, a recovery-focused suicide management program should include stimulating, enhancing, and creating an environment that is facilitative of these suicide-recovery elements.
Impeding elements
The impeding elements are the factors that hinder or slow down suicide recovery. Identifying these factors that contribute to suicide aids in contextualizing suicide recovery and, subsequently, in reducing suicide risk by conceptualizing and implementing an evidence-based suicide management program that addresses the impeding elements of suicide recovery. Both the suicide attempt survivors and mental health professionals agreed that the impeding elements include: (a) being afraid to ask for help, and lack of social and professional support; (b) family problems; (c) feeling of being a burden; (d) resistance or lack of commitment to the treatment process; (e) academic stress; and (f) history of trauma or abuse.
In connection with asking for help and social and emotional support as facilitative elements, not asking for help prevents them from relating with significant persons; thus, impeding them from receiving social and professional support. On one hand, when suicide attempt survivors asked for help and got engaged in their treatment and safety plan, fewer mental health admissions, emergency department visits, and suicide attempts were experienced. However, on the other hand, a lack of social and professional support leads to suicidality, as the participant expressed: When I was in that hole, I was afraid to ask for help. After my attempt, I was ashamed of how weak I was for doing it. I feared that I would hear this from others. Thank God, my parents kept reaching out to me. They enrolled me in therapy even though I did not believe in it before. (P2)
Family problems are very powerful triggers of suicidality. Both suicide attempt survivors and mental health professionals reported that the family plays a very important role in recovery. Family problems that are not resolved or when they worsen impede one’s process of healing, as a participant shared: I also see problems at home due to the mental health concerns of the youths. The family, oftentimes, does not believe in this kind of health problem, and they do not give support… stigma at home can be destructive. (MH7)
Most mental health professionals shared that these youths reported feelings of being a burden to others. To end their lives is to stop being a burden to others. Suicidality required them to seek help and doing so was perceived as a burden by suicide attempt survivors. This was narrativized: I bottled up all my feelings because I did not want to be a burden to others. Looking back, I dreaded that feeling when I thought of being a burden. To describe, it was a heavy burden that led to self-hatred. I hated myself for being a burden or just the thought of it. (P2)
Engagement in the process is an important step in suicide recovery; hence, resistance or lack of commitment to recovery is considered an impeding factor. As verbalized: The other hindrance that I see is when the clients resist doing their part in the recovery process. This is manifested through behaviors that include non-compliance with therapy or not attending therapy sessions regularly. Most of the time, it is only when they have problems that they seek therapy sessions. This prevents them from sustaining their progress in their therapy. Moreover, their lack of commitment to getting better oftentimes leads them to neglect their part in their recovery. This leads them to depend on others to make the desired changes in their lives. This slows down or even stops their progress. (MH3)
Furthermore, mental health professionals pointed out that youths are triggered to suicidality due to academic factors. As the participant narrated: The reasons for suicide varied but mostly academics. They reported that when they could not do their tasks in school, they felt they were a failure. They were afraid of how their parents would react to this. (MH7)
History of abuse is emphasized to contribute to suicidality. The strongest environmental risk factor in their childhood associated with suicidal thoughts and behaviors is maltreatment or abuse. The participant shared: In addition, a history of abuse contributes to suicidality. When they suddenly remember a history of abuse that they never even thought existed before. It’s like, all of a sudden, they remembered something, and it was probably something that triggered them, which is usually the behavior before suicide. Or when they became exposed again to trauma, and so she may wish to have died before, even if she may not exactly experience violence again, at this time, youths with suicidality would tend to wish that they should have ended their life before. (MH1)
All in all, the impeding conditions to suicide recovery are the risk factors that should be reduced. Suicide stigma has always been why youths do not ask for help whenever they experience suicidality. This can also be combined with the dread of being a burden to others. When they feel hopeless and helpless, their motivation to recover dwindles, and their commitment to the process becomes questionable. History of abuse leads to and complicates suicidality. These triggers and their recurrence can disrupt the suicide recovery progress. Hence, in conceptualizing the suicide management program, relapse prevention should include steps to address these impeding factors.
Procedural elements
These elements encompass the recommended suicide management strategies and interventions from the youths who survived suicide attempts and the mental health professionals. These elements were plotted in a paradigm that shows how important it is that we target recovery, keep track of the recovery process, and gatekeep the sustenance of suicide recovery; thus, focusing on recovery is another tool to address the increasing prevalence of suicide. Six procedural steps that would explicate the paradigm of recovery-focused psychological intervention and suicide management, namely: (1) Suicide Risk Appraisal; (2) Stabilization; (3) Intake Assessment; (4) Intervention; (5) Suicide Recovery Rehabilitation; and (6) Transition.
Suicide risk appraisal
Immediately after the suicide attempt, an initial suicide risk appraisal is significant to know the level of risk. Suicide risk appraisal is necessary because it will dictate the course of action and suicide management techniques that are appropriate for suicide management. A mental health professional shared: All attempters should undergo clinical and rapid suicide assessment by an expert mental health worker or psychiatrist. Many of them remain clinically depressed and still suicidal. (MH6)
All clients need to be screened for suicidality, the current level of suicide risk, mood status, and the operational risk and protective factors.
Stabilization
After a suicide attempt, stabilizing the emotional and psychological distress has emerged from this phenomenological inquiry. Often, this distress was the trigger for the suicide attempt. Mental health professionals reported that stabilization strategies include suicide first aid and immediate implementation of a safety plan to assist the clients in identifying a list of coping strategies that they can use in a suicide crisis. As narrated: Our center’s immediate intervention for suicidality is developing an immediate intervention of a safety plan. When they expressed or have identified suicide risk, we immediately implement the safety plan, which is also integrated and regularly checked during the whole intervention course. In terms of a specific intervention, what we must follow is the Suicide First Aid for Filipinos, which is more of an immediate response. (MH1)
Based on these findings, it is helpful to integrate into the stabilization process of suicide attempt survivors the recovery support plan that necessitates collaboration with family members, friends, and other significant persons.
Intake assessment
This procedural step was deemed helpful to allow a comprehensive assessment of the contextual, facilitative, and impeding elements in conceptualizing each client's unique suicide recovery process. As a mental health professional verbalized: This means that we have parameters to follow. We need to see important parameters, such as the mentality and intentions, post-suicide gestures, accessibility of suicide means or weapons, and level of risk... Aside from the suicide risk appraisal, suicide is just a symptom of a mental health problem. So, it doesn't mean that when the person is suicidal, they are already depressed. You look at the totality. We need to assess them to better manage the condition. We need to know the patient's history of suicide, the main diagnosis, relational dynamics, causes of suicide, and conditions to consider for suicide safety monitoring. (MH5)
Mental health professionals put importance on case conceptualization. Nonetheless, it is noteworthy in this procedure that the suicide attempt survivors and mental health professionals had different stances. Very significant is when mental health professionals solely perceive suicidality as a symptom of mental health illness, thus, case conceptualization and diagnosis may not be holistic and accurate.
Intervention
In terms of strategies that indicate suicide management and intervention, it was found that there was a minimal number of programs being implemented. The emphasized therapies and approach did not directly address suicidality, more so, suicide recovery, but are included in mental health problems’ treatment plans. As a mental health professional shared: … but, for the more long-term interventions, we do not have a specific program for suicidality. Our interventions target the cause of why the person had suicidal ideations or attempted suicide, which is, for example, depression. So, the focus is more on depression or other problems. This means that the main protocol for suicide intervention is a safety plan, which is modified periodically. The clients appraise their safety plan to align it with therapy and identify the skills developed over the sessions. The first techniques taught are basic relaxation and calming exercises… social skills, and focusing on family and friends. Another technique that can be used as an intervention is making use of psychoeducation. (MH3)
Mental health professionals have different stances on medication. For some, medication is not always an immediate course of action but, for others, medication is automatically given; however, they agree that effective treatment involves pharmacotherapy, psychiatric interventions, and different types of psychotherapy, such as DBT and CBT-SP, to address mental health concerns and other factors surrounding suicidality to facilitate the suicide recovery process to take place.
Suicide recovery rehabilitation
This is the core of the suicide recovery procedural element. This study posits that on top of the interventions given to address mental health concerns associated with suicidality, and to focus on the process of suicide recovery, rehabilitation should be provided in the aim of restoring health by following the IMSR process.
23
This was emphasized by suicide attempt survivors, as one of them shared: Suicide recovery is not easy. It is not linear. It seemed that I lost something; I was feeling weak and lacked motivation. I was not the same one who could brush off my negative feelings. It was my dark days as if buried. I felt I had lost the will to live, and I did not like it. I did not like myself because of that. So, I studied what I felt. When I could not do it by myself anymore, I sought help. What I learned was I needed to identify the factors that caused what I felt and how to handle them. This was not easy because I had to fight demons in my head. I constantly remembered my painful experiences, and they were not easy to let go of. However, things changed when I went back to myself and helped myself, one step at a time. I got to be mindful of what I felt, and the symptoms: bodily and behavioral. It was not easy; there were a lot of bumps. But the more I was engaged in the process, the more that I was making sure of my healing process. Recovery was gaining back my life. (P3)
As the participants emphasized, although, with some perplexity, suicidality is a manifestation of a lost will to live or lost hope. Triangulation of the narratives of suicide attempt survivors and mental health professionals yielded this step in the suicide management program. According to the narratives, suicide recovery rehabilitation should include methods, techniques, tasks, and activities to facilitate the 5 steps of the IMSR. It should aim to resolve the crisis in each stage of the suicide recovery process by monitoring the suicidality behaviors and promoting suicide recovery actions.
Transition
The last procedural step focuses on (a) relapse prevention; and (b) re-entry to the community. Possible relapse triggers are inevitable and the youths suffering from suicidality are prone to it. Hence, the participants expressed their perceptions about managing suicide and sustaining suicide recovery .
Relapse prevention
Relapse prevention is essential before the end of any intervention program because it is inevitable that the clients encounter difficulties and experience problems after therapy. Skills to prevent relapse include: (1) seeking help right away, (2) enhancing problem-solving skills, (3) facilitating social support, and (4) psychoeducation about suicide recovery. At the end of the suicide management program, the clients should know that they improve their help-seeking behaviors whenever they encounter some warning signs. As they expressed: There are many clients who, through therapy, became better and finished therapy; but, in the course of life, they encountered some problems again. When they go back to therapy, we worry about their mental health concerns, but when they were asked how they were responding to their problems, they would express that they were struggling, but since they could cope, they went to therapy to ensure that they carried on. They realized and expressed that they could do something. They went back to therapy to be proactive about it and be more equipped to handle things. (MH7)
Re-Entry
This is the procedural element that suicide attempt survivors have recognized as essential in preventing relapse. If mental health professionals work together to weave these mental health support programs into a collaborative, coherent, and comprehensive system, re-entry may be easier for these survivors. As a mental health professional expressed: Re-entry to the clients’ community becomes more accessible and safer when society is educated about suicidality and other mental health problems. The programs for suicide awareness for teachers, school staff, and parents help build their sensitivity and stigma reduction. Postvention should also be well-established so that the act of suicide is not sensationalized. A suicide-informed approach should be observed in dealing with a mental health crisis. (MH3)
The procedural elements are necessary for conceptualizing the suicide management and intervention program. The perceptions of mental health professionals and suicide attempt survivors were recognized to have gaps, thereby influencing how mental health professionals may handle each client's supposedly unique suicide recovery process. The procedural elements that emerged in our study were presented to show that the suicide attempt survivors have their perceptions about the steps or procedures of suicide management they observed and experienced.
Discussion
Suicide research studies are conducted to understand better and predict suicidality. Suicide management strategies and intervention programs need to be improved and implemented in a methodical and collaborative healthcare system to better handle suicide and help decrease suicidality. 10 Suicide prevalence remained persistently high, and given the adverse effects of the COVID-19 pandemic, the suicidality rate is anticipated to increase. The existing milieu in suicide management shows that even though youths consulted mental health professionals, some still slipped from the care of treatment and got caught in the trap of failed recovery. These gaps characterize a fragmented healthcare system that results in unresolved suicidality even for those undergoing treatment, 24 thus, posing a challenge to the recovery of suicide attempt survivors, who are increasing in number.
Despite some similar general viewpoints, the gaps in the healthcare system on suicidality may originate from the differences in perspectives of mental health consumers and carers. Based on their stands, 4 elements of suicide recovery influence its process, namely: (1)
As suicide continues to be a puzzle, synthesizing the contextual elements of suicide and suicide recovery may help us better understand this condition. Moreover, suicide recovery is not very clear even for mental health professionals. Their contextualization of the phenomenon, particularly if they vary, impacts how they handle suicidality, what treatment programs the mental health professionals choose to implement, and the recovery process suicide attempt survivors go through. Further, pertinent to this study are the contextual conditions of suicide recovery from the youths who suffered from suicide and went through recovery. However, despite how mental health professionals contextualize suicide and suicide recovery phenomena, the consumers' needs and concerns are the prime considerations in the treatment planning. Even if mental health professionals looked at suicidality as solely a symptom of mental health illnesses, the approaches to be utilized in managing suicidality should be aligned with where the consumer is coming from.
The challenge to mental health professionals is that their consumers do not see their suicidality as a symptom of mental health illnesses. This is validated by studies that postulate that treating the underlying mental health diagnoses does not always resolve suicidality.25,26 Also, notwithstanding that there is a link between suicide and mental disorders as most mental health professionals contend, there are still many suicides that happen as an impulse or occur in the absence of a mental disorder. Furthermore, if suicide recovery is not apparent to, or worse, not believed in by mental health professionals, interventions will only revolve around reducing suicide risks, and suicide recovery will remain unexplored and unknown in managing suicidality. In this context, suicide is yet to be fully understood. However, the complexity of suicide is rooted in the intention of a person to deliberately kill oneself; 27 and escape the experience of (a) psychological distress; 28 (b) suffering or psychache; 29 (c) severe sense of psychological pain; 30 (d) aggression toward the self; 31 (e) deep emotional pain; 32 (f) hopelessness and helplessness; 33 and (g) pressurizing turmoil. 34 Also, the complexity of this phenomenon lies in the different dimensions, such as social, cultural, and psychological aspects, that interplay to increase or decrease the risk of suicidal behavior, which, in turn, diversified and changed the characterization of suicidality. Noteworthy is with still high suicide stigma, it is still difficult to promote help-seeking behaviors; 35 thus, if the suicidality rate increases despite high suicide stigma, then, such increase may be due to increasing cases.
What is lost in the healthcare system without suicide recovery are the opportunities to be fully aware and hopefully grasp the concepts of a suicide recovery action plan, namely, (1) acknowledging brokenness and vulnerabilities; (2) confronting their sources of pains; (3) owning oneself; (4) identifying life anchors; and (5) being fully aware of one's unique suicide recovery process. 23 As such, there is a need to give suicide recovery process a spotlight in the treatment so that it can be placed in the right position in the puzzle.
The facilitative elements or factors leading to suicide recovery should be recognized to assist the youths in attaining their inflorescence. They were unanimous in identifying these conditions, which corroborated with the following authors, namely, (a) social and emotional support;14,36,37 (b) resilience; 38 (c) help-seeking behaviors;14,39,40 and (d) keen observation of and objective awareness of suicide recovery behaviors.4,14,41 However, great strides have already been accomplished in identifying the best practices for assessing these elements for suicide prevention in the past decade,25,42 but treatment and management goals should include following the suicide recovery process, rather than merely focusing on symptom-reduction. 11
Our phenomenological study agrees with the Zero Suicide Initiative, which disseminates best practices in suicide care by promoting evidence-based, suicide-specific interventions, and intensified care, monitoring, and engagement during crises. 43 However, our IMSR adamantly recommends recovery-focused or recovery-specific interventions that aim to assist suicide attempt survivors in going through the recovery process. Hence, identifying the facilitative elements and enhancing these conditions may aid the suicide attempt survivors in resolving the suicide recovery conflicts, namely: (1) assimilation (taking in and understanding one's suicidality and recovery) vs desolation (emptiness and unworthiness); (2) adjustment (making changes to balance conflicting needs) vs disheartenment (discouragement or faltering in the recovery); (3) self-love (taking care of self compassionately) vs dejection (sadness or depressed state); (4) grounding (connecting to reasons of recovery) vs doubt (loss of conviction on suicide recovery); and (5) sustainability (actively participating in maintaining recovery) vs desperation (hopelessness and defeat). 23 It is believed that these crises are overcome by acknowledging and managing these predominant suicidality behaviors: (1) resistance, (2) rumination, (3) rejection, (4) rootlessness, and (5) reproach. In doing so, the suicide recovery value emerges in each stage, namely, (1) acceptance; (2) bravery; (3) compassion to self; (4) determination; and (5) engagement. It is hoped that the facilitative elements and varying perspectives will be carefully woven into the treatment, creating an environment susceptible to suicide recovery.
Similarly, the impeding conditions to suicide recovery are the risk factors that should be reduced. These factors reinforce the suicidality behaviors and intensify the crises. These results corroborate the study of Pisani et al. 42 which posits that comprehensive risk assessments should identify both the risk and the protective factors that point out possible fluctuations in the stability of the person’s mental health. Hence, in conceptualizing the suicide management program, relapse prevention should include steps to address these impeding factors. Relapse prevention tasks emphasize the skills learned during therapy and allow the client to apply effective problem-solving strategies in gatekeeping from the recurrence of self-directed violence, 44 thereby managing these impeding factors.
The procedural elements are also crucial in conceptualizing the suicide management and intervention program. Like the Zero Suicide Initiative, the procedural aspects can provide a structure to eventually develop an evidence-based practice, 45 not for suicide prevention but for suicide recovery. To wit, suicide risk appraisal instruments, according to Posner et al. 46 and Madan et al. 47 include the use of the highly validated Columbia Suicide Severity Rating Scale (C-SSRS) because it explores both lifetime and recent suicidal thoughts and behaviors. Further, stabilization strategies include suicide first aid for Filipinos 48 and immediate implementation of a safety plan to assist the clients in identifying a list of coping strategies that they can use in a mental health crisis.49,50 The case conceptualization shows how the carer and client understood the suicide story. 44 Effective treatment involves pharmacotherapy, psychiatric treatment, and different types of psychotherapy, such as DBT and CBT-SP, to address mental health concerns. 51 Finally, the transition step includes relapse prevention and re-entry to the community.
The question remains: which of these suicide management practices, more so those that are recovery-focused, are already implemented, and what do the youths suffering from suicidality receive? Such a predicament in the mental health system manifests the cracks in the health care for suicidality. Nonetheless, when the healthcare system is systemic because there is a unified context of suicide among all stakeholders and consumers' views and needs are considered, the mental health professionals become more capable of engaging them and become purposive in targeting and monitoring their suicide recovery progress. Moreover, while there are many factors why people who went through treatment still die by suicide, there were 3 causes that were identified, namely: (1) inadequate ability to detect suicide risk; (2) ineffective implementation of evidence-based, and suicide-specific interventions; and (3) low quality of healthcare during critical periods. 43 These reasons are heavily influenced by how mental health professionals contextualize suicide and being uninformed about suicide recovery. If suicide recovery is included in the picture of suicide treatment and management, mental health professionals may know better what strings to pull and what strings work for suicide recovery. Thus, our phenomenological study may help guide mental health carers to carry out suicide care and management programs for recovery. Unlike the clinical care systems focused on mental health in general, with these suicide prevention approaches, namely, Zero Suicide, 52 LifeSpan, 53 and European Alliance Against Depression (EAAD), 54 the Inflorescence Suicide Management Program (ISMP) is proposed.
Proposed Inflorescence Suicide Management Program
ISMP is a year-round program conceptualized to promote and incorporate suicide recovery in the healthcare for suicidality. It includes 3 phases, namely:
Tilling hope (suicide recovery campaign)
This aims to address the gaps or fragmentation identified in the healthcare system for suicide management. This includes: (a)
Tending hope (clinical application)
ISMP has a clinical process to follow. A mastery of the knowledge and skills is required to implement this process flow, particularly the Suicide Recovery Rehabilitation (SRR). This includes: (a)
Toiling for hope (sustainable inflorescence suicide management program)
This is the evaluation and monitoring of the whole program to ensure its sustainability, involving: (a)
Limitations and future directions
Interpretation of the findings of this current study should be limited to its focus. We delved into (1) lived experiences of suicide recovery of Filipino youths, whose last suicide attempt was at least a year ago at the time of the study; and (2) perspectives of mental health professionals (guidance counselors, clinical psychologists, and psychiatrists) on suicide recovery. Moreover, the sample size is small, and more rigorous research is needed to validate our proposed ISMP.
It will be interesting to know more about the concepts of suicide recovery and how they can aid in establishing systemic healthcare for suicide management. Also, it will be a success when a unifying concept is based on suicide and suicide recovery among all mental health professionals. Overall, the findings of this study may also serve as a basis and guide for future researchers who aim to develop an intervention program focused on recovery in managing suicidality. It is also suggested that the emergent recovery-focused suicide management program be examined and pilot-tested with more aggregate samples and cross-cultural settings for compatibility and comparison purposes.55-58
Footnotes
Author Contributions
The authors confirm significant contributions to the paper as follows: study conception and design: Bautista, Reyes, and Delariarte; data collection: Bautista; analysis and interpretation of results: Bautista, Reyes, and Delariarte; draft manuscript preparation: Bautista, and Reyes. Author. All authors reviewed the results and approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
All procedures performed in the present study that involved human participants were with the ethical standards of the Ethics Review Committee (ERC) of The Graduate School, University of Santo Tomas.
Informed Consent
Each participant in the current study gave informed consent before voluntary participation. In addition, participants were briefed on the nature of the study and were assured that all data collected would be kept confidential, and that participation was purely voluntary without remuneration.
