Abstract
Background
This study describes adaptation and modification of World Health Organization (WHO) recommended group interpersonal psychotherapy (IPT-G) for depressed peripartum adolescents. The adaptation process includes accommodating contextual factors and strategies to address intervention implementation barriers, such as engagement problems with adolescents, caregivers, and providers, and stigma and dearth of mental health specialists. The modifications include and adolescent relevant iterations to the therapy format and content.
Methods
A multi-stakeholder led two-stage intervention adaptation and modification process integrating mixed qualitative methods were used with pregnant and parenting adolescents, their partners, and health care workers. In-depth interviews focusing on personal, relationship, social, and cultural barriers experienced by adolescents were carried out modeled on the Consolidated Framework for Implementation Research. Focus group discussions with depressed adolescents on their experiences, feedback from caregivers, partners, health workers inform focused modifications. An IPT expert committee of three practitioners, along with UNICEF adolescent officer, and mental health policy expert from Ministry of Health and representative community advisory body reviewed the adaptations and modifications made to the WHO IPT-G manual.
Discussion
Integration of mental health needs of peripartum adolescents as demonstrated in the stakeholder engagement process, adaptation of key terms into locally relevant language, determination of number of sessions, and user-centric design modifications to digitize a brief version of group interpersonal psychotherapy are presented.
Adolescent Mental Health in Sub-Saharan African Context
Perinatal Depression in Adolescents in LMICs
Globally, depression is the leading cause of disease burden in women of reproductive age.1-3 Estimate prevalence of depression during perinatal period is 11–18% worldwide, and 30–50% in low-and-middle-income countries (LMICs).2-5 Adolescents suffer disproportionate burden of mental health problems due to the global demographic transition and paucity of services and systems that are responsive to their needs. Most perinatal depression in LMICs occurs in adolescents, as 50% of the world’s population are adolescents, and 85% adolescents live in LMICs.6,7 Pregnant adolescents are 2 to 9 times more likely to develop perinatal depression. 3 This scenario is exaggerated in Sub-Saharan Africa (SSA) where the population below 15 years of age is five times higher than those above 55 years.1,2,8,9 In Kenya, where this study will take place, 32% of total population are adolescents, and nearly 26% of women give birth before the age of 18.8-11 High prevalence of adolescent pregnancies and perinatal depression in vulnerable adolescents has resulted in a tremendous public health burden in Kenya with cascading effects on the well-being of the offspring to damaging impact on family and community health.8-17
Evidence-Based Perinatal Depression Interventions and Implementation Model
This proposed project aims to address the perinatal mental health intervention and service gaps in Kenyan adolescents by adapting, testing, and informing the implementation of the WHO Mental Health Gap Action Program (mhGAP) for depression. Considering limited resources in LMICs, there is a growing evidence for the use of stepped-care models to deliver depression care. 18 The stepped-care approach provides intervention by starting with the least intensive evidence-based intervention (EBI) that is still expected to generate effect, and adding more intensive EBI options for patients who do not successfully respond to low-intensity EBI.
Most evidence-based perinatal depression intervention programs (including WHO mhGAP) in LMICs are focused on adults, with only a handful of implementation and effectiveness programs focusing on adolescent mothers. Although a body of epidemiological research in adolescent pregnancies in LMIC context have examined critical social determinants of mental health,11,15,19 intervention research for reducing early and unintended adolescent pregnancies and mental health problems have been very limited.5,11,12,15,16 A handful of innovative intervention studies in LMICs has focused on depressed adolescents: Group interpersonal psychotherapy for depressed war affected adolescents20-22; ongoing Problem Management Plus for vulnerable refugee youth from Syria 23 ; task-shifting low intensity/dose adolescent depression intervention24,25; and studies on perinatal depression for a wide range of reproductive-aged women as seen in Thinking Healthy Program piloted in Pakistan and in Vietnam.9,12-14,17,25-27 In a worldwide effort to make intervention relevant and accessible to diverse LMIC contexts, the WHO has been actively developing manualized depression interventions that are building on the mhGAP framework,26,28 with consideration of low cost task-shifting/sharing implementation strategies, a stepped-care intervention to more effectively utilize treatment resources, and a collaborative care model to promote case management. 29 Collaborative-stepped-care models involve collaboration among multiple providers (e.g., non-specialists and professional health workers) to offer several levels of treatments to patients with different levels of needs. While many depression EBIs recommended by WHO are highly relevant to perinatal depression in adolescent girls, there is a dearth of intervention implementation guidelines on more complex populations such as adolescents in perinatal spectrum who need depression treatment and other related services (e.g., life skills and parenting skills). Because of the differences in the levels of maturity in development and living context (e.g., marginalized by society and parent–child co-living arrangement and dynamics) between adolescents and adults, additional engagement strategies may be needed to ensure EBIs match the developmental level of adolescents and living contexts. 4
IPT evidence base: Summary of notable researches that have impacted global dissemination of IPT.
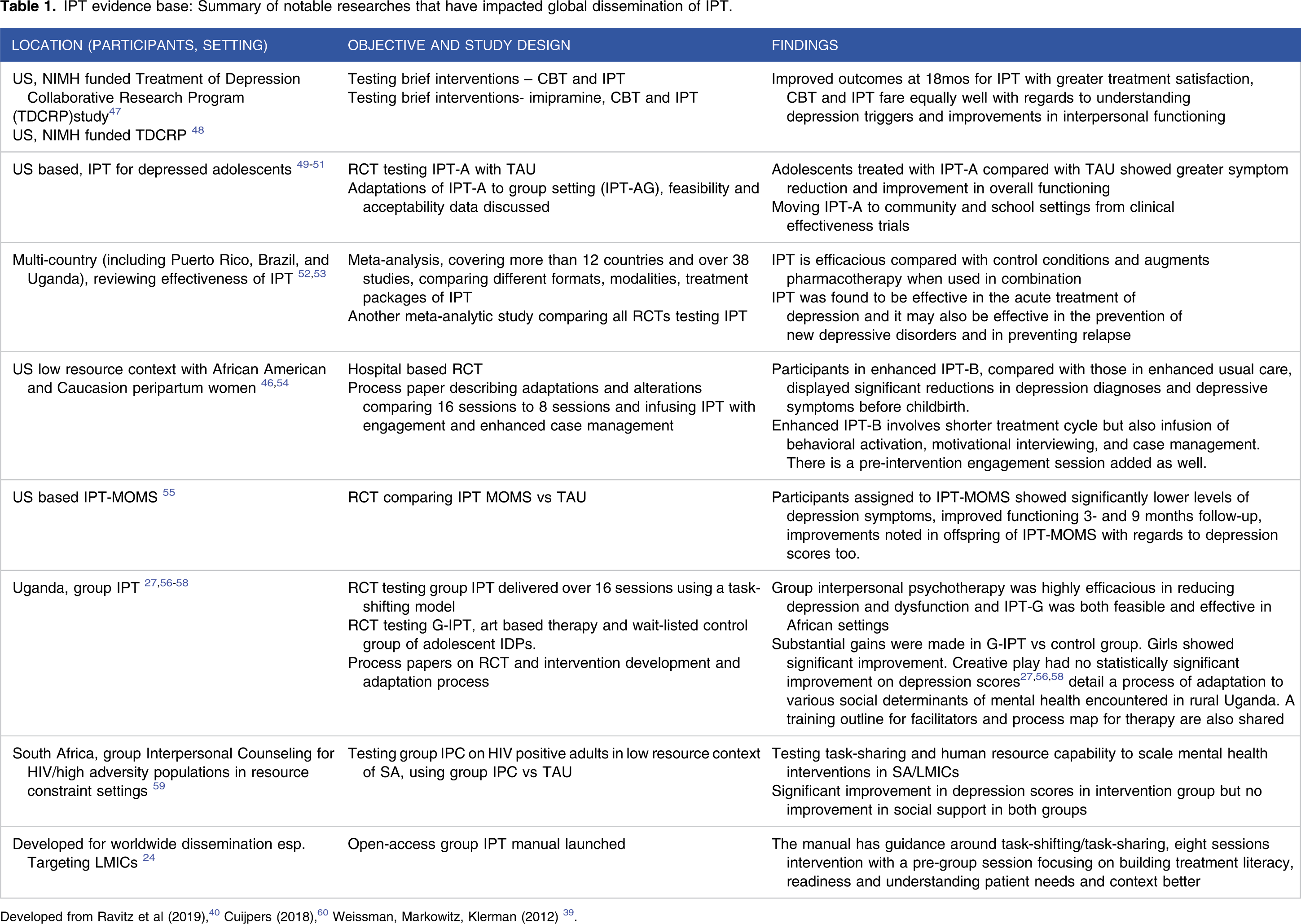
CFIR mapped qualitative inquiry to inform adaptation and modification of IPT-G.
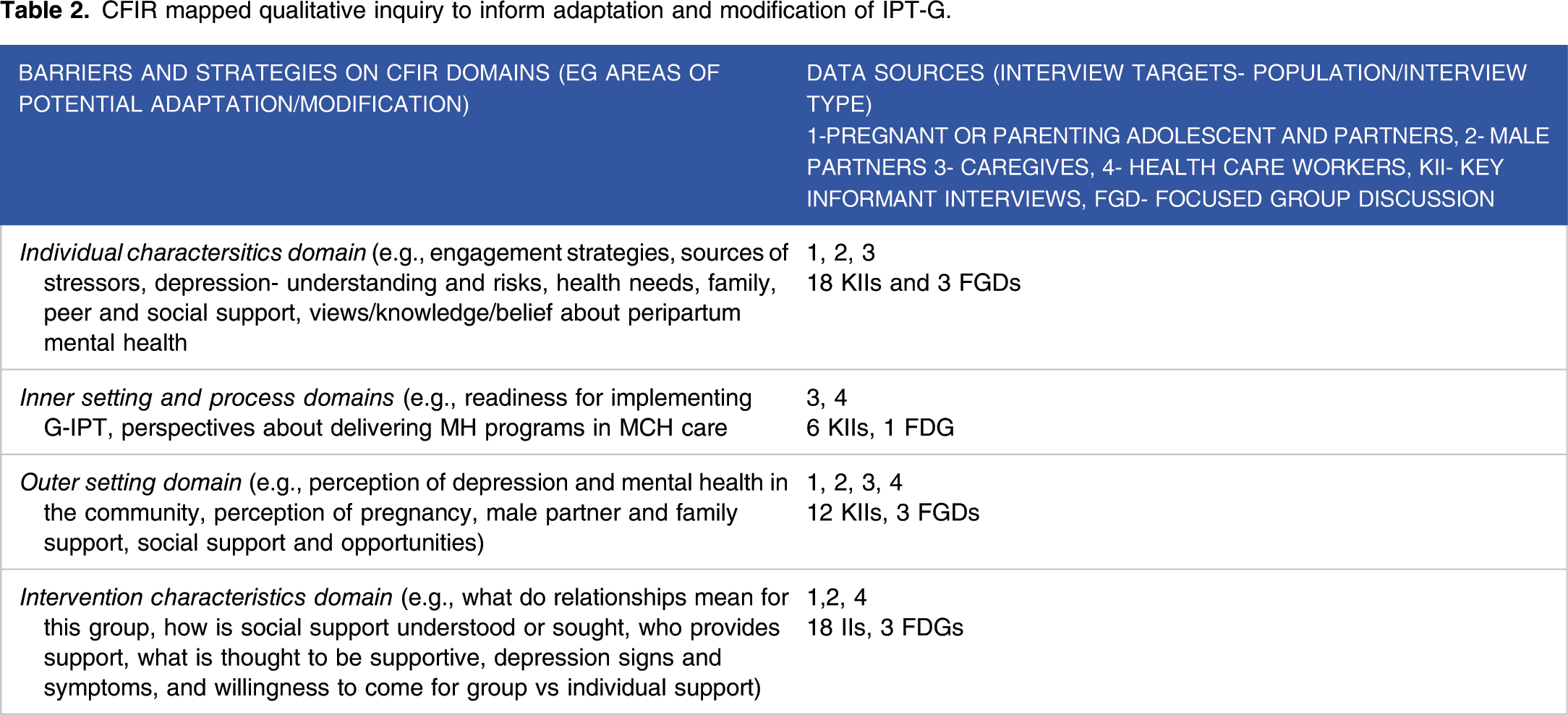
Challenges and Gaps in Perinatal Depression Care for Adolescents in LMICs
While there is existing epidemiological and interventions research on perinatal depression, adolescent mental health, and child development in LMIC contexts,9,13,15,22,25,26,30 the challenge to intervene often originates from multiple levels including, lack of a service system, limited number of trained competent health staff, minimal social support from family or communities, limited perinatal mental health interventions that fit adolescents’ living contexts and developmental needs, and a lack of evidence.16,17,21,22,24-27,31-34 Addressing adolescent pregnancy-related health burden demands new ways of organizing maternal and child health (MCH) services that considers health care resources and tackles multiple needs of this group (e.g., psychosocial and financial stress, social life, education, and developmental status). Services need to be restructured so that they are patient-responsive and integrate mental health with primary health care and community settings. The new organization should ensure involvement of key stakeholders and enable them to adopt EBIs, while re-engineering institutional and policy support in sustainable ways.
The provision of mental health services for pregnant adolescent girls faces numerous challenges and additional individual, familial, communal, and health system strategies might be needed. At an individual level, in these resource-constraint contexts, the complex adolescent development pathways encounter adverse social determinants: poor educational opportunities and attainment; poor contraceptive use,6,7,33 food insecurity, limited resources for survival, and lack of knowledge or awareness of health problems and service resources. These resources become first set of barriers to seeking help in time.9,35 At the family and relationship level, support from families diminishes as girls become pregnant because of stigma.10,13 Studies from SSA have documented that domestic abuse by family members, male partners, and relatives,8,9,13,35 as well as dejection and social stigma from within the familial and communal networks are common experiences of pregnant adolescents.3,6,7,14,36
These experiences prevent adolescents from seeking support from large internal and external networks. Ultimately pregnant adolescents rely on mothers and maternal relatives. At the service provider level, most MCH facilities do not have mental health workers to provide mental health related services. The health professionals and staff (including community health workers) are not trained in screening mental health needs and in providing psychological support/intervention as part of routine MCH care for pregnant adolescents.1,2,4,37,38 At the policy level, poor recognition of the problem and the burden of socio-economic costs associated with adolescent pregnancy contribute to poorly developed child and adolescent health and mental health policy and plans.3,5,39,40 To effectively address the multiple needs of pregnant adolescents and to successfully transport/implement mental health EBIs for pregnant adolescents in Kenya, consideration of all four aspects and levels of barriers and strategies is required.
Applying Implementation Science Methodology to Adapt IPT-G + mhGAP/Stepped Care Model for Adolescents in Kenya
This approach is consistent with WHO mhGAP recommendation. However, knowledge about how to effectively implement the mhGAP stepped-care model for adolescent special population and whether it results expected intervention effectiveness have not been systematically studied in low resource settings. This study applies two implementation frameworks of Consolidated Framework for Implementation Research (CFIR)41,42 and Proctor et al’s conceptual model for implementation evaluation.
43
The study systematically identifies potential implementation barriers of the mhGAP approach in MCH settings and develops and integrates implementation strategies to enhance mhGAP model for adolescents with perinatal depression in Kenya (see Figure 1). These frameworks have been described at length in another study protocols.
44
Integrated implementation adaptation framework for qualitative study.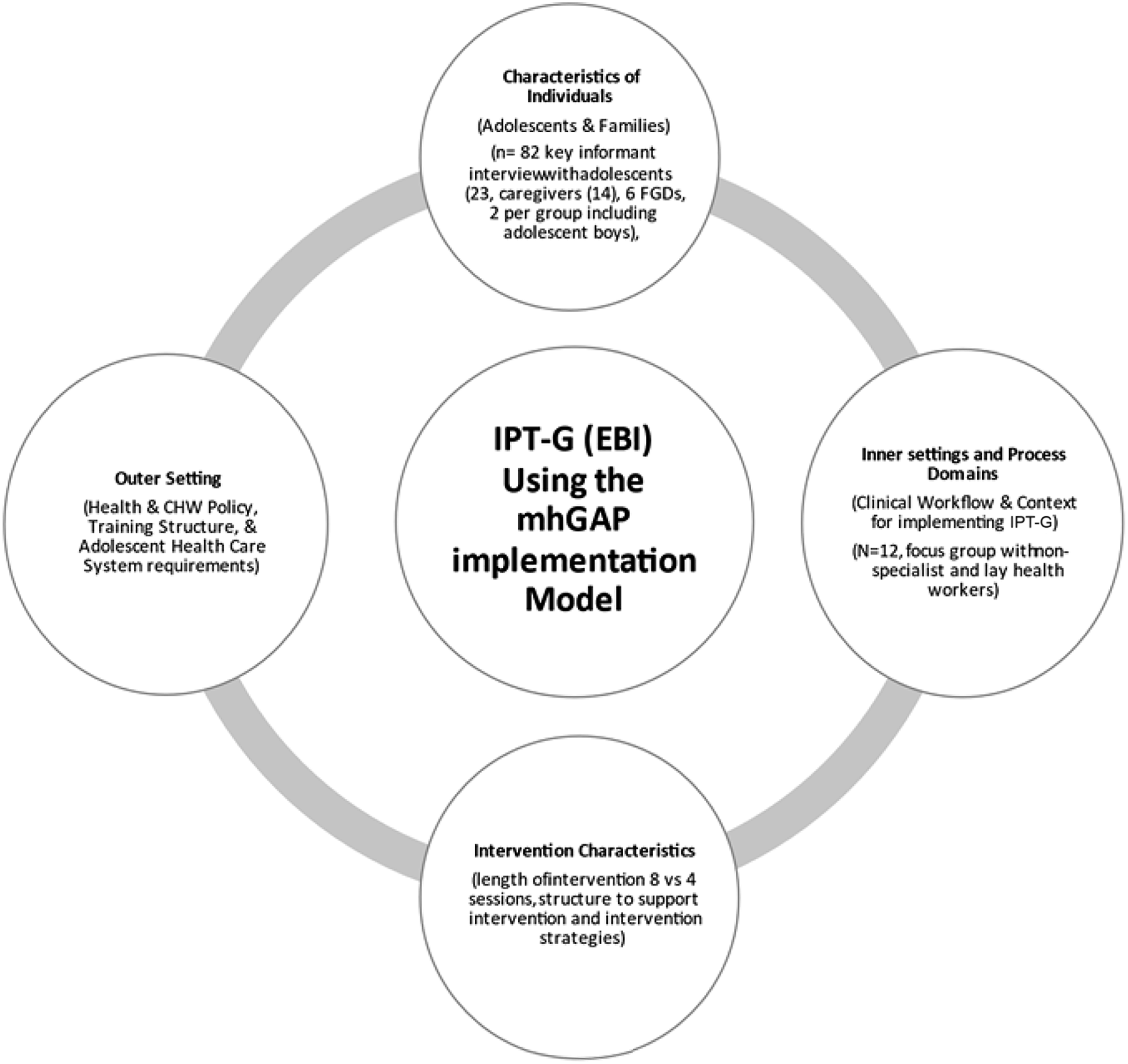
Objectives of the Study
The overall goal of this study was to adapt IPT-G mhGAP stepped-care model for adolescent perinatal depression in Kenya in primary care. We applied an integrated framework (adapted from CFIR and Barera and Aaron’s frameworks described in the methods section) to guide the qualitative study. Two sub-aims were studied 1. To identify barriers and related factors (i.e., factors in 4 CFIR domains) that may influence IPT-G and mhGAP approach of intervention implementation 2. To identify potential strategies to overcome barriers and optimize the intervention implementation. 3. To develop adapted version of IPT-G intervention within the mhGAP-IG framework and initiate a workforce capacity building model embedded within stepped care training approach for non-specialist health worker and lay health workers in addressing adolescent perinatal depression. 4. These aims necessitate adaptation of the IPT-G manual to be suitable for use by these health care workers for peripartum adolescents ages 13–18 years who are suffering from depression. We have also adopted Barrera et al and Aarons model to carry out these adaptations.
The clinical presentation of peripartum adolescents often includes malnutrition, exposure to HIV, STIs, and intimate partner violence. Therefore, anxiety, trauma-related reactions, and poor daily functioning is commonly seen. The process of adaptation of IPT-G requires understanding multilevel barriers and stakeholder involvement in the delivery of the intervention at the primary health care facilities in Nairobi County in Kenya. As the intervention would be delivered jointly by ANC/MCH nurses and community health workers, it requires modifications that are culturally suitable for the facilitators to better understand the rubrics of this particular type of psychotherapy and peripartum adolescent needs.
Once the intervention has been adapted a strategy for mapping the clinical workflow and then training the facilitators in delivering IPT-G, including developing a plan for ongoing clinical and peer supervision would be derived. Using a partnership approach this work will involve the Ministry of Health, Nairobi County and other NGO stakeholders to ensure the program is developed in a way that if shown to be effective, could be implemented at scale.
Testing Different Modalities of IPT
Group and individual psychotherapies
IPT like most other therapies was developed as a one-on-one therapy that addressed individual challenges using the above-mentioned problem areas. It offered a framework to normalize depression as emanating out of stressful communication, poor interpersonal relationships, and therefore poor sense of adequacy in relationships. The group modality became popular as IPT was transported outside North-American/European context. It became a way of engaging with people in communities/cultures where stigma was high. It was also a way in which problem solving along the 4 IPT problem areas could take place in cultures marred by poverty, food insecurity, violence, etc. Group became a resource to question, mold, and interrogate cultural and interpersonal relationships of these peripartum adolescents who are in a challenging life transition/s for which they were not prepared. Behind the broad context of adolescent pregnancy, there are also issues of how men or boys do not go through similar abuse, social stigma or moral judgment, abandonment of the adolescent by the partner, family, and her primary caregivers, and withdrawal of key institutional support from school, health facility, or community. These social inequalities make for a stimulating and thought-provoking discussion with young people in groups, to identify solutions to the problem areas IPT champions that would most work for them,
Combined group and individual IPT delivery
In the combined delivery it means beginning with individual case-formulation, describing how the group will operate, sharing how other participants might be alike, how groups would participate towards individual and collective well-being, and address problem areas and interpersonal challenges together. The individual session typically known as pre-group session is further improvised to be like an engagement session meant to elicit barriers to someone’s treatment, understanding motivational currents, addressing barriers building momentum. This is then followed by group delivery where participants follow the facilitated sessions with active feedback, sharing and role-playing. There are collective, home-based and individual assignments that go back to the theme of depression, social and relationship connectedness, and daily functioning. Towards the end the participants go back to one or two individual sessions to explore personal learnings, mapping whether goals were met and explore additional resources and work plan for them. These strategies become useful when one is working with vulnerable populations like pregnant adolescents and in a context where individual one-on-one therapy may not be feasible.
Need for adaptation and modification of IPT
IPT has been very open to its translation as well as adaptation in diverse geopolitical contexts. Weissman et al 45 specify two issues that pertain to boundaries of adaptation: (a) good therapist fidelity and (b) patient being seen in a time-limited therapy and defining that time frame from the outset clearly. We anticipate that there needs to be two types of adaptation. One, addressing concerns and needs of adolescent girls and second, modification needs to be around peripartum context-covering pregnancy and childbirth experience which has been addressed in individual IPT but not in groups. Another point of consideration for this modification is that these adolescents are mostly going to experience an unanticipated, unplanned pregnancy and the consequence of this would be dropping out from school, social and familial stigma, discrimination within family and in the community, domestic violence, and abuse. At times pregnancy in addition would expose them to HIV/STI, it may be a result of a rape or abusive context. The content modifications need to be responsive to these contextual and cultural issues. 46 Engagement and stigma-reduction strategies would be critical and need to be embedded in the intervention. Lack of clarity about how poor knowledge, relationship support, and resources exacerbate mental health challenges, the engagement strategies are meant to stimulate and motivate adolescents to rethink their options, understand rubrics of depression, learn more about sexual and reproductive health, and about their rights and available educational, community, and health resources. For the facilitators, engagement means added stances that create an alliance between young person and the group as well as the facilitator. Stigma-reduction strategies involve ways in which pregnancy, depression stigmas can be addressed in the IPT-G sessions, as well as how facilitators can provide the participants with tools to combat community and self-stigma in the future. Stigma-reduction strategies involve sharing the role of self-stigma in the development of depression, learning assertiveness tools to deal with discrimination, and using social support from peers in the group, community health workers, and other significant support figures to engage in prosocial behavior (taking medications on time, continuing with studies, livelihood, and caring for oneself and the baby, etc).
Methods and Design
Adaptation and modification process
The adaptation and modification followed a two-stage process integrating mixed qualitative methods with expert feedback and review. In a nutshell, in-depth interviews focusing on personal, relationship, social and cultural barriers experienced by adolescents would be carried out modeled on Consolidated Framework for Implementation Research. The mhGAP adaptation will involve several iterative stages of consultation with collaborators on this grant (Ministry of Health, Nairobi County, UNICEF, UNFPA), IPT experts and a spectrum of researchers in public mental health, pediatrics and programming staff covering adolescent SRH, mental health, maternal and child health, and Antenatal clinic in primary health centers at Nairobi county and Ministry of Health. An IPT expert committee of three reviewers along with a Kenya Ministry of Health, Mental health officer and representative community advisory bodies would review the adaptations and modifications made to the WHO IPT-G manual. Studies have also demonstrated that the extent of cultural adaptation positively impacts intervention fidelity.
49
See Figures 2 and 3 that detail the adaptation process. Intervention adaptation and implementation model. Source Proposed Four sessions therapy model.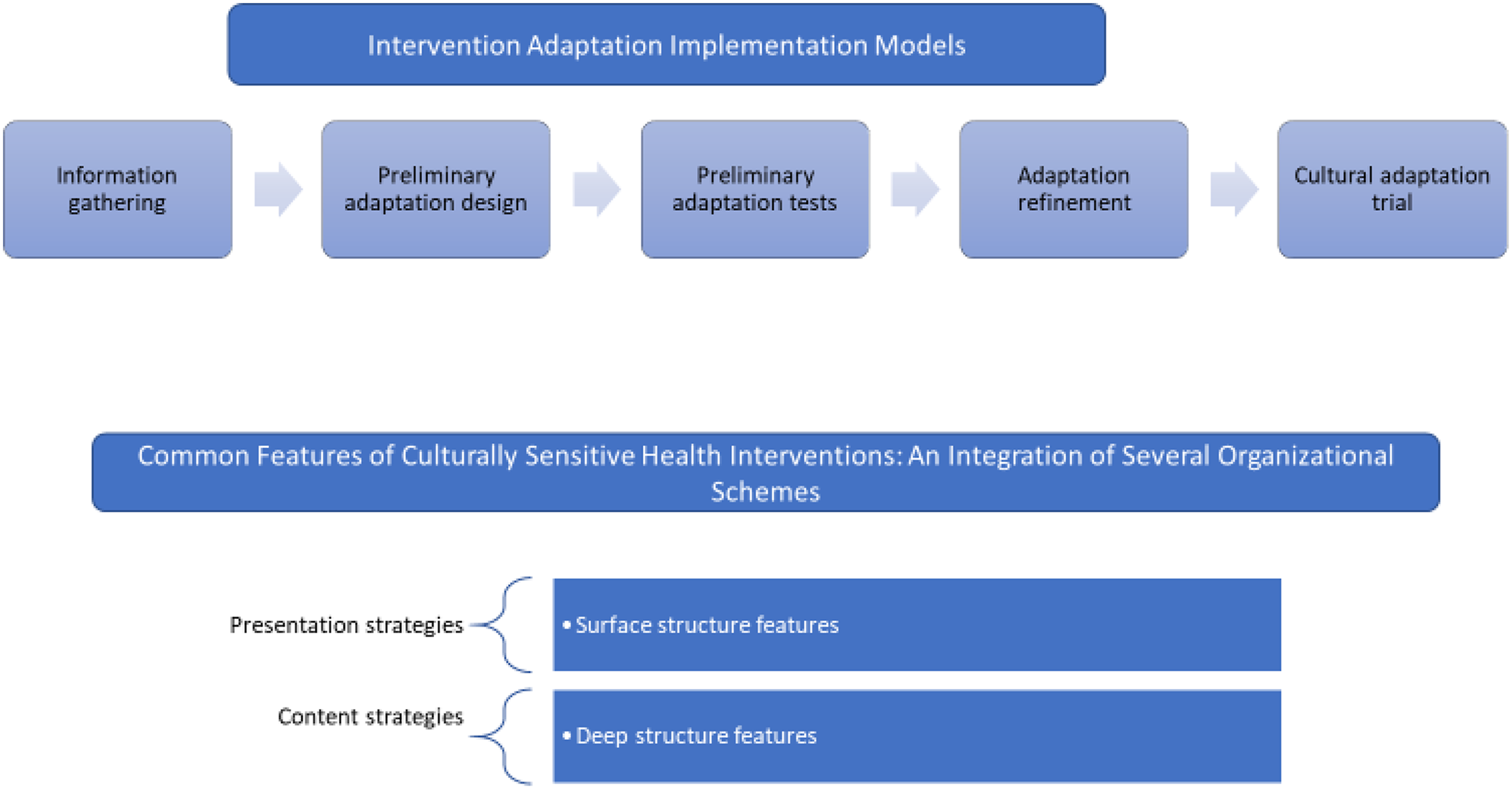
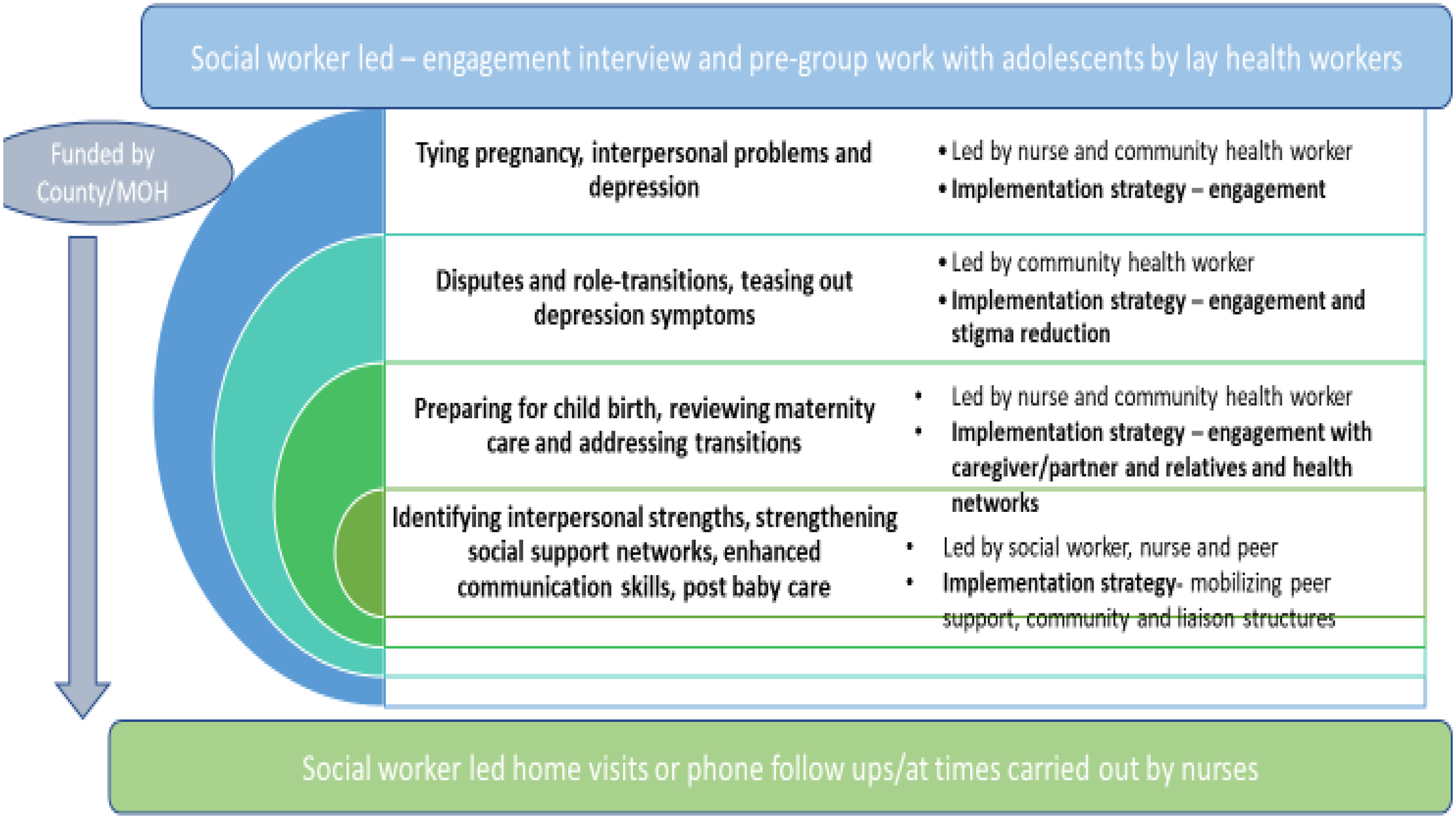
Participants, setting, and ethical approval
Participants interviewed during the adaptation process.
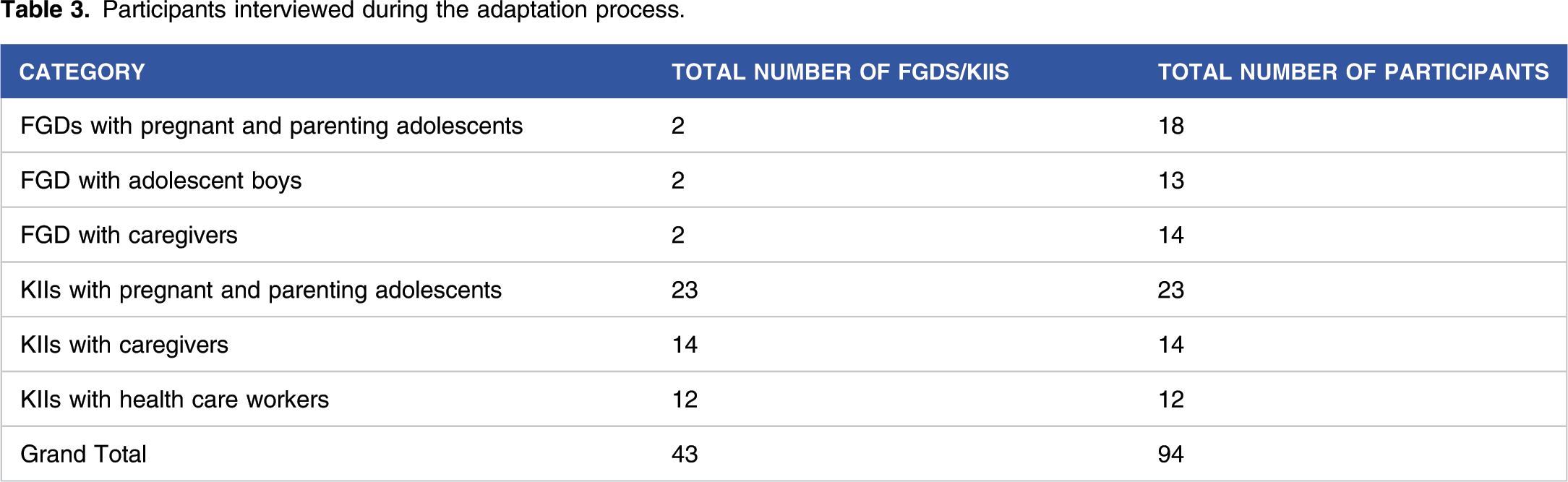
Data Collection and Analysis
Data was collected between May 2019 and January 2020 at the health facilities mentioned above. The average interview length was 40 minutes with the longest being 2 hour and 20 minutes. Participants were recruited through engagement with the health facility In-charges and community health volunteers (CHV) who had been engaged to identify eligible participants. Each CHV works under a community health assistant who oversees their activity. The eligible participants were consented by two research assistants in the health facility. A space was provided by the facility which provided visual and auditory privacy for these interviews to be conducted. In the KIIs, the participant voluntarily answered all the questions from the interviewer and appropriate probing done for deeper understanding. The FGDs were done in a circle siting positioning whereby questions were voluntarily answered by any group participant and follow-up probes done to enable clarity. The moderator probed to exploit all the viewpoints before moving to the next question. Participants were offered transport reimbursement and snacks upon completion of the interview. The interview was recorded, conducted in both Kiswahili and English. It was transcribed by a research assistant and then the transcripts were read by other authors. All transcripts were de-identified.
The transcripts were uploaded on Qualitative Solution for Research (QSR) NVivo version 10 software. A thorough initial reading was done without coding to ensure adequate familiarization with the data set as guided by thematic analysis principles. 59 The coding process was conducted independently by different coders, and after conclusion, there was agreement on the framework and the generated NVivo output. Thematic content analysis was conducted keeping the CFIR domains in mind and the sub-themes under each domain indicated in Table 2. It was an integrated approach of both deductive and inductive. Some of the themes were determined deductively/prior to coding as guided by the study objectives, and therefore the analysts explored the content to identify common patterns and coded the data in to the deductively identified theme. In addition, inductive which is grounded approach was also utilized, whereby new themes emerged and identified from the rich data text content. The analysis started from the first batch progressing towards the last interview. Saturation of theme was determined after at least 3 subsequent interviews with no new/emerging theme. The stage was the adaptation of the intervention on the basis of qualitative interviews and expert feedback. Usually adaptation process starts with information gathering using qualitative methods → preliminary design adaptation which in our case would be minimal as there exists a framework and guideline for IPT-G already → preliminary adaptation tests utilizing → cultural adaptation trial (see Figure 2) Barrera et al 62 recommend that attention needs to be paid in two areas of adaptation-presentation strategies-how the intervention is packaged, its presentation is engaging and age appropriate, has some resonance to the peripartum adolescents. The content strategies reflect the relevant structure and meaning around the techniques used, their adaptation to the context, and applicability to the population in question. These issues have also been flagged off by Weissman and colleagues20,45 in making IPT more accessible to diverse geopolitical settings.
Results and Discussion
Table 3 provides demographic information of our participants. The findings of the CFIR mapped interviews are offered in Table 4. We learnt that in terms of the five CFIR domains the following themes for IPT-G adaptation came up. 1. Characteristics of Individuals-we were strongly encouraged by the health care workers as well as caregivers to address the unique challenges experienced by peripartum adolescents and the adolescents themselves suggested offering an integrated approach that involves caregivers, addresses maltreatment, mental health knowledge gap, stigma, and use of technology to improve access to mental health care when needed. Participant feedback around CFIR domains for potential modifications and adaptations of IPT-G.
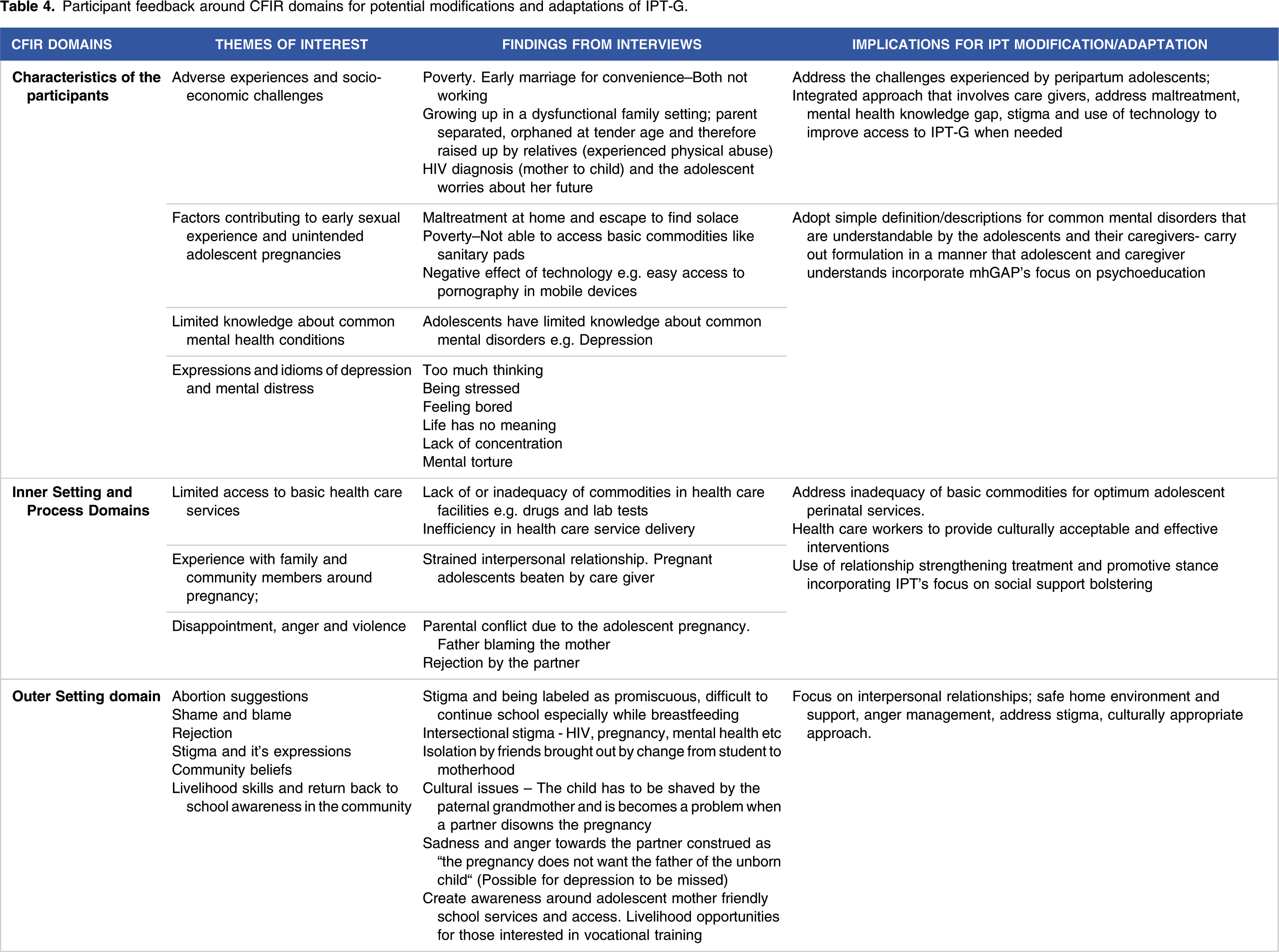
Some quotations from adolescents and caregivers shared some insights such as “What caused (to get pregnant) is that I was studying but my father died and left us, so it was difficult to get school fees” KII with adolescent “He said that I should abort to show that the child is his, so I decided it is better that I forget him”- KII with adolescent “I feel that the lack of a father-figure contributed; you know absence of a father and that gap was the cause” KII with caregiver “Job is just the casual ones whereby I am called today but tomorrow it is not there I stay by the door side; when you get something you eat, if you don’t get that is how it goes” KII with caregiver “She cannot go to school then after coming back from school she comes to breast-feed, what kind of shame will that be to other students in school”- FGD with caregiver
It was also recommended by community and facility health care workers that we adopt simple definition/descriptions for common mental disorders that are understandable by the adolescents and their caregivers—carry out formulation in a manner that adolescent and caregiver understands well and to incorporate mhGAP’s focus on psychoeducation. “Okay; mine I did mentorship especially for pregnant mothers and breastfeeding mothers and I have some training in some certificate in psychology and counseling so basically I am able to detect; though there are those who keep information to themselves but given the chance, if I am given more orientation, I believe I may be able to have a closer ability of detecting challenges when the mothers come on board in a given session”- KII with HCW 2. Inner setting and process domains: our multiple stakeholders in their interviews shared that in the long run it would be critical to address the inadequacy of basic commodities for optimum adolescent perinatal services and to this effect it would be important to leverage existing community health structures and community-based organizations to address adolescent perinatal mental health issues. Suggestions of task-sharing and ways to make it more sustainable were recommended. Even peer led interventions were recommended. Some vignettes from the participants highlight the issues here. “They felt that I failed to raise my daughter well, they started to blame me that I pampered her since she is the only child, you see? That was the first thing, “you used to love that child so much now see,” they blamed me, I am the one who was blamed so much….but I continued to give her support and a CHV helped us link her to ANC” – FGD with caregiver “let’s say sometimes I go to church and talk to somebody like a leader who encourages and advises me and I feel much better”- KII with adolescent mother “We do need to talk to them and tell them “since you made a mistake you shouldn’t repeat the mistake so it is better to go to the doctor to be injected” (Family planning method)” – KII with caregiver
Health care workers felt that with training they could provide culturally acceptable and effective interventions. Use of relationship strengthening treatment and promotive stance incorporating social support bolstering was strongly recommended by caregivers and adolescents themselves. “Yes I would like to go through a training that would offer me like a paper you see sometimes I would like to go maybe to a school to talk to teachers or something but if you don’t have something to qualify you to mental health issues then you are disregarded because it’s like you are not a psychologist you are not” -KII with HCW 3. Outer setting: We identified through our caregivers and health workers that we needed to focus on conveying the value of forming strong interpersonal relationships. The community members also conveyed how advocating for safe home environment, caregiver support and disseminating information on good parenting skills were thought to be equally important.
One adolescent shared her experience as being the following- “I went and explained to my mother how it was and she held me like a child and I stayed at her home until I gave birth to my first born” -KII with adolescent
There were a number of female caregivers who shared experiences around being stigmatized and chastised for their daughters’ early pregnancy. “When they heard that news, there is one of my brothers who said, “you refused to stay in your marriage and left,” you get it; I mean being told things, “you got out of your marriage now look at the behaviors that you have started to teach your child,” – KII with a caregiver “They felt that I failed to raise my daughter well, they started to blame me that I pampered her since she is the only child, you see? That was the first thing, “you used to love that child so much now see,” they blamed me, I am the one who was blamed so much” – KII with a caregiver.
There were also suggestions that health care workers need to be empowered around addressing pregnancy and mental health associated stigma using a culturally appropriate approach.
One of our health care workers made the following comments: “Integration is when we incorporate mental health care into all service points like when someone comes to my clinic he/she is able to be screened for mental health and just the same way we are doing with TB as in every work station somewhere even from the gate the soldier can screen and know that this is a person with depression or stress or what and they may be able to assist them in a way or another. So that is the integration that-that mental health that someone-any client is able to be screened for mental health issues at every work station facility”. Yes, because previously people used to feel like mental health is-they used to stigmatize the mental health and they used to attach it to people who are mad they are in Mathari but mental health issues start from- as in with us even us the health care workers could be struggling with mental health issues and we transfer them to our clients, so it is very important when from really primary health care everyone is so conscious about their own mental health so that even as they take care of clients, they are sober and they give quality care and just to protect them from those clients from having bigger issues of mental health like depressions” – FGD with HCW. 4. Intervention Characteristics: On the issues around specific characteristics that the intervention needs to incorporate there were strong recommendations that it should include multilayered support system that includes caregivers especially the female parent, peers, partner, religious leaders, and health care workers covering all aspects of mental and physical health. “ Okay; mine used to just keep quiet but when I see her keeping so much quiet I tell her let’s go for a walk; then we walk and go to friends' places those who don’t know her story and we talk” – FGD with a caregiver “When we went to Mathari (mental hospital) they said that she is not sick she was being disturbed with the things she was using, she was abusing drugs” – KII with a caregiver
There were also recommendations to develop plans once the baby is there on the scene. Developing back to school plan during intervention including empowerment on livelihood skills and prevention of subsequent unintended pregnancy were thought to be really critical. “For assistance I would just like somebody to give me support to go back to school because parents are complaining so much, when I go back to school and accomplish my dreams I will have been helped” – KII with an adolescent mother “Let’s say like talking to her, let’s say if it is family planning, she should be told to use, because she can get used and perhaps go and get another pregnancy and come back to my house” – KII with a caregiver “Mine says that she doesn’t like going back to school but she likes making dreadlocks so much; that’s her dream” – KII with a caregiver
Given these findings from our extensive interviews and feedback from various stakeholders, we identified key intervention adaptation strategies to carry out relevant content and process modifications. Barrera et al 62 talk about use of five strategies in this regard. Peripheral strategies include modifying observable properties of the intervention to increase relevance to the group in question which would include minor adaptations such as inserting references to school or age relevant examples of stressors. It may also mean underscoring the challenges around pregnancy. Linguistic strategies require simplification of language, making it more comprehensible to the group in question. Some of the adolescents who are between ages 13–15 years might not be able to understand problem areas well or may need more explanations around somatic conditions underlying depression. Peer-, school-, and self-image- related metaphors may need strengthening. Constituent involving strategies require sharpening the focus on the intervention content along the needs, preferences, cultural knowledge of peripartum adolescents. Sociocultural strategies akin to the constituent involving ones require context level modifications so that community, family, and adolescent cultural viewpoints are added into the work. Finally, modifications are also needed at the level of specific evidence towards which the intervention aims to create awareness. In this case, the evidential strategies would aim to use both the epidemiological and cultural evidence around adolescent pregnancy, depression, social support, and additionally experiences from individuals with similar backgrounds to increase the perceived relevance of information during the group intervention. In a systematic review and meta-analysis of cultural adaptations carried in low-intensity psychological treatments, Shehadeh et al 49 found that most adaptations were around language translations and use of more culturally appropriate metaphor 49 ; however, Chowdhary et al 63 identified the need to focus more on the intervention implementation requirements than the content level adaptations for evidence-based interventions to be successful in a different context from which they were originally developed. 63
Aarons et al 64 suggest that though these adaptations are critical for the intervention to fit the needs of subsets of service users, these should not affect the core components or elements of the intervention as such. Given those characteristics define its nature and likely produce the intervention effects. This cautionary guidance was also shared by the intervention developers as this protocol was discussed with them. There are two other adaptation and modifications framework extended by Aarons et al 64 and Stirman et al 56 in addressing process and content issues. Aarons et al 64 broadly classify adaptations into content (what will be presented) and process (how information will be presented). However, these authors discuss additional adaptations such as process adaptations include presentation, dosage/intensity, ordering, forestalling (putting or delaying aspects of interventions), and selective integration. Other adaptations include exclusion and supplementation of material. These adaptations according to Aarons and colleagues are impacted by client level, provider level, and client-provider relationship level attributes. These adaptations can allow for testing multilevel patient outcomes such as therapeutic alliance, engagement in care, family spacing and adoption of SRH services, and improvement in HIV treatment adherence. Stirman et al 56 echo similar sentiments and develop 12 different types of content adaptations. Additionally, the spelling out of significant contextual modifications such as format, setting, channel of delivery, and intervention recipients, as these may not impact the intervention content but fidelity or clinical outcomes significantly. We have explained these contextual factors in this study through the lenses of Consolidated Framework for Implementation Research (CFIR) that maps out inner and outer setting, characteristics of participants, intervention, and process. 65 This paper outlines the overall study design trying to contextualize WHO mhGAP guidelines for peripartum adolescents and placing CFIR as a framework that would lead to mhGAP-IG and IPT-G implementation in Kenya. 45 Stirman et al 56 talk about the need to discuss whose decision was to modify the intervention and to specify the stakeholder engagement as well as spell out the background and concerns of each of the stakeholder (was it provider, what level of specialization, different clinical team providers, researcher, supervision, intervention developer, etc). They also talk about the modifications to training and evaluation process. Procedures for training are critical and changes to these procedures impact fidelity, clinical and process outcomes. Content level modifications according to Stirman and colleagues, 56 need to be evaluated at multiple levels such as individual, cohort, population, provider, unit, hospital, and community levels. They generated a long list of content modifications such as—tailoring, adding, repeating or removing elements, shortening, lengthening, substituting or re-ordering elements, integrating another approach, integrating the intervention into another approach, loosening structure, and departing from the intervention. The authors highlight the need to differentiate between modifications of program content and form of delivery as being critical to the exercise of intervention adaptation.
Discussion
CFIR mapped domains and corresponding challenges and opportunities driving the adaptation.
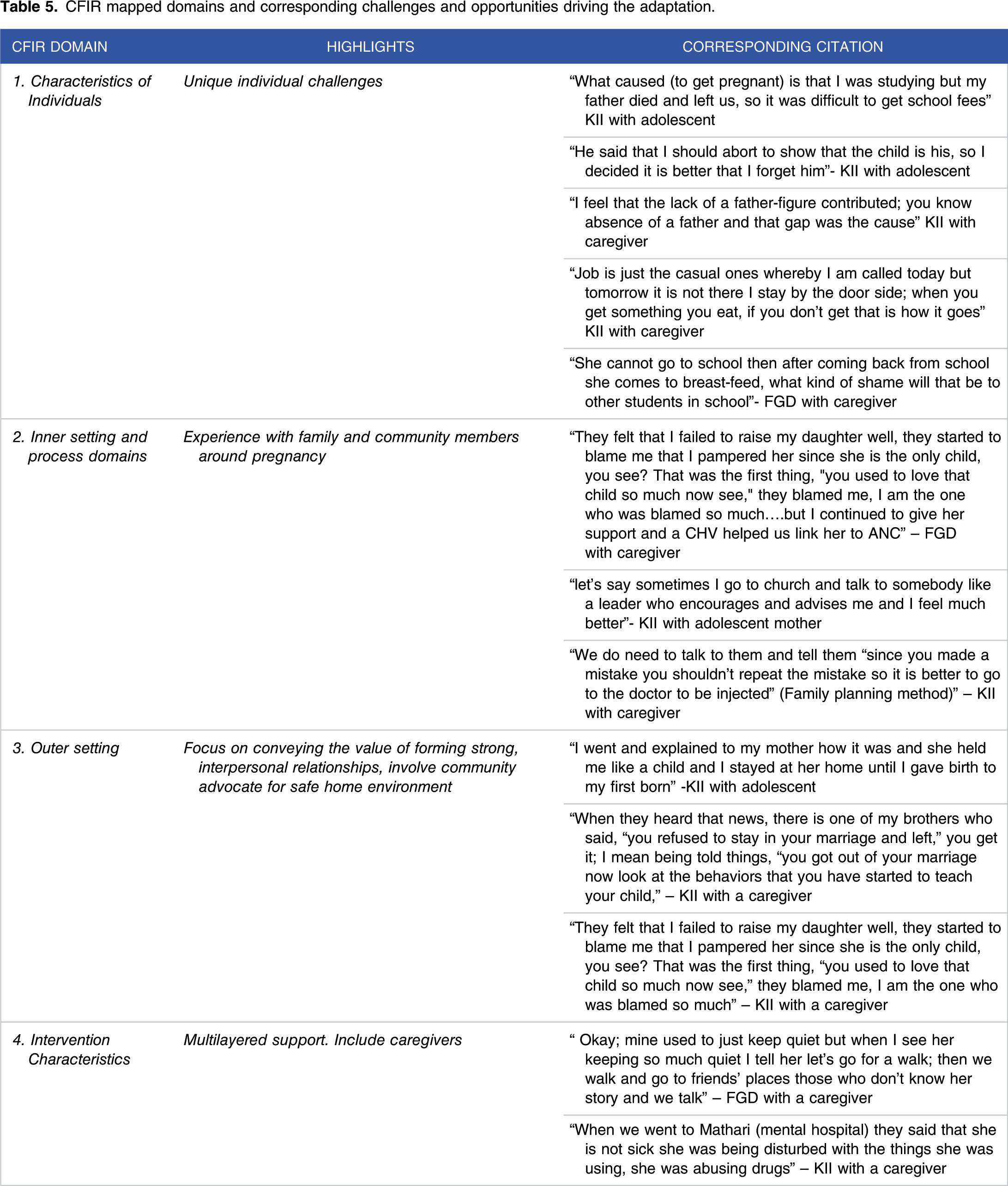

Developing Adaptations Responsive to Task-Sharing/Task-Shifting
Task-shifting can be understood as a deliberate process, whereby the task to be shifted is defined and described, and where funding is moved to the new individual assigned to the task. Task sharing is also a considered action involving health professionals working together in teams to deliver a task or service that they may not have carried out before. 66
In addition to the steps taken to adapt and test intervention implementation of IPT-G, it is very pertinent for this study to make adjustments that allow for task-sharing and task-shifting as added strategies. In SSA akin to other geopolitical settings, there is a great momentum towards infusing lay workers with relevant specialist skills so that services and information can reach masses. Task-sharing in this study would mean nurses offering mental health and psychosocial services that are ordinarily offered by psychologists to primary health care adolescent clients and task-shifting involves inclusion of lay and non-specialist community health workers to deliver IPT-G. In the Kenyan context, even though appeals for task-shifting have been made, the right funding and policy support to allow for lay health workers to formally join the workforce has not worked out clearly yet. There are ongoing efforts and a bill in the parliament to offer a minimum wage for this cadre of workers to feel supported and recognized.
In this adaptation as recommended by WHO IPT-G, it would be critical to have nurses and community health workers work together collaboratively in an effort to integrate IPT-G into routine ANC/MCH care for peripartum adolescents. This requires additional work around building collaborative care model and work plan, engagement at facility levels, and having collective buy-in of facility and community staff.
Infusing IPT-G With Additional Tools
Task-sharing/shifting and stigma-reduction would be included as additional strategies to empower the facilitators and supervisors of the facilitators (all personnel based at primary health care). Additionally, collaborative care principles would be infused in the intervention so that care is triangulated with appropriate assessment, intervention and follow-up pathways.
A facility and community-based mapping exercise to identify available resources, support structures and both governmental and non-governmental initiatives focusing on educational schemes, livelihood support, parenting skills and health camps and food banks would be provided. This resource mapping tool would be an asset to strengthening the group intervention and readily offer support. This would also be an example of how psychosocial and practical support can be infused with a mental health intervention. 67
Parenting skills, maternity care information and sexual and reproductive health information, and linkages to appropriate clinics/personnel would be made by the facilitators in order for more hands-on information to be disseminated. The delivery of the baby, getting ready to embrace maternity experience, and information about MCH clinic services and basic infant care would be critical. We will use the WHO’s Care for Child Development package 68 which is currently being implemented in primary health care MCH clinics in Nairobi county.
Support involving rights-based information, self-care, and social protection would be added in form of messages around family spacing, prevention against intimate partner violence, adherence to TB, HIV, and medications for chronic conditions. Infusing right information about psychopharmacological intervention for both facilitators and adolescents would be important.
Understanding Where Digital Versions are Useful
Part of the adaptation process would involve engaging in a prototype development for digital version of IPT-G. At this formative moment, it is kept open between testing an SMS version or developing a web-based brief therapy version. It would be critical, to further review, during the formative work which version may be useful for which population (13–15 years old adolescents vs 16–18 years old adolescents). It is likely that the more depressed pregnant adolescents might benefit from an in-person encounter. It is also likely that the digital portal might offer solutions towards addressing constraints in follow-up meeting post-delivery of the adolescent mother, or in assisting community health workers keep a tab on their development post intervention.
A disabled adolescent or one with chronic illness might benefit from web-based intervention. It might also appeal to someone who has taken up full time employment or returned back to school. We are currently developing a Moodle based mhGAP and IPT-G training for health care workers keeping the COVID-19 related restrictions in physical meetings and workshops and to make it more efficient on health care workers’ time.
Importance of Dose-Full vs Brief
Whilst not immediately clear at the moment, but the formative adaptation inquiry and later implementation effectiveness trial might also help in understanding the categories of adolescents who might benefit from full versus brief intervention. Practical constraints demand those interventions be made briefer, more accessible and made catchier using digital or multimedia modalities. However, clinical needs of this complex population also necessitate offering them a full dose of the intervention that is unadulterated with other distractions (see figure 2).
Serving an Underserved Population of Vulnerable Adolescent Girls
Ultimately the intervention has to demonstrate internal and external validity in being relevant and suitable to the needs and concerns of depressed adolescents dealing with pregnancy and impending motherhood. For adolescents as young as 13–15 years, this would be a significant transition and incorporating information, support, and mental health and maternity care components would be paramount.
Tension Between Implementation With Fidelity and Successful adaptation
This is one of the biggest fault-lines in mental health implementation research. Our approach is to develop strong practice-policy-research partnership and engagement so that adoption of group IPT as an evidence-based practice comes from a health system, its providers and key decision makers who are on board with the ideas. The testing of IPT-G with a joint nurse practitioner and community health worker delivery approach, has its challenges but it also offers an opportunity for joint regulation, oversight on delivery process. We will work towards identifying strategies that bolster participation and adherence to key IPT-G thematic areas and delivery pathways. There is a delicate balance between contextual needs that shape adherence to intervention and those that would allow understanding the spirit of the intervention including developing sound competency structure.
Training and Supervisory Structure
In order for this intervention adaptation and ultimately for the intervention uptake to be successful, the overall approach is to think about multilevel capacity building along the lines of WHO mhGAP and Kenya mental health policy guidelines recommendations. The recommendations include a master TOTs structure for health facility and community stakeholders including repeat, structured trainings on WHO mhGAP 8 priority conditions. This is then infused with provider self-care, patient-centered care, psychological first aid, ethical and responsive communication modules, as well as WHO QualityRights training. The trainings are differentiated for community health workers and non-specialist health workers. A special orientation is held for specialist health workers such as psychiatrists and psychologists who are part of implementation process and at times key policy makers are included in this orientation. The purpose of these extensive trainings is to offer a pipeline that connects from the ground level basic services to highly specialist services at the top of the WHO care pyramid.
Conclusion
Cultural and psychometric issues around adaptation and modifications of evidence-based interventions have been refined over last decade or so. EBIs developed in high income or global North contexts need substantial adaptations before these can be tested in culturally varied or in LMIC contexts. IPT is a widely acceptable and culturally congruent approach that has proven feasibility, clinical effectiveness, and acceptability in Sub-Saharan African contexts. Adaptations that stay true to the core values of the original intervention and at the same time be delivered in viable, culturally relevant manner poses challenging issues around fidelity and quality of training/dissemination issues. The paper outlines these challenges as well as brings out strategies to balance questions of adaptations, fidelity, and intervention modification for peripartum adolescents in Kenyan primary care settings.
Footnotes
Acknowledgments
The authors would like to thank Nairobi County health directorate, Ministry of Health, UNICEF (Fatima Gohar, Joanna Lai) UNFPA (Ademola Olajide, Lilian Langat), WHO Kenya country office, Kariobangi and Kangemi health facility staff, Samuel Kiogora from Ministry of Health Kenya and NIMH and Fogarty program officers and The authors would like to thank Obadia Yator, Martha Kagoya and Vincent Nyongesa for their research support to this study. Special thanks for due to Myrna Weissman and the wonderful exposure to the ISIPT 2019, 2021 meeting clarifying fundamentals of IPT and welcoming testing and adaptation of IPT in LMICs. Thanks to Sahiba Turgesen for her editorial assistance. Discussions with Geoff Curran, Laura Damschroder, Bruce Chorpita and Enola Proctor have been very helpful in refining the implementation questions. The authors would like to thank Darius Nyamai for his editorial assistance and analysis of transcripts.
Author Contributions
MK developed the paper, MMK and HKY helped in conceptualizing the original study’s specific aims and methodology, and CO, SS, IP, and JU are mentors on this study and they contributed to the development of the research study and they all read and approved the draft. NC, SW are collaborators in providing technical assistance on use of mhGAP and IPT manuals published by WHO. HV, NG, and RL are collaborators on the IPT adaptation in this study and they all read human subjects’ sections and approved the paper.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Fogarty International Center of the National Institutes of Health under Award Number K43TW010716. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The first author was funded by Fogarty Foundation K43 grant (2018-2023) and the co-authors are her mentors or collaborators on this study.
Ethics approval and consent to participate
The study which has been approved by Kenyatta National Hospital/University of Nairobi ethical review committee (approval no. P694/09/2018). The study received approval from Nairobi County health directorate (approval no. CMO/NRB/OPR/VOL1/2019/04) and approval from National Commission for Science, Technology and Innovation (NACOSTI/P/19/77705/28063). The informed consent to participate would be sought from all study participants including stakeholders and advisory committee members from whom data would be collected.
Consent for publication
All study participants would be asked for their consent to publish the findings of this work. The key study participants and their family member data would be anonymized, and the personal information would be kept confidential.
Availability of data and material
NIMH funded research requires the data to be made available in publicly available. The data from this study would be made available on repositories such as Clinicaltrials.gov, RDoCdb, FIC webpage. All the personal information would be de-identified, and the data put on excel sheets for research use. Some interview transcripts would be kept by the researcher and may be shared on reasonable request.
