Abstract
Aims:
This study examines factors potentially contributing to unattended mental health needs among primary care patients in Lebanon’s Shatila Palestinian Refugee Camp in order to understand the prevalence of such needs and improve clinical practice with refugees and other vulnerable groups.
Methods:
Data collection (2012-13) involved researcher administered structured surveys of primary healthcare-clinic patients (n = 254) using the K6, the PC-PTSD, and the Modified-MINI mental illness screens. Chi. Sq., ANOVA and Principal Component analysis evaluate associations and differences in sample characteristics; Logistic regression evaluates factors associated with unattended-positive-mental-health-screens.
Results:
The sample (n = 254) included 55% females and 45% males; aged 18 to 89, M = 40.4 (±13). About 51.6% (n = 132) screened positive for mental illness, for these individuals only 11.4% (15 of 132) spoke to their physician about mental illness or had an acknowledged record of psychological problems. Thus 88.6% (n = 117) of those who screened positive, had unattended positive-screens. Univariate tests indicated that patients with “negative-screens,” those with “attended positive-screens,” and those with “unattended positive-screens” differed in their social and psychological characteristics as well as their relationship with the primary care setting. Overall multivariable Logistic results indicated that patients with unattended positive-screens were 34% less likely to have higher SES scores for each step up in status [OR = 0.66; CI: 0.48-0.89] and 58% less likely to have access to a provider for advice or assistance [OR = 0.42; CI: 0.20-0.88]. They were 2.2 times more likely to be females [OR = 2.20; CI: 1.22-3.95], and 5.26 times more likely to attribute their mental illness to a physical illness [OR = 5.26; CI: 2.36-11.74].
Conclusion:
Large numbers of patients screen positive for mental illness who do not have their mental health need addressed during their primary care visit. This seems an issue rooted in a lack of psychoeducation about what is mental versus physical illness, female specific access to care, stigma toward mental illness, and cross-SES-communication. Improved communication in primary care, especially as it serves vulnerable refugee populations might significantly reduce the prevalence of untreated mental illness.
Differences between true and treated prevalence are often attributed to factors inhibiting patient access to medical care. 1 In primary care settings, an “unattended mental health need” can be defined as the extent to which a serious mental illness (SMI), extant during a patient contact, remains unaddressed, unrecognized, undocumented, or absent from consideration. It is an index of a mental health service gap extant among patients who have accessed a service provider but whose SMI remains unattended to. 1 While, the integration of mental health care and primary care is an objective of first world nations,2,3 in most Middle Eastern countries, given the limited number of specialist providers, it is the default norm. 4 In Lebanon, 17% of the general population met criteria for at least 1 DSMIV/CIDI mental disorder, while only 10.9% have obtained mental health treatment. Two-thirds of that treatment was provided in the general medical sector. 4 No estimates are available as to the numbers of patients actually accessing primary medical care whose mental illness remains unattended to during their primary care visits—that is where mental health treatment could have been offered but was not. This study will determine the prevalence of such mental health need in primary care in Lebanon’s Shatila Palestinian Refugee camp and consider the relative importance of various factors associated with this lack of attention to mental illness.
Shatila, though largely populated by Palestinians, is home to new Syrian refugee arrivals and non-refugees, all having experienced armed conflict. Refugees and other populations exposed to armed conflict and displacement are at elevated risk for poor mental health and have evidenced high rates of acute stress and chronic mental disorders. 5 Socioeconomic disadvantage, another factor associated with poor mental health outcomes particularly in protracted conflict-effected situations, often characterizes the refugee situation. In Middle Eastern countries, conflict has impacted 85% of the population. 6 Shatila has seen a range of armed conflicts since its establishment in 1949. Shatila houses 25 000 people in a single square kilometer, wherein 60% to 80% were living below the poverty line. There are no municipal services, insufficient housing, Lebanese legal restrictions on employment opportunities, and prohibitions against owning property for Palestinians and Syrians.7-9 Yet Shatila has provided a source of inexpensive housing, where other non-refugee groups have found a home. It is not fenced in; it is a Beirut neighborhood described “. . .as a refugee camp pulsating with energy. . .where community life is lived in the streets. . .a jumble of concrete buildings, set at odd angles to one another, canopied with tangled electric wires and dank with poor drainage. . ..[where] shoppers jostle among bins of bright eggplants and peppers that overflow into walkways between market stalls, and hawkers chant discounts as sunset approaches, [and where] among long-time residents, . . .new layers of community are growing as Syrian refugees. . .[join the mix and] form their own networks.” 10 A prevalence study of Burj-el-Barajneh Palestinian refugee camp, near Shatila, found 29% of patients diagnosed with a mental disorder. Among patients using Burj-el-Barajneh’s specialty mental health clinic, 28.8% experienced depression, 15.6% anxiety, and 11% psychotic symptoms. 11 Although nongovernment organizations and the United Nations Relief and Works Agency in Shatila offer primary health care, specialty mental health treatment is unavailable within the camp.
Withchen et al 12 note that despite their high prevalence “it is paradoxical that mental disorders in primary care—and the way they are managed—remain poorly studied (p. 116).” They further indicate that most of the study has been confined to western nations. Only 1 major international study has directly addressed the question of prevalence, recognition, and treatment of a wide range of mental disorders in primary care. This benchmark study is the WHO study Psychological Disorders in Primary Care, and was conducted in 18 countries in the 80s. 13 In terms of recognition and treatment, the study revealed that GPs recognized only 49% of the mental disorder. Moreover, only about half of all cases recognized received some specific intervention. There was also considerable variation between countries in terms of prevalence, recognition, and treatment. Given the elevated risk for poor mental health of individuals exposed to armed conflict, the extensive refugee populations in camps around the world, and the total reliance of the Shatila population on primary care for addressing mental health problems, it seems important to consider the prevalence of mental health need and factors associated with how it is addressed in the Camp.
Methods
The University of California, Berkeley, Mental Health and Social Welfare Research Group’s Mack Center on Mental Health and Social Conflict project completed data collection involving researcher-administered surveys at 2 primary-care clinics in Shatila between June 2012 and June 2013 (n = 254). Patients, ⩾18 years of age, were recruited in the clinic waiting rooms via convenience sampling. Of the 290 whom were approached, 87.6% gave informed oral consent. Surveys were administered in private areas. Committees for Human Subject Research at all participating institutions approved study protocols.
Instruments and Measurement
The structured, 7-page-survey required 30 to 45 minutes to complete. It inquired into participant mental health and into potential factors contributing to their mental health status—participants’ demographic characteristics, social circumstances, medical history, and health behavior. Information on patient attitudes toward the mentally ill and religious beliefs was obtained only from the last 135 interviewees—questions were added to the study given feedback from initial interviews.
The K6, a screen for severe mental illness (SMI) was developed by the Harvard School of Medicine with support from the U.S. government National Center for Health Statistics 15 (the Arabic K6 version was previously validated for use in Lebanon). 16 K6 responses about symptoms are standardized via a 5-point-Likert scale ranging from 0 = “All the time” to 5 = “None of the time”—higher scores indicating the absence of symptomology (reverse coded from the original 15 version). The scale does not address psychotic symptomology. Scores for the 6-item screen range from 6 to 30. A K6 score of 6 to 18 is considered a positive-screen for SMI. The K6 reliability measured by Cronbach’s alpha is .88; its sensitivity and specificity .36 and .96, respectively, against structured diagnostic interviews with a score of 18 and lower for diagnosing the presence of any 30-day DSM-IV disorder. 17 These statistics replicate those initially reported by Kessler et al. 15 K6 reliability in the current sample was Alpha = .84 (N = 254).
The PC-PTSD is used in medical settings in the U.S. and among veterans to screen for PTSD.
18
It documents participant-reported PTSD symptoms employing a dichotomous Yes/No response. PC-PTSD has showed good internal consistency (α = .87), test-retest reliability (
A Modified-Mini Screen based on The Mini International Neuropsychiatric Interview (MINI); Schedule C14,21 was used to assess the presence of psychosis. It is described as having good to excellent reliability with Kappa ⩾ .75 for most diagnoses as well as support for its validity.14,22,23 Three Yes/No questions addressing negative symptomology associated with Schizophrenia (significant flattening of affect, alogia, and avolition prominent during the interview) were added to the 7 positive symptomology questions (related, for example, to hallucinations or delusions) in the Modified-Mini.
A score ⩾6 was deemed to place a person “at moderate likelihood of having a mental illness [that required] further clinical assessment.” 21 The Scale’s reported sensitivity and specificity are respectively: 80% and 97%. 24
Health status measures included a
Also considered was a measure of
Primary care characteristics measured included indications of whether the
We measured obstacles to primary care which included indications of a patient’s belief that the
Patient beliefs about mental illness measures included: The
Also measured was the patient’s belief in
Demographics and social circumstance measures taken into account included:
Other social circumstance measures included were
Data analysis
The data were analyzed using IBM SPSS Statistics version 26 (2020). Univariate statistics, Chi Square, and 1-way ANOVA, were used to assess sample characteristics; Principal Component analyses to create socioeconomic status (SES) and health measures; Logistic regression to determine which factors were associated with membership in each of the 3 potential screening outcome groups—that is, those who “screened negative for mental illness,” who had “attended positive-screens” and those with “unattended positive-screens.” The multivariable approach (using only those variables with information available for the total sample (n = 254)) regressed “unattended positive-screen status” on: participants’ health scores, the patient’s relationship with the primary care clinic, and the obstacles patients reported to receiving medical care—taking into account their demographics and social circumstances—as a means of determining the relative importance of these potential factors. Two of the 3 refugee membership groupings were included in each model, the third being the contrast. In order to ensure that no differences were accounted for by variance in the contrast group, the models were rerun rotating the contrast. The process did not alter the results thus 1/0 variables for Palestinians and Syrians with the non-refugees as the contrast are reported herein.
Results
The sample (n = 254) included 55% (n = 140) females and 45% (n = 114) males, aged 18 to 89 (Mean = 40.4; SD = 13); 73.9% (n = 187) were married; 72.5% (n = 185) reported less than a high school education; 18% (n = 46) reported no education at all. On average people lived in the camp for 21.1 years (±17), and were more likely to report having stable housing 63.4% (n = 161) than not (see: Table 1).
Demographic, social, disability characteristics, and beliefs of primary care patients by their mental health screen status and patient service outcomes.
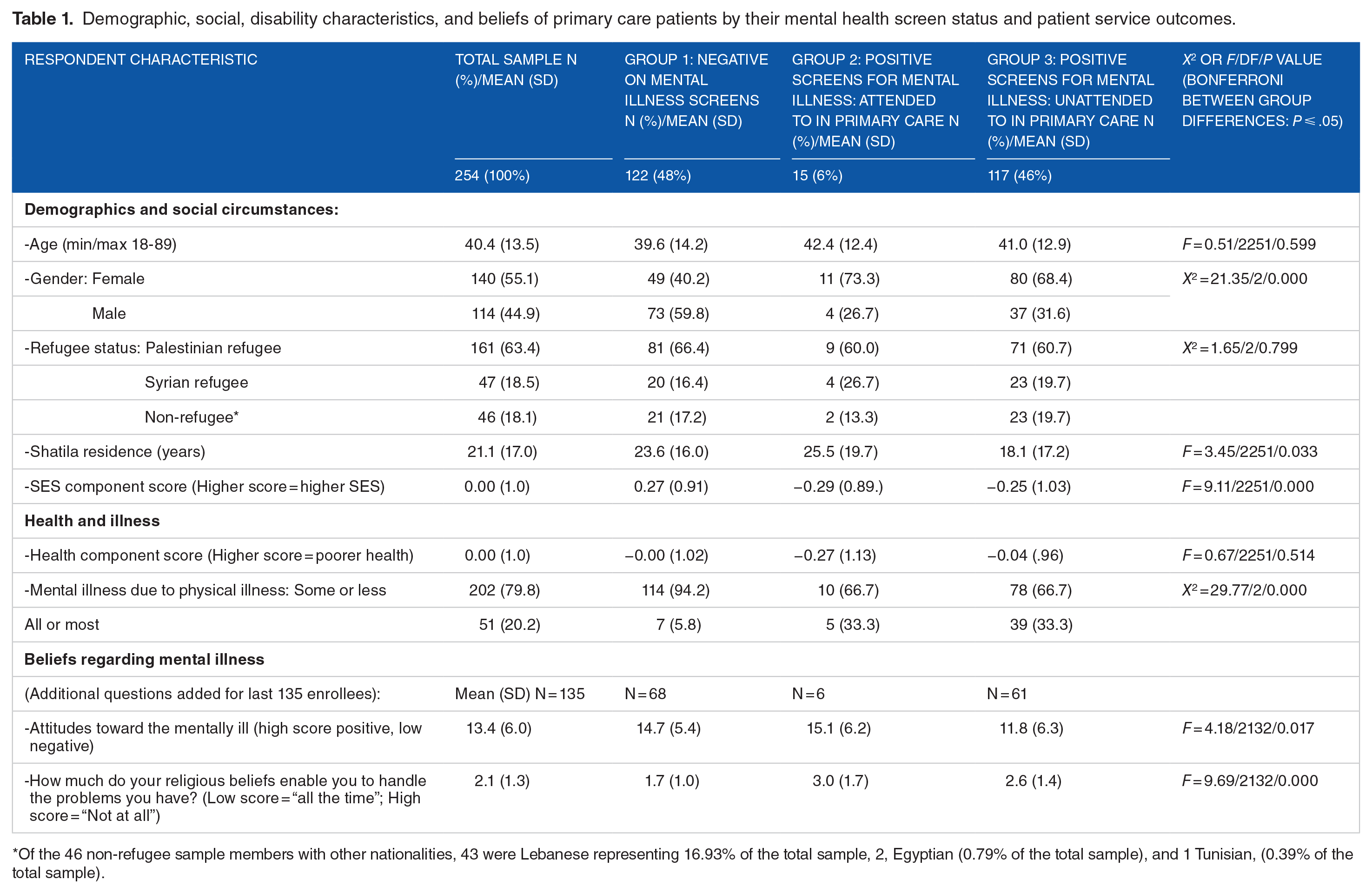
Of the 46 non-refugee sample members with other nationalities, 43 were Lebanese representing 16.93% of the total sample, 2, Egyptian (0.79% of the total sample), and 1 Tunisian, (0.39% of the total sample).
Fifty-two percent (N = 132) had positive screens for mental illness; 35%, SMI-alone; 5%, PTSD-alone; 11%, co-morbid-SMI/PTSD, and 0.1% co-morbid-psychotic-spectrum-disorder-SMI-PTSD.
Of those who had “positive-screens,” 11.4% (15 of 132) reported speaking to their physician about mental illness or had an acknowledged record of psychological problems. Thus, according to patient self-reports, 88.6% (n = 117) of the cases that had positive-screens were cases of unattended to mental illness. Of these 117 cases: 98 (83.8%) at the time of interview had mental health conditions that were the “same or worse than usual,” and 51 (43.6%) had greater than 2 weeks during the past thirty days when they were unable to work because of their mental illness. None of these statistics differed significantly between those 15 individuals whose mental illness was addressed and those in the unattended to group.
Patient reported characteristics of the primary care service and obstacles to care.
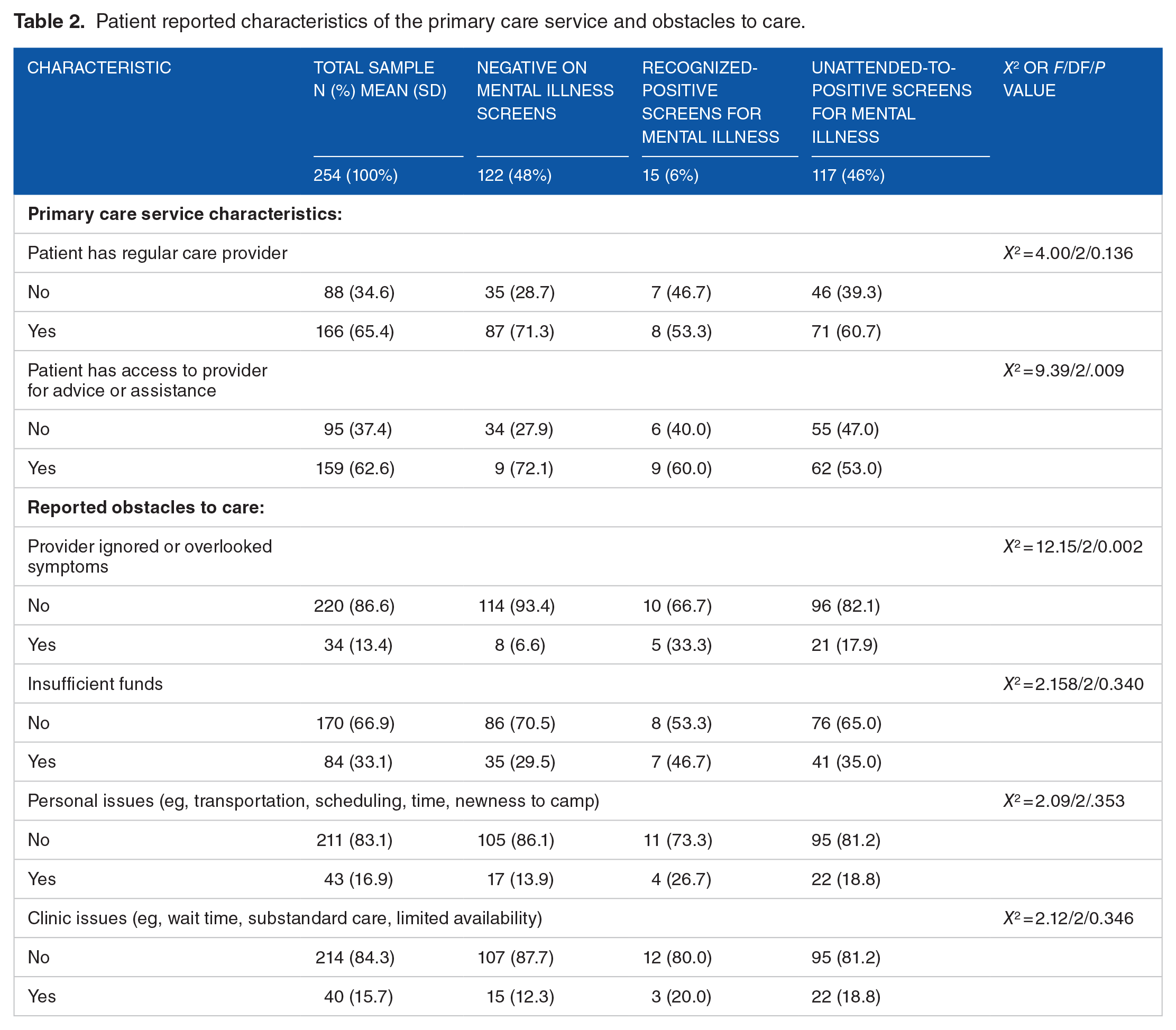
“Negative-screens for mental illness” were distinguished by being less likely to be female [OR = .30; CI: 0.18-0.51], to believe that their religious beliefs enabled them to handle their problems [OR = .55; CI: 0.40-0.75] and that their provider ignored or overlooked symptoms [OR = 0.29; CI: 0.12-0.66]. They were more likely to be longer-term Shatila-residents (2% more for each year) [OR = 1.02; CI: 1.001-1.032], with higher SES scores [OR = 1.73; CI: 1.33-2.26], to believe they could contact a provider for advice and assistance [OR = 2.13; CI: 1.21-1.72], and to have more positive attitudes toward the mentally ill [OR = 1.08; CI: 1.02-1.14].
“Attended positive-screens” were distinguished by being most likely to be females [OR = 2.93; CI: 1.66-5.15], having lower SES scores [OR = 0.62; CI: 0.46-0.83], reporting their psychological symptoms were due to physical illness [OR = 6.57; CI: 2.74-15.75], and believing that their provider ignored their symptoms [OR = 3.50; CI: 1.52-8.06].
“Unattended positive-screens” were distinguished by having fewer years of Shatila residence [OR = 0.98, CI: 0.96-0.99], having less access to a provider for advice or assistance [OR = 0.44, CI: 0.25-0.74], having more negative attitudes toward people with mental illness [OR = 0.92, CI: 0.86-0.98], and more faith that their religious beliefs would enable them to cope with psychological problems [OR = 1.60, CI: 1.21-2.12].
The multivariable Logistic model (see Table 3) considering all available factors with sufficient responses from participants, indicated that patients with unattended positive-screens were 34% less likely to have higher SES scores for each step up in status [OR = 0.66; CI: 0.48-0.89] and 58% less likely to have access to a provider for advice or assistance [OR = 0.42; CI: 0.20-0.88]. They were 2.2 times more likely to be females [OR = 2.20; CI: 1.22-3.95], and 5.26 times more likely to attribute their mental illness to a physical illness [OR = 5.26; CI: 2.36-11.74]. (“Attitudes toward the mentally ill” and “religious coping with psychological problems” were not included in the model given the limited number of respondents who were asked to address these questions.)
Factors contributing to unattended to serious mental illness in primary care (N = 254).
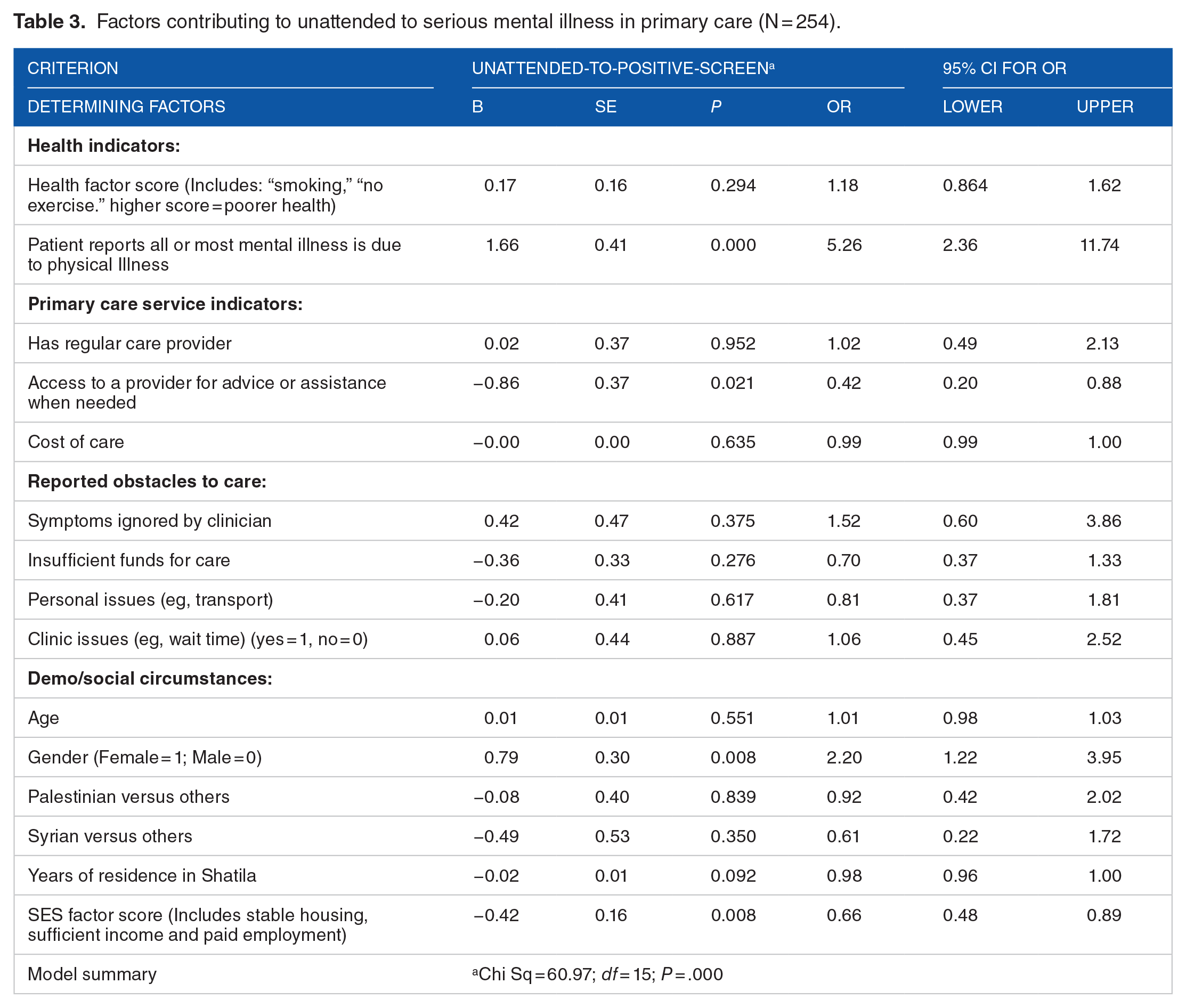
Discussion
This study examined factors potentially contributing to unattended mental health needs among primary care patients. The finding of 51.6% screening positive for SMI, PTSD, and psychotic-spectrum disorder with high comorbidity in a primary care setting is a clear indication of an under-resourced system that requires greater attention to mental health needs of presenting patients. This is especially true since the major survey of the mental health needs of the Lebanese population reports that two-thirds of mental health treatment in Lebanon is provided in the general medical sector. 4 Given this assertion, it is especially problematic to note that 88.6% of those with positive-screens for mental illness were in the unattended group. Study findings further indicated that these conditions were stable and disabling with 83.8% of participants reported as being the “same or worse than usual” and 43.6% involving periods of greater than 2 weeks during the past 30 days when the patient was unable to work because of their mental illness. These results are confirmatory of the conclusions previously reported in the literature indicating that such patients remain inadequately diagnosed and treated27-29 despite recognition of the issue and attempts to provide resources to cope with the disease. 3
While most of the factors considered with respect to unattended status generally distinguished between positive and negative-screens, most notable among the study findings is that unattended-positives are distinguished from other patients with or without mental illness by the patient’s perception that they do not have access to a provider for advice and assistance. Lack of such access increases the likelihood that their mental illness will go unattended by 58% and appears to be a communication issue in service provision. While this result may (given the univariate results) be partially attributable to the patient’s newness to the service, the lack of significance of camp residence duration in the multivariable model puts the burden on the communication itself—that is, that patient’s perception that despite visiting the primary care clinic and seeing a physician they do not have access to a provider for advice and assistance. It further offers what appears to be a new approach to this problem not addressed in this literature; one where patient/provider relationship building associated with improving communication skills needs to be a focus of future interventions. Such an approach would focus on efforts by the physician to enable patients to seek advice on their conditions and to engender trust that the physician is not ignoring or overlooking their symptoms (a factor 3.5 times more likely to be reported among positive-screened patients in this study). Such reports may involve what has been referred to as “diagnostic overshadowing”—that is “. . .when symptoms of physical illness are attributed to the service user’s mental illness, increasing the risks of treatment delay and the development of complications”—a phenomena that engenders mistrust and is sometimes an excuse for failure in primary care to attend to the needs of persons with mental illness. 30
The results also confirm the importance of attitude toward mental illness, significantly negative in the Middle East, as a factor in unattended need.31-33 For each point in the negative direction on the 20-point range of the attitudes toward mental illness scale, there was an associated 8% increase in risk of becoming an unattended positive-screen, one standard deviation increased one’s risk by 48%. The importance of significant self-stigma, indicated in the attitudinal response of the unattended positives might be the focus of relationship building interventions as well. 25
The strongest predictor in the multivariable model of unattended-positive-screen-status was the belief that the patient’s psychological symptoms were due to their physical illness. It increased the probability of an unattended positive screen by more than 5-fold. It is a clear indicator of a need for psychoeducation in the communication process. The importance of such psychoeducation in ensuring the proper course of treatment cannot be underestimated—depression, prevalent among the study’s positive-screens leads to failures in treatment compliance, lack of attention to one’s on-going health requirements, and to “giving up hope”—a key factor in patient recovery from any physical illness. Failure to attend to the psychological component of physical health care is a clear factor in negative outcomes in treatment.34-36
What is of most concern is where and with what group of patients these mental health needs are going unattended. There is considerable agreement that the risks of developing mental disorders such as depression, anxiety, post-traumatic stress disorder (PTSD) and psychoses are greater among migrant populations in general5,37 and those experiencing forced migration in particular. 38 Forced migrants including refugees, the people of Shatila and—if we may be so bold to infer from this project’s findings—others, including asylum seekers, who have experienced torture, armed conflict, and human trafficking (for slavery or sexual exploitation), require approaches that are different from those used for the rest of the population. 39 Certainly, they require increased attention to their mental health needs in primary care settings, usually the only place to which they can bring these concerns.
Finally, only compounding the need are the continually recurring risk characteristics—female gender40,41 the second strongest factor and lower SES42,43—remain important indicators of need for patient outreach as they add to the probability of having an unattended mental health condition.
Limitations
Conclusions based on the study findings are inferential from the study sample, cross-sectional, and locked in a point-in-time. The PC-PTSD given previous reports should have had a better α (internal consistency). The K-6 may have insufficient sensitivity and a too large (close to 100%) specificity, potentially yielding a heightened risk of false negatives assessed by this instrument. This however would imply that our finding of significant numbers of unattended positive-screens is a conservative estimate. The reported factors contributing to unattended mental illness are associations, not established causation. These findings however document the extent of the problem. They are consistent with clinical and empirical reports of obstacles related to failures to recognize and treat mental illness in primary care, and they offer new points of intervention for improving the recognition of mental health need in primary care settings.
Conclusion
A very large number of primary care patients are screening positive for mental illness and do not appear to have their mental health care needs attended to during their service contact. Their unattended mental illness status can result from a lack of access to a provider for advice and assistance—a communication issue in service provision that may be partially attributable to their newness and limited availability of the service, as well as significant self-stigma, and compensation by reliance on their faith to enable their coping with their psychological issues. It would appear that increasing the availability of access to primary care and a focus on improving communication around mental health issues through psychoeducation in the primary care setting would significantly increase the visibility of psychological problems among primary care providers, address the psychological components of physical health care, and perhaps greatly enhance all health outcomes.
Footnotes
Funding:
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The research was funded by the Mack Center on Mental Health and Social Conflict.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Availability of Data and Materials
Data will not be shared given initial agreement with data gathering sites.
