Abstract
Introduction:
Postpartum depression affects mothers at 4 to 6 weeks after delivery. Adolescent pregnancy can lead the expectant girl to drop out of school, receive poor obstetric care, and family support. Adolescent mothers are prone to severe postpartum depression as compared to older women. Early sexual initiation increases the risk of unintended pregnancies and potentially increases HIV exposure. WHO recommends Group interpersonal psychotherapy (IPT-G) as an evidence-based intervention for use in both primary care and community settings. We will assess the acceptability and feasibility of community health workers (CHWs), delivering IPT-G among postpartum adolescents (PPA) living with HIV.
Method:
This is a pilot feasibility study testing CHWs’ delivery of IPT-G to postpartum adolescents and young women living with HIV who will be attending the prevention of mother-to-child HIV transmission (PMTCT) clinics in 2 primary care health centers. Young women aged 15 to 24 years and 6 to 12 weeks postpartum will be eligible for participation. Our study is a two-arm intervention implementation study with one receiving group IPT and another one treatment-as-usual (TAU). We intend to treat the TAU group so that we will offer IPT-G post-intervention. There will be 2 groups running in the 2 facilities. Depression will be assessed using the Edinburgh postnatal depression scale (EPDS); those with EPDS >10 become eligible for the intervention. Besides, HIV-related stigma would be screened using HIV/AIDS Stigma Instrument (HASI–P), and social functioning rated using the World Health Organization’s Disability Assessment Schedule 2.0 (WHODAS 2.0). CHWs will deliver IPT-G for 8 sessions (1 session per week). The intervention group will receive immediate IPT-G, and the wait-list control group will receive deferred IPT-G as part of our intent to treat the group.
Primary outcome measure and analysis:
Descriptive statistics will be used to compare changes in depressive symptoms, HIV-related stigma, and social functioning between baseline and 8 weeks, and between 16 weeks and 24 weeks. The changes will be explored along with the differences between intervention and treatment as usual groups reporting effect sizes (Cohen’s d). Longitudinal continuous outcome variables across the time points will be analyzed using the Generalized Linear Model. For qualitative data, any emerging themes from KIIs and FGDs will be identified: framework matrixes, queries, and cross-tabulations will be used to analyze and interpret the data in view of assessing acceptability and feasibility of IPT-G.
Ethics and dissemination
The Kenyatta National Hospital-University of Nairobi approved this study of Nairobi Ethics and Research Committee (Approval No. P97/02/2018). The findings will be published in peer-reviewed journals and also shared with Kenya’s National AIDS Control Council.
Keywords
Introduction
Depression and anxiety are the most common mental health conditions that co-occur with HIV, as documented in a recent meta-analysis of studies from Sub Saharan Africa (SSA) reporting a 24% prevalence of depression among people living with HIV. 1 Importantly, another meta-analysis found that depression treatment improves adherence to antiretroviral therapy (ART). 2 Poor mental health has also been associated with HIV disease progression independent of its effects on adherence to care. 3
Adolescent mothers have a higher prevalence of postpartum depression than adult mothers, with an estimated prevalence of postpartum depression in adolescent mothers ranging from 26% to 50%. 4 A study from Malawi found that adolescents living with HIV had a depression prevalence of 18.9%. 5 A similar study investigating mental health outcomes among vertically HIV-infected adolescents in Kenya found almost a similar depression prevalence of 17.8%. 6
HIV prevalence in female adolescents aged 15 to 24 years in Kenya has been reported at 4%. 7 Adolescent girls and young women (AGYW) in Kenya are 2 times more likely to be HIV positive than their male counterparts. 8 Common adversities for adolescents living with HIV are poor sexual and reproductive health (SRH) and service uptake, poor access to services, high exposure to sexual and gender-based violence (SGBV), stigma and discrimination, and often poor social and family support. Perinatal adolescents who are living with HIV experience multiple difficulties, which result in poor mental health. 9
The Kenyan Demographic and Health Survey (KDHS, 2014) reports women’s first birth at a median age of 20.3, which is similar to the median age (20.2) of their first marriage. 10 Youth initiate sexual intercourse at a median age of 18.0 for females and 17.4 for males. 11 Sexual initiation by age 15 is reported among 15% of females and 21% of male adolescents. 11 A pregnant girl faces losses in education and employment and may face challenges in future work. 12 Adolescent mothers from low-resource communities are often born to parents with low educational and employment attainment and may also have a history of early childhood traumatic experiences. Having poor social support networks severely affects psychological functioning and long term functioning. 13
Some studies have categorized risk factors for depression among adolescents living with HIV in 3 levels: (a) individual (age, gender, HIV diagnosis, and severity),14,15 (b) interpersonal (family support), and (c) structural or social factors (social support from peers, bullying from peers, or receiving support to ensure ART adherence). 16 Besides, a similar study has also reported social and structural factors, such as poverty, access to health, or education services as predisposing factors to depression in this vulnerable population. 17 All the above risk factors may lead to poor adherence to ART, sexual risk-taking, thus contributing to disease progression or transmission. 18
Implementation gaps include lack of personnel, poorly trained personnel, high workload, and lack of structured mental health services in primary health care settings. However, there is evidence that community health workers (CHWs) and nurses at primary health facilities could provide simple, evidence-based interventions that might impact the population. 19 The development of Kenya’s pledging 30% of all service delivery to be community-led BY 2020 will make it feasible to introduce tailored psychosocial interventions. 20
Interpersonal Psychotherapy (IPT) was developed by Gerald Klerman and Myrna Weissman in the United States in the 1980s to address interpersonal issues that they believed aggravated depressive illness. 21 World Health Organization (WHO) modified IPT into 8 group sessions with 1 pre-group session, which is individually conducted. This version can be administered by non-specialist personnel. 22 IPT focuses on improving interpersonal relationships and enhancing the social functioning of an individual. Its core principles focus on understanding grief and loss, role dispute, a role transition, improving social skills, and bolstering social support 22 (see Table 1).
Four (4) IPT problem areas.

IPT was adapted for depressed patients with differing characteristics and depression subtypes, such as adolescents. 23 Group IPT (IPT-G) has been delivered to women living with HIV (WLWH) in Kenya with the intention of scaling-up the intervention to address depression in women seeking HIV and GBV services. 24 The challenge here is the scarcity of trained personnel and optimizing group psychotherapies to address individual problems. Utilizing CHWs to administer IPT-G could improve coverage. 24 Such approaches would speed the translation and scale-up of mental health care for people living with HIV in LMICs. 25
In treatment studies, IPT reduced symptoms of depression and anxiety and improved relationship quality, social adjustment, and social support. 26 In a meta-analysis of 38 studies, IPT was effective, both as an independent treatment and in combination with pharmacotherapy, and the authors concluded that IPT is one of the most empirically validated treatments for depression. 27 This study is likely to yield findings that, in the future could inform scaling up of treatment in Kenya to other PMTCT clinics within primary health care low-resource settings.
Methods
Study design
This is a pilot feasibility study among postpartum adolescents and young adult women to assess acceptability, appropriateness, fidelity, adoption, and short-term sustainability. The IPT-G includes a total of 8 sessions: 1 session per week being delivered by primary health care volunteers in 2 county health care clinics in Nairobi.24,25
Study population and site
The study will be conducted at 2 primary health care facilities within Nairobi county, Kenya. The lead researcher will identify 2 community health assistants (CHAs) and 6 community health volunteers (CHVs) and carry out training and capacity building around depression diagnosis, mental health assessment using mhGAP guidelines, and IPT-G intervention. These CHVs and CHAs forms a team of community health workers (CHWs) who will help recruit, follow up, and deliver the intervention. Health facility staff will be engaged in tracking acceptability and feasibility of evidence-based depression care guidelines in primary health care (PHC). At county health clinics in Kariobangi and Kangemi, 24 postpartum adolescents (aged 15-24 years) at 6 to 12 weeks post-delivery and living with HIV will be recruited at the PTMCT clinic. Those with severe depressive symptoms with suicidal ideation will be excluded and referred to psychiatric facility for medication and we will report and keep a track of services provided to them.
Study objectives
We felt that no separate curriculum was needed as HIV stigma and adherence, psychosocial needs are mapped well on the IPT theoretical framework of transitions, loss, disputes, and isolation. Additionally, there are clear guidelines around HIV management in adolescent mothers and also around critical psychosocial needs of this group, which we have infused into group IPT. We intend to assess the implementation outcomes of IPT-G for this vulnerable population living with HIV, and our findings could inform the process of further adaptation once our study is completed.
The primary objectives of the study are the following:
To assess the acceptability and feasibility of IPT-G among PPA when delivered by community health workers;
To determine if IPT-G will improve adherence to ART as measured by viral load suppression and the CASE adherence index; and
To determine the effects of IPT-G on depressive symptoms (decreasing interpersonal stress and strengthening social support), HIV-related stigma (enhanced social skills, role transition, and interpersonal skills building), and social functioning (enhanced decision making, communication skills, and infant outcomes).
Recruitment and consenting procedures
Adolescents living with HIV aged 15 to 24 and who are 6 to 12 weeks postpartum will be recruited for participation. Study purpose, procedure, benefits, risks, and willingness will be discussed, and those who meet inclusion criteria will sign informed consent. Upon receiving ethical approval, authority will be sought from Nairobi county director of health services who will provide instructions to the facility in-charges through a routine demonstrative chain. The health center management (usually medical or nursing officer) of the 2 facilities will be informed on the nature and scope of the study. Health center managers will use their CHA to identify in 3 CHVs with a minimum educational level of Grade 12. Eligible CHWs who are willing will sign an informed consent form. A 2-day workshop on IPT-G Protocol will be conducted for all the CHWs. The clinical study supervisor will maintain continuous coaching and monitoring of their skills during the piloting period and even during the main study including meeting them prior to the sessions for practice and organizing supervisory meetings in groups and individually. Piloting of IPT-G among 6 postpartum adolescents will be carried out for 8 sessions to enhance the skills of the CHWs. The schedule of sessions will be shared with the study participants and contacts maintained through mobile phones.
After consent, EPDS will be used to screen depression among PPA with a cut-off score of >10, which is indicative of moderate to severe depression. A total of 24 pieces of papers will be allocated binary numbers 1 (for the intervention group) and 2 (for the wait-list control group) with 12 participants in each category group. Participants will randomly pick a folded piece of paper from the 24 pieces placed inside a box and those with numerical 1 will form intervention group and those with numerical 2 will form the wait-list control group (see Figure 1).
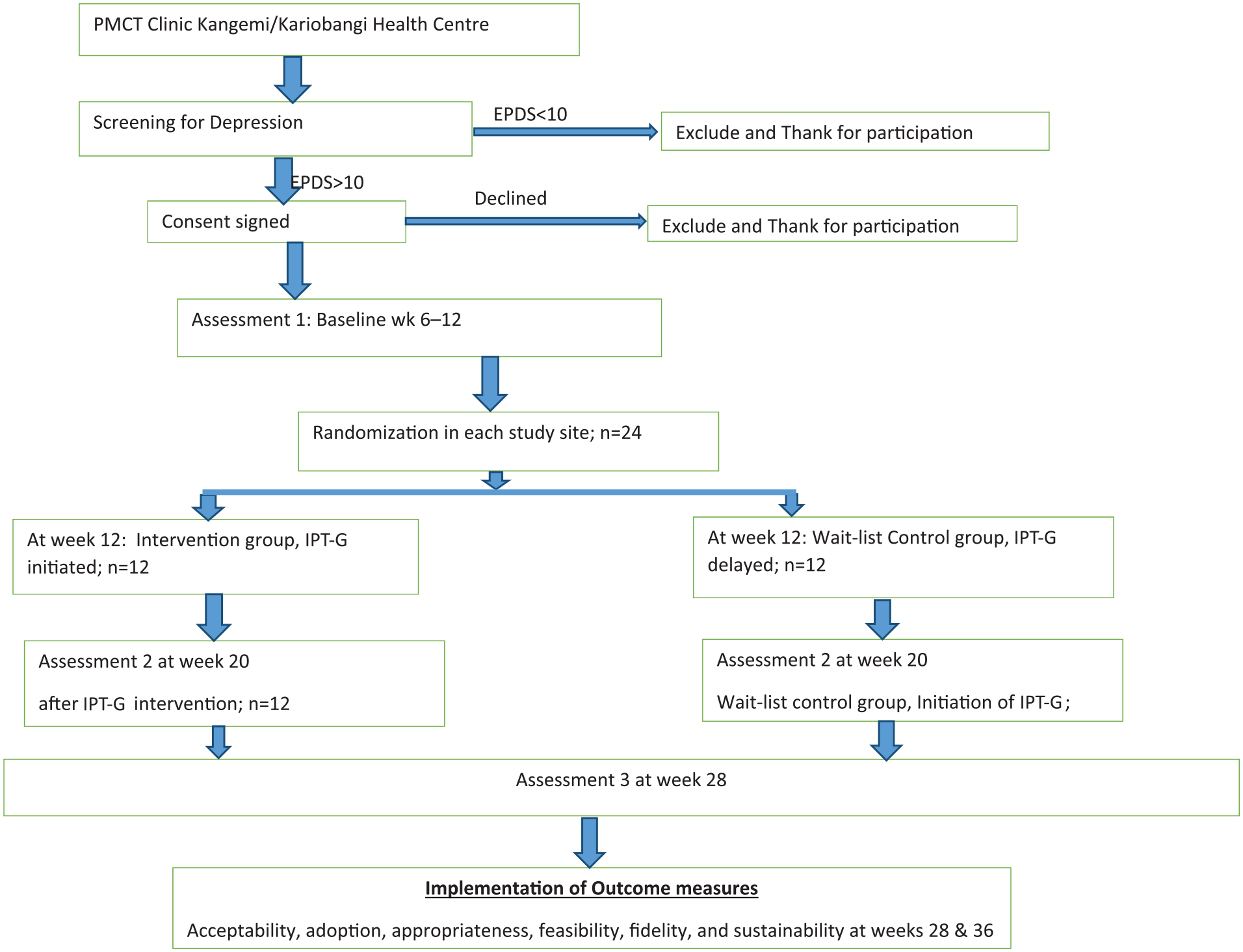
Implementation study flow.
Implementation framework description
In our study, we will use Proctor’s implementation evaluation model that looks into 3 outcomes of an intervention: Implementation (acceptability, feasibility, fidelity, appropriateness, adoption, sustainability); Service (efficiency safety, patient-centeredness, timeliness), and client (satisfaction, function, symptomatology). 28 Improvements will be examined at an individual level and within the providing system whereby our interest is to explore: (a) acceptability and feasibility of IPT-G, (b) time requirement, efficiency, and safety of IPT-G, and (c) individual changes in depressive symptoms, HIV-related stigma, and social functioning on comparing before and after IPT-G intervention delivery.
Both CHA and CHVs are categorized as community health workers and have formal education beyond primary school. They are 2 different cadres—one is formally hired in the health facility, and the other CHV are volunteers and not paid workforce. In LMICs, a lot of work is being tested for task-sharing by CHVs. CHAs have a more technical health background and could support the CHVs with ongoing mentorship and supervision on the psychosocial and community work. IPT-G will be administered by primary health care CHWs. Two-day training for CHAs and CHVs will be conducted by lead researcher, clinical supervisor, and the 2 research supervisors who are both IPT trained. After that, continuous supportive supervision will be maintained all through the weekly session to the completion of the study to monitor, address challenges, and mentor them. Before each session, there would be supervisory practice meetings, and after every session, follow up group supervision would take place to ensure that the IPT-G protocol is maintained.
Eight sessions of IPT-G for intervention group will be initiated at week 12 postpartum in the intervention group. Meanwhile, the wait-list control group receives treatment as usual (TAU), which is routine prevention of mother-to-child transmission clinic services tailored to postpartum mothers, as well as check-in with psychiatric nurses or clinical officers. If they detect depression, they will send the patients to the psychiatry clinic, which is run weekly by a team of specialists at the health facility. At week 20 postpartum among the control group, IPT-G will be administered, and a follow-up assessment using relevant instruments for all participants will be conducted at week 28 and 36 postpartum. IPT-G techniques, such as communication analysis and decision analysis will help address issues related to life events that trigger distress and matters HIV-related as non-acceptance of ones HIV status, considering oneself as being inferior due to HIV and justifying community discrimination based on HIV status which becomes themes that are linked to depression. 29 Hence this will empower the PPA at home and within the community. Effects from IPT-G will be ascertained by comparing scores of depressive symptoms, HIV-related stigma, and social functioning before, during, and after IPT-G intervention.
Intervention description
IPT-G has been developed into a manual by WHO for use in LMICs and it talks about 4 problem areas: life transition, loss and grief, conflicts/disputes, and loneliness/social isolation. Our work was to adapt it in an adolescent-friendly language and infuse information around HIV and HIV related care cascade, stigma to make the IPT themes, and group session planning effective. IPT-G sessions (90 minutes per session) will be administered weekly for 8 sessions as per the protocol. The IPT-G approach will aim to understand the current depression and link depression to current life events (problem areas) that influence interpersonal relationships and then obtain new ways to deal with existing problems. We will probably consider a more extensive follow-up study for adaptation of IPT-G to this vulnerable population while utilizing findings on barriers and facilitators from the current research. IPT-G techniques and approaches can be used to improve ART adherence and HIV-related stigma in adolescent mothers. We have trained our IPT-G facilitators in these techniques, and Kenyan PMTCT has good policies and resources for adolescents and women living with HIV to consider. 29 Each session will be composed of 6 participants. Our study participants are few and are PPA who are continuing with routine mother and child clinic follow-ups; hence the study is expected to progress as planned without any delay. Again, our sample size is small and thus easy to follow-up as these adolescents tend to stay around in the neighborhoods where we have recruited them. There isn’t a great deal of mobility with a little baby around, and we anticipate that it is easy to track them with the help of CHWs (see Table 2).
Group IPT tasks and session overview.
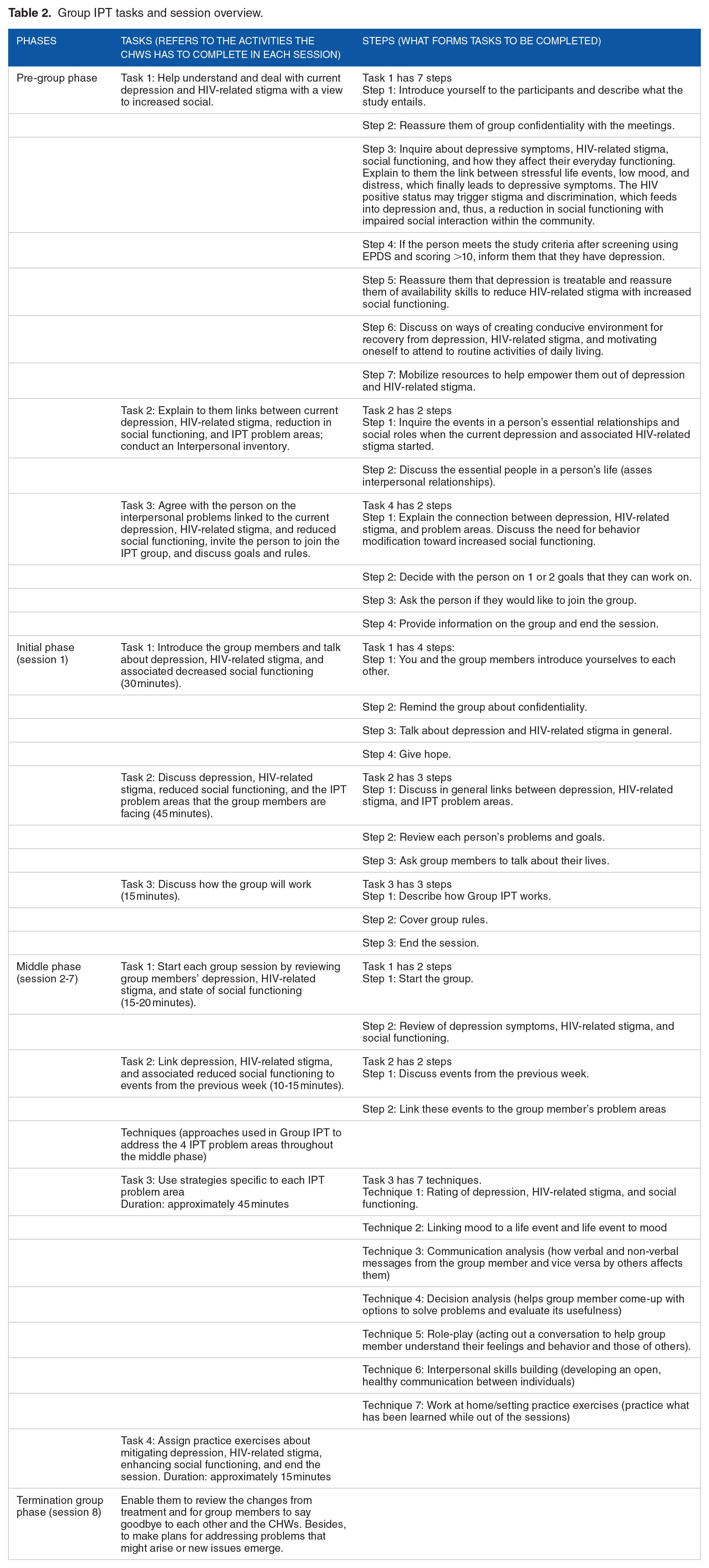
At 28 weeks, postpartum semi-structured qualitative interviews will be conducted among the participants to explore the general perception of the participants about IPT-G. The Clinical Outcomes for Routine and Evaluation-Outcome Measure (CORE-OM) will be administered in between sessions and also at the end of therapy to evaluate session wise functioning and improvement. Assessment of changes in postpartum depression in EPDS scores, HIV related stigma, and social functioning will be assessed. CHV facilitators will be assessed using the IPT-G fidelity tool and with structured qualitative interviews.
Data Collection Procedures
After approval by KNH/UON Ethics Review Board, National Commission for Science, Technology, and Innovation and Ministry of education, the recruitment process will take place at the 2 health facilities. One CHA and 3 CHVs will be identified for each study site. CHVs are respected and trusted by the community. Based on the fact that they live within the community, they understand the culture of the community they serve. CHWs will act as facilitators for intervention-IPT and recruit participants.
Each participant will be allocated a study code, and their personal details de-identified to enhance confidentiality. PPA found to have severe depression with suicidal ideations will be excluded from the study, and referral will be done for further mental health care. Participants will be given informed consent to sign. Three weeks before the rolling out of the intervention, depressive symptoms and the Interpersonal Inventory will be evaluated.
At the first intervention phase known as the initial group phase, the lead researcher will conduct a baseline survey for all the 24 participants. EPDS 30 will be administered to determine perinatal depression, and the impact event scale will be used to determine traumatic experiences and HIV/AIDS. Stigma Instrument–PLWHA (HASI–P) 31 will be used to assess HIV related stigma for postpartum adolescents living with HIV. Interpersonal connectedness will be assessed using the IPT inventory. 32 Pro-social behavior will be assessed using the WHO Disability Assessment Schedule 2.0, 33 viral load 29 and Case Adherence Index 34 will be used to assess ART adherence.
After completion of the first assessment, IPT-G for depression will be initiated with the initial group phase (session 1), which will systematically progress up to the termination phase (session 8). Appropriate strategies and tasks will be implemented as laid out by the IPT-G manualized guidelines. Subsequent assessments will be done in-between sessions at week 12, week 20, week 28, and week 36. The lead researcher will assess facilitators on fidelity and competency using the IPT rating scale and participant outcomes every week using CORE-OM. Feasibility and acceptability of the IPT-G within the health centers will be assessed through in-depth interviews, focus group discussions (FGDs). Also, observations recorded during the intervention process will be conducted.
On completion of IPT-G, in-depth interviews will be conducted in the 2 study sites to evaluate feasibility and acceptability. Sessions will be recorded with note-taking for cross-references when performing the data analysis process. After the IPT-G sessions, all participants will be referred to the USAID funded DREAMS project for self-help and livelihood training. 35
Sample Size
For pilot and feasibility trials, a formal sample size calculation may not be appropriate. 36 In this exploratory trial, the objective is not to prove the superiority of the treatment but to test trial procedures and processes and to get estimates of parameters for the main trial sample size calculation. 37 Using the current flat rules of thumb for overall pilot trial sample size, a minimum sample size of 12 subjects per treatment arm is adequate. 36 Through convenient sampling, a representative sample of 24 participants (12 from each study site) will be distributed randomly and half of this population will act as intervention group and the other becomes wait-list control group in view of achieving intent to treat using IPT-G.
Outcome Measures and Instruments
Socio-demographic and Clinical Questionnaire will assess the general health status of mother and infant, level of social support, age, marital status, educational level, and occupation.
Edinburgh Postnatal Depression Scale (with 10-questions) is suitable for assessing postpartum depression. 30 A cut-off of >10 will be used to screen postpartum depression where the responses are 0 to 3, and the maximum possible total scores are 30. A recent study on the validation of EPDS against both DSM-5 and ICD-10 diagnostic criteria for depression upheld that a score of 11 or more is the optimal cut-off. 38 The assessment tool has previously been used in Kenya in a similar study. 39 A study on developing and validating of EPDS in Kenya reported internal reliability ranging from 0.77 to 0.81. 40
HIV/AIDS Stigma Instrument—PLWHA (HASI—P). The instrument has 33 items and is used to assess HIV related in 6 areas: verbal abuse, negative self-perceived, health care neglect, social isolation, fear of contagion workplace stigma, and the total stigma arising from the sum of all the subscales. It was validated within 5 African countries Lesotho, Tanzania, Malawi, Swaziland, and South Africa. Internal reliability reported ranges from 0.76 to 0.90. 31 The mean response of each item was calculated and summed together to generate a score. Descriptive calculations included measures of dispersion.
Clinical Outcomes for Routine and Evaluation-Outcome Measure (CORE-OM) has 34 items to assess in 4 domains: well-being (4 items), symptoms or problems (12 items), functioning (12 items), and risks (6 items). 41 A recent study in the Kenyan sample working on factor analysis of CORE-OM across the 34 items reported internal reliability with a Cronbach’s α = 0.92. 42
Impact of Event Scale-Revised (IES-R) is used to assess Post-traumatic stress disorder (PTSD)/psychological distress following a traumatic event that has 5 responses 0 to 4 in a 22 items instrument. 43 A recent study that used IES-R to assess breast cancer knowledge and barriers to screening in Kenya reported internal reliability with a Cronbach’s α = 0.80. 44
Scores from all items are added together, and the sum total ranging from 24 to 32 represents mild symptoms of PTSD, 33 to 38 represents the best cut-off for a probable diagnosis of PTSD and scores of 39 and above depicts high enough symptoms of PTSD that can suppress the immune system. 43
WHODAS 2.0 (World Health Organization Disability Assessment Schedule 2.0) is a 36-item version, self-administered inquiring one’s social functioning in the last 30 days 33 and has 6 domains assessing disability in all of them. Item response theory-based scoring will be used and multiple levels of difficulty for each item and summary score by differentially weighting the items and levels of severity. A study done in Kenya on the effect of behavioral intervention concerning psychological distress among women used WHODAS 2.0 reported internal reliability with a Cronbach’s α = 0.66. 45
The Center for Adherence Support Evaluation developed the CASE Adherence Index, which is a good tool for assessing adherence levels while using Anti-retroviral Therapy. 34 It has 3 questions with score >10 that depicts good adherence and <10 signals for poor adherence. 34 A previous study in Kenya assessing determinants of adherence to ART among adolescents living with HIV at a comprehensive care clinic using the CASE Index reported high internal reliability with a Cronbach’s α = 0.696. 46
Testing ARTs Adherence Using Viral Load. CD4 and viral load will be extracted from the participant’s PMTCT clinic file. This will be undertaken during the initial session of IPT-G within week 6 to 12 post-delivery and thereafter at week 36 during the follow-up session. Virologic failure will be defined by a persistently high viral load of ⩾1,000 copies/ml at least after 6 months of using ART. 29
Interpersonal Inventory is an understanding of the client’s interpersonal relationship and level of interaction in a given context. 22
The Malawi Developmental Assessment Tool (MDAT) consists of 136 items and has good sensitivity (97%) and specificity (82%). The tool for assessing child growth and development contains 4 domains: gross motor, fine motor, language, and social domains of development, each with 34 items. Malawi, where the assessment tool kit was developed, and Kenya share socio-cultural similarities. Reliability was reported as Kappa (k) (K > 0.75) for 99%, which represents 134/136 of the items. We will construct normal reference ranges for the children of the participants passing items using logistic regression analysis against the decimal age as the explanatory variable. 47
Qualitative process evaluation alongside clinical outcomes will be used where FGDs and in-depth interviews will be used to assess acceptability, feasibility, fidelity appropriateness, adoption, and short-term-sustainability. During FGDs and In-depth interviews, audio recording, observations, and field notes will be compiled after each session. When analyzing the findings, common themes around PPD, HIV-related stigma, and social functioning will be generated.48,49 In-depth interviews will be conducted for selected participants and CHVs, and the health facility in-charges 50 (see Table 3).
Constructs and measures.
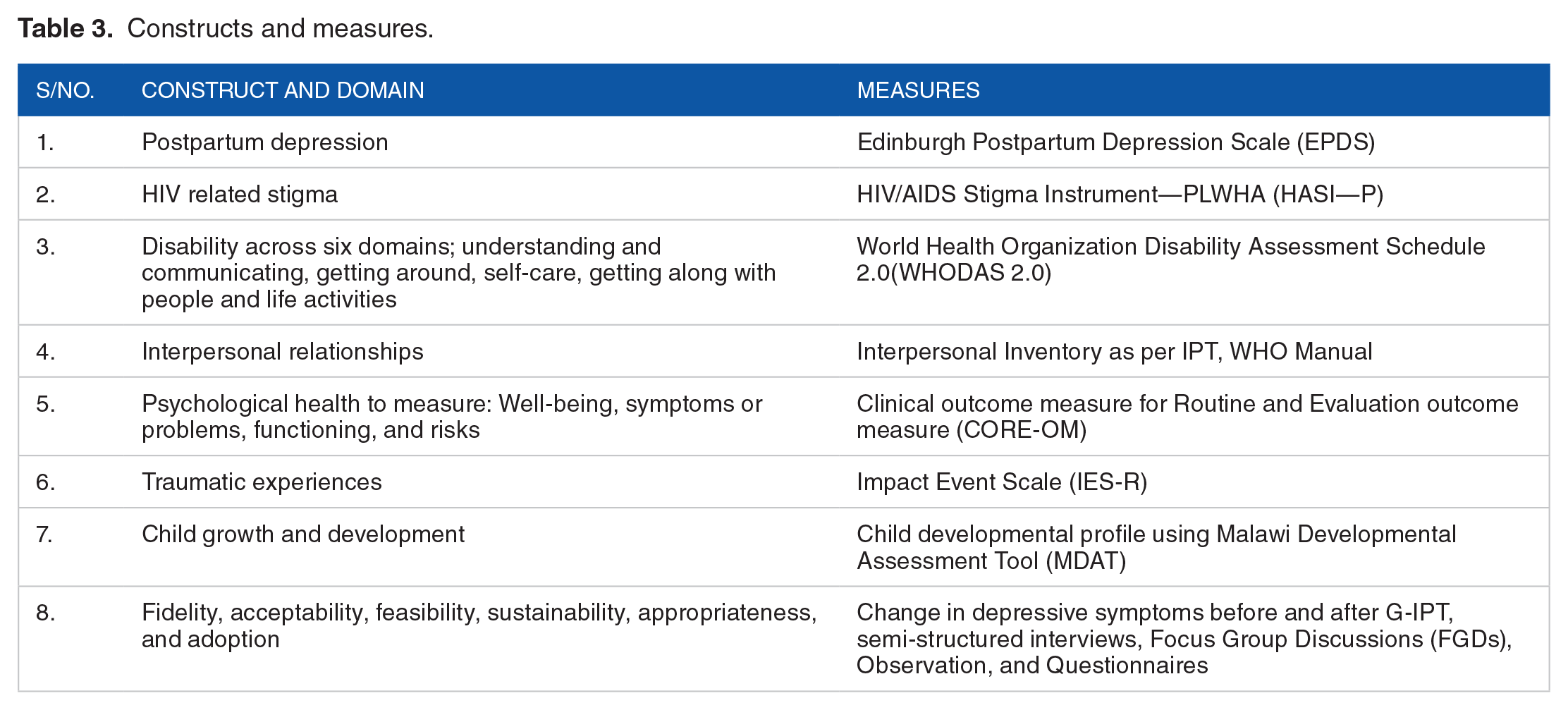
Statistical Analysis
Socio-demographic and baseline characteristics
Demographic data and both primary and secondary outcomes will be reported for each subject. Changes between baseline and 8 weeks and between 16 weeks and 24 weeks will be explored along with the differences between experimental and control groups reporting effect sizes (Cohen’s d). Comparisons will be made between groups at every point, whereas within groups, comparisons will be performed between baseline and specific follow-up, separate for every study group. Associations between potential confounders and effect modifiers will be tested in multiple linear and logistic regression models on continuous and binary outcomes variables respectively by testing the main effect, creating interaction terms, stratification, and carrying out adjusted and unadjusted analysis.
Longitudinal continuous outcome variables across the time points will be analyzed using the Generalized Linear Model (generalized estimated equations for continuous outcomes and mixed effect model for binary outcomes) to estimate the effect of variations due to groups (between-groups effect) and due to follow-up time (within-groups effect). Interactions between time and group will be assessed, and, in the absence of such an interaction, the overall difference between groups and across the 2 follow-up assessments will be calculated, reporting 95% CIs and P-values.
To investigate the effect of loss to follow-up on the intention-to-treat analysis, sensitivity analysis will be done by modeling response indicator and incomplete out variable, jointly using Heckman selection models. Secondary outcomes will be analyzed with the same procedures adjusting for baseline characteristics. All the necessary assumptions will be tested, and the findings will be reported before inferential statistics are calculated. Despite the sample size being underpowered, the findings of this study aimed to assess the feasibility of IPT-G being delivered by CHVs.
Qualitative data
Qualitative data will be collected using FGDs, key informant interviews (KII), and semi-structured questionnaires. FGDs will be done among 6 participants and 4 facilitators from each study site. KII from each study site will involve a health facility in-charge (nursing officer), PMTCT nurse, and mentor mother at PMTCT, CHA, 2 CHVs, and 3 participants. Mentor mothers are women living with HIV who have been trained to work in harmony with health workers and other peer educators with a view to help the HIV infected persons. They help mobilize adolescents who attend the PMTCT clinic. 51 Purposive sampling method will be used to select the study sample population for the FGD and KII. The researcher shall conduct FGD of 6 to 8 participants each for the following: participants, community health workers, and IPT-G therapists. The FGDs and KII will be recorded, after which the audio files transcribed for qualitative data analysis purposes. Detailed notes taken during the FDGs will act as a back-up for capturing the non-verbal communications. Qualitative data will be analyzed by Qualitative Solution for Research (QSR) NVivo 10, whereby all transcriptions will be uploaded in NVivo software and nodes created thematically using a grounded theory approach. Any emerging themes will be identified; framework matrixes, queries, and cross-tabulations will be used to analyze and interpret the data. The lead researcher shall document process outcomes to assess acceptability, feasibility, and fidelity of the intervention.
Data safety and monitoring
Coding and use of numbers will be utilized to protect the identity of the participant. Confidentiality of data, interviews, audio-recordings, and other documents for the study will be kept under a lockable cabinet and can only be accessed by those conducting the study.
For medical/clinical emergencies, MK, who is the senior author and also a Clinical psychologist and Senior Lecturer at the Department of Psychiatry-University of Nairobi, will be the key point person on psychosocial management. KL and JG will advise on matters arising from IPT-G processes during the entire study period. Referrals to Kenyatta National Hospital for specialized mental health care will be made for those participants deemed to have severe perinatal depression, anxiety, HIV related stigma, suicidal ideations, and participants whose children have a poor developmental profile.
Discussion
The results of this study will seek to demonstrate the efficacy of IPT-G to address depression in postpartum adolescents living with HIV. The intervention delivery by CHVs also provides a unique opportunity for care. The intervention strategy was developed in a participatory manner to ensure relevance and feasibility. This project brings together the researchers, PCH management, and health worker teams to ensure capacity development and multi-stakeholder participation in IPT-G. The use of CHVs and CHAs as facilitators and mobilizers could provide valuable information around how to scale up IPT-G services. There is no trained IPT persons integrated in the clinic team at the moment. We know that it can be integrated in primary care and there is enormous need to provide depression intervention since the health facility doesn’t offer any intervention. Based on our study and through task-sharing approach, we have championed, we will demonstrate its sustainability and will hope to have greater buy in by health facility in-charges and Nairobi county program officers.
Strengths of this study
➢ The study will address culturally specific alterations to the WHO recommended group IPT.
➢ This study will provide feasibility data to inform a subsequent clinical trial.
➢ This mixed-methods study will use participant qualitative interviews to supplement feasibility data providing additional insight into how postpartum adolescents and young women experience depression and how psychotherapy helps improve their functioning.
➢ This study will assess the pilot effectiveness of IPT-G when administered by community health care workers and provide pointers to task-sharing benefits and weaknesses.
➢ Addresses challenges of adolescent pregnancy, which is a novel area of research not previously investigated in terms of intervention implementation in Sub-Saharan Africa.
Limitations of this study
➢ The inquiry is not powered for a definitive study but offers only feasibility data.
➢ Our study sites are low-resource urban settings, which may not help replicate issues of rural populations of adolescents living with HIV or health facility-based task-shifting around psychosocial interventions.
Footnotes
Acknowledgements
Health center in-charge from each study site (Kangemi and Kariobangi), Prof Ruth Nduati of Department of M.Med (Pediatrics), University of Nairobi-Chair of the Advisory group and technical advisor in this study, Dr Alfred Osoti, Lecturer, Department of Obstetrics/Gynaecology, University of Nairobi (member), Dr Beatrice Amugune, Senior Lecturer Department of Pharmacy, University of Nairobi(member). Grateful to Martha Kagoya, MSc Clinical Psychologist, Department of Psychiatry, the University of Nairobi, who is the clinical supervisor to this study and Vincent Nyongesa, who was the research assistant for this study.
Funding:
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Manasi Kumar has received funding from Fogarty International Centre’s K43 TW010716
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Authors Contributions
YO is the lead researcher who is working on the study as part of his PhD dissertation and led the writing of the manuscript. MK, KL, and JG are the first author’s PhD mentors. All mentors assisted in the development of the intervention strategy, survey, design of the qualitative process evaluation, and analysis strategy. All authors participated in manuscript editing and approved the final manuscript.
