Abstract
Objectives:
Lasting, unexplained and high levels of pain may cause anxiety in patients with chronic fatigue syndrome. The objectives of the current study were to test assumptions of the association between pain and anxiety in patients diagnosed with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) and to clarify the role of depression in this relationship.
Methods:
Data were collected from 664 participants (age 18-65 years) with 133 ME/CFS patients and 201 healthy controls from Norway and 330 CFS patients from Spain. Binary logistic regression model was applied to test relationships between the included variables in the samples.
Results:
Both pain and depression made significant direct contributions to the level of anxiety. The strongest risk for higher levels of anxiety was the combination of high levels of depression and high levels of pain in the overall sample (OR = 49.70; P < 0.001), not so much in the Spanish cohort (OR = 11.99; P < 0.0001) and most of all in the Norwegian cohort (OR = 88.21; P < 0.001) sample.
Conclusions:
It was the combination of high pain levels and high levels of depression that to the greatest extent increased the risk of anxiety in patients with CFS/ME. Whatever diagnostic criterion that is applied, anxiety and depression should be mandatory to assess in the clinical assessments performed for diagnosing the ME/CFS. Approaches addressing anxiety-related pain and treatment of depression should be warranted.
Introduction
Pain is reported by 90% of patients with myalgicencephalomyelitis/chronic fatigue syndrome (ME/CFS). Of these, 42% report moderate or severe pain. 1 Pain symptoms are included in the most recent developed case definitions for ME/CFS.2-4 There are huge variations in self-reported pain among the ME/CFS patients, ranging from mild to severe, from rare to more frequent, experienced in various parts of the body and contributing to illness burden and reduced quality of life. 5
Pain reports vary with age, gender, and psychological factors. Older people report more pain than younger people, 6 and women tend to report more pain than men.7,8 Mental health problems are common in patients with chronic pain disorders.9-12 Anxiety and depression are more common in patients with neck pain than in healthy controls, 13 and are important predictors of pain and disability. There is a bidirectional relationship between pain and mental health problems.11,14,15 Onset of anxiety and depression may be a consequence of pain and associated with number of pain locations 16 and with more severe pain. 17 Both anxiety and depression are associated with worsening of pain 18 and a history of depression or anxiety with an increased risk of developing chronic pain. 15
Lasting, unexplained and high levels of pain may provoke anxiety in patients with chronic fatigue syndrome (CFS) or ME/CFS, but they are not always a comorbid condition. For example, one study on patients diagnosed by the Fukuda criteria (CFS) 19 and evaluated by SCID (Structured Clinical Interview for DSM-IV) showed that 18% had anxiety and depression. Fourteen percent had anxiety and 14% had depression only. 20 Around 50% of this sample did not fulfill the criteria for either anxiety or depression. A couple of other studies have found pain intensity to be associated with anxiety, 21 and higher levels of anxiety about health were associated with increased levels of pain. 22 Another study of chronic fatigued patients diagnosed by the Canadian Consensus Criteria (CCC, ME/CFS) 3 and assessed by HADS (Hospital Anxiety and Depression scale) 23 found 38% to have anxiety and only 18% had depression at a clinical level. 24
Anxiety is, as shown above, related to pain, and vice versa. However, it has received relatively little attention in this patient group. Pain is a symptom that is alarming, and therefore often attracts the full attention of both patients and health care professionals. This may indicate that mental conditions such as anxiety, that should be capable of alleviation, are not noted, so adequate treatment is not offered. Therefore, it is important to establish the nature of the association between pain and anxiety. Our hypothesis is that patients who report a certain level of pain may also have more anxiety.
The present study aims to test whether, in patients with ME/CFS, pain is associated with an increased risk of reporting higher levels of anxiety. Previous studies have revealed associations between pain and depression as well as between anxiety and depression. Therefore, a pain-depression interaction also is included in the analyses.
Method
Study procedures and participants
This cross-sectional study sought to examine pain and anxiety, and a possible interaction effect of depression, in patients diagnosed with ME/CFS, and in healthy controls. The study comprised samples from both Norway and Spain with 463 patients recruited from tertiary health care in both countries and 201 healthy controls from Norway.
Participants
Norwegian samples
The Norwegian sample consisted of 133 patients diagnosed with ME/CFS (104 females [78.2%] and 25 males [18.8%]) diagnosed by the Canadian Consensus criteria (CCC) 3 and of 201 healthy controls (138 females [68.7%] and 59 males [29.4%]). Patients were enrolled in the study when attending a tertiary ME/CFS center for evaluation of their diagnoses. Physicians experienced in CFS and ME/CFS diagnosed the patients. Patient’s symptoms were assessed in a clinical interview to decide whether they satisfied the symptom criteria or not. To exclude other somatic and/or psychological conditions that might explain the patient’s symptoms, a number of blood tests were taken and a psychological interview was carried out.
Patients who fulfilled the CCC and healthy controls were asked to participate in data sampling in a ME/CFS biobank/thematic register. The healthy control group was recruited from among first time blood donors at the same hospital. To ensure that the blood donors had no other diseases, they went through an extended medical examination 5 to 6 weeks before inclusion in the data sampling. The current study material is a sample of convenience collected from March 2013 to June 2018. Of those patients contacted for an appointment, a total of 38% refused to participate in data sampling. Almost 16% of those who agreed to participate in biobank/register sampling and made appointments did not in fact attend. The final number of participants (ie 133 patient and 201 controls) reflects the number of participants available and included in the data sampling when the analyses started.
For recruitment, the participants had to be between 18 and 65 years old and fluent in the Norwegian language. They were informed about the purpose of the data sampling and signed a written informed consent form before inclusion. The outcome measurements were completed by pen and paper at home. To prevent missing data in the questionnaires, a research nurse ensured that the participants filled out the whole form.
The study and all data collection were approved by the Institutional Review Board at Oslo University Hospital (ref: 2011/8355) and by the Norwegian Regional Ethical Committee (ref REK 2011/473, and REK South-East, ref: 2017/375).
Spanish sample
The second sample was a cross-sectional community-based cohort study with 330 ME/CFS individuals (283 females [85.8%] and 45 males [13.6%]) from different geographical areas across Spain. Data were surveyed via online REDCap from a single outpatient tertiary-referral center (CFS/ME Clinical Unit, Vall d’Hebron University Hospital, Barcelona, Spain) from September 2017 to April 2018. Most patients were referrals with compatible self-reported clinical findings and symptom exacerbation, from primary health care settings from all over Spain (primarily from the region of Catalonia). Patients who met the 1994 CDC/Fukuda case definition for CFS were potentially eligible for the study. In addition, a comprehensive clinical examination for each individual was conducted by a specialist physician with extensive experience in diagnosing the condition in the local health care setting. Written informed consent was obtained from all participants before enrollment in the study. The study was approved by the local IRB and the Clinical Research Ethics Committee of the Vall d’Hebron University Hospital.
Measures
Anxiety and depression
The Hospital Anxiety and Depression scale (HADS) 23 was used for assessment of anxiety and depression. The HADS is developed to assess anxiety and depression within groups of patients attending medical hospitals. The instrument is a valid and feasible efficient screening instrument for anxiety and depression.25,26 Participants respond to 14 questions on anxiety and depression on a scale ranging from 0 (low) to 3 (highest). The HADS scale has two separate 7-item subscales for measuring cognitive and emotional aspects of both anxiety and depression. A clinical level of anxiety and depression is supposed to be a score of 8 or above on the respective scales. 23 For CFS patient populations also, the threshold score on the depression scale of HADS indicating a possible clinical diagnosis of depression is suggested to be 8. 27 For the statistical analysis, the anxiety variable was divided into 2 levels, with participants scoring ⩾8 placed in the high-anxiety group, and those scoring below this level placed in the low-anxiety. This variable was used as an dependent variable in the logistic regression model. Depression was also dichotomized with the clinical threshold score of ⩾8, and it was regarded as an independent variable in the interaction analysis. The Cronbach’s alpha score for anxiety was 0.86, and for depression it was 0.93.
Bodily pain
Pain was assessed by The Medical Outcomes Study Short-Form 36 Surveys (SF-36). 28 This is a self-report questionnaire consisting of 8 subscales: Bodily pain, Physical functioning, Role physical (role limitations due to physical health problems), General health perceptions, Role emotional (role limitations due to emotional problems), Social functioning, Vitality and Mental health. SF-36 generally demonstrates adequate validity and test–retest reliability across applications, and is frequently used to assess health-related quality of life and functioning level associated with chronic somatic illness. 29 Previous research has shown SF-36 also to be a valid and reliable instrument for health-related quality of life, including bodily pain, in Norwegian and Spanish patient samples.8,30,31
The 2-item SF-36 Bodily Pain Scale (BPS) assesses bodily pain intensity and interference of pain with normal activities. 28 Intensity in BPS is measured on a 6-point rating scale (1 = none to 6 = very severe). Pain interference of BPS is evaluated on a 5-point rating scale (1 = not at all to 5 = extremely). The original response to the 2 BPS items is recoded and the raw scale score is computed as a simple algebraic sum of the recoded values. Then the raw scale score is changed to a 0 to 100 scale so that high scores define low pain (0 = very severe and extremely limiting pain to 100 = no pain, or limitations due to pain). 28
Research supports a unitary construct of pain severity, as strong correlations between measures of pain intensity and measures of pain disability have been demonstrated.32,33
The BPS variable was independent variable in the regression analysis. To test the interaction effect between pain and depression or anxiety, a graded pain variable with 3 different levels was computed: high level of pain (0-30), medium level of pain (31-70), and low level of pain (71-100). This classification of pain levels is not uncommon in numerical scales. 34
Demographics and covariates
The DePaul SymptomQuestionnaire (DSQ) 35 is an illness specific questionnaire, an extended and standardized symptom registration tool with 100 questions on various items. DSQ was used to assess demographic information such as age, gender, and educational level for the participants in all the subsamples. In addition, DSQ contains one question about former psychiatric illness (FPI) with the following wording: “Have you ever been diagnosed or received treatment for any of the following.” The participants are asked to mark if and when they were diagnosed, and if possible the year of treatment, and what kind of treatment they received for the following illnesses: “severe depression, severe depression with melancholia, bipolar disorder, anxiety, schizophrenia, eating disorders or substance abuse.” A total score was computed for FPI by summing up number of times each participant marked FPI in the questionnaire form.
Statistical analyses
Data analyses consisted of descriptive statistics using SPSS (SPSS Inc. Released 2009, PASW Statistics for Windows, Version 21.0. Chicago: SPSS Inc.). Regression modeling was performed by the statistical software R version 3.5.2, which is a free software environment for statistical computing and graphics from the R Foundation. Descriptive statistics (mean, standard deviation or proportions) were calculated for healthy controls, and for the Norwegian and for the Spanish samples. Then the 3 subsamples were merged into a total sample to increase the power of the analyses. Binary logistic regression analyses were performed to determine the likelihood (Odd Ratio) that participants with more pain would report higher level of anxiety. The associations between pain, anxiety, and covariates were tested in a binary logistic regression model (see Figure 1). The pain, depression, age, gender, and FPI variables were entered into the model where age, gender, and FPI were controlled for in the logistic regression analyses. Pain and depression were represented in an interaction variable with multiple groups combining the 3 levels of pain (low, medium and high) and the 2 levels of the depression variable (low and high). The total Odds Ratio effect was calculated per 10 units of decrease in pain score and 1 unit of the depression score. Anxiety as a dependent variable and depression as an independent variable were both categorized as high (⩾8) or low (<8) in all analyses. The effects were measured by calculating odds ratios (OR) with corresponding 95% confidence intervals (CI). An alpha-level was set at <.05 to indicate statistically significance. The Hosmer-Lemeshow statistical test was used for testing goodness of fit for the logistic regression model.
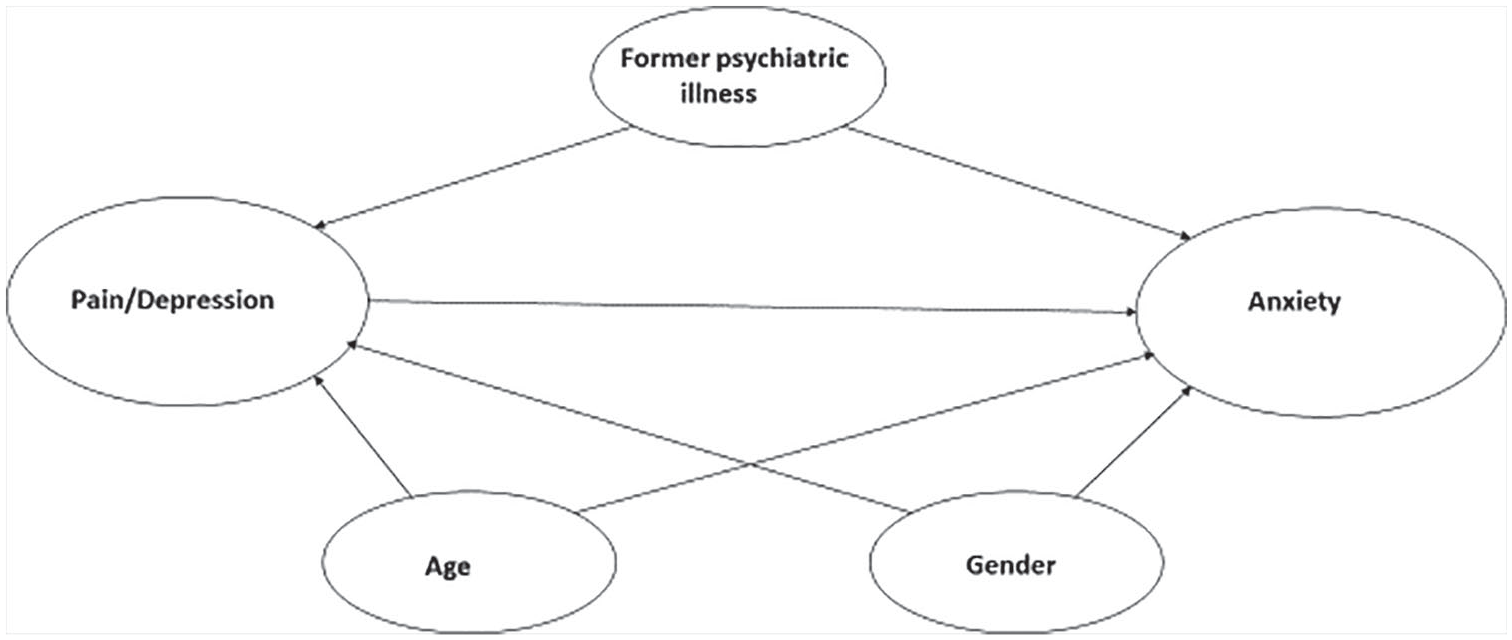
Model of the pain-depression interaction on the risk of higher level of anxiety tested in logistic regression analyses controlling for former psychiatric illness, age, and gender.
Results
Sample characteristics
Age, gender, educational level, pain, and psychological variables for the total sample and for the 3 subsamples are presented in Table 1. There are significant differences in all variables between all the subsamples. The Spanish sample had significantly higher level of pain, anxiety, depression, age, and more FPI, as well as a higher educational level, compared with the Norwegian sample. In the Spanish sample, a total of 74.8% had a high level of anxiety, compared with 21.1% in the Norwegian patient group. In addition, a significantly higher proportion of the Spanish patients were in the high pain group (68.5%) compared with the Norwegian patient sample (37.6%). The same pattern of occurrence was seen for depression scores, with 70.3% of the Spanish sample and only 15.8% of the Norwegian sample in the high depression group. For the healthy control group, the prevalence of high anxiety, high pain, and high depression was 10.4, 1.5, and 2.5, respectively.
Demographics, anxiety, depression, and pain variables for the total sample, the healthy controls, the Norwegian and the Spanish patient samples.
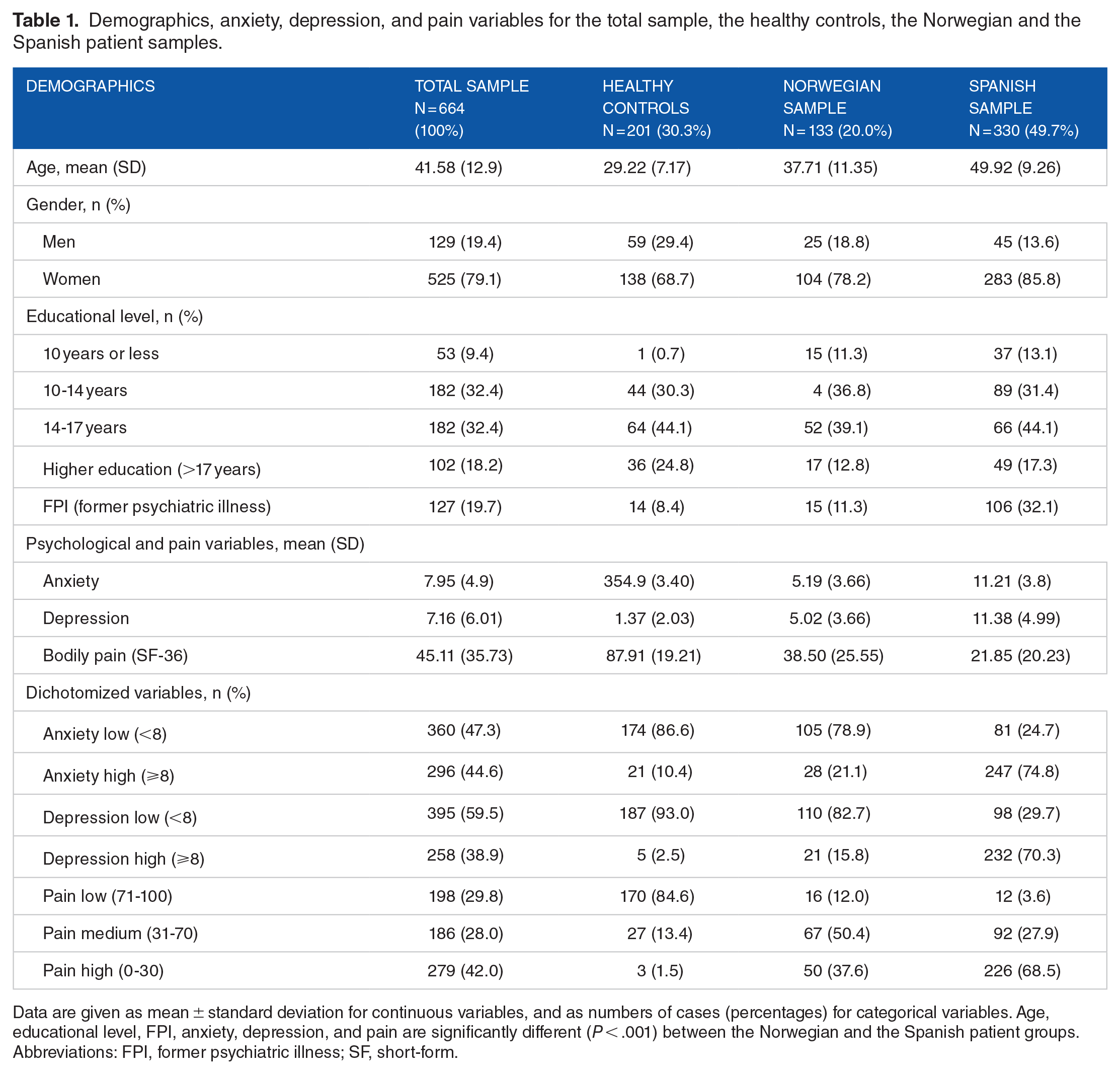
Data are given as mean ± standard deviation for continuous variables, and as numbers of cases (percentages) for categorical variables. Age, educational level, FPI, anxiety, depression, and pain are significantly different (P < .001) between the Norwegian and the Spanish patient groups. Abbreviations: FPI, former psychiatric illness; SF, short-form.
Pain x depression interaction predicting anxiety
The results of the regression analyses predicting anxiety are presented in Table 2. Both pain and depression made significant direct contributions as well as interaction effects to the prediction of anxiety, although some of the results are insignificant for low levels of depression.
Logistic regression analyses on the association between the presence of high anxiety (HADS anxiety score ⩾8) and the various combinations of the pain and the depression, adjusted for age, gender, and FPI.
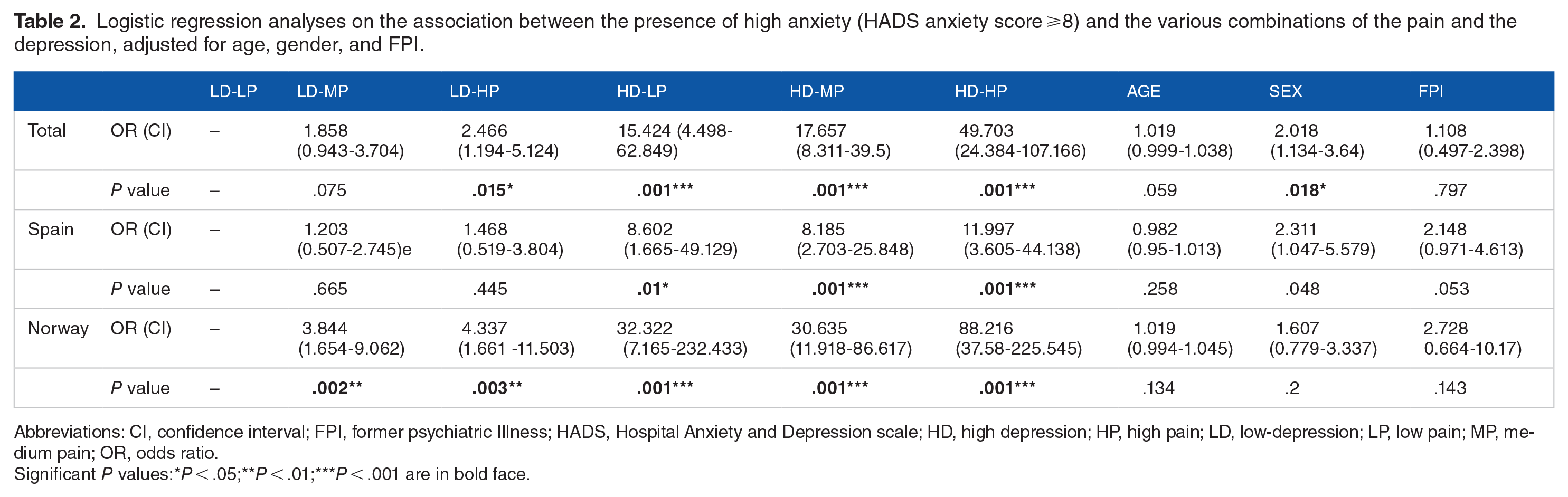
Abbreviations: CI, confidence interval; FPI, former psychiatric Illness; HADS, Hospital Anxiety and Depression scale; HD, high depression; HP, high pain; LD, low-depression; LP, low pain; MP, medium pain; OR, odds ratio.
Significant P values:*P < .05;**P < .01;***P < .001 are in bold face.
The association between pain, depression, and more anxiety was seen in both the total, the Norwegian and the Spanish samples. There is a clear indication of interaction effects for high depression in combination with either low, medium, or high pain, that are significantly associated with the risk of higher anxiety for all populations.
For the Norwegian group, there is also an interaction between low depression and medium and high level of pain although this is not as strong as the interactions between high depression and low, medium, and high pain. In the Spanish group, it is the combination of high depression and the various pain levels that increase the risk of more anxiety.
For the total sample, it seems that higher levels of depression interact with pain at all levels of pain. There is little difference between the results for high depression and low pain level (OR = 15.42) and for high depression and medium pain level (OR = 17.66). The strongest risk for higher levels of anxiety is the combination of high levels of depression and high levels of pain in the total sample (OR = 49.70), the Spanish sample (OR = 11.99), and most of all in the Norwegian (OR = 88.22) sample. In the Norwegian sample, there is also an interaction effect between low depression and both medium (OR = 3.84) and high pain (OR = 4.34). This indicates that pain, more than depression, increases the risk for higher level of anxiety.
For the healthy control group, there were no significant effects on anxiety. The number of participants with medium and high pain categorical variables as well as with high anxiety and high depression categorical variables were very small (not shown in table). The Hosmer-Lemeshow Goodness of Fit test revealed a chi-square value of 7.523 (df = 8) and a P value of .48. Basically a small chi-square value with larger P value indicates a good logistic regression model fit. The overall classification accuracy was 84.3%. This implies that the model adequately fits the data.
Discussion
The results revealed an association between increased pain and the risk of greater anxiety. For the overall sample, including both patients and healthy controls, an interaction effect of pain and depression on anxiety was revealed. This implies that the relationship between pain and anxiety is associated with the presence of depressive symptoms. The more depressive the symptomatology, the higher risk of greater anxiety when in pain. This same pattern, with only small differences, was found in the 2 patient samples as well. The OR is greatest in the Norwegian patient sample. The combination of high depression and high pain has an OR of 88 on anxiety compared with 12 and 49 in the Spanish and overall samples, respectively. In the Norwegian patient group, there is an effect on anxiety of low depression, combined with medium and high pain. This was not found in the Spanish sample. However, there is a positive effect of low depression and different levels of pain in the Spanish sample, but this is not significant and is therefore an uncertain outcome. This may be due to the fact that the number of patients with low depression is smaller in the Spanish than in the Norwegian group.
Even if the direction of causation between pain, depression, and anxiety is still unclear, both pain and depression have an impact on the level of anxiety. The higher the pain and the greater the depression, the more likely is a clinical level of anxiety that requires further investigation and treatment. Many other studies have shown that the coexistence between anxiety, depression, and pain, regardless of the direction of causation between them, have the negative impact of increasing and worsening each other.17,18,21,22 It is previously also stated that pain reduces physical and social function in these patients. 5 It is obviously credible that for patients with CFS or ME/CFS, the psychological and pain variables studied could be associated with increased fatigue or other symptoms required for the diagnosis in several of the CFS/ME case definitions. This should be further investigated in another study.
Strengths and limitations
The current study investigated 3 different subsamples collected in different countries that proved to be relatively different. The levels of anxiety, depression, and pain also vary between the samples. The 2 patient groups had significant higher levels of the included variables than the healthy control group. This is in line with previous research 13 showing more anxiety and depression in patients in pain than in healthy controls. Moreover, the occurrence of high anxiety, high depression, and high pain in the Spanish patients is higher than in the Norwegian sample. The distribution of the 3 pain levels also varied between the samples. The same measurement methods were applied in all samples and both SF-368,31 and HADS25,26 have shown good validity and reliability when translated and used in the 2 countries. The differences in the variables between the 2 samples may be because they really are different, or it may be due to cultural factors affecting the experiencing and reporting of such symptoms. The Norwegian patients went through an extended psychological examination to rule out primary psychological illness before a diagnosis was made. It is unclear whether psychological assessment was part of the Spanish CFS diagnosis. Different ways of handling psychological issues when diagnosing the patients might explain the higher levels and higher occurrence of anxiety and depression in the Spanish sample. The Spanish sample is diagnosed by the Fukuda criteria (CDC) which appears more inclusive than the CCC applied in the Norwegian sample. Thus, there may be 2 very different samples. At the same time, there is a large overlap in the symptom criteria in Fukuda and the more stringent CCC. This means that part of the Spanish sample may also satisfy the CCC. Although there are differences in the level and prevalence of the studied variables, the pattern between them is the same.
It is more unclear whether this was a part of the diagnostic examination in the Spanish sample. Different ways to handle psychological issues when diagnosing the patients might explain the higher levels and higher occurrence of anxiety and depression in the Spanish sample. Moreover, the participants were not randomly assigned to the study, and no data are available on those who refused to take part, or who agreed to participate but withdrew from data sampling. This implies that the selection of patients in the Spanish sample is somewhat unclear. We do not know whether patients with more or fewer symptoms are selectively included in the current study. That the risk for anxiety is higher for patients with more pain, and even stronger if they are also depressed, can nevertheless be established. In addition, not all patients with CFS or ME/CFS have symptoms of anxiety or depression. It is important to identify and treat both anxiety and depression as they can be a burden to patients with CFS or ME/CFS.
Several patients from the Spanish group reported mental health problems at earlier times. This is in accordance with research showing that a history of depression and anxiety may increase the risk of developing pain later. 15 In addition, patients with previous depression or anxiety may more easily develop mental health problems later. A significantly higher proportion of the Spanish sample had higher levels of anxiety, depression, and pain than in the Norwegian sample. Even though there were differences regarding the proportions and levels of the included variables, the same pattern between the variables appeared in both groups.
There may be overlap between depression and fatigue. In the current study, HADS was used for assessing depression. This instrument was developed for use in patients with medical conditions and symptoms of somatic illness. In order that the symptoms of somatic disease and depression or anxiety should not be confused, somatic symptoms such as fatigue were removed from the questionnaire. The selected items in HADS are based solely on psychic symptoms that may reduce the overlap between the 2 variables. Questions used in HADS-depression scale are anhedonic such as “do you take as much interest in things as you used to?,” “laugh as readily?,” “do you feel cheerful?” or “feel generally optimistic about the future?,” and actually are not a part of fatigue. Nevertheless, some overlap between HADS-depression and fatigue is found. 36 This indicates that depression might have an overall smaller effect in the pain-anxiety relationship, and that fatigue should have been treated as a covariate in the current analyses. At least depression and fatigue should be explored further in another study, probably using diagnostic interviews, for example the structured clinical interview for the diagnostic statistical manual (SCID), in order to clarify the relationship between depression and fatigue.
The 2 samples also differed as regards demographic variables. Research has shown that age 6 and gender 7 impact on pain reports. More pain reports in the Spanish sample may thus be due to older age and a higher proportion of women. However, age, gender, and previous history of mental illness were all adjusted for in the statistical analyses without affecting the results. It is interesting that the patient groups differ with respect to the included variables. However, this is not the focus of this article, and should be further investigated in another study.
This study is a large-scale data sample collected in 2 different European countries. Since the results are similar in the 2 subsamples, they were not conditioned by a purely transcultural factor. However, to confirm this point, the study should be expanded with samples of ME/CFS individuals from culturally more diverse parts of Europe. The patients in this study were recruited from tertiary health care in both countries. Future studies should include patients who seek out and are treated in other parts of the health care system. While the CCC was applied in Norway, the Fukuda criteria were used in Spain. That different sets of criteria were used in the 2 countries may also have resulted in significantly different characteristics of the patient sample. This use of different criteria, providing diverse selection, is interesting and should be studied in more detail in another study.
The patients were recruited in 2 different countries, different criteria were used for diagnosis, and no data exist on patients who refused to participate or withdrew. There are also differences in the extent and level of symptoms, and also age and history of mental health varies between the samples. The major differences between the samples might be limitations of the current study, but in spite of the differences the pattern between the studied variables are consistent across various conditions. This may in fact be a strength to the study findings. This may imply that the relationship between pain, depression, and anxiety that emerges here can be generalized to patients fulfilling either the Fukuda or the CCC case definitions. The results show that pain, in combination with a clinical level of depression, increases the risk of anxiety. Patients who report pain may have both anxiety and depression. As revealed in other studies, pain, anxiety, and depression negatively affect and can sustain each other.16-18 This may also be the case for patients with CFS or ME/CFS. Thus, mental aspects should be identified regardless of which criteria used for diagnosis. The most important requirement is to offer patients adequate treatment, whether this is pain relief, or help to treat and cope with mental symptoms.
Conclusion and implications
In spite of studying samples with significantly different characteristics, the results revealed the same pattern of associations between pain and anxiety. Approaches to anxiety-related pain as well as treatment of depression to improve ME/CFS would be justified. These are both factors about which something can be done, and which is a burden to the illness. Therefore, it is important to map anxiety and depression, and not just pain. Assessment of these variables should be an integral part of the diagnostic investigation of patients with ME/CFS.
Footnotes
Acknowledgements
We want to thank statistician Christoffer Haug Laache at University of Oslo for invaluable help with the data analyses, Semhar Abraham and Hilde Haukeland at the Oslo University Hospital, CFS/ME center for their contribution in the data sampling, Derek Pheby at Buckinghampshire New University for language editing as well as the participants who provided us with valuable data.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
EBS initiated and planned the study in collaboration with the research group, contributed to data collection, analysis of data and writing the article with input from all authors.
JC-M conceived and planned the original idea of the study, collected the data from the Spain cohort, helped supervise the findings and contributed to analysis and interpretation of the results.
JA was involved substantially in planning and supervision of the study, aided in interpreting the results and drafted the manuscript.
IH was involved in planning of the study, interpreting the results and discussing the analysis and the drafts of the manuscript.
A-MM was involved in planning of the study, interpreting the results and discussing the analysis and the drafts of the manuscript.
All authors provided critical feedback and contributed to the final version of the manuscript.
