Abstract
Objectives:
Study 1 investigated if the elderly’s perception of experiencing life problems moderates the effect of spousal living arrangements on their mental health, while study 2 first assessed loneliness as a mediator on the spousal living arrangements and mental health relationship, and then tested 2 moderated-mediation models whereby perceived problems moderates the mediation.
Methods:
Study 1 involved 135 participants aged 60 years and above (mean = 70.96; SD = 6.16); Study 2 involved 122 participants aged 65 years and above (mean = 74.85; SD = 6.91).
Results:
This study found simple moderation and mediation effects of perceived problems and loneliness, respectively, on the spousal living arrangements and mental health relationship. Furthermore, results showed that perceived problems moderate the loneliness and mental health link in a moderated-mediation model.
Discussion:
Findings inform potential interventions for elderly mental health. Interventions could focus on reducing loneliness and problems faced by the elderly, especially those with nonspousal living arrangements.
An increasing number of countries are facing an aging population, and this problem brings challenges such as a higher prevalence of illnesses, and poorer overall well-being of the community. 1 In Singapore, the elderly comprise 13.1% of the population 2 and this percentage is expected to grow to 19% by 2030. 3 As such, Singapore has to contend with many key aging-related matters, one of them being the high prevalence rate of mental health issues among Singapore’s elderly population.4,5
While good mental health is associated with better quality and satisfaction of life, 6 poor mental health contributes to higher somatic symptoms among elderly with chronic illnesses 7 and higher risks of mortality and morbidity. 8
Research has shown that the living arrangement of the elderly influences their mental health. Numerous studies have demonstrated both direct9,10 and indirect11,12 negative effects that living alone has on mental health. Accordingly, it is plausible that elderly who live with family members receive more support, and consequently have better mental health. The focus of previous studies has primarily been on the effects of living alone, with concerns that the elderly might not have access to the social, physical, or financial support that living with others might bring. The current study aims to enhance the understanding of how other kinds of living arrangements might be associated with elderly mental health. Specifically, we examined the relationship between spousal (ie, living with spouse and children, or living with spouse only) versus nonspousal (ie, living with children only, living alone, or living with others) living arrangements on mental health. A focus on spousal living arrangements, as opposed to other living arrangements, was chosen in this study because of the essential role that the spouse plays in elderly mental health.13,14
Spousal Living Arrangements and Elderly Mental Health
Previous research on how spousal living arrangements affect elderly mental health has been inconclusive. Some studies found a positive influence (eg, reduced depressive symptoms) of spousal living arrangements on elderly mental health.15,16 In contrast, other studies have found no significant positive association of spousal living arrangements on elderly mental health.17,18 The heterogeneity in findings for the association between living arrangements and mental health suggests that a deeper examination of the relationship is required. Specifically, a beneficial line of inquiry would be to examine the mechanisms through which living arrangements could affect elderly’s mental health.
Spousal Living Arrangements, Loneliness, and Elderly Mental Health
One important determinant of mental health that could also be affected by living arrangements is that of feelings of loneliness that the elderly might face. Loneliness is defined as “a deep sense of emptiness, worthlessness, lack of control, and personal threat.”19(p453) Research has consistently demonstrated that loneliness negatively affects mental health in elderly across various cultures.20-22
However, many elderly couples develop interdependence after long years of marriage, which might compensate for the loss of emotional support when other nonspousal relationships deteriorate. 23 In line with this reasoning, elderly who live with their spouses could experience less loneliness than those in nonspousal living arrangements.24,25
Recent studies have also found that loneliness mediates the relationship between living alone and mental health.11,12 However, no study has examined whether the effects of other living arrangements (eg, with spouse, without spouse but with others, with spouse and others, etc) on mental health are also mediated by loneliness. Thus, the current research aims to investigate if loneliness mediates the relationship between spousal (and nonspousal) living arrangements and elderly mental health.
Moderating Role of Perceived Problems
As mentioned, research examining the independent effect of spousal (and nonspousal) living arrangements on elderly mental health has been inconclusive, suggesting the possibility of heretofore unexplored moderators of the relationship. Some studies have shown tentative evidence of the moderating role of perceived problems on this relationship. For instance, Chan et al 16 found that poor social networks moderated the link between spousal (and nonspousal) living arrangements and elderly mental health. A Finnish study also found that health problems and unemployment contributed substantially to the mental health of adults in nonspousal (relative to spousal) living arrangements. 26
Furthermore, the negative impact of perceived problems, across various life domains (ie, physical health, social, or financial), on mental health is well-documented. Poor health and functional disability have been closely associated with poor mental health such as anxiety and depression.27,28 In addition, individuals who have poor social networks are more likely to have depression,29,30 higher stress, and lower self-esteem. 31 Finally, elderly who suffer from financial problems are more likely to have poorer mental health compared to those with minimal financial problems.32,33 These findings suggest that perceived problems from various domains have direct detrimental effects on elderly mental health.
Another possibility is that perceived problems could moderate the relationship between the loneliness experienced by the elderly and their mental health. Elderly who feel lonely could be more adversely affected by problems in their lives, compared with elderly who perceive their lives to be relatively problem-free. For instance, elderly with health problems may find it physically more difficult to seek social support to combat their feelings of loneliness. In turn, their feelings of loneliness could facilitate declines in mental health. In another example, Gulseren 34 showed that loneliness is more strongly associated with depression when elderly have health problems such as chronic diseases. Aylaz et al 35 also explained that elderly who experience loneliness, together with other social, health, and financial difficulties, are more vulnerable to having depression.
Goals of Current Research
The primary goal of this research is to investigate the mechanisms that underlie the link between spousal living arrangements and elderly mental health. Study 1 investigated whether perceived problems moderate the relationship between spousal living arrangements and mental health. With an aim of investigating the results of study 1 in a more in-depth manner, study 2 re-evaluate the model with another key variable, “loneliness.” Study 2 explores if loneliness mediates the spousal living arrangements and mental health relationship. Study 2 also explores whether perceived problems moderate the mediation relationship. Specifically, we conduct 2 moderated-mediation models to evaluate the moderating effects of perceived problems on the spousal living arrangements and mental health link, as well as the loneliness and mental health link.
Study 1
Previous studies have demonstrated that perceived problems negatively influence elderly mental health28,33 and that living with a spouse predicts better mental health in cases where the elderly are experiencing problems that require support from others. 16 In study 1, we sought to examine the moderating effect of perceived problems on the relationship between spousal living arrangements and mental health. We hypothesized that spousal living arrangements are linked to better mental health, but only in the presence of perceived problems.
Method
Participants
Participants were recruited with use of posters and fliers at public places around Singapore, by convenience sampling, and word-of-mouth. The recruitment notices included the following inclusion criteria: at least 60 years old, and be literate in either English or Mandarin. Each participant received a mail-in survey and mailed their completed consent forms and surveys back to the University, after which they were compensated S$25 for their time. Two bi-lingual speakers used translation–back translation technique to produce Mandarin versions of the consent form and questionnaire.
Measures
Living arrangements
Participants were classified into 5 living arrangements: (1) live with spouse only, (2) live with children only, (3) live alone, (4) live with spouse and children, and (5) live with others. For our analyses, participants who were living with spouse and children, or living with spouse only, were coded as spousal living arrangements, while those elderly living with children only, living alone, or living with others were coded as nonspousal living arrangements.
Perceived problems
Participants responded to an open-ended question: “What problems are you facing, if any?” and were asked to elaborate on the specific nature of their problems. Although the open-ended question asked participants to specify the domains in which they were experiencing problems (ie, physical health, social, or financial), the number of responses that explicitly specified the domains of problems were too small to be meaningfully separated into the major domain categories. Hence, the responses on this measure were dummy-coded, specifically for an “absence” or “presence” of perceived problems.
Mental health
Mental health was assessed using the Mental Health Component Summary of the Short Form–12 Health Survey (SF-12 MCS 36 ). The SF-12 MCS examines overall mental health, emotional role functioning, social functioning, and vitality. A greater score indicates better mental health. Cronbach’s alpha for this sample was .66.
Analytical approach
The analysis was adjusted for age because a significant negative correlation between age and mental health was found, r = −0.31, P < .001. Older individuals tend to report poorer mental health. In addition, subjective social status was also controlled for because numerous studies have found significant associations between social status and mental health. 37 This measure was assessed on a 10-point social ladder scale as to which level participants think their family was at (1, lowest; 10, highest). A higher score indicates higher social status.
The main analyses applied a 2 (living arrangement) × 2 (perceived problems) analysis of covariance (ANCOVA) to assess the main effects of perceived problems and living arrangements, and their interaction effect on mental health, while controlling for age and subjective social status.
Results
In all, 135 elderly, aged 60 years or older (meanage = 70.96, SDage = 6.16, rangeage = 60-96, 53.5% women) completed a questionnaire titled “Study on older working adults.” Singapore is multi-ethnic with a Chinese majority 38 and our sample approximated the national variation and distribution for each major ethnic group. Specifically, participants recruited were Chinese (85.8%), Malay (7.5%), Indian (4.2%), and 1.9% reported “others.” In addition, 35.9% were living with spouse and children, 28.2% were living only with children, 18.9% were living only with their spouse, 11.7% were living alone, and 5.3% reported living with others who were not their immediate family members.
After adjusting for covariates, factorial ANCOVA found significant main effects for perceived problems, F(1, 106) = 10.75, P < .01, η2 = .09, and living arrangements, F(1, 106) = 4.31, P < .05, η2 = .04. Spousal living arrangements were associated with better mental health than nonspousal living arrangements, with means of 74.81 (SD = 2.12) and 67.77 (SD = 2.64), respectively. In addition, elderly who perceived problems also had lower mental health scores than those without perceived problems, with means of 65.75 (SD = 2.93) and 76.82 (SD = 1.69), respectively.
A significant interaction effect was found between living arrangements and perceived problems, F(1, 106) = 5.90, P < .05, η2 = .05. In an absence of perceived problems, there was no significant difference in the mental health of elderly across living arrangements. However, in the presence of perceived problems, elderly with spousal living arrangements had significantly higher mental health than those with nonspousal living arrangements (see Table 1).
Effects of spousal versus nonspousal living arrangements and perceived problems on mental health.
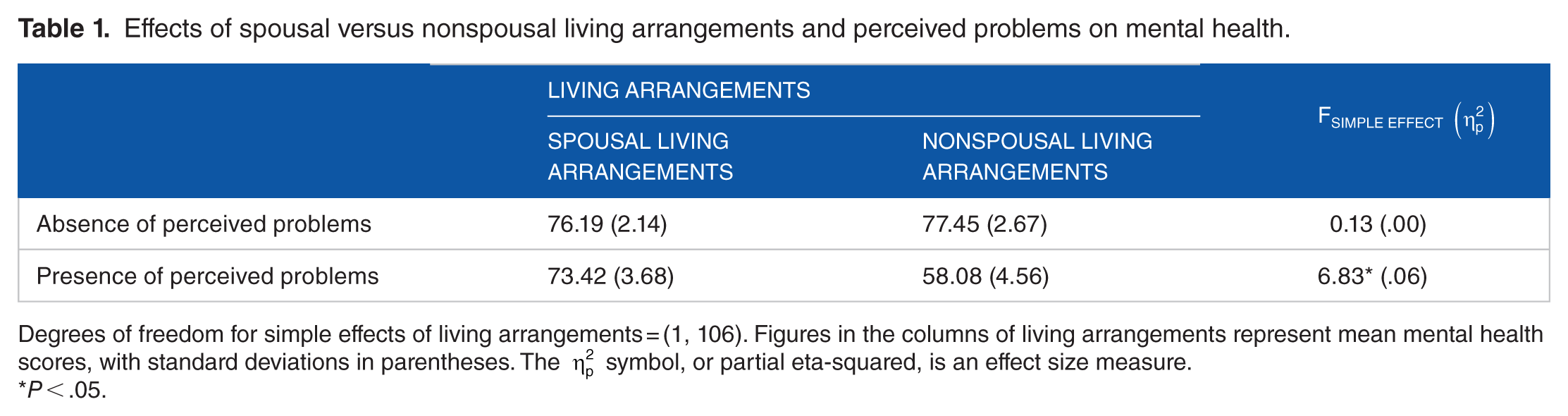
Degrees of freedom for simple effects of living arrangements = (1, 106). Figures in the columns of living arrangements represent mean mental health scores, with standard deviations in parentheses. The
P < .05.
Study 1 discussion
Study 1 demonstrated that perceived problems influence the spousal living arrangements and mental health relationship. Spousal living arrangements predict better mental health, but mainly when elderly perceive problems. These findings provide more insights into those of Chan et al 16 where elderly living with their spouses reported less mental health issues than those in nonspousal living arrangements, when they had a poor social network. Joutsenniemi et al (2006) also reported a similar pattern of results with an adult population, where health problems and unemployment moderated the relationship between spousal (and nonspousal) living arrangements and mental health. In light of study 1 findings, perhaps the benefits to mental health that elderly receive from spousal living arrangements found by Chan et al 16 were experienced because of the presence of problems in the elderlies’ lives, for which their live-in spouses could provide support toward.
In other words, the link between spousal living arrangements and better mental health could be explained by the additional emotional, financial, and instrumental support, together with social integration opportunities that spouses may provide.39,40 Cohen 41 explained that elderly may develop an interdependent relationship with their spouses, and this co-dependency might serve as an essential coping resource when problems arise. In the absence of perceived problems, elderly might still be independent, adaptable, and functional,42,43 hence reducing the importance of spouse living arrangements on mental health. The current study also offers an explanation for previously inconclusive results16,17 by including a condition (ie, presence of perceived problems) in which spousal living arrangements could affect mental health.
Study 2
Study 1 found that spousal living arrangements are more predictive of mental health than nonspousal living arrangements, particularly when elderly perceive problems. To further enhance our understanding of the relationship between living arrangement and mental health, study 2 had 2 primary aims.
The first aim was to examine whether loneliness mediates the relationship between spousal living arrangements and elderly mental health. Recent studies have demonstrated that loneliness mediates the link between living alone and mental health.11,12 It is plausible that loneliness might also mediate the relationship between spousal living arrangements and mental health. Furthermore, previous literature found that spousal living arrangements are negatively associated with loneliness, 25 which in turn strongly influences elderly mental health.20,21 We hypothesized that loneliness would mediate the relationship between spousal living arrangements and mental health.
The second aim of study 2 was to ascertain if perceived problems would moderate the mediation effect of loneliness on the relationship between spousal living arrangements and elderly mental health. There are 3 possible ways in which perceived problems could moderate the mediation effect of loneliness on the relationship between living arrangement and mental health. First, perceived problems could moderate the relationship between spousal living arrangements and mental health (see Figure 1). Second, it could moderate the relationship between loneliness and mental health (see Figure 2). Third, it could moderate the relationship between spousal living arrangements and loneliness. However, the current study only tested the first 2 moderated-mediation models because their simple moderation effects have been supported by past research.16,35 In contrast, the third moderated-mediation model was not tested because of weak support from past literature. To the best of our knowledge, no research has shown support for the moderation effects of perceived problems on the spousal living arrangement and loneliness relationship. Furthermore, only a limited number of studies have performed adequate analysis to accurately identify perceived problems as being independently related to loneliness. 44 Thus, there is no reason to expect that the absence or presence of problems perceived by the elderly would systematically moderate the level of loneliness experienced from spousal versus nonspousal living arrangements. Therefore, study 2 examined 2 moderated-mediation models in which perceived problems could moderate the relationships between spousal living arrangements and mental health (Figure 1), and between loneliness and mental health (Figure 2).
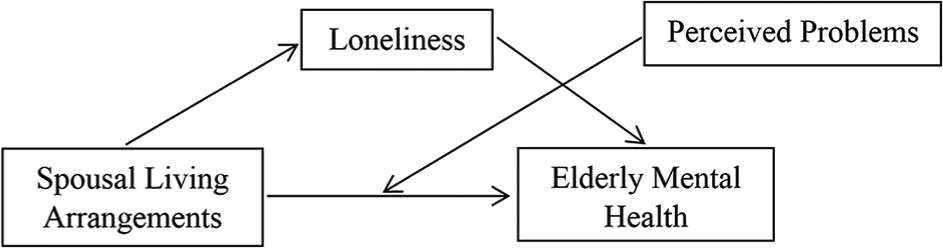
Moderated-mediation model, with perceived problems moderating the effects of spousal living arrangements on mental health.
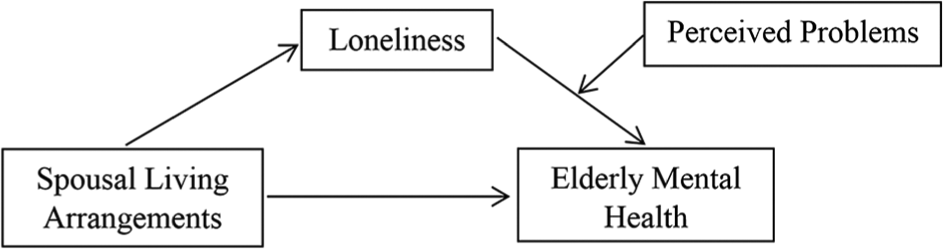
Moderated-mediation model, with perceived problems moderating the effects of loneliness on mental health.
Method
Participants
Participants were recruited via grassroots organizations and senior activity centers, convenience sampling, and word-of-mouth. Participants needed to be at least 65 years old, and be conversant or literate in either English or Mandarin. Prior to the study, they were briefed about the procedures and asked to sign a consent form, after which, they proceeded to complete the questionnaire on their own if they were literate, or have the questionnaire read out to them face-to-face if they were not literate. They were then compensated S$5 as a token of appreciation for their time. Two bi-lingual speakers used translation–back translation technique to produce Mandarin versions of the consent form and questionnaire.
Measures
Living arrangements
Similar to study 1, living arrangements where elderly were living with spouse and children, or living with spouse only were coded as spousal living arrangements while elderly living with children only, living alone, or living with others were coded as nonspousal living arrangements.
Perceived problems
Participants were asked, “In the past four weeks, do you think you had difficulty in the following areas?” Participants were then prompted to indicate specifically if they had difficulties in the physical health, financial, or social domains. Once again, even though the specific domains of perceived problems (ie, physical health, social, financial) were assessed, the small sample size limited our ability to separate responses into discernible content categories in a statistically meaningful way. Hence, responses were coded for the “absence” or “presence” of perceived problems.
Loneliness
The 8-item short form of the UCLA Loneliness Scale (ULS-8) was used to assess subjective feelings of loneliness. The ULS-8 has been reported to be a reliable, valid, and a preferred substitute for the original ULS-20. 45 Cronbach’s alpha for this sample was .85.
Mental health
Similar to study 1, the SF-12 MCS was used to examine overall mental health, emotional role functioning, social functioning, and vitality. 36 Cronbach’s alpha for this sample was .85.
Analytical approach
As with study 1, a significant negative correlation was found between age and mental health, r = −0.19, P < .05. Older individuals tend to report poorer mental health. Thus, age was controlled for in subsequent analyses. Moderated-mediation analyses were conducted using PROCESS Macro in SPSS. The Hayes PROCESS Macro is a “conditional modeling program that utilizes an ordinary least squares-based path analytical framework to test for both direct and indirect effects.”46(p810) Bootstrapping was applied to produce bias-corrected and accelerated confidence intervals (CIs) from 5000 resamples with α = .05. 47 Bootstrapping has also been found to provide powerful and reliable estimates in smaller samples. 48 PROCESS model 4 was selected to examine if loneliness mediates the spousal living arrangements and mental health relationship. PROCESS models 5 and 14 were then selected to examine the moderating effects of perceived problems on the spousal living arrangements and mental health relationship, and on the loneliness and mental health relationship, respectively, in separate moderated-mediation models.
Results
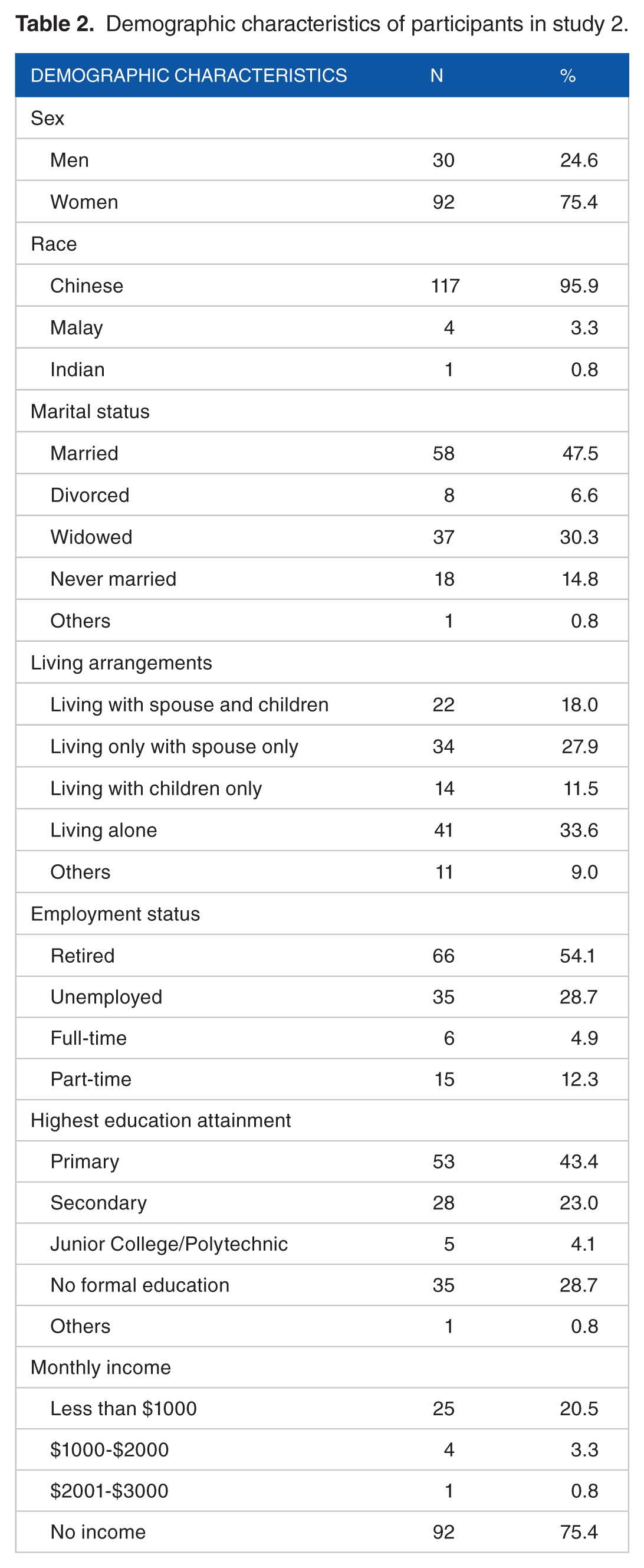
In all, 122 participants aged 65 years or older (meanage = 74.85, SDage = 6.91, rangeage = 65-96, 75.4% women) completed a questionnaire titled “Well-being of elderly.” To minimize selection bias, participants were recruited from 6 different residential regions spread out geographically across Singapore. Demographic characteristics of participants are shown in Table 2. When participants were asked if they were currently facing any perceived problems, 45.9% responded with “no problems,” 18.0% responded with “health problems only,” 4.1% responded with “financial problems only,” 7.4% responded with “social problems only,” and 24.6% responded with “more than one problem.”
Demographic characteristics of participants in study 2.
Mediation analysis using PROCESS model 4 showed that the indirect effect of spousal living arrangements on mental health via loneliness was significant (a path: B = −1.75, SE = 0.98, P = .08; b path: B = −3.77, SE = 0.30, P < .001; 95% CI, 0.26-13.77, excluding zero). The direct effect of living arrangements on mental health also remained significant after accounting for loneliness and age, B = −8.99, SE = 3.24, t = −2.78, P < .01. Hence, this model described a partial mediation effect of living arrangements with spouse on mental health.
Thereafter, moderated-mediation analysis using PROCESS model 5 demonstrated that the interaction effect between living arrangement and perceived problems was not significant after controlling for loneliness and age, B = 4.74, SE = 6.16, t = .77, P > .05. In other words, the direct effect of spousal living arrangements on mental health was not moderated by perceived problems. That said, results suggested different patterns of conditional direct effects. In the presence of perceived problems, results suggested an association between spousal living arrangements and mental health, B = −9.10, SE = 4.37, P < .05. In the absence of perceived problems, results suggested no association between living arrangements with spouse and mental health, B = −4.35, SE = 4.56, P > .05. Moving on, the indirect effect of spousal living arrangements on mental health via loneliness was significant (a path: B = −1.74, SE = 0.98, P = .08; b path: B = −3.32, SE = 0.33, P < .001; 95% CI, 0.12-12.63, excluding zero). In essence, this model described a simple mediation effect of spousal living arrangements on mental health, without moderation of the presence of perceived problems. Therefore, analyses did not provide support for the moderated-mediation model in Figure 1.
Another moderated-mediation analysis using PROCESS model 14 reported a significant overall effect, B = −3.40, SE = 2.09 (95% CI, −9.06 to −0.44, excluding zero). As shown in Table 3 and visually represented in Figure 3, a significant loneliness and perceived problems interaction indicated that perceived problems moderated the loneliness–mental health link in a moderated-mediation model. In the same vein, a larger indirect effect of living arrangement on mental health was observed in the presence of perceived problems, B = 6.40, SE = 3.33 (95% CI, 0.36-13.47, excluding zero), compared with an absence of perceived problems, B = 3.00, SE = 1.93 (95% CI, 0.25-7.94, excluding zero). The direct effect of spousal living arrangements on mental health after controlling for age was marginally significant (see Table 3). Other parameters of this moderated-mediation model are reported in Table 3. In essence, this model demonstrated a partial mediation effect of spousal living arrangements and mental health via loneliness, with perceived problems moderating the loneliness–mental health link. Therefore, results showed support for the moderated-mediation model depicted in Figure 2.
Moderated-mediation analysis with unstandardized parameter estimates, using perceived problems as moderator of the loneliness–mental health relationship.
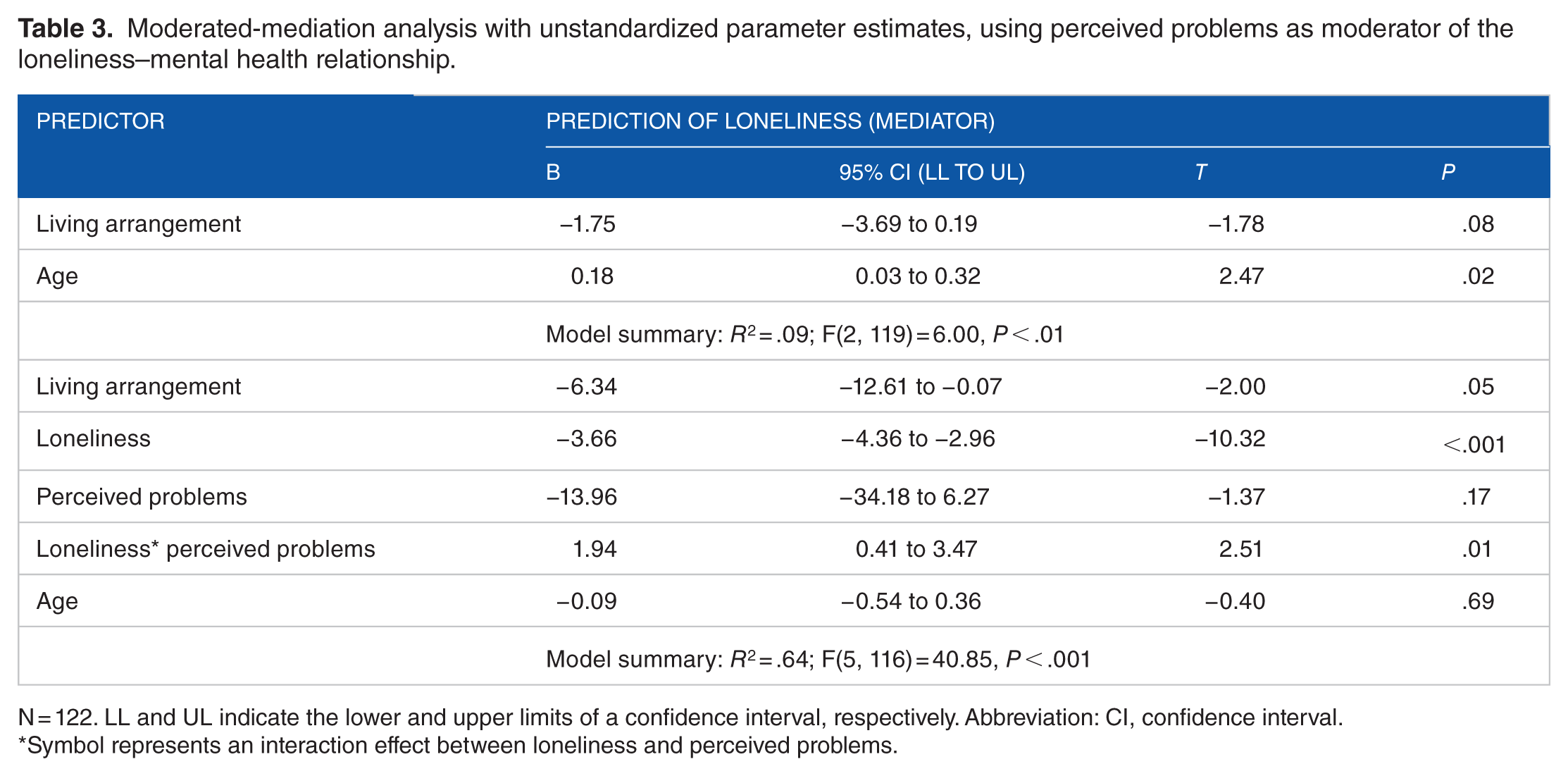
N = 122. LL and UL indicate the lower and upper limits of a confidence interval, respectively. Abbreviation: CI, confidence interval.
Symbol represents an interaction effect between loneliness and perceived problems.
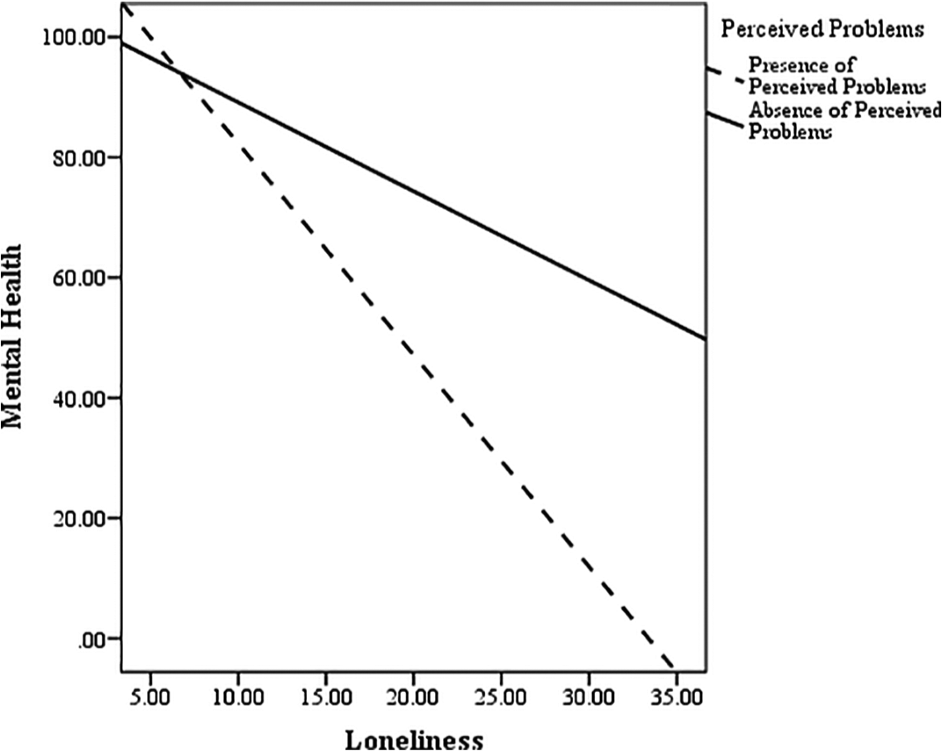
Moderating effect of perceived problems on the loneliness–mental health relationship in a moderated-mediation model.
Study 2 discussion
The finding that loneliness mediates the spousal living arrangements and mental health relationship is consistent with past studies demonstrating a similar mediating role of loneliness on the effect of living alone and lower mental health.11,12 While these studies found that living alone predicts increased loneliness, the present study found that living with a spouse predicts decreased loneliness. More precisely, spousal living arrangements are associated with lower loneliness levels than nonspousal living arrangements are, which then positively influences mental health. Our finding is also consistent with past studies that have demonstrated independent relationships between spousal living arrangements and loneliness, 25 and between loneliness and mental health.21,19
However, the moderated-mediation effect of perceived problems on the spousal living arrangements and mental health link was not significant (model 5; Figure 1). This result was unexpected as study 1 and previous research 16 have demonstrated that perceived problems moderate the relationship between spousal living arrangements and mental health. However, study 1 and previous studies did not consider the mediating effect of loneliness. This result could be due a stronger indirect effect of loneliness, which suppresses the weaker moderating effect of perceived problems. That said, results suggested different patterns of conditional direct effects although there was no significant interaction effect between living arrangement and perceived problems on mental health. Future studies with larger sample sizes might provide adequate statistical power to detect a significant moderation effect of perceived problems.
The second moderated-mediation model (ie, model 14; Figure 2) was supported. In this model, perceived problems moderated the loneliness and mental health relationship, and strengthened the indirect relationship between spousal living arrangements and mental health via loneliness. Specifically, spousal living arrangements predict decreased loneliness, which then interacts with perceived problems to predict different mental health outcomes. In the absence compared with presence of perceived problems, mental health decreases less significantly as loneliness increases, hence buffering against the negative effects of loneliness on elderly mental health. These moderated-mediation findings could also be better understood when the negative effects of perceived problems on mental health are considered (Hobfall, 2001).28,33 Therefore, elderly who are lonely and experience physical health, social, or financial problems present the highest risk of having poor mental health.
General Discussion
Previous research has focused on the specific effects of living alone on elderly mental health,9,11 while largely ignoring differential effects on mental health of other kinds of living arrangements. The current research chose to focus on spousal living arrangements, as opposed to other living arrangements, because of the key independent role that the spouse plays in elderly mental health.13,14 Furthermore, existing research on the spousal living arrangements and mental health16,18 has been inconclusive, and did not consider other potential key moderator or mediator variables. In study 1, we aimed to fill the research gaps by investigating if perceived problems moderate the relationship between spousal living arrangements and mental health. Study 2 aimed to investigate the results of study 1 in a more in-depth manner, by re-evaluating the model with another key variable, “loneliness.” Specifically, study 2 first explored if loneliness mediates the relationship between spousal living arrangements and mental health, and then tested the moderating effects of perceived problems in 2 moderated-mediation models.
Study 1 found that perceived problems moderate the spousal living arrangements and mental health relationship. Study 2 found a mediating effect of loneliness on the relationship between spousal living arrangements and elderly mental health; study 2 also found a moderating effect of perceived problems on the mediation model (ie, moderated-mediation). Unexpectedly, the first moderated-mediation model (Figure 1) was not significant. Specifically, the moderation effect of perceived problems on the spousal living arrangements and mental health relationship was not significant, although there was a significant indirect effect of loneliness on the spousal living arrangement and mental health relationship. The second model (Figure 2) demonstrated a significant moderated-mediation effect, such that spousal living arrangements predict lower loneliness levels, which in turn interact with perceived problems to predict different mental health outcomes. As loneliness increases, mental health decreases more significantly in the presence, compared with the absence, of perceived problems. With support from previous studies,20,49 the current finding suggests that reducing problems faced by the elderly buffers the negative effect of loneliness on elderly mental health.
In view of Singapore’s aging population, the current findings can inform intervention efforts to improve elderly mental health. For instance, more resources should be directed to elderly in nonspousal living arrangements, so as to reduce feelings of loneliness. Recent interventions addressing elderly loneliness have demonstrated high effectiveness by targeting maladjusted social cognition. 50 Governments could also design social policies and public intervention programs aimed at reducing loneliness, and health, social, and financial problems faced by the elderly population. Furthermore, family members and caretakers could be mindful of any significant problems or signs of loneliness of the elderly, which should be promptly resolved. These initiatives could play a role protecting elderly mental health.
This research has some limitations. First, the study design is cross-sectional, and hence cannot evaluate the causal relationships among variables or rule out possible confounds. For example, the aging process could be an alternative explanation for the elderly facing more perceived problems, which could in turn moderate the influence of other factors (eg, living arrangements) on mental health. Future studies might employ a longitudinal study design to investigate the causal relationships among variables.
Second, the length of the questionnaire distributed in study 2 had to be restricted due to logistical limitations. Thus, subjective social status was not measured and controlled for in study 2. Because of the close association between social status and mental health, 37 the effects of social status might distort the actual relationship between main variables and mental health. Future research can address this limitation by controlling for the effect of social status. Other potential confounds not controlled for in this study (eg, sex and education attainment) could also be considered in future studies.
Third, the measure of perceived problems could not be investigated in its specific domains in this study because the number of responses that explicitly specified the domains of problems was too small to be meaningfully separated. Future studies might employ a larger sample size, such that sufficient data from specific domains of perceived problems could be gathered and analyzed. In addition, specific domains of perceived problems could be clearly operationalized to provide a better understanding of the model.
Another limitation of the current research is that there is an over-representation of Chinese participants in the sample. Although this proportion is representative of the ethnic composition of Singapore, it nonetheless means that our sample is relatively homogeneous. In addition, most participants were recruited from senior activity centers, where elderly are more likely to already have greater social support and higher mental health. Future studies should better coordinate with residential committees to recruit more ethnic-minorities and homebound elderly, who might be more likely to experience problems of physical frailty, mobility issues, or less social support.
Conclusions
The current research examined the mechanisms underlying spousal living arrangements and elderly mental health relationship. It demonstrated the moderating and mediating effects of perceived problems and loneliness, respectively. A significant moderated-mediation model showed that spousal living arrangements predict lower levels of loneliness, which in turn interacts with the presence or absence of perceived problems to affect mental health differently. These findings highlight the importance of reducing loneliness and monitoring the problems faced by the elderly, especially those who are in nonspousal living arrangements, to protect their mental health. In light of a worldwide trend of increasingly aging populations, this line of research contributes to an understanding of how individuals can age successfully, improving the mental health of communities as a whole.
Footnotes
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Mitsui Sumitomo Welfare Grant. We also wish to acknowledge the funding support for this project from Nanyang Technological University (NTU) under the Undergraduate Research Experience on CAmpus (URECA) program. The findings and views in this report are that of the authors’ own, and do not represent the views of any organizations. This work is also based on a thesis available in NTU’s repository of papers; permission has been granted by the university to publish this work.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
LKS and JSP contributed to the research design and implementation, results analysis, and writing of the manuscript.
