Abstract
Introduction:
Atypical antipsychotics are frequently initiated in the intensive care unit (ICU) to treat delirium. Many patients continue on these agents at hospital discharge despite a lack of data to support long-term use.
Objectives:
The primary aim of this study was to determine underlying risk factors for continuation of antipsychotics at hospital discharge in medical intensive care unit (MICU) and surgical intensive care unit (SICU) patients when evaluated as separate cohorts.
Methods:
A single-center, retrospective study in patients newly initiated on quetiapine, risperidone, or olanzapine in a 22-bed mixed medical-surgical ICU admitted from January 2017 to July 2018.
Results:
A total of 78 (62.9%) MICU patients and 46 (37.1%) SICU patients met the inclusion criteria during this time frame. A total of 29 MICU patients (37.2%) were prescribed antipsychotics at hospital discharge compared to 25 SICU patients (54.3%), P = .063. The percentage of MICU patients prescribed antipsychotics at hospital discharge was significantly higher in patients ⩾60 years of age (22 [75.9%] vs 26 [53.1%], P = .045), with a history of dementia (5 [17.2%] vs 1 [2%], P = .015), admitted with hemorrhagic stroke (5 [17.2%] vs 2 [4.1%], P = .049), and initiated on risperidone (3 [10.3%] vs 0%, P = .022). The risk of pre-existing dementia remained significant in a multivariate logistic regression that controlled for confounding variables, odds ratio (OR) = 10 (95% confidence interval [CI]: 1.11-90.5, P = .040). The percentage of SICU patients prescribed antipsychotics at discharge was significantly higher in those with severe traumatic brain injury (TBI; 8 [72.7%] vs 0%, P = .004) and initiated on quetiapine (19 [76%] vs 9 [42.9%], P = .022).
Conclusion:
Antipsychotics were commonly continued at hospital discharge in both MICU and SICU patients. Several risk factors for continuation of antipsychotics were identified in these two cohorts. Future efforts assessing the appropriateness of antipsychotics at transitions of care are warranted.
Background
Atypical antipsychotics are frequently initiated in critically ill patients to treat or manage intensive care unit (ICU) delirium. 1 As patients recover from their critical illness, approximately one-third of patients remain on these agents at hospital discharge.2–9 Although there is some evidence to support using antipsychotics to treat ICU delirium in critically ill patients, 10 the results of the recently published Modifying the Impact of ICU-Associated Neurological Dysfunction-USA (MIND-USA) trial demonstrated that intravenous haloperidol or ziprasidone had no significant impact on reducing the duration of delirium compared to placebo. 11 The risk-benefit ratio of antipsychotics must be carefully balanced, particularly when used in older patients. All atypical antipsychotics have the potential to produce sedation, orthostatic hypotension, cardiac arrhythmias, and sudden cardiac death 12 ; and are associated with 1.6 to 1.7 fold increased risk of death compared to placebo when used to treat dementia-related psychosis and behavior disturbances. 13 Therefore, the 2018 Pain, Agitation/sedation, Delirium, Immobility, and Sleep disruption (PADIS) guidelines recommend that antipsychotics should be discontinued immediately upon resolution of delirium. 14
Risk factors for initiation of antipsychotics in the hospital include age ⩾75 years, male sex, black race, history of dementia, admission to a medical service, requiring mechanical ventilation, and having a higher severity of illness.2,3 Risk factors for continuation of antipsychotics at hospital discharge include age <75 years, discharge to a facility, use of atypical antipsychotics, admitting diagnosis of traumatic brain injury (TBI), and patients requiring longer durations of antipsychotic therapy and hospital length of stay (LOS).3–9 Patients initiated on quetiapine were three times more likely to be discharged on this medication compared to the use of other antipsychotics. 3
The previous studies that have evaluated the risk of continuing antipsychotics have combined both medical and surgical ICU patients and most of the evidence is derived from a large, retrospective study.3–9 Given the different reasons for admission and possible variations in comorbidities and severity of illness between medical intensive care unit (MICU) and surgical intensive care unit (SICU) patients, the aim of this study was to determine risk factors separately for these patients.
Methods
This is a single-center retrospective study in all ICU patients ⩾ 18 years of age who were newly initiated on quetiapine, olanzapine, or risperidone in a 22-bed mixed medical/surgical intensive care unit (MSICU) from January 2017 to June 2018 at a 617-bed academic medical hospital with a level-I trauma center. The ICU is staffed by four teams comprised of an attending, fellow, and residents or physician assistants. The nursing-to-patient ratio is typically 1:1, and nurses cross-cover both medical and surgical ICU patients. There is not a specific protocol for initiating antipsychotics for agitation or delirium in this ICU. The choice of antipsychotic and decision to initiate therapy is based on provider preference. Patients are generally prescribed antipsychotics if they are not responding to sedative or analgesic therapy and failed nonpharmacological management of delirium. Quetiapine, olanzapine, and risperidone were selected for review in this study because they have been previously identified as the most common oral atypical antipsychotics continued at hospital discharge in ICU patients.3,8 Antipsychotic agent and duration of therapy by hospital location were identified using MedMined® Surveillance Advisor. All patients identified in this report were reviewed and included in the analysis if they received ⩾1 dose of quetiapine, olanzapine, or risperidone during their stay in the MSICU. Patients were included if they received more than one type of oral antipsychotic or were switched to alternative antipsychotic during their admission. Patients who were prescribed antipsychotics prior to admission or died during the hospital admission were excluded from the study. This study was approved by the institutional review board, which waived the need for informed consent.
We collected the following variables from the electronic medical record: age, sex, admitting ICU service, admission diagnosis, presence of TBI and admitting Glasgow Coma Scale (GCS), past medical history, geriatric and/or psychiatric consultation, antipsychotic medications, ICU and hospital LOS, and hospital disposition. The time to receive the first dose of oral atypical antipsychotics and the atypical antipsychotic(s) initiated, added, or switched to during the hospital stay were documented. The indication for use and duration of therapy in the ICU and post-ICU were captured. The indication for use was based on documentation in the patient’s medical record. The duration of delirium was determined by reviewing the date of the first and last positive Confusion Assessment Method for the Intensive Care Unit (CAM-ICU) score. A history of dementia was based on the International Classification of Diseases, 10th Revision, Clinical Modification (ICD-10-CM) diagnosis codes or a key word search in the medical record. Other factors associated with delirium were captured including: requirement for mechanical ventilation, duration of mechanical ventilation, administration of opioids or benzodiazepines, and presence and duration of urethral catheter and physical restraint use. We evaluated antipsychotic-related adverse events to control for other possible reasons these agents may be discontinued prior to hospital discharge. The incidence of QTc prolongation (QTc ⩾ 500 millisecond), over-sedation, or any antipsychotic-related adverse event documented in the medical report was collected. The percentage of patients who had a documented adverse event that subsequently prompted lowering of the dose or discontinuation of the agent was also captured.
Patients with or without an active prescription for atypical antipsychotics at discharge were compared using appropriate statistical tests. Independent t-tests were used to analyze continuous outcomes and Wilcoxon Signed-Rank tests were used to assess nonparametric data. Pearson chi-square tests were used to summarize categorical outcomes. A P value < .05 was considered statistically significant. A multivariate logistic regression was used to calculate the odds ratio (OR) with 95% confidence intervals (CIs) for each covariate that significantly affected continuation of antipsychotics at discharge. Covariates with a P value < 0.2 were eligible for inclusion in the final model using a backward selection method. Statistical analyses were performed using SPSS, version 25.0 (IBM Corp, 2017).
Results
A total of 279 patients were prescribed quetiapine, olanzapine, or risperidone in the MSICU between January 2017 and June 2018 (Figure 1). Among these patients, 124 patients (44.4%) were newly initiated on these agents during their hospitalization. A total of 78 patients (62.9%) were admitted to the MICU compared to 46 patients (37.1%) admitted to the SICU. A total of 29 patients in the MICU (37.2%) were continued on atypical antipsychotics at hospital discharge compared to 25 patients in the SICU (54.3%) (P = .063). The MICU patients initiated on atypical antipsychotics were significantly older (62.5 ± 15.3 years vs 55.8 ± 18.0 years, P = .029) and had a higher mean Charlson Comorbidity Index (3.76 ± 1.88 vs 3.04 ± 2.59, P = .029) than the SICU patients. The MICU patients more often presented with alcohol withdrawal syndrome (7 [9%] vs 0%, P = .036), were more likely to be initiated on quetiapine compared to risperidone or olanzapine (62 [79.5%] vs 29 [60.9%], P = .025), and more often discharged to a skilled nursing facility (27 [34.6%] vs 3 [6.5%], P < .001; Table 1). A total of 23 SICU patients (50%) who were initiated on atypical antipsychotics were admitted secondary to trauma. Among these patients, 17 patients (73.9%) had a TBI with a median GCS on admission of 10 (interquartile range [IQR] = 6.5-14). Eight of the TBI patients (72.7%) were classified as severe with an admitting GCS < 9.
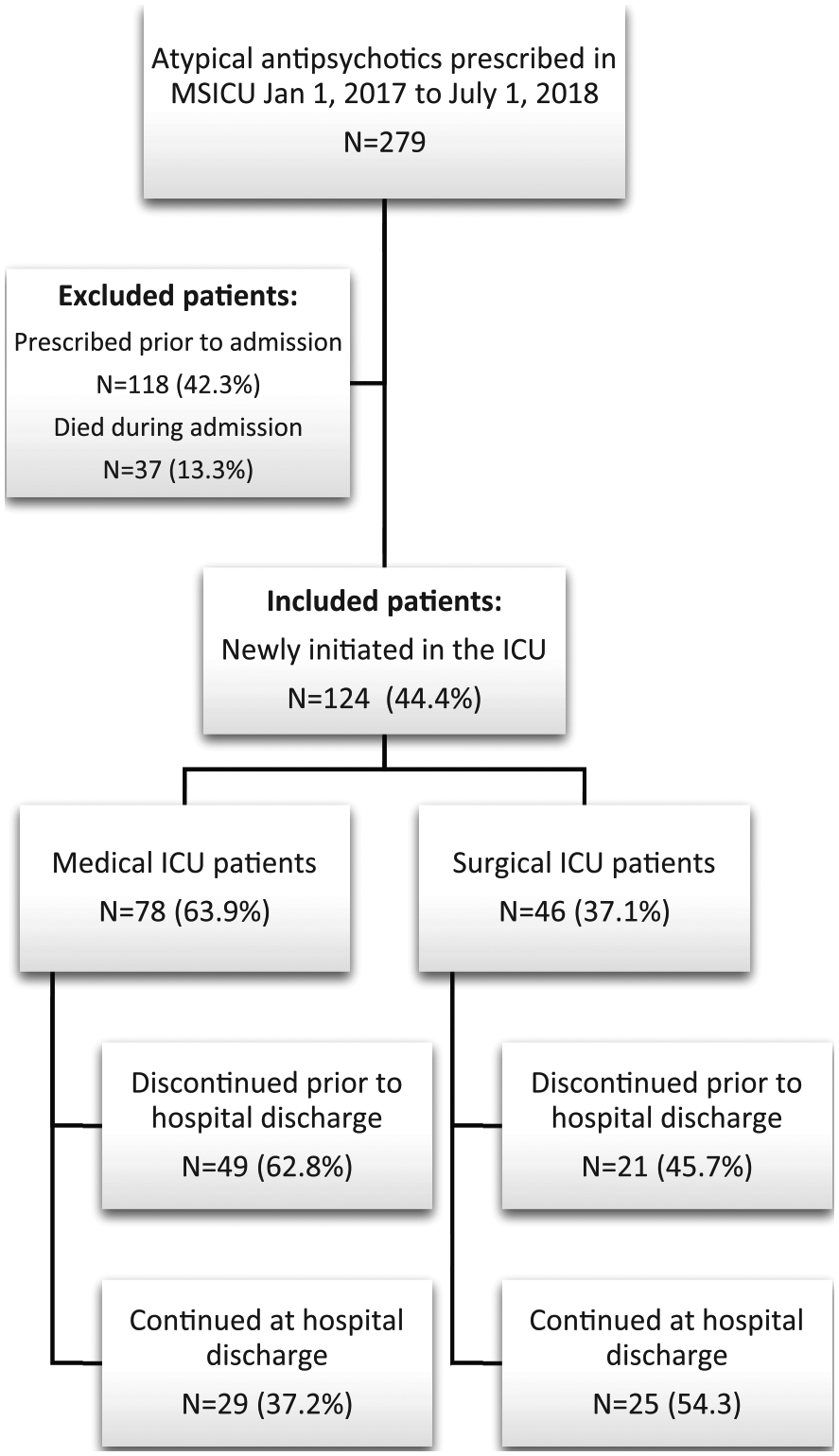
Flow diagram of included patients.
Baseline characteristics among medical and surgical ICU patients newly initiated on atypical antipsychotics.
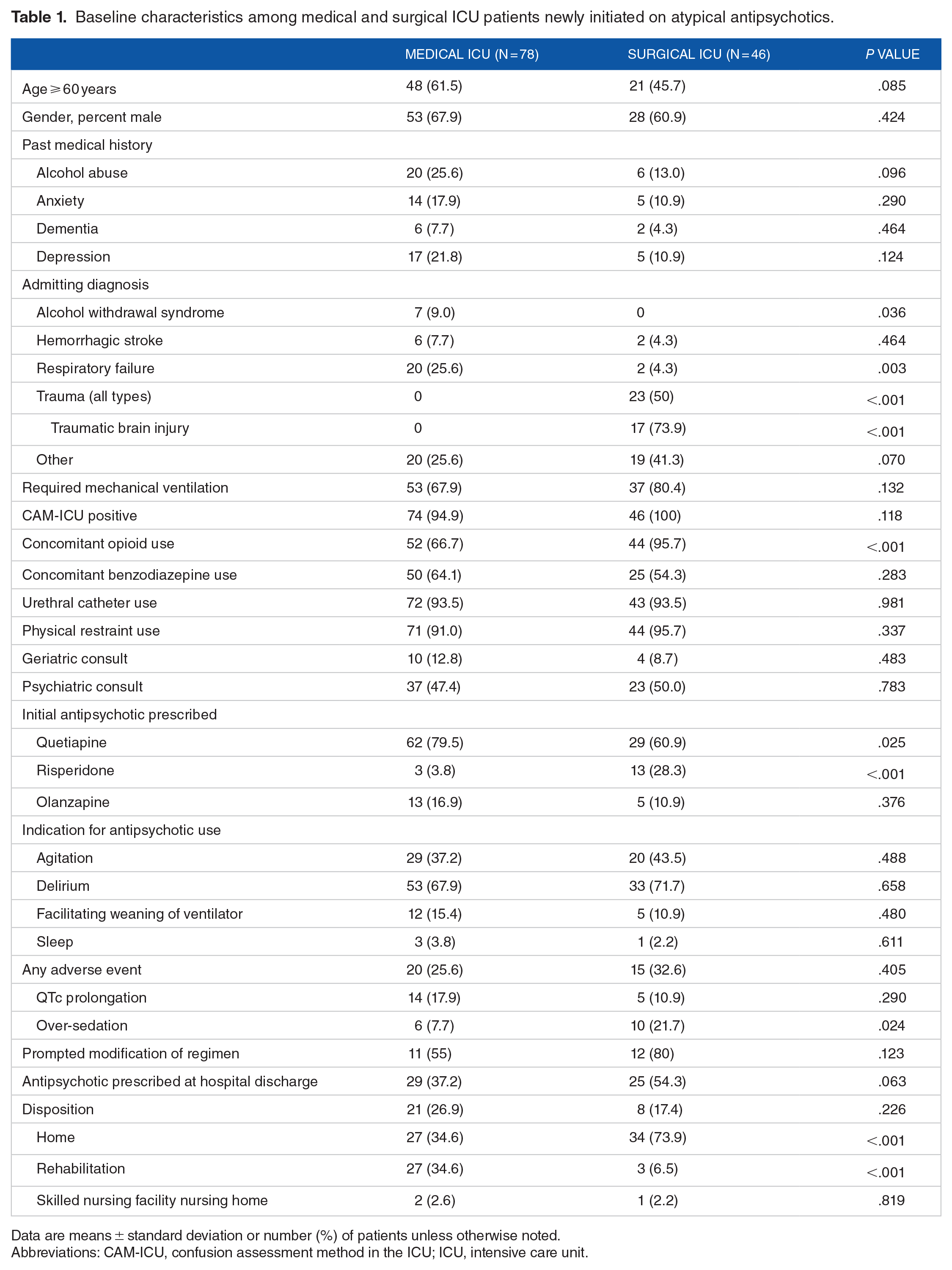
Data are means ± standard deviation or number (%) of patients unless otherwise noted.
Abbreviations: CAM-ICU, confusion assessment method in the ICU; ICU, intensive care unit.
The risk factors for continuation of atypical antipsychotics at hospital discharge in MICU and SICU patients are listed in Table 2. The percentage of MICU patients prescribed antipsychotics at hospital discharge was significantly higher in patients ⩾60 years of age (22 [75.9%] vs 26 [53.1%], P = .045), with a history of dementia (5 [17.2%] vs 1 [2%], P = .015), admitted secondary to hemorrhagic stroke (5 [17.2%] vs 2 [4.1%], P = .049), and initiated on risperidone (3 [10.3%] vs 0%, P = .022). The risk factor of pre-existing dementia remained significant after controlling for patients’ age, admitting diagnosis, and initial antipsychotic in a multivariate logistic regression, OR = 10 (95% CI: 1.11-90.5, P = .040). The MICU patients who were continued on antipsychotics at hospital discharge had a longer mean duration of therapy post-ICU (7.43 ± 5.25 vs 4.53 ± 3.27, P = .015) and cumulative days of therapy (10.8 ± 8.63 vs 6.92 ± 4.44, P = .012) and more likely to be discharged to a skilled nursing facility (15 [51.7%] vs 12 [24.5%], P = .015). The percentage of SICU patients continued on antipsychotics at hospital discharge was significantly higher in patients admitted with severe TBI (8 [72.7%] vs 0%, P = .004) and those initiated on quetiapine compared to olanzapine or risperidone (19 [76%] vs 9 [42.9%], P = .022). The SICU patients who were discharged on antipsychotics were more likely to go to rehabilitation facility compared to other locations (22 [88.0%] vs 12 [57.1%], P = .018).
Risk factors for continuation of atypical antipsychotics at hospital discharge.
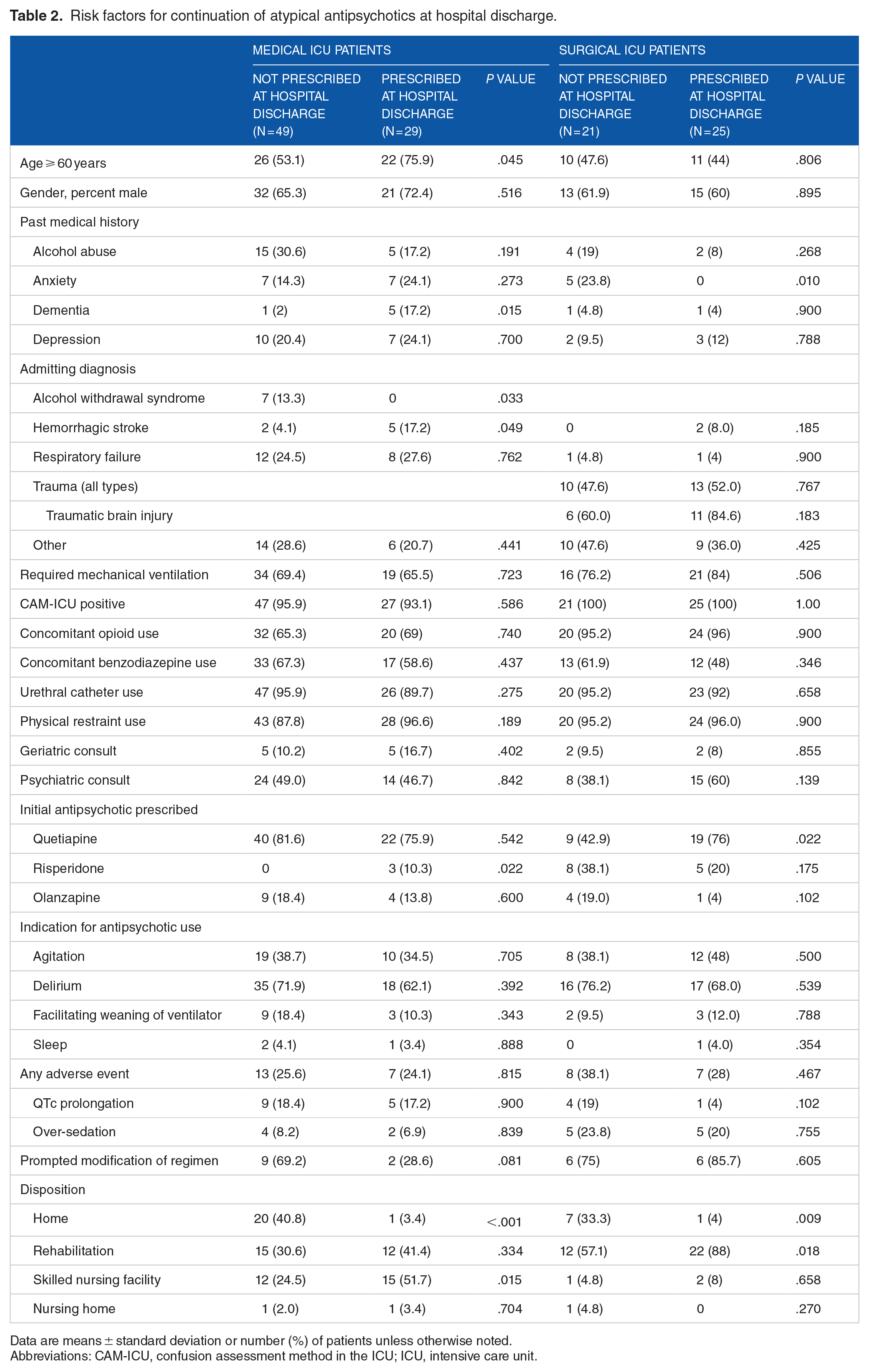
Data are means ± standard deviation or number (%) of patients unless otherwise noted.
Abbreviations: CAM-ICU, confusion assessment method in the ICU; ICU, intensive care unit.
A total of 35 antipsychotic-related adverse events (28.2%) were reported, of which, 23 (66%) prompted either a lowering of the dose or discontinuation of the medication. A total of 20 antipsychotic-related adverse events (25.6%) occurred in the MICU cohort compared to 15 (32.6%) in the SICU cohort (P = .405; Table 1). There was no correlation between the occurrence of adverse events and decreased likelihood of continuing atypical antipsychotics at hospital discharge when evaluating each ICU cohort separately (Table 2).
Discussion
Among the MICU patients, those who were older, had dementia at baseline, or admitted with hemorrhagic stroke were more likely to be discharged on atypical antipsychotics. Pre-existing dementia was associated with continuation of atypical antipsychotics after controlling for confounding variables. The SICU patients were started on atypical antipsychotics less often than the MICU patients, but when prescribed, they received them for a significantly longer duration. Among the trauma patients, those with severe TBI were more likely to be prescribed atypical antipsychotics at discharge compared with mild or moderate TBI. The MICU patients prescribed risperidone were more likely to be discharged on antipsychotics, whereas, the SICU patients prescribed quetiapine had a higher risk of continuing antipsychotics at discharge. The SICU patients were more likely to develop antipsychotic-related over-sedation compared to the MICU patients, but this did not appear to influence the risk of continuation of these agents at hospital discharge.
Delirium is an acute, temporary state of confusion characterized by fluctuation in mental status, inattention, and disorganized thinking or altered level of consciousness.15,16 Although delirium is commonly associated with short-term outcomes such as prolonged mechanical ventilation, hospital and post-ICU stay, increased ICU and hospital mortality, and greater healthcare costs; it is also associated with long-term disability such as cognitive impairment, decreased functional status at 6 months, and three-fold higher risk of mortality at 6 months.17–19 Patients who develop delirium may never regain baseline cognitive capacity and longer duration of delirium is associated with disability in activities of daily living and worse motor-sensory skills. 19 Both older age and pre-existing dementia are associated with a longer duration of delirium and a higher likelihood of being initiated on antipsychotics.20–23 In a study evaluating antipsychotic use among hospitalized patients, age ⩾75 years, and dementia were significant risk factors for initiation of antipsychotics. Conversely, age <75 years was associated with a lower risk of being discharged on antipsychotics. 2 In our study, we found that age ⩾60 years and patients with a history of dementia increased the likelihood of continuing antipsychotics at discharge in a MICU cohort. The higher risk of antipsychotics prescribed at discharge and the threshold of 60 years of age is consistent with previous literature that demonstrated that this group of patients is more susceptible to polypharmacy and inappropriate prescribing of medications. 24 We hypothesize that the significantly older mean age in MICU patients and higher percentage of pre-existing cognitive impairment contributed to persistent delirium that was unresolved at hospital discharge and led to the on-going need for antipsychotics. This warrants further study, as we did not capture the presence or resolution of delirium at hospital discharge in these patients.
Agitation and delirium can occur in up to 50% of patients with mild to moderate TBI in the first 4 days after the trauma. 25 Posttraumatic delirium is thought to be caused by neuro-inflammation, neurotransmitter imbalance, and structural brain damage. 26 Although the incidence of delirium is high in TBI patients, previous studies have not demonstrated that TBI is associated with a longer duration of delirium.23,27,28 Therefore, the reason patients with severe TBI were more likely to be discharged on atypical antipsychotics compared to those with nonsevere TBI in our study is unclear. A similar pattern was observed in the study by Kram et al 6 which found that among TBI patients, 23.7% were discharged on antipsychotics compared to 7.4% without a discharge prescription (P = .004). However, the authors did not find a correlation with the severity of TBI and risk of continuing antipsychotics. Further research is needed to evaluate the risks and benefits of long-term antipsychotic use in this patient population.
Most atypical antipsychotic utilization in the hospital among MICU patients occurred outside of the ICU. In the MICU patients who were discharged on antipsychotics received them for a mean duration of 7.43 ± 5.25 days in the hospital after leaving the ICU. The high post-ICU utilization of antipsychotics highlights an opportunity to perform an antipsychotic “time-out” to re-evaluate the status of delirium at transition of care and the current need for antipsychotics. One study evaluated the impact of an antipsychotic discontinuation bundle preintervention and postintervention in 281 patients transferred from the MICU. 29 The intervention resulted in significantly fewer patients discharged home or transferred from the MICU on antipsychotics (27.9% vs 17.7%, P = .014) and higher rate of therapy discontinuation within 72 hours of ICU discharge (61.5% vs 35.9%, P = .01). Future quality improvement initiatives that engage hospitalists and primary-care physicians to assess the appropriateness of atypical antipsychotics at various touchpoints in patients’ care and identify opportunities to wean patients off antipsychotics are warranted.
The purpose of this study is to identify risk factors associated with continuation of atypical antipsychotics at hospital discharge in MICU and SICU patients. Although we evaluated patterns of use, the retrospective nature of this study prevents us from knowing if prescriptions for antipsychotics at discharge were intentional or the result of poor medication reconciliation at transitions of care leading to inadvertent prescribing. Furthermore, we cannot determine if utilization of antipsychotics at discharge was actually appropriate, given the patients’ medical condition. However, we suspect that most of antipsychotic use, particularly in elderly patients, would be considered inappropriate based on previous literature. For example, in a study that prospectively evaluated the appropriateness of high-risk medications started in elderly ICU patients, 80% of patients initiated on antipsychotics were considered inappropriate to continue at hospital discharge. 5 In our study, the time from the first positive CAM-ICU score until initiation of antipsychotics was 4.26 ± 4.05 days in MICU patients and 4.80 ± 4.67 days in SICU patients. This suggests that many of the patients had signs of refractory delirium and agitation that failed to respond to nonpharmacologic interventions such as frequent reorientation, early mobilization, and reducing sleep disruption prior to initiating antipsychotics. In addition, a significant proportion of patients had a history of alcohol abuse or a primary diagnosis secondary to alcohol withdrawal and required a psychiatry consult to manage patients’ symptoms. Therefore, the prescribing patterns in these patients may not reflect how antipsychotics are commonly used at other institutions.
Conclusion
A significant percentage of MICU and SICU patients newly initiated on atypical antipsychotics remained on these agents at hospital discharge. Several risk factors influencing continuation of therapy existed in the two cohorts. Age ⩾60 years, pre-existing dementia, hemorrhagic stroke, and initiation of risperidone were associated with continuation of antipsychotics at discharge in the MICU cohort. In the SICU cohort, patients with TBI and those initiated on quetiapine were more likely to be discharged on antipsychotics. The high percentage of older patients and those with dementia prescribed atypical antipsychotics at discharge is concerning, given the known risks associated with long-term use in these patients. Implementation of strategies to prevent delirium and actively wean off antipsychotics once delirium has resolved may help reduce initiation and unnecessary continuation of these agents at hospital discharge.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Made a substantial contribution to the concept or design of the work: ARL, SA
Acquisition, analysis or interpretation of data: ARL, AT, DA, MP, SA
Drafted the article or revised it critically for important intellectual content: ARL, SML, AT, DA, MP, SA
Approved the version to be published: ARL, SML, AT, DA, MP, SA
