Abstract
Animal-type melanoma is an exceedingly rare histological variant of melanoma in humans. The name was coined to reflect similar histological features to melanomas in grey horses. We present a case of animal-type melanoma. The neoplastic cells were heavily pigmented with an epithelioid morphology, round nuclei and prominent eosinophilic nucleoli. Only occasional mitotic figures were identified. The tumour cells had diffuse and nodular growth patterns with involvement of the dermis and the subcutaneous tissue. The patient had a “benign cellular blue naevus” excised 9 years earlier from the same site. Review of the previous case revealed heavily pigmented epithelioid cells with similar morphology to the current case. Nuclear pleomorphism was minimal and only a single mitotic figure was present. The lesion extended to the margins of excision. The diagnosis of animal-type melanoma was made on the current case and on the previously misdiagnosed case.
Recurrence of this case nine years following incomplete excision further supports the hypothesis that animal-type melanoma is a distinct histological type of malignant melanoma with an indolent clinical course.
Introduction
William Dick was first to describe a heavily pigmented melanocytic neoplasm in the skin of grey horses in 1832 (Dick, 1832). The morphological parallel between these lesions and similar neoplasms in humans was first recognised by Darier in 1925 and the term “melanosarcoma” was introduced (Darier, 1925). Since then, only a few isolated cases have been reported (Kazakov et al. 2004; Punjabi et al. 2006; Tuthill et al. 1982; Levene, 1979; Pathy et al. 1993; Requena et al. 2001; Howard et al. 2005; Sass et al. 2006) and only a few series of cases have been published (Batolo and Lentini, 2004; Antony et al. 2006; Crowson et al. 1999; Zembowicz et al. 2004).
Animal-type melanoma is an exceedingly rare variant of melanoma. The tumour affects all age groups including children with a predilection for middle-aged to old adults (Antony et al. 2006). There is no sex or site predilection. The prognosis is unclear given the rarity of this lesion; however it is believed to be associated with an indolent clinical course.
Case Report
A 61-year old female presented with a dark pigmented nodular lesion with irregular edges on the right arm. The lesion had a variegated colour with shades of blue-black, measured 1.7 cm. The patient was uncertain of the duration of the lesion. The clinical impression was that of a malignant melanoma. The lesion was excised. The patient had a previous history of a “benign cellular blue naevus” at the same site removed 9 years previously. Following excision of the current lesion the patient underwent wider excision followed by a sentinel node biopsy.
Examination of the current case revealed a pigmented melanocytic lesion (Figs. 1 A, B and C). The lesion involved the full thickness of the dermis and extended into the subcutaneous tissue. Maturation was absent. There was no evidence of junctional or intra-epidermal components. The cells were arranged in nodules, sheets and fascicles and showed epithelioid morphology. The neoplastic cells were focally separated by sclerotic collagen. The cytoplasm showed pigment deposition ranging from fine granular light brown melanin to dark coarse deposits focally obscuring the nuclear detail. Where visible the nuclei were vesicular with prominent eosinophilic nucleoli. Nuclear pleomorphism was present but not prominent. Occasional mitotic figures were seen (<3/50 HPFs). There was no evidence of epidermal hyperplasia, ulceration, necrosis, regression, lymphovascular space invasion or perineural invasion. A host lymphocytic response was absent.
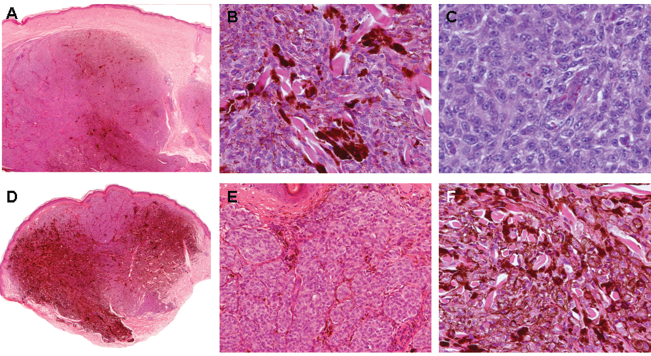
Haematoxylin and eosin section of the recurrent animal-type melanoma (
Review of the previous lesion revealed a heavily pigmented dermal melanocytic proliferation with cytological features similar to those seen in the current specimen (Figs. 1 D, E and F), however nuclear pleomorphism was minimal and only two mitotic figures were identified on multiple deeper levels. The lesion occupied the papillary and reticular dermis and extended to a depth of 4 mm. The superficial aspect of the lesion showed a nested appearance and was lightly pigmented whereas the deep part and the periphery showed confluent sheets of heavily pigmented cells separated by sclerotic collagen bands reminiscent of a blue naevus. The lesion was present at the deep and radial margins of the specimen. No junctional component was present.
The neoplastic cells in both lesions were positive for S-100 protein and HMB45. MIB1 highlighted the presence of occasional positive melanocytic cells in the dermis.
The diagnosis of animal-type melanoma was made on the current case and on the previously misdiagnosed “blue naevus”.
The sentinel lymph node was negative for malignancy. The patient is free of disease 46 months following the re-excision.
Discussion
Animal-type melanoma is a distinct histological type of malignant melanoma. The tumour is characterised by a neoplastic proliferation of melanocytes with striking pigment synthesis hence the alternative terms “pigment synthesising melanoma” (Antony et al. 2006) and “melanoma with prominent pigment synthesis” (Crowson et al. 1999; Kazakov et al. 2004). The lesion usually involves the full thickness of the dermis. The pattern of melanin pigmentation ranges from fine granular to coarse deposits. A pagetoid component is very rarely seen (Crowson et al. 1999). The tumour cells are arranged in sheets and/or nests. In some cases the tumour cells infiltrate the adventitial dermis of follicular and adnexal structures. The close association of tumour cells to the follicular sheath has prompted an alternative terminology for this neoplasm, namely pilar neurocristic hamartoma (Crowson et al. 1996).
It is important to recognise this lesion and distinguish it from other benign and malignant hypercellular pigmented melanocytic lesions, in particular, cellular blue naevus, pigmented epithelioid blue naevus, malignant cellular blue naevus, deep penetrating naevus, pigmented spindled and epithelioid variants of Spitz, malignant melanoma arising in naevi of Ito and Ota and regressed melanoma with prominent melanophages.
Cellular blue naevus is a well-circumscribed, symmetrical and fibrotic lesion with a “dumbbell” configuration and shows two distinct alternating hypercellular and hypocellular zones. The hypercellular zone is made up of nests of plump oval cells with bland round nuclei containing delicate chromatin and small blue nucleoli. The collagenised hypocellular areas are made up of spindle-shaped cells with prominent pigment laden macrophages, reminiscent of a common blue naevus. Mitotic figures are rare and no atypical forms are present.
Epithelioid blue naevus is a rare variant of blue naevus that is usually but not always associated with the Carney complex. The lesion is poorly circumscribed and is made up of two cell types. The predominant component shows heavily pigmented globular cells with vesicular nuclei and eosinophilic nucleoli, and the second shows lightly pigmented polygonal cells. The cells fail to show maturation with depth. Mitoses are rare. The reported cases have not recurred or metastasised. Zembowicz et al. compared epithelioid blue naevi with animal-type melanoma and found that both lesions have overlapping morphological features. They concluded that they represent part of the spectrum of pigment synthesizing melanoma (Zembowicz et al. 2004).
The pigmented epithelioid variant of Spitz naevus is a symmetrical and well-circumscribed lesion. The epidermis usually shows epidermal hyperplasia with hyperkeratosis. The intra-epidermal component shows nested and lentiginous proliferation of heavily pigmented epithelioid melanocytes with abundant eosinophilic cytoplasm, uniform vesicular nuclei and prominent eosinophilic nucleoli. Intraepidermal spread is limited to the lower half of the epidermis. Mitoses are usually confined to the junctional component.
Deep penetrating naevus is usually a symmetrical wedge-shaped compound melanocytic lesion. The junctional component is composed of nests of melanocytes. The dermal component extends to the deep reticular dermis and may reach the subcutis. It usually follows neurovascular bundles and adnexal structures. The melanocytes in the superficial dermis tend to have epithelioid morphology with vesicular nuclei and small eosinophilic nucleoli whereas the deep aspect of the lesion is made up of spindle-shaped cells. Melanophages are present. Mitoses are usually absent.
Malignant blue naevus often arises from malignant transformation of a cellular blue naevus or rarely, de novo. The neoplastic cells show spindle morphology, marked nuclear pleomorphism and brisk mitotic activity. Necrosis is often seen. These morphologic features are helpful in distinguishing animal-type melanoma from a malignant blue naevus.
Regressed melanoma is characterised by reduced numbers of melanoma cells and a chronic inflammatory cell infiltrate, melanophages, horizontal scarring and telangiectatic blood vessels.
Given the rarity of animal-type melanoma, its biological behaviour is uncertain. Although there are three reported cases of patients who died from widespread metastatic disease (Levene, 1979; Crowson et al. 1999; Batolo and Lentini, 2004), it is generally regarded as a neoplasm with an indolent clinical course. The term “pigmented epithelioid melanocytoma” was proposed by Zembowicz and associates to reflect the low grade nature of the tumour (Zembowicz et al. 2004).
The diagnosis is based on the presence of intradermal deeply pigmented melanocytes with epithelioid morphology. Mitotic count is low but mitoses are almost always seen in the dermal melanocytes. Therefore careful examination of the histological sections and examination of multiple deeper levels is essential. It is important to recognise this entity and distinguish it from other lesions because of the prognostic implication. Although the lesion was incompletely excised local recurrence occurred after nine years. This further supports the theory that animal-type melanoma is a distinct type of melanoma with a less aggressive clinical course than vertical growth phase melanoma with similar histological parameters (Crowson et al. 1999). However, the lesion has a metastatic potential, therefore full excision with sentinel node biopsy (Crowson et al. 1999) and long term follow up are indicated. Molecular and cytogenetic studies may provide further insight into the pathogenesis of animal-type melanoma and may explain the indolent behaviour of this rare type of melanoma.
Footnotes
Acknowledgment
The authors thank Professor P. McKee for confirming the diagnoses.
