Abstract
Introduction:
Significant associations between allergic rhinitis and bronchial asthma have been established and as a result of bronchial hyper-responsiveness, patients can have deranged pulmonary function tests. We aim to compare previous such studies with the result of our study done in India wherein we identify among allergic rhinitis patients who despite not having overt asthmatic symptoms, have pulmonary function derangements, quite possibly at a subclinical disease level.
Materials and Methods:
We studied 74 patients of allergic rhinitis and after meticulous clinical work up, they underwent blood tests including hemogram, absolute eosinophil count, and total serum IgE followed by pulmonary function tests.
Results:
Out of 74 patients 60 (81%) had intermittent allergic rhinitis whereas only 14 (19%) had persistent allergic rhinitis. Pulmonary function tests showed reversible obstruction, ie, >10% improvement in FEV1 with inhaled bronchodilators (as seen in asthma) in 18 (24.3%), mild obstruction in 14, and moderate obstruction in 4 cases.
Conclusion:
The study emphasizes the importance of pulmonary symptoms and the performance of pulmonary function tests in cases of allergic rhinitis patients to rule out latent asthma.
Introduction
Allergic rhinitis (AR), a common inflammatory condition affecting upper airways mainly the nose and often eyes, is characterized by symptoms such as sneezing, rhinorrhea, pruritus, and congestion which usually occur on exposure to allergens such as pollen, mites, dust, and other stimuli. Allergic rhinitis patients often have comorbidities, asthma being one of the most common. At least as many as 80% of asthma patients have symptoms of AR and up to 40% of patients with AR have associated asthma.1,2 Current pathophysiological studies suggest both conditions as manifestations of chronic inflammatory syndrome of the common airway or ‘united airway disease’.3,4 Both of these disorders affect between 25% and 50% of the population and mar the health and quality of life of individuals and societies leading to social and financial burdens at a global level.
The frequent co-occurrence of both these conditions and their proven close relationship in various studies led World health Organization (WHO) and the ARIA (Allergic Rhinitis and its Impact on Asthma) initiative to issue documents in 2001 and in 2008, which provide a comprehensive overview of the etiopathogenesis, diagnosis, and treatment of AR. The update proposes that management as one condition one airway-one disease, may alleviate the other coexisting disorders. 5 Patients having persistent AR should be checked for asthma. This also is one of the key goals in the Finish Allergy Programme 2008-2018, to reduce the load of allergic rhinitis and asthma in the community. 6 Although few studies have been done in India to see the prevalence of asthma in patients of AR, results of our study compare previous studies and help further analyse, assess, and model to propose standards of evaluation, norms, and guidelines for AR patients.
We also aim to recognize elements which help better identify cases with AR who, despite having absent overt asthmatic symptoms, may have pulmonary function alterations, possibly at a subclinical disease level.
Materials and Methods
This is a prospective study done in the department of Otorhinolaryngology, Head and Neck Surgery, of a tertiary care hospital during a period of 2 years from January 2013 to December 2015. A total of 74 patients with features of AR who presented to our outpatient department were enrolled in the study. After obtaining written informed consent, the patients were given a structured questionnaire requesting demographic details (age, gender, and residence), data on smoking, personal history, family history, history of atopy, and clinical features of AR (frequency and severity). They were further classified into intermittent AR, and persistent AR as per WHO-ARIA initiative. Recruited patients subsequently underwent hemogram with erythrocyte sedimentation rate (ESR), total serum IgE testing, absolute eosinophil count (AEC), chest X-ray, and pulmonary function tests. Presence of asthma was indicated by reversible airway obstruction with administration of a bronchodilator agent as shown by ⩾10% increase in FVC (forced vital capacity) or FEV1 (forced expiratory volume in 1 second).
All cases were put on medical treatment as per ARIA guidelines and then examined for symptom relief on follow up.
Results
Out of 74 patients diagnosed with AR, 41 were males and 33 females (1.24:1 male-to-female ratio). Age ranged from 8 years to 51 years with maximum patients in 21-30 age group. History of smoking was present in 19 (25.6%) of patients out of which 7 (9.4%) were active and 12 (16.2%) passive smokers whereas 55 (74.4%) were nonsmokers. In total, 11 (14.8%) had positive family history of ‘united airway’ disease (asthma or AR) whereas 63 (85.2%) had no such family history. Maximum patients 44 (59.4%) belonged to
Clinical profile of patients with allergic rhinitis.
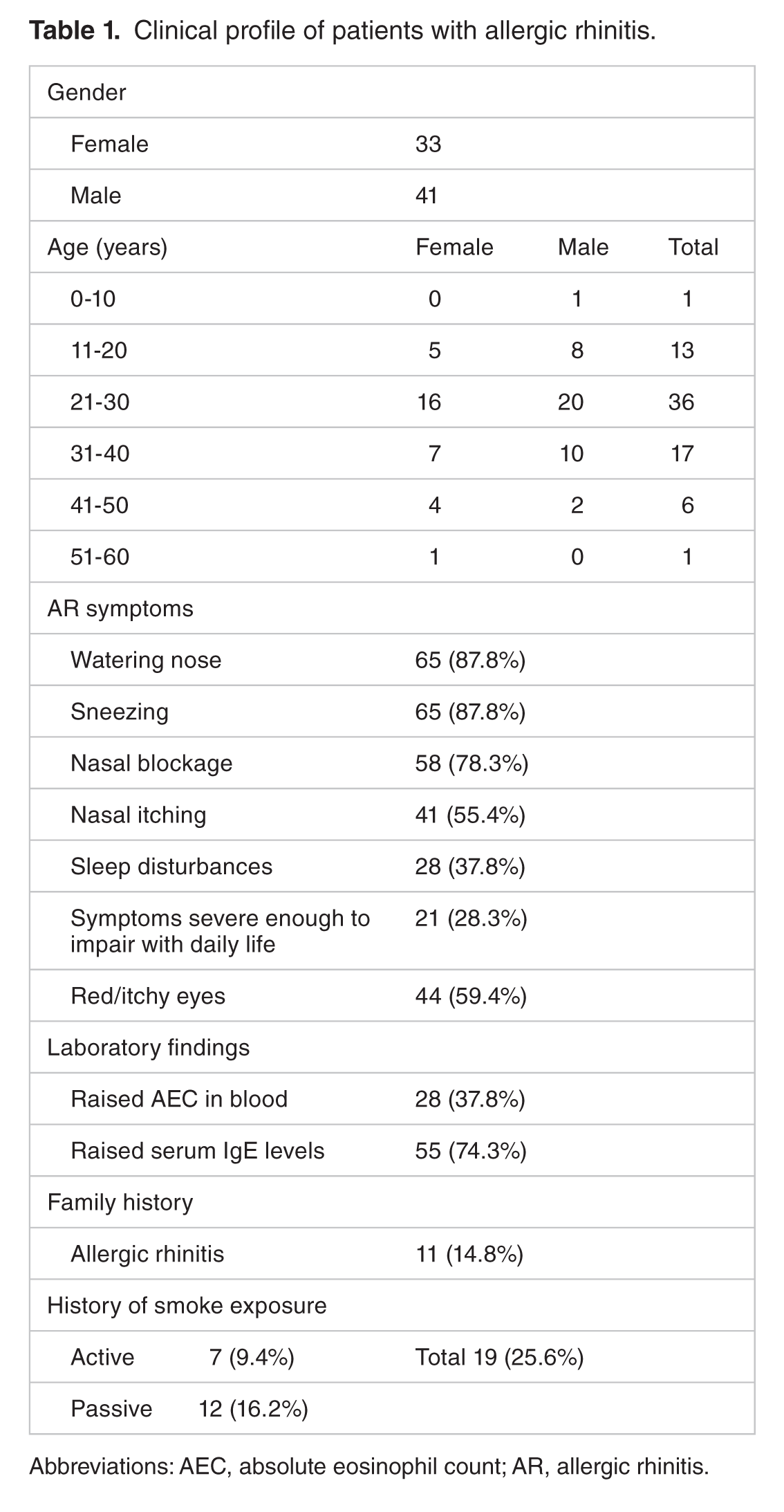
Abbreviations: AEC, absolute eosinophil count; AR, allergic rhinitis.
Watering nose and sneezing were the most common symptoms seen in 65 cases (87%) followed by nasal blockage in 58 (78.3%) cases. They were classified into intermittent AR and persistent AR as per WHO initiative ARIA. Out of 74 patients 60 (81%) had intermittent AR wheras only 14 (19%) had persistent AR. Mild AR symptoms were present in 35 (47.2%) and moderate-severe symptoms of AR were seen in 39 (52.8%) patients. Pulmonary function test (PFT) showed reversible obstruction, ie, >10% improvement in FEV1 with inhaled bronchodilators in 18 (24.3%), mild obstruction in 14 and moderate obstruction in 4 cases – Table 2. Comorbid latent asthma was more commonly detected in persistent AR group (35.7%) as compared with intermittent AR cases (21.6%) – Table 3.
Status of pulmonary function in patients with allergic rhinitis.
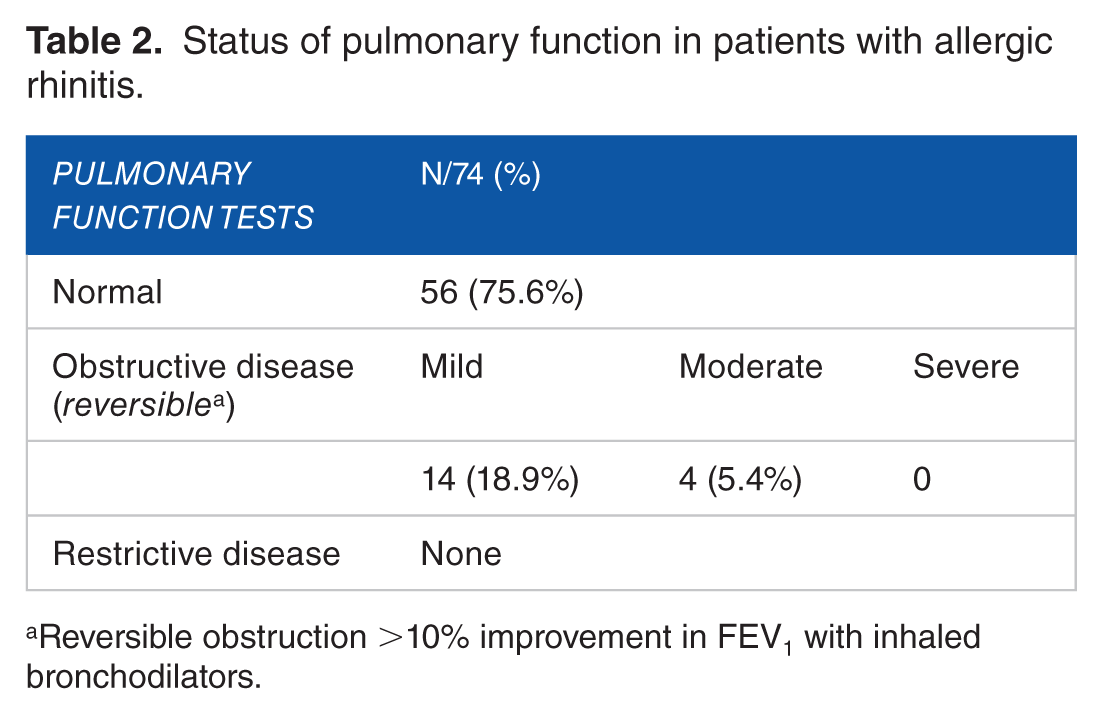
Reversible obstruction >10% improvement in FEV1 with inhaled bronchodilators.
Break up of allergic rhinitis cases and presence of associated latent asthma.
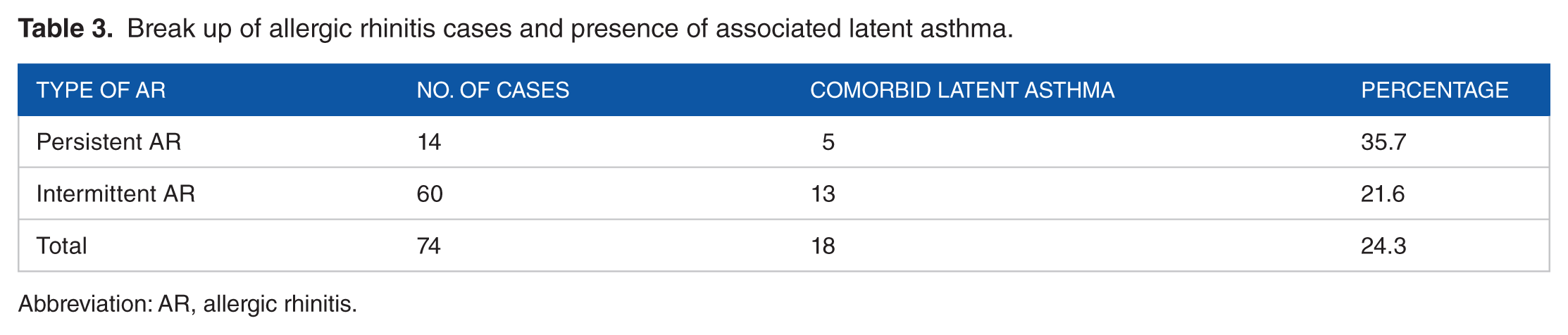
Abbreviation: AR, allergic rhinitis.
Discussion
The percentage of males (53.8%) was seen marginally higher than females (46.1%) in our study. This is similar to a study done by Patel et al 7 wherein out of 70 AR patients 52.8% were males and 47.1% females. Many of our AR cases were within agegroup of 21-30 years and the mean age of patients in our study was 33.12 years although one patient (1.3%) was elderly. This inference that elder patients had lesser risk of asthma, AR, and their association is in accordance with various studies 8 although many authors have validated the opposite pattern as well.9,10
In our study, watering nose and sneezing were the most common presenting symptoms in 65 (87.8%) patients. This is similar to the study done by Patel et al 7 in which most common symptom was rhinorrhea (100%) followed by sneezing present in 95.7% patients and nasal blockage in 22.8% patients. Only 25.6% of AR patients in our study were smokers (9.4% active and 16.2% passive). This is also in agreement with study done by Bugiani et al 11 who also found lower prevalence of AR in smokers. Bugiani gave a possible explanation that AR patients either do not start smoking or they stop sooner.
The association between allergic diseases and socioeconomic status is contentious. Most of our patients belonged to lower socio-economic class 44 (59.4%) and this is in accordance with studies which have suggested AR and asthma to be more frequent in families with low socioeconomic status, whereas sensitization to aerial allergens appears to be more common in persons with higher socioeconomic status during childhood. 12 However, this might also be linked to other uncontrolled variances in life style and environmental exposures among the groups, and demands for further studies.
The basic investigations required in the evaluation of a patient with suspected AR include complete blood picture with peripheral eosinophil percentage, AEC, total IgE levels, nasal smear examination for eosinophils. A normal eosinophil count is less than 350 cells/µL of blood. The relationship between eosinophilia and allergic conditions has been well established in various studies. 13 In our study, AEC was raised only in 37.6% of patients of AR which is similar to studies done by Venkateswarlu and Murali Mohan 14 and Sonawane et al. 15 IgE facilitated allergic sensitization is the cause of allergic diseases and raised total IgE. Despite wellknown limitations it is frequently included diagnostic criterion for allergic diseases. In 1985, Bousquet et al in a study reported the mean total serum IgE levels was 38 ± 43 KU/L-180 KU/L in normal people and 94 ± 93 KU/L in allergic individuals. Moreover asthmatics had higher mean IgE levels than those suffering from AR. 16 In our study, serum IgE was raised in 74.3% of patients.
Routinely carrying out skin prick tests or radio-allergosorbent test (RAST), enzyme linked immunesorbent assay (ELISA) tests to evaluate the atopic skin status of all these cases is not feasible in most of the outpatient clinics of developing countries. Similar to other authors we too made an attempt to determine the patients who could be given treatment related to allergic symptoms based on the findings acquired from correlation of specific symptoms with the blood markers (total IgE levels and peripheral eosinophils). 17
Allergic Rhinitis and its Impact on Asthma (ARIA) classification has been endorsed by numerous studies. In total, 81% of our patients had intermittent AR, whereas only 19% had persistent AR, and mild AR was present in 35 (47.2%) and moderate-severe symptoms of AR were seen in 39 (52.8%) patients. This is similar to study done by Bachert et al 18 who found that 59% of his subjects had intermittent, 41% persistent rhinitis, 25% mild, and 75% moderate-severe AR whereas in a study done by Navarro et al 19 46% were intermittent, 54% persistent, 43% mild, and 57% moderate-severe AR.
There is evidence showing that patients with AR may have an increased prevalence of bronchial hyper-responsiveness and alterations in the functional testing of breathing. 20 In a study done by Jeffery et al 21 on 107 patients of AR deranged pulmonary function tests were observed in 39.1% of cases and 26.1% of patients were diagnosed with asthma. Our study showed 18 (24.3%) of AR patients had PFT similar to asthma. Pulmonary function test showed mild obstruction in 14 (18.9%) whereas moderate obstruction in 4 (5.4%). This is in accordance with studies done by Simons 4 and Patel et al 7 wherein associated asthma was present in 15.3% patients. These results point to the presence of substantial variations in the prevalence of the different types of AR as per characteristics of study population and in context to health care.
Conclusion
The study highlights the significance of PFT in AR for recognizing the upper and lower airway disease as a continuum of single disease process and thus importance be given to history of chest symptoms in AR patients to check for latent asthma.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
SM: Protocol design
JM: Data collection and analysis, manuscript review
APS Technical assistance
SJ and NN: Study execution and Data collection
SB: Manuscript editing and Final approval.
