Abstract
Introduction:
Tracheostomy is a vital airway procedure for critically ill patients with acute respiratory failure. This study presents a rare but serious complication: the fracture and migration of a tracheostomy tube into the tracheobronchial tree, and discusses its management.
Case Presentation:
A 43-year-old male, with a tracheostomy tube in place for 8 years following a neck blast injury, presented with a foreign body in his airway. Chest X-ray revealed a fractured metallic tracheostomy tube lodged in the left main bronchus. The tube was successfully removed by rigid bronchoscopy under general anesthesia, and the patient was discharged in good condition with a new tracheostomy tube.
Discussion:
Tracheostomy tubes, typically made of polyvinyl chloride or metal, can fracture due to prolonged use without regular check-ups, or replacement. Patients may present with mild respiratory symptoms or be asymptomatic. Diagnosis is confirmed by X-ray, and removal is performed via rigid bronchoscopy.
Conclusion:
Fractured tracheostomy tubes are a rare but potentially fatal complication requiring urgent bronchoscopy. Regular follow-up, proper care, timely tube replacement, and patient education are essential to prevent such occurrences.
Introduction
Tracheostomy is a commonly performed airway procedure in the intensive care unit (ICU) to facilitate ventilation in critically ill patients. 1 It can be lifesaving in cases of airway obstruction and acute respiratory failure. It is a relatively safe procedure with a mortality rate of less than 5%. 2 There are several types of tracheostomy tubes, with plastic and metallic tracheostomies being the most frequently utilized. Numerous patients with laryngotracheal lesions require long-term tracheostomy tube placement and extended care. 3
Complications of tracheostomy can be classified as early or late. Early complications include infection, hemorrhage, pneumothorax, and tracheostomy tube obstruction or displacement. Tracheostomal stenosis, innominate artery erosion, and tracheoesophageal fistula are among the problematic late complications.4,5 A rare late complication with potentially fatal consequences is the fracture and subsequent aspiration of a tracheostomy tube into the tracheobronchial tree, necessitating urgent intervention due to the risk of airway compromise. Published reports of a fractured tracheostomy tube presenting as a foreign body in the left bronchus are infrequent.6,7 This study presents our experience with such a case involving a 43-year-old male patient who had been tracheostomized for 8 years, in which he was diagnosed with and successfully treated for a broken metallic tracheostomy tube aspirated into the left main bronchus. This case report has been reported in line with the SCARE Criteria. 8
Case Presentation
A 43-year-old male, known for aphonia and subglottic stenosis, was referred to our hospital for further investigation and removal of a suspected fractured metallic tracheostomy tube. The patient had been tracheostomy-dependent since 2014, following the ligation of the right internal and external carotid arteries due to a blast injury. His tracheostomy was complicated by a tracheocutaneous fistula, which was closed at our hospital. Shortly after the closure, the patient developed stridor, necessitating a reopening and bronchoscopy that revealed subglottic stenosis. A stainless-steel tracheostomy tube and a gastrostomy tube were inserted; the latter was removed before discharge, and the patient returned home in stable condition.
In 2015, the patient underwent fiberoptic laryngoscopy at another hospital, which revealed complete subglottic stenosis with granulation tissue causing impaired vocal cord mobility. He underwent bronchoscopy with potassium-titanyl-phosphate (KTP) laser and balloon dilation. Four years later, the balloon was removed, and the patient remained tracheostomy-dependent and stable on room air. His medical history was significant only for diabetes mellitus which was controlled with metformin.
In October 2022, the patient returned to our hospital for evaluation and management of a foreign body lodged in his airway. During the routine care of his tracheostomy, this distal part of his metallic tracheostomy got detached, the patient didn’t feel any respiratory distress, but he sought medical advice. On arrival to the emergency room, he was hemodynamically stable, with normal respiratory function and chest auscultation. Oxygen saturation was normal, with good bilateral air entry. Arterial blood gases showed mild respiratory alkalosis with decreased PO2, O2 saturation was 88% in the room air, but this was corrected immediately to 95% on 2 l nasal cannula.
Laboratory investigations were normal, but a chest X-ray revealed a metallic foreign body in the left main bronchus, identified as a fragment of the fractured tracheostomy tube (Figure 1). The patient was taken to the operating room for bronchoscopic removal under general anesthesia, but the initial attempt was unsuccessful. A few days later, a second attempt with rigid bronchoscopy under general anesthesia successfully extracted the fractured tracheostomy tube from the left main bronchus, and a new tracheostomy tube was placed without complications (Figure 2). The first attempt utilized flexible fiberoptic bronchoscopy, which proved inadequate for removing the metallic foreign body due to the object’s weight and the difficulty in securely handling it. In the second attempt, a rigid bronchoscope which offered greater maneuverability and grasping power, ultimately enabling successful removal of the metallic fragment. The rigid bronchoscope was inserted through the subglottis, where moderate narrowing was observed. Despite this, the scope was successfully advanced past the subglottic stenosis, the metallic part of the detached tracheostomy was held using forceps, and it was pulled out and removed. As a part of preparation for the second attempt we prepared a standby extracorporeal membrane oxygenation (ECMO) in the room, and the team was ready for possible thoracotomy in case if the endoscopic attempt fail.

Chest X-ray of the patient shows the radio-opaque tracheostomy tube lodged along the left main bronchus (arrow).
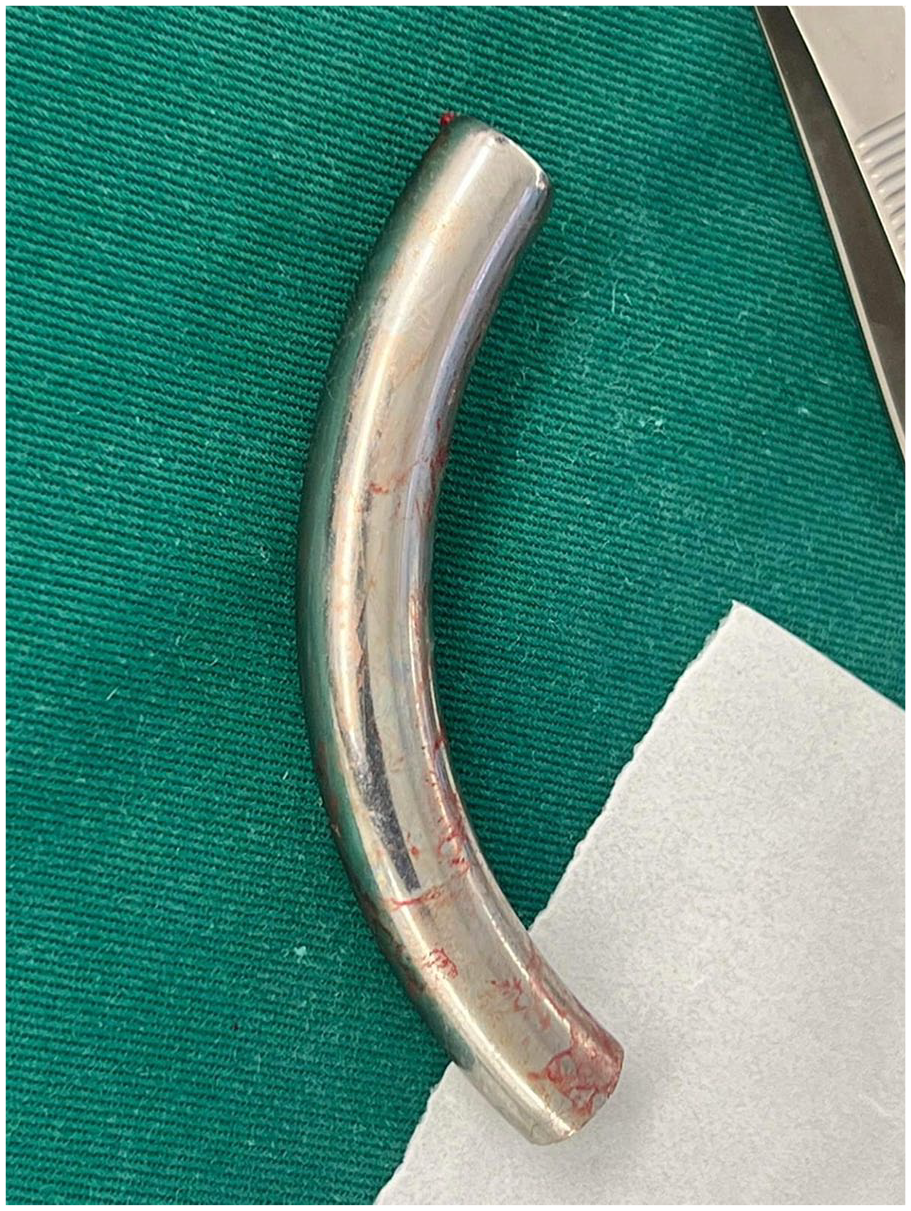
Photograph showing the tube after removal by rigid bronchoscopy.
ECMO was prepared using a left femoral vein cannula, right femoral artery cannula, and right internal jugular vein cannula but was removed postoperatively after confirming normal International Normalized Ratio (INR) levels. On postoperative day one, the patient was in good general condition, with a well-functioning polyvinyl chloride (PVC) tracheostomy, stable vital signs, and a normal chest X-ray (Figure 3). He tolerated oral intake, leading to his discharge on the first postoperative day. Specific instructions were provided to the patient at the time of discharge, emphasizing the need for regular follow-up visits, routine cleaning, and timely replacement of the tube to prevent similar complications in the future.

Chest X-ray after removal of the tube.
Discussion
Tracheostomy procedures are performed for various indications, including bypassing airway obstruction and preventing aspiration. The procedure is typically undertaken temporarily, with the tracheostomy tube removed once the underlying cause is resolved. However, in certain cases, such as the one presented here, the primary disease persists, necessitating permanent retention of the tracheostomy tube, which predisposes the patient to late complications. Among the various complications associated with tracheostomy, fracture and dislodgement of the tracheostomy tube are among the rarest. This complication presents with non-specific respiratory symptoms and is frequently misdiagnosed as other medical conditions, such as pneumonia, chronic bronchitis, and asthma. 9
The initial case of fractured tracheostomy was documented in 1960 by Bassoe and Boe. 3 Subsequently, analogous cases have been sporadically reported in the literature. The majority of these cases are observed in males and occur more frequently in metallic tracheostomy tubes. The most prevalent lodging sites reported in the literature were the trachea and the right main bronchus,4,10,11 while the most common fracture sites were the junction between the flange and the tube, and less frequently in the fenestration sites on fenestration tubes.4,12 In the present case, the fracture occurred at the flange-tube junction, and the tube was dislodged in the left main bronchus, which is an atypical site of dislodgement. Tracheostomy tubes are fabricated from metal, silicone, or polyvinyl chloride (PVC). The metallic tubes are more suitable for repeated and prolonged use as they can be cleaned and sterilized, in contrast to the PVC tubes that are typically disposable. Contemporary metallic tracheostomy tubes are composed of stainless steel, which is less susceptible to rust, corrosion, or fracture compared to historical metallic tracheostomy tubes that were manufactured from silver, copper, or zinc, all of which were vulnerable to corrosion by alkaline tracheal secretions. 13 Despite this, metallic tracheostomy tubes have fractured in the majority of documented cases in the literature. Several potential causes of tracheostomy tube fracture have been reported, including: deterioration due to prolonged use without adequate patient follow-up, mechanical stress from repeated removal, sterilization, and reinsertion, chemical reaction with bronchial alkaline secretion, manufacturing defects, and accidental trauma or damage resulting from dislodgement or impact with foreign objects, such as fingers or clothing.3,13 -15 It is evident that the majority of tracheostomy tube fractures are attributed to prolonged use of the same device. These cases are predominantly encountered in developing countries where economic constraints impede patients from periodically replacing the tubes and adhering to long-term follow-up appointments.
In this case, the aforementioned situation applies to the present report, wherein the fracture of the tracheostomy tube occurred in a patient who had been utilizing tracheostomy tubes for 8 years without regular follow-up examinations. Fracture and aspiration of tracheostomy tubes may manifest with acute or chronic respiratory symptoms, such as dyspnea or cough. Consequently, healthcare providers must be cognizant of this uncommon complication as a potential cause of such symptoms, as delayed diagnosis can result in more severe manifestations, including bronchiectasis and pneumonia. 11 Nevertheless, in certain instances, fractured tubes may not impede air passage, resulting in an absence of symptoms and subsequent delayed diagnosis. This can ultimately lead to lobar or segmental consolidation, abscess formation, or collapse due to obstruction of the tube lumen by mucus. 16 Therefore, when tracheostomy fracture and dislodgement are suspected, the diagnosis can be confirmed through chest radiography and managed with flexible or rigid bronchoscopy. The significance of this report lies in its presentation of a case involving a fractured and aspirated metallic tracheostomy tube that, despite causing minimal symptoms, was promptly diagnosed and managed.
This report also demonstrates the potential for tracheostomy tube fracture and aspiration in the home care setting, particularly in patients requiring prolonged use of metallic tracheostomy tubes in situ. Furthermore, the patient in this report presented with subglottic stenosis, which poses a significant challenge and results in a compromised airway. To mitigate this complication, several preventive measures can be implemented, including replacing the tracheostomy tube every 6 months, performing daily or alternate-day cleaning of the tube, conducting regular medical evaluations, and providing comprehensive education to both the patient and caregiver regarding tracheostomy care and maintenance.4,10
Conclusion
Tracheostomy tube fracture and migration into the tracheobronchial tree represents a rare but potentially fatal complication that may arise from various etiologies. Expeditious identification and management through bronchoscopy are essential, and the medical team should be prepared for potential thoracotomy or ECMO as necessitated. This complication can be mitigated through regular clinical evaluations, routine tube maintenance, periodic tube replacement, and patient education regarding tracheostomy care.
Footnotes
Authors’ note
Maher Deeb is also affiliated with General Surgery Department, Al-Quds University, Jerusalem, Palestine.
Consent to participate
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Author contributions
Mohammad Fityani: Investigation, Writing—original draft, Visualization. Yazan Juma: Writing—original draft, Visualization. Mohammed Omari: Writing—original draft, Visualization. Imad Tayyem: Writing—original draft, Visualization. Raghad Sweity: Project administration, supervision, Writing—review & editing. Maher Deeb: supervision, Writing—review & editing. Yousef Abu Asbeh: Project administration, supervision, Writing—review & editing.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article:
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All the available data are provided in this submission.
