Abstract
Introduction:
Intracranial empyema is a rare but serious and life-threatening infection. It is an accumulation of purulent material in the subdural or extradural space leading to development of subdural empyema or intracranial epidural abscess, respectively. The incidence of morbidity and mortality is high because the diagnosis is often unsuspected. Infections of dental origin could be responsible for such condition.
Case reports:
A 22-year-old female and 30-year-old male patients, both with no significant medical history, presented with subdural empyema and intracranial epidural abscess, respectively, both complicating pan-sinusitis of dental origin. Successful outcomes were achieved with surgical drainage of the lesions, antibiotic therapy, and extraction of affected teeth. Female patient underwent further management for neurological sequelae, while male patient was discharged without neurological complications.
Discussion:
Intracranial suppuration of odontogenic origin is an uncommon but extremely serious complication. The most common dental origins are caries with periapical involvement and periodontitis. Wisdom tooth extraction is the most common preceding dental procedure for this infection. A multidisciplinary approach is essential for the identification and treatment of suspected oral sources. Antibiotic therapy with surgical approach is the gold standard treatment.
Conclusion:
This sequel to odontogenic infection is quite rare, but it can be prevented by a good oral hygiene and removal of abscessed teeth.
Introduction
Suppurative intracranial infections of odontogenic origin are rare but potentially life-threatening, encompassing subdural empyema, meningitis, sagittal sinus thrombosis, brain abscess, and less frequently epidural abscess.1,2 An intracranial empyema is a collection of pus either in the subdural space (subdural empyema, SDE) or in the extradural space (epidural abscess, EDA). 3 Mortality rates have significantly been declined, due to improved medical imaging, antibiotics, and surgical techniques.4,5 These complications often result from contiguous spread or direct invasion from nearby infection sites, notably paranasal sinus and odontogenic sources. They often progress rapidly manifesting with symptoms such as meningismus, neurological deficits, and seizures. Urgent surgical drainage associated with simultaneous eradication of the primary source of infection and antibiotics are crucial for effective management.1,6 In this report, we present 2 cases of intracranial complications arising from a dental origin treated successfully with surgical and medical interventions at Fattouma Bourguiba University Hospital Monastir.
Case Reports
Clinical case 1
A 22-year-old female patient, with no significant medical history, was admitted to Fattouma Bourguiba University Hospital for the treatment of SDE complicating left anterior pan-sinusitis. She presented with symptoms of sinusitis, later developing paresthesia, and altered consciousness. The urgently performed face and brain Computed Tomography (CT) scan disclosed extensive sinus involvement on the left side (Figure 1A to C) and a well-defined, hypodense, crescent-shaped subdural collection in the right parietal area, measuring approximately 7 mm in size, consistent with SDE (Figure 1D).

Axial slices on face and brain CT scan revealed extensive sinusitis involving the left maxillary sinus (A), anterior ethmoid (B), and frontal sinus (C). Additionally, it identified a well-defined, hypodense, crescent-shaped subdural collection in the right parietal area, measuring approximately 7 mm in size, consistent with SDE (D).
An emergent craniotomy was carried out to evacuate the infectious collection, followed by Claforan, Gentamicin, and Vancomycin therapy. Dental examination identified multiple severely decayed teeth (26, 16, and 46) (Figure 2).

Intra oral examination revealed multiple severely decayed teeth (26, 16, and 46).
The face and brain CT scan showed a deep decay on the antral tooth 26 (Figure 3A and B).

(A, B) Coronal slices on Face and brain CT scan revealed a deep decay on the antral tooth 26.
This finding strongly suggested that tooth 26 was the probable source of infection, thereby confirming the odontogenic origin of the condition. Surgical removal of all the decayed teeth was performed (Figure 4A). During the extraction of tooth 26, an oro-antral communication occurred (Figure 4B), allowing pus aspiration for microbiological investigation.

Extraction of the decayed teeth (26 and 16) (A). Subsequently, an oro-antral communication created after extraction of the tooth 26 (B).
Staphylococcus aureus was detected, susceptible to antibiotics. The patient recovered well and was transferred to the neurosurgery department for further management of neurological sequels. The extraction sites healed with closure of oral fistula (Figure 5).
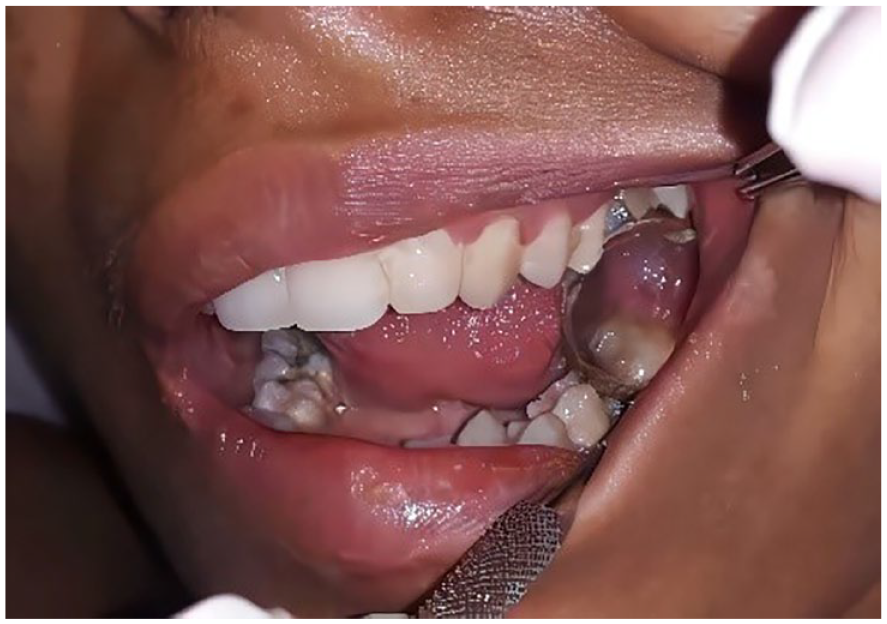
The extraction sites were healed, and it appeared that the oral fistula had closed.
Clinical case 2
A 30-year-old male patient, with a history of alcohol, cannabis, and smoking (15 pack-years), was admitted to Fattouma Bourguiba University Hospital for the treatment of a frontal right intracranial EDA. The patient had no prior history of medical or surgical treatments. He had a recent seizure and fever. The urgent brain CT scan revealed a millimetric right frontal extradural empyema measuring approximately 19 × 5 × 24 mm3, and causing ventricular compression and midline shift, indicative of hydrocephalus (Figure 6A to C). These findings were indicative of complications arising from right ethmoid-maxillary sinusitis of dental origin (Figure 6D).

Axial and sagittal slices on the brain CT revealed a millimetric, lentiform, right frontal extradural empyema measuring approximately 19 × 5 × 24 mm3. This empyema was causing compression of the ipsilateral ventricle and had resulted in an 18 mm midline shift, contributing to the compression under the falx cerebri and the onset of hydrocephalus (A-C). Additionally, coronal slices on the face and brain CT scan disclosed a right ethmoid-maxillary sinusitis of dental origin (D).
Immediate administration of high-dose intravenous treatments of Claforan, Vancomycin, and Metronidazole was initiated. However, the patient’s condition deteriorated with altered consciousness, anisocoria, and left hemiplegia. He was intubated, ventilated, and transferred to the intensive care unit ICU, where he underwent emergency decompressive craniotomy, and abscess drainage. Antibiotic treatment continued. Tests for hepatitis, HIV, and HBs Ag (Hepatitis B surface antigen) all returned negative. Despite mild neurological deficits, the patient responded well to surgery and antibiotic treatment and was transferred to neurosurgery department for further evaluation and management. The patient’s comprehensive workup was largely negative, except for oral examination revealing decayed teeth (16, 18). This dental examination provided a potential source of the infection (Figure 7).

Intra oral examination revealed multiple severely decayed teeth (16 and 18).
The CT scan revealed the presence of a right oro-antral communication associated with tooth 16 (Figure 6D). Surgical removal of decayed and periapically involved teeth (16 and 18), presuming the epidural abscess to be of odontogenic infection led to significant pain reduction and successful healing of extraction sites (Figure 8).

Extraction sites were healed without any oral fistula: (A) Day 5 post extraction and (B) Day 13 post extraction.
After antibiotics, craniotomy with abscess drainage and comprehensive dental care, the patient was discharged without neurological issues. Recovery was excellent 1 year later.
Discussion
Intracranial suppurations including meningitis, abscesses, SDEs, and EDAs, are rare but serious conditions requiring immediate medical and neurosurgical intervention due to their life threatening nature.6,7 Their incidence has significantly declined in recent decades.8,9 Brain abscesses, SDEs, and EDAs are among commonly encountered suppurative lesions of the central nervous system (CNS). 10 Dental infections, though uncommon, account for approximately 3% to 10% of brain abscess cases.8,11-13 Dental infections or procedures can lead to bacterial dissemination from the oral cavity, with periodontitis or caries involving molars posing the highest risk for intracranial infections.6,14 This observation aligns with the experiences of our patients. Dental procedures, including tooth extraction, root canal therapy, periodontal treatment, and dental prophylaxis, are linked to intracranial abscesses, with tooth extraction being particularly associated.10,11,14,15 Ewald et al 16 proposed diagnostic criteria for odontogenic intracranial abscesses:(i) absence of an alternative source of bacteremia; (ii) presence of oral microflora bacteria in the abscess; and (iii) clinical signs of active dental disease.6,9 Severe odontogenic infections may spread intracranially via 4 primary pathways: most commonly via contiguous spread, especially from upper jaw teeth, as observed in our patients; less frequently through systemic hematogenous bacteremia; direct venous drainage; and lymphatic drainage.5,6,17,18 Facial fractures with cerebrospinal fluid leaks and concurrent odontogenic infection increase the risk of intracranial abscess formation via direct sinus or hematogenous spread. 19 Infections from posterior teeth in the upper jaw are more likely to lead to brain abscesses due to their proximity to the maxillary sinus.20,21 An abscess on the same side as the odontogenic source indicates a contiguous spread, as seen in our second patient. Conversely, an abscess on the opposite side or in the posterior brain suggests a hematogenous route, as observed in our first patient. These observations provide valuable insights into infection spread pathways.6,8,9 Various risk factors increase vulnerability to severe dental infections, including weakened immune systems (eg, diabetes), medication use (eg, non-steroidal anti-inflammatory drugs), alcohol, tobacco, drug abuse, and malnutrition.5,10,22 Intracranial infections present with diverse clinical features, including focal neurological deficits, altered consciousness, seizures, headache, fever, nausea, vomiting, and meningismus. Patients may exhibit specific neurologic symptoms like hemiparesis. Generalized tonic–clonic seizures, as observed in our second patient, aid diagnosis. Signs of pansinusitis and dental infection may also be evident during evaluation.1,3,4,7,10,11,22,23 Computed tomography (CT) and magnetic resonance imaging (MRI) are mainstays in diagnosing CNS infections. Radiologic differentiation between SDE and EDA hinges on their relationship to the falx cerebri; SDEs typically remain unilateral, with crescent-like shapes (Figure 1), while EDAs can cross the midline.7,14,22,23 CT is cost-effective for abscess diagnosis, while MRI offers higher sensitivity for small collections and differentiating epidural from subdural.1,4,7,10,11 CT is preferred for neurosurgical planning.10,22,24 Our patients underwent CT scans, obviating further imaging needs. Clinicians should consider dental issues as potential sources of complications. Maxillary dental assessment through sinus CT and dental history helps identify odontogenic sources. 25 Lab tests often show inflammatory syndromes, necessitation prompt blood cultures. 22 Common oral bacteria like Streptococcus viridans and anaerobic bacteria often contribute to these infections.5,10,14,16,17,24 Standard management involves early surgical drainage, eradicating the primary septic source, and high-dose intravenous antibiotics. 10 Initial broad-spectrum antibiotics cover aerobic and anaerobic bacteria, sometimes sufficing alone. CT-guided aspiration aids in management, reducing risks.3,7 Some authors suggested a non-surgical strategy for stable patients with minor midline deviation.3,4,8,10,24 Antibiotic cessation criteria include normalized inflammatory markers and MRI resolution. 6 Surgery relieves compression, evacuates pus and identifies pathogens, often via craniotomy or burr holes. Early surgery within 72 hours reduces disability risk to 10%, compared to 70% with delayed surgery.4,10,14,24 Addressing extracranial infection sources is vital; for dental-related sources, comprehensive treatment and infectious foci eradication are essential to mitigate the risk of hematogenous infection.10,14,25
Conclusion
Intracranial abscesses of odontogenic origin pose life-threatening risks but are largely preventable. Advancements in diagnosis and treatment have lowered mortality and morbidity rates. Dental pathology precedes neurological symptoms in 40% of cases, with caries and periodontitis being common factors. Vigilant clinicians should consider such complications in patients with fever, headache, and neurological deficits. A multidisciplinary approach involving otolaryngologists, neurosurgeons, microbiologists, and oral surgeons is crucial. Early diagnosis, neuroimaging, surgical intervention, antimicrobial therapy, and elimination of dental sources are key. Maintaining good oral hygiene through regular dental care helps prevent complications and intracranial spread.
Footnotes
Acknowledgements
The authors thank Pr Samir Boukattaya for the proofreading of this article.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration Of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
I.A. was responsible for case identification and management, data collection, literature review, manuscript preparation, revision and editing. N.D. was responsible for revision and editing, supervision and oversight, approval and finalization. H.Z. was responsible for case identification and management, data collection, literature review. M.B.K. was responsible for supervision and oversight, approval and finalization. All authors read and approved the final manuscript.
Author Note
This paper represents rare occurrences with significant clinical implications. It provides valuable insights into the potential risks and complications associated with dental infections. It adds to the existing literature, provides educational value, offers insights into clinical management, and highlights preventive measures.
Informed Consent
A written informed consent for patient information and images to be published was provided by the patient(s).
