Abstract
The objective of this study was to evaluate the outcomes of the nasolabial flap in the management of oral submucous fibrosis (OSMF). The descriptive case series included 75 patients diagnosed with OSMF who underwent surgical intervention under general anesthesia. Preoperative mouth opening measurements were compared with postoperative measurements taken after 2 months. Regarding mouth opening, out of the 75 patients, 4 (5.3%) had unsatisfactory results after treatment, while 22 (29.3%) experienced satisfactory outcomes. The majority of patients, 49 (65.3%), achieved normal mouth opening (more than 30 mm) following the Nasolabial flap procedure. This indicates that the Nasolabial flap yielded favorable results in terms of restoring normal mouth opening and benefiting the patients. Based on the findings of this study, the Nasolabial flap was determined to be a viable surgical option for managing oral submucous fibrosis due to its ease of operation, reliable flap vascularity, and low post-operative complication rate. The only drawback identified was the presence of a surgical scar, which can be addressed through secondary correction procedures.
Introduction
Oral submucous fibrosis (OSF) is a potentially malignant, chronic, and debilitating disease with a multifactorial etiology that affects the oral cavity, occasionally the pharynx, and rarely the larynx. It is characterized by oral mucosal blanching, rigidity, and intolerance to hot and spicy foods, leading to a progressive inability to open the mouth due to the development of vertical fibrous bands and loss of elasticity in the labial/buccal tissues. 1 OSF has a malignant transformation rate of 7% to 30% to oral squamous cell carcinoma (OSCC), with long-term follow-up studies reporting conversion rates of 7.6% over 17 years.2,3 The prevalence of OSF has significantly increased in South Asian countries, posing a significant public health problem, and there is an emerging trend of OSF cases in other nations due to population migration.1,4-6
The pathogenesis of OSF is multifactorial, with the betel nut component of areca nut, particularly the alkaloid arecoline, playing a significant role in collagen production and the development of oral submucosal fibrosis. 7 Genetic predisposition, immunological dysregulation, nutritional deficiencies, and autoimmune factors have also been implicated in OSF.8,9 Recent investigations have further elucidated various aspects of OSF, including molecular changes associated with differential gene expression and epigenetic modifications, providing prospective biomarkers and therapeutic targets. 10 Non-invasive diagnostic methods such as tissue auto fluorescence and salivary biomarkers have shown promise in early OSF detection and monitoring. 11
Management of OSF includes traditional therapies like steroids and antioxidants, as well as novel modalities such as pentoxifylline and collagenase, which have demonstrated efficacy in reducing fibrosis and improving symptoms. 7 Surgical techniques like tongue flaps and free tissue transfer have gained interest in the treatment of advanced OSF cases.4,12 Rehabilitation programs involving speech therapy, physiotherapy, and psychosocial support are essential for enhancing the quality of life for OSF patients. 13
Furthermore, when comparing the outcomes of different treatment modalities, the nasolabial flap has shown favorable results in restoring normal mouth opening and addressing functional limitations associated with OSF. Studies have reported satisfactory outcomes with the nasolabial flap, with a majority of patients achieving normal mouth opening postoperatively.4,12 Compared to other surgical techniques such as tongue flaps or free tissue transfer, the nasolabial flap offers advantages in terms of simplicity, reliable vascularity, and lower postoperative complication rates. 4
The nasolabial flap has been found to be a versatile and well-established option for reconstructing moderate facial deformities, including intraoral defects caused by OSF.14,15,16 However, it is important to consider individual patient characteristics and the extent of OSF involvement when determining the most appropriate treatment approach. Within the realm of surgical treatment, the nasolabial flap has been used for repairing intraoral deformities and has a well-established history dating back centuries. 14 The flap’s strong vascular supply contributes to its high rate of survival and versatility in reconstructing moderate facial deformities.15,16,17 The nasolabial flap can be based superiorly or inferiorly depending on the vascularity required and is suitable for reconstructing defects in the cheek, nose, lips, and intraoral region.18-20 The current case study aimed to evaluate the outcomes of the nasolabial flap in the surgical treatment of oral submucous fibrosis.
Methods
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
Surgical methods
An inferiorly based nasolabial flap was preferred for oral cavity repair. In its superior two-thirds, the medial incision line was closely aligned with the nasofacial fold and was 3 to 4 mm medial to the lower third of the nasolabial fold. This was done to reduce distortion after flap transfer, and improve the arc of rotation. The flap’s base measured 1.5 to 2.5 cm in breadth (Figure 1). A flap with a wider base is more difficult to rotate into place, while a flap with a narrower base has a lower blood supply and can only deliver a small amount of tissue. Approximately 0.5 to 0.75 cm anterior to the medial canthus, the medial and lateral poles of the incision taper upward. The lower edge of the flap was at the level of the oral commissure. Uni-stage nasolabial flaps were used to fill lateral defects of the oral cavity (lateral third of palate, socket, floor of mouth, and retromolar triangle). A no. 15 scalpel blade was used to deepithelialize the flap’s inferior 2 to 2.5 cm (Figure 2). For palatal and retromolar trigone defects, a transbuccal tunnel was created posterior to the upper buccal sulcus using Metzenbaum scissors. Similarly a transbuccal tunnel was created posterior to the lower buccal sulcus to simultaneously close the defect of the lateral of the floor of the mouth and the socket. 14 For the lesion in the central third of the oral cavity (middle palate, floor of the mouth, upper and lower alveoli) or the anterior tongue, a 2-stage nasolabial flap was used. Using dissecting scissors, the flap was lifted from superior to inferior in a supramuscular plane. In the superior part of the dissection, the angular branch of the facial artery is frequently cut off. The tunnel was large enough to comfortably fit 1 to 2 fingers (1.5-2.0 cm). The flap was then moved intra-orally without tension and inserted with a series of interrupted 3-0 absorbable sutures. 14
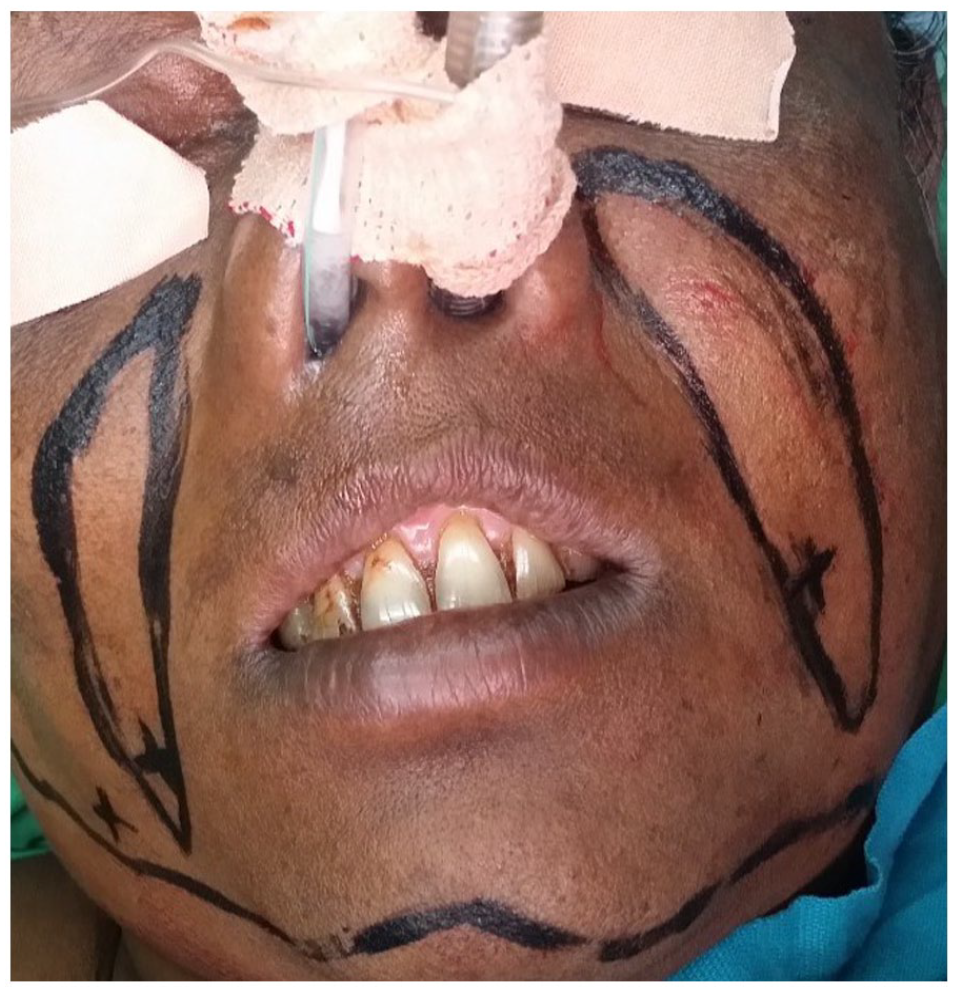
Initial presurgical planning, placing the inferior one-third to one-half of the nasolabial portion of the incision medial to the fold will allow for an improved arc of rotation and esthetic result. The base of the flap is 2 cm wide in this patient.

Nasolabial flap raised in a supramuscular plane of dissection and the inferior 2 cm de-epithelialized in preparation for single-stage transfer.
As with a “skin-lift” rhytidectomy, the donor site was extensively undermined in the subcutaneous plane. After that, the donor defect was closed in layers (Figure 3). Once the incision had healed, the skin along the nasal face of the incision was invert to leave a shallow scar. On the other hand, a slightly deeper scar along the nasolabial folds (with minimal eversion at the moment of closure) gave a more natural look. The flap was divided and inset 3 weeks following the initial treatment. During this time, the majority of patients were able to handle a soft diet. It was crucial to eliminate the whole trans buccal part of the flap during flap division, rather than simply dividing the buccal flap and flush with the cheek tissue. Otherwise, this mostly resulted in visible long-term filling at the level of the transverse commissure. 14
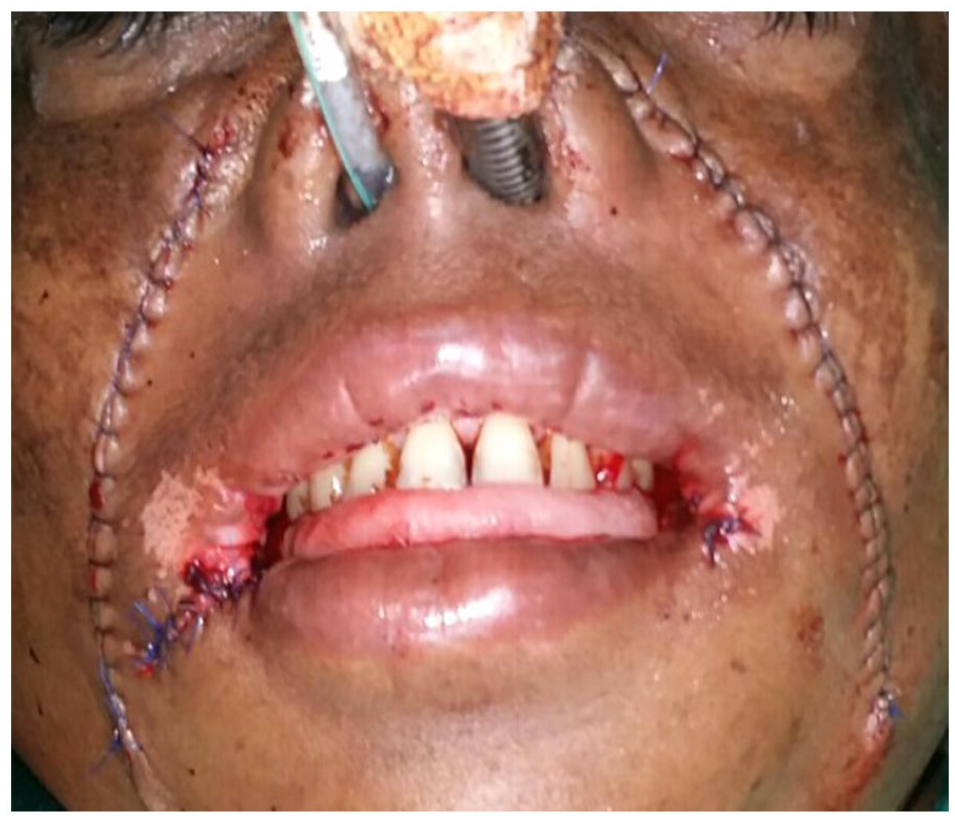
View of the post-surgical layered flap closure.
On a case-by-case basis, follow-up appointments were made in the Outpatient Department. On the second month postoperatively, the mouth opening was measured and reported based on the findings. A Vernier caliper was used to measure the mouth opening. It was measured in millimeters. All of the observations were recorded on a Performa that had already been prepared. The pre and post treatment mouth opening improvement in patients treated with a nasolabial flap is shown in (Figures 4 and 5).

Pre surgical mouth opening status of patient.

Post surgery improved mouth opening status of patient.
The number of participants and outcome of nasolabial flap treatment
The average patient age in this study was 43.32 ± 1.69 years. Male and female patients were 50 (66.7%) and 25 (33.3%), respectively. Out of 75 patients, 04 (5.3%) of the patients found unsatisfactory mouth opening because of the nasolabial flap treatment whereas 22 (29.3%) patients found adequate results. Majority of the patients—49 (65.3%) had a normal mouth opening with nasolabial flap treatment (Table 1).
Distribution of nasolabial flap outcome from patients (n = 75).

Discussion
Progressive difficulty in mouth opening, oral ulceration, intolerance to spicy food (burning sensation), altered salivation, depapillation (paleness of oral mucosa), altered mobility of the tongue, blanching, rigidity, and stiffening of the oral mucosa are prominent clinical signs and symptoms utilized for the diagnosis of oral submucous fibrosis (OSF). 9 A distinguishing feature of the condition is the formation of a prominent vertical fibrous ridge in the cheeks, along with rigidity of the buccal mucosa, akin to the texture of a board. 4 Trismus, difficulties in eating, and swallowing are all common manifestations of the soft tissue fibrosis observed in our patients. 10 It is important to note that OSF does not spontaneously resolve or improve upon discontinuation of areca nut chewing. Instead, the disease typically remains stable or progresses, affecting additional areas of the oral mucosa and ultimately leading to the development of oral cancer. 21
Medical therapy is recommended early in the disease, but for individuals with moderate to severe OSF, surgical intervention becomes necessary at the late and irreversible stage. 22 Various surgical techniques, including post-incision defect reconstruction and fibrous band release, are employed, such as the use of skin grafts, insular mucoperiosteal flaps, bilateral tongue flaps, superficial temporal fascial flaps with split skin grafts, radial forearm flaps, and flaps from the anterolateral side. 23 The nasolabial flap, among other options like buccal fat pad transplantation, offers a long-term, relapse-free, and cost-effective therapeutic approach for repairing mucosal lesions in inferiorly based reconstruction of the oral cavity. 24
The nasolabial flap is a vascularized regional lobe in the head and neck area, with its blood supply derived from either the facial artery (for inferior base) or the superficial temporal artery through the transverse facial and infraorbital arteries (for superiorly based flaps).23,24 Superiorly based flaps are suitable for reconstructing nasal, lower eyelid, and cheek abnormalities, while inferiorly based flaps are ideal for repairing lip, oral commissure, and anterior oral cavity defects.18-20,25 During the procedure, an incision line closely following the nasofacial fold was made using a Bard Parker blade #15. 24 The width of the flap base, similar to the study by Qayyum et al was approximately 1.5 to 2.5 cm to ensure an adequate blood supply. 20 Narrower based flaps may compromise blood flow, while wider based flaps can be challenging to rotate into position. 1 To facilitate transfer, a transbuccal tunnel, with a size of 1.5 to 2 cm to accommodate 1 or 2 fingers comfortably, was created at the posterior biting margin, allowing tension-free movement into the oral cavity. This technique, as described by Rahpeyma and Khajehahmadi is referred to as tunnelized nasolabial flaps. 25 Closure of the surgical site was achieved using 3-0 absorbable sutures. Care was taken to avoid including hair-bearing skin intraorally, ensuring the creation of a flexible and non-edematous flap due to the nature of the skin. The nasolabial flap offers a long-term, relapse-free, and cost-effective treatment option for oral submucous fibrosis. After fibrous band release, inferiorly based nasolabial flaps are utilized for repairing mucosal lesions. The proximity of the defect and the ease of closing the donor site are additional advantages of using the nasolabial flap, with the resulting extraoral scars being concealed within the nasolabial fold.18,19
Comparative studies by Pandey et al and Patil et al have shown that the nasolabial flap, with its good patient acceptance, rapid epithelialization, and minimal morbidity at the donor site, yields favorable results similar to buccal fat pad transplantation in terms of intra- and postoperative complications.12,24 Alternative reconstruction methods such as split thickness skin grafts, palatal island flaps, and tongue flaps are associated with significant postoperative complications, including raphe development, fibrosis, and postoperative dysphagia or aspiration risk. 24
The average age of patients in our case series was 43 years, with a minimum age cutoff of 30 years. Eckardt et al also reported a similar frequency and percentage of patients aged 67 years, ranging from 49 to 85 years. 23 Mehta et al conducted a study with 2 age groups, 1 overlapping with our study and the other ranging from 21 to 40 years, demonstrating positive outcomes in both groups. 17 Regarding gender distribution, male patients constituted 68% of our patient population, while female patients accounted for 32%.26,27 Out of the 75 patients included in our study, 5.3% experienced poor mouth opening outcomes after nasolabial flap therapy, while 29.3% had satisfactory results. In a study by Kamath et al, 10% of participants reported unsatisfactory outcomes. 1 Interincisal openings ranged from 30 to 40 mm in 90% of our cases. Qayyum et al reported an average postoperative mouth opening ranging from 29 to 39 mm, with a mean of 32.9 mm within 6 months of surgery. 20
Complications associated with the nasolabial flap procedure include the trapdoor effect, which manifests as an elevated bulging deformity of tissue within the semicircular confines of a U, C-, or V-shaped scar.20,22,25 Other potential complications include postoperative intraoral hair growth, loss of the nasomaxillary crease, and the development of a surgical scar. To address these complications, the nasomaxillary crease can be recreated using a periosteal suture, and the bulkiness of the flap can be minimized by meticulously removing all excess fat, resulting in a well-camouflaged scar.
In critically analyzing the outcomes of our case series, it is important to consider certain limitations in addition, potential areas for improvement. Firstly, due to the inherent nature of a case series design, the absence of a control group limits our ability to directly compare the effectiveness of the nasolabial flap with other treatment options. Future studies incorporating comparative analyses or randomized controlled trials would provide more robust evidence for the efficacy of the nasolabial flap in OSF management. Additionally, although our study reported satisfactory results in terms of mouth opening improvement, long-term follow-up data and assessments of functional outcomes beyond mouth opening would be valuable to comprehensively evaluate the overall impact of the nasolabial flap on patients’ quality of life. Furthermore, the presence of complications such as the trapdoor effect, postoperative hair growth, and development of surgical scars underscores the need for careful consideration of patient selection, flap design, and surgical techniques to minimize adverse effects. Collaborative efforts and multi-center studies involving larger sample sizes would enhance the generalizability of our findings and provide a more comprehensive understanding of the role of the nasolabial flap in the surgical management of OSF.
Conclusion
In conclusion, our case series on the use of the nasolabial flap in the surgical management of oral submucous fibrosis (OSF) demonstrates its potential as a valuable treatment option. Our findings showed that the nasolabial flap could successfully enhance mouth opening and reduce OSF symptoms. The treatment has benefits including low postoperative complication rates, reliable vascularity, and simplicity. To reduce potential risks, however, cautious patient selection and surgical methods must be used. While our study adds to the body of knowledge on the management of the nasolabial flap in OSF, more research that includes comparative analyses and long-term follow-up assessments is necessary to strengthen the body of knowledge. Overall, the nasolabial flap shows promise as a surgical approach for addressing the functional limitations and improving the quality of life of patients with OSF.
Footnotes
Acknowledgements
None.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author’s Note
Zafar Ali Khan is also affiliated to Departemnt of Oral and Maxillofacial Surgery, Frontier Medical and Dental College Abbottabad, Pakistan.
Author contributions
Conceptualization, H.U., A.M., S.F. and Z.A.K.; methodology, H.U., K.K.G. and Z.A.K.; software, K.K.G. and O.B.; validation, H.U., Z.A.K., N.A. and A.H.; formal analysis, A.M. and Z.A.K.; investigation, H.U., A.M. and S.F.; resources, Z.A.K., K.K.G. and O.B.; data curation, H.U., A.H., A.M., N.A. and Z.A.K.; writing—original draft preparation, H.U., A.M., S.F., K.K.G., and O.B.; writing—review and editing, A.H., N.A. and Z.A.K.; visualization, Z.A.K., A.M., N.A. and A.H.; supervision, A.M. and Z.A.K.; project administration, Z.A.K. All authors have read and agreed to the published version of the manuscript.
