Abstract
Maintaining a patent airway is critical for treating patients with severe inhalation injuries. Percutaneous Dilatational Tracheostomy (PDT) has been used effectively for many patients treated in the Intensive Care Unit (ICU). In addition to its safety for use at the bedside, according to Friedman et al. PDT has the same or even lower complication rate than surgical tracheostomy. PDT can be performed in a shorter time and is more cost-effective. Herein, we report a 44 year old obese woman who sustained an inhalation injury related to a burn. The patient fell headfirst into a pot of boiling water at the time of the burn. The patient showed signs of inhalation injury and suffered a second-to-third degree burn injury. She was treated in the ICU, and early PDT was performed. The procedure was performed by first locating the trachea, followed by a 1-cm incision made between the second and third tracheal ring. She was intubated successfully and treated in the ICU for 7 days. The anesthesiologist chose to perform an early PDT to prevent further complications. This procedure was done successfully despite many comorbidities from the patient, such as being an obese female and having a short neck, which makes finding the exact location for the incision challenging. In this case, the early decision to proceed with PDT showed promising results in decreasing the patient's mortality risk.
Introduction
Maintaining a patent airway is critical for treating patients with severe inhalation injuries, but there has been much debate on achieving this goal. Percutaneous Dilatational Tracheostomy (PDT) has been effective for many Intensive Care Unit (ICU) patients. In addition to being safe to operate at the bedside, percutaneous tracheostomy has the same or even lower complication rate compared to traditional open tracheostomy, PDT can be performed quicker and more cost-effective.1 -3 According to previous studies, 4 performing early tracheotomies within 2 days after hospital admission may decrease mortality, pneumonia cases, and ICU stays compared to those done 14 to 16 days following endotracheal intubation. 4
Patient Information
This case report presents a 44 year old obese woman who sustained inhalation injury due to a burn. The patient showed signs of inhalation injury and suffered from a second-to-third degree burn injury on 32% of total body surface area. Previous disease history was unknown.
Clinical Findings
The patient, as seen in Figure 1, was referred from the previous hospital with a burn injury on the mucous membranes of the lips, mouth, and eyes full of edema. The patient was intubated with endotracheal tube (ETT) no 6.5, with a depth of placement 22 cm from the central incisors, and was fixed with thread on the right lip corner. The patient had spontaneous, symmetrical breathing, with a respiratory rate of 20×/minute, SpO2 of 100% with T-piece 10 lpm. Blood pressure 128/79 mmHg, heart rate 98x/minute, warm extremities, capillary refill time <2 seconds with no spontaneous bleeding (Figure 2).
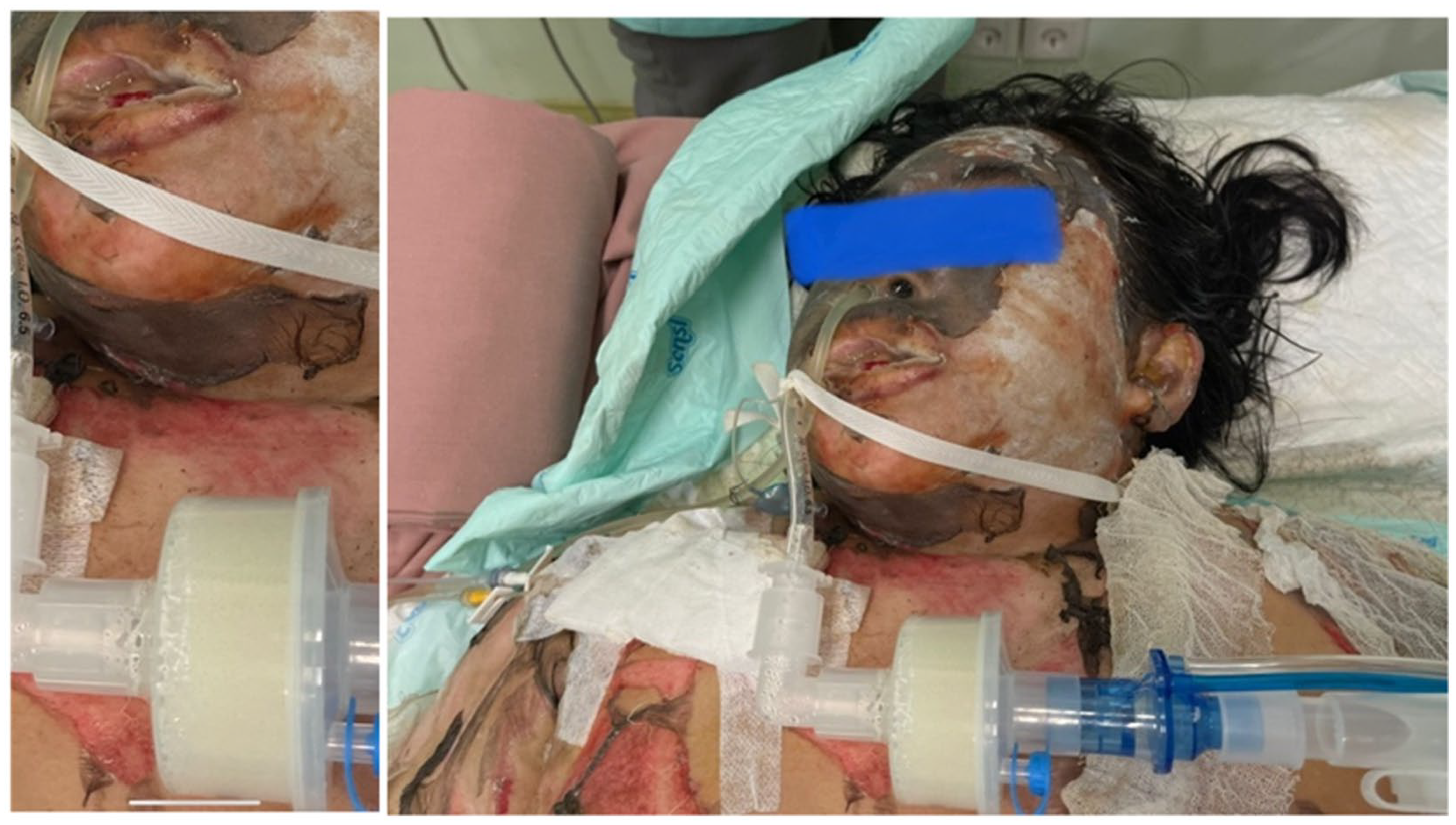
Patient’s condition when first admitted.
Timeline

Case timeline.
Diagnostic Assessment
Physical examination showed head and neck edema along with the burn injury. Burn status: head neck 5%, anterior trunk 5%, right arm 9%, left arm 6%, left leg 3%, and back 4%. Upon nasogastric tube (NGT) insertion, brownish fluid was obtained. During laboratory testing, it was found that there was a high value of leucocytes 28 880 103/µl. There was also a rise in the blood glucose value to 242 mg/dL and a low albumin value of 2.5 gr/dL. After being taken in for culture, the sputum obtained from the tracheal secretions revealed Acinetobacter baumanii bacteria, which then treated with tigecycline. The patient was diagnosed with grade II-III burn injury comprising of 32% total body surface area with stress ulcer and leucocytosis.
Therapeutic Intervention
The patient was treated in the ICU, and an early tracheostomy was performed. Percutaneous dilatational tracheostomy was done by first locating the trachea by using a 10cc syringe. When the syringe showed signs of air bubble and no bleeding occurred the anaesthesiologist proceed to make a 1-cm incision between the second and third tracheal ring. A ventilator was set to PSV/CPAP PS 10 Peep 5 trig 3 FiO2 50%. She was intubated successfully and treated in the ICU from 23rd February to 2nd March 2022. The patient underwent percutaneous dilatational tracheostomy to facilitate the passage of a large amount of sputum, avoiding ETT obstruction. Tangential excision and debridement were also done to treat the burn injury after the PDT was done. PDT was performed prior to debridement to maintain the patient’s airway and provide easier access for debridement because the patient’s mouth area was heavily plastered while the patient was still using an ETT. The patient received a 25% plasbumin transfusion of 100 ml for 2 days during treatment (Figure 3).

Patient's condition after PDT was done.
Follow-up and Outcomes
The results of performing early tracheostomy using the percutaneous dilatational tracheostomy method showed a promising result. In this case, PDT was done to secure the airway and avoid ETT obstruction due to sputum hypersecretion after inhalation injury. The length of ventilator day in this patient was 5 days. The patient was discharged safely from the ICU after 7 days of treatment. Patient was then moved to a normal ward still canulated but was able to breathe spontaneously. The reason to keep the PDT after being discharged from the ICU was to have better management of patient’s secretions and to avoid aspiration. After 2 weeks in a normal ward, patient was then discharged and was referred back to the first hospital for further follow-up. The patient can’t return to our hospital because of the distance and constrained in costs. There is also no follow up for Pseudomonas infection at the PDT site.
Discussion
Among burn cases, inhalation injury is a serious injury that significantly raises death and morbidity rates. Confirmed inhalation injuries may result in a 30% to 40% increase in death. The damage typically causes tracheobronchitis, secondary lung colonization, and late sepsis, in addition to edema of the periglottic tissues. Estimating the severity of inhalation injury and its precise significance in the etiology of pulmonary complications has been proven to be challenging.5,6 A clinician initially considers the patient's history and the stated mechanism when assessing a patient who has a suspected inhalation injury to assess the possibility of an inhalation injury. Facial burns, singed facial or nasal hair, soot or carbonaceous material on the face or in the sputum, and indications of airway blockage such as stridor, edema, or mucosal injury are important physical exam findings. 7 In this case report, we diagnose the patient with inhalation injury due to the presence of a burn injury on the mucous membranes of the lips, mouth, and eyes full of edema.
The confirmation of inhalation injury can be done using a variety of techniques, such as fiberoptic bronchoscopy (FOB), chest computed tomography (CT), carboxyhemoglobin measurement, radionuclide imaging using Xenon, and pulmonary function testing. 7 Unfortunately, these further testing couldn’t be done on the patient due to cost constraints.
Burns to the airway structures may result in severe swelling of the tongue, epiglottis, and aryepiglottic folds, which may then restrict breathing. The production of edema is brought on by the reactive oxygen species increasing the endothelium's permeability to proteins. Within a few hours, fluid resuscitation and airway edema will develop simultaneously which will cause the upper airway to become anatomically distorted or externally compressed that eventually will affect the airway care. The severity of obstruction that may subsequently develop cannot likely be predicted from the initial field airway assessment. Hence, in this case PDT is done early to prevent further complications. 8
Tracheostomy is one of the primary treatments for patients with inhalation injury since it avoids many complications which may occur to the patients. The complications include upper airway obstruction, the need for prolonged mechanical ventilation, inability to handle secretions, respiratory tract irritation, respiratory obstruction in patients with deep facial burns, vomit aspiration, and injuries. The procedures can be conducted through 2 methods, that is, (1) the conventional tracheostomy, where the procedure is done in the operating room, and (2) percutaneous dilatational tracheostomy or PDT, where the procedure is done bedside in the ICU.1,2
The role of conventional tracheostomy in burn management brings out many controversies. It is said that conventional tracheostomy is most likely to cause a pulmonary infection, among many other procedure complications. Percutaneous tracheostomy has become a standard procedure in ICU patients since Ciaglia et al 1 first described their technique in 1985. PDT is now more recommended because it causes less infection with smaller incisions, resulting in faster spontaneous closure of the stoma after removing the tube. 2 According to American Academy of Otolaryngology, although the overall PDT complication rate is low, serious adverse events, including death, have been reported. PDT-related death occurs in 1 out of every 600 patients who undergo PDT where 31% of these deaths occur due to hemorrhage connected to PDT. Another study stated, most of the serious bleeding incidents were related to unrecognized and unanticipated anatomical variations in the vascular anatomy. Critical care physicians are recommended to consider using other tools that could provide a better understanding of the anatomy of the neck to guide PDT procedures and improve their safety. The use of ultrasound before, during, and after PDT could play a role in landmarking, identifying vulnerable structures, choosing the appropriate tracheostomy size, and providing real-time guidance for needle penetration. 9 Despite the recommendation, there will still be conditions where ultrasound is not easily accessible hence we provide a case report of performing PDT without USG guidance.
Many studies have compared the mortality rate between performing early tracheostomy and tracheostomy according to the established recommendation, which is 2 to 3 weeks after endotracheal intubation. 4 A further comprehensive evaluation of research and meta-analysis revealed that early tracheostomy shortened the mechanical ventilation period and hospital stays. A significant decline in-hospital mortality was also noted in the most extensive trials under consideration. 10
In our case, the anesthesiologist chose to do an early PDT within 18 hr after the incident to prevent further complications. This procedure was done successfully despite complicating factors of the patients, such as obesity and short neck, which may cause difficulty in finding the exact surgical incision site. 3
After undergoing the PDT procedure, the patient demonstrated good outcome and a low mortality risk. The patient was treated on a ventilator for 5 days and showed no pulmonary infections. The incision site was observed to heal well. After 7 days in the ICU, the patient was moved to the medical ward before being discharged from the hospital.
Conclusion
It is important to prioritize securing the airway in patients with burn and inhalation injuries. Conventional ETT may not be the best option for this case because it is susceptible to clotting and obstruction due to excessive secretions. PDT was chosen over the traditional tracheostomy because it is less invasive, has a lower complication rate, and a faster recovery time. Early PDT was done to avoid the risk of further complications and obtain a better outcome. In this case, an early decision to proceed with the PDT procedure showed remarkable results.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Note
This article was presented at the 7th International Conference and Exhibition on Indonesian Medical Education and Research Institute (7th ICE on IMERI), Faculty of Medicine, Universitas Indonesia.
We appreciate the exceptional support of the 7th ICE on IMERI committee during the manuscript preparation and peer-review process.
Author Contributions
All authors contributed to the design of work, drafted he article, and approved the final version of the manuscript.
