Abstract
Orofacial granulomatosis is a condition that manifests clinically as painless labial enlargement, perioral and mucosal edema, oral ulcers, and gingivitis. It is characterized by non-necrotizing granulomatous inflammation of the oral and maxillofacial region. When the swelling only affects the lips, the pathology is called Miescher’s granulomatous cheilitis; however, when it also causes facial paresis and lingua plicata, it is known as Melkersson-Rosenthal syndrome. We report a case that was successfully treated with a combination of a local (intralesional) steroid, a systemic antibiotic, and a systemic steroid. After 6 months of therapy, we observed improvement in gingival hyperplasia and buccal mucosa and lip edema.
Keywords
Introduction
The term orofacial granulomatosis (OFG) describes a group of conditions characterized by typical features of noncaseating granuloma, lymphocytic infiltration, and edema at various sites in the oral cavity. 1 There are 2 clinical variants of the syndrome: Melkersson-Rosenthal syndrome, which is characterized by unilateral facial nerve paresis, lingua plicata, and chronic unilateral labiofacial edema; and granulomatous cheilitis, an inflammation that only affects the lip. 2 There is no sex predilection. The specific pathophysiology of the syndrome is still unknown, despite the involvement of numerous etiological agents such as genetic, immunological, allergic, and viral factors. According to the literature, the syndrome may be linked to sarcoidosis, tuberculosis, and Crohn’s disease.3,4 The clinical manifestations are variable. Lips are the most frequent site of painless, asymmetric edema, and one or both lips may be involved. The face, gingiva, buccal mucosa, tongue, and palatal mucosa can all be affected.5,6
Case Report
A 15-year-old male patient presented at the Oral Medicine Department of the University Clinical Center with swelling of the upper lip that had persisted for 3 years. The patient claimed that the edema of the lip recurred numerous times each year without causing any pain. There was no history of allergies or systemic disease. The patient’s allergic tests for nutritive and inhalational allergens proved negative, in consultation with an allergist.
The clinical examination revealed edema, redness, and fissuring of the upper lip (Figure 1), with unilateral edema and fissures on the buccal mucosa, and gingival hyperplasia in the upper jaw (Figures 2, 3a and b). On palpation, the lip was firm and painless. The gingiva was hyperplastic in both jaws, particularly in the area around the front teeth. Poor oral hygiene was observed. Laboratory investigations revealed that the complete blood count, urinalysis, biochemistry, liver and renal function tests, and thyroid hormones were normal. Consultation with a gastroenterologist ruled out Crohn’s disease, and consultation with a pulmonologist excluded tuberculosis and sarcoidosis (PPD test was negative). Following gastroenterological and lung examinations, the diagnosis of an isolated case of orofacial granulomatosis was confirmed. Chest radiography and a series of blood tests were requested to rule out Crohn’s disease, tuberculosis, and sarcoidosis. Our patient denied having any gastrointestinal (GI) symptoms but underwent endoscopy and colonoscopy to rule out possibility of CD. His PPD result was negative, however he was referred for a chest X-ray to exclude tuberculosis and sarcoidosis.

Photograph showing the upper lip at presentation.

Photograph showing maxillary gingival hyperplasia.

(a and b) Frontal and profile photographs showing the enlarged lips and lip fissures.
On oral panoramic X-rays (Figure 4), periapical alterations in teeth 21 and 22, deep caries in teeth 36, and radix relicta in teeth 46 were clearly discernible. Antibiotics (amoxiclav tablets, 625 mg twice daily) were administered as a premedication before extraction and endodontic treatments.
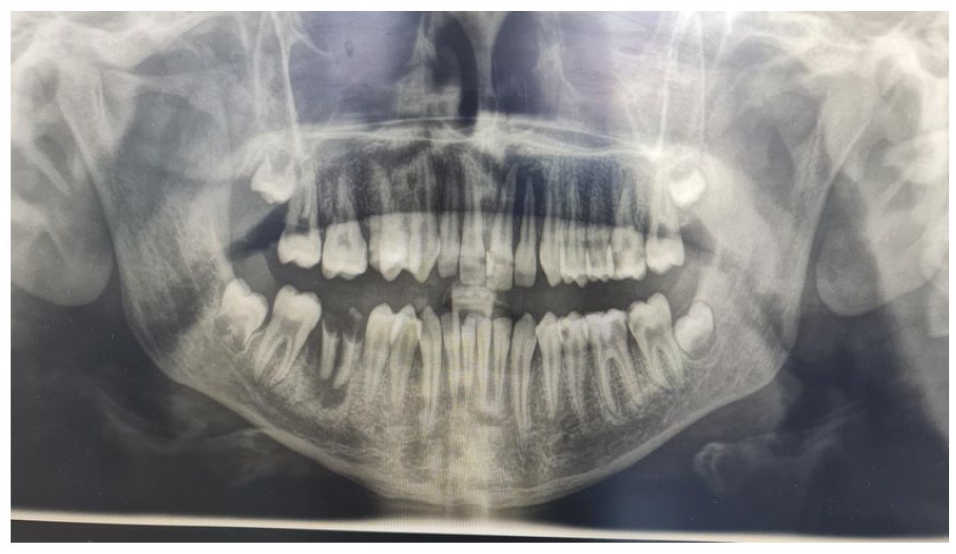
Oral panoramic radiograph.
In consultation with an oral surgeon, we used antibiotics for prophylaxis before tooth extraction and endodontic treatments due to dentoalveolar abscess teeth 36, 46, 21, 22. The antibiotic isn’t prescribed to treat OFG, but rather to treat odontogenic infection. Amoxiclav 625 mg twice daily for 1 week was prescribed as prophylaxis.
Endodontic treatment was performed on teeth 21 and 22, and teeth 36 and 46 were extracted to eliminate foci of dentogenic origin. We administered oral prednisone (5 mg twice daily for 10 days) because the edema of the lip and buccal mucosa, fissures, and gingival inflammation were persistent. We injected intralesional steroid injections (40 mg Triamcinolon acetonid) at a frequency of 1 ml per week for 3 weeks to the upper lip because the edema had not entirely subsided. This injection was administered under local anesthesia to avoid the pain associated with the increase of tissue pressure of the edematous lip. After the initial injection, we observed a reduction of the lip size. Six months later, clinical evaluation showed improvement of the lip edema, but with slight cheek swelling, mainly toward the left side, with an asymmetric facial appearance (Figure 5). At the 9-month follow-up, there were no signs of recurrence. No mucosal alterations were present (Figure 6a and b). Non -surgical treatment was started to treat the periodontal inflammation after 9-month of follow-up. The patient provided written informed consent.

Photograph of the lips after 6 months of treatment.

(a and b) Profile and frontal photographs showing the lips after 9 months of treatment.
Histopathology
A biopsy was performed from a gingival sample. The sample was stained with CK-MNF immunohistochemical stain, which marks epithelial components. Under the squamous epithelium without atypia, dense lymphoplasmacytic inflammatory infiltrate and some multinucleated giant cells could be seen. There was also a proliferation of lymphatic vascular vessels (Figure 7a and b).

Histopathologic view: (a) CK-MNF stain and (b) H&E stain.
Discussion
Although several hypotheses, such as infection, genetic predisposition, and allergy, have been proposed, the precise cause of orofacial granulomatosis is still unknown. 7 As in our case, no correlation was found between OFG and systemic conditions such Crohn’s disease or sarcoidosis in a study by Marcoval et al 8 There is no standard protocol for treating this disease; however, several researchers recommend using steroids as the first line of treatment, particularly during the acute stage. 9 If the underlying cause of OFG can be treated, not only will symptoms disappear more quickly, but steroid treatment can be used more sparingly and for a shorter period. Although corticosteroids are frequently used to treat OFG, adverse effects occur with long-term use. They have been demonstrated to be beneficial in reducing facial edema and preventing recurrence. 10 Dar et al used an intralesional combination of triamcinolone, metronidazole, and minocycline, and observed a significant improvement in lip swelling after 1 month of treatment. After applying an intralesional combination of triamcinolone, metronidazole, and minocycline for 1 month, Dar et al observed a substantial reduction in lip edema. 11 Similarly, Stein and Mancini successfully treated 2 children with a combination of oral prednisolone and minocycline. 12 Cheiloplasty is reserved for the most complicated cases with a major lip deformity or cases that are resistant to therapy. 13
Conclusion
Orofacial granulomatosis can be recurrent and may involve inflammation not only at the labial level, but also the gingival, lingual, buccal, or suborbital levels. Differential diagnosis is required to exclude infections, Crohn’s disease, sarcoidosis, and allergic reactions. Biopsy remains the most definitive way to diagnose the condition. 14 A reference treatment for orofacial granulomatosis has not been established because there is a lack of evidence in the literature. Due to the limitations of this case report, further research in the form of randomized case-control trials is needed to confirm the efficacy of our treatment choice; however, the triamcinolone acetonide injection procedure appears to be the most suitable in labial and buccal cases to prevent recurrence.
Footnotes
Acknowledgements
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
