Abstract
Vascular access is the Achilles tendon of hemodialysis and is considered the lifeline for patients with end stage renal disease. Arteriovenous fistulas and grafts are the preferred traditional access for performing dialysis therapy. However, some patients exhaust the traditional routes of dialysis vascular access for different reasons. In search for alternatives, other unusual vascular routes have been explored, such as transhepatic and translumbar approaches, as the last resort to preserve life in this unfortunate population. Here, we present the unusual case of a 66-year-old female who ran out of the traditional vascular access options and became catheter dependent via the right femoral vein. However, due to recurrent femoral catheter infections, extensive skin calciphylactic lesions and her body habitus, other routes were explored and the decision was to use the transhepatic approach. Traditionally, the right and middle hepatic veins are used to insert these catheters. However, the use of the left hepatic vein was not reported in the literature. Hence, in order to avoid the skin lesions seen in our patient, the dialysis catheter was inserted using the left hepatic vein. Overall, this case highlights the challenges of securing a reliable vascular access to perform dialysis therapy and brings attention to other vascular dialysis routes in certain clinical scenarios.
Keywords
Introduction
Long-term hemodialysis access is considered the lifeline for patients with end-stage renal disease and can often provide a challenge. In cases where more traditional routes of vascular access are exhausted, the transhepatic approach for dialysis catheter placement can be a feasible option. 1 However, despite the high procedural success rate, transhepatic dialysis catheters are associated with high risk of dislodgment and migration (37%), infection (21.7%), and thrombosis (17.4%).2,3
When using the transhepatic approach, the inferior vena cava and right atrium are usually accessed via either the right or middle hepatic veins. Accessing the left hepatic vein using the anterior abdominal approach is rarely reported. Here, we describe the unusual case of a dialysis woman who exhausted her vascular access options and became catheter dependent via the right femoral vein. 4 Due to recurrent femoral catheter infections, a transhepatic dialysis catheter was placed using the anterior approach in the left hepatic vein.
Case Description
A 66-year-old African American female was presented with end stage renal disease on hemodialysis with multiple comorbidities including diabetes mellitus, hypertension, peripheral artery disease with bilateral above the knee amputation, diabetic retinopathy leading to blindness, and morbid obesity (body mass index 46 kg/m2). The patient had poor vasculature and was catheter dependent. She had multiple failed fistulas and grafts in the upper extremities. For the last 18 months, she had been dialyzing via femoral dialysis catheter. Prior to her current presentation, she developed severe calciphylaxis with large skin involvement including the lower abdominal wall and under the breast areas. Due to her body habitus and extensive skin lesions, the patient developed recurrent femoral catheter-related infections necessitating frequent dialysis catheter exchanges. Thus, the decision was made to explore different sites for inserting the dialysis catheter in order to avoid the dialysis therapy interruption. However, the patient’s body habitus and her severe general debility precluded the trans-lumbar approach. Accordingly, the decision was to insert a transhepatic dialysis catheter. Due to the extensive skin calciphylaxis-related lesions under the breast areas, the only option was to use the substernal area to access the liver. An attempt to access the middle hepatic vein failed. Subsequently, the left hepatic vein was accessed using 15 cm 22-gauge spinal needle under ultrasound guidance and positioning was confirmed with contrast injection. Next, a 0.018 in guidewire was advanced into the inferior vena cava and right atrium without difficulty. Using a transitional sheath, the wire was then exchanged for a 145 cm stiff 0.035 in wire (Amplatz, Boston Scientific, Natick, MA) (Figure 1). After creating the subcutaneous tunnel in the usual fashion, dilating the tract and inserting the peel away sheath, a 31 cm 14.5F Glidepath catheter (Bard, Tempe, AZ) was inserted in the traditional fashion and all sites were closed (Figure 2). Injection of contrast confirmed the appropriate catheter tip positioning in the proximal right atrium (Figure 3). The catheter was used for dialysis for approximately 5 months without requiring any intervention (Figure 4). The patient was provided comfort care and died 18 months following the initial transhepatic catheter insertion. During this period, the catheter was changed 4 times due to dislodge and/or dysfunction.

Fluoroscopic image showing an Amplatz wire in the right atrium.

Contrast injection confirming the catheter position with the tip of the catheter is within proximal right atrium. The hepatic veins are also filled with contrast.

Post catheter placement image showing the final position of the catheter traversing the left hepatic vein.
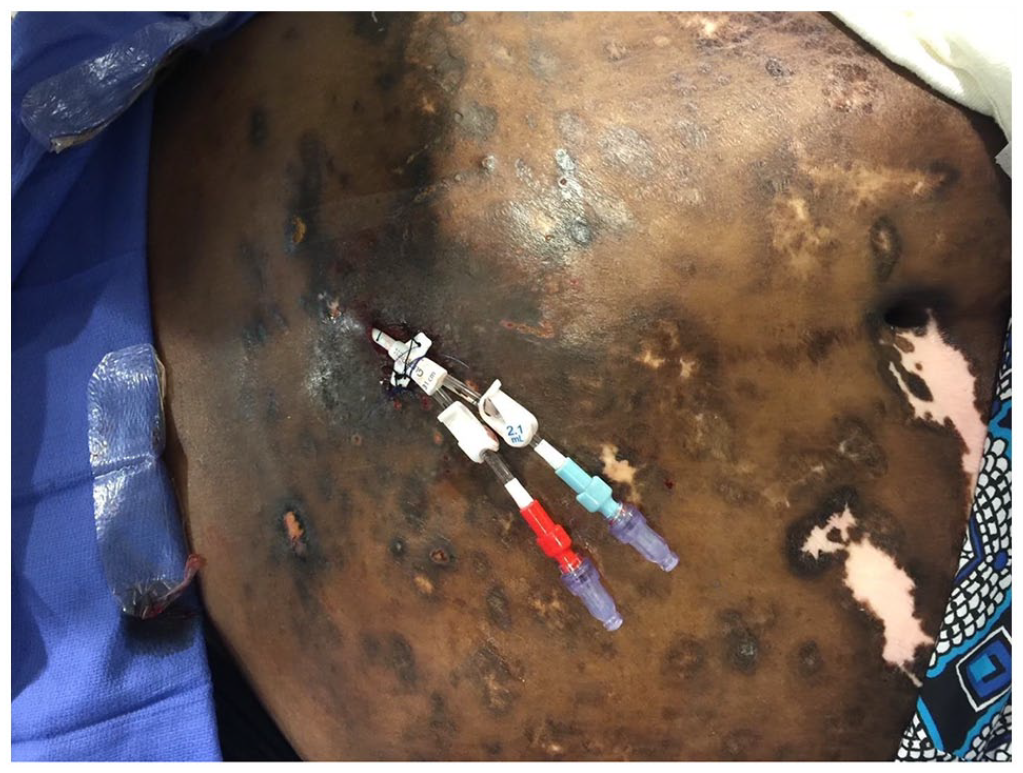
Severe calciphylactic lesions involving extensive areas of the skin; the transhepatic dialysis catheter is in place.
Discussion
The National Kidney Foundation guidelines recommend the utilization of the internal jugular (IJ) veins for dialysis catheter placement as the first choice as compared with other venous sites. 5 The advantage of using IJ site for dialysis catheters is related to preserving the sites in the upper and lower extremities for creating future grafts and fistulas.5,6
On the other hand, the subclavian site is associated with increased risk of venous stenosis or occlusion, which could compromise the creation of future dialysis access. 6 Dialysis femoral catheters are associated with increased risk of infection and stenosis of the affected veins. 7 Accordingly, among patients who have exhausted other venous access sites, percutaneous transhepatic venous access becomes a viable option to resume dialysis therapy.2-4 In the case presented, the patient exhausted all options for creating any vascular access in the upper extremities. Further, she had bilateral lower extremity amputation as a complication of long-term uncontrolled diabetes, which precluded her from creating a thigh graft. Notably, due to her body habitus, the dialysis femoral catheter was compromised by the recurrent infections and subsequent exchanges with frequent dialysis therapy interruptions. In order to overcome these challenges, the transhepatic route was utilized as the last reasonable option to resume dialysis. For transhepatic dialysis catheters, the right and middle hepatic veins are usually accessed using the lateral approach. However, due to the extensive skin lesions of calciphylaxis and inability to rotate the patient on the procedure table, the left hepatic vein was used to insert the dialysis catheter, an approach that was not reported previously in the literature. Therefore, one can speculate that choosing the left hepatic vein potentially is more advantageous than the right or middle veins as it may reduce the catheter dislodgment and migration. Finally, it is worth mentioning that trans-renal approach to insert the dialysis catheter has been reported in the literature with reasonable outcomes. 8
In conclusion, this case highlights the challenges encountered in the dialysis patients whom ran out of options to perform renal replacement therapy. Moreover, it draws the attention to utilizing the transhepatic route as a feasible alternative for dialysis access in certain clinical settings.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
All authors contributed equally to this article. All authors read and approved the final manuscript.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Written informed consent was obtained from the legal guardian of patient for publication of this case report and accompanying images.
