Abstract
Background:
Transcatheter aortic valve replacement (TAVR) is nowadays generally accepted as the treatment of choice for high- to intermediate-risk patients with severe aortic stenosis not suitable for the standard surgical replacement. Many vascular accesses have been described for the valve delivery, comprising the common iliac artery as the arterial site of access.
Methods:
From September 2008 to June 2014, 440 patients underwent TAVR at our institution. We report a series of 12 patients that have undergone TAVR via a trans-iliac (TI) retroperitoneal surgical approach and also discuss its feasibility, security, and medium-term follow-up.
Results:
The 30-day survival rate was 92%. Only 1 local vascular access major complication occurred requiring an iliac-femoral bypass grafting with a vascular graft. Two patients experienced transient neurological ischemic attack. At 3-year follow-up, all the 11 patients were alive and well and the echocardiographic evaluation revealed good function of the prosthesis.
Conclusions:
The TI route seems to be feasible with a low profile of local complications. It may be a reasonable access alternative to the femoral artery and to the trans-apical approach. A broader, prospective study is advisable to gain general consensus on this approach.
Keywords
Background
More than 75 000 aortic valve replacements are performed annually worldwide. 1 In the last two decades, a growing portion of these procedures have been performed with the technology of transcatheter aortic valve replacement (TAVR).
Procedures such as TAVR, endovascular aneurysm repair (EVAR), and thoracic endovascular aneurysm repair (TEVAR) normally require large-bore arterial access and typically use a trans-femoral (TF) route. 2
For the current available TAVR delivery catheters (14-20F), the minimal femoral and iliac diameter should be 5.5 to 6 mm; additionally, there should be limited vessel calcifications to reduce local damage and possible vascular complications.
In 20% to 30% of patients, the standard TF access is precluded due to small caliber or diffusely diseased vessels. 3 In few selected cases, the intra-abdominal iliac artery may be larger and easily approached by a small surgical incision over the groin to gain access to the retroperitoneal space. As for all the transcatheter procedures, the main risks may be local major or minor vascular complications. 4
Materials and Methods
We have retrospectively analyzed the TAVR institutional records from September 2008 to June 2014: we performed 440 Edwards Sapien S3 and Sapien XT implantations (Edwards Lifesciences, Irvine, CA, USA), 329 of these by a TF approach, 99 trans-apical (TA), and 12 trans-iliac (TI).
The aim of this article is to assess the feasibility, security, and medium-term follow-up of the TI approach for the transcatheter valve procedure.
In our series, the implanted prosthesis were Edwards Sapien S3 in 11 patients (#23 in 6 cases and #26 in the other 5 cases) deployed by Retroflex sheath and Edwards Sapien XT #23 in only 1 case, deployed by Novaflex sheath.
We focused our attention on the demographics, operative technique, morbidity, and mortality. We also considered at least the 3-year follow-up.
The series included 10 women (83.3%) and 2 men (16.7%) with a median age of 83.1 years (range 76-89). The characteristics of the population and the risks factors are listed in Table 1.
Baseline characteristics of the population.
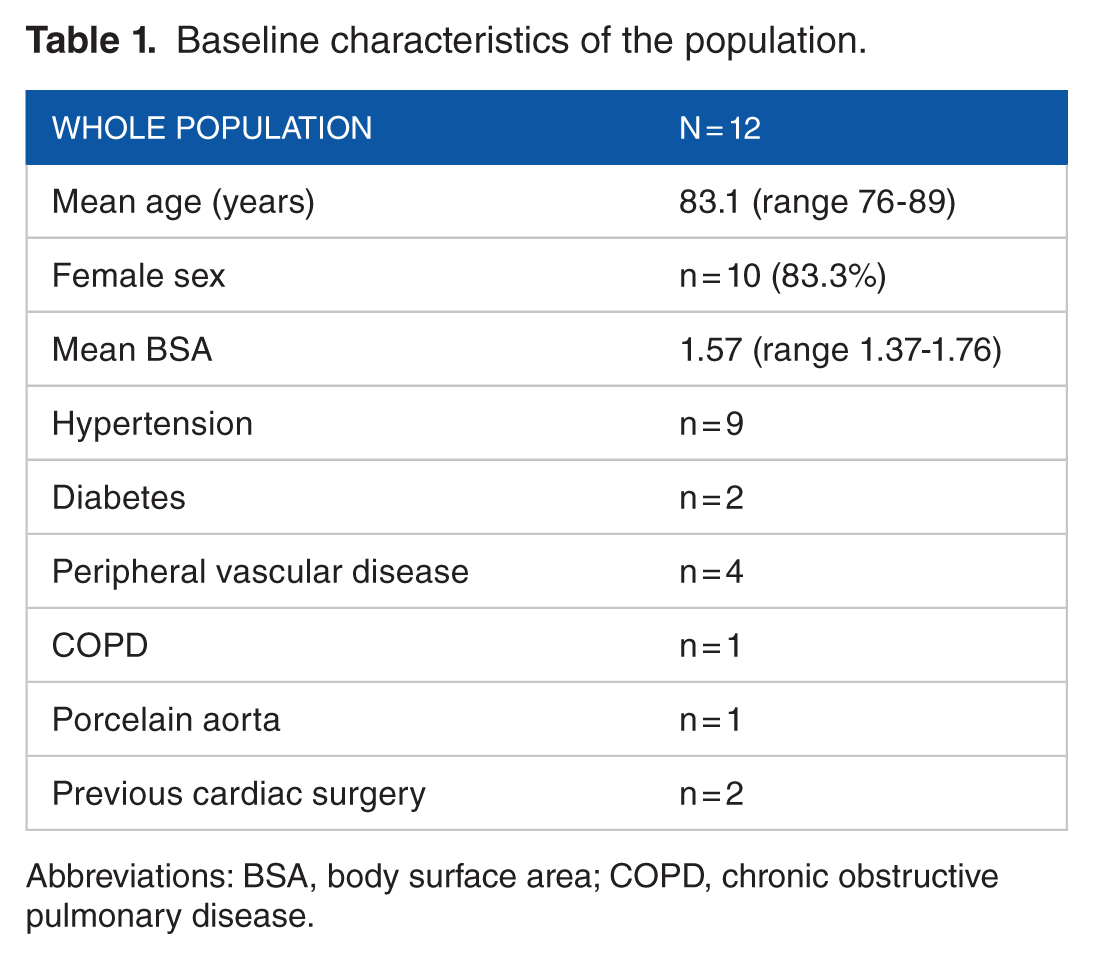
Abbreviations: BSA, body surface area; COPD, chronic obstructive pulmonary disease.
There were 1 case of porcelain aorta and 2 with previous cardiac surgery (coronary artery bypass grafting).
Preoperative assessment
All the patients received a computed tomography (CT) scan to detect the aortic annulus size, the coronary arteries’ height, and the course and diameter of the aorta until the femoral arteries.
For the artery, the minimum accepted lumen diameter at the groin (in the transverse axial images) was normally 7.0 mm for a #23 Sapien S3 valve (22F sheaths) and 8.0 mm for a #26 Sapien S3 valve (24F sheaths), whereas it was less (6.0 mm) for #23 Edwards Sapien XT (16F sheath).
The TA and other vascular routes were excluded because of a poor left ventricular function, severe obstructive pulmonary disease, or a small vascular diameter in the presence of severe atherosclerotic disease, calcifications, and tortuosity.
We chose to directly approach the iliac artery after checking the CT (Figure 1) in the following cases:
Less than 1-mm difference between maximal arterial diameter and procedural sheath;
A high degree of calcification (especially circumferential) at the level of the femoral arteries;
Low grade of iliac tortuosity;
Very high femoral bifurcation;
No previous abdominal surgeries.
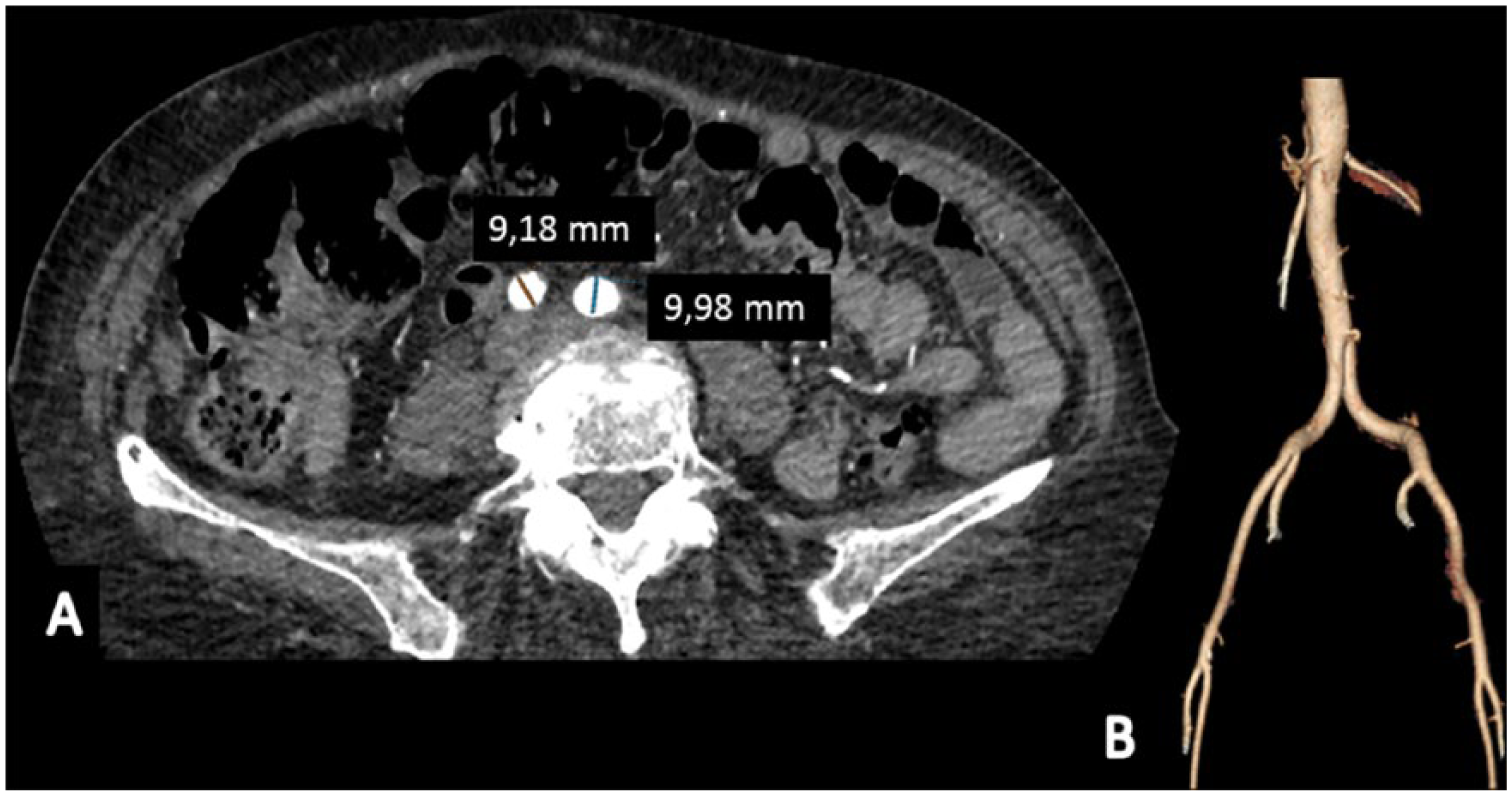
Preoperative computed tomography (CT). We chose to go for the trans-iliac route whenever the femoral arteries are too small, high, or calcified and there is moderate tortuosity of the iliac axes in the absence of circumferential calcifications. (A) Large iliac diameters allowing a safe procedure. (B) Three-dimensional reconstruction of a suitable retroperitoneal access (in this case the femoral arteries were too small compared with sheath diameter).
Surgical plan
A surgical retroperitoneal TI access was planned in these cases.
All patients received the operation under general anesthesia. The common iliac artery was exposed through an oblique incision 2 cm above the inguinal ligament. After surgical exposure of the vessel, it was manually examined to evaluate calcification. The purse-string sutures were made to fix the sheath to the artery during the procedure (Figure 2).
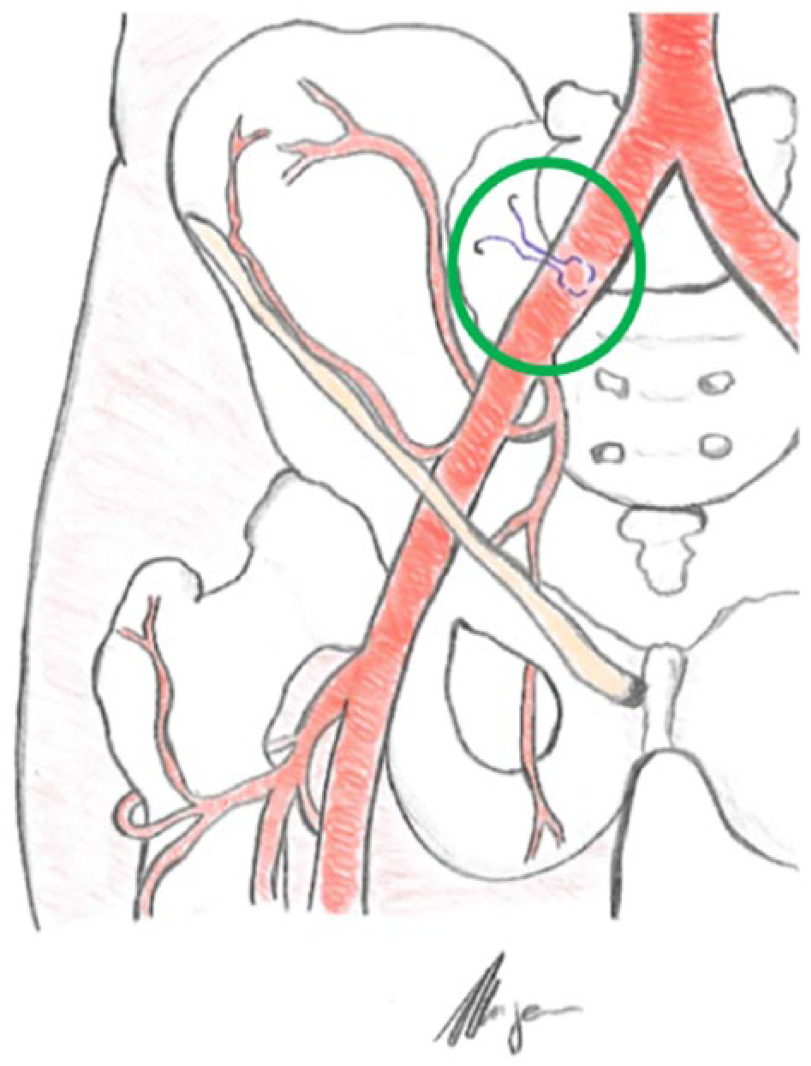
Schematic drawing showing the site of the purse-string stitch on the common iliac artery (green circle).
All wire, dilator, and sheath manipulations were done under fluoroscopy. Following systemic anticoagulation with intravenous heparin and elevation of the activating clotting time (ACT) to 200-250 seconds, the artery was punctured and a wire advanced into the descending thoracic aorta. The appropriate sheath was then inserted after the opportune predilatation (Figure 3).
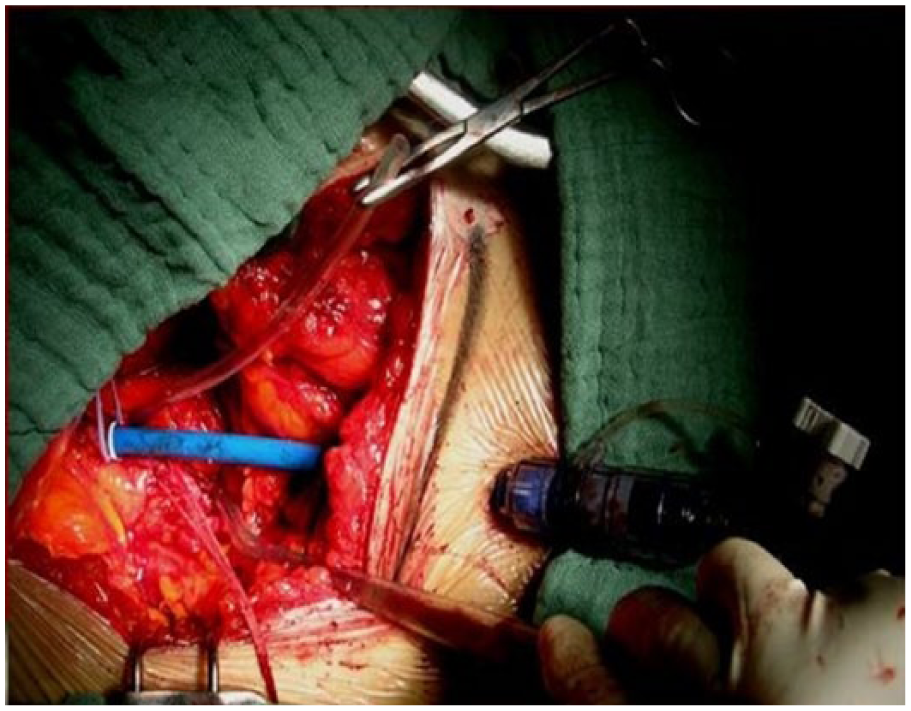
Intraoperative image showing the surgical retroperitoneal trans-iliac access with the implanted sheath for the valve delivery.
Following the delivery of the transcatheter prosthesis, the sheath was pulled down into the distal external iliac artery and an abdominal aortogram completed to exclude proximal arterial injury.
The sheath was then removed and the puncture site directly examined for localized access damage. The kind of artery repair was based on the amount of damage present and the judgment of the surgeon. When minimal damage was present, a primary transverse closure of the artery was undertaken with polypropylene suture. In situations where arterial damage was more extensive, the artery was opened longitudinally and the artery debrided and repaired with a prosthetic patch and polypropylene suture. When localized arterial damage was extensive, the artery was replaced with an appropriately sized Dacron graft. All repairs or replacements were undertaken through the initial skin incision. A surgical result was considered acceptable when there was the presence of a normal pulse distal to the site of repair or replacement, and there was no visible stenosis at the site of repair or replacement and no palpable thrill. 5
Normally, a small drainage tube is positioned and removed within 24 hours. The abdominal wall near the incision is also irrigated with local anesthetic to reduce postoperative pain.
Results
The whole population presented with a New York Heart Association (NYHA) dyspnea class III/IV and had a high mean logistic euroSCORE I (21.33). The echocardiographic characteristics of the population are summarized in Table 2.
Preoperative features.
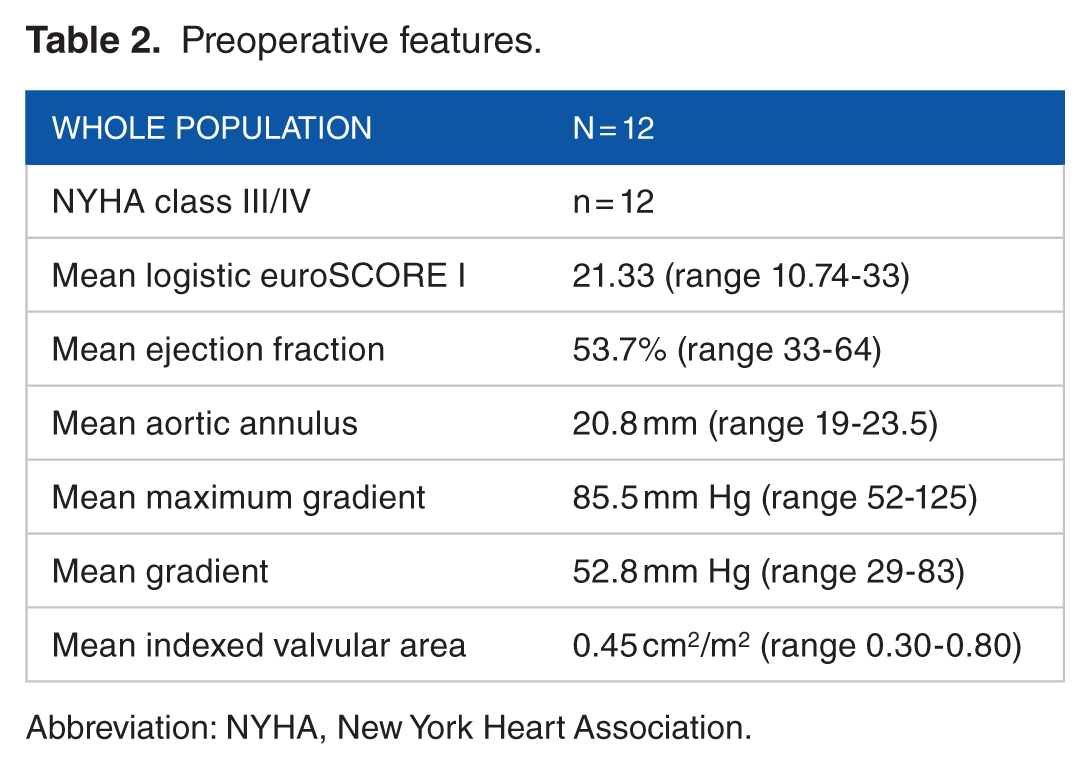
Abbreviation: NYHA, New York Heart Association.
Procedural feasibility
The retroperitoneal TI approach was successful in all the 12 patients. All valves were correctly positioned. No technical problems were encountered.
Procedural safety
All the safety endpoints were analyzed according to VARC-2. One patient died in the perioperative period because of the rapid onset of hypotension with hemodynamic deterioration due to massive incoercible right hemothorax. Two patients developed transient cerebral ischemic attacks (with negative cerebral CT scan). Only 1 patient had undergone iliac-femoral bypass grafting by means of a vascular prosthesis because of the laceration of a very fragile vessel at the removal of the sheath (Table 3).
Operative complications.

Abbreviation: TIA, transient ischemic attack.
Follow-up
We followed up all the 11 patients survived at least for 3 years. At discharge, all patients were on NYHA class I/II. The mean ventriculo-aortic gradient ranged between 6 and 20. Four patients had a mild perivalvular leakage.
The mean follow-up period was 60 months (Table 4). All patients followed up were on NYHA class I/II. The mean ventriculo-aortic gradient ranged between 7 and 23 (mean 10) and we encountered 6 mild to moderate perivalvular leaks. No patient had local vascular problems at the procedural access site.
Follow-up.
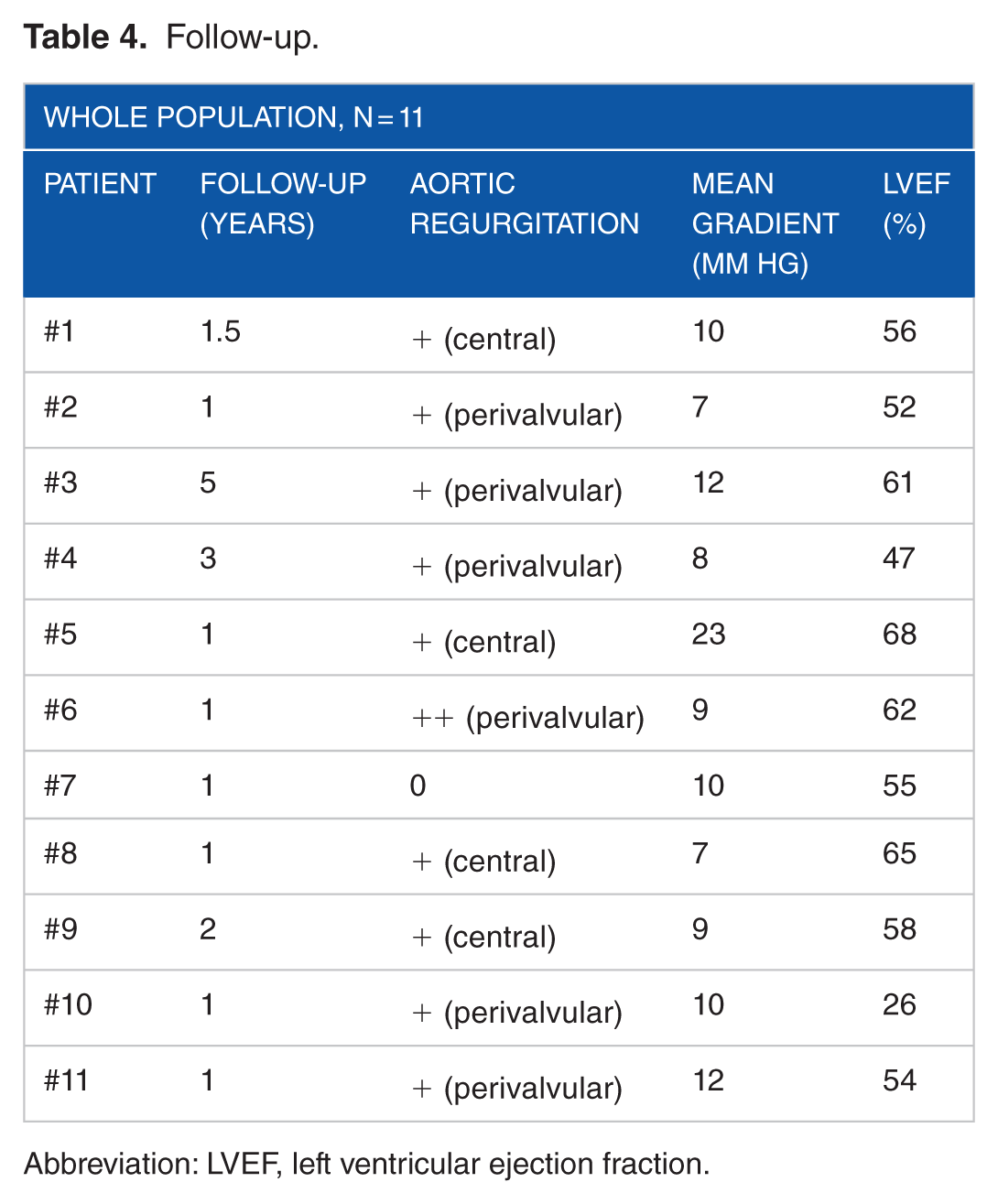
Abbreviation: LVEF, left ventricular ejection fraction.
Discussion
It is common practice, as recommended by the international guidelines, that the patient selection and access site choice for TAVR should be based on a preoperative multidisciplinary team approach (the so-called Heart Team) and that this procedure should be executed in a hybrid operative room by an experienced and specialized TAVR team.
TF TAVR is the more frequent access route for transcatheter purposes and is classically less invasive than the TA implant because it can also be performed under local anesthesia, with a small groin incision or total percutaneous approach and it does not require chest incision and drainage.
With the evolution of the knowledge and improvements in the delivery systems, the precision of TF TAVR is nowadays equal to that of TA TAVR and the risk of local vascular complications is mitigated by newer and smaller catheter sheaths leading to a widespread use of the TF route. The TF route is bordered by a moderate incidence of local vascular complications, normally reported between 1.9% and 17.3% in the literature. Major damage (dissection, laceration, rupture) requiring percutaneous or direct surgical intervention has been reported in 2.0% to 7.4% of the TF-TAVR population. 6
Failed closure or excessive bleeding with ProStar or Perclose ProGlide systems (Abbott Vascular, Abbott Park, IL, USA) requiring transcatheter intervention or surgery has been reported in 4.4% to 8.7%.7,8
When the TF access is not feasible because of the severity of the atherosclerotic disease, tortuosity, and/or heavy calcification or small diameter, other routes must be considered to reduce perioperative morbidity.
Actually, the TA TAVR approach could be an alternative to TF TAVR for patients with poor peripheral vasculature, even though it may carry additional risks. The TA approach may be reasonable in patients with good left ventricular function and no severe pulmonary disease. Classically, it requires a 5F femoral arterial sheath for angiography and a 5F or 6F femoral venous sheath. The procedure requires a left mini-thoracotomy at the fifth or sixth intercostal space carrying a relative risk of closure-related complications, but it offers a very quick and direct route for prosthesis delivery. 9
The retroperitoneal TI approach is still less investigated, but in some specific situation could give another route of access for TAVR purposes. It requires a small oblique incision 2 to 3 cm above the inguinal ligament and normally allows for a safe and direct management of the intra-abdominal vessel. We chose this particular access site whenever the femoral arteries are not suitable for the procedure, either in case of small caliber and/or in case of heavy focal calcification. Thus, if the more proximal arterial tree presents good spots and caliber, it should be taken into account by an experienced team.
The outcomes of our series show that the TI approach is feasible in selected patients with poor classical vascular accesses and considered to be of high risk for the TA approach.
Our early procedural mortality rate by the TI approach was low, with a 30-day survival rate of 92%. We report only 1 vascular-access-related complication, requiring an iliac-femoral vascular grafting, well functioning at follow-up.
The results of our work, by virtue of the low morbidity and mortality rates, confirm that retroperitoneal TI may be an alternative access route to the delivery of valvular prosthesis. We report a low vascular access route complication rate even with the use of older large sheaths.
We believe that nowadays, with the progressive reduction of the sheath diameter and the possible use of more atraumatic sheathless devices, the option of TI route could be applicable in a particular subset of patients in whom the arterial distal arterial access is advisable but the femoral route is not achievable or safe.
Study limitations
The main limitation of this discussion is the single-center experience. No randomization has been made. The small sample size is a strong limiting factor and also only 1 type of TAVR prosthesis was used. The experience discussed, and the relative follow-up, concerns the use of larger and older vascular sheaths.
Conclusions
A direct retroperitoneal TI approach for the TAVR procedure seems to be a feasible and safe access in a selected population in whom the other classical vascular routes are impracticable or at high risk. Nevertheless, despite the continuous evolution and improvements in the delivery sheaths and vascular closure devices, it is important to search for alternative approaches to classical TF access. 10
A large, prospective study using multiple different valves and newer, smaller sheaths is desirable to gain broad consensus on this approach.
Obviously, all the clinical decisions within the Heart Team must always be guided case by case.
Footnotes
Acknowledgements
The authors would like to thank all the personnel involved in the clinical management of the TAVR patients.
Author Contributions
MG writing, PT supervision, MP data collection and supervision, GP supervision, LS clinical management, MA supervision.
Declaration of conflicting interests:
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: M.G. is consultant to Medtronic.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Because of the retrospective nature of this work, our in-hospital Board of Review did not find any need for ethical approval, provided the full anonymous collection of the data.
Informed Consent
We state that the patients gave their consent to anonymous collection of the data.
