Abstract
In addition to inducing lethal DNA damage in tumor and stromal cells, radiation can alter the interactions of tumor cells with their microenvironment. Recent technological advances in planning and delivery of external beam radiotherapy have allowed delivery of larger doses per fraction (hypofractionation) while minimizing dose to normal tissues with higher precision. The effects of radiation on the tumor microenvironment vary with dose and fractionation schedule. In this review, we summarize the effects of conventional and hypofractionated radiation regimens on the immune system and tumor stroma. We discuss how these interactions may provide therapeutic benefit in combination with targeted therapies. Understanding the differential effects of radiation dose and fractionation can have implications for choice of combination therapies.
Introduction
To date, radiobiological models have been primarily focused on improving the therapeutic ratio of radiation treatment by enabling a toxic dose of radiation to tumor cells while sparing normal tissue. The linear quadratic (LQ) model of radiobiology is based on differential DNA repair in normal and tumor tissues. The LQ model predicts single-strand lethal damage (α parameter in LQ equation) and double-strand lethal damage (β parameter in the LQ equation) induced by ionizing radiation. Subsequent sublethal damage repair can also be modeled. The LQ model predicts that delivery of radiation dose in small fractions induces maximum tumor cell death compared with single-dose delivery, with minimal effects on normal tissue. 1
Traditionally, delivery of doses of 50 to 70 Gy using multiple fractions of 1.8 to 2 Gy per fraction in the curative setting of solid tumors is preferred to deliver the best therapeutic ratio. Recent technological advances in planning and delivery of external beam radiotherapy such as 3-dimensional image guidance, modulation of beam intensity and multileaf collimators, and 4-dimensional tumor tracking have allowed conformal delivery of larger doses per fraction while minimizing dose to normal tissues with higher precision. Thus, hypofractionated and extreme hypofractionated delivery schedules have been employed in treatment of many tumor types to increase tumor cell death while maintaining the therapeutic ratio. Stereotactic body radiation therapy (SBRT) and stereotactic radiosurgery (SRS) deliver focused, high-dose radiation in 1 to 5 fractions. Both SBRT and SRS have been used effectively for the treatment of lung, liver, brain, prostate, and recurrent head and neck cancers, among others.2–6 Damage to tumor cell DNA is thought to account for only part of the efficacy of hypofractionated regimens. 7 Many studies indicate that, in addition to direct impact on DNA, the effects of high-dose radiation on the tumor microenvironment (TME) may play a role in tumor control by SBRT and SRS.7–10
Profound evidence of the effect of radiation on the TME can be demonstrated by the abscopal effect, in which focal radiation can result in out-of-field responses. First reported in 1953, the abscopal effect is thought to occur through radiation-induced activation of immune responses within the TME. 11 Although clinical reports of abscopal immune responses induced by radiation alone are relatively rare, 12 recent advances in immunotherapy have renewed interest in radiation-induced immune responses. Ionizing radiation can alter interactions between tumor cells and their microenvironment and lead to immune cell priming. Cellular and DNA damage induced by radiation can result in the generation and release of tumor-associated neoantigens,13,14 as well as release of cytokines from both tumor and stromal cells.15–17 These events can shift the balance toward an immunoreactive, as opposed to immunosuppressive microenvironment, leading to the recruitment and activation of cytotoxic T cells. As such, radiation may expand the use of immunotherapeutics into nonimmunogenic tumors. Likewise, clinical reports suggest that radiation may rescue response in patients who have acquired resistance to checkpoint inhibitors. 18 Several clinical trials are underway to determine the effects of combination therapy with radiation and immune checkpoint inhibitors. 19 However, the optimal dose and fractionation schedules and predictive biomarkers required for radiation-induced immune priming are unclear.
In addition to the effects on the immune system, hypofractionated radiation therapy can also have profound effects on stromal tissue that may either promote or decrease tumor responses. Hypofractionated radiation can have both direct and indirect effects on the tumor vasculature20,21 and may synergize with antiangiogenic therapy.22–24 In addition to its effects on the tumor vasculature, radiation may also induce release of protumor cytokines and growth factors from cancer-associated fibroblasts (CAFs) 25 and lead to remodeling of the extracellular matrix (ECM)26,27 and decreased radiation response. This review summarizes radiation-induced immune and stromal effects and highlights differences that may arise from conventional versus hypofractionated radiation schedules.
Radiation Effects on the Immune System
Escape from immune surveillance is increasingly being recognized as a hallmark of cancer. Two aspects of immune escape are the ability to suppress immune reactivity and the ability to evade immune recognition. 28 Radiotherapy in combination with immunotherapy may aid in activating an immune response and switching the TME from immunosuppressive to immunoreactive. It was previously thought that radiation had a suppressive effect on the immune system, particularly due to the radiosensitivity of lymphocytes.29–31 Studies now suggest that radiation can stimulate the immune system, particularly through high-dose, hypofractionated administration. Preclinical studies demonstrating radiation effects on the immune TME are listed in Table 1.
Radiation effects on the immune microenvironment.
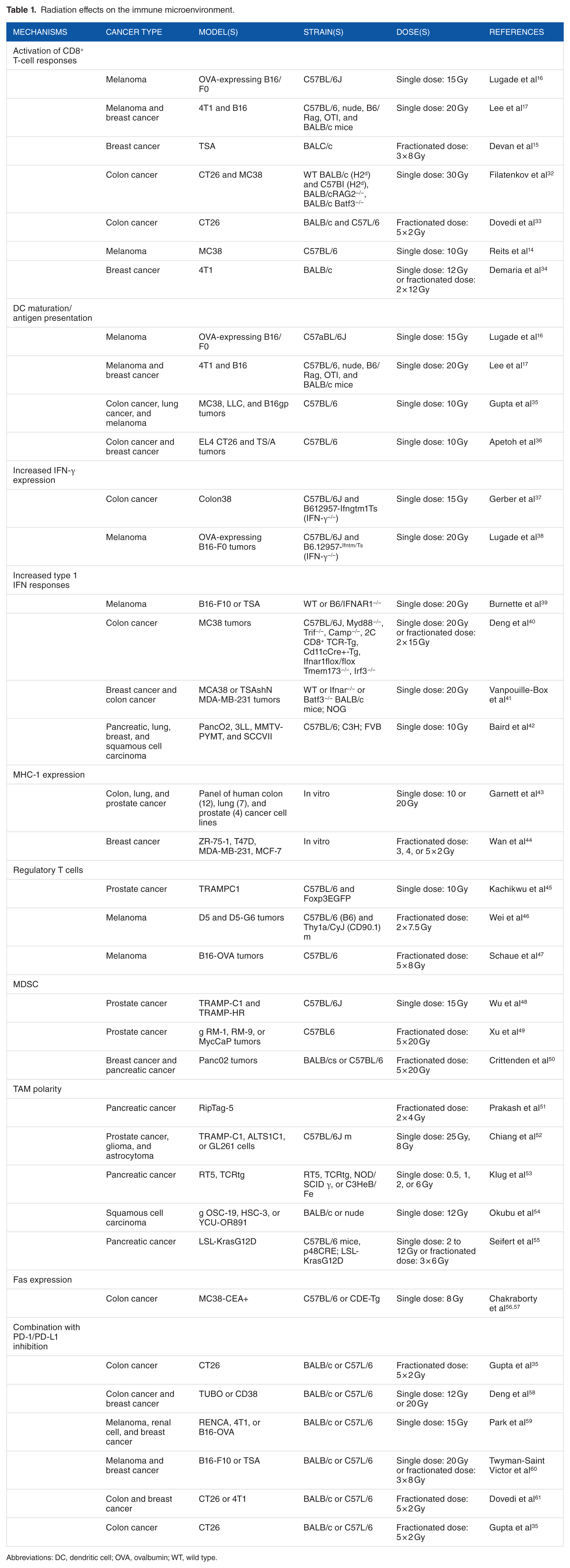
Abbreviations: DC, dendritic cell; OVA, ovalbumin; WT, wild type.
Cytotoxic T cell–driven radiation-induced tumor regression
The optimal radiation dose and fractionation regimens to activate cytotoxic immune responses are unclear. Many studies have suggested that ablative or hypofractionated radiation is superior to conventional fractionation schemes for the activation of antitumor CD8+ T-cell response.15–17 High-dose radiation induces enhanced double-strand breakage leading to increased cell death of tumor cells, as well as release of tumor antigens and cytokines, such as IFN-γ, that promote activation of cytotoxic CD8+ T cells.16,17 In a murine model of ovalbumin (OVA)-expressing B16-F10 melanoma, Lugade et al 16 compared the effects of a single dose of 15 Gy radiation to fractionated radiotherapy (5 × 3 Gy). Although T-cell responses were observed in both regimens, the single 15 Gy dose resulted in increased numbers of antigen-presenting cells and CD8+ T cells within tumor-draining lymph nodes, increased frequency of IFN-γ–secreting cells, and increased cell lysis by CD8+ T cells compared with fractionated regimens. In addition, ablative radiotherapy (20-Gy single dose) was reported to induce tumor rejection in an immunocompetent murine model of B16 melanoma but failed to induce regression in immunodeficient nude mice or mice that had been depleted of CD8+ T cells. 17 Although an initial response was observed in mice treated with moderate doses of fractionated radiation (4 × 5 Gy), tumors relapsed in a manner similar to T-cell–depleted mice. These findings suggest that fractionated regimens may result in death of infiltrating lymphocytes, resulting in relapse or recurrence. However, differential effects of radiation on tumor cell death between ablative and fractionated radiation could not be ruled out in this study. In contrast, a study in TSA breast carcinoma xenografts showed that hypofractionated (3 × 8 Gy) but not ablative (20-Gy single dose) radiotherapy resulted in an abscopal effect when combined with an anti-cytotoxic T cell–associated protein-4 (CTLA-4) antibody. 15 Likewise, evidence of T-cell activation following SBRT has been documented in patients with early-stage non–small-cell lung cancer (NSCLC). Increases in activated T cells were detected in the peripheral blood of patients with NSCLC following a total dose of 48 Gy in 6 to 8 fractions of SBRT. 62 In addition, changes in both CD8+ and CD4+ T cells have been documented in NSCLC following SBRT. 63 The proportion of overall CD8+ T cells and CD4+ T cells as well as activated CD4+ T cells expressing GATA-3, T-bet, and ROR-γt increased following SBRT in patients with NSCLC, whereas the levels of CD4+ FoxP3+ regulatory T cells (Tregs) decreased.
Most of the studies have suggested that high-dose radiation regimens are required for optimal induction of T-cell immune responses following radiotherapy, but less is known regarding conventional fractionation schedules. Filatenkov et al 32 demonstrated that while an ablative single dose (30 Gy) induced a robust CD8+ T-cell–dependent response that lead to tumor regression, addition of fractionated therapy (10 × 3 Gy) following this dose diminished the response. These findings indicate that conventional fractionation schedules may have a detrimental effect on the immune microenvironment that may result from death of infiltrating lymphocytes, resulting in relapse or recurrence. However, a recent study reported local and systemic immune responses that resulted in tumor clearance and abscopal effects in mice bearing dual CT26 colon carcinoma xenografts in which a single tumor site was treated with a conventional fractionation regimen (5 × 2 Gy) in combination with an anti-programmed cell death protein-1 (PD-1) monoclonal antibody. 33 Despite a reduction in T-cell number 24 hours after each fraction, there was expansion of local polyclonal T-cell responses and increases in infiltrating T cells in both irradiated and nonirradiated tumor sites 7 days after the conclusion of treatment, suggesting that conventional fractionation may also stimulate cytotoxic T cell responses. Interestingly, there was a high level of concordance between T-cell receptors from irradiated and nonirradiated tumors, whereas only 0.5% of T cells were unique to the irradiated tumor. This indicates that most of the reactive T cells in this model were responding to preexisting antigens rather than neoantigens created by radiation-induced injury. These findings are consistent with a previous study that showed increased intracellular peptide pools and expression of unique class I major histocompatibility molecules (MHC-1) in a dose-dependent manner. 14 Therefore, the formation of neoantigens may be optimal at doses higher than those delivered during conventional radiation regimens.
Dendritic cells aid in the activation of an antitumor immune response following radiotherapy
As the major antigen-presenting cell in antitumor immunity, dendritic cells process antigenic material and present tumor-associated antigens (TAAs) to CD8+ T cells, thereby aiding in their activation. Many studies have reported enhanced priming of T-cell responses after treatment with hypofractionated radiation due to increased presentation of TAA to CD8+ T cells in draining lymph nodes.16,17,35,36 In mouse models of thymoma and breast cancer, dendritic cells have been shown to be important in the antitumor T-cell–mediated immune response through radiation-induced release of high-mobility group box 1 (HMGB1) by dying tumor cells, which act on toll-like receptor 4 (TLR-4) expressed by dendritic cells, aiding in processing and cross-presentation of TAA. 36 In a B16 melanoma model, increases in antitumor immunity after radiation of tumors with a single dose of 10 Gy was dependent on infiltration of both CD8+ T cells and CD11c+ dendritic cells. 35 In this model, therapeutic efficiency was found to depend on the radiation-induced activation status of dendritic cells and not dependent on the presence of antigens. These findings are consistent with another study which also found that single high-dose radiation (20 Gy) resulted in activation and maturation of dendritic cells, improving T-cell priming in a mouse model of B16 melanoma. 17
Radiation-induced IFN-γ expression aids in T-cell activation
Radiation can influence cytokine production in the TME and alter the ways in which immune cells traffic to the tumor and function. Radiation promotes necrotic cell death, causing the release of DNA and damage-associated molecular patterns (DAMPs) including HMGB1 and ATP. The DAMPS can activate inflammatory signaling pathways which result in the release of a multitude of pro-inflammatory cytokines such as IFN-γ, TNF-α (tumor necrosis factor α), TGF-β (transforming growth factor β), interleukin (IL)-6, IL-10, IL-1α, IL-1β, and IFN-β that can be either immunosuppressive or immunostimulatory depending on their target cell.36,64,65,38,39 One of the most essential cytokines for radiation-induced T-cell priming is IFN-γ. IFN-γ is produced by cytotoxic T cells on antigen-specific activation, indicating presence of tumor antigen–specific cytotoxic T cells following radiation. 65 In a murine model of colon cancer, Gerber et al 37 demonstrated the necessity of IFN-γ release in radiation-induced immunity. In this study, increased secretion of IFN-γ was observed by CD8+ T cells after treatment with a single dose of 15 Gy and depletion of CD8+ T cells greatly reduced intratumoral levels of IFN-γ. Increased secretion of IFN-γ by CD8+ T cells was associated to increased lytic capability. Although IFN-γ was shown to have no effect on tumor cell growth, radiation-induced tumor regression was not evident in IFN-γ knockout mice, indicating its essential role in radiation-induced immune responses. Likewise, IFN-γ production within the TME in response to radiation has been shown to influence the antitumor immune response in a murine model of B16 melanoma. 38 In this study, a single dose of 15 Gy localized radiation led to increased T-cell trafficking through upregulation of vascular cell adhesion protein 1 (VCAM-1) on tumor vasculature as well as the chemoattractants MIG and IP-10 in wild-type mice but not in IFN-γ–negative mice, demonstrating the importance of IFN-γ in the radiation-induced T-cell–mediated immune response.
Radiation-induced type 1 interferon–dependent responses
Type 1 interferons (IFN-α and IFN-β) are important for activation of both innate and adaptive immune responses and are well known for their role in viral immunity. 66 In addition to natural killer and T-cell activation, type 1 interferons can also play a role in cross-priming of dendritic cells during adaptive immune responses. 67 Induction of type 1 interferon responses has been shown to be important in tumor reduction in response to radiotherapy.39,40 Local, single dose of 20-Gy radiation to B16 melanoma tumors in mice resulted in increased gene expression of IFN-β. 39 IFN-β production led to expansion of antigen-specific T cells and tumor reduction in a T-cell–dependent manner. In addition, the IFN-α/β receptor was necessary for the therapeutic benefit of radiotherapy to these tumors. Radiation-induced activation of type 1 interferon pathways correlated with abscopal responses in combination with anti-CTLA immunotherapy in mice treated with hypofractionated (3 × 8 Gy) regimens in a murine model of immune refractory mammary carcinoma. 41 Similar to previous studies, abscopal responses were abrogated in mice in which the interferon receptor had been knocked down in the irradiated tumor. These effects were not observed with single high-dose treatment in this study, as treatment with a single dose of 20 Gy in combination with anti-CTLA immunotherapy failed to induce IFN-β secretion or abscopal responses.
Radiation-induced expression of type 1 interferons can be initiated through recognition of DAMPs by toll-like receptors (TLRs).36,68 However, studies conducted in mice deficient for the TLR adaptor proteins MYD88 and TRIF failed to show any difference in radiation-induced immune responses compared with wild-type animals. 40 Alternatively, induction of type 1 interferons can be mediated through the TLR-independent Gas-STING pathway.69,70 Recognition of cytosolic DNA by the cGAMP synthase cGAS leads to the generation of cGAMP which then binds to and activates the endoplasmic reticulum protein STING (stimulator of interferon genes). STING activation results in the nuclear translocation of transcription factors which promote expression of type 1 interferons.69–71 CD11c+ dendritic cells, which are thought to have taken up exogenous tumor cell DNA, have been shown to be the major producers of IFN-β after radiation treatment, although STING-dependent activation of type 1 interferons has also been observed in tumor cells.40,41,72,73 Deng et al 40 showed that radiation-induced IFN-β was abrogated in dendritic cells from STING-deficient mice and these mice lacked the ability to cross-prime reactive T cells in response to radiation compared with wild-type controls. Treatment with exogenous IFN-β was able to restore this effect. Knockdown of cGAS in TSA breast cancer xenografts was shown to impair radiation recruitment and activation of CD8α+ tumor-infiltrating dendritic cells and led to a reduction in priming of tumor-specific CD8+ T cells in tumor-draining lymph nodes and spleen. 41 These studies indicate that STING-mediated induction of IFN-β may play an important role in radiation-induced immune priming. Furthermore, co-treatment with cGAMP or STING agonists has been shown to amplify the radiation-induced antitumor immune response and result in tumor regression.40,42
The optimal dose and fractionation schedule are unclear for STING-mediated activation of type 1 interferon responses. IFN-β–driven immune responses have been observed at both high and low radiation doses.39–42,72,73 However, Vanpouille-Box et al 41 reported that accumulation of cytosolic DNA was attenuated by the expression of the DNA exonuclease Trex1. Trex1 upregulation was observed in a dose-dependent manner after treatment with radiation and correlated with a reduction in cytosolic DNA at single doses above 12 Gy, but not on fractionation with lower doses. In addition, accumulation of cytosolic DNA in tumor cells was associated to time in S-phase.73,74 Higher radiation doses may induce blocks in cell cycle which decrease S-phase–dependent accumulation. However, more work is needed to understand the effects of conventional radiation on type 1 interferon response.
MHC-I upregulation by tumor cells following radiotherapy
Tumor cells present TAAs on MHC-I, which is recognized by cytotoxic T cells specific to that antigen, leading to lysis of tumor cells by cytotoxic T cells. One mechanism through which tumor cells escape immune recognition is through downregulation of MHC-I expression, which decreases their antigen presentation and recognition by lymphocytes. Studies more than 20 years old have shown that radiation can increase MHC-I expression by tumor cells, which may lead to enhanced immune recognition of tumor cells.75–77 In 1994, Klein et al 75 showed that irradiation of glioblastoma cells isolated from patients increased MHC-I expression in 4 out of 8 cases and was dose dependent, with the highest increase in MHC-I following 12 Gy. In 1996, Santin et al 76 demonstrated that high doses of radiation of 50 to 100 Gy upregulated MHC-I in human ovarian cancer cell lines. In 1997, Santin et al 77 showed similar effects in cervical cancer cell lines, with 25, 50, or 100 Gy leading to increased expression of MHC-I. More recently, a panel of 23 human colon, lung, and prostate cancer cell lines were analyzed for their expression of MHC-I following a single dose of 10 or 20 Gy radiation. 43 About 35% of the cell lines had upregulation of MHC-I expression following irradiation with 10 and 20 Gy, all of which were colon and lung cancer cell lines, and none of which were prostate cancer cell lines. The 10 to 25 Gy of radiation has also been shown to upregulate MHC-1 expression in a human melanoma cell line, MelJuSo. 14 In addition, a radiation dose of 25 Gy increased MHC-I binding to antigenic peptides. Therefore, MHC-I upregulation appears to be a mechanism by which high-dose, hypofractionated radiation induces antitumor immunity and this response differs among types of cancer and between patients of the same cancer type. Although limited studies have been performed with conventional radiation regimens, lower doses of radiation have also been shown to upregulate MHC. 44
Radiation effects on Tregs
Although radiation is known to induce antitumor immunity, some dose and fractionation schedules have been shown to increase the proportion of Tregs, which can impair the therapeutic effects of radiation. The Tregs have been shown to increase in mice lacking tumors following whole-body radiation as low as 0.25 to 0.5 Gy, which is representative of that given during conventional radiotherapy. 45 In addition, the same study found that a local, single dose of radiation (10 Gy) to a murine model bearing melanoma resulted in increased Tregs in both the spleen and in the tumors. Elimination of Tregs along with radiotherapy improved tumor growth delay and regression. Local irradiation with 10, 20, or 30 Gy in human patients with cervical cancer has been shown to decrease CD8+ and CD4+ T cells but have no effect on FoxP3+ Tregs and therefore shifts the balance of lymphocytes by enriching for an immunosuppressive, regulatory subtype. 78 These increases in Tregs following radiation is thought to result from their increased radioresistance compared with other T-cell subtypes.
In contrast, hypofractionated radiation treatment (5 × 8 Gy) in a murine model of melanoma found that radiation reduced the number and impaired the functionality of FoxP3+CD4+ Tregs, both in the blood and within the TME. 46 The reduction was equal to that of conventional T cells 0 to 2 days following radiation but greater than conventional T cells 4 to 7 days after radiation, indicating that Tregs are slower to recover. This study also found that local tumor radiation increased both the proliferation and the functionality of both host T cells and adoptively transferred T cells, and tumor radiation plus adoptive T-cell transfer significantly inhibited tumor cell growth.
The differences in Treg enrichment or depletion are most likely dependent on the radiation dose and fractionation schedule given. In a murine model of B16 murine melanoma expressing the antigen OVA, local, single dose of 5 Gy increased the Treg population but did not increase the effector T-cell response. 47 Alternatively, a single dose of 7.5 or 10 Gy resulted in a decrease in Tregs in the spleen and an increase in anti-OVA T cells, whereas a single dose of 15 Gy of radiation increased both the effector T-cell response and the Treg population. In this study, the best tumor control was seen following irradiation with 2 fractions of 7.5 Gy and the Treg population was lowest with this dose and fractionation schedule.
Radiation effects on myeloid derived dendritic cells
Myeloid-derived suppressor cells (MDSCs) are a heterogeneous group of myeloid cells that are defined by their functional ability to induce immunosuppression.79,80 In mice, 2 distinct subsets of MDSCs have been described: monocytic MDSCs (m-MDSC), which bear the phenotype CD11b+, Ly6ChighLy6G−, and granulocytic MDSCs (g-MDSC), which bear the phenotype CD11b+, Ly6ChighLy6G+.81,82 In humans, a single subset of MDSC has been identified, characterized by the phenotype CD11b+CD14−CD33+. 65 The MDSCs accumulate within the TME in response to the pro-inflammatory microenvironment and suppress the activation of both CD4+ and CD8+ T-cell responses.80,83,84 Influx of MDSC into the TME has been reported after both single high-dose and conventional fractionation regimens and are often associated with an influx of tumor-associated macrophages (TAMs).16,48,52,85 In a murine model of prostate cancer, Wu et al 48 showed that a single high dose of radiation (15 Gy) resulted in recruitment of MDSCs mediated by radiation-induced release of IL-6 from tumor cells. Likewise, Xu et al 49 reported increases in both m-MDSC and g-MDSC in tumors after radiation (5 × 3 Gy) treatment in 2 prostate xenograft models, RM-1 and Myc-Cap. Tumor influx was shown to be dependent on expression of colony-stimulating factor 1 (CSF-1) by the tumor cells on radiation treatment and blockade of CSF-1 was found to retard tumor regrowth after radiation. Although increases in peripheral blood MDSCs were observed after radiation treatment in the model, there were no increases in MDSCs in secondary lymphoid organs. Similarly, Crittenden et al demonstrated in a murine model of breast cancer that hypofractionated radiation treatment (3 × 20 Gy) leads to reduction in peripheral MDSC in the blood and spleen. This decline in MDSCs was linked to radiation response of the tumor, with declining numbers of MDSCs reported on decreased tumor burden. 50
Radiation-induced Fas expression by tumor cells
Although CD8+ cytotoxic T cells appear to be involved in high-dose, hypofractionated radiation-induced tumor regression, the mechanism by which this occurs is complex and not fully understood. CD8+ cytotoxic T cells mediate their lytic ability through release of granzyme and perforin and through engagement of Fas ligand (FasL) on their surface with Fas on target cells. Engagement of Fas with FasL leads to apoptosis through a caspase 1–mediated mechanism. 86 High-, single dose radiation has been shown to upregulate Fas expression by tumor cells, leading to increased cytotoxic T cell lysis through a Fas/FasL-dependent mechanism. 87 Murine MC38 colon adenocarcinoma cells expressing carcinoembryonic antigen (MC38-CEA+) showed increased expression of Fas following different doses of irradiation in vitro, which was highest following a single dose of 20 Gy, and this corresponded with increased lytic ability of CEA-specific cytotoxic T cells. The increased lytic ability of CEA-specific cytotoxic T cells was blocked with addition of anti-FasL, demonstrating the importance of the Fas/FasL interaction. In the same study, B6 mice injected with MC38-CEA+ tumor cells and irradiated with 8 Gy showed increased Fas expression. Adoptive transfer of CEA-specific cytotoxic T cells decreased tumor growth rate and volume. The same group subsequently demonstrated that, using the MC38-CEA+ murine model, vaccination with recombinant viruses expressing CEA and co-stimulation of T cells followed by a single dose of 8 Gy led to upregulation of Fas and significant reduction of tumors through a Fas/FasL-mediated pathway. 57 These studies indicate that Fas upregulation following high-dose, hypofractionated radiation is a mechanism through which cytotoxic T cells facilitate their antitumor activity.
Radiation effects on macrophage recruitment and polarization
Many studies in a variety of tumor models have shown that radiotherapy induces recruitment of macrophages into the tumor site, irrespective of dose and fractionation regimen. 87 Radiation-induced recruitment of TAMs was shown to be dependent on increased expression of the chemokine CSF-1. 49 Gene transcription of CSF-1 was demonstrated after radiotherapy, and blocking of the CSF-1 receptor in a xenograft model of prostate cancer treated with 5 fractions of 3 Gy reduced radiation-induced macrophage recruitment. 49 Alternatively, hypofractionated or high-dose single-fraction radiotherapy may promote TAM recruitment through induction of hypoxia by disruption of the tumor vasculature.85,88 Ceradini et al 88 showed that HIF-1–induced expression of stromal-derived factor 1 (SDF-1), which promoted recruitment of TAMs in a xenograft model of glioma following a single dose of 15 Gy.
The impact of increased presence of TAMs after radiation is unclear and is dependent on their polarization into either M1 or M2 subtypes. Although M1 macrophages promote inflammation and antitumor immune responses, those of the M2 phenotype are thought to support tumor growth, angiogenesis, and metastasis. 89 The impact of radiation on macrophage polarization may be related to dose and fractionation. Conventional doses of radiation have been shown to promote M1 polarization. Treatment of pancreatic tumor xenografts with radiation given as 4 Gy in 2 fractions resulted in a switch in tumor-infiltrating macrophages from a protumorigenic M2 phenotype to an antitumorigenic M1 phenotype. 51 Likewise, increased infiltration of T cells into tumors and tumor killing mediated by iNOS+ M1 macrophages through expression of TH1 cytokines have been reported in murine models of pancreatic cancer and melanoma after low-dose radiation treatment.51,53 Interestingly, this effect was not observed on high-dose radiation in these studies. Moreover, many studies have demonstrated M2 polarization after treatment with single high-dose and hypofractionated radiation regimens.52,54,55 M2 polarization often occurs in hypoxic areas 90 and thus may be promoted by the vascular damage and hypoxia associated with high-dose radiation.
Effects of Radiation on the Tumor Stroma
In addition to its effect on the immune microenvironment, many studies have shown that radiation can alter the tumor stroma with varying effects observed with different dose regimens. Preclinical studies demonstrating changes in the tumor stroma induced by radiation are listed in Table 2.
Radiation effects on the tumor stroma.
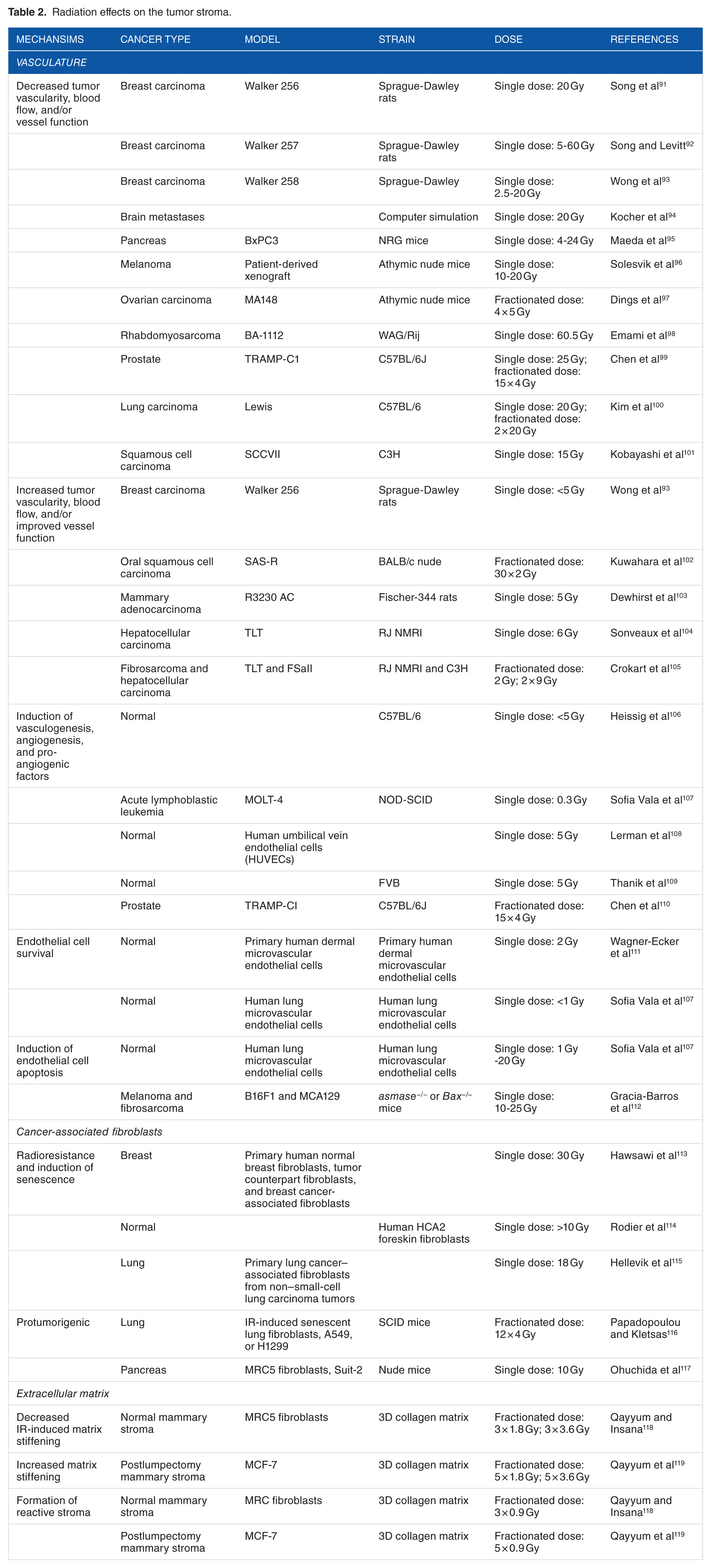
Effects of radiation on the tumor vasculature
The most well-studied effect of radiotherapy on the TME is on the tumor microvasculature. Tumor blood vessels do not resemble normal blood vessels in that they are morphologically immature, irregular in diameter, and are more permeable. Mature blood vessels are more radioresistant than developing human blood vessels. Therefore, immature tumor blood vessels and thus tumor endothelial cells are more sensitive to radiation. 120 The radiation-induced effects on tumor blood vessels vary widely, especially within animal models, and are dependent on total radiation dose and fractionation schedule as well as tumor type, site, and stage.9,121 However, vascular damage is primarily observed at doses greater than 5 to 10 Gy. In several studies looking at varying radiation doses on vasculature in Walker 256 tumors grown subcutaneously in the hind legs of rats, irradiation with 5 to 20 Gy decreased vascular volume in a dose- and time-dependent manner; however, a single dose of 30 or 60 Gy caused lasting decreases in vascularity and functional vessels in the tumors.91–93 In general, exposure to a single low dose of radiation resulted in tumor blood flow initially increasing and returning to pre-irradiation levels quickly, whereas high doses (>10 Gy) of radiation in a single exposure reduced tumor blood flow dramatically and resulted in destruction of tumor vasculature, changing tumor oxygen levels, and causing indirect cell death resulting in tumor volume decrease. These findings are supported by bioinformatics studies which indicate that high-dose radiation may have a profound effect on the tumor vasculature. 94 Using computer modeling of clinical data, changes in tumor vasculature in response to radiation were found to contribute to 19% to 33% of the overall effect from a single high-dose (20 Gy) radiosurgery in brain metastases.
Low-dose radiation schedules are associated with stimulation of angiogenesis and neovascularization, whereas endothelial cell survival is reported at conventional doses of 2 Gy.102,111 Furthermore, irradiation of mammary adenocarcinoma xenografts with doses of 5 Gy resulted in an increase in vascular density and perfusion. 103 In addition, in vitro endothelial cell studies showed that low-dose (<5 Gy) radiation stimulated angiogenesis through increased vascular endothelial growth factor (VEGF) secretion by stromal cells106,107 as well as vasculogenesis.108,109 In a study by Lerman et al, 108 low-dose radiation was also found to induce endothelial cell migration and vasculogenesis in an SDF-1–dependent manner. In addition, low-dose radiation has been shown to promote tumor vessel survival and maturation in an SDF-1–dependent manner during fractionated radiotherapy (15 × 4 Gy) in a murine prostate model. 110 The response of tumors to radiation is related to the supply of oxygen through adequate blood perfusion of the tumor, which may be improved at low radiation doses. Doses below 10 Gy have been found to promote tumor vessel relaxation and improve oxygenation.104,105 Fractionated regimens were found to have the maximum effect on tumor growth delay, presumably due to reoxygenation of the tumor. 105
In contrast, radiation doses higher than 10 Gy per fraction are associated with severe vascular damage leading to deterioration of the TME.8,95 A number of studies have focused on radiation-induced vascular changes of human tumor xenografts in rodents using high-dose irradiation in single-dose or several fractions. Irradiation of human melanoma xenografts with 10 to 15 Gy in a single exposure caused almost half of the tumor vessels to become nonfunctional within a week of treatment. 96 In addition, irradiation of human ovarian carcinoma xenografts with 5 Gy /fraction for a total dose of 20 Gy resulted in a decrease in vascular density to about half of that observed in control xenografts. 97 Likewise, irradiation of rhabdomyosarcomas grown in the scalp of rats with increasing single doses of radiation decreased blood flow rapidly, by about 50%, but lower doses used in the study had restoration of blood flow within 24 hours. 98 Irradiation of mouse prostate tumors grown in the thigh of mice with 25-Gy single dose decreased vascularity by 25%. 99 Single-dose radiation treatment (20 Gy) of Lewis lung tumors of mice grown subcutaneously in hind limbs decreased tumor blood flow initially but recovered by 4 days after irradiation. Interestingly, recovery could be suppressed by irradiating again with 20 Gy at 2 days but not 4 days after initial irradiation. 100
High-dose radiation has been shown to induce endothelial cell apoptosis through both direct DNA damage and ceramide signaling.9,112,122 Although endothelial cell damage has been shown to be a major factor in the biological mechanism of SBRT and SRS, this phenomenon is sometimes transient and may lead to neovasculogenesis via HIF-1 induction 95 and recruitment of bone marrow–derived CD11b+ cells which may serve as a source of endothelial cell replenishment.88,123 Tumors treated with fractionated radiation at 24-hour fractions had less vascular damage than tumors treated with a single high dose of radiation, indicating repair of damaged endothelial cells and thus restoration of tumor blood vessels.9,99,101 Interestingly, treatment with anti-VEGF or anti-VEGFR2 right before high-dose radiotherapy increased ceramide levels and resulted in a higher fraction of apoptotic endothelial cells. 124 In addition, restoration of blood flow after fractionated radiation could be suppressed through preventing influx of bone marrow–derived cells through inhibition of SDF-1 signaling. 85
Although SBRT and SRS may disrupt tumor vasculature and developing blood vessels, leading to enhanced cell death, they may also generate increased regions of hypoxia. 85 Modeling of tumor control probability has indicated that single high-dose regimens may result in impaired local control of hypoxic tumors, compared with hypofractionated regimens. 125 It is still under investigation if the loss of reoxygenation with ablative radiation can be overcome by hypofractionated radiation regimens and may require combination therapy with hypoxic cell radiosensitizers to obtain tumor control with lower dose and toxicity.126–128
Effects of radiation on CAFs and the ECM
In the stroma of human carcinomas, CAFs are the most abundant cell types and play a significant role in tumor cell growth, angiogenesis, and invasiveness.129–132 Large numbers of CAFs present in tumors are associated with high-grade malignancy and poor prognosis. 132 Within the TME, CAFs control the release of paracrine signals that regulate the behavior of other cells within the tumor and can stimulate the recruitment of cells involved in angiogenesis and inflammatory processes.133,134 Through the secretion of SDF-1 into tumor vasculature, CAFs can recruit endothelial progenitor cells to promote tumor blood vessel formation and contribute to tumor recurrence.134,135 In addition, reactive CAFs are an important source of cytokines and immunomodulators, which influence the inflammatory process during tumor development.131,136 The CAFs are also responsible for deposition of key ECM proteins (eg, collagen, fibronectin, and laminin) as well as secreting ECM-degrading enzymes (eg, matrix metalloproteinases),129,130 which promotes migration of CAFs and degradation of the ECM, allowing the invasion of tumor cells. 137 Primary lung tumor CAFs have been found in brain metastases derived from lung carcinomas. 138
Both normal tissue fibroblasts and CAFs have been found to be radioresistant cells, being able to survive high doses of radiation totaling above 50 Gy.113,116,139 However, the studies investigating the effects of radiation on CAFs are limited. Most of the studies investigating fibroblast response to radiation were conducted using normal connective tissue fibroblasts. In vitro studies have shown that fibroblasts develop an irreversible senescent phenotype when exposed to a dose >10 Gy of radiation, 114 whereas low doses of radiation induce reversible DNA damage without growth arrest. 115 Senescent fibroblasts release proteolytic enzymes, cytokines, growth factors, and reactive oxygen species, creating a protumorigenic environment.114,116,117,140,141 In a xenograft rodent model, co-transplantation of senescent fibroblasts with cancer cells increased the stimulatory effects of fibroblasts and promoted tumor growth.116,141 Interestingly, the senescence response is more pronounced after a single high dose of radiation in lung CAFs compared with when the equivalent dose is fractionated into smaller doses, indicating that the size and number of fractions in radiotherapy play an important role in the response of fibroblasts to radiation. 115 However, the overall effect of senescent fibroblasts on tumor progression is debated. The cancer-promoting effects of senescent fibroblasts may be organ or tumor specific and better models need to be developed to validate the response of fibroblasts to radiation.
Radiation injury triggers an inflammatory response within the TME, recruiting stromal fibroblasts.142,143 Enhanced release of inflammatory components, especially TGF-β, causes differentiation of the fibroblasts, resulting in the release of inflammatory mediators, ECM proteins, and a decrease in ECM-degrading enzymes secreted from the CAFs.144–147 Over time, excessive accumulation of ECM proteins within the TME thickens and stiffens the tissue, leading to the development of fibrosis. 146 This process creates a reactive stroma that promotes tumor growth. 148 The extent of radiation-induced fibrosis depends on the dose of radiation and the amount of tissue volume exposed. Qayyum and Insana used a 3-dimensional model of the mammary stroma to investigate fractionated radiotherapy on collagen matrix stiffness and fibroblast activation. Increases in the dose per fraction reduced the formation of reactive stroma necessary for tumor progression and mitigated matrix stiffening induced by radiation alone. 118 A lower dose per fraction caused greater activation of fibroblasts when compared with the higher doses. In an in vitro model mimicking postlumpectomy mammary stroma with residual disease, higher doses of radiation per fraction were more effective in reducing the protumorigenic microenvironment through prevention of fibroblast differentiation. However, higher doses per fraction increased ECM stiffening, which could stimulate the growth of surviving cancer cells over time. 119
The therapeutic effect of high-dose radiotherapy in certain cancers may be due to a reduction in the tumor promoting properties of CAFs. Hellevik et al 149 investigated ablative doses of radiation on CAFs isolated from freshly resected lung tumors from patients with NSCLC. Exposure to a single high dose of radiation (18 Gy) caused a change in the secretory profile of signaling molecules involved in inflammation, angiogenesis, and tumor growth by the lung CAFs. SDF-1, angiopoietin-1, and thrombospondin-2 (TSP-2) were all downregulated, whereas the release of basic fibroblast growth factor (bFGF) was upregulated. Conditioned media from irradiated CAFs did not affect the proliferation or migratory capacity of lung tumor cells in vitro but did partially reduce migratory capacity of endothelial cells, suggesting radiation of CAFs reduces their pro-angiogenic properties. In addition, high single dose of radiation resulted in increased expression of integrins and altered secretion of matrix metalloproteinases resulting in inhibition of the proliferative, migratory, and invasive capacity of lung CAFs. 115 However, both single-dose and fractionated radiotherapy elicited a radioprotective response by pancreatic stellate cells on pancreatic cancer cells both in vitro and in vivo. 150
Combining the Effects of Radiation on the TME With Targeted Therapies
Immune checkpoint inhibitors
Although radiotherapy has long been known to activate tumor immunity, clinical applications of radiation in combination with immunotherapy have only recently shown promise. The success of immune checkpoint inhibitors directed against the CTLA-4, and the PD-1 pathway has revived clinical interest in using radiation to prime the immune system, particularly in tumors that are not immunogenic or have previously failed immunotherapy. Preclinical evidence of synergy between checkpoint inhibitors and radiation has been demonstrated in numerous animal models, although the optimal timing, dose, and fractionation regimen are not clear. Most of these studies were performed with single ablative doses or hypofractionated regimens.15,34,58–60 CTLA-4 blockade with a monoclonal antibody plus 1 or 2 fractions of 12 Gy leads to improved survival of mice bearing 4TI breast cancer xenografts. 34 This improved survival corresponded with inhibition of lung metastases that was dependent on CD8+ but not CD4+ T cells. In addition, the combination of hypofractionated radiotherapy with CTLA-4 blockade also led to an abscopal effect in a TSA murine model of breast cancer. 15 In this study, 3 fractions of 8 Gy, but not a single dose of 20 Gy, to the primary tumor site, plus addition of an anti-CTLA-4 monoclonal antibody, led to an improved tumor response at the primary site and a secondary, nonirradiated site. This corresponded to an increase in IFN-γ–producing CD8+ T cells, indicating effector function.
PD-1 and PD-L1 inhibition has also been reported to synergize with radiotherapy. Upregulation of PD-L1 in the TME was observed by Deng et al 58 following a high dose of 12-20 Gy radiation. Addition of an anti-PD-L1 monoclonal antibody improved radiation-induced antitumor response in a CD8+ T-cell manner and reduced numbers of MDSCs. In addition, Park et al 59 demonstrated that SBRT in combination with anti-PD-1 therapy led to regression of both primary irradiated tumors as well as an abscopal effect.
Although these studies are encouraging, a clinical study of combination therapy with anti-CTLA-4 and radiation treatment in melanoma patients suggested many patients were nonresponders or developed resistance. 60 In an animal study designed to recapitulate the clinical trial, the investigators analyzed response to combination treatment with anti-CTLA-4 and radiation in a B16-F10 melanoma model. Although they demonstrated that the combination therapy was more effective than either treatment alone, and responses were observed in both irradiated and nonirradiated tumors, this was not the case in all mice. Mice which failed to respond had evidence of T-cell exhaustion. Transcriptomic profiling revealed upregulation of PD-L1 in the TME of nonresponders and addition of anti-PD-1 to the treatment regimen improved responses in both the naïve B16-F10 tumors and the resistant sublines. In addition, SBRT, anti-CTLA-4, and anti-PD-1 were found to have differential effects on tumor immunity. Although radiation was found to expand the diversity of peripheral T-cell clones, anti-CTLA-4 inhibited Tregs, shifting the balance toward cytotoxic T cells. Addition of anti-PD-1 to the combination therapy prevented T-cell exhaustion and further enhanced T-cell expansion. 60
Numerous clinical trials are currently underway to assess the combination of checkpoint inhibition and radiotherapy (reviewed by Crittenden et al 151 ). Although the results are still forthcoming, preliminary data suggest that there may be clinical benefit to combination therapy. A phase 1 trial combining ipilimumab (anti-CTLA-4) in radiation treatment of NSCLC, colorectal carcinoma, sarcoma, and renal cell carcinoma demonstrated a partial response in 10% of patients and clinical benefit in 23% of patients. 152 Response correlated with increased peripheral CD8+ T cells, CD8+/CD4+ T-cell ratio, and activation of T cells as defined by expression of 4-1BB and PD-1 on CD8+ T cells. Although results of clinical trials combining PD-1 inhibition and radiation are still forthcoming, case studies demonstrated that the combination may yield therapeutic advantage. A case study of a patient with metastatic melanoma treated with whole brain radiation given as 30 Gy in 10 fractions in combination with PD-1 blockade with pembrolizumab showed complete, durable resolution of disease, including brain metastasis. 153
The optimal sequence for delivery of radiation and immunotherapy is still unclear. Murine studies indicate that optimal expression of PD-L1 occurs within 3 days after radiation treatment, and concomitant, but not sequential, treatment is required for T-cell–mediated tumor regression.35,61 In a study of 75 patients with melanoma brain metastases treated with checkpoint therapy in combination with SRS, the administration of either anti-CTLA-4 (ipilimumab) or anti-PD-L1/PD-1 (pembrolizumab or nivolumab) within 4 weeks of SRS resulted in increased early radiographic response, compared with treatment separated by more than 4 weeks. 154 However, there was no significant difference observed between concurrent and nonconcurrent therapy, indicating that radiation-induced changes in immune responses are sustained for a short window following treatment. In contrast to this study, secondary analysis of the KEYNOTE-001 phase 1 trial revealed that progression-free survival was significantly longer in patients who had received any form of radiotherapy prior to starting the trial. 155 The median time between radiotherapy and the start of pembrolizumab was 9.5 months for patients who received extracranial radiotherapy and 11.5 months for patients who received thoracic radiotherapy. These findings indicate that, for some patients, the immune priming effects of radiation may be long-lasting, and there may still be increased clinical benefit for checkpoint inhibitors in patients who have recurrent disease following radiation therapy. Although studies investigating the effects of checkpoint inhibition prior to radiotherapy are limited, palliative radiation was shown to induce a robust immune response in a patient with refractory disease previously treated with the PD-1 inhibitor nivolumab, indicating that radiation priming may be able to prolong the effects of and/or overcome prior resistance to PD-1 inhibition. 18 The optimal sequence, dose, and fractionation schedule will most likely vary depending on type of immunotherapy combinations, as well as tumor features such as immunogenicity and genetic status.
Antiangiogenic agents
The release of angiogenic growth factors such as VEGF and FGF after radiation has been well-documented, and blockade of VEGF signaling has been shown to potentiate radiation effects in animal models.106,107,124 Several angiogenesis inhibitors are under clinical investigation in combination with radiotherapy.156,157 Combination treatment with bevacizumab, a humanized antibody to VEGF-A, has been shown to decrease regions of hypoxia within the TME and improve response to chemoradiation in many types of cancer including rectal, head and neck, colon cancer, and glioma.158–162 In a study comparing the effects of low-dose bevacizumab in meningiomas, which had received prior radiation to those that had not, Furuse et al reported significant radiological responses in 4 of 6 tumors that had been previously irradiated. No response was observed in tumors that had not received radiation, leading the investigators to conclude that the effects of bevacizumab were most likely due to postradiation changes in the TME rather than an effect on tumor cells.22,163 Likewise, low dose bevacizumab has been reported to decrease radiation necrosis164,165; however, this effect was less evident after hypofractionated radiotherapy in tumors with large target volumes. 166
Sunitinib is a small molecule tyrosine kinase inhibitor that acts to inhibit downstream signaling pathways of VEGF and has been shown to synergize with both conventional and hypofractionated radiation in animal models of cancer. 167 Sunitinib has been shown to increase tumor cell apoptosis and improve oxygenation through vasculature normalization in animal models of cancer.168,169 Several clinical trials are currently in progress that will assess the safety and efficacy of sunitinib as a combination therapy (reviewed in Kleibeuker et al 170 ). Although the optimal dosing and timing of sunitinib combined with radiation have not yet been determined, data from initial trials are encouraging. In a phase 2 trial of concurrent sunitinib and Intensity Modulated Radiotherapy (IMRT) in patients with oligometastases, a local control rate of 75% and a distal control rate of 52% were observed. Mean time to progression was 9.5 months, and 11 patients remained disease free at the 2-year follow-up. 171 Promising results were also observed with SRS and SBRT in patients with metastatic renal cell carcinoma who received concurrent sunitinib.172,173 Theoretically, sunitinib may also have an effect on postirradiation changes and has been shown to prevent neovascularization in animal models.157,174 However, to date, use of sunitinib as a maintenance therapy after irradiation has not shown clinical benefit.173,175,176
Conclusions
Understanding the differential effects of conventional fractionation versus SBRT and SRS on the TME may help to inform choice and improve response to combination therapies. Likewise, improved knowledge of the effects of radiation dose and fractionation on the TME may help to optimize treatment planning of radiation delivery. Although hypofractionation may promote enhanced CD8+ T-cell responses, efficacy may be diminished by death of infiltrating lymphocytes (particularly in irradiated lymph nodes) and other microenvironmental changes such as increased tumor hypoxia and polarization of M2 macrophages. Dose modulation with heterogeneous high- and low-dose regions within the tumor may provide a hybrid form of radiation delivery that may promote the antitumor effects of both high-dose and conventional fractionation regimens.
In light of the increasing knowledge of the effects of radiation on the TME, new radiobiological models are needed to allow the radiation oncologist to optimize the treatment plan based on the TME characteristics. Hypofractionated treatments with dose per fraction more than 10 Gy is becoming more popular and accepted in radiation oncology due to advances in treatment delivery techniques; hence, new radiobiological models are being developed. The conventional fractionation models using the LQ equation and the 4Rs of radiobiology (
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
KMA, NJF, and JSM wrote the first draft of the manuscript. KMA, NJF, AR, LR, YY, APD, FM, and JSM contributed to the writing of the manuscript; agree with manuscript results and conclusions; jointly developed the structure and arguments for the paper; and made critical revisions and approved final version. All authors reviewed and approved the final manuscript.
Disclosures and Ethics
As a requirement of publication, authors have provided to the publisher signed confirmation of compliance with legal and ethical obligations including but not limited to the following: authorship and contributorship, conflicts of interest, privacy and confidentiality, and (where applicable) protection of human and animal research subjects. The authors have read and confirmed their agreement with the ICMJE authorship and conflict of interest criteria. The authors have also confirmed that this article is unique and not under consideration or published in any other publication, and that they have permission from rights holders to reproduce any copyrighted material. The external blind peer reviewers report no conflicts of interest.
