Abstract
Risk groups for mucormycosis include persons with immunosuppressed immune system and uncontrolled diabetes. The patients suffering from corona virus or post covid patients have been found to be entrapped with this fungal infection due to suppression in the immune system. Also the major attack was reported in those patients who were in Intensive Care units. It arises due to the fungal infection of various species and can occur simultaneously with covid. The development of black fungus mostly affects lungs, eyes, brain, and skin and is not at all contagious. Proper diagnostic can only predict that the patient is in invasive attack of which mucor species. It is better to take prevention by wearing medicated masks, hand gloves, wearing glasses, avoid dusty and damp places.
Introduction
The most distressed infectious disease of the century COVID-19 is really becoming threatening day by day by regular mutation of the virus. The people are exhibiting mild to severe symptoms depending upon the extent of infection encountered by the virus and their own individual immunity. In many parts of the globe the disease has brought the wave of death storm which is really heart wrenching. The world health organization and all the health centers have been continuously alarming the people to follow the covid protocols of continuous use of medicated masks, sanitization by using sanitizers and washing hands properly with soaps, maintaining physical distancing but yet the second wave has empowered various parts of the globe and had tragic effects on mankind. People are greatly affected by its adverse effects on lungs thereby causing multiple other ailments which becomes a matter of worry. Besides this aggressive attack of black fungus caused by group of molds called mucormycetes thereby entitled as Mucormycosis, is a subject of great grave for the health workers .The present article tries to emphasize the effect of black fungus on recovered covid patients as a critical post covid symptom as people are pushed back to ICU again. People are still unaware of the attack of various types of fungus in the hospitals which overpower the human system because of low immunity in the body. Mucor produces about millions of spores (Figure 1) which are microscopic spherical, dark-hued structures, which are dispersed in air.1-4 When the spores land on moist surfaces, like soil or plant material, they begin to germinate and produce thread like structures called mycelia. The mycelia branch out and feed on sugars in their surroundings and grow.
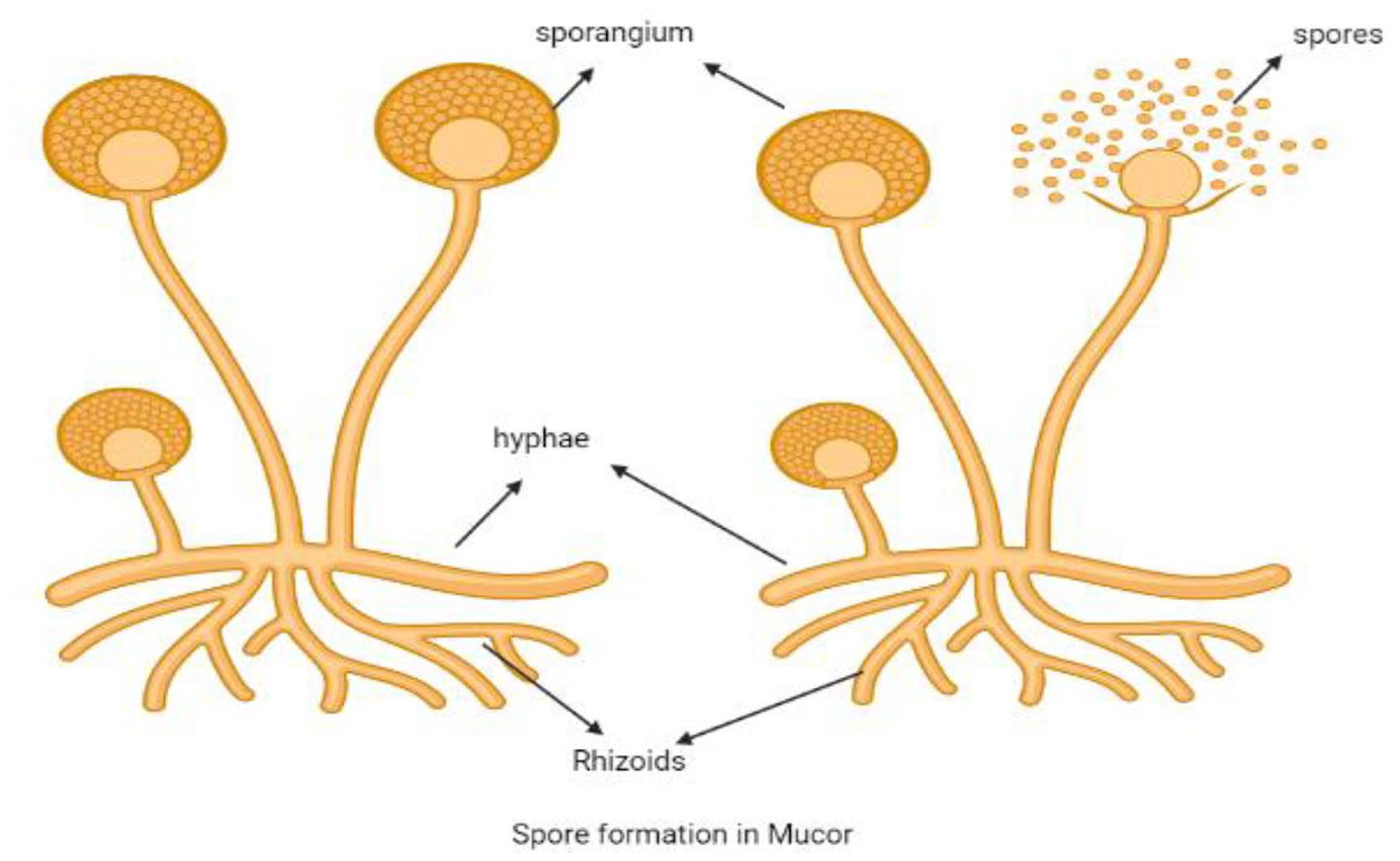
Spore formation in mucor.
Fungal spores measure 1000th to 100th of a millimeter. The density of the spores—the number of spores per cubic meter of atmosphere—varies depending on the fungus, the location (vegetation and exposed earth), and season. In tropical areas like in India, spore counts are generally higher during the summer than during the monsoons. But compared to the 1000 to 5000 spores per cubic meter outdoors, the count inside homes is typically 100 to 250 only. About 90% of the total spore population in the air is only due to 5 to 10 species. There are many fungi which causes allergy and they belong to Ascomycota, basidiomycota. Aspergillus, Penicillium, Didymella, Pleospora, Alternaria, Cladosporium, Epicoccum, are collectively referred as Basidiospores which mainly trigger to allergy. Sporobolomyces and Tilletiopsis produce small spores which severely causes Asthma. Most of the patients are suffering from mucormycosis and aspergillosis which is really very fatal for humans. Initial treatment of mucormycosis typically requires early aggressive surgical debridement of infected tissues in combination of antifungal medicines as suggested by the doctor. The most common prescribed as search from literature 5 is amphotericin B deoxycholate (Amb) or liposomal amphotericin B (L-AmB).
Mucormycosis or zygomucosis is a type of fungal infections caused by fungi in the order of Mucorales. Molds belonging to the order Mucorales, most commonly Rhizopus species, Rhizomucor, Others include Mucor species, Apophysomyces species, and Lichtheimia (formerly Absidia) species. 6 Mucor (Figure 2) is a type of fungi that has a widespread occurrence and is commonly found in soil, digestive systems, plant surfaces, rotten vegetable matter. Most species of mucor are unable to infect humans in endothermic conditions due to their inability to grow in warm environment close to 37°C. Some are thermotolerant species such as mucor indices that causes often rapidly spreading infection in humans. Mucormycetes are thermotolerant molds that are found in the environment. 7 The sample study investigation of Environment reveals that Mucormycetes are commonly found in soil, but are rarely found in air samples targeting fungal spores.8-11 It mostly affects the sinus, lungs, skin, and brain.
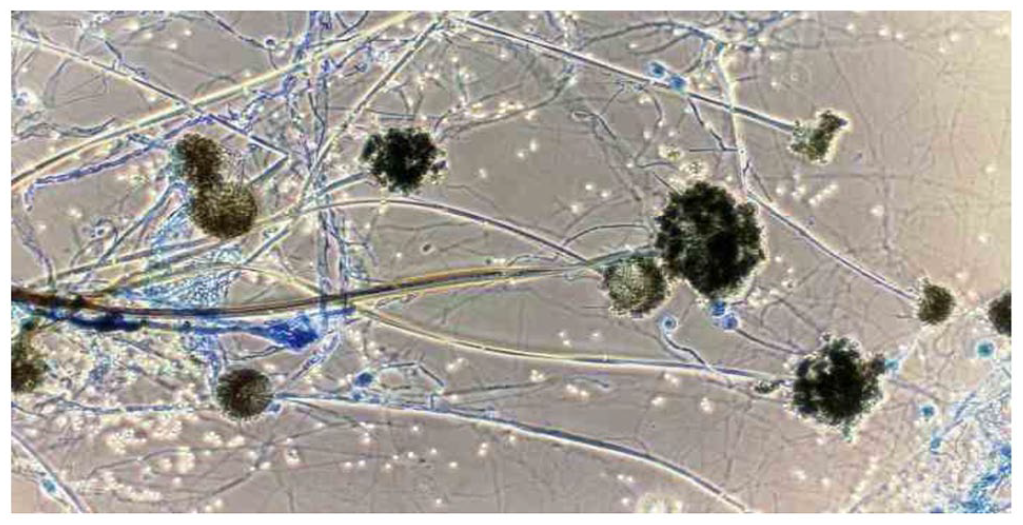
Photo of mucor (Courtesy OpIndia, News Report, 19th May 2021).
Conveyance of mucor
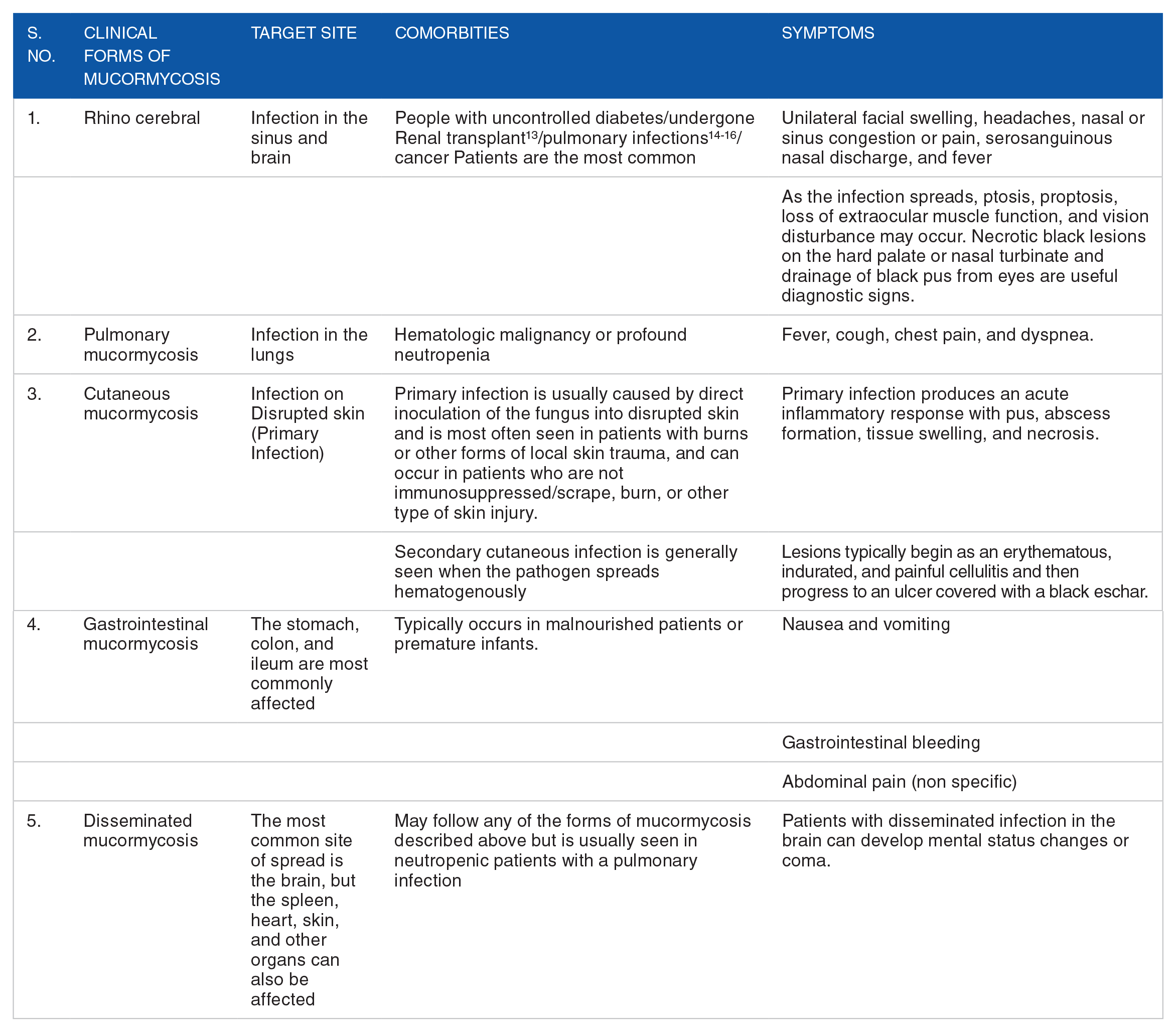
Conditions such as prolonged ICU stay, co-morbidities, weak immune system, excessive use of steroids can increase the chances of being susceptible to mucormycosis. Besides this hospital linens, negative pressure rooms, water leaks, poor air filtration, non-sterile medical devices, may also be the reason of this fungal infection. It has been declared as a epidemic in Rajasthan in India 12 air filtration, non-sterile medical devices, and building construction. There are 5 major clinical forms of mucormycosis
A flowchart has been depicted explaining the Molecular pathogenesis of patients suffering from DKA (Figure 3) and Molecular pathogenesis of Immunosuppressed patients (Figure 4).
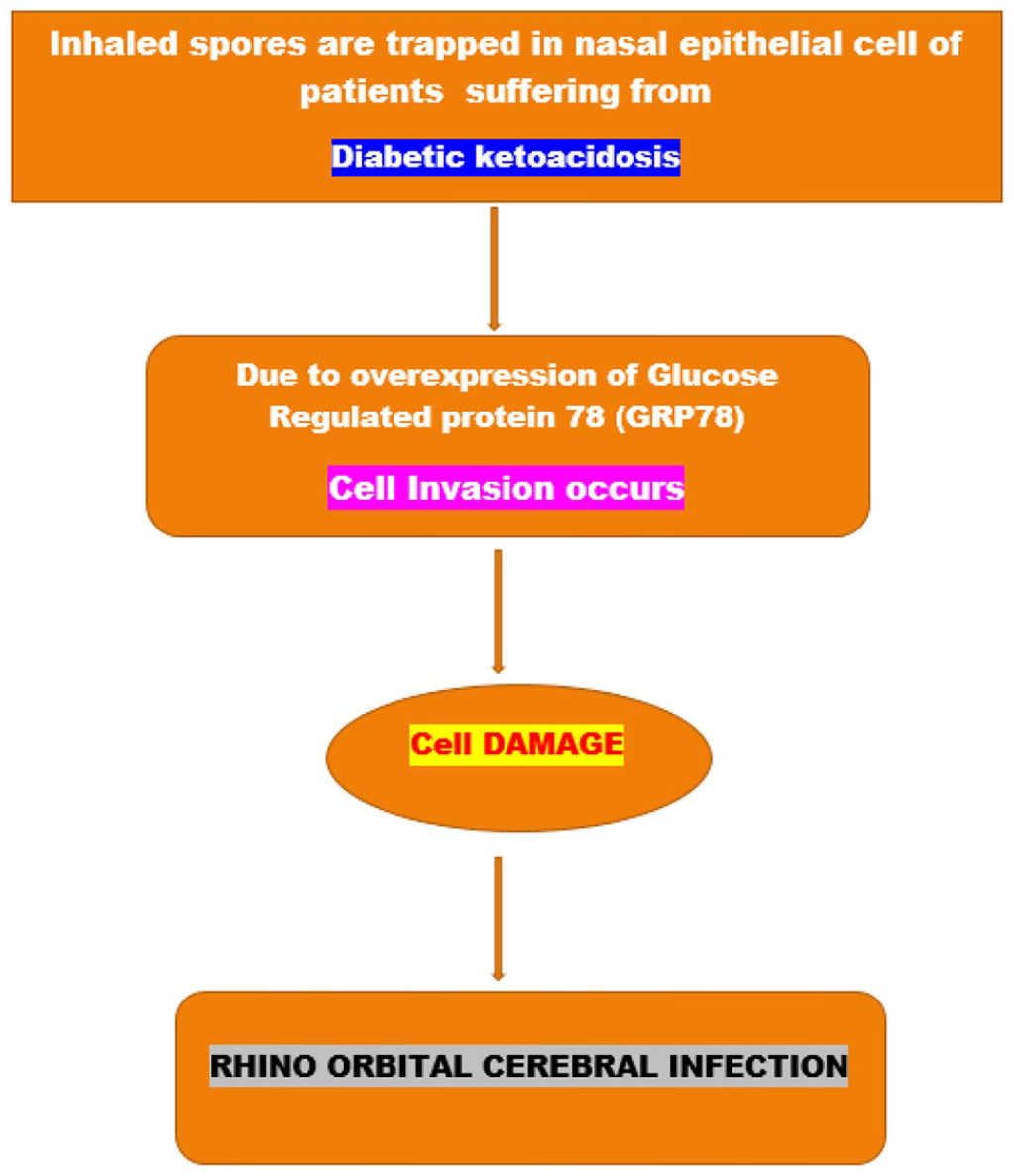
Molecular pathogenesis of patients suffering from DKA.
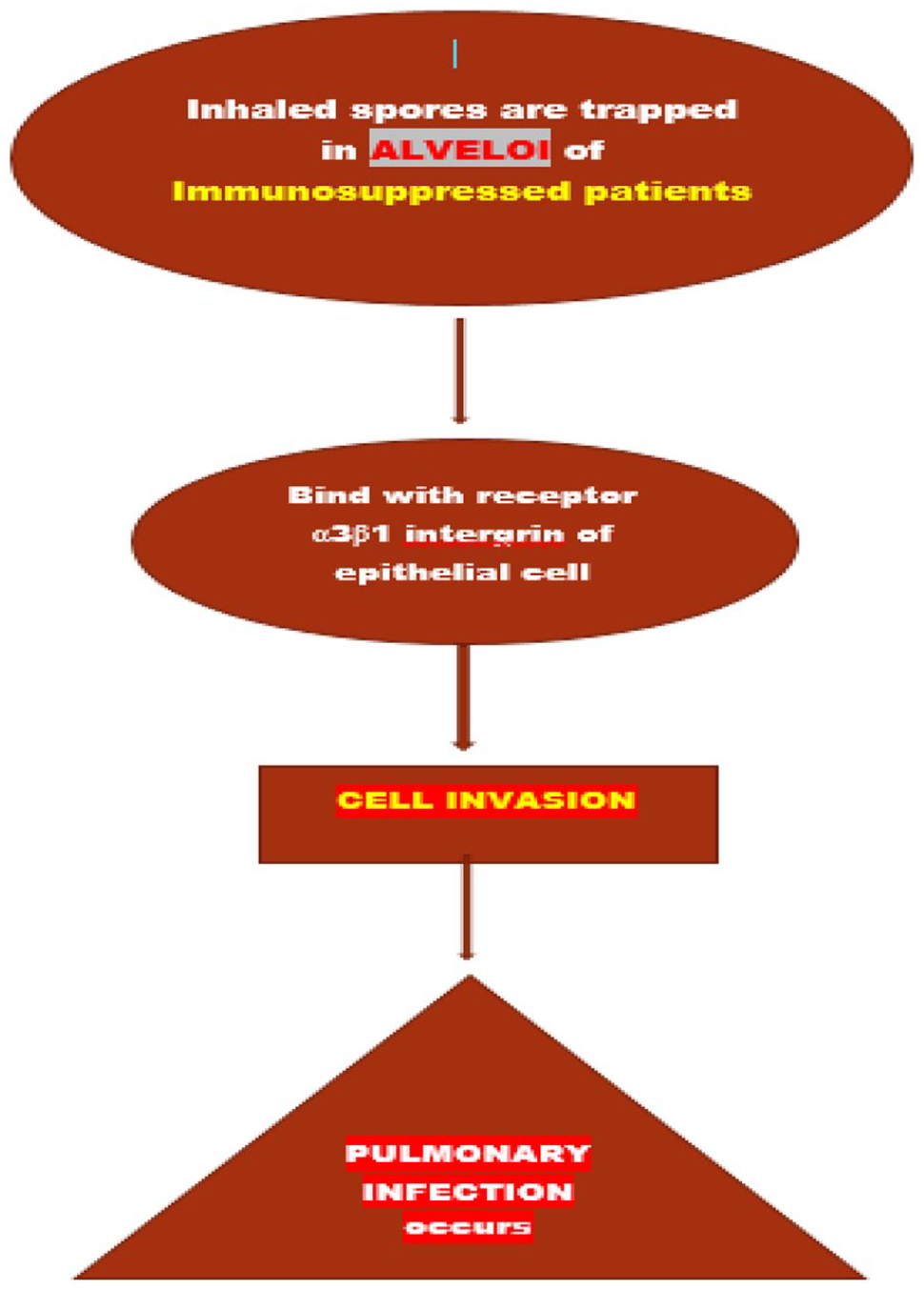
Molecular pathogenesis of Immunosuppressed patients.
Following are the photos (Figure 5) of patients suffering from mucormycosis.

(A) 45 Year old woman with poorly controlled insulin dependent diabetes mellitus had facial and periorbital swelling. Image taken from N Engl J Med. 1995;333:564. doi:10.1056/NEJM199508313330906. (B) Cutaneous mucormycosis of scalp and eyelids in a child with type I diabetes mellitus. Taken from Case Rep. 2015;81:275-278. doi:10.4103/0378-6323.152740.
In General we can mention Risk groups for mucormycosis include persons with compromised immunity.
Like suffering from covid 19, HIV, AIDS, cancer, with Transplant of organ/stem cell, skin trauma, burns, or surgical wounds; iron overload; excessive intravenous drug use; malnourishment; and premature infants, low number of white blood cells (Neutropenia).
Steroids are given to COVID-19 patients who are at risk which increases the sugar level both in diabetic and non diabetic patients. It means it suppresses the immune system and should only be given if it is very necessary. The following table shows the percentage data in the tabular form.

Diagnosis
A definitive diagnosis of mucormycosis typically requires histopathological evidence or positive culture from a specimen from the site of infection. Specimens from sterile body sites offer stronger evidence of invasive infection compared to colonization.21,22 Culture of non-sterile sites (eg, sputum) may be helpful in patients with infection that is clinically consistent with mucormycosis. Mucormycetes may be difficult to differentiate from other filamentous fungi in tissue; experienced pathological and microbiological assistance is often helpful. No routine serologic tests for mucormycosis are currently available, and blood tests such as beta-D-glucan or Aspergillus galactomannan do not detect mucormycetes. DNA-based techniques for detection are promising but are not yet fully standardized or commercially available. 23 Even biopsy of the tissue should also be taken into notice.
Preventive Measures
A lot of measures can be adapted to prevent the exposure of fungi.
Wear an N95 Mask.
Avoid Gardening/yard work in order to not get exposed to soil. If you can’t avoid then wear shoes, long pants, and a long-sleeved shirt when doing outdoor activities such as gardening, yard work, or visiting wooded areas.
Wear gloves when handling materials such as soil, moss, or manure.
Try to avoid areas with a lot of dust like construction or excavation sites.
Avoid direct contact with water-damaged buildings and flood water after hurricanes and natural disasters.
To reduce the chances of developing a skin infection, clean skin injuries well with soap and water, especially if they have been exposed to soil or dust.
If minor symptoms are observed immediately consult your doctor for antifungal medication which may help prevent serious complications.
Fungal Disease Related to COVID-19
It is very important to have a laboratory testing to know whether the person is suffering from fungal infection because the symptoms of both covid 19 and fungal infection are very common such as fever, cough, and shortness of breath in the early stages. It is found that some patients to have COVID-19 and a fungal infection at the same time. During recent studies it has been found that fungal co-infections are reported with increasing frequency and can be associated with severe illness and death.24-28 Therefore awareness is very important. The most common fungal infections in patients with COVID-19 include aspergillosis (infections caused by the fungus Aspergillus) 29 or invasive candidiasis. 26 which has been associated with pulmonary aspergillosis24-27 referred as CAPA.13,15,16,21,22 It has been observed that the testing should be done from lower respiratory track in the lungs to track the infection for Aspergillus galactomannan antigen and fungal culture. Health care associated infections such as blood streams infections by Candida27,30 has been also reported for hospitalized patients. Limited resources of health care facilities like gloves, gowns is also a key factor of the fungal spread like C.Auris. Medical workers should consider Pneumonias causing respiratory illness due to fungal infections if a person particularly is negative for Covid 19.
Conclusions
Our utmost responsibility during this phase is to educate the society bout the disease. It is very important to note that the fungal diseases and covid 19 can occur together.27,30 Clinical testing should be done very peculiar and accurate to track the major cause of ailment. The diabetic level should be controlled properly in order to balance the immune system. There can be attacks from multiple fungus depending on the site where it targets and affects. A lot of caution and proper directed medication should be given to patients by monitoring all the parameters especially periodical monitoring of sample of the air in hospitals especially the intensive care units to check for the presence of spores. It should be ensured that the humidifiers used during oxygen therapy are sterile. The recovering patients should be advised to remain indoors until they regain their natural strength and immunity. Also patients engaged in farming or gardening should be advised to take rest and develop their natural immune. At last it could be summarized that concerted efforts of revamping surveillance, diagnosis, and management along with public awareness and patient education are the requisites of managing COVID 19 and mucormycosis syndemic in India. 31
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
The authors have tried to collect maximum information regarding mucor. Both authors have contributed their best the review.
