Abstract
The lengthy tuberculosis therapy is emblematic of how hard drug-persistent infections are to eradicate. Phenotypic variation within clonal bacterial communities contributes to drug evasion and has major implications for the treatment of drug-persistent infections. We reported that single mycobacterial cells exhibit differential drug susceptibility, contingent on their inherent phenotypic variation in DNA damage response. Individual cells experiencing severe DNA damage massively induce the SOS response and exhibit signs of programmed cell death (PCD), such as unbalanced growth, chromosomal fragmentation, autolysis, and release of the intracellular content. Toxin-antitoxin systems are known to contribute to PCD in model microorganisms by targeting essential cellular processes, and they might function similarly in mycobacteria. We have found that the toxin MazF and a Clp protease, possibly responsible for degrading the MazF cognate antitoxin MazE, are induced during harsh conditions in a model organism for tuberculosis, and that cells that are about to lyse from drug exposure display a buildup of toxin. Deeper analysis of PCD in mycobacteria may reveal whether this process belongs to a broader strategy for the community’s survival. Finally, disrupting the balance between survival and PCD may prove useful to tackle drug evasion in mycobacterial persistent subpopulations.
Keywords
Commentary
Tuberculosis is not a disease of the past, but rather a growing concern on the global scale, affecting approximately 10 million people every year and causing more deaths than any other infectious agent alone. 1 Mycobacterium tuberculosis is an airborne and primarily a pulmonary pathogen, which can also spread to other organs, especially in children and in people weakened by preexisting disorders, aging, or poor living conditions. This pathogen is not easily cleared by the host but can persist in a variety of clinical and subclinical forms, which can reactivate. Persistent bacilli are recalcitrant to drugs and require prolonged combination therapy, which causes adverse effects, often resulting in patient nonadherence and drug resistance. 2 Genetic drug resistance is largely responsible for the aggravation of the tuberculosis pandemic, and it accounts for a quarter of all deaths associated with antimicrobial resistance. 3 While drug-sensitive tuberculosis is 85% curable in about 6 months of treatment, only 50% of drug-resistant tuberculosis cases can be cured in up to 2 years, also using second-generation drugs such as fluoroquinolones that cause severe adverse effects and have less predictable efficacy. 4 The sluggishness and relative inefficacy of the antitubercular therapy are associated with the inherent ability of the pathogen to generate phenotypic variants that better endure treatment, and with poor penetration of drugs into the sites of infection, conceivably enhancing the adaptive responses of the pathogen. 5
Microbes are known to employ a variety of strategies to circumvent the lethality of antimicrobials, spanning from transient phenotypic changes to stable genetic mutations. We refer to phenotypic drug persistence when a minority of cells happen to be in a particular phenotypic state, conducive to adaptation to inhibitory doses of drug but not genetically transmissible. This state can be associated with variation in the growth rate or in given cellular processes, which offer an adaptive advantage to the best-fit individuals. Cell-to-cell variation can either spontaneously arise from probabilistic sources or be induced by exogenous stimuli, such as nutrients sources, host defenses, intermittent exposure to suboptimal doses of drugs, and drug mechanism of action. As drug persistence is associated with phenotypic variation and largely multifactorial, its underlying dynamics still remain elusive.
Despite its complexity, bacterial drug persistence can be inferred from the mortality pattern of a cell population confronted with the drug, which consists of at least 2 phases. This biphasic mortality pattern starts with an initial phase of linear decay upon drug exposure, followed by a plateau, which indicates either a bacteriostatic effect or a balanced equilibrium between cell division and death. 6 Moreover, a cell population that resumes growth in the absence of drug pressure from a drug-persistent cell dies with a biphasic pattern similar to that experienced by the initial population, once the drug is reintroduced. The recurrence of a biphasic pattern of mortality over multiple generations of survivors is suggestive of phenotypic drug persistence and rules out the possibility of genetic-based drug resistance. Although drug persistence is not transmitted to the progeny as a genetic trait, the survival of drug-persistent cells offers a long-term propagation potential, wherein genetic mutations may progressively arise among survivors, favoring drug resistance in the community. 7
Unlike drug-resistant cells that continue to actively proliferate during exposure to inhibitory doses of drug, drug-persistent cells derive from individuals that experience behavioral alterations either before or after drug exposure, including but not limited to changes in the growth rate. The relation between the growth state and drug persistence constitutes a long-standing debate. Although growth and metabolic abeyance are usually associated with an enrichment in drug-persistent cells, several studies, including ours, have reported that drug persistence occurs under a broad spectrum of growth and metabolic states. 5 Furthermore, the growth rate can be considered as an indicator of physiological alterations happening in the cell, rather than the very source of these alterations. We and others have shown that alterations in different cellular processes derive from both intrinsic sources and from sensing physical events in the outside environment, enhancing the spectrum of behaviors of individual cells confronted with stressful conditions.5,6,8
For instance, injuries to DNA can arise from both endogenous and exogenous insults, against which bacterial cells deploy an arsenal of DNA repair systems. During genotoxic stress, drug exposure or starvation DNA can break, and the highly conserved DNA recombinase RecA forms nucleoprotein filaments with single-stranded DNA, triggering the SOS response by inducing proteolytic inactivation of LexA, the suppressor of the SOS regulon. 9 We have recently reported that intrinsic phenotypic variation in SOS DNA damage response is associated with differential drug susceptibility in mycobacterial subpopulations. 10 In particular, we did quantitative single-cell imaging of fluorescent reporter strains of RecA grown inside a microfluidic device, alternating between optimal growth conditions and fluoroquinolone exposure. Under optimal growth conditions, more than 50% of mycobacterial cells transiently express RecA as fluorescent pulses, which tend to resolve spontaneously, implying a stochastic source of DNA damage events. Interestingly, cells experiencing DNA damage events (RecA pulsing) are more susceptible to fluoroquinolone treatment, whereas healthier cells (RecA nonpulsing) are more likely to survive. Although, as with most single-cell scenarios, also the opposite events can happen, undue responses to DNA damage are generally detrimental for mycobacterial cells, especially if treated with a drug that exacerbates DNA damage. 10
Interestingly, RecA-pulsing cells are more likely to grow at slower rates, suggesting a putative mechanism of cell cycle inhibition, possibly to favor DNA repairing toward cell rescue. Checkpoints of cell cycle progression are critical during replication problems or DNA damage both in eukaryotes and prokaryotes. 9 For instance, SulA is a reversible inhibitor of the cell division machinery in Escherichia coli, whose activity is repressed by protease degradation to enable growth resumption. Genes encoding cell division inhibitors are often positioned close to lexA on the chromosome, and their product acts on the cell wall following initiation of the SOS response. This also applies to the putative cell wall hydrolase of M. tuberculosis Rv2719c, which is induced during the SOS response, localizes on the cell wall and might be a DNA damage checkpoint. 9 By contrast, if the DNA damage is irreversible, cell cycle inhibition is conducive to death. Indeed, we found that a fraction of mycobacterial cells experiencing severe DNA damage after fluoroquinolone treatment exhibit high RecA levels, filamentation, growth arrest, chromosomal fragmentation, and autolysis, followed by the release of nucleic acids in the proximal area (Figure 1). These events are reminiscent of programmed cell death (PCD), and consistent with previous findings in model microorganisms. 11 PCD is well described in eukaryotes, where it plays key functions in tissue morphogenesis and homeostasis, and immunity. 12 Likewise, prokaryotic cells, subject to particularly adverse events, can undergo PCD through mechanisms that closely resemble those occurring in eukaryotes. 11 For instance, bacteria subject to nutrient limitation, phage infection, or exposure to xenobiotic and genotoxic molecules, experience apoptotic-like processes, resulting in inhibition of cell division, chromosomal condensation and fragmentation, ribosomal RNA degradation, membrane depolarization, and remodeling up to death (Figure 2).11,13 Although PCD is less intuitive in unicellular organisms, it can be readily justified by picturing individual cells within heterogeneous communities engaged in cooperative behaviors, as with biofilms. 14 Community living provides protection from external onslaughts, conceivably enhancing single-cell persistence behaviors. In addition, PCD brings about DNA release (Figure 1), which in eukaryotes induces immune responses, and in prokaryotes not only provides structural and nutritional support to the community, but can also foster natural transformation events (Figure 2).12,13,15
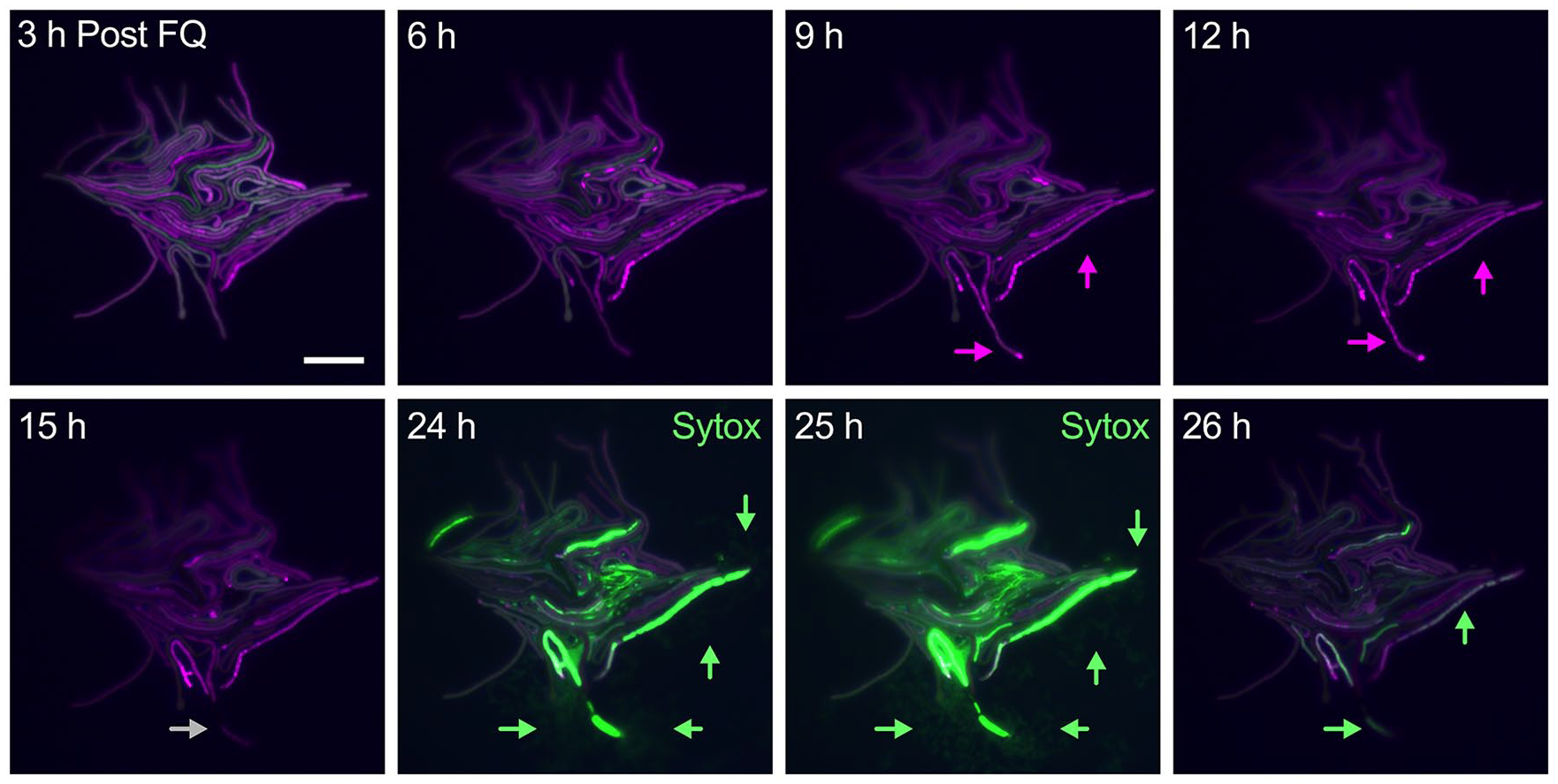
Severe DNA damage can lead Mycobacterium smegmatis cells to PCD and DNA release. Representative time-lapse microfluidic microscopy (n = 3) of a dual fluorescent reporter strain of recA transcription (green) and translation (magenta). 10 Individual cells were first grown in 7H9 medium until a microcolony was formed and challenged with ciprofloxacin 1 µg/mL (FQ). The image series show a microcolony during the period of FQ washout. Magenta arrows indicate cells having high RecA::mCherry levels and signs of DNA fragmentation. Gray arrow points to a cell that has undergone autolysis. After 24 hours of FQ washout, Sytox dye 0.5 µM was perfused to stain nucleic acids in permeabilized cells, and was revealed using the green fluorescence channel. Green arrows indicate strong permeation of Sytox into severely damaged cells, as well as the release of nucleic acids in the extracellular environment around them. GFP and mCherry fluorescence and phase contrast are merged. Scale bar, 10 µm. GFP, green fluorescent protein; PCD, programmed cell death.
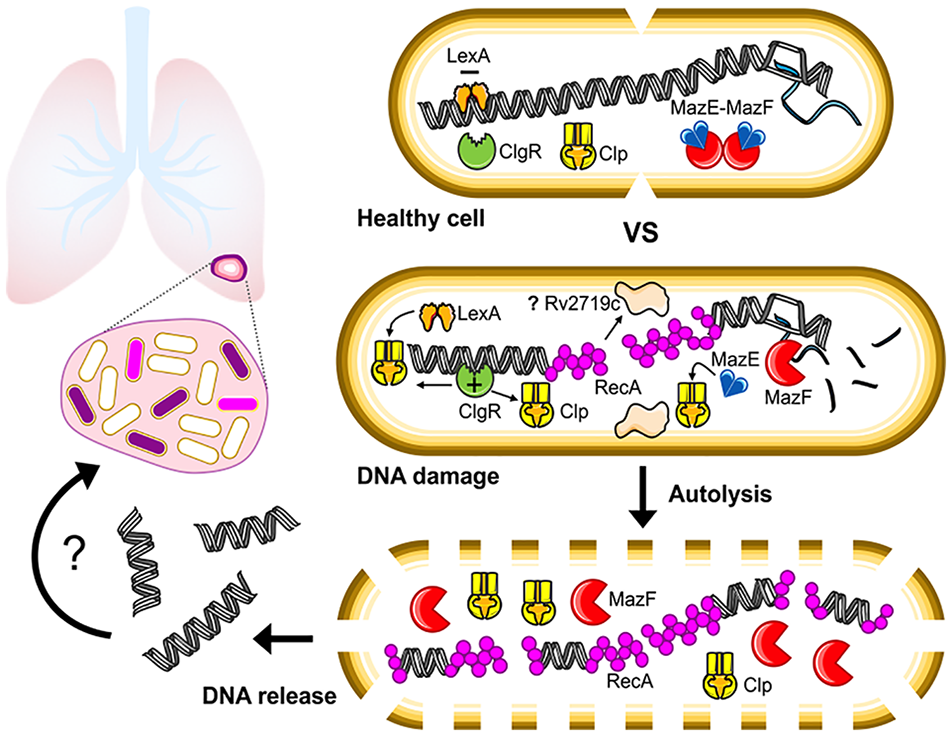
Schematic representation of the putative interaction between the SOS response and MazEF system and their implication in mycobacterial PCD. Clonal mycobacterial communities are subject to intrinsic phenotypic variation in DNA damage, which is also influenced by genotoxic agents present in the host microenvironments (top-left schematic). Different single-cell colors indicate RecA expression levels and reflect the extent of DNA damage response: no (white), moderate (purple), and high (magenta). In genetically healthy cells (upper-right schematic), the transcriptional factor LexA represses the SOS DNA damage response genes. DNA replication and transcription take place, and the antitoxin MazE nullifies the toxic activity of the toxin MazF. In cells experiencing severe DNA damage (middle-right schematic), the repressor LexA is released from the SOS box of the genes implicated in the SOS response, including recA, whose expression is also positively regulated by ClgR. ClgR also induces the expression of Clp proteases, which are conceivably responsible for the degradation of LexA and MazE dimers. Once the SOS response has been triggered, the toxin MazF can start to degrade the cell mRNA, affecting protein synthesis and replication. Proteins acting on the cell wall, such as the hydrolase Rv2719c, might also interfere with cell division. If the cell is unable to repair the DNA damage (lower-right schematic), RecA foci increase throughout the chromosome, whose integrity is severely impaired by fragmentation. The levels of Clp protease and MazF toxin increase, the bacterial cell wall undergoes structural modifications and no longer functions as a barrier, leading the cell to autolysis and to release its DNA into the surrounding environment. The genetic material disseminated from the dying cell could serve as a source of nutrients and stability for the mycobacterial community and might be transferred to some recipient cells.
Different modes for PCD have been reported in bacteria and their common denominator is DNA damage; however, many facets remain cryptic. 13 The SOS response is at the crossroads of cell survival and death, depending on the damage severity, and the cell promptness to restrain its own metabolism pending recovery from damage. In prokaryotes, there may be sensors of the magnitude of cellular damage, analogous to the transcriptional regulator p53 in eukaryotes. 11 Both LexA and toxin-antitoxin systems (TA) could play this role, influencing the directionality of the SOS response toward life or a death sentence, similar to autophagy in eukaryotes (Figure 2).
TA systems are genetic modules broadly spread in prokaryotes, usually associated with stress response mechanisms, growth inhibition, and PCD. In short, toxins target essential cellular processes and antitoxins interact with their cognate toxin, neutralizing its toxic effects. Usually toxins are nucleases that interfere with different steps of gene expression. 16 There are 4 major TA families, but type II, where both toxin and antitoxin are proteins expressed from the same promoter, is highly represented particularly in mycobacteria. The abundance of TA systems in M. tuberculosis raised questions about their implication in pathogenesis, quiescence, and persistence. However, their actual biological functions remain poorly understood. 5 The MazEF TA system is highly conserved in prokaryotes and is the second largest group in M. tuberculosis, whose genome encodes 10 MazEF systems, which are differentially induced under several in vitro and host-related stressful conditions. 17 MazF toxin is a stable sequence-specific RNA interferase that ultimately affects protein synthesis. M. tuberculosis also secretes MazF in the host, inducing inflammation. 17 In contrast, MazE antitoxin is extremely labile but continuously synthesized in growing cells, to impede MazF from exerting its noxious effect. Although this control system may not seem cost-effective for a healthy cell, it becomes beneficial once the cell is threatened, as the antitoxin MazE is rapidly degraded by cellular proteases, such those from the Clp family, causing bacteriostasis and enabling the cell to cope with the hazard. 16
Interestingly, mycobacterial recA is repressed by LexA and positively regulated by ClgR, which is also a transcriptional activator of the Clp proteases. 10 As a consequence, during DNA damage, Clp proteases may not only contribute to the degradation of LexA, promoting the SOS response, but also degrade MazE leading to MazF-mediated bacteriostasis. Both the SOS response and the MazEF system have been described as PCD mechanisms, also having a possible interaction contingent on the extent of DNA damage (Figure 2). 13 Although deeper understanding of PCD in bacteria, especially in mycobacteria, is needed, the very fact that both the SOS response and MazEF are broadly conserved across species corroborates their physiological relevance. Now we need to clarify the drivers of PCD and the effects on the community, and what sets the boundaries between cell survival, persistence, and death.
Inspired by the existing knowledge on bacterial PCD and the likely implication of TA systems, we have started to address this subject in mycobacteria. We measured the levels of expression of different mycobacterial proteases during starvation and after exposure to antitubercular drugs and found that they are induced and positively correlate with the toxin MazF but inversely correlate with the antitoxin MazE in the fast-growing tuberculosis model Mycobacterium smegmatis (Figure 3A), consistent with model species.11,13 Furthermore, we performed time-lapse microfluidic microscopy and single-cell analysis of a dual fluorescent reporter strain of MazF and ClpP1P2 in M. smegmatis, treated with a frontline antitubercular drug (Figure 3B). Interestingly, individual cells experiencing autolysis express higher MazF toxin levels just before dying, whereas cells that are going to survive and resume growth during drug washout exhibit lower levels of toxin (Figure 3C). Not surprisingly, MazF::mCherry and ClpP1P2::GFP were positively correlated also at the single-cell level consistent with our bulk-cell measurements (Figure 3A). Our pilot study suggests that the intracellular levels of MazF toxin might contribute to single-cell decision-making between life and death. Next, we shall further probe the implication of the SOS response in determining single-cell fate, the alleged interaction between growth slowdown in RecA-pulsing cells, MazF levels, and PCD, and whether the single-cell behavior is stress-specific or other factors, such as cell age, phenotypic variation, and cell-to-cell interaction could also govern PCD mechanisms.
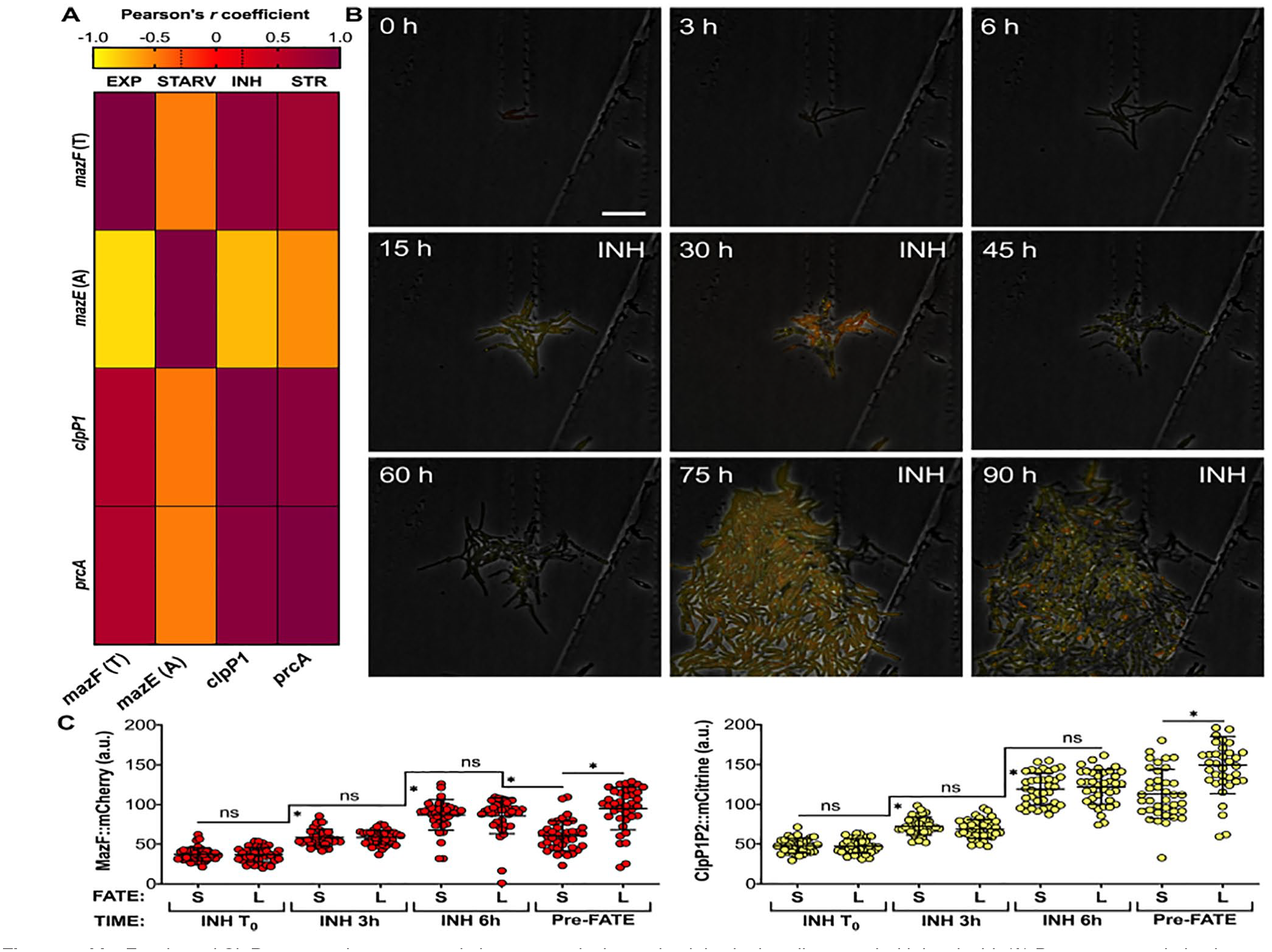
MazF toxin and ClpP protease hyperaccumulation are conducive to death in single cells treated with isoniazid. (A) Pearson r correlation between mRNA expression levels of the toxin MazF, the antitoxin MazE, and the proteases ClpP1 and PrcA, in exponentially growing M. smegmatis cells (EXP), in cells starved with HdB medium (STARV), and stressed with either 50 μg/mL isoniazid (INH) or 1.25 μg/mL streptomycin (STR), equal to 10-fold the minimum inhibitory concentration (10X-MIC). The color in each cell represents the Pearson r value for each correlation pair, averaged among different time points (0, 3, 6, and 24 hours) (n = 3). The genes and the conditions examined are indicated. In the gradient scale, values close to −1 (yellow) indicate negative correlation, values close to 1 (red-purple) indicate positive correlation, significance thresholds are indicated by dotted lines, and values close to 0 are not significant. (B) Representative time-lapse microfluidic microscopy (n = 2) of a dual fluorescent reporter strain of M. smegmatis, expressing MazF fused to a red fluorescent protein and ClpP1P2 fused to a yellow fluorescent protein. Individual cells were grown in 7H9 medium until a microcolony was formed and then challenged twice with isoniazid 50 µg/mL (10X-MIC). Phase contrast, red and yellow fluorescence are merged. Scale bar, 10 μm. (C) Single-cell MazF::mCherry (left panel) and ClpP1P2::mCitrine (right panel) fluorescence of a subpopulation that survived (S) and a subpopulation that lysed (L), monitored at 0, 3, and 6 hours after INH treatment and the frame before growth resumption or lysis (Pre-FATE). Significance by 2-way ANOVA followed by Tukey multiple comparisons test, *P < .0001 (n = 114 single cells, from 2 independent experiments). ANOVA indicates analysis of variance; mRNA, messenger RNA.
It stands to reason that if the life of an individual cell is jeopardized, an intricate intracellular signaling network to prevent death, as well as an extracellular network in an attempt to warn neighboring cells of the threat, should take place. However, if death is unavoidable, the cell can take advantage of the last gesture of sacrifice to spread its own genetic material in the environment. We can assume that the gesture of suicide of an individual cell, typically surrounded by its direct kin and belonging to a larger community (microcolony), has both altruistic and selfish implications, such that the self-sacrificing cell not only provides support to its kin, reminiscent of kin selection, 14 but also ensures the preservation of its own genetic material within the community (Figure 2). 12 It is worth mentioning that horizontal transfer of chromosomal DNA has been demonstrated in some mycobacterial species, 15 and that mycobacteria can generate biofilm-like structures in vitro, during redox stress or in the presence of host-cell debris. 18 However, the formation, homeostasis, and effects of M. tuberculosis biofilm in vivo remain open to investigation. In the future, it will be important to examine whether the typical aggregates formed by M. tuberculosis both in vitro and in vivo, enable kin recognition, 14 cell-to-cell communication via a specific molecular lexicon, and transfer of genetic material ultimately favoring the community as a whole.
In conclusion, quantitative analysis of single cells at high spatiotemporal resolution, by time-lapse microfluidic microscopy, is helping to reveal the spectrum of behaviors of clonal bacterial communities under threat.5,8 Improved understanding of the single-cell dynamics of life versus death may enable artificial manipulation of PCD mechanisms, causing an imbalance in the community’s homeostasis. For persistent pathogens, such as M. tuberculosis, this may entail reduced adaptive capacity, enhanced drug lethality, and better control of the tuberculosis pandemic.
Footnotes
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: G.M. was supported by the French National Research Agency (ANR-17-CE11-0007-01); the French Government’s Investments for the future (ANR-10-LABX-62-IBEID), and by the Institut Pasteur.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
LBT performed the experiments, data analysis and contributed to manuscript preparation. GM conceived and made some experiments, wrote, and prepared the manuscript.
