Abstract
This review summarizes the literature on inhaled amphotericin B for invasive aspergillosis prophylaxis in patients with neutropenia secondary to hematologic malignancy treatment or stem cell transplant. Six trials, 2 randomized controlled and 4 with historical controls, were identified. Three inhaled amphotericin B deoxycholate trials found a reduced invasive aspergillosis incidence, 1 reaching statistical significance. Three inhaled liposomal amphotericin B trials demonstrated similar reductions with 2 finding statistical significance. Relative risk reductions for invasive aspergillosis were routinely 40-60%. Both formulations were without reported systemic or severe adverse effects. The most common adverse events were cough, bad taste, and nausea. Discontinuation rates ranged from 0-45%. The only randomized, placebo-controlled trial utilized inhaled liposomal amphotericin B reported a nearly 60% relative risk reduction.
Inhaled liposomal amphotericin B 12.5 mg twice weekly is an alternative for invasive aspergillosis prophylaxis in high risk neutropenic patients with hematologic malignancies and stem cell transplant recipients when recommended azole agents are contraindicated or should not be used.
Introduction
Aspergillus infections cause substantial morbidity and mortality in immunocompromised populations. Aspergillus is a common environmental mold, with the primary exposure route being spore inhalation. 1 Recent studies found 10% of patients with hematologic malignancies will develop a life-threatening invasive aspergillosis (IA) infection during treatment with fatality rates approaching 29%. 2 Neutropenic patients with IA infections are estimated to incur an additional US$36,000 to US$59,000 in hospital costs. 3 Risk of IA is elevated in immunocompromised patients with prolonged neutropenia (>7 days). 1 Invasive pulmonary aspergillosis (IPA) infection rates are increased in patients undergoing allogeneic stem cell transplant (SCT) secondary to extended periods of immunosuppression via therapies to prevent and treat Graft vs Host Disease (GvHD). 1 The incidence of IPA is particularly prevalent during neutropenic episodes associated with first induction chemotherapy in acute myeloid leukemia (AML) patients. Invasive pulmonary aspergillosis risk is also increased in patients with refractory and relapsing acute leukemia undergoing re-induction chemotherapy regimens. Preventing IPA in leukemia patients avoids delays in subsequent chemotherapy treatment.1,4
The American Society of Clinical Oncology and Infectious Diseases Society of America (IDSA) Clinical Practice Guideline update recommends prophylaxis with mold-active oral triazole (posaconazole, voriconazole, and isavuconazole) or a parenteral echinocandin in patients experiencing extended periods of neutropenia and at >6% risk for IA. 5 High-efficiency particulate air (HEPA) filtration is also recommended to reduce environmental exposure to mold. 1 Intravenous amphotericin B (AmB), deoxycholate and lipid-based formulations, has a broad spectrum of activity including Aspergillus fumigatus and Aspergillus flavus.6,7 Intravenous liposomal amphotericin B has prophylactic efficacy approaching that of voriconazole use 8 ; however, systemic AmB is associated with severe adverse effects including nephrotoxicity, hepatotoxicity, infusion-related reactions, and electrolyte imbalances limiting its role in prophylaxis.6,7 An in vitro study found that a jet nebulizer deposits liposomal AmB particles of similar sizes and in similar locations as Aspergillus spores in the lungs. Nebulizing either deoxycholate or liposomal AmB results in pulmonary drug concentrations sufficient to inhibit Aspergillus growth with minimal systemic effects. 9
A prior review in 2006 reported insufficient data to make a definitive recommendation for inhaled AmB (InAmB) use in hematologic disease based on the data then available. 10 Controlled trials evaluating the use of InAmB prophylaxis in patients with prolonged neutropenia secondary to hematologic malignancies treatments are reviewed.
Literature Search
The literature search was completed using Ovid Medline® (1946-November 2018). The search terms used were amphotericin B, aerosolized, aspergillosis, and prophylaxis. A bibliography search of reviewed full text articles was conducted to identify additional trials. Inclusion criteria were prophylactic use of InAmB, neutropenia secondary to hematologic conditions, English language, and controlled trials in humans. Figure 1 depicts the manual selection process for identifying qualifying trials. Six qualifying trials were identified (Table 1).11-16
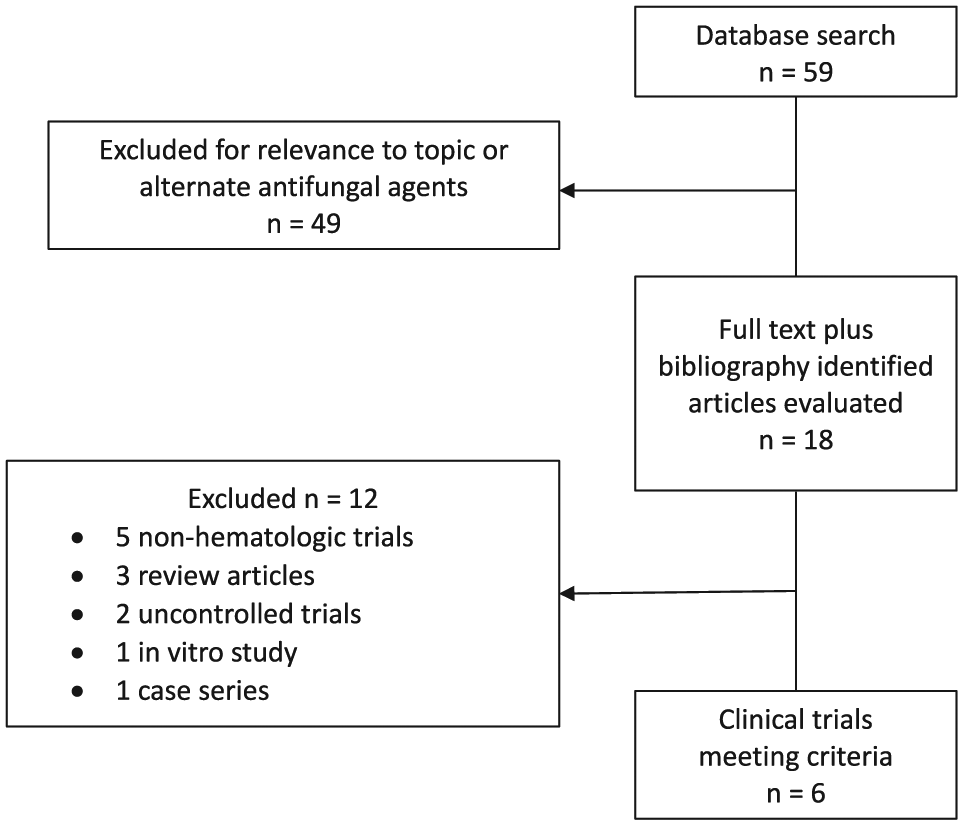
Summary of study selection.
Clinical Trials for Prophylactic Nebulized Amphotericin B.
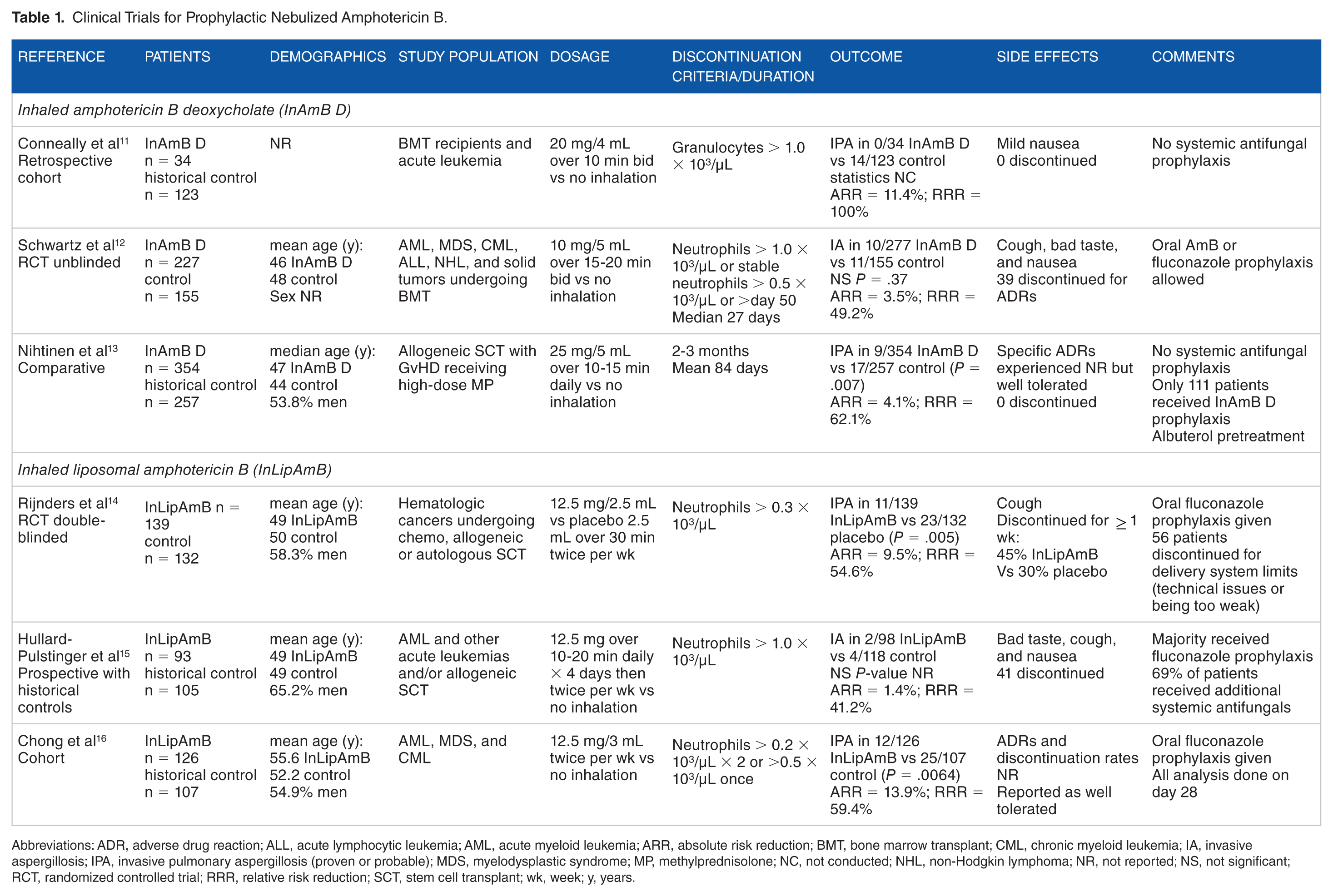
Abbreviations: ADR, adverse drug reaction; ALL, acute lymphocytic leukemia; AML, acute myeloid leukemia; ARR, absolute risk reduction; BMT, bone marrow transplant; CML, chronic myeloid leukemia; IA, invasive aspergillosis; IPA, invasive pulmonary aspergillosis (proven or probable); MDS, myelodysplastic syndrome; MP, methylprednisolone; NC, not conducted; NHL, non-Hodgkin lymphoma; NR, not reported; NS, not significant; RCT, randomized controlled trial; RRR, relative risk reduction; SCT, stem cell transplant; wk, week; y, years.
Results
Amphotericin B deoxycholate
Conneally et al 11 conducted a retrospective cohort study after instituting a prophylactic inhaled amphotericin B deoxycholate (InAmB D) protocol for persistent granulocytopenia. Subjects from the first 12 months (24 patients) following InAmB D initiation were compared with historical controls from the preceding 24 months (123 patients). Evaluated patients included those with acute leukemia, aplastic anemia, solid tumors, lymphoma, or bone marrow transplant (BMT) recipients with granulocytopenia (<0.5 × 103/µL) persisting for >10 days. Patient demographics were not delineated. The Cirrus nebulizer with a Pall Ultipor filter was used to administer InAmB D 5 mg in 3 mL 5% dextrose over 10 minutes twice daily. Patients received this regimen until their granulocyte count recovered to >1.0 × 103/µL.
IPA occurred in 11.4% of the historical control group, whereas no patients experienced IPA in the InAmB D group. Statistical analysis was not conducted, but numerical results favored InAmB D. Secondary analysis found no patient in either group experienced IPA while being cared for in a HEPA filtration room. Mild nausea was the most common adverse event reported, but no patient required InAmB D discontinuation. 11 Strengths include the use of a control group. Limitations included single-center, retrospective study design, lack of statistical analysis, and presence of several confounders including treatment advances not available in the historical control group and inconsistent use of HEPA filtration.
Schwartz et al 12 performed an unblinded, prospective, randomized, multi-center, controlled trial in patients ⩾18 years of age to study the efficacy of InAmB D in neutropenia (<0.5 × 103/µL) anticipated to last >10 days. The InAmB D group (227 patients) was compared with a control group (155 patients) who received no InAmB D. Patients were stratified by center and disease state: AML, myelodysplastic syndrome (MDS), and chronic myeloid leukemia (CML); acute lymphocytic leukemia (ALL) and relapsed non-Hodgkin lymphoma (NHL); and solid tumors undergoing BMT. Patients were randomized in a 13:10 ratio to account for an anticipated 30% dropout in the InAmB D group. Nebulizers used were the RespirGard II, PariBoy, or Pari IS II. Prophylactic InAmB D was administered as 10 mg in 5 mL sterile water over 15 to 20 minutes twice daily beginning with chemotherapy administration. Oral AmB and/or oral fluconazole was allowed for Candida infection prophylaxis. The InAmB D regimen was continued until neutrophil recovery (count > 1.0 × 103/µL), 50 days of treatment, stable neutrophil count in patients whose count never got below 0.5 × 103/µL, or death during the trial. The primary endpoint was proven, probable, or possible IA.
Proven, probable, or possible IA occurred in 7% of control patients and 4% of the InAmB D patients (P = .37). The overall incidence of IA (5%) was lower than anticipated (10%), resulting in inadequate power to identify a difference. Half of the IA cases in the InAmB D group occurred between 5 and 29 days after patients prematurely stopped prophylaxis. Per protocol analysis also failed to demonstrate a statistically significant difference (P = .27). Early discontinuation of InAmB D occurred in 31% of patients, following 6 days (median) of therapy, consistent with enrollment predictions. No systemic adverse effects were detected although mild cough, bad taste, and nausea were reported, leading to 39 patient discontinuations and accounting for 55% of all early terminations. Adverse effects in the control group were not reported. 12
Strengths include randomization, stratification by center and disease states, and intent-to-treat analysis. All patients were cared for in similar units, without HEPA filtration. Limitations of the study include no blinded adjudication of IA outcomes, no inhaled placebo control group, and being underpowered.
Nihtinen et al 13 conducted a retrospective, comparative review in patients who had received allogeneic SCT at a single center. Patients undergoing allogeneic SCT from 1996 to 2000 were not treated prophylactically with InAmB D and served as the control group (257 patients). During 2001-2005, 354 patients were included in the comparator group. The evaluated population included several hematologic malignancies (AML, ALL, CML, multiple myeloma, MDS, NHL) with CML (29.2%) being the most common in the control group and AML (27.2%) in the InAmB D group. Prophylactic InAmB D was only administered to the 111 patients experiencing acute GvHD and who received high-dose methylprednisolone (10 mg/kg) therapy for 2 to 3 months. Statistical analysis was performed comparing the 257 control group patients with the entire 354 patients identified from 2001 to 2005. No systemic prophylactic antifungals were used in either group. The type or model of nebulizer used was not reported. The dose was 25 mg in 5 mL sterile water inhaled over 10 to 15 minutes once daily. Patients were pretreated with 1 to 2 doses of inhaled albuterol. The primary endpoint was cumulative incidence of proven or probable IA as determined by the European Organization for Research and the Treatment of Cancer–Mycoses Study Group (EORTC-MSG) criteria. 17
Proven or probable IA occurred in 6.6% of control patients vs 2.5% of InAmB D (P = .007). Even though only 111 of 354 of patients received prophylactic InAmB D, a >60% relative risk reduction (RRR) in the IA incidence was observed. InAmB D delayed initial diagnosis of IPA from 95 to 155 days posttransplant in the historical control vs InAmB D groups. The authors reported inhalations were well tolerated with no discontinuations due to adverse effects. No specific adverse reactions were reported. 13
Overall health of patients was better in the intervention than in the control group, possibly due to a shift from CML to AML or medical advances occurring between comparison periods. Strengths include administering InAmB D to a select high-risk population, consistent use of HEPA filtration rooms, and a large sample size. Limitations include the retrospective study design, shift in the predominant population, 69% of patients in the intervention group did not receive InAmB D prophylaxis, statistical analysis was performed on the entire 354 patients in the 2001-2005 group, and potential for medical advances to influence study outcomes.
Liposomal amphotericin B
Rijnders et al 14 completed a randomized, double-blind, placebo-controlled trial of inhaled liposomal amphotericin B (InLipAmB) during neutropenia in 139 intervention and 132 control patients with hematologic malignancies. Patients were stratified by SCT and use of HEPA filtration rooms. Patients beginning chemotherapy with an anticipated neutropenia (<0.5 × 103/µL) duration of >10 days or starting chemotherapy for allogeneic or autologous SCT were enrolled. All patients received prophylactic fluconazole orally. Nebulizers used were Halolite and ProDose adaptive aerosol jet nebulizer systems. Patients received AmB 12.5 mg in 2.5 mL or placebo inhaled over 30 minutes daily for 2 consecutive days weekly. Prophylaxis continued until neutrophil recovery (count > 0.3 × 103/µL) or 12 treatment doses. Patients could receive additional courses for subsequent occurrences of neutropenia. The primary endpoint was proven or probable IPA infection as determined by the EORTC-MSG criteria. 17
Proven or probable IPA developed in 14% of placebo and 4% of InLipAmB patients in the intent-to-treat population (P = .005), with similar findings in the per protocol population (P = .007). There were no serious adverse reactions reported. Cough as the reason for discontinuation was reported by 11.5% of the InLipAmB vs <1% in the placebo group (P = .002). The number of patients permanently discontinuing was not reported. Over a third of all study patients discontinued therapy for at least 1 week during treatment, with most patient discontinuations being for weakness or a technical problem with the nebulizer. 14
Strengths were prospective study design including a matched placebo group, and statistical analysis of intent-to-treat and per protocol groups. Limitations include single center, early study termination for slow enrollment, lower threshold criteria for neutropenia resolution, and high rate of administration difficulties.
Hullard-Pulstinger et al 15 conducted a prospective, non-randomized, open-label, phase II trial to determine efficacy and safety of InLipAmB (93 patients) in the setting of persistent neutropenia vs untreated historical controls (105 patients). Patients with anticipated neutropenia (<0.5 × 103/µL) for >10 days due to induction/consolidation chemotherapy for acute leukemias and/or allogeneic SCT were included. Most (100/201) of the patients had de novo AML. The devices used were jet stream nebulizers. The InLipAmB dose was 12.5 mg in 3.125 mL distilled water over 10 to 20 minutes on 4 consecutive days and then twice weekly until neutrophil recovery (>1.0 × 103/µL). The primary endpoints were toxicity and reduction of proven or probable IPA.
The incidence of proven or probable IPA was 3.4% in historical controls and 2% in the InLipAmB group. Statistical analysis was not reported for the primary outcome. Systemic antifungal therapy was common, 65% in the control group and 70% in InLipAmB group. Per protocol prophylaxis patients had a 63% lower systemic antifungal use than controls. Ten enrolled patients never received a nebulization treatment, although all eventually received systemic antifungal therapy. Ultimately, 41 patients (44%) discontinued InLipAmB early or refused treatment (13 patients) during subsequent chemotherapy courses. Forty-two patients (41.7%) reported therapy as unpleasant or very unpleasant (2 patients). No systemic adverse reactions were reported; most common complaints were bad taste, cough, and nausea. Patients adhering to the protocol received a mean of 43.6 days of treatment, whereas those discontinuing early received a mean of 26.7 days. 15
Strengths include the use of a control group and prospective safety evaluation. Limitations include the open-label study design, no IPA statistical analysis reported, and confounding factors such as medical advances that may have occurred when using historical controls.
Chong et al 16 conducted a prospective cohort study to evaluate efficacy and cost efficiency of InLipAmB in neutropenic patients (126 patients) vs historical controls (107 patients). The evaluated population consisted of patients with newly diagnosed or relapsed AML, MDS, or CML. The most common diagnosis was AML, 83.3% in the control and 89% in the InLipAmB group. The ProDose and Akita® adaptive aerosol delivery (AAD) nebulizers were used in the trial; both are adaptive aerosol jet nebulizer systems. All patients received prophylactic oral fluconazole. Intervention patients received InLipAmB 12.5 mg in 3 mL twice a week coinciding with the first chemotherapy cycle. Prophylaxis continued until neutrophil recovery defined as 2 consecutive counts >0.2 × 103/µL or 1 count >0.5 × 103/µL. The primary endpoint was incidence of proven or probable IPA during the first and second chemotherapy cycles (28 days total).
IPA occurred in 23.4% of historical control patients and 9.5% of InLipAmB patients (P = .0064). Systemic antifungal therapy usage was reduced from 49.5% in the historical control group to 27% in the InLipAmB prophylaxis group. An accompanying analysis determined that the prophylactic costs of InLipAmB were more than recovered by reductions in diagnostic and systemic antifungal therapy costs. No serious adverse reactions related to InLipAmB were reported. Therapy discontinuation rates were not reported. 16
Strengths include use of a control group and cost analysis. Limitations include single center, no randomization, unblinded, no placebo control, high IPA incidence, and lower neutrophil endpoints. Medical advancements since the controls were treated and no reporting of discontinuation data or adverse event rates are potential confounding variables.
Discussion
Six InAmB Aspergillus prophylaxis trials in immunocompromised patients secondary to treatment of hematologic malignancies or SCT were evaluated. In total, 879 control patients were compared with 973 patients who received InAmB.11-16 Two trials were prospective, randomized, and controlled,12,14 whereas 4 trials employed historical controls.11,13,15,16 Four studies included a mixture of SCT recipients and/or hematologic malignancy patients,11,12,14,15 whereas the single studies included allogeneic SCT recipients receiving high-dose steroids for GvHD, 13 or patients with hematologic malignancies without SCT. 16 The primary endpoint for all of the trials was proven or probable IPA or IA incidence. One study also included possible IPA, but the rates were low enough to not impact the overall results (1 patient in both the control and InAmB D groups). 12 Dosing regimens ranged from 10 to 25 mg/day for InAmB D patients vs InLipAmB 12.5 mg twice per week, with or without an initiation phase. Different nebulizers were used in the trials, but all were jet type, which should limit appreciable effect on the results. Criteria for diagnosis IA or IPA varied, with the EORTC-MSG criteria (3/6 studies), used most commonly.13,14,16 All trials required histologic evidence for proven infection.11-16 A total of 3 trials, 1 InAmB D 13 and 2 InLipAmB, identified statistical significance in favor of InAmB prophylaxis.14,16 Two historically controlled trials failed to report a statistical analysis on IA incidence limiting their use in this analysis.11,15
Overall IPA incidence was highest in Rijnders et al 14 (4% InLipAmB vs 14% control) and Chong et al 16 (9.5% InLipAmB vs 23.4% control), both were conducted in the same center in the Netherlands. The higher IPA rate may be attributed to the more rigorous surveillance and diagnostic testing used compared with other studies, ie, EORTC-MSG criteria in addition to high-resolution computed tomography for abnormal chest X-ray or day 5 of unexplained fever.13,16 The IA incidence varied in the other studies from 0% to 4% of the InAmB population vs 3.4% to 11.4% of controls.11-13,15 Relative risk reduction ranged from 49% to 100% in the InAmB D trials. The 100% RRR occurring in a historically controlled trial with only 34 patients receiving prophylaxis and no formal statistical analysis. 11 In the InLipAmB trials, there was an RRR of 41%-59%.14-16
Efficacy was the primary focus of the studies; however, the adverse effect profile is also important when considering InAmB for clinical practice. The most common InAmB adverse events were cough, bad taste, and nausea. There were no reports of any severe or systemic adverse events. A prior evaluation of InAmB D tolerability using 10 mg 3 times daily demonstrated a greater incidence of adverse effects with >50% intolerant to the initial regimen. 18 Increased age and chronic obstructive pulmonary disease correlated with greater intolerance to InAmB D. 18 A subset of 77 patients in the Rijnders trial were enrolled in a protocol to evaluate the impact of InLipAmB on pulmonary function. 11 No significant decline in pulmonary function was noted in 68% of InLipAmB vs 79% of placebo patients (P = .2) though a higher cough incidence was noted, 74% vs 26% (P < .0001), respectively. 19 No studies reported systemic adverse effects.11-16,18-20 Albuterol pretreatment was used in 2 trials to reduce pulmonary adverse reactions, but the impact of this intervention is unclear.15,20 Anywhere from 0% to 45% of patients discontinued InAmB prophylactic treatment for at least 1 week of therapy: InAmB D (0%-31%) and InLipAmB (0%-45%). Adverse effects accounted for approximately half of the discontinuations in the trials that reported discontinuation reasons.12,14 In the randomized trials, 45% of the discontinuations were from non-compliance or protocol violations in Schwartz et al 12 compared with 37% for weakness or technical issues with the nebulizer in Rijnders et al. 14 The InAmB D regimens administered once or twice daily vs the twice weekly dosing for InLipAmB may contribute to differences in protocol/non-compliance discontinuations. This is supported by a prior InAmB D tolerance study in which 52% of patients required a dose decrease or therapy discontinuation. 18
A recent meta-analysis of invasive fungal infections prophylaxis in hematologic disease 8 supports current IDSA guidelines listing posaconazole and voriconazole as the recommended prophylaxis agents for IPA. 5 Posaconazole was shown to be the most effective and is recommended in SCT patients with GvHD. 8 Early posaconazole trials helped establish mold-active triazoles as first line therapy for IA prophylaxis.21,22 A posaconazole in severe GvHD trial did not significantly reduce invasive fungal infections compared with fluconazole, 5.3% vs 9% (P = .07), but in a secondary analysis, it was superior for reducing proven or probable IA, 2.4% vs 7.6% (P = .004). 21 The reported frequency of discontinuation for adverse effects was similar at 34% for posaconazole and 38% for fluconazole. The overall treatment discontinuation rate was higher with 54% of posaconazole and 59% of fluconazole patients not completing 16 weeks of treatment. 21 An additional posaconazole trial in neutropenic patients demonstrated a reduction in proven or probable invasive fungal infections when compared with control fluconazole or itraconazole, 2% vs 8%, respectively (P < .001). 22 The IA infection rate analysis revealed a similar beneficial effect at 1% and 7% (P < .001). Discontinuation rates for adverse events were 8% in each group, and overall discontinuation rates were 11% for posaconazole and 9% for the control group. 22 These findings are consistent with the 2 randomized trials conducted with InAmB.12,14 Mold-active oral triazoles represent a more rigorously studied and convenient IA prophylaxis choice.
Aspergillus resistance to azole drugs including posaconazole is a growing concern. Resistance develops with prolonged exposure and is a risk in patients with chronic pulmonary aspergillosis due to the lengthy duration of therapy. 23 In addition, environmental exposure to azoles used as fungicides for crops is a known cause of increasing resistance. 23 Antifungal Susceptibility Testing (AFST) can be used to identify resistant strains of Aspergillus. Resistance in the United States is currently low; however, in Europe, it is prevalent enough that AFST is routinely recommended for voriconazole therapy. 1 Azole-resistant strains of Aspergillus have already become prevalent in the Netherlands and are documented to have spread through Europe and parts of Asia as well. 24 All 6 reviewed trials were conducted in European countries.11-16 Completely avoiding prophylactic azole use is not possible, because InAmB is a locally acting agent that protects against inhaled Aspergillus spores but provides no systemic prophylaxis against Candida. Fluconazole has little activity against Aspergillus and is not sufficient for IA/IPA prophylaxis. In total, 4 of 6 reviewed trials used or allowed patients to use fluconazole as Candida prophylaxis in addition to the InAmB.12,14-16 There was no obvious trend in outcomes based on fluconazole usage. With azole resistance on the rise, it would be advantageous to have an alternative strategy for prophylaxis such as InAmB. No prophylactic IA studies have been conducted to date comparing InAmB with posaconazole, isavuconazole, or voriconazole.
Azole antifungal agents are substrates and inhibitors of the cytochrome P450 enzyme system, particularly 3A4 and 2C19 isoenzymes, and inhibit permeability glycoprotein membrane transporter. 1 This results in clinically significant drug interactions with agents such as vinca alkaloids, cyclophosphamide, cyclosporine, tacrolimus, sirolumus, and tyrosine kinase inhibitors. The IDSA guidelines strongly recommend against co-administration of azoles with agents known to potentially result in toxic levels when combined. Although usually well tolerated, azoles may cause hepatotoxicity, neurotoxicity, dermatological problems, and QTc interval prolongation. Trough serum concentrations of all IPA prophylactic azoles are recommended for patients receiving prolonged courses or interacting agents. Echinocandins are recommended as alternatives to azole antifungals for IA prophylaxis. Echinocandins are generally well tolerated and associated with fewer serious drug interactions than azole antifungals, but require daily intravenous administration. 1
The 2016 IDSA Aspergillosis guidelines recommend InLipAmB over InAmB D, but do not recommend a regimen. 1 The 2017 European Society of Clinical Microbiology and Infectious Diseases Aspergillus diagnosis and management guidelines do not include a recommendation for InAmB prophylaxis for patients with hematologic conditions. 25 The guidelines do assign a level A recommendation for InLipAmB prophylaxis in lung transplant patients and a level C recommendation in heart transplant patients based on a level I quality of evidence scores. 25 InAmB is not associated with significant systemic adverse reactions or drug interactions. Although tolerability related to local reactions; bad taste, cough, and nausea combined with technical issues may limit its use. 14 InAmB may be an option for IPA prophylaxis in patients with hematologic malignancies and SCT recipients in areas of high azole resistance or with contraindications to IPA prophylactic azole therapy. InLipAmB regimens are preferred over InAmB D that requires more frequent administration and has been associated with more adverse events. 25 InLipAmB 12.5 mg twice weekly should be the preferred regimen as it has the most supporting evidence in hematologic neutropenic patients and was the regimen used in the only randomized, placebo-controlled double-blind trial. 14 There are currently no ongoing trials registered with The European Union Clinical Trials Register or clinicaltrials.gov evaluating InAmB in hematologic patients, but studies continue in lung transplant recipients, which will provide further safety and tolerability data.
Relevance to Patient Care and Clinical Practice
In the last 10 years, 3 trials have been conducted which met inclusion criteria for the review. One trial was a retrospective comparative review evaluating 111 allogeneic SCT patients with GvHD who received InAmB D prophylaxis. This trial found a statistically significant difference in favor of InAmB D for prophylaxis with 0 patients discontinuing for adverse effects. 13 These results were more favorable, 62.1% RRR vs 49.2% RRR than observed in Schwartz et al 12 which was a larger randomized trial but failed to reach statistical significance. Two trials; 1 prospective non-randomized, open-label, phase II trial 15 and 1 prospective cohort trial 16 evaluated the use of InLipAmB in patients with various hematologic malignancies with and without SCT. In these trials, 14 of 219 patients experienced IA or IPA compared with 29 of 225 in the control groups. Patients in the Hullard-Pulstinger et al 15 trial experienced a low overall incidence of IA, which likely influenced its ability to identify statistical significance, whereas Chong et al 16 reported statistically significant efficacy rates comparable with those of Rijnders et al. 14 The relative risk reductions for all 3 ranged between 41.2% and 62.1%.15,16 Discontinuation rates, when reported, were also similar to Rijnders et al. 14 There have not been any trials conducted directly comparing InAmB D with InLipAmB for safety and efficacy. However, in the trials published in the past 10 years, the InLipAmB dosing regimens were twice weekly compared with once daily in the InAmB D study. Further studies need to be conducted to evaluate whether this regimen increases patient compliance.
Overall, high-quality data on InAmB for IA prophylaxis is limited to only 2 randomized controlled trials with conflicting efficacy conclusions.12,14 No comparative trials have been conducted using InAmB and currently recommended azole therapies. Evidence does not support its routine use in patients able to receive recommended therapies.
Summary
IPA has high mortality rates, is difficult to treat, and complicates chemotherapy treatment in patients with hematologic malignancies and/or SCT. InAmB should not be considered a first line for IPA prophylaxis; however, it may be an appropriate option in patients when azoles are contraindicated secondary drug interactions, toxicity, or in areas with high rates of azole resistance and potential azole failure. Based on the reviewed trials, InLipAmB 12.5 mg twice weekly would be the preferred regimen.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author’s Note
The material in this manuscript has not been previously presented elsewhere.
Author Contributions
MJD, MAG, and BJG contributed to the project conception, the literature search, and manuscript preparation. All authors critically reviewed and approved the final manuscript.
