Abstract
Multiple sclerosis (MS) is a neurodegenerative disease characterized by neuroinflammation and demyelination that results in axon loss. Multiple sclerosis has been shown to be the result of an autoimmune response caused by a mixture of genetic and environmental factors. Dendritic cells are prominent antigen-presenting cells that interact with various molecules to regulate the immune system. The dysfunction of various features of immune regulation, including interleukins (ILs), CD4+ T cells, and suppressor of cytokine signaling (SOCS1), has been implicated in the pathogenesis of MS. T cells, particularly through the malfunction of B7-costimulatory pathways, have been shown to affect the progression of the disease. SOCS1 is important in regulating the function of T cells through its interactions with other nearby genes, especially CLEC16A, with abnormal decreases in SOCS1 expression leading to the exhibition of MS symptoms. The activation of IL-23 receptors on CD4+ T cells is pivotal to their differentiation into pathogenic TH17 cells. Several promising compounds that downregulate gene expression of IL-23 and IL-23R have been discovered but require further investigation for efficacy and safety. Given their role in the severity and progression of MS, therapies that decrease these dysregulations may ultimately decrease symptoms and in turn improve patients’ quality of life.
Introduction
Multiple sclerosis (MS) is a neurodegenerative disease characterized by inflammation of the central nervous system (CNS). It has been reported that in MS, there is an autoimmune response that leads to myelin deterioration and axonal loss, but the specific cause of the disease has yet to be determined. 1 One widely studied possible cause of MS is a triggered response to the Epstein-Barr virus (EBV).2,3 It has been speculated that the viral infection results in the upregulation of antigen-specific cytotoxic T cells, which remain throughout the body for several years postinfection. 2 When these cytotoxic T cells target self-peptides in the CNS, this often results in autoimmunity, such as MS. Although this link has been implicated in literature, conclusive evidence supporting this as the unique cause of MS is currently lacking.4,5
Although EBV may play a key role in disease onset, multiple lines of evidence suggest a genetic component to the onset and severity of the disease. Although the role of heredity is yet to be fully understood, variations in specific genes, especially those relating to inflammation, have been associated with an increased risk of MS and corresponds well with the increased inflammatory response observed in the advancement of MS.6–9 This is further supported by the increased incidence of MS in those with dysregulation of T-cell differentiation, particularly effector T cells.7,9
Naïve CD4+ T cells can mature into different effector T-cell types including helper T (TH) (TH1, TH2, and TH17) and regulatory T (Treg) cells. 10 IFN-γ–secreting TH1 cells and interleukin (IL) 17–secreting TH17 cells are present in MS lesions in the CNS and are known to be integral in the pathogenesis of MS in human and mouse models.11–14 Conversely, addition of Tregs in experimental autoimmune encephalomyelitis (EAE), a mouse model simulating MS, shows a tolerogenic effect, whereas depletion of Tregs increases symptom severity. 15 This differentiation of TH cells is initiated by the interactions between naïve CD4+ T-cell populations and antigen-presenting cells (APCs), primarily dendritic cells (DCs). 16 This communication involves the B7/T-cell costimulatory pathway and the stimulation of T cells with cytokines produced by DCs. Under normal circumstances, peripheral DCs in an immature state do not initiate TH cell differentiation and show very low expression of costimulatory molecules and cytokines.17,18 On receiving signals classified as pathogenic, immature DCs become activated and mature. This process is characterized by increased antigen uptake, increased class II major histocompatibility complex (MHCII) molecule expression, increased expression of costimulatory molecules (such as B7 molecules), and increased secretion of cytokines. 19 Different cytokines secreted by mature DCs are responsible for manifestation of the different subsets of TH cells. TH17 differentiation occurs via IL-6, IL-23, and IL-17 signaling; TH1 via IL-12 signaling, whereas Treg development occurs through interactions with IL-10.20–23
The notion that DCs are of critical importance in the pathogenesis of MS is well established. For instance, high amounts of CD8α+-type conventional DCs (cDCs) and plasmacytoid DCs (pDCs) are seen in the white matter and cerebrospinal fluid (CSF) of MS subjects.24,25 Patients with MS have been shown to have higher amounts of cDCs that secrete IL-12 and express CD80, both of which are markers associated with the differentiation of the pathogenic TH1 population. 26 Furthermore, cDCs acquired from patients with MS show an increased secretion of proinflammatory cytokines involved in MS pathogenesis, such as IL-6 and IL-23, compared with healthy individuals.27,28 It has been observed that populations of cDCs can infiltrate the CNS and facilitate epitope spreading in EAE mouse models. 29 As DCs interact with and are involved in different aspects of immune regulation that have been shown to increase risk of MS onset, the focus of this review is to highlight the role of immune regulation in the development and progression of MS, particularly regarding DCs, the associations of DCs and the B7/T-cell costimulatory pathway, as well as the resulting cytokine release and functions associated with T cells (see Table 1).
Important molecules dysregulated in MS pathogenesis.

Abbreviation: MS, multiple sclerosis.
This table illustrates the important molecules and pathways involved in immune regulation that play a role in the induction of MS on dysregulation.
Methods
A literature review was conducted using the database Web of Science with a combination of the key word “multiple sclerosis” with “dendritic cells,” “interleukins,” “cytokines,” and “costimulatory pathway.” From the 186 articles generated, those the authors did not have access to (33 articles) were excluded, resulting in the inclusion of 153 total articles considered for this review.
DCs and MS
Dendritic cells can be divided into 5 subsets that exist in mice and humans: cDCs, CD11b+-type cDCs, pDCs, Langerhans cells, and monocyte-derived DCs (MoDCs).30–37 Of these 5 subsets, pDCs and cDCs are of hematopoietic origin and stem from a DC progenitor cell that matures in response to FLT-3 signaling. 38 It has been shown that cDCs and pDCs are present in high amounts in white matter lesions of patients with MS,24,39 suggesting that they may play a role in the disease. Conventional DCs promote cytotoxic T-cell activation and primarily function to induce adaptive immune responses that target tumors and intracellular pathogens.30,38 CD11b+-type cDCs are responsible for CD4+ T-cell activation and promote humoral immunity, particularly regarding antibody production and cytokine secretion. 38
There is evidence supporting the involvement of the various subsets of DCs in the pathogenesis of MS. For example, in EAE, cDCs alone are able to sufficiently present antigen, activate autoreactive T cells, and facilitate CNS inflammation.29,40,41 All of these symptoms are significant, as they are each key features of EAE development and severity, which in turn would translate to MS severity in humans. It has also been demonstrated that pDCs have the ability to influence the differentiation of immunosuppressive Tregs that monitor self-tolerance to prevent autoimmunity. 42 In addition, increased pDCs have been observed in the inflamed regions of the CSF of patients with MS when compared with healthy controls,25,43 indicating that the upregulated immunosuppression demonstrated by the overexpression of pDCs exacerbates MS symptoms. This has been further supported by a recent study showing a greater number of pDCs in the CSF of patients in relapse compared with those who were in remission. 25 Together, this indicates that the influence of overexpressed pDCs on Tregs results in the suppression of the typical mechanism that monitors self-tolerance, contributing to autoimmunity.
On infection or inflammation, monocyte precursors are activated into MoDCs through granulocyte-macrophage colony-stimulating factor (GM-CSF), which shares characteristic qualities with hematopoietic-derived DCs. 44 Inflammatory monocytes extracted from GM-CSF–deficient mice are unable to develop into MoDCs, which indicates that GM-CSF is required for the generation of MoDCs. 45 Co-culturing these MoDCs with naïve CD4+ T cells resulted in the in vitro differentiation of TH17 cells. 37 This indicates that the interactions between these activated MoDCs and T cells result in the differentiation of T cells into TH17 cells, contributing to demyelination and inflammation at MS lesions. Consistent with the observed dysregulation of the IL-23/IL-17 axis in MS, MoDCs in the blood of patients with MS show increases in IL-23 synthesis in addition to increased ability to induce TH17 differentiation. 28 Based on this evidence, there is a correlation between DCs and MS. Dendritic cells interact with other molecules and when these communications are impaired, the result is the misregulation of various immune control mechanisms and the secretion of cytokines that lead to CNS inflammation and the progression of MS symptoms, as will be discussed below (see Figure 1).
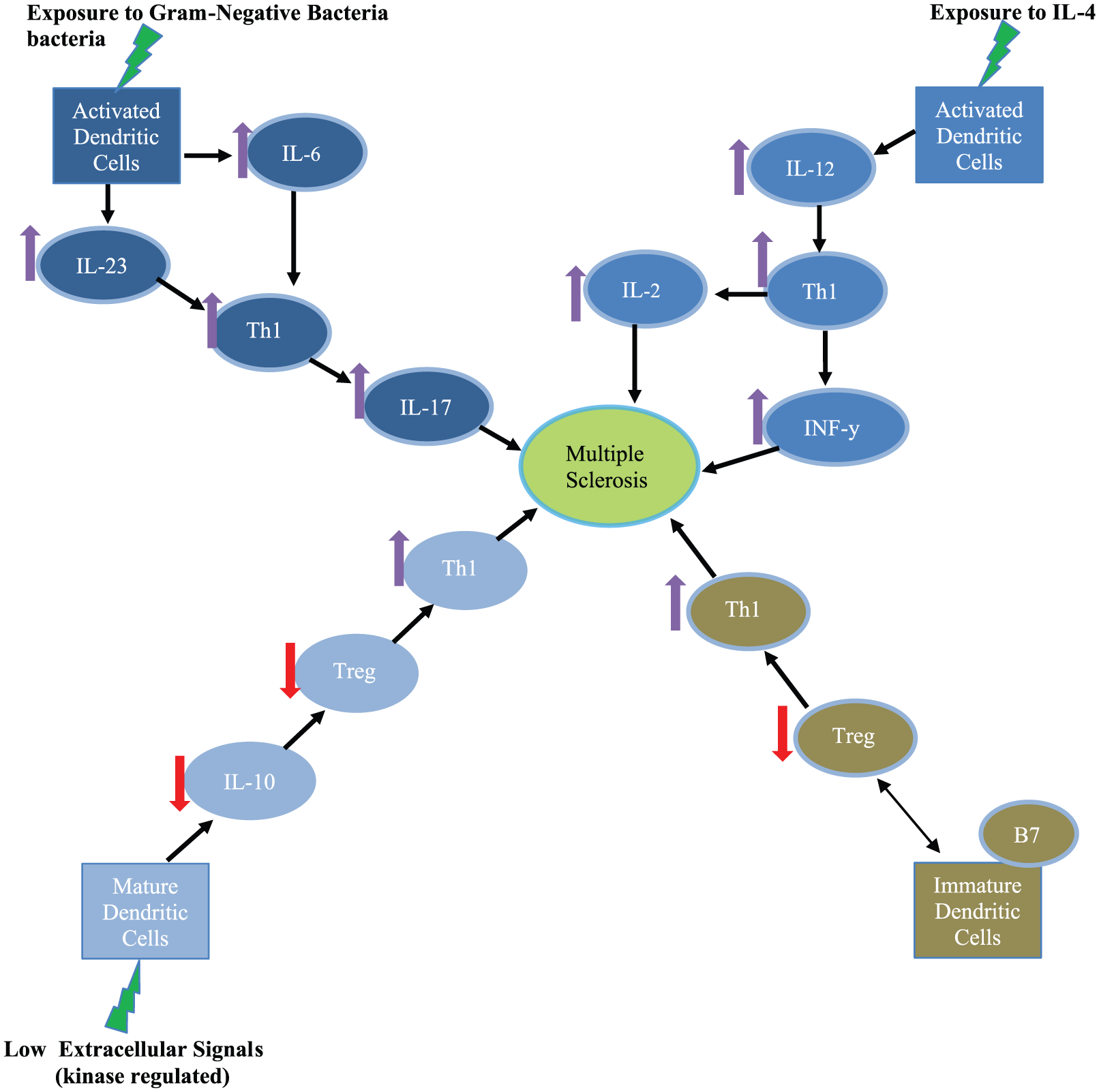
The pathogenesis of MS involves the dysfunction of immune regulation. Proper immune regulation depends on a delicate balance among the various immune responsive factors, which first requires their release from dendritic cells. Furthermore, the characteristics of dendritic cells (eg, maturity) will determine which of the various inflammatory cytokines (predominately interleukins) will be secreted. These cytokines will interact with naïve helper T cells at their surface and will promote either induction of or tolerance to autoimmunity. This figure illustrates pathways that have been implicated in the pathogenesis of MS on their dysfunction, as is highlighted (red arrows = downregulation, purple arrows = upregulation, green lightning bolt = trigger). IL indicates interleukin; MS, multiple sclerosis; TH, helper T; Tregs, regulatory T cells.
IL-23 and MS
Previous work has established that IL-23 is one of the key molecules responsible for maintaining the activity of TH17 lymphocytes.22,46,47 While transforming growth factor β and IL-6 are also involved in the differentiation of TH17 cells, stimulation with these cytokines alone is not enough to generate TH17 cells with effective pathogenicity. 22 Rather, it is IL-23 that is mainly released from DCs, subsequently acting on IL-23 receptors (IL-23R) found on naïve CD4+ T cells, inducing their specialization into pathogenic TH17 cells. 28 In EAE, the presence of IL-23 has been shown to increase IL-17 levels, which robustly enhances the manifestation of symptoms. 7 Moreover, IL-23 has also been found to be upregulated in the serum of patients with MS.48,49
It was previously hypothesized that MS, along with several other inflammatory autoimmune diseases, was completely facilitated by TH1 activation mediated by IL-12. The hypothesis that IL-12–mediated TH1 cells are the sole cause of autoimmune pathogenesis originates, at least in part, due to early studies focusing on the IL-12p40 subunit. For instance, it was observed in early studies that the knockout of IL-12p40 ameliorated the symptoms of MS in various models.50,51 This was accepted until several studies demonstrated that TH17 lymphocytes served a key role in the pathogenesis of several autoimmune diseases including MS.7,52-57 It is now known that IL-23 shares the IL-12p40 subunit with IL-12p70, with IL-12p40 bound to IL-23p19 rather than IL-12p35. 58 Furthermore, it has recently been shown that IL-23 may play a more important role than IL-12 in MS and other autoimmune diseases.59,60 For instance, removal of IL-23p19 was sufficient to cause resistance to EAE onset.52,60 Similarly, literature also shows that mice having dysfunction of several parts of the IL-12-TH1-IFN-γ pathway were still susceptible to EAE.50,51,61
Despite research supporting that IL-23 serves a greater role in autoimmunity than IL-12, studies continue to focus on the shared IL-12p40 subunit. For example, a study focusing on the potential therapeutic effects of Trabid downregulation of histone demethylase Jmjd2d discussed how this should result in suppression of IL-12p40 levels. 62 However, this broader TH1/TH17 focus could fall out of favor if more IL-23p19–specific therapeutic approaches to MS are discovered. A potential shift toward IL-23p19–specific therapeutic approaches is possible as research suggests that therapeutically targeting both TH1 and TH17 subsets results in unwanted side effects. In humans, it has been shown that autosomal recessive deficiencies in IL-12p40 and IL-12β1 subunits results in mendelian susceptibility to mycobacterial disease.63–68 Likewise, IL-12–deficient mice are susceptible to Listeria, Mycobacterium, Leishmania, and Toxoplasma, whereas IL-23–deficient mice are very resistant to these same pathogens.69,70 In addition, a recent study comparing the effects of anti–IL-12p40 therapy and anti–IL-23-p19 therapy showed that both were effective in reducing EAE symptoms. Anti–IL-12p40 therapy caused several side effects associated with the inhibition of both TH1 and TH17 functions, including the paradoxical pathogenic role of decreased IFN-γ levels. 71 The effects of anti–IL-12p40 therapies on patients with MS were observed in phase 2 clinical trials. However, the beneficial effects of targeting this subunit were not determined to be sufficient enough to warrant further development.72,73 Unfortunately, within the context of MS, there has also been an issue of clarity with IL-23p19–specific therapies. Interestingly, despite observing therapeutic success using antibodies that target IL-23p19 in other autoimmune diseases and EAE,71,74,75 there have been no such clinical trials using this approach in patients with MS to date. Such anti–IL-23p19 therapeutic options include tildrakizumab and guselkumab. Both of these monoclonal antibodies (mAbs) have specifically shown to be promising treatments for plaque scoriasis.76,77 Further studies focusing on these antibodies within the context of MS could prove to be a valuable asset to progressing treatment options.
Although there is an interest to use antibodies, it is important to note that even direct antagonism of IL-23p19 with mAbs comes with certain issues that need to be circumvented. Almost all protein-based therapeutic approaches produce neutralizing antibodies, causing a reduction in efficacy.78–83 For example, research observing the effects of repeated therapeutic administration of the mAb, natalizumab, shows loss of efficacy over time due to the body developing neutralizing antibodies toward mAbs.84,85 One approach used to avoid the issues associated with mAbs is RNA interference (RNAi), specifically RNAi of IL-23 expression within pathogenic APCs. RNA interference is a method of silencing gene expression posttranscriptionally. 86 In 2006, Vaknin-Dembinsky et al observed that MoDCs from patients with MS transfected with antisense oligos containing a specific complementary RNA sequence to IL-23 decreased the amount of biologically active IL-23. In addition, pathogenic CD4+ T cells of patients with MS cultured with the media from antisense-transfected DCs produced less IL-17. 28 Antisense oligonucleotides have recently been used in studies to target the messenger RNA (mRNA) transcripts of proteins believed to be important in autoimmune diseases such as Crohn disease.87,88 Moreover, a study conducted by Kalantari et al explored the effects of IL-23 knockdown by RNAi in bone marrow–derived DCs (BMDCs), one of the main contributors to IL-23 production and TH17 differentiation in autoimmune diseases. The BMDCs of EAE mice were extracted and transduced with lentiviral vectors engineered to express small hairpin RNA (shRNA) that complemented sequences of IL-23p19 RNA as well as CD40 RNA. This eliminated the barrier of developing an administration technique that was practical in a clinical setting. When transduced, BMDCs are co-cultured with CD4+ T cells of EAE mice, and a decrease in T-cell proliferation to the pathogenic subset can be observed. 89 In addition, IL-23p19–specific shRNA transduction appears to aid in the maturation of BMDCs toward the tolerogenic subset, increasing IL-10 production, whereas the production of IL-6, IL-12, and IFN-γ is greatly reduced. 90 Unfortunately, despite the observed success of IL-23–specific antisense treatment, there have not been further studies or any clinical trials that test this specific therapeutic approach. The next step in RNAi therapies targeting IL-23 would be further studies replicating the lentiviral vector approach to better understand the potential effectiveness and pitfalls of implementing this as a clinical treatment.
As another alternative to developing antibodies that target the IL-23p19 subunit, associated adenovirus (AAV) vector containing a soluble recombinant IL-23 receptor (sIL-23R) homology region was developed. 91 Expression of this inactive and soluble form of IL-23R requires one injection when administered via an AAV8 vector, thus avoiding continuous administration. The injection of sIL-23R-containing AAV8 into mice improved EAE clinical symptoms by blocking the IL-23/IL-23R interaction via competitive inhibition. Specifically, AAV8 administration of sIL-23R was shown to delay clinical onset, slow disease progression, reduce inflammatory infiltration, and reduce demyelination in the CNS. 92 From previous studies revealing that AAV8 vectors only function in the periphery, it was presumed that the inhibitory effects of sIL-23R did not occur in the CNS, but rather inhibition of IL-23 signaling in the periphery allowed less IL-23 to enter the CNS.93,94
However, several questions have been raised that have yet to be answered from these recent findings. In particular, the effects that IL-23R has on inflammatory cytokine transcription factors must be further explored. In mice and humans, sIL-23R administration was found to decrease TH17 differentiation and STAT3 phosphorylation.92,95 STAT3 of the JAK-STAT pathway is an important transcription factor downstream of IL-23R and IL-6R signaling.96,97 In the initial stages of TH17 development, solely IL-6R signaling results in the phosphorylation of STAT3.96,97 Phosphorylation of STAT3 results in its association with a transcription factor complex that directly controls the genes for IL-17A, IL-17F, and IL-23R. The upregulation of IL-23R then enhances IL-23R–mediated STAT3 phosphorylation in a positive feedback manner, stabilizing the production of IL-17 in pathogenic TH17 cells.96,97 Contrary to these observations in the IL-23R-STAT3 pathway, gene expressions induced by STAT3 activation (such as IL-17A, IL-17F, and IL-23R) were not decreased in media of myelin oligodendrocyte glycoprotein (MOG40-55)–cultured splenocytes from EAE mice following sIL-23R treatment compared with untreated MOG40-55 culture media. Instead, an increase in IFN-γ expression correlated with amelioration of EAE symptoms was observed. 92 The lack of change in cytokine levels suggests that a transcription factor complex regulates the fate of pathogenic TH17 commitment rather than single independent transcription factors. 98 Regarding the increase in the expression of IFN-γ in sIL-23R–treated mice, the accompanying reduction in EAE symptoms that was observed is consistent with current literature suggesting that IFN-γ is a negative regulator of IL-23/IL-17 immune responses.99–104 However, there is also literature reporting positive associations with CNS lesions in EAE as well as MS and higher levels of IFN-γ, suggesting a pathogenic role.22,50,105–107 To date, the specific role of IFN-γ in the pathogenicity of MS seems paradoxical as the role of IFN-γ changes depending on the stage of the disease.108–110 Because there are no significant changes seen in cytokine levels except IFN-γ, it is possible that inhibition of the IL-23/IL-23R interaction promotes a compensatory mechanism whereby IFN-γ increases. It is also possible that replication of the experiment that Miralles et al 92 performed could yield changes in cytokine levels. Seeing as this particular therapeutic approach to the negative regulation of TH17 cells is rather new, further clarification of the exact mechanism of action of sIL-23R on the amelioration of EAE symptoms is warranted.
Associations between MS and the B7/T-Cell Costimulatory Pathway
T-cell costimulatory pathways, particularly the pathway involving B7 molecules (B7-1/CD80 and B7-2/CD86) and the protein receptors they act on (CTLA-4 and CD28), have been implicated in the pathogenesis of MS,111,112 but their role in autoimmune diseases has been highly contested within the literature. A few recent studies have suggested that when faulty, the signals involved in the B7-CD28/CTLA-4 costimulatory pathway can trigger the activation of autoreactive T cells that contribute to the development of MS through the alteration of Treg activity and the induction of pathogenic TH17 cells.113,114 To become activated, T cells require 2 signals,115,116 the first of which is antigen-specific due to the communication between the T-cell receptor (TCR) and an antigenic peptide, which is presented by an APC on an MHC molecule. The primary APCs that function in relation to this pathway are DCs, as mentioned previously. The second signal, which directly determines the functional response of the T cells to the TCR-MHC binding, occurs through the interaction of the CTLA-4 and CD28 receptors and the B7 molecules that are already expressed in low levels on DCs.111,117 Alternatively, binding of CTLA-4 to the B7 molecules inhibits an immune response by downregulating the costimulatory activation through the prevention of CD28 binding and reducing the antigen-presenting ability of APCs, which diminishes the triggering of T-cell activation.118–121 The balance of T-cell activation is preserved by the immunomodulation activities of DCs in promoting immunity and/or tolerance. 122 When DCs are dysfunctional, it can lead to aberrant T-cell activation that prevents the body from properly reacting to both threats and benign targets.
Mouse models strengthen the association between the T-cell costimulatory pathway and MS. Using the EAE model, mice were treated with a combination of CTLA-4-Ig (or abatacept, a B7 antagonist that binds to B7 molecules to prevent T-cell stimulation) and MOG35-55. Following treatment, EAE was exacerbated with more pronounced effects occurring in vivo than in vitro. 8 It has been shown that ipilimumab, a drug used to treat metastatic melanoma through the inhibition of CTLA-4, and subsequently the downregulation of B7 molecules, mediates the development of MS based on an observed increase in disease progression through clinical and magnetic resonance imaging activity. 118 This information, in conjunction with 2 other case studies that showed similar effects in patients undergoing treatment with ipilimumab, suggests that CTLA-4 serves a protective role against MS through its typical inhibitory activity in T cells, which is lost once CTLA-4 is downregulated.123,124 CTLA-4 is constitutively expressed on Tregs and binding to the B7 molecules present on the surface of DCs has previously been shown to upregulate CTLA-4 once T cells are activated, which suppresses immune activation. 125 When CTLA-4 is downregulated, it has been shown to lose its ability to inhibit Tregs, which causes these cells to become overactive and results in the dysfunction of effector T cells, which in turn can promote autoimmunity. 126 When CTLA-4 is blocked, it has been shown to induce differentiation of naïve T cells into TH17 cells, which have been implicated in the pathogenesis of MS. 127 Other studies have recently challenged the position that CTLA-4 has a critical role in the onset or progression of MS. In a recent study, patients treated with abatacept, a B7 antagonist, did not see a therapeutic effect. 128 These results are in direct contrast to previous findings suggesting abatacept is a potential therapeutic regulator of neuroinflammation.129,130 These contradictory findings may be explained by low disease activity prior to treatment.
Furthermore, specific polymorphisms of CTLA-4 have been reported by some groups to have varying effects on risk of MS, particularly the +49 A/G*G-CT60*G haplotype. One study using a Flemish cohort found a significant increase in the +49 G allele in patients with MS compared with their control group. 120 In contrast, studies performed using Italian, Japanese, Iranian, German, Hungarian, and Polish cohorts were unable to conclude that there was an association between CTLA-4 polymorphisms and MS in their patients.131–134 It should be noted that the sample sizes for some of these studies were small. Based on the differing groups in which a connection between CTLA-4 and MS was observed, the association is perhaps indicative of an ethnic component, which requires further investigation to elucidate the true nature of the relationship.
PD-1/PD-L1 Association with MS
Programmed death-ligand 1 (PD-L1 or B7-H1) is another member of the B7-costimulatory pathway that has been linked to MS. PD-L1 is constitutively expressed on DCs and binds to the programmed death receptor (PD-1) on activated T cells, which then upregulates the production of inflammatory cytokines, such as IL-10. It also reduces T-cell proliferation by suppressing TH1 cell differentiation and DC function. 135 This pathway is important in subduing T-cell activity, known as T-cell exhaustion, when a virus or other abnormality is present in the CNS to reduce neuroinflammation. 136 Once the T cell is exhausted, it is only weakly activated, which leaves PD-1 better capable of limiting the T-cell response. 137 PD-1 is also vital in regulating tolerance and autoimmunity. PD-L1 is upregulated in MS lesions, which results in the downregulation of T-cell response and the prevention of autoimmunity.135,138 One hypothesized role of PD-1 is a suppressive effect on APCs, particularly DCs, that infiltrate the CNS, which results in the downregulation of TH17 cells. 139 In downregulating this type of pathogenic T cell, PD-1 serves as a modulator of immunity, which in turn reinforces its role in preventing the occurrence of disease.
One important aspect of PD-L1/PD-1 is regarding prominent MS treatments, particularly interferons or signaling proteins released by cells in response to pathogens. 140 IFN-β is most widely used in MS treatment and has been shown in vivo to act through the upregulation of PD-L1, which results in a decrease in neuroinflammation and a therapeutic effect for patients with MS.140,141 A previous study illustrated that PD-L1 expression inversely correlates with strong CNS inflammation in MS plaques, further suggesting that PD-L1 acts in a protective manner, downregulating the inflammation associated with T-cell extension into the CNS. 142
Several studies have shown a correlation between the upregulated expression of PD-1/PD-L1 and the associated MS stage using the EAE mouse model. A study using in vitro techniques first found that PD-L1 overexpression by DCs had the potential to prevent the induction of EAE. 143 These data were then reinforced by later in vivo studies, where MS was induced following MOG immunization in PD-L1 knockout mice and more severe EAE developed relative to the control. 135 Similarly, Ortler et al 142 were also able to show using flow cytometry that following immunization with MOG in PD-L1 knockout mice, there was a significant increase in T-cell infiltration in the brain, indicating a correlation between the increased severity of EAE and absence of PD-L1 in mouse models. Other studies have shown that T cells interact with DCs, which then leads to the upregulation of PD-1/PD-L1 expression.122,144 As stated previously, elevated PD-1/PD-L1 levels can limit the severity of EAE, if not prevent its induction. This indicates that PD-1 overexpression due to its interactions with DCs may hold therapeutic value. Based on this evidence, one possible avenue of MS treatment may lie in the upregulation of PD-1/PD-L1, which needs to be further explored in later research.
Suppressor of Cytokine Signaling and its Association with MS
A key gene involved in the function of TH cells and Tregs is SOCS1, a member of the SOCS family. In general, SOCS genes are important in the regulation of cytokine signaling and autoimmune responses through the JAK/STAT pathway.145–147 SOCS1 plays a role in the regulation of immune cell homeostasis as well as in inflammation. 148 SOCS1 suppresses DC activity by inhibition of STAT1, which normally activates DCs. 149 SOCS1 has been shown to play a key role in regulating DCs regarding autoimmunity, as SOCS1-deficient DCs are overly susceptible to IL-4 and IFN-γ, 2 inflammatory cytokines. This enables the production of autoreactive antibodies and systemic autoimmunity. 150 Single-nucleotide polymorphisms (SNPs) near SOCS1 have an association with MS by reducing SOCS1 gene expression and initiating the differentiation of T cells to a pathogenic TH17 phenotype, increasing in the risk of MS onset as described earlier.151–153 Research has shown that SNPs that cause the loss of SOCS1 function do not act through nearby genes that associate with SOCS1. Instead, SOCS1-deficient Tregs lose their suppressive activity. This causes the production of increased levels of IL-17, which induces the specialization of TH17 from naïve T cells.151,153 This evidence indicates that a main role of SOCS1 is to suppress systemic autoimmunity, such as is present in MS, through its standard interactions with DCs.
Another gene expressed by APCs, particularly DCs, is C-type lectin domain family 16A (CLEC16A), which associates with SOCS1 in regulating immune response.149,150 Polymorphisms of this MS risk allele (especially a SNP at rs12708716 found within intron 19 of CLEC16A that results in reduced SOCS1 expression) influence the susceptibility for various autoimmune diseases, specifically MS, through the reduction in SOCS1 protein expression in the thymus. 9 It has been reported that in the absence of the SOCS1 protein, mice experienced systemic inflammation as well as the development of thymocytes. 148 These symptoms are similar to those observed in MS, providing further evidence that the SOCS1 gene plays an important role in the pathogenesis of MS, with reduction in SOCS1 expressions leaving DCs over-responsive to cytokines and resulting in autoimmunity as discussed above. Based on this evidence, SOCS1 and its relationship with CLEC16A and the associated effects on DCs should be further explored. Such studies would aid in determining whether there is therapeutic potential in new treatments for MS geared toward the upregulation of SOCS1 protein expression through targeting of the associated SOCS1 and CLEC16A genes.
Summary
Multiple sclerosis is a neurodegenerative disease characterized by inflammation of the CNS that results in demyelination. Although the cause of MS is still unknown, it is believed to result from a mixture of viral, genetic, and environmental factors. It has largely been attributed to an autoimmune response stemming from EBV due to its prevalence in patients with MS, but immune misregulation plays a clear role in the presentation of disease symptoms. Both TH1 and TH17 cells are important to MS pathogenesis and are known to primarily be stimulated by DCs. 16 This pathogenic stimulation is a combination of myelin-specific antigen presentation, costimulation, and cytokine signaling.17–19 Therefore, understanding and altering the interaction between DCs and CD4+ T cells is important for developing possible treatments for MS.
Cytokine signaling involving TH cells and DCs likely plays a significant role in MS pathology. The suppression of cytokine signaling between DCs and CD4+ TH cells plays a large role in MS progression through its associations with other genes, which in turn helps T cells function within the immune system.28,152 When cytokine function is abnormal, this leads to an autoimmune reaction within the body. Thus, cytokine regulation is a good potential therapeutic target for patients with MS. 9 The upregulation of IL-23 is widely accepted as a key checkpoint in the pathogenesis of MS because of its protective and differentiative role in TH17 cells. 7 Finding ways to decrease the elevated serum and CNS levels of IL-23 in MS and EAE models is a major point of interest. Therapeutic approaches such as IL-23p19–specific mAbs, antisense oligos against IL-23 mRNA, and sIL-23R have shown to downregulate the expression of IL-23 in MS models.28,89,92 However, further research should be done in the extracted cells of patients with MS to elucidate the role of these potential treatments in disease progression to develop effective clinical versions to use as treatments. In addition, further study into the IL-23R-STAT3 pathway and its role in IL-17 and IL-23R regulation is a promising avenue that could lead to improved treatment of MS.92,98
Multiple sclerosis onset has also been linked to the B7/T-cell costimulatory pathway, particularly the B7-CD28/CTLA-4 costimulatory pathway. The B7 molecules, CD80 and CD86, interact with receptors found on DCs and when the balance of these interacting proteins is off, exacerbated symptoms of MS often develop. Although it has been suggested that CTLA-4 serves a protective role in the brain that leads to MS once inhibited,123,124 there is conflicting research regarding this,133,134 calling for additional study to determine the true nature of this relationship. There has also been a lack of consistency in the effects of CTLA-4 polymorphisms on varying cohorts,131–134 which indicates a possible ethnic relationship between MS and variations in CTLA-4. The PD-L1/PD-1 costimulatory pathway has also been recently reported to play a role in the progression of MS when downregulated by DCs. Therefore, using therapies that increase PD-1/PD-L1 activity holds promise for slowing MS disease state.
In this review, we have illustrated the need for more research into the impact of DCs on immune regulation in MS. By looking at the interactions between DCs and T cells, there is opportunity to further elucidate the role of ILs, CD4+ T cells, PD-1/PD-L1, CTLA-4, and SOCS1 in MS onset and progression due to the irregular activity found in each during disease. More research into the role of the PD-L1/PD-1 costimulatory pathway may result in further treatment avenues to slow MS progression. We have also demonstrated a need to further analyze the role of IL-23 in the differentiation of TH17 cells, enabling greater understanding of the role of IL-23R in MS. The effects of the upregulation of SOCS1 in patients having an autoimmune disease also require deeper investigation. Continued focus in these areas may result in potential therapeutic value for patients living with MS, ultimately having a long-term impact and improving their quality of life.
Footnotes
Acknowledgements
The authors would like to thank Tia M Spagnuolo, MS, CF-SLP; Teresa Wasiluk, MS; and John Forsberg, MS, for reviewing the manuscript. They would also like to thank Austin Ford for his initial thoughts on the manuscript.
Peer review:
Three peer reviewers contributed to the peer review report. Reviewers’ reports totaled 515 words, excluding any confidential comments to the academic editor.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
GS and AP conceived the concept, wrote the first draft of the manuscript, contributed to the writing of the manuscript, and jointly developed the structure and arguments for the paper. GS, AP, and TW agree with manuscript conclusions and made critical revisions. GS contributed to the formatting and compilation of manuscript. All authors reviewed and approved the final manuscript.
